Zimbabwe A Decade of HIV Prevention Research Danuta

Zimbabwe: A Decade of HIV Prevention Research Danuta Kasprzyk, Ph. D and Daniel Montaño, Ph. D University of Connecticut, CHIP March 17, 2011 University of Zimbabwe 1

Overview • Zimbabwe Background • Behavior Change Research: Applying the Integrated Behavioral Model (IBM) – CPOL – Male Circumcision • Strategies to Improve Family Functioning Among Families with HIV Positive Parents – Family Health Study 2

Zimbabwe: Basic demographics • 11. 39 Million people • Median Age: 17. 6 (M=16. 3; F=18. 8) • 5. 95 Million 15 -49 year olds • 41% children under 5 years of age • 70% live in rural areas • 70% of population is women and children • Two majority ethnic groups – 70% Shona; 30% Ndebele • English, Shona and Ndebele are the official languages 2007 – 2008 UN estimates/CIA Factbook estimates 3
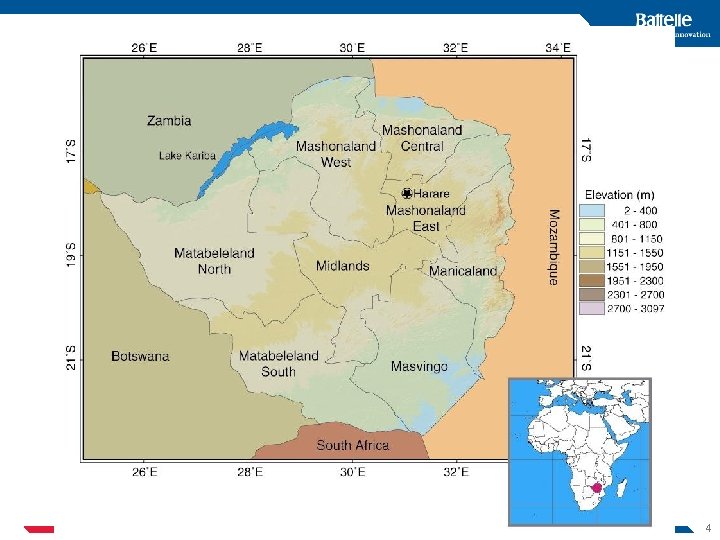
4
Zimbabwe: Basic demographics • Annual population growth = 0. 6 • Adult Literacy 90%: – women 87. 6%; – men 93. 7% • Percent of primary school enrollment – boys 88%, – girls 87% • Per capita expenditure on health = $146 US 2007 – 2008 UN estimates/CIA Factbook estimates 5
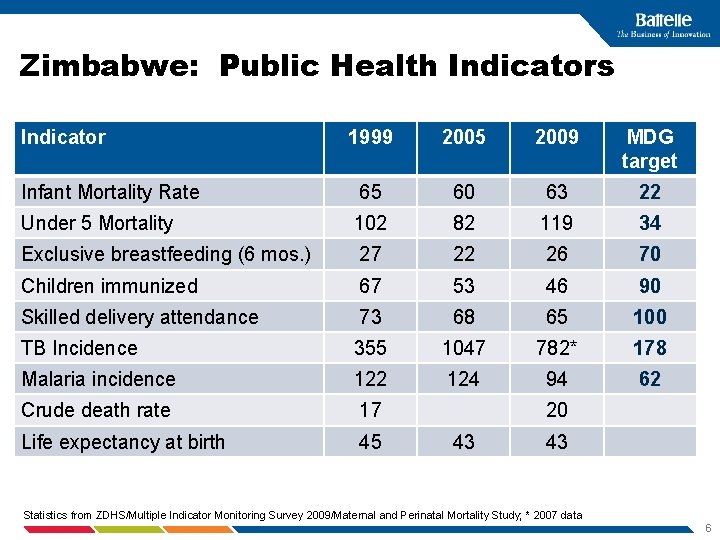
Zimbabwe: Public Health Indicators Indicator 1999 2005 2009 MDG target Infant Mortality Rate 65 60 63 22 Under 5 Mortality 102 82 119 34 Exclusive breastfeeding (6 mos. ) 27 22 26 70 Children immunized 67 53 46 90 Skilled delivery attendance 73 68 65 100 TB Incidence 355 1047 782* 178 Malaria incidence 122 124 94 62 Crude death rate 17 Life expectancy at birth 45 20 43 43 Statistics from ZDHS/Multiple Indicator Monitoring Survey 2009/Maternal and Perinatal Mortality Study; * 2007 data 6
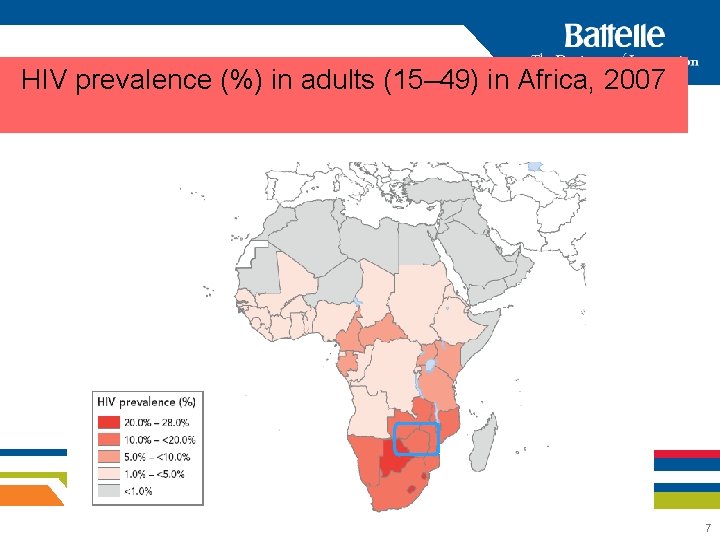
HIV prevalence (%) in adults (15– 49) in Africa, 2007 7
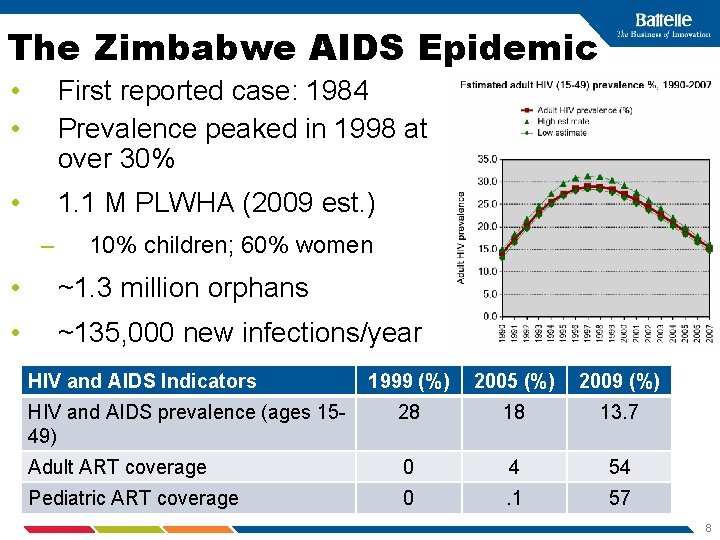
The Zimbabwe AIDS Epidemic • • First reported case: 1984 Prevalence peaked in 1998 at over 30% • 1. 1 M PLWHA (2009 est. ) – 10% children; 60% women • ~1. 3 million orphans • ~135, 000 new infections/year HIV and AIDS Indicators 1999 (%) 2005 (%) 2009 (%) HIV and AIDS prevalence (ages 1549) 28 18 13. 7 Adult ART coverage 0 4 54 Pediatric ART coverage 0 . 1 57 8
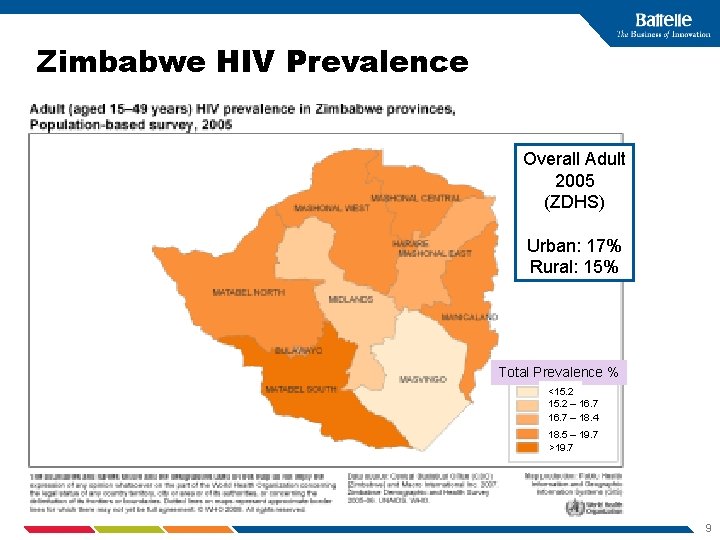
Zimbabwe HIV Prevalence Overall Adult 2005 (ZDHS) Urban: 17% Rural: 15% Total Prevalence % <15. 2 – 16. 7 – 18. 4 18. 5 – 19. 7 >19. 7 9

