Ziyad AlMagwashi Abdulaziz Bayounis Meshari AlMeshari LUQ Objectives

Ziyad Al-Magwashi Abdulaziz Bayounis Meshari Al-Meshari

LUQ Objectives Structures in LUQ Organs Not to Miss The Spleen Ø Anatomy Ø Splenomegaly Ø Hemolytic Anemias Ø Tumors Ø Abscess Ø Trauma Splenectomy

Case 1 Ahmed is a 45 -year-old translator coming from Kenya recently. He comes to the ED because he is bothered by pain in his upper abdomen, mostly on the left side. You learn that he lived on his family’s farm in Kenya. What structures lie in the left upper quadrant of the abdomen? Hint: 10
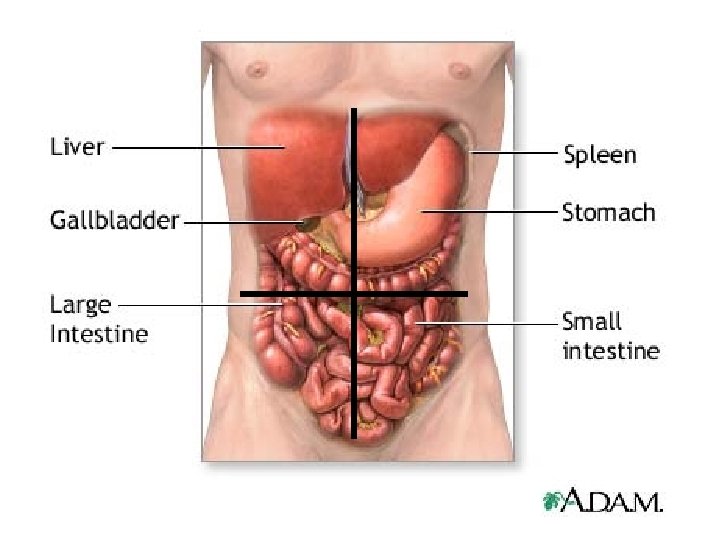

Structures in the LUQ 1. ? 7. Left suprarenal gland 2. ? 8. Jejunum and proximal ileum 3. Spleen 8. Left colic (splenic flexure) 4. Stomach 9. Transverse colon: left half 5. Left Kidney 10. Descending colon: superior part

Case 1 Continued… You order a full work-up for Ahmed and find that he has marked eosinophilia. What other tests do you want to request?
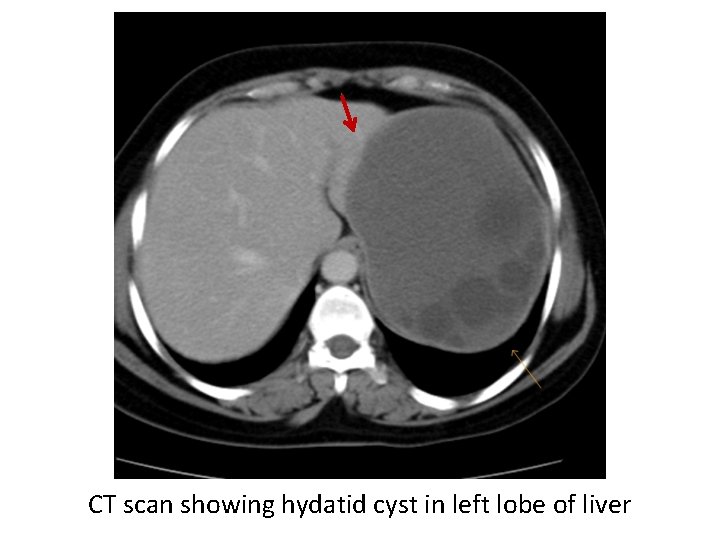
CT scan showing hydatid cyst in left lobe of liver

