Intro to Spinal Orthopedic Tests Dr Michael P










































































- Slides: 102

Intro to Spinal Orthopedic Tests Dr. Michael P. Gillespie

Vertebrobasilar Circulation Assessment Vascular Insufficiency may be aggravated by positional change in the cervical spine. Assessment of the vertebrobasilar circulation must be done if cervical adjustment or manipulation is to be performed.

Predispositions to Cerebrovascular Accidents Headaches, migraine Dizziness Sudden severe head or neck pain Hypertensive

Predispositions to Cerebrovascular Accidents Cigarette smoking Oral Contraceptives Obesity Diabetes

Cerebrobasilar Testing Positional change in the cervical spine compresses the vertebral artery at the atlantoaxial junction on the side opposite of rotation. In the normal patient, the diminished blood flow does not cause any neurological symptoms, such as dizziness, nausea, tinnitus, faintness, or nystagmus.

Clinical Signs and Symptoms of Cerebrovasular Episodes Vertigo, dizziness, giddiness, light-headedness Drop attacks, loss of consciousness Diplopia Dysarthria

Clinical Signs and Symptoms of Cerebrovasular Episodes Dysphagia Ataxia of gait Nausea, vomiting Numbness on one side of the face Nystagmus

Barre-Lieou Sign Procedure: Patient rotates head from one side to the other. Positive Test: Vertigo, dizziness, visual blurring, nausea, faintness, nystagmus. Structure affected: Vertebral artery on the same side of head rotation. Consider patency of the carotid arteries and the communicating cerebral artery circle.

Barre-Lieou Sign

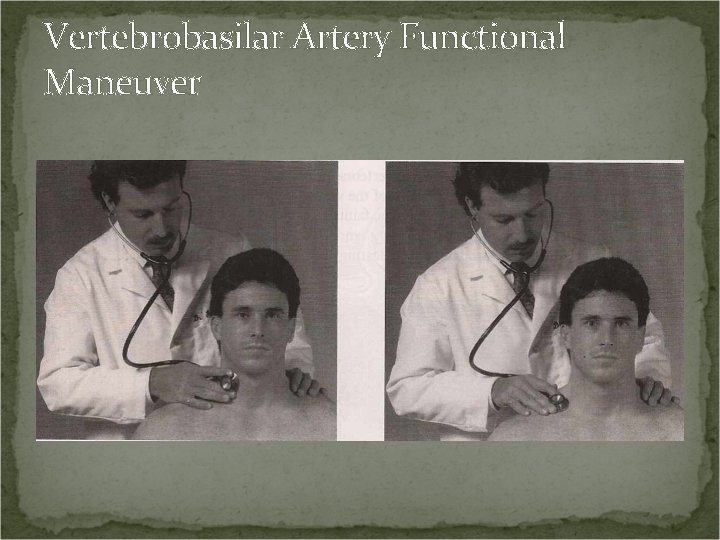
Vertebrobasilar Artery Functional Maneuver Procedure: Palpate and auscultate the carotid arteries for pulsations and bruits. Instruct the patient to rotate and hyperextend the head.

Vertebrobasilar Artery Functional Maneuver Positive Test: If pulsation or bruits are present at either the carotid or subclavian arteries the test is positive. Structures Affected: It may indicate stenosis or compression of the carotid or subclavian arteries.

Vertebrobasilar Artery Functional Maneuver

Dekleyn’s Test Procedure: Patient supine, head off table. Instruct pt. to hyperextend and rotate head. Hold 15 to 30 seconds. Repeat opposite. Positive Test: Vertigo, dizziness, visual blurring, nausea, faintness, and nystagmus. Structures Affected: Vertebral, basilar, or carotid artery stenosis or compression.

Dekleyn’s Test

Clinical Signs and Symptoms of Cervical Strain or Sprain Cervical and upper back pain Cervical and upper back stiffness Cervical and upper trapezius tightness Reduced cervical range of motion Cervical extensor spasm

Differentiating Between Strain and Sprain Cervical strain is an irritation and spasm of the muscles of the cervical spine with or without partial muscle fiber tearing. Cervical sprain is a wrenching of the joints of the cervical spine with partial tearing of its ligaments.

Categories of Strain Mild: Slight disruption of muscle fibers with no appreciable hemorrhage and minimal amounts of swelling and edema.

Categories of Strain Moderate: Laceration of muscle fibers with an appreciable amount of hemorrhage into the surrounding tissues and a moderate amount of swelling and edema. Severe: Complete disruption of the muscle tendon unit, possibly with tearing of the tendon from the bone or a rupture of the muscle through its belly.

Categories of Sprain Mild: Slight tears of a few ligamentous fibers. Moderate: More sever tearing of ligamentous fibers but not complete separation of the ligament.

Categories of Sprain Severe: Complete tearing of a ligament from its attachments. Avulsion: A ligament that attaches to a bone is pulled loose with a fragment of that bone.

O’Donoghue’s Maneuver Procedure: Patient seated. Put the cervical spine through resisted range of motion, then through passive range of motion. Positive Test: Pain during resisted range of motion or isometric muscle contraction signifies muscle strain. Pain during passive range of motion may indicate a sprain of any of the cervical ligaments.

O’Donoghue’s Maneuver Structures Affected: Cervical spinal muscles and/or cervical spinal ligaments. Since resisted range of motion mainly stresses muscles and passive range of motion mainly stresses ligaments, you should be able to determine between strain and sprain or a combination thereof.