Zichire Origin • Zi. CHIRe formed in July 2000 after obtaining funding to join NIMH Collaborative HIV/STD Prevention Trial • We operate with a formal Memorandum of Understanding with Battelle and University of Zimbabwe (UZ) • 2 collaborating institutions: – Battelle, Centers for Public Health Research and Evaluation – UZ, Medical School, Department of Community Medicine – UZ, Department of Psychology 10

University of Zimbabwe Zichire office 11

Research in Zimbabwe • Ten studies conducted since 2000 – RCT HIV/STD Prevention Trial, 8 yrs, NIMH – Alcohol and risky behavior, 4 yrs, NIAAA – Male Circumcision uptake in, 4 yrs, NIMH – Family Health Study: psychosocial support intervention, 6 yrs, NINR – Neuro-cognitive effects of HIV, UW grant, Pilot study – STD Etiology Study, pilot, NIMH – UNICEF: Male Champions rapid assessment evaluation – CDC: - Mopani Junction Radio Drama formative research and pilot impact evaluation - Young Adult Survey development - Health educational pamphlet design technical assistance 12

BEHAVIOR CHANGE RESEARCH: APPLICATION OF THE INTEGRATED BEHAVIORAL MODEL (IBM) 13

Origin and Application of the IBM • In USA – Project SAFER • In Zimbabwe – Project SAFER – CPOL Trial – Male Circumcision 14
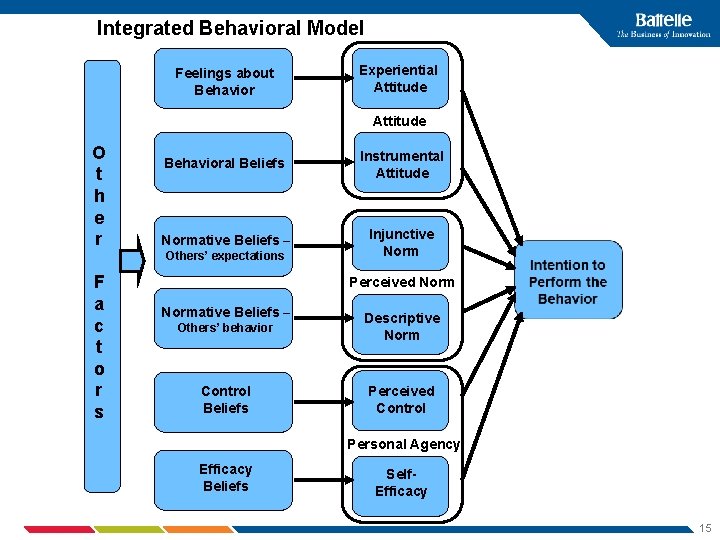
Integrated Behavioral Model Feelings about Behavior Experiential Attitude O t h e r Behavioral Beliefs Instrumental Attitude Normative Beliefs – Injunctive Norm Others’ expectations F a c t o r s Perceived Normative Beliefs – Others’ behavior Descriptive Norm Control Beliefs Perceived Control Personal Agency Efficacy Beliefs Self. Efficacy 15

HIV/STD Prevention Trial • NIMH funded, Multi-national Collaborative 2 -armed RCT to test HIV/STD prevention intervention • First multi-national test of the Community Popular Opinion Leader (CPOL) Model Intervention: • Multi-site: Conducted in 5 countries – China/UCLA; India/JHU; Peru/UCSF-UCLA; Russia/Medical College of WI; Zimbabwe/Battelle India China Peru 16

HIV/STD Prevention Trial • Accrued cohort through purposive selection of approximately 185 individuals (30 Growth Points) • Conduct Baseline (N=5, 547) • Personal Interview Assessment: – Demographic, Behavioral Risk, IBM – Health Assessment, including STD symptoms – Biologic samples (Bacterial and Viral STDs) • Implement intervention (15 growth points randomly assigned) • Follow-ups at 12 and 24 months (30 growth points) 17

18

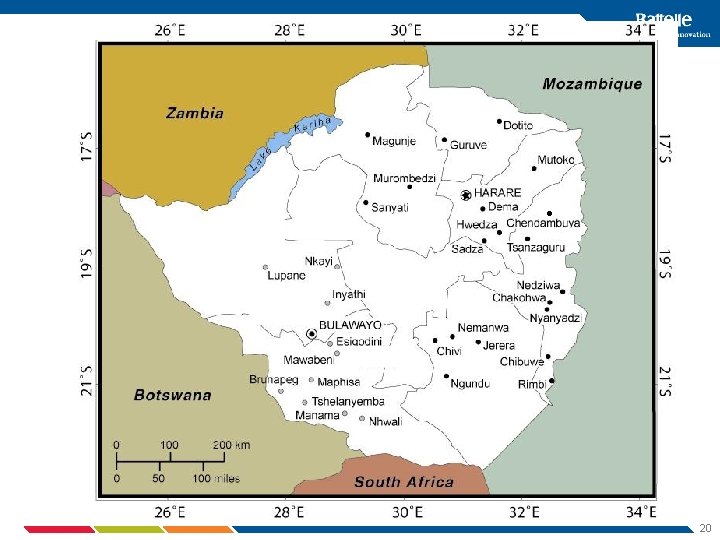
People shopping at Gokwe Growth Point Shops at Dema Growth Point Recruitment Sites Local women selling vegetables outside a store at Nedziwa Growth Point Men drinking Chibuku at a bottle store in Mamina 19 Growth Point
. 20

CPOL Behavioral Intervention • Diffusion of Innovation Theory • Uses Community Popular Opinion Leaders – Deliver persuasive messages to peers to encourage behavior change – Opinions and behavior diffuse through community to become norm • CPOLs trained to have conversations with peers – Focus on effective conversation skill training – Use self as example of behavior change – Assumes CPOLs will target the right issues - Attitudes, norms, self efficacy 21

Application of IBM: Original intent • Apply IBM to: –Inform content of CPOLs’ messages –Structure CPOL conversations with community members –Measure intermediate outcomes - Determine whether behavior change can be explained by change in IBM constructs • Collaborative Trial decisions: –These plans were not implemented across 5 study sites 22

Additional NIAAA funding • Allowed us to apply the IBM to: – Identify appropriate targets for intervention messages – Assess whether those targets were impacted • Qualitative elicitation interviews to identify: – Underlying issues/beliefs for each IBM construct – 8 behaviors: condom use with different partners, monogamy, talking to partners about sex, sex in context of alcohol use, transactional sex • Develop culturally appropriate IBM construct measures for each behavior 23

Final IBM Survey • Measured constructs for each behaviour – Behavioural intention/motivation – Attitude: 9 -14 behavioural beliefs – Perceived Norm: 4 -6 normative beliefs - All three measured with 5 -pt Strongly disagree – Strongly agree – Self-Efficacy: 6 -11 self-efficacy beliefs - 5 -pt Certain I could not – Certain I could • Translated and back-translated to Shona and Ndebele • Conducted survey – Baseline, 12 -mo, 24 -mo 24
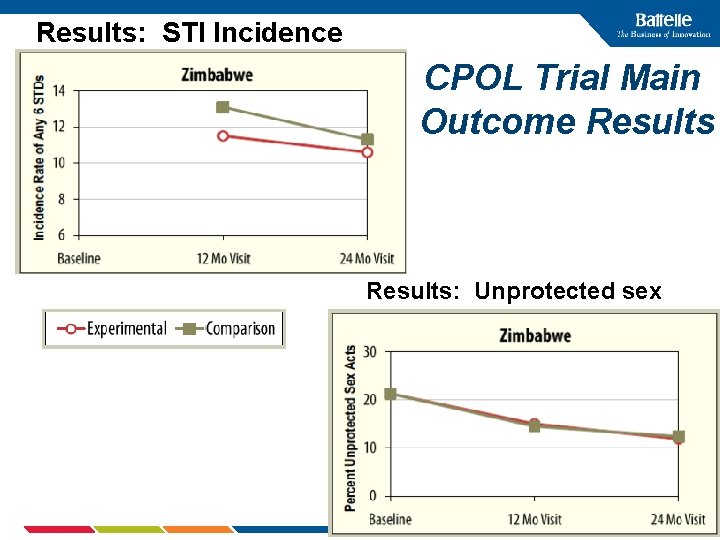
Results: STI Incidence CPOL Trial Main Outcome Results: Unprotected sex 25