Case 2 Sami is 59 -year-old 30 pack year smoker who has recently lost 15 kg, and has a cough with blood tinged sputum. However, he mainly complains to you about the discomfort he feels in his left upper abdomen, which on palpation feels hard and nodular. Given the history, what is the most likely cause of this man’s abdominal masses? Hint: Strong suspicion of lung cancer.
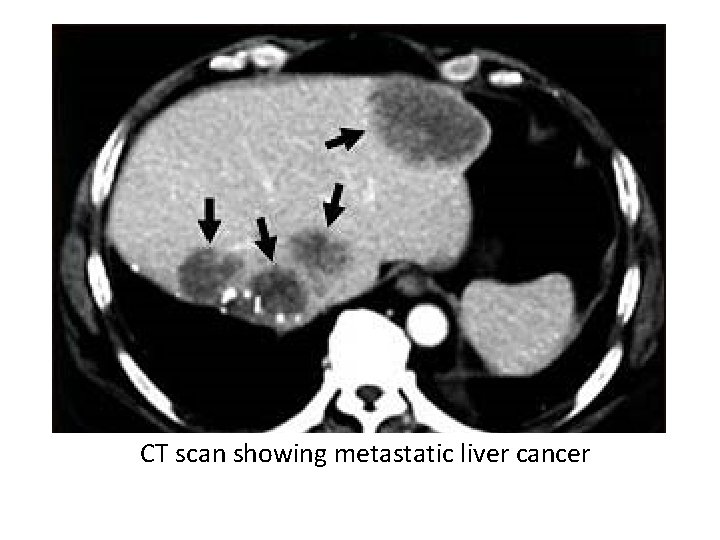
CT scan showing metastatic liver cancer
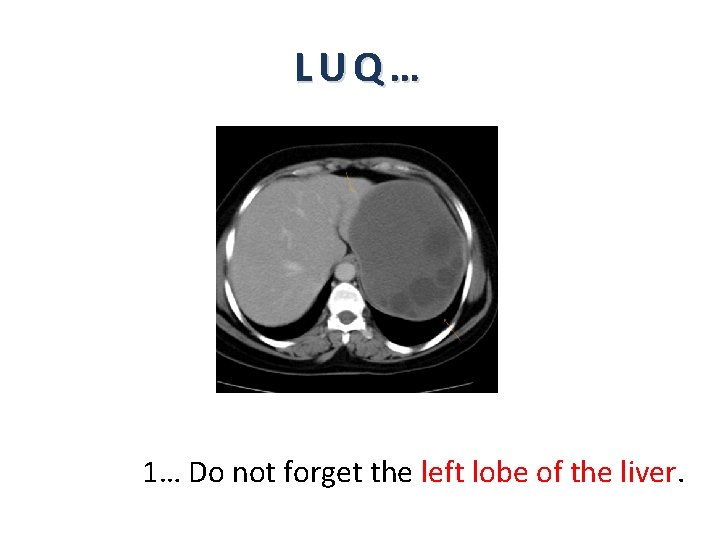
LUQ… 1… Do not forget the left lobe of the liver.

Case 3 Sarah is 30 -year-old overweight woman who has a history of gallstones. She is brought by her husband to the ED because she feels like there is a “painful bump on her stomach”. She mentions that she had an episode of severe pain that felt like “it was stabbing right through me to my back” a month ago but did not seek any help because she does not like hospitals. On palpation you feel a firm mass with an indistinct lower border that is resonant to percussion. Taking into account one of the complication of gallstones and her previous attach of abdominal pain, what is a possible diagnosis? Hint: Hx of stabbing pain radiating to the back.
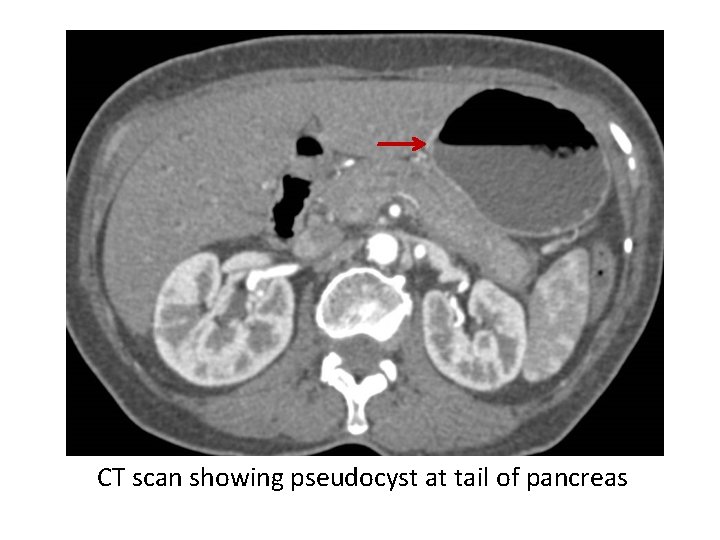
CT scan showing pseudocyst at tail of pancreas
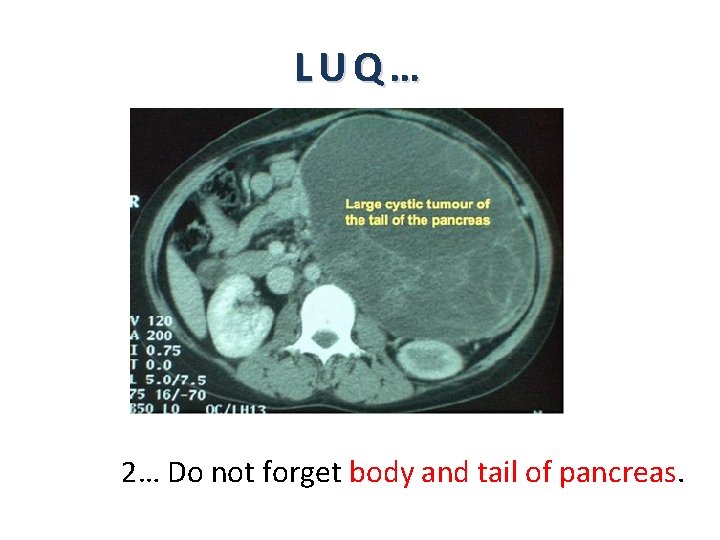
LUQ… 2… Do not forget body and tail of pancreas.