O’Donoghue’s Maneuver

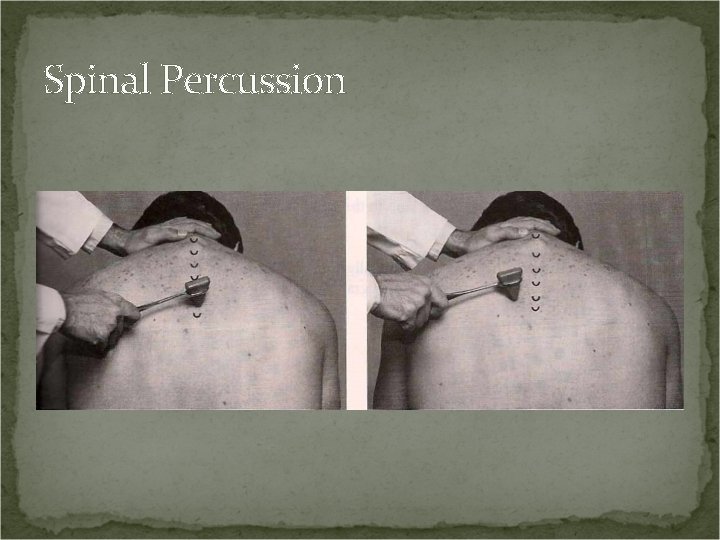
Spinal Percussion Test Procedure: Patient seated. Head slightly flexed, percuss the spinous process and associated musculature of each cervical vertebrae with a reflex hammer.

Spinal Percussion Test Positive Test: Local pain may be a fractured vertebra with no neurological compromise. Radicular pain may be a fractured vertebra with neurological compromise or a disc lesion with neurological compromise. A ligamentous sprain could also elicit pain upon percussion of the spinous processes.

Spinal Percussion Test

Rust’s Sign Procedure: A patient with severe injury to the upper cervical spine will grasp the head with both hands to support the weight of the head on the cervical spine. The supine patient will support the head while attempting to rise. Positive Sign: The patient stabilizes the head. It might include slight traction.

Rust’s Sign Structures Affected: This could represent severe muscular strain, ligamentous instability, posterior disc defect, upper cervical fracture, or dislocation.

Rust’s Sign

Cervical Instability Clinical Signs and Symptoms Severe cervical pain. Patient stabilizing the head. Little or no cervical motion. Severe cervical muscle spasm. Upper extremity neurological dysfunction. Lower extremity neurological dysfunction.

Space-Occupying Lesions Clinical Signs and Symptoms Cervical pain. Upper extremity neurological symptoms. Lower extremity neurological symptoms.

Valsalva’s Maneuver Procedure: Have the patient bear down as if defecating and focus the bulk of the stress on the cervical spine. Ask if the patient feels pain and have them point to the location.

Valsalva’s Maneuver Positive Test: Local pain with increased pressure could indicate a space-occupying lesion (e. g. disc defect, mass, osteophyte) in the cervical canal or foramen.

Valsalva’s Maneuver

Dejerine’s Sign Procedure: Patient seated. Instruct them to cough, sneeze, and bear down as if defecating (Valsalva’s maneuver). Positive Test: Local pain or pain radiating to the shoulders or upper extremities indicates an increase in intrathecal pressure. Structures Affected: Space-occupying lesion.

Cervical Neurological Compression and Irritation Clinical Signs and Symptoms Cervical pain. Upper extremity radicular pain. Loss of upper extremity sensation. Loss of upper extremity reflexes. Loss of upper extremity muscle strength.

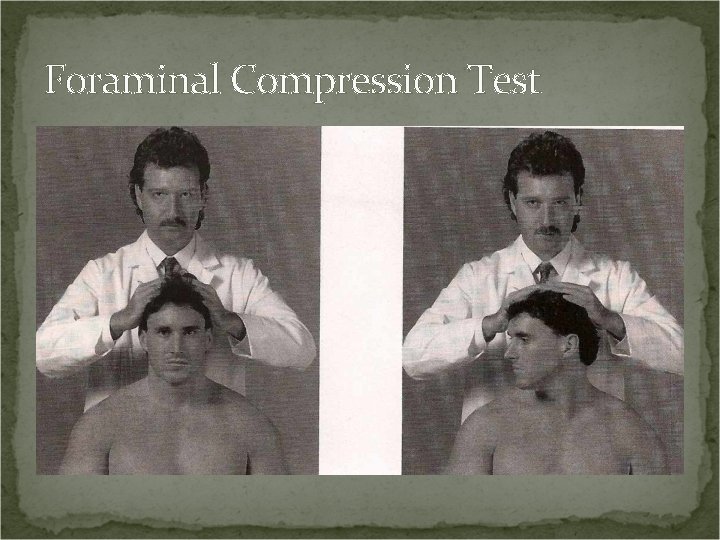
Foraminal Compression Test Procedure: Patient seated. Exert strong downward pressure on the head. Repeat with b/l rotation. Positive Test: Local pain may indicate foraminal encroachment without nerve root pressure or apophyseal capsulitis. Radicular pain may indicate pressure on a nerve root.

Foraminal Compression Test

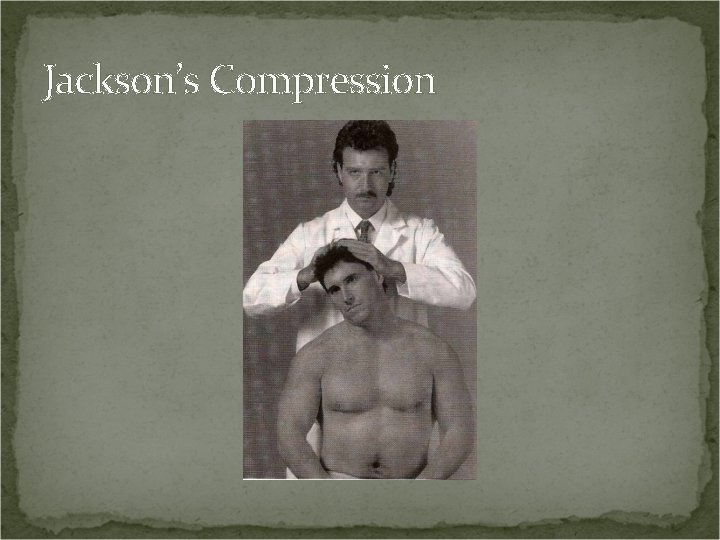
Jackson’s Compression Procedure: Laterally flex the head and exert strong downward pressure. Perform b/l. Positive Test: Local pain may indicate foraminal encroachment without nerve pressure or apophyseal joint pathology. Radicular pain may indicate pressure on a nerve root.