CPOL Trial Results Summary • Equal change in behavior in both Intervention and Control sites – Unprotected sex with non-spousal/live-in partners reduced by 33% • Incidence in combined STD/HIV outcome declined equally • CPOL Intervention did not add anything over and above the counseling and testing intervention • Why no differential effect? 26

IBM Analysis • Computed model constructs – mean of beliefs underlying construct • Correlation of constructs with Intention • Correlation to identify construct beliefs that best explain Intention and behavior: – Behavioral beliefs underlying Attitude – Normative beliefs underlying Perceived Norm – Efficacy beliefs underlying Self-Efficacy 27

CONDOM USE – STEADY PARTNER 28

Correlations IBM Constructs with Intention to Use Condoms with Steady Condom Use Steady (n=2, 212) r beta Attitude . 46 . 16** Perceived Norm . 49 . 17** Self Efficacy . 65 . 49** Multiple R . 69 All correlations significant with p < 0. 01; Multiple R significant with p < 0. 01; ** beta weight significant with p < 0. 01 29
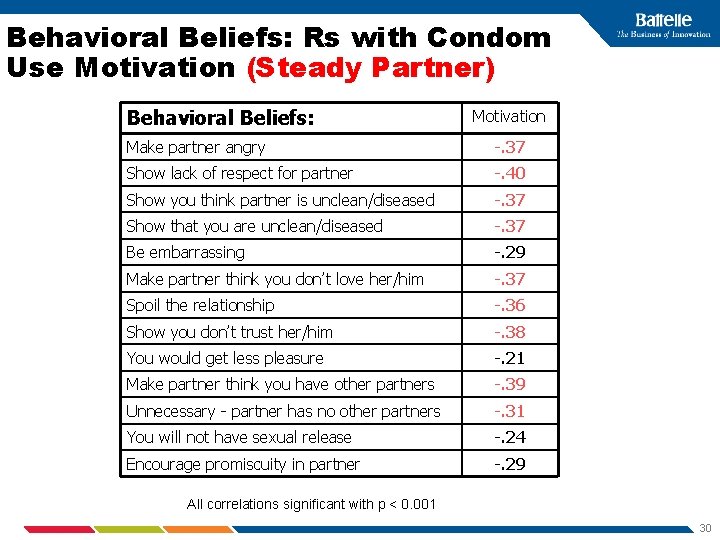

Behavioral Beliefs: Rs with Condom Use Motivation (Steady Partner) Behavioral Beliefs: Motivation Make partner angry -. 37 Show lack of respect for partner -. 40 Show you think partner is unclean/diseased -. 37 Show that you are unclean/diseased -. 37 Be embarrassing -. 29 Make partner think you don’t love her/him -. 37 Spoil the relationship -. 36 Show you don’t trust her/him -. 38 You would get less pleasure -. 21 Make partner think you have other partners -. 39 Unnecessary - partner has no other partners -. 31 You will not have sexual release -. 24 Encourage promiscuity in partner -. 29 All correlations significant with p < 0. 001 30

Normative Beliefs: Rs with Condom Use Motivation (Steady Partner) Normative Beliefs: Your family Motivation Your closest friends Radio shows or radio dramas Your partner . 29 . 25 . 20. 56 All correlations significant with p < 0. 001 31
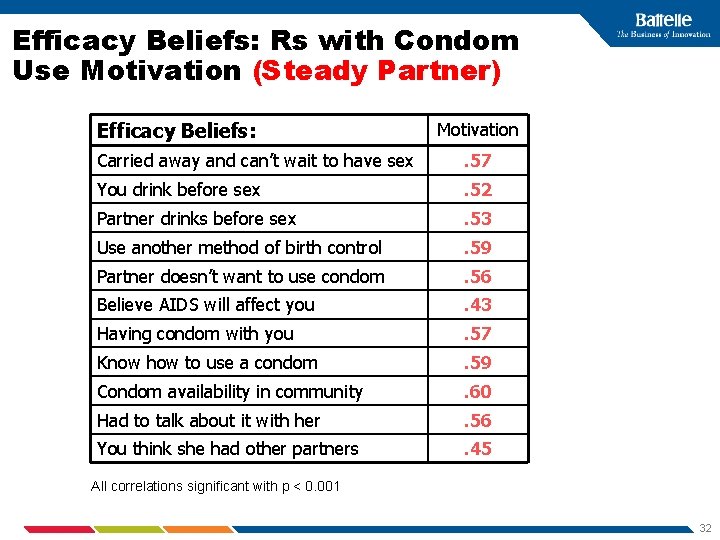
Efficacy Beliefs: Rs with Condom Use Motivation (Steady Partner) Efficacy Beliefs: Motivation Carried away and can’t wait to have sex . 57 You drink before sex . 52 Partner drinks before sex . 53 Use another method of birth control . 59 Partner doesn’t want to use condom . 56 Believe AIDS will affect you . 43 Having condom with you . 57 Know how to use a condom . 59 Condom availability in community . 60 Had to talk about it with her . 56 You think she had other partners . 45 All correlations significant with p < 0. 001 32

Was there differential impact? • Computed change score for each measure – 24 -month minus Baseline • Tested for significant difference: –Intervention vs. Control –If constructs were targeted appropriately, expected greater change for Intervention vs Control 33