Question A patient with suspected carcinoma of the stomach. What do you expect to find on palpation? Nothing. Do not expect to feel a mass in a patient with carcinoma of the stomach. Browse’s Introduction To The Symptoms And Sings Of Surgical Disease, 4 th Edition, P 425


Anatomy of Spleen The largest lymphoid organ in the body. Located in LUQ behind 9 th, 10 th and 11 th ribs. Weighs about 80 -150 g. Varies in size and shape between people, but commonly fist-shaped, purple, and 4 in long. It lies with it’s long axis along the line of the 10 th rib and has an anterior notch. Because the spleen is protected by the rib cage (lying behind the 9 th, 10 th and 11 th ribs) we cannot easily palpate it unless it is abnormally enlarged.

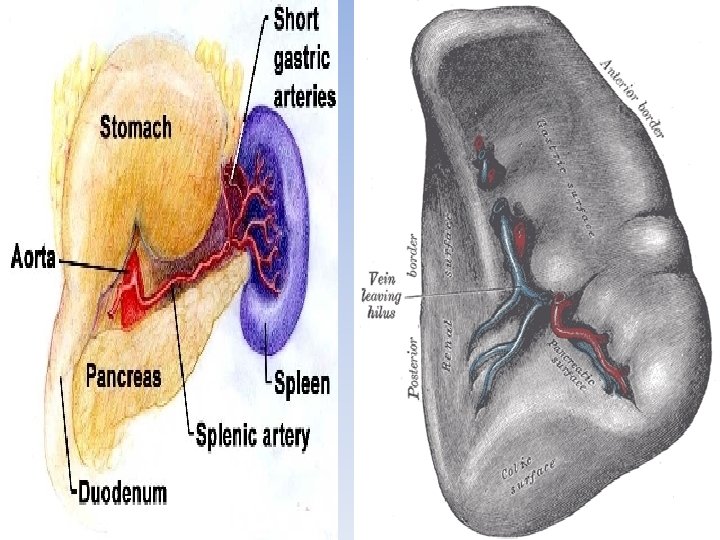
Splenic Blood Supply The spleen receives its blood supply from: Splenic artery (largest branch of celiac artery) Short gastric arteries (gastroepiploic arteries) The splenic vein carries blood from the spleen then it communicate with SMV to form portal vein. The nerves accompany the Splenic artery and are derived from the Celiac plexus. The hilum of the spleen is related to the pancreatic tail.

Functions of Spleen The spleen plays multiple supporting roles in the body: 1. Filter: Phagocytosis of old and abnormal red blood cells. 2. Stores platelets (1/3 of platelets stored in spleen). 3. Immune: Produce antibodies (Ig. M) and Opsonin. 4. Reservoir: Contains about 8% of red blood cell mass. 5. Hematopoiesis: in fetal life and hematological disorders.
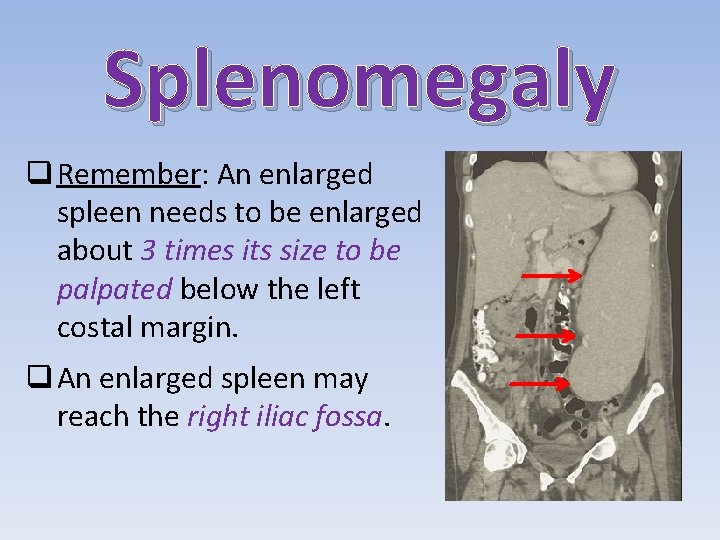
Splenomegaly q Remember: An enlarged spleen needs to be enlarged about 3 times its size to be palpated below the left costal margin. q An enlarged spleen may reach the right iliac fossa.