Jackson’s Compression

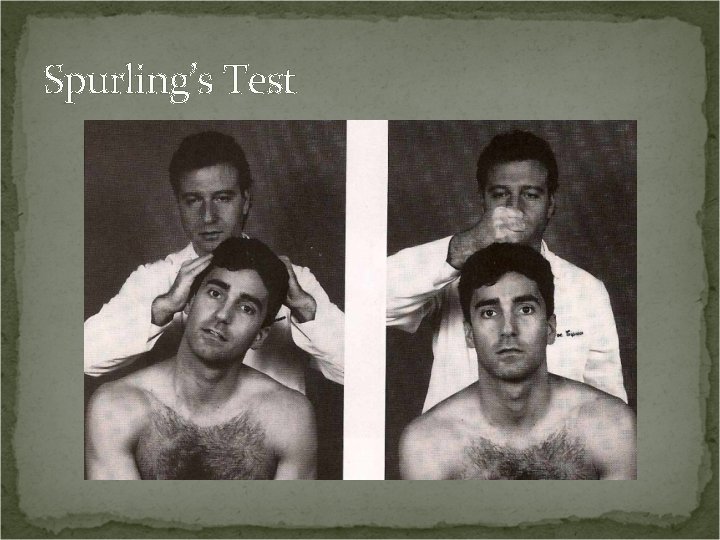
Spurling’s Test Procedure: Laterally flex the patient’s head and gradually apply strong downward pressure. If no pain is elicited, put the patient’s head in a neutral position and deliver a vertical blow to the uppermost portion of the patient’s head.

Spurling’s Test Positive Test: Local pain indicates facet joint involvement. Radicular pain indicates nerve root pressure.

Spurling’s Test

Distraction Test Procedure: Grasp beneath the mastoid processes and press up on the patient’s head. This removes the weight of the patient’s head on the neck.

Distraction Test Positive Test: If local pain increases, suspect muscle strain, spasm, ligamentous sprain, or facet capsulitis. Relief of radicular pain indicates either foraminal encroachment or a disc defect.

Distraction Test

Shoulder Abduction Test (Bakody’s Sign) Procedure: The patient should abduct the arm and place the hand on top of the head. Positive Test: A decrease or relief of the patient’s symptoms indicates a cervical extradural compression problem (i. e. herniated disc, epidural vein compression, or nerve root compression).

Shoulder Abduction Test (Bakody’s Sign)

