ZollingerEllison Syndrome ZES Author Jennifer Hanna MD MBA

Zollinger-Ellison Syndrome (ZES) Author: Jennifer Hanna, MD, MBA Level: Intermediate Academic Affiliation : Duke University, General Surgery Research Fellow Version No: 1. 2 Submitted: December 2012 Editors’ Review: August 2015

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) • No Disclosures

4 Learning Objectives • Learn the clinical syndrome associated with ZES • Learn the radiographic findings associated with ZES • Learn how to make the diagnosis of ZES • Learn the medical and surgical treatment options for patients diagnosed with ZES

5 Outline • Introduction • Epidemiology • Classification, Nomenclature, and Histology • Clinical Manifestations • Radiographic Findings • Diagnosis • Medical and Surgical Management • Surveillance • Prognosis

6 Introduction • Patients have gastrin-secreting tumors with associated clinical consequences • Can occur sporadically or as a manifestation of multiple endocrine neoplasia type 1 (MEN 1) • Medical therapy consisting of acid suppression is standard of care for patients with ZES as part of the MEN 1 syndrome • Many patients with sporadic ZES are surgical therapy candidates

7 Epidemiology • Incidence in the US ranges from 0. 1 to 1% of patients with peptic ulcer disease (PUD), though this may be an underestimation • Most patients diagnosed between ages of 20 and 50 • Male to female ratio 1: 5: 1 • 70% form in duodenum, with remainder arising in pancreas and less often peripancreatic lymph nodes

8 Classification, Nomenclature, and Histology • Gastrinomas are derived from enteroendocrine cells, arising mainly in the pancreas, but also in the small intestine • Histologically, most gastrinomas are welldifferentiated neuroendocrine tumors with abundant neurosecretory granules – Malignancy cannot be predicted by morphology alone • Designation of tumor as a gastrinoma is based upon presence of clinical syndrome, not by histology

9 Clinical Manifestations • Gastrinoma results in high gastric acid output for 2 reasons: – Gastrin has trophic action on parietal cells and histaminesecreting enterochromaffin-like cells – Gastrin stimulates parietal cells largely via histamine release • Over 90% of patients with ZES develop PUD – Mostly with solitary ulcers <1 cm in diameter – Mostly in first portion of duodenum – Recur more often • Diarrhea can also be a prominent feature
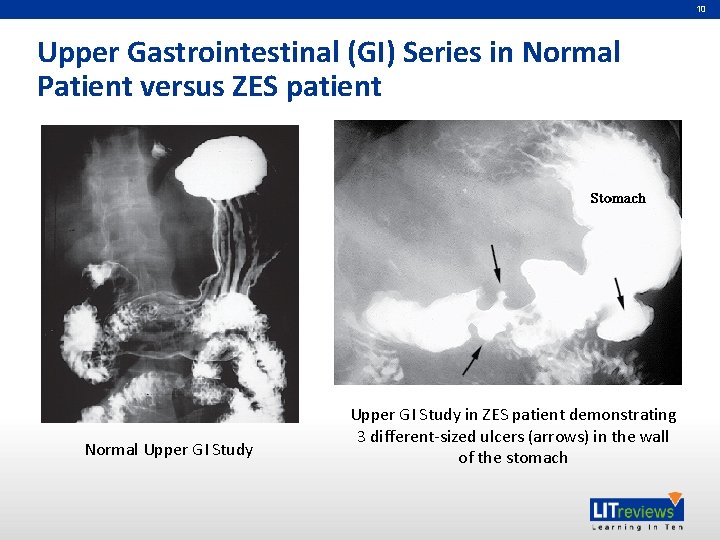
10 Upper Gastrointestinal (GI) Series in Normal Patient versus ZES patient Normal Upper GI Study in ZES patient demonstrating 3 different-sized ulcers (arrows) in the wall of the stomach
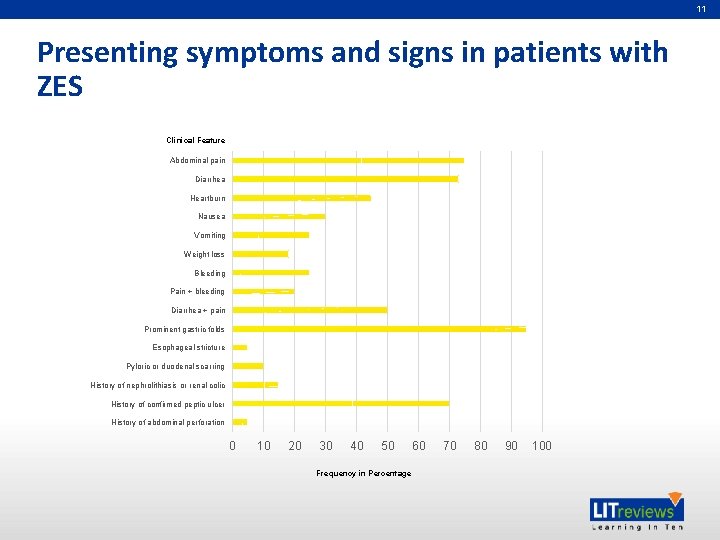
11 Presenting symptoms and signs in patients with ZES Clinical Feature Abdominal pain Diarrhea Heartburn Nausea Vomiting Weight loss Bleeding Pain + bleeding Diarrhea + pain Prominent gastric folds Esophageal stricture Pyloric or duodenal scarring History of nephrolithiasis or renal colic History of confirmed peptic ulcer History of abdominal perforation 0 10 20 30 40 50 Frequency in Percentage 60 70 80 90 100