Differential Change (Steady Partner Condom Use) Mean Change Condom Use: Control Intervention Sig. Behavior . 70 1. 24 NS Motivation . 38 . 49 NS 34
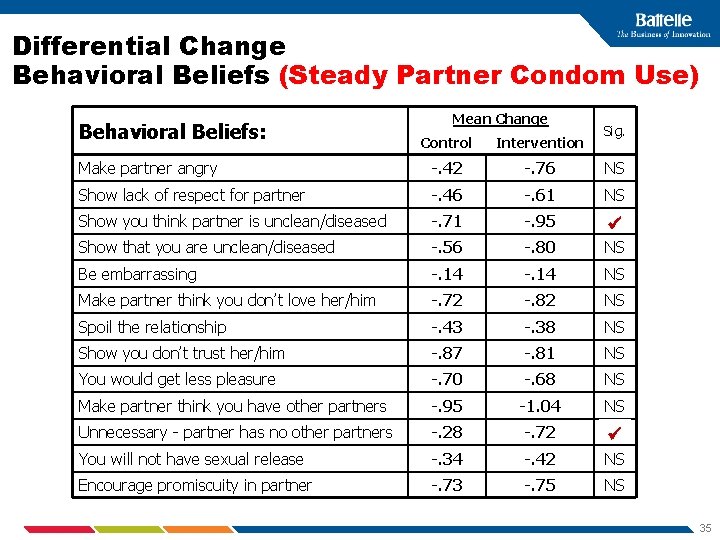
Differential Change Behavioral Beliefs (Steady Partner Condom Use) Behavioral Beliefs: Mean Change Sig. Control Intervention Make partner angry -. 42 -. 76 NS Show lack of respect for partner -. 46 -. 61 NS Show you think partner is unclean/diseased -. 71 -. 95 Show that you are unclean/diseased -. 56 -. 80 NS Be embarrassing -. 14 NS Make partner think you don’t love her/him -. 72 -. 82 NS Spoil the relationship -. 43 -. 38 NS Show you don’t trust her/him -. 87 -. 81 NS You would get less pleasure -. 70 -. 68 NS Make partner think you have other partners -. 95 -1. 04 NS Unnecessary - partner has no other partners -. 28 -. 72 You will not have sexual release -. 34 -. 42 NS Encourage promiscuity in partner -. 73 -. 75 NS 35
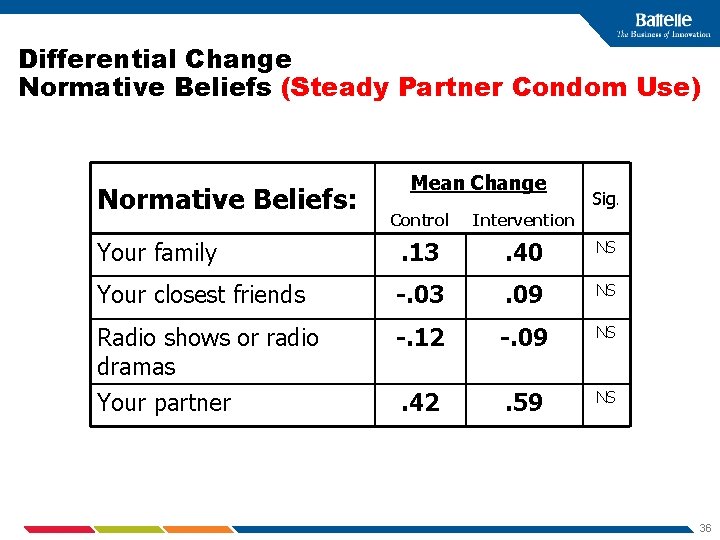
Differential Change Normative Beliefs (Steady Partner Condom Use) Normative Beliefs: Mean Change Sig. Control Intervention Your family . 13 . 40 NS Your closest friends -. 03 . 09 NS Radio shows or radio dramas Your partner -. 12 -. 09 NS . 42 . 59 NS 36
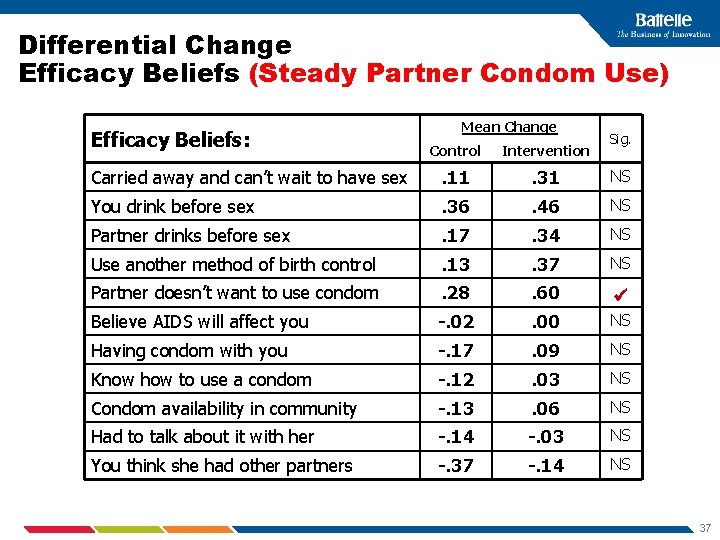
Differential Change Efficacy Beliefs (Steady Partner Condom Use) Efficacy Beliefs: Mean Change Sig. Control Intervention Carried away and can’t wait to have sex . 11 . 31 NS You drink before sex . 36 . 46 NS Partner drinks before sex . 17 . 34 NS Use another method of birth control . 13 . 37 NS Partner doesn’t want to use condom . 28 . 60 Believe AIDS will affect you -. 02 . 00 NS Having condom with you -. 17 . 09 NS Know how to use a condom -. 12 . 03 NS Condom availability in community -. 13 . 06 NS Had to talk about it with her -. 14 -. 03 NS You think she had other partners -. 37 -. 14 NS 37

STICKING TO ONE PARTNER MONOGAMY 38

Behavioral Beliefs: Rs with Monogamy Motivation Behavioral Beliefs: means you would not get the variety in sexual partners you need means you would not be sexually satisfied does not fit into our culture is difficult because you have a high sex drive is difficult since it is traditional for men to have multiple partners makes men less manly means you will not have HIV is something that you cannot commit to means men would get sick means men would lose prestige or standing in the community means women will not get ahead in their jobs Motivation -. 12 -. 28 -. 09* -. 32 -. 20 -. 12. 05* -. 30 -. 12 -. 13 -. 12 All correlations significant with p < 0. 004, except * 39

Normative Beliefs: R with Monogamy Intention Normative Beliefs: your spouse or steady partner your family your closest friends your culture your church radio shows or radio dramas Intention . 21. 15. 20. 12. 13 All correlations significant with p < 0. 001 40
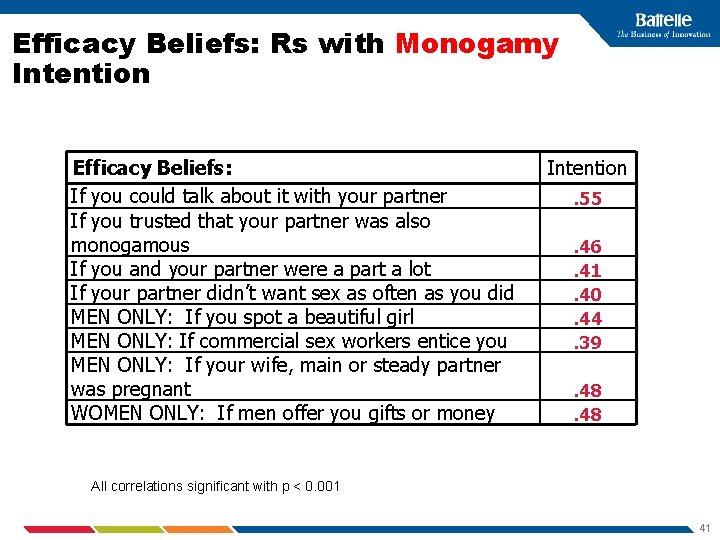
Efficacy Beliefs: Rs with Monogamy Intention Efficacy Beliefs: If you could talk about it with your partner If you trusted that your partner was also monogamous If you and your partner were a part a lot If your partner didn’t want sex as often as you did MEN ONLY: If you spot a beautiful girl MEN ONLY: If commercial sex workers entice you MEN ONLY: If your wife, main or steady partner was pregnant WOMEN ONLY: If men offer you gifts or money Intention. 55. 46. 41. 40. 44. 39. 48 All correlations significant with p < 0. 001 41