Thoracic Spine

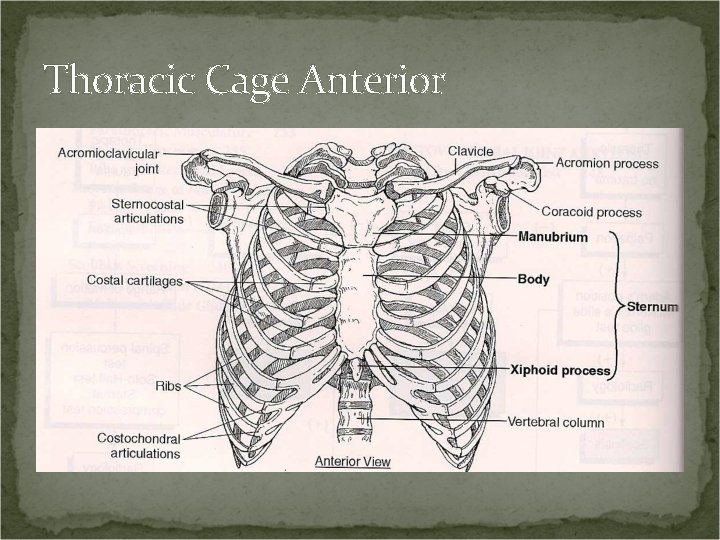
Thoracic Cage Anterior

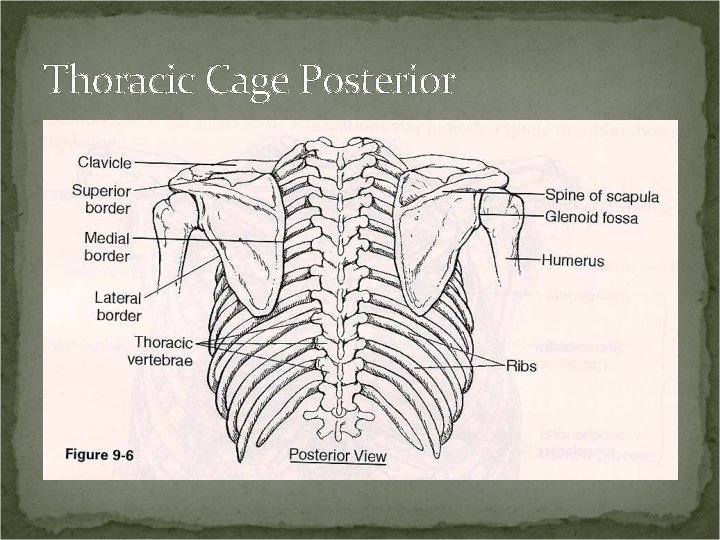
Thoracic Cage Posterior

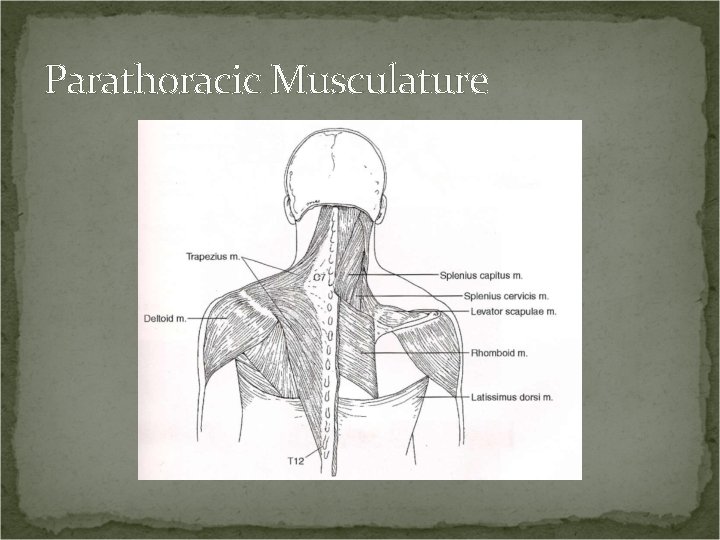
Parathoracic Musculature

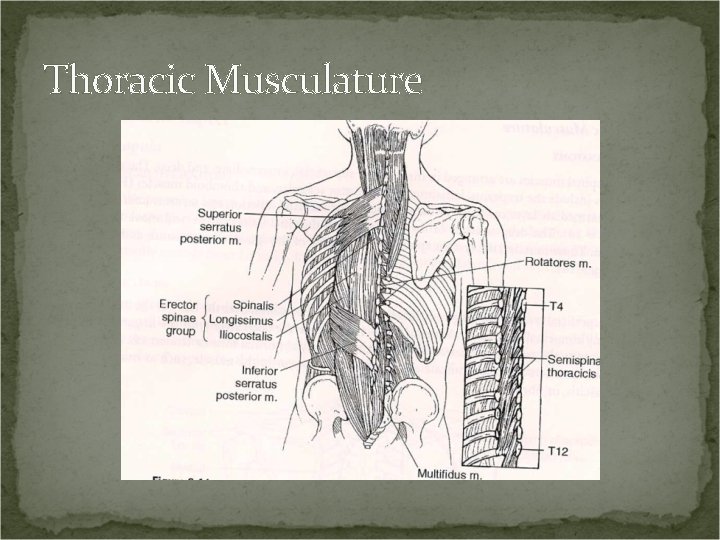
Thoracic Musculature

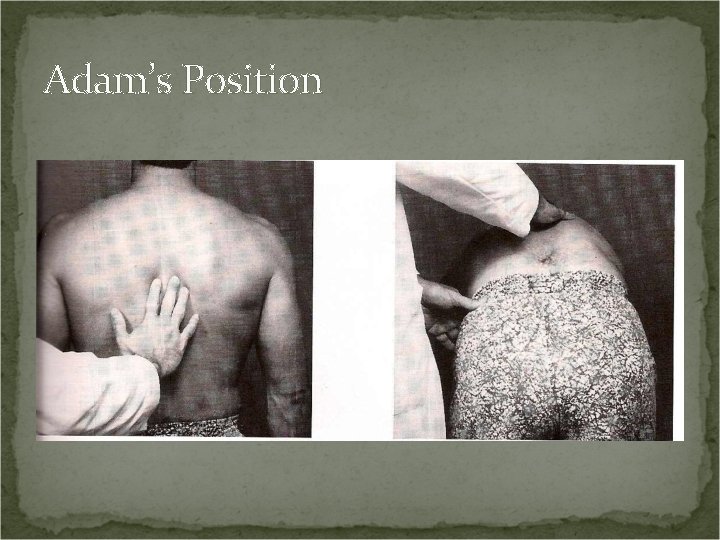
Adam’s Position Procedure: Patient standing. Stand directly behind and inspect for scoliosis, hyperkyphosis, or kyphoscoliosis. Next. Patient should flex forward at hips. Inspect again. Positive Test: If scoliosis, hyperkyphosis, or kyphoscoliosis reduces with forward bending: poor posture, overdevelopment of unilateral spinal and/or upper extremity musculature, nerve root compromise, leg length deficiency, or hip contracture.

Adam’s Position If scoliosis, hyperkyphosis, or kyphoscoliosis does not reduce with forward bending: structural deformity (i. e. hemivertebra, compression fracture) or idiopathic scoliosis.

Adam’s Position

Spinal Percussion Procedure: Patient seated, head slightly flexed, percuss the spinous processes and associated musculature. Positive Test: Local pain may indicate a fractured vertebra without neurological compromise or ligamentous sprain. Radicular pain may indicate a fractured vertebra with neurological compromise or a disc defect with neurological compromise.