Splenomegaly - Causes

MASSIVE Splenomegaly Cross midline extending into the right iliac fossa. Most important causes: 1) Hematological Chronic myeloid leukemia Myelofibrosis 2) Infections Malaria Schistosomiasis Visceral lishmaniasis 3) Others Tropical splenomegaly Lysosomal storage diseases (Gaucher’s & Nieman-Pick disease)

Approaching SPLENOMEGALY History: ü Fever, malaise, anorexia, foreign travel or with in an immigrant population infections ü Weight loss, malaise, night sweats, pruritis and tendency to bleed malignancy ü Anemia, fatigue, jaundice, gallstones and family Hx of similar symptoms hemolytic anemia ü Neurological problems, mental retardation, skeletal deformities storage diseases
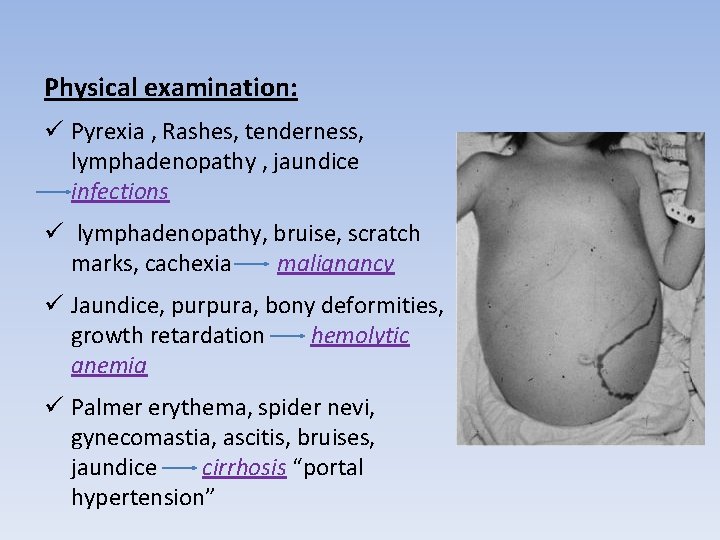
Physical examination: ü Pyrexia , Rashes, tenderness, lymphadenopathy , jaundice infections ü lymphadenopathy, bruise, scratch marks, cachexia malignancy ü Jaundice, purpura, bony deformities, growth retardation hemolytic anemia ü Palmer erythema, spider nevi, gynecomastia, ascitis, bruises, jaundice cirrhosis “portal hypertension”

Investigations: ü CBC , ESR , BLOOD FILM ± bone marrow biopsy ü Urea & electrolytes ü Liver function tests ü Specific tests for infections and rheumatic diseases ü U/S ü CT scan

Hemolytic Anemias Hereditary spherocytosis: Autosomal dominant inheritance. The most common congenital hemolytic anemia. The red cell membrane lacks the necessary protein assembly (spectrin & ankyrin) decrease cellular plasticity with membrane loss the RBCs are small, dense, & deformed haemolysis (by the spleen)

Hemolytic Anemia (Cont. ) Clinically: ü hemolytic anemia, splenomegaly, jaundice is almost always present. ü Periodic exacerbation (follows viral infections). ü Due to haemolysis 85% patients will form pigmented gall stones. Lab: ü Anemia, high bilirubin (indirect), spherocytes seen on blood smear, reticulocyt count increased. ü Coombs test negative. ü Large spleen risk of traumatic rupture.

Hemolytic Anemia (Cont. ) Treatment: ü Splenectomy is the sole treatment for hereditary spherocytosis, associated gall stones cholecystectomy ü Splenectomy should be delayed in children until age of 6 years – why not earlier or later? To minimize risk of post-splenectomy infection, but before gallstones have time to form.
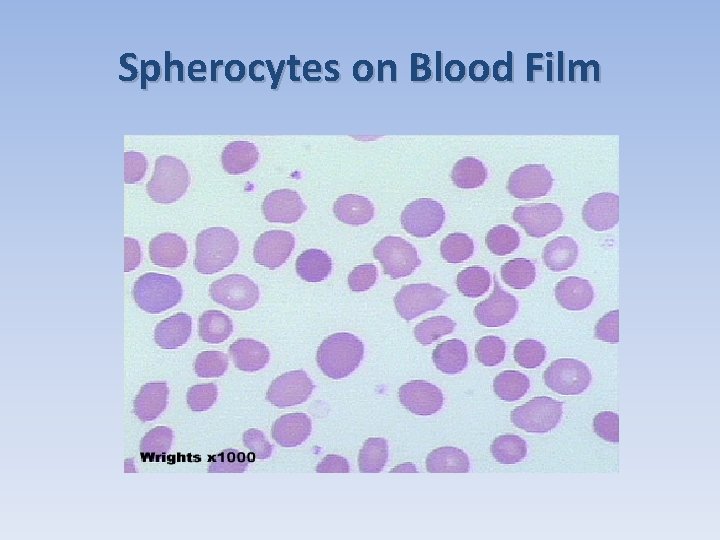
Spherocytes on Blood Film

Sickle Cell Disease Autosomal recessive inheritance Due to replacement of normal hemoglobin A ( Hb-A) by sickle hemoglobin Hb-S (valine instead of glutamic acid in the 6 th position of the Beta chain of globin). Patients well have sickled shaped RBCs. Those RBCs well be destroyed by the spleen causing splenomegaly (splenic sequestration). Splenic microinfarcts lead to auto infarction.