Differential Change – Monogamy Mean Change Condom Use: Intention Control Intervention Sig. . 09 . 07 NS 42
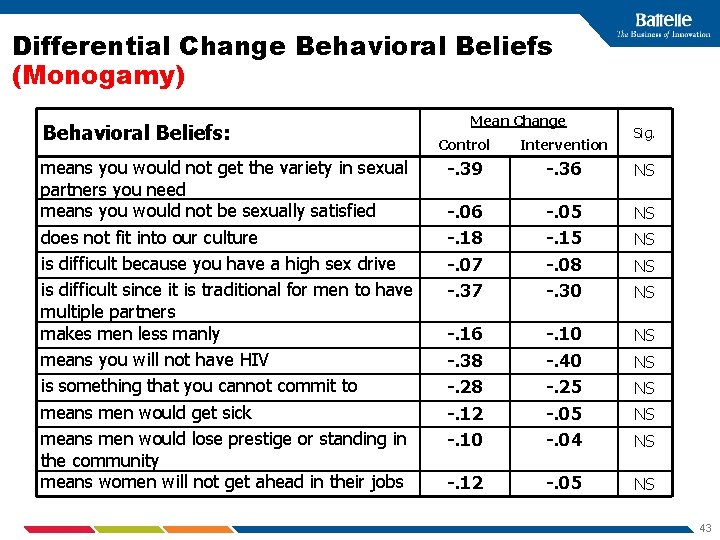
Differential Change Behavioral Beliefs (Monogamy) Behavioral Beliefs: means you would not get the variety in sexual partners you need means you would not be sexually satisfied does not fit into our culture is difficult because you have a high sex drive is difficult since it is traditional for men to have multiple partners makes men less manly means you will not have HIV is something that you cannot commit to means men would get sick means men would lose prestige or standing in the community means women will not get ahead in their jobs Mean Change Sig. Control Intervention -. 39 -. 36 NS -. 06 -. 18 -. 07 -. 37 -. 05 -. 15 -. 08 -. 30 NS -. 16 -. 38 -. 28 -. 12 -. 10 -. 40 -. 25 -. 04 NS -. 12 -. 05 NS NS 43
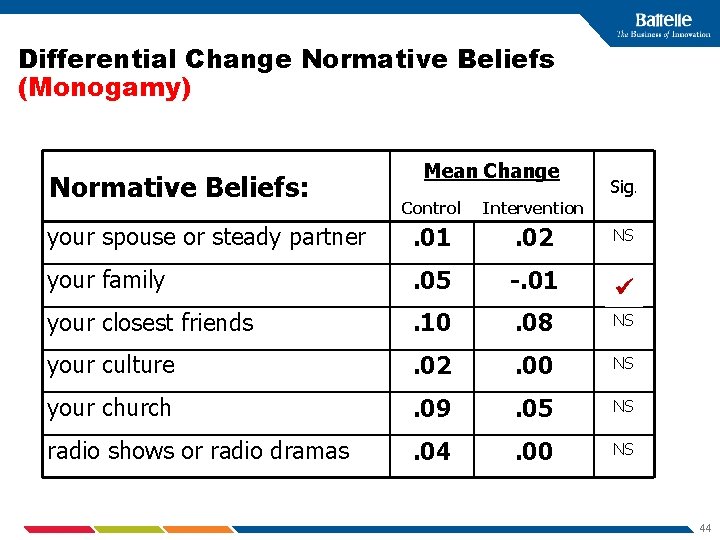
Differential Change Normative Beliefs (Monogamy) Normative Beliefs: Mean Change Sig. Control Intervention your spouse or steady partner . 01 . 02 your family . 05 -. 01 your closest friends . 10 . 08 NS your culture . 02 . 00 NS your church . 09 . 05 NS radio shows or radio dramas . 04 . 00 NS NS 44
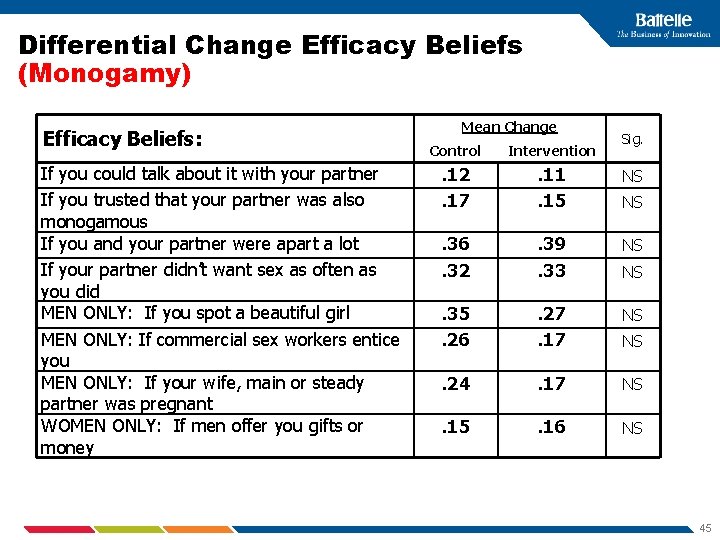
Differential Change Efficacy Beliefs (Monogamy) Efficacy Beliefs: If you could talk about it with your partner If you trusted that your partner was also monogamous If you and your partner were apart a lot If your partner didn’t want sex as often as you did MEN ONLY: If you spot a beautiful girl MEN ONLY: If commercial sex workers entice you MEN ONLY: If your wife, main or steady partner was pregnant WOMEN ONLY: If men offer you gifts or money Mean Change Sig. Control Intervention . 12. 17 . 11. 15 NS . 36. 32 . 39. 33 NS . 35. 26 . 27. 17 NS . 24 . 17 NS . 15 . 16 NS NS 45

Impact and Process Evaluation • CPOLs had conversations • CPOLs expressed frustration: – Did not know what to target in conversations • Data shows CPOLs did not target/impact critical beliefs – Training successful in motivating conversations and conversation skills – Not successful in teaching CPOLs how to target and change beliefs shown to be key in changing behavior 46

Enhanced CPOL Intervention • IBM complements CPOL – CPOL provides channel of persuasive communication – IBM provides behavioral theory to identify targets of persuasive messages • Train CPOLs in IBM conceptualization • Train CPOLs to have guided conversations – Use IBM conversation guide to systematically identify beliefs to target for each person – Target issues identified • Train CPOLs to develop messages for target beliefs identified in this research 47

Enhanced CPOL intervention • Used in roll-out to comparison sites • Trainers and CPOLs extremely positive –CPOLs understood IBM conceptualization –Expressed greater confidence in: - Having targeted conversations with peers - Having an impact on behavior • Not evaluated 48

Closing the Gap in Male Circumcision Uptake Environmental and Behavioral Factors Shaping Male Circumcision Decisions in Zimbabwe Funded by: National Institute of Mental Health 49
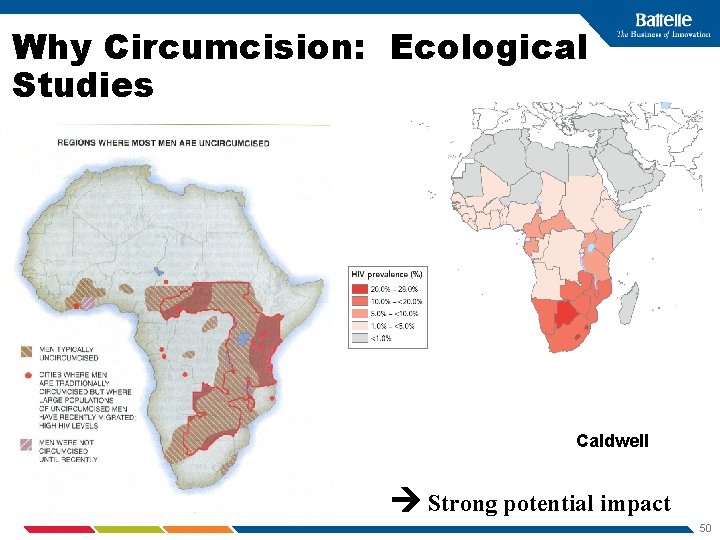
Why Circumcision: Ecological Studies Caldwell Strong potential impact 50
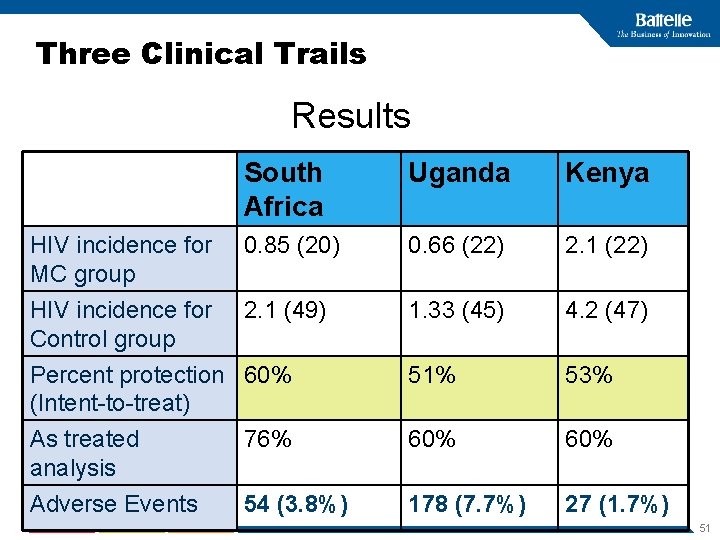
Three Clinical Trails Results South Africa Uganda Kenya HIV incidence for MC group 0. 85 (20) 0. 66 (22) 2. 1 (22) HIV incidence for Control group 2. 1 (49) 1. 33 (45) 4. 2 (47) Percent protection 60% (Intent-to-treat) 51% 53% As treated analysis 76% 60% Adverse Events 54 (3. 8%) 178 (7. 7%) 27 (1. 7%) 51

The Problem • Consensus (WHO, UNAIDS) that MC be included in comprehensive HIV prevention programs where – HIV prevalence > 15% – Heterosexual transmission – Large proportion men (> 80%) not circumcised • High prevalence countries are implementing MC programs 52

Scaling Up MC Scaling up of MC to reach 80% of adult and newborn males in 14 African countries by 2015 would require: • Almost 12 million MCs to be performed in the peak year, 2012 alone (206, 000 done since 2008) • Over 1. 1 million MCs in Zimbabwe in peak year, 2012 – 4, 583 MCs per day – 150 to 200 doctors + nurse teams (each doing 30/day) 53

Operations Research Needed • RCT study sites – Some success in scaling up – Encountered barriers to MC adoption - Kenya, Orange Farm • Research is needed to: – Determine factors affecting - MC uptake and adoption – Investigate - Environmental and policy implications - Behavioral determinants – Include all stakeholders / target groups 54