Spinal Percussion

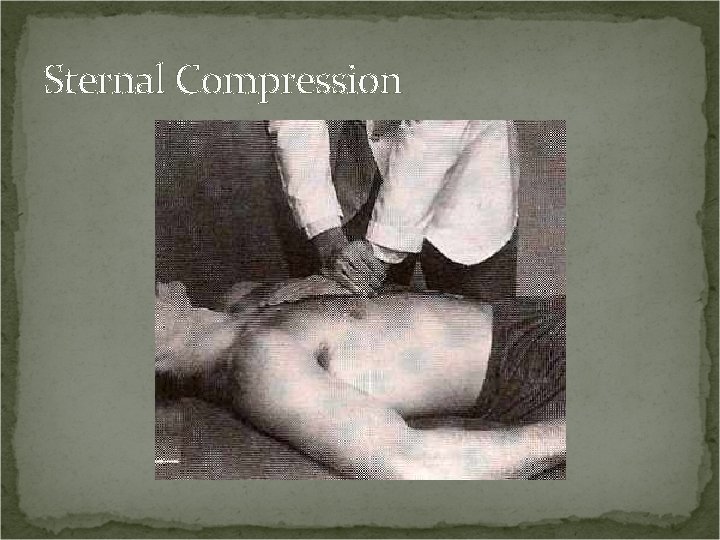
Sternal Compression Procedure: Patient supine. Push down on sternum. Positive Test: Pressure on the sternum compresses the lateral borders of the ribs. If a fracture is present here, pain will be produced or exacerbated. Note: If trauma has occurred and you suspect a fractured rib, radiographs should be performed first before performing this test.

Sternal Compression

Beevor’s Sign Procedure: Patient supine. Patient should hook fingers behind neck and raise the head towards the feet. Mimic a sit-up.

Beevor’s Sign Positive Test: The umbilicus will not move in a patient with not thoracic root lesion. Umbilicus moves superiorly: bilateral T 10 – T 12 lesion Umbilicus moves superiorly and laterally: Unilateral T 10 – T 12 nerve root lesion on opposite side. Umbilicus moves inferiorly: bilateral T 7 – T 10 nerve root lesion. Umbilicus moves inferiorly and laterally: Unilateral T 7 – T 10 nerve root lesion of the opposite side.

Beevor’s Sign

Schepelmann’s Sign Procedure: Seated patient. Flex at waist to right and left. Positive Test: Pain on side of lateral bending: intercostal neuritis. Pain on opposite side of lateral bending: fibrous inflammation of the pleura or intercostal sprain.

Schepelmann’s Sign

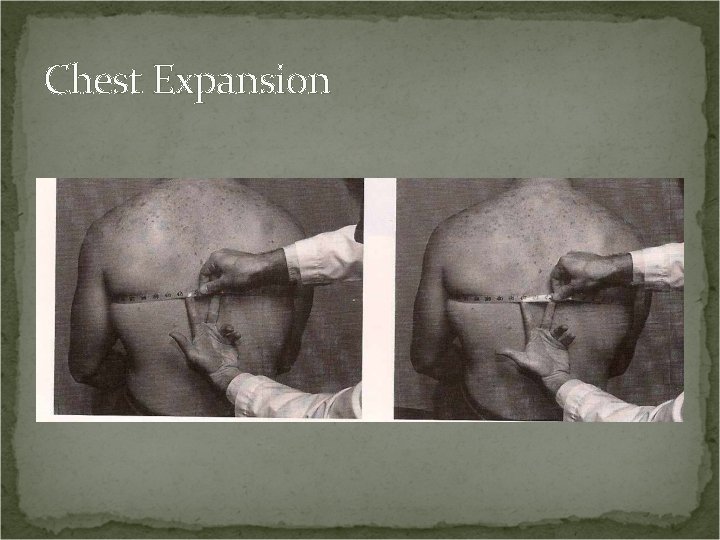
Chest Expansion Procedure: Patient seated. Place a tape measure around the patient’s chest at the level of the nipple. Instruct patient to exhale and record the measurement. Instruct the patient to inhale maximally and record the measurement.

Chest Expansion Positive Test: Normal chest expansion for a man is 2 inches or more. Normal chest expansion for a woman is 1 inch or more. A decrease in chest expansion indicates an ankylosing condition at the costotransverse or costovertebral articulation.