Sickle Cell Disease (Cont. ) Diagnosis confirmed by electrophoresis (more than 80% of hemoglobin is Hb-S ). Complications include pigment gall stones formation. Management: ü Prevent crisis (avoiding hypoxia, dehydration, etc), ü Vaccinations (against pneumococcal and haemophilus influenza), ü Hydroxyurea, folic acid (sever hemolysis), & exchange transfusion to reduce the frequency of crisis or as a prophylaxis before pregnancy or surgery.
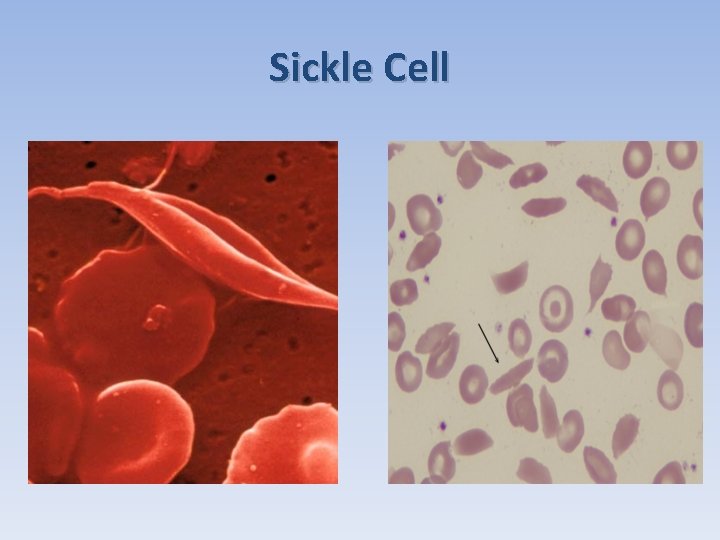
Sickle Cell
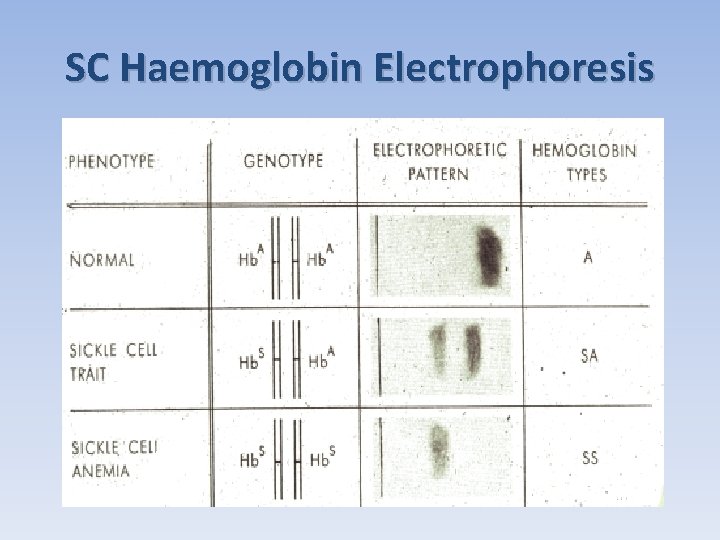
SC Haemoglobin Electrophoresis

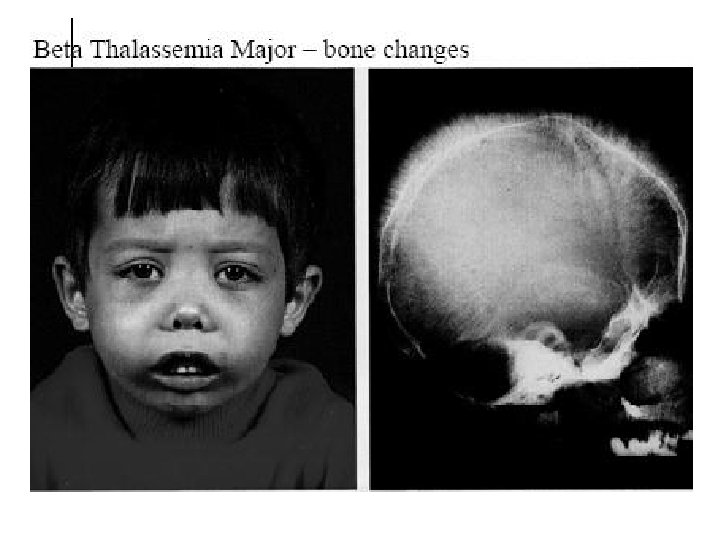
Thalassemia Autosomal recessive inheritance more in the Mediterranean population. These hereditary hemolytic anemia’s result from a hemoglobin underproduction. Beta Thalasemia is the most common type. Hemoglobin electrophoresis in Thalasemia major reveals absence of hemoglobin A and an increase in hemoglobin F. Treatment includes blood transfusions, iron chelation and splenectomy.