Overall Goals • Identify and understand factors affecting motivation to adopt MC • Seven main study groups: – Policy makers and stakeholders – who may promote MC – Clinicians – who may recommend or perform MC – Adolescent boys (13 -17) – who may adopt MC – Adult men (18 -30) – who may adopt MC – Women – who may impact men’s MC decisions – Expectant parents – who may decide for infants re MC – Parents of young boys (13 -17) – who may decide for teen sons re MC 55
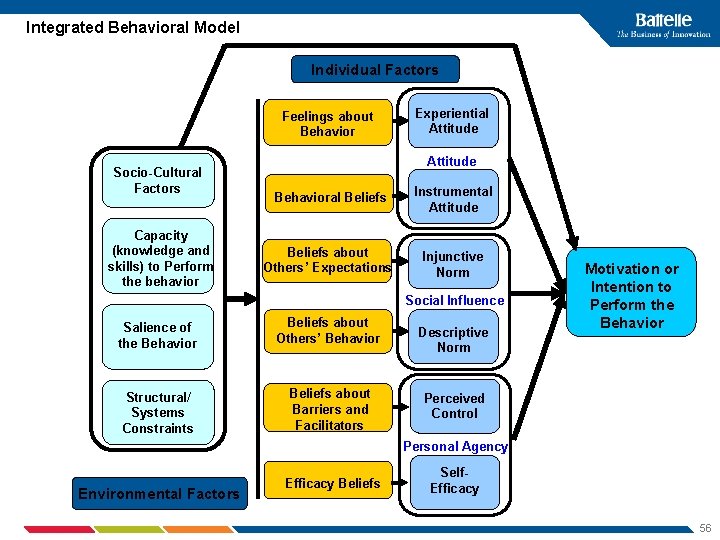
Integrated Behavioral Model Individual Factors Feelings about Behavior Socio-Cultural Factors Capacity (knowledge and skills) to Perform the behavior Experiential Attitude Behavioral Beliefs Instrumental Attitude Beliefs about Others’ Expectations Injunctive Norm Social Influence Salience of the Behavior Beliefs about Others’ Behavior Structural/ Systems Constraints Beliefs about Barriers and Facilitators Descriptive Norm Motivation or Intention to Perform the Behavior Perceived Control Personal Agency Environmental Factors Efficacy Beliefs Self. Efficacy 56
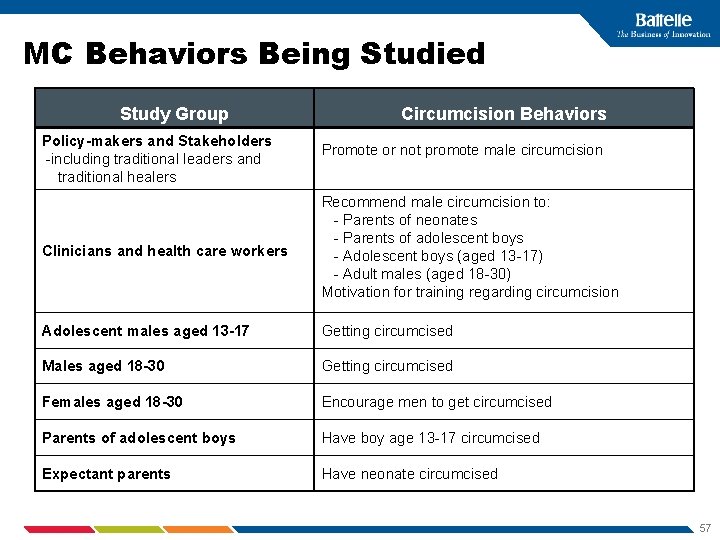

MC Behaviors Being Studied Study Group Policy-makers and Stakeholders -including traditional leaders and traditional healers Circumcision Behaviors Promote or not promote male circumcision Clinicians and health care workers Recommend male circumcision to: - Parents of neonates - Parents of adolescent boys - Adolescent boys (aged 13 -17) - Adult males (aged 18 -30) Motivation for training regarding circumcision Adolescent males aged 13 -17 Getting circumcised Males aged 18 -30 Getting circumcised Females aged 18 -30 Encourage men to get circumcised Parents of adolescent boys Have boy age 13 -17 circumcised Expectant parents Have neonate circumcised 57
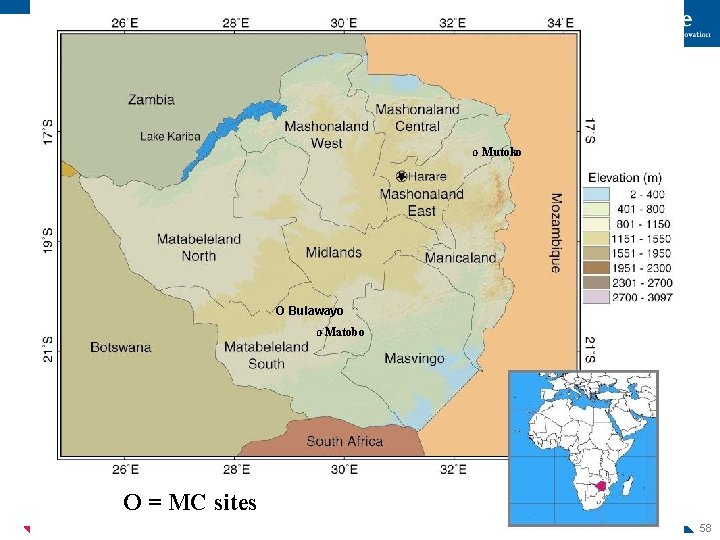
O Mutoko O Bulawayo O Matobo O = MC sites 58
Study Design • Three main study phases, each including: – Data collection – Analysis – Each following from prior phase • Integrated Behavioral Model guides all three phases • Carried out in 4 sites: – Two urban (Harare, Bulawayo) – Two rural (Mutoko, Matobo) • Results will be provided to policy-makers – Throughout each phase – At conclusion of each phase 59

Three Phases and Progress to Date • Qualitative Study – Individual semi-structured interviews – 320 interviews conducted with study groups • Quantitative Survey – 7460 face-to-face interviews with study groups – Interviews in process • Message development and testing – Design messages targeting issues identified in survey analysis – Test MC message impact on small samples – To be done after survey data shows us most important issues to focus messages on 60

Circumcision Center Interviewing clinicians Interviewing Adults and Parents Adolescents who may be targets of MC 61

Operations Research will: ØClose the gap in uptake through: üEvidence-based message design üEvidence-based community mobilization 62

The Zichire Family Health Study Psychosocial Support to HIV/AIDS Affected Children in Zimbabwe Funded by: National Institute of Nursing Research 63
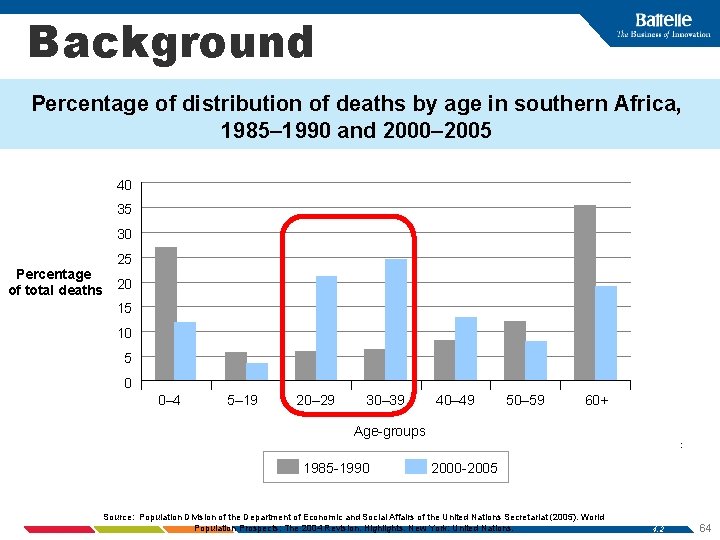
Background Percentage of distribution of deaths by age in southern Africa, 1985– 1990 and 2000– 2005 40 35 30 25 Percentage of total deaths 20 15 10 5 0 0– 4 5– 19 20– 29 30– 39 40– 49 50– 59 60+ Age-groups : 1985 -1990 2000 -2005 Source: Population Division of the Department of Economic and Social Affairs of the United Nations Secretariat (2005). World Population Prospects: The 2004 Revision. Highlights. New York: United Nations. 4. 2 64