Chest Expansion

Lumbar Spine Orthopedic Tests

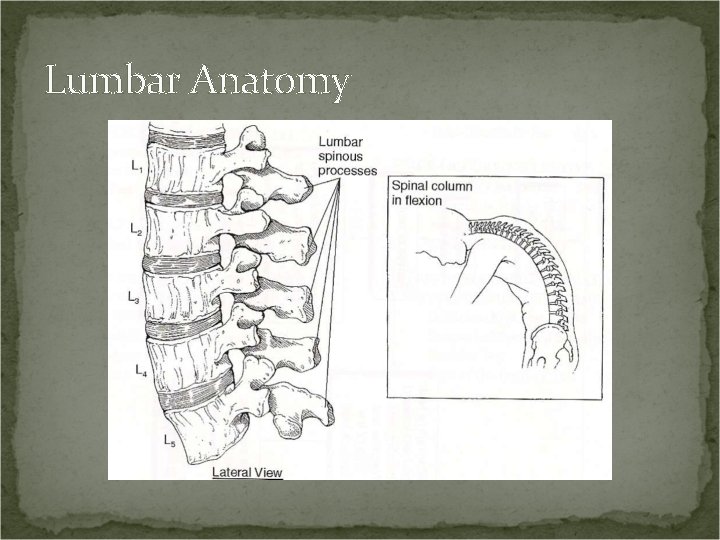
Lumbar Anatomy

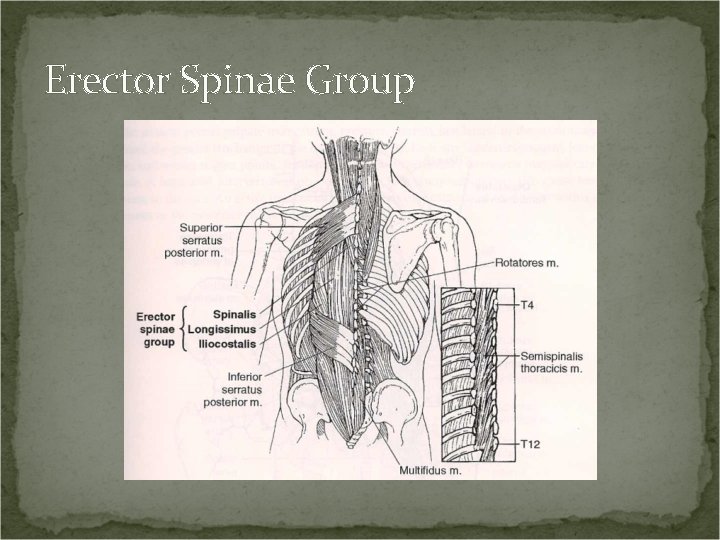
Erector Spinae Group

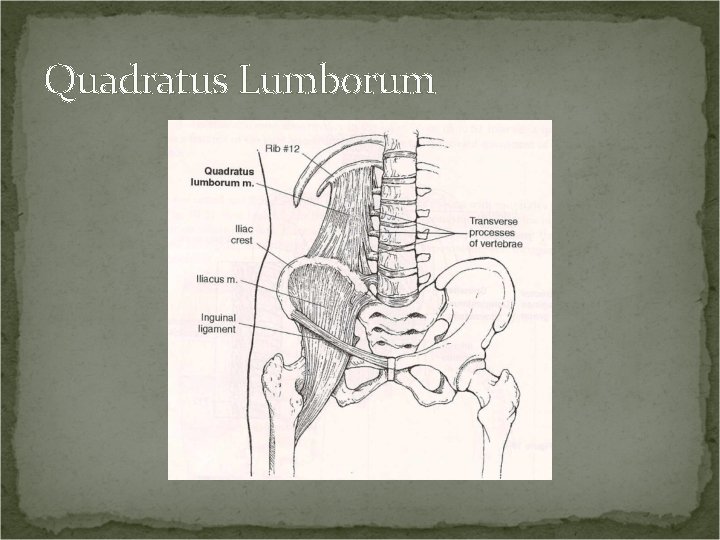
Quadratus Lumborum

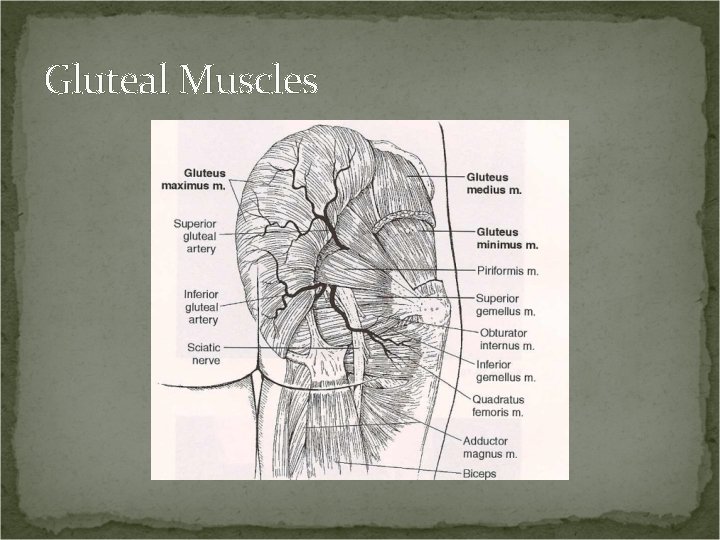
Gluteal Muscles

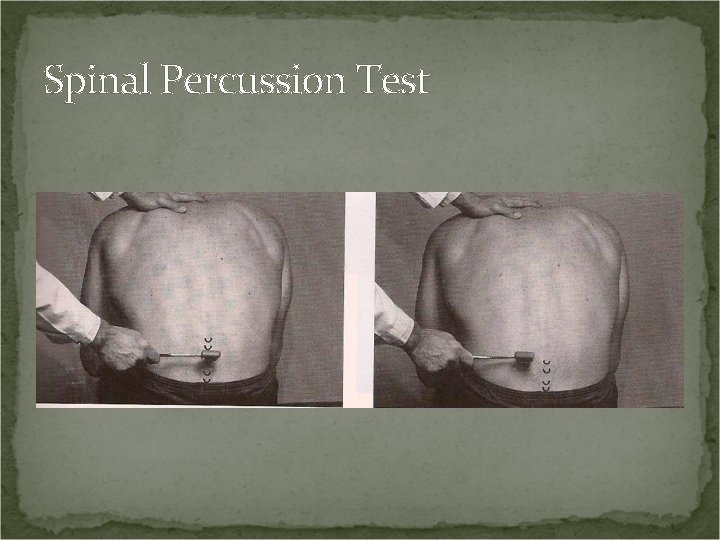
Spinal Percussion Test Procedure: Patient seated. Bent slightly forward. Tap the spinous processes and associated musculature with a reflex hammer. Positive Test: Local pain – fracture without neurological compromise. Radicular pain – fracture or disc defect with neurological compromise. Pain in paraspinal musculature – muscle strain.

Spinal Percussion Test

Referred Pain Vs. Radicular Pain Lower extremity pain may be referred from lumbopelvic tissues or viscera. It may also be radicular pain from the nerve roots of the spine. Referred pain patterns – the spinal pain is more aggravating than the lower extremity pain. Referred pain is poorly localized and dull. Radicular pain patterns – the leg pain is more aggravating than the spinal pain. Radicular pain is sharp and well localized.

Lumbar Nerve Root & Sciatic Nerve Irritation/Compression Neurogenic radicular lower extremity pain may be caused by any one of several factors. Tension, irritation, or compression of a lumbar nerve root or roots can cause radicular pain.