Idiopathic thrombocytopenic purpura (ITP) ITP is the condition of having a low platelet count (thrombocytopenia) of no known cause (idiopathic). Most causes appear to be related to antibodies against platelets (Ig. G antiplatalets). Often ITP is asymptomatic, however a low platelet count can lead to visible symptoms, such as purpura, petechiae, bleeding gums, ecchymoses and more seriously bleeding diathesis from GI tract.

ITP (Cont. ) Acute ITP (AITP) usually seen in children following viral infection. Chronic ITP usually affect adults (usually idiopathic but may occur with autoimmune disorders, e. g. SLE, thyroid disease, CLL and HIV).

ITP Treatment 1. 2. 3. 4. Steroids. Intravenous immunoglobulin (I. V. Ig. G). Medical therapy is the 1 st line (steroids& IVIG) If failed Splenectomy (most patients well respond 70%). 5. Intravenous Anti-D. 5. Platelet transfusion (reserved for intracranial or extreme hemorrhage).

Autoimmune Hemolytic Anemia Is an acquired hemolytic anemia resulting from antibodies that are produced by the body against its own red cells. Distinguishing feature is a positive direct Coombs test this identifies antibodies on the red cell surface. Usually after 50 years, female to male 2; 1, acute onset. The type of antibody attached to the red cell determines the mechanism of hemolysis. Divided by their optimal binding Tempreture: Ø Warm AIHA (37˚C) Ig. G mediated. Ø Cold AIHA (<4˚C) Ig. M mediated.

AHA (Cont. ) Causes: 1. Idiopathic 2. Warm AHA: a) Idiopathic (40 -50% of cases) b) Secondary to drugs, connective tissue disease (warm antibodies, may benefit from splenectomy) 3. Cold AHA: infections( EBV, Mycoplasma pneumonia) The hemolysis occurs intravascularly & not in within the spleen. 4. Drugs: Penicillin, cephalothin, streptomycin, methyldopa, quinidine, aspirin, phenacetin and several sulfonamides. Physical Findings: ü Pallor, jaundice and splenomegaly are the main physical findings.

AHA Treatment Directed towards the hemolytic anemia and any underlying disease: 1. Blood transfusion, steroids are the primary Rx. 2. Splenectomy in Warm AIHA not responsive to medical Rx or requiring Large steroid doses.

Splenic Tumors Benign and malignant infiltration: 1. Leukemia's (acute, chronic, lymphoid & myeloid) 2. Lymphomas(Hodgkins and non-hodgkins) 3. Myeloproliferative disorders 4. Metastatic tumors(commonly from lung breast and melanoma) 5. Histiocytosis X 6. Hemangioma, lymphangioma 7. Splenic cysts 8. Hamartomas 9. Eosinophilic granuloma

Splenic Abscess Splenic abscess is rare - it should be suspected when there is progressive splenic enlargement and is associate with bacteraemia and abscess formation at other sites Causes: 1. Bacterial Streptococcus, Staphylococcus, Enterococcus (predominant in most reports). 2. Fungal -Candida 3. Unusual flora -Burkholderia pseudomallei actinomycotic and mycobacterial abscesses, most typically seen in immunosuppressed patients.
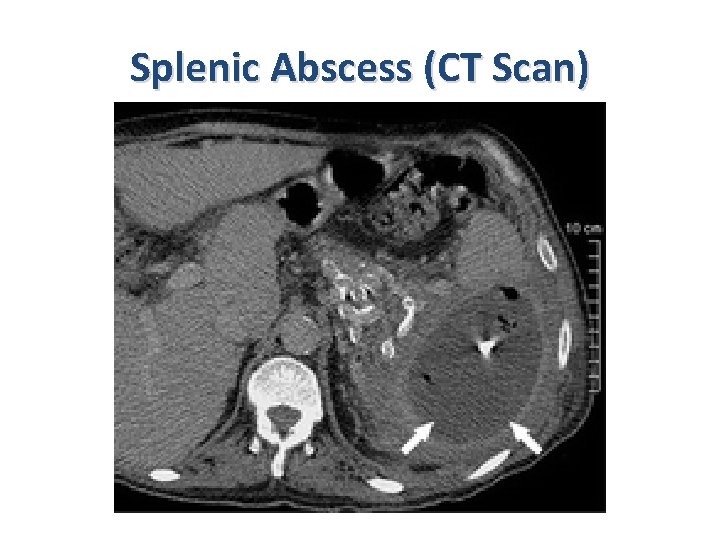
Splenic Abscess (CT Scan)