Impact of HIV • HIV rates are still high in Zimbabwe – Approximately 1. 4 million PLWHA (aged 15 -49) – Approximately 180, 000 new infections a year • Treatment is still fairly rare • About 35, 000 -40, 000 individuals on ART • Mortality is high – Over 3, 200 individuals die a week • Individuals, children and families are highly impacted • Little research on psychosocial effects conducted in high prevalence countries 65

Family Health Study • Why this Study? – Knowledge about HIV/AIDS high, infections continue, 1 in 5 individuals has HIV – Some evidence that behavior change is occurring (2001 1 of 3 infected; 2005 – 1 of 5 infected) – While behavior has changed somewhat, the reduction in prevalence of HIV is also due to mortality associated with infections maturing – Mortality rates continue to be high – Individuals, children and families are highly impacted, but little research on psychosocial effects is conducted in high prevalence countries 66

67

Meeting needs of Families living with HIV and AIDS • Most interventions focused on meeting needs of orphans and vulnerable children, target basic needs • Some teach skills such as home-based care • Support groups for PLWHA exist • Support groups for families do not • Very few programs target the psycho-social needs of children or families who are living with the consequences of HIV, especially in SSA 68

AIDS the Endless Song of Sorrow In our heart is a song A voice that forever sings A cry for the pain it brings For in the world we are living Is full of sorrow AIDS the eternal song of sorrow Children’s emotions despair To the serenity of loneliness So hurtful of our hearts Deprived of all the happiness For a tear will forever be shed In the pain of today and tomorrow To the part that sings AIDS the endless song of sorrow 69

Project TALC Results • Research by Mary Jane Rotheram and colleagues demonstrated that: – HIV has a long term negative impact on adjustment of both parents and their adolescent children; – Impact is intergenerational (is experienced by the offspring of the adolescents of parents living with HIV); – A coping skills intervention can improve outcomes (4 -year followup) for both parents and their adolescent children – Has a positive impact (6 year follow-up) on the adolescent child’s offspring • The team also established that among adolescents, young adults, and parents living with HIV about: – 33%-50% maintain transmission acts, – 33% do not take recommended medications, and – 70% experience mental health problems 70

Project TALC Zimbabwe • The primary goal in this project is to provide psychosocial support to children living with a parent who has HIV/AIDS • We will do this by: – Implementing a Randomized Control Phase II Community -based Trial to evaluate an intervention (Project TALC) • Working in 4 residential areas (Harare, Bulawayo) with a cohort of at least 400 families where a parent has HIV/AIDS 71
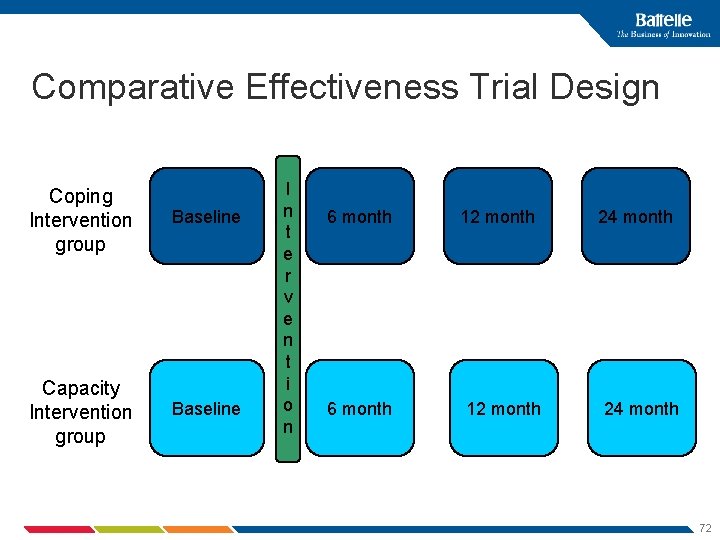
Comparative Effectiveness Trial Design Coping Intervention group Baseline Capacity Intervention group Baseline I n t e r v e n t i o n 6 month 12 month 24 month 72

Study Phases and Goals • Census – To Identify families with 12 -18 year olds • Health Screening – To identify HIV + parents • Baseline – To obtain pre-intervention measures • Intervention implementation • Follow-ups – 6 -mo, 12 -mo, 24 mo – To assess impact of intervnetion 73

Zichire Mobile Office: Starting the Health Assessment 74

Census Results • Housing Units identified: 9, 442 • Housing Units enumerated: 8, 256 (87%) • Family Units enumerated: 14, 205 - average families per HU: 1. 7 - Average family size: 3. 8 • Families with children (12 -18 yrs) in residence identified: 5 972 (40%) • Families with resident parent and biological child (1218): 4, 297 • 35% of children (12 -18) do not live with biological parent 75

Approaching a housing unit Results on site: Getting ready: Testing Results 76
Health Screening Results • Harare and Bulawayo Health Screening – 6, 570 adults eligible for Health Screening – 2, 548 (39%) adults had Health Screening – 1, 823 (72%) had blood draw for HIV test – 363 HIV positive – 234 (9%) self-reported HIV+ - 34% males and 24% females reported HIV+ status – 20% individuals HIV positive – 32% had previously been tested 77
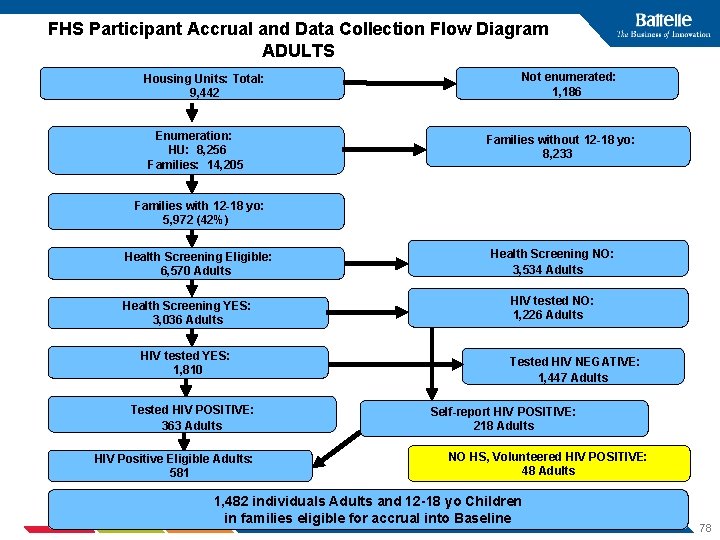
FHS Participant Accrual and Data Collection Flow Diagram ADULTS Housing Units: Total: 9, 442 Enumeration: HU: 8, 256 Families: 14, 205 Not enumerated: 1, 186 Families without 12 -18 yo: 8, 233 Families with 12 -18 yo: 5, 972 (42%) Health Screening Eligible: 6, 570 Adults Health Screening YES: 3, 036 Adults HIV tested YES: 1, 810 Tested HIV POSITIVE: 363 Adults HIV Positive Eligible Adults: 581 Health Screening NO: 3, 534 Adults HIV tested NO: 1, 226 Adults Tested HIV NEGATIVE: 1, 447 Adults Self-report HIV POSITIVE: 218 Adults NO HS, Volunteered HIV POSITIVE: 48 Adults 1, 482 individuals Adults and 12 -18 yo Children in families eligible for accrual into Baseline 78

Baseline Methods • Approached families identified via Census and Health Screening • Explained we were in final phase of the study • Explained we identified them in the first phases of the study • Confirmed that families have: – At least one parent living at home – At least one child aged 12 -18 living at home (not in boarding school) • Explained that Baseline may make families eligible for a program we were implementing in their neighborhood • Scheduled Baseline Assessment with each parent • Recruited adolescent with parental permission 79

Baseline Recruitment and Assessment 80

Baseline • 1, 482 individuals Adults and 12 -18 yo Children in families eligible for accrual (of this, n=38 were HIVspouses) • 1, 007 individuals were interviewed • One adult and one child aged 12 -18 in family • Measures: Adults – Demographics – Psychosocial: stress, depression, anxiety, family functioning and communication, QOL, social support, HIV knowledge, disclosure of HIV status, coping with illness – Parenting skills – Behavioral risks: substance use, sexual risk – Health: clinical assessment, treatment documentation 81

Measures – child level • Demographics, including living situation • Index of school involvement/success: – School attendance, grade level attained, performing at grade level, academic grades, – educational aspirations, truancy, suspensions/expulsions, behavioral problems at school • Psychological symptoms of emotional distress • Family interactions and communication • Global self-esteem • Sexual behavior • Alcohol and substance use 82