Lumbar Nerve Root & Sciatic Nerve Irritation/Compression Intraspinal canal compressions – disc lesions, spinal stenosis, degenerative disc disease, hypertrophic changes, malignancy. Extraspinal canal compressions – muscle dysfunction, extradural defects, masses.

Lumbar Nerve Root & Sciatic Nerve Irritation/Compression Clinical Signs and Symptoms Lower back pain Lower extremity radicular pain Loss of lower extremity reflexes Loss of lower extremity muscle strength Loss of lower extremity sensation

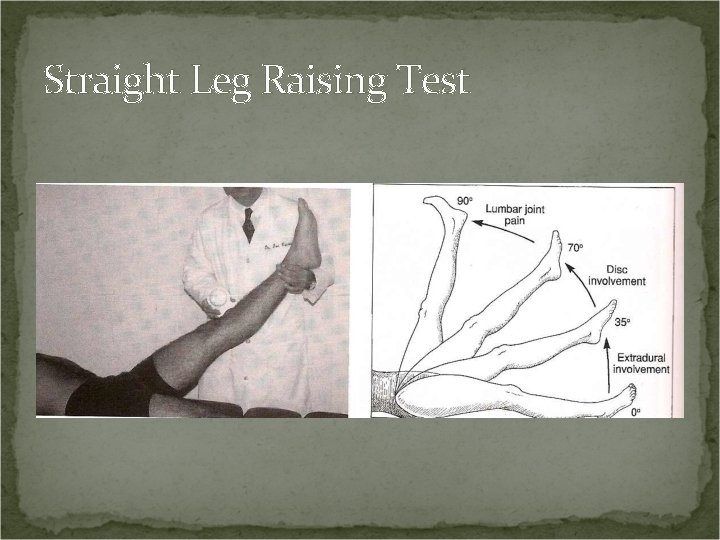
Straight Leg Raising Test Procedure: Patient supine. Raise the patient’s leg to a point of pain or 90 °, whichever comes first.

Straight Leg Raising Test Positive Test: This test stresses the sciatic nerve and spinal nerve roots L 5, S 1, and S 2. Pain after 70° of hip flexion – lumbar joint pain. Pain at 35° to 70° – sciatic nerve roots tense – pain due to IVD pathology. Pain between 0° to 35° – extradural sciatic involvement (spastic piriformis, SI joint lesion). Dull posterior thigh pain – tight hamstring.

Straight Leg Raising Test

Antalgic Lean Sign Procedure: Observe the patient while standing. Patients with disc protrusions that place pressure on a nerve root will lean in a direction that reduces the mechanical pressure on the disc.

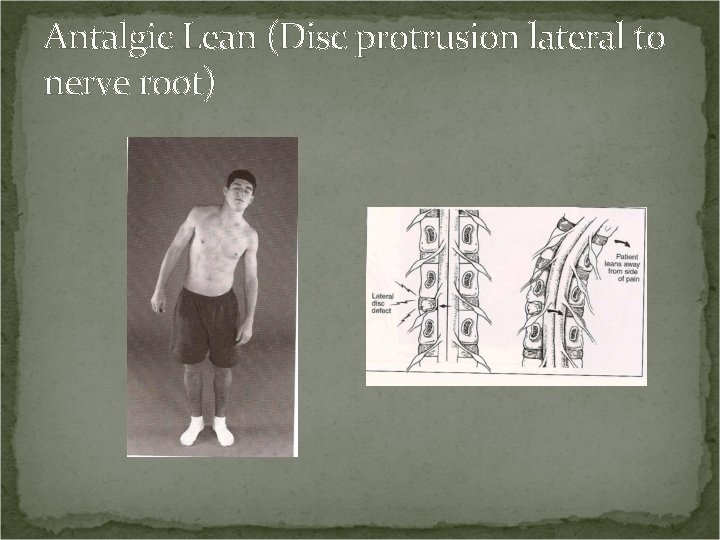
Antalgic Lean (Disc protrusion lateral to nerve root) Positive Sign: If the disc protrusion is lateral to the nerve root, the patient will lean away from the side of pain. Leaning away pulls the nerve root medially away from the disc defect and relieves pain.

Antalgic Lean (Disc protrusion lateral to nerve root)

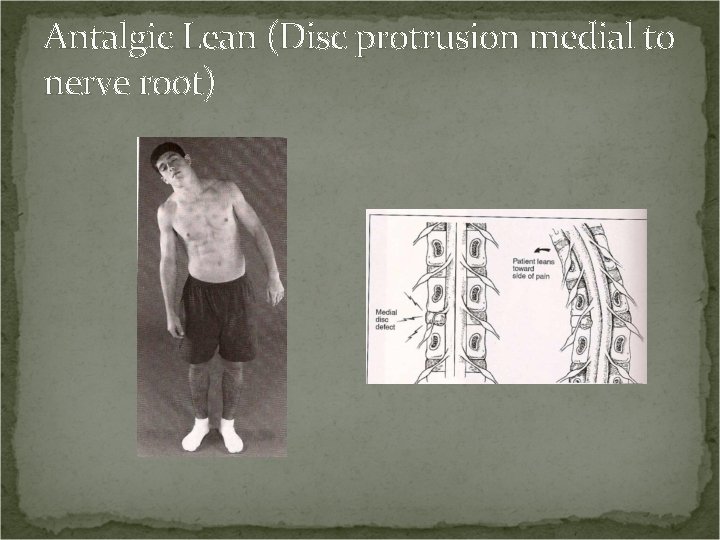
Antalgic Lean (Disc protrusion medial to nerve root) Positive Sign: If the disc protrusion is medial to the nerve root, the patient will lean toward the side of pain. Leaning towards the side of the lesion pulls the nerve laterally away from the disc defect, reducing pressure on the nerve root.