Splenic Abscess (Cont. ) Patient usually present with: ü Fever (>90%) ü Abdominal pain (>60%) typically occurs suddenly, with a punctum maximum in the left hypochondrium (>39%) ü Pleuritic chest pain around the left lung base (>15%) is aggravated by coughing or forced expiration. ü General malaise

Splenic Abscess Treatment ü Medical therapy: Start antibiotics immediately after taking blood cultures (antifungal if fungus suspected). ü Surgical Therapy: 1. Percutaneous drainage: q Percutaneous drainage is indicated for easily accessible uniloculated or biloculated abscesses with otherwise favorable features, as described previously, and also for surgical patients at very high risk who cannot tolerate general anesthesia or surgery. q The procedure includes a risk of iatrogenic injury of the spleen, colon (splenic flexure), stomach, left kidney, and diaphragm. 2. Splenectomy.

Splenic Abscess Treatment (Cont. ) 3. Open drainage: Open drainage is used when the abscess cannot be drained percutaneously. Depending on the location of the abscess, 1 of 3 access routes can be employed: A. Transpleural: Usually requires resection of the 12 th rib in the posterior axillary line and drainage of the abscess through the diaphragm B. Abdominal extraperitoneal : Accesses the abscess through the lateral abdominal wall and between the peritoneum and the flat abdominal muscles C. Retroperitoneal : Used when the abscess extends to the flank

Splenic Vein Thrombosis - Case A 23 -year-old man with episodes of hematemesis and hematochezia was admitted to ED with clinical signs of anemia and splenomegaly. Lab results showed hematocrit, 22. 2%; hemoglobin, 7. 5 g/d. L; international normalized ration (INR), 1. 22. Results of his liver function tests, as well as the rest of his biochemical examinations, were within normal limits. An emergency endoscopy performed showed enlarged bleeding gastric varices but no esophageal varices This led us to consider that the enlarged varices may be secondary to splenic vein thrombosis. Ultrasound and CT scan revealed his enlarged spleen and an engorged splenic artery with a diameter of 1 cm, and a fusiform dilated splenic vein measuring 5 × 6 × 9 cm. Daniel Paramythiotis, et al. Massive variceal bleeding secondary to splenic vein thrombosis successfully treated with splenic artery embolization: a case report. Journal of Medical Case Reports 2010, 4: 139
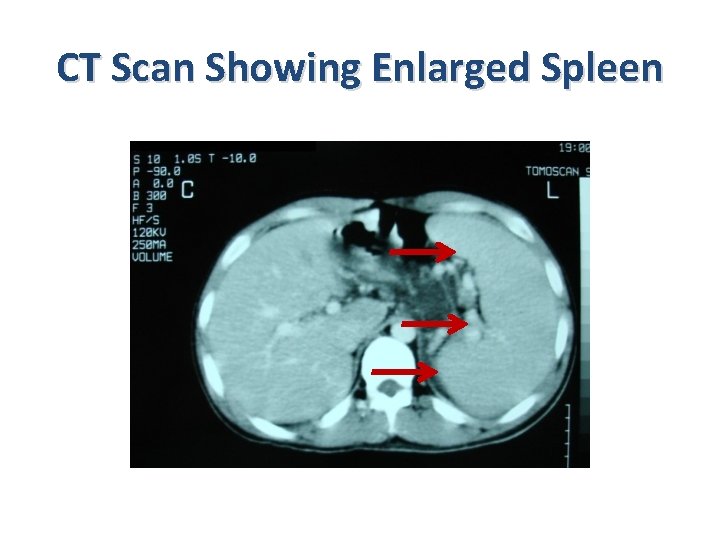
CT Scan Showing Enlarged Spleen

Splenic Vein Thrombosis Sinistral portal hypertension (SPH) is a clinical syndrome of gastric variceal hemorrhage in the setting of splenic vein thrombosis (SVT), mostly due to pancreatic pathology. Unlike patients with generalized portal hypertension, most patients with SVT are usually asymptomatic and have a normal hepatic function. Bleeding from gastric varices (GVs) is generally more severe than from esophageal varices, although it occurs less frequently.