12 Diagnosis • Should be suspected in patients with findings suggestive of acid hypersecretion, diarrhea, or personal or family history of MEN 1 • Tests for Diagnosis: – Fasting serum gastrin concentration >1000 pg/m. L is diagnostic Higher levels with pancreatic, larger, and metastatic tumors – Secretin stimulation test Can differentiate gastrinoma from other causes of hypergastrinemia Positive test is rise in serum gastrin by >200 pg/m. L Discontinue proton-pump inhibitors (PPIs) 1 week prior to test

13 Tumor Localization • Computed tomography (CT) and magnetic resonance imaging (MRI) • Endoscopic Ultrasound • Somatostatin Receptor Scintigraphy • Other Techniques – Angiography and selective arterial stimulation – Venous sampling with calcium gluconate – Localization at time of laparotomy

14 Goals of Therapy in ZES • Control of the complications resulting from autonomous release of gastrin • Control of the tumor itself

15 Medical Management • GOAL: Limit clinical manifestations and complications of peptic ulcer disease • Formal acid secretory studies should guide dosage of acid suppressants, with goal of reducing gastric acid secretion to below 10 m. Eq/h prior to next dose • When formal studies are not available, PPIs are initiated and maintained at high dosage using symptoms alone to guide dosage changes

16 Medical Management: PPIs and Somatostatin Analogs • First line agents: PPIs (eg, omeprazole, lansoprazole, pantoprazole, esomeprazole) – Block acid secretion by irreversibly binding to and inhibiting the hydrogen/potassium ATPase that reside on the luminal surface of parietal cell – Effects last for more than 24 hrs – Start with high dose of a PPI, though gradual dose reduction is possible with control of acid output • Second line agents: somatostatin analogs (eg, octreotide) – Inhibit gastrin secretion

17 Surgical Management • Treatment of sporadic gastrinoma without evidence of metastatic disease, not for patients with ZES as part of MEN 1 • Exploratory laparotomy and resection with curative intent • Likelihood of surgical cure is especially high for gastrinomas that lie within the gastrinoma triangle • Gastrin secretion may not return to normal post-op, leading to need for prolonged anti-secretory therapy • Vagotomy at time of resection may obviate need for post-op medical therapy

18 Post-Resection Surveillance • 3 and 6 months: History & physical (H&P), serum gastrin, and CT/MRI • Long-term: H&P, tumor markers every 6 -12 months for years 1 -3, and imaging as clinically indicated

19 Metastatic Disease • Evident at time of diagnosis in ~1/3 rd of patients • Liver is the major site, with bone being second most common site • Somatostatin receptor scintigraphy and MRI are best tests for detection • Most common cause of morbidity and mortality in ZES • Treatment includes somatostatin analogs • Liver-directed therapies: – – Resection Radiofrequency ablation and cryoablation Hepatic artery embolization Chemotherapy
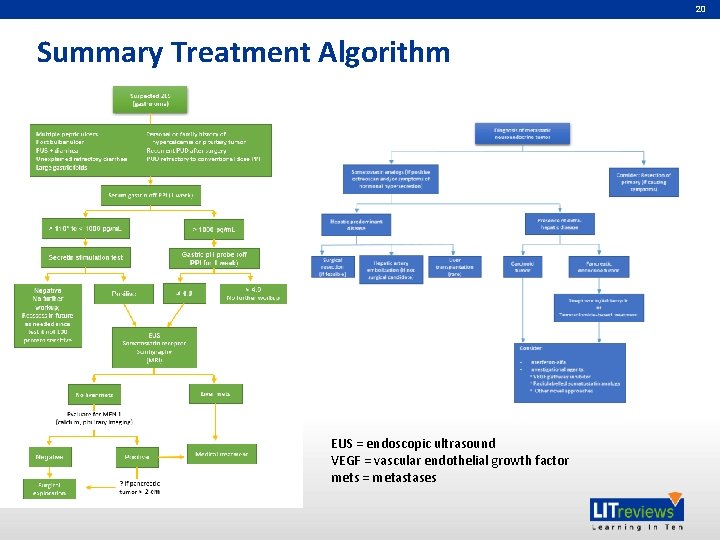
20 Summary Treatment Algorithm EUS = endoscopic ultrasound VEGF = vascular endothelial growth factor mets = metastases

21 Prognosis • Mortality depends upon whether tumor is benign or malignant and extent of disease involvement • Patients with metastases to the liver had a 10 -year survival of 30% compared with a 15 -year survival of 83% in those without metastases to the liver • Patients with MEN 1 had a lower rate of metastases to the liver at time of initial diagnosis (6%) • Fasting serum gastrin level at time of initial diagnosis provides an indication of disease extent and prognosis in patients with sporadic ZES

22 Summary • Patients with ZES have gastrin-secreting tumors with associated clinical consequences • Can occur sporadically or as a manifestation of MEN 1 • Medical therapy consisting of acid suppression is standard of care for patients with ZES as part of the MEN 1 syndrome • Goal of therapy in ZES is control of the complications resulting from autonomous release of gastrin, mainly PUD and control of the tumor itself • Liver is most common site of metastatic disease, which is most common cause of morbidity and mortality in ZES

23 References • Rice-Townsend SE & Norton JA. (2008). “Zollinger-Ellison Syndrome. ” Current Surgical Therapy. (88 -93). Philadelphia: Mosby Elsevier. • Goldfinger SE. (Sep 20, 2011). “Clinical manifestations and diagnosis of Zollinger-Ellison syndrome (gastrinoma). ” Up. To. Date. Retrieved from http: //www. uptodate. com/contents/search • Goldfinger SE. (Oct 26, 2010). “Management and prognosis of the Zollinger-Ellison syndrome (gastrinoma). ” Up. To. Date. Retrieved from http: //www. uptodate. com/contents/search

Partners in Academic Medicine
- Slides: 24