Antalgic Lean (Disc protrusion medial to nerve root)

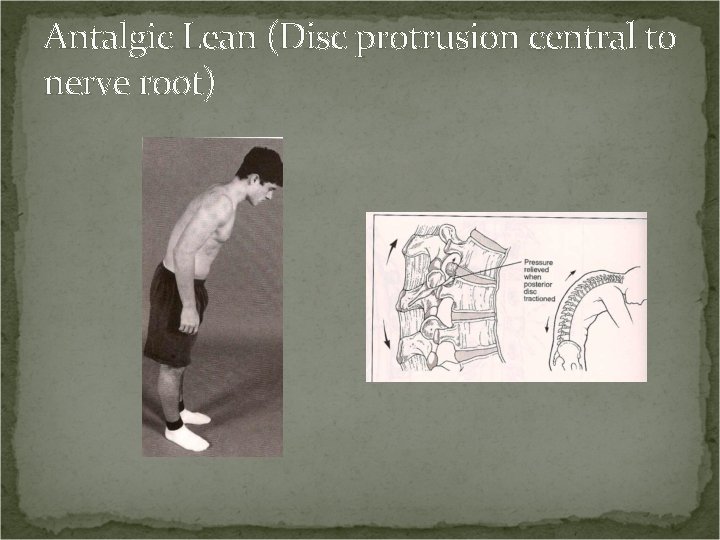
Antalgic Lean (Disc protrusion central to nerve root) Positive Sign: If the disc protrusion is central to the nerve root, the patient may assume a flexed posture. Leaning forward puts the posterior portion of the disc under traction, which can reduce the surface area of the disc that comes into contact with the nerve.

Antalgic Lean (Disc protrusion central to nerve root)

Kemp’s Test Procedure: Patient seated or standing. Stabilize the PSIS with one hand. Reach around the patient with the other hand passively bend the dorsolumbar spine obliquely backward. Positive Test: Pain in the lower back is a positive test for lumbar spasm or facet capsulitis. Radicular pain suggests a disc lesion.

Kemp’s Test

Space-Occupying Lesions Space-occupying lesions can consist of the following: Disc defect, degenerative change, synovial cyst, fracture, tumor, or some combination of these factors. Space-occupying lesions can lead to spinal stenosis. Narrowing of the tubular structures of the spine. Naorrowing of the central canal, lateral recess, or intervertebral foramen.

Space-Occupying Lesions Clinical Signs and Symptoms Lower back pain Lower extremity radicular pain Lower extremity weakness Loss of lower extremity reflexes Loss of lower extremity sensation

Valsalva’s Maneuver Procedure: Instruct the seated patient to bear down as if straining at stool. Concentrate the stress at the lumbar region. Ask if pain is increased and have the patient point to it. Positive Test: The test increases intrathecal pressure. Positive test indicates a space-occupying lesion.

Valsalva’s Maneuver

Dejerine’s Triad Procedure: Patient seated. Instruct the patient to cough, sneeze, and bear down as if straining at stool. Positive Test: Increased local pain suggests a spaceoccupying lesion.

Lumbar Vs. Sacroiliac Joint Involvement Lumbar and/or radicular pain in the leg can be caused by either a lumbar condition or by a sacroiliac joint condition. The following tests help to differentiate between the two sources of pain.

Sacroiliac Joint Syndrome Clinical Signs and Symptoms: Lower back pain Sacroiliac joint pain Aggravated by sitting Alleviated by standing or walking Lower extremity radicular pain

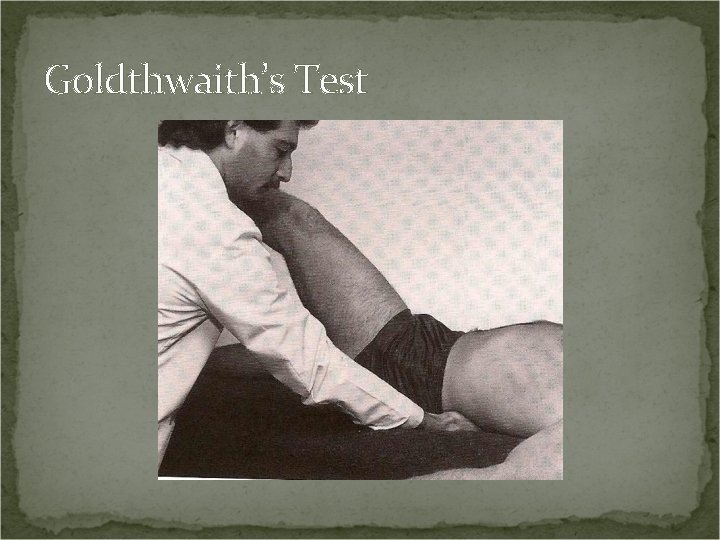
Goldthwaith’s Test Procedure: Patient supine. Place one hand under the lumbar spine with each finger under an interspinous space. With the other hand perform a straight leg raising test. Positive Test: Radicular pain before the fanning out of the lumbar vertebra indicates an extradural lesion such as a sacroiliac joint lesion. Radicular pain during lumbar fanning indicates an intradural lesion such as a space-occupying lesion. Local pain after lumbar fanning indicates a posterior lumbar joint disorder.

Goldthwaith’s Test

Nachlas Test Procedure: Patient prone. Approximate the patient’s heel to the buttock on the same side. Positive Test: Stretches the femoral nerve (largest branch of the lumbar plexus). Radicular pain to the anterior thigh – compression or irritation of the L 2 – L 4 nerve roots by an intradural lesion. Pain in the buttock – SI joint lesion. Pain in the lumbosacral joint – lumbosacral lesion.

Nachlas Test