SVT (Cont. ) Treatment: ü Splenectomy is considered the treatment of choice for splenic vein thrombosis complicated by variceal hemorrhage or hypersplenism (symptomatic).
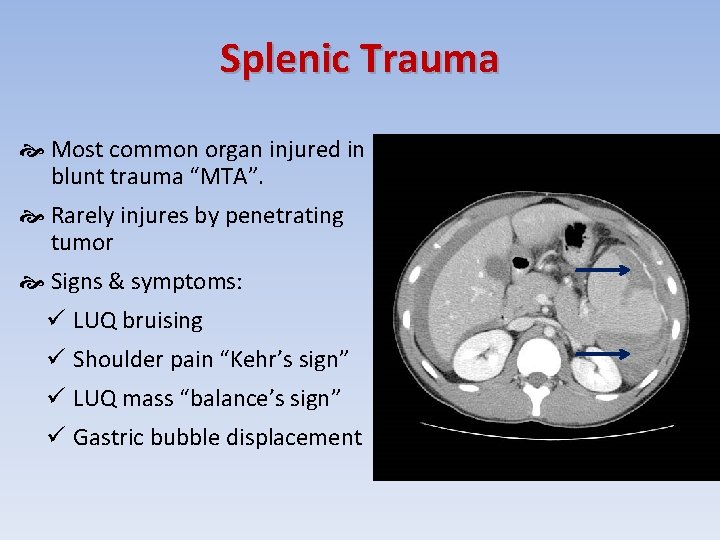
Splenic Trauma Most common organ injured in blunt trauma “MTA”. Rarely injures by penetrating tumor Signs & symptoms: ü LUQ bruising ü Shoulder pain “Kehr’s sign” ü LUQ mass “balance’s sign” ü Gastric bubble displacement

Splenic Trauma (Cont. ) Initial diagnostic procedures in an unstable patient is DPL , US “FAST = focused assessment with sonar for trauma” In a stable patient CT scan LAPAROTOMY Management goals: ü Resuscitation ü Salvage in hematomas and simple lacerations is the primary goal; suture lacerations, ligate splenic vessels. ü If above failed or severe rupture causing instability splenectomy is indicated.

Splenic Trauma (Cont. ) Indications for Non-operative Management: ü Hemodynamically stable ü <2 units transfused ü No increasing hematoma size when followed by U/S ü Stable Hb estimations Note: Keep in mind! There is a risk of delayed rupture of hematomas so observe patient 7 -10 days
SPLENECTOMY
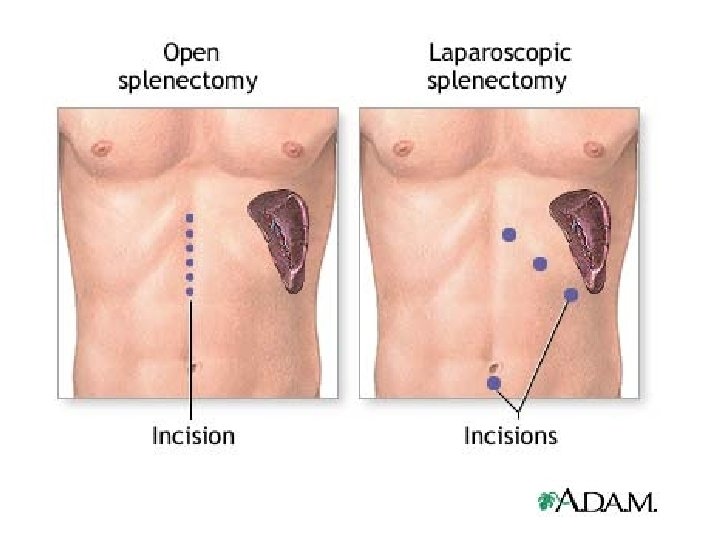

Indications of Splenectomy 1. Trauma (usually blunt but it could be penetrating) 2. Cysts. 3. Congenital Hemolytic anemia: A. Hereditary spherocytosis(most common) B. Hereditary elliptocytosis C. Thalasemia 4. Auto-immune A. ITP B. Auto-immune hemolytic anemia

Indications (Cont. ) 5. For Symptom relief, such as: A. Hypersplenism B. Splenic Vein thrombosis C. Infectious mononucleosis 6. Hematologic malignancies A. Hairy cell leukemia B. Hodgkin’s lymphoma 7. TTP 8. Splenic artery aneurysm 9. Splenic abscess 10. Ectopic spleen
Complications of Splenectomy A. Immediately postoperative: § Peripheral Blood changes Ø Leukocytosis Ø Thrombocytosis Ø Presence of Howell-Jolly bodies § § Hemorrhage Atelectasis (left lower lobe, most common) Subphrenic Abscess or hematoma Pancreatitis or pancreatic fistula (as a result from parenchymal manipulation)

Complications (Cont. ) B. Postsplenoectomy Sepsis § Overwhelming sepsis usually with encapsulated Organism: Ø Pneumococcus or Haemophilus A. In 4. 25% of splenectomized Pt. B. Fatal 50% of the time Ø Vaccinations for Streptococcus pneumoniae and H. influenze should be given to all splenectomized Pt. , more effective if given 10 -14 days before surgery. Ø Prophylactic Penicillin given to <18 y. o children.

- Slides: 61