Intervention • Implemented intervention in 4 residential areas, among our families • 717 individuals participated in our interventions – Adult HIV + parents (354), teen children (363) – Half went through the ‘coping’, half through the ‘capacity’ intervention • Adult Intervention: 14 sessions • Adolescents’: 10 sessions • Assessed psychosocial, behavioral and HIV endpoints at 6 - and 12 and 24 - month FUs 83

Baseline Results • 431 parents assessed – 398 Index parents – 33 spouses • 478 children assessed • All assessments included: – Health and symptom assessment (HSA) – Psychosocial assessment (PSA) 84

Parent sample • Mostly female (83%) • Mean age 41 years • Mean of 3. 6 children • 98% attended school • 90% go to church or place of worship • Importance of religion • 91% Very important • 8% Somewhat important • 1% Not important at all 85
Health • General Health PARENTS % Poor Fair Good Very Good Excellent 13 34 20 7 26 • Satisfaction with Health PARENTS % Very Dissatisfied 14 25 Neither Satisfied Very Satisfied 5 36 20 86

Use of Health Care: Last 6 months • 1. 3 (mean) visits to a doctor or other health care worker • 67% had no visits to a doctor or other health care worker • 1% saw a traditional healer • 2. 3 (mean) visits to a health clinic 87

Sexual Practices and Sexual History • 24% of men and 49% of women had no sexual partner in the past year • 63% men and 48% women had one partner • 7% men and 1% women had 2 partners, • 6% men and 2% women had 3+ partners • 63% of men and 47% of women reported using a condom at last sex 88

Shona Symptom Scale (11 items) (α=. 88) Symptoms % Yes Thinking deeply/thinking about many things 52 Lose temper or get annoyed over trivial things 23 Nightmares or bad dreams 28 Stomach was aching 34 Run down and tired 42 Generally unhappy 36 Moments life was so hard, felt like crying, or 38 cried 89
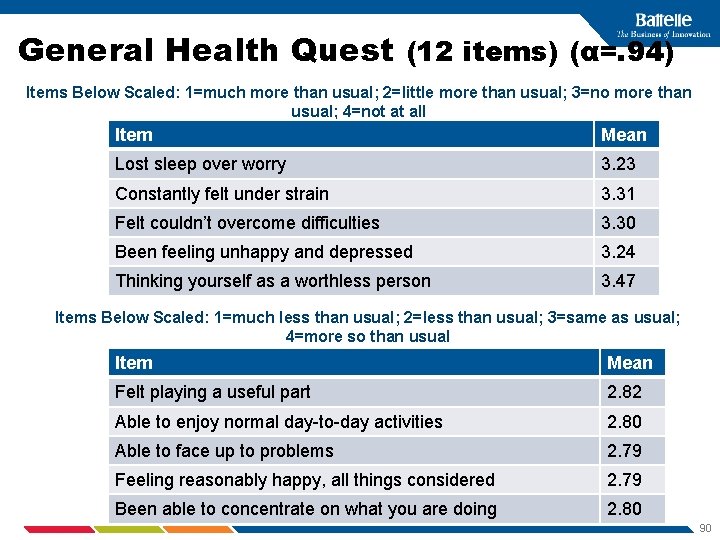

General Health Quest (12 items) (α=. 94) Items Below Scaled: 1=much more than usual; 2=little more than usual; 3=no more than usual; 4=not at all Item Mean Lost sleep over worry 3. 23 Constantly felt under strain 3. 31 Felt couldn’t overcome difficulties 3. 30 Been feeling unhappy and depressed 3. 24 Thinking yourself as a worthless person 3. 47 Items Below Scaled: 1=much less than usual; 2=less than usual; 3=same as usual; 4=more so than usual Item Mean Felt playing a useful part 2. 82 Able to enjoy normal day-to-day activities 2. 80 Able to face up to problems 2. 79 Feeling reasonably happy, all things considered 2. 79 Been able to concentrate on what you are doing 2. 80 90

Disclosure of HIV results to at least one person is: 87% • sister (35%) or daughter (30%) • spouse (29%) • mother (21%) or father (8%) • brother (19%) or son (23%) • best female friend (15%) or best male friend (8%) • aunt (8%) • ministers (3%) 91

How did your family react to results? • They: – were supportive after hearing you had HIV (98%) – wanted to make sure you are all right (96%) – said it was your partner’s fault that you had HIV (31%) – said your partner is a bad person (26%) – asked if you or your partner had sex with others (19%) – said it was your fault you had HIV (7%) – said you are a bad person (3%) 92
Family Relationships and Interactions Parents report overall good relationships with their children age 12 -18 years 97% of mothers and 94% of fathers report good relationships with all of their teenage children Talk about: Mothers Fathers Delay of sex 81% 72% Abstinence/avoiding sex 82% 72% Boy/girlfriend relationships 75% 66% Sex and sexuality 58% 54% Condom use 35% 39% HIV/AIDS 79% 70% 93

Children’s Demographics • Mean age: 14. 9 • 51% males • 90% live with mother; 40% live with father • 83% in school; – 96% 12 -15 year olds; 57% 16 -19 year olds • 92% go to church, mosque, or other place of worship • 96% learned about HIV and AIDS in school 94

Family Relationships and Interactions Children report overall good relationships with family members, esp. mothers – 97% of teens report good relationships with mother – 83% of teens report good relationships with father Talk about: Mothers Fathers Delay of sex 83% 30% Abstinence/avoiding sex 63% 29% Boy/girlfriend relationships 50% 30% Sex and sexuality 38% 15% Condom use 25% 12% HIV/AIDS 68% 34% 95

Children’s Measures • Youth Risk Behavioral Surveillance System (YRBSS) – Assessed risk • Shona Symptom Scale (11 items) – α =. 70 • General Health Questionnaire (12 Items) – Assesses stress, anxiety, depression – α =. 85 • Edinburg Depression Scale (12 items) – α =. 84 96

Children’s Risk Behaviors • 19% have boy/girlfriend • 7% (22) had sex (age range 14 -20) • 90% who had sex were 16 -18 years old • 4 had forced sex • Sexual activity in last 3 months • 5 teens, with 1 partner each • 53% used a condom at last sex • Less than 10% have tried alcohol, cigarettes, or other substances (marijuana, glue sniffing) 97

Shona Symptom Scale (11 items) Symptoms Thinking deeply/thinking about many things Lose temper or get annoyed over trivial things Nightmares or bad dreams Stomach was aching Run down and tired Generally unhappy Moments life was so hard, felt like crying, or cried % Yes 17 15 13 26 17 13 12 98
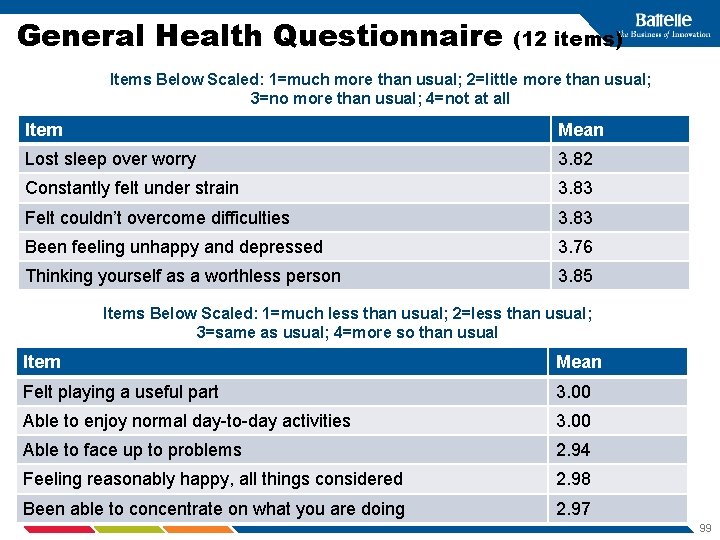
General Health Questionnaire (12 items) Items Below Scaled: 1=much more than usual; 2=little more than usual; 3=no more than usual; 4=not at all Item Mean Lost sleep over worry 3. 82 Constantly felt under strain 3. 83 Felt couldn’t overcome difficulties 3. 83 Been feeling unhappy and depressed 3. 76 Thinking yourself as a worthless person 3. 85 Items Below Scaled: 1=much less than usual; 2=less than usual; 3=same as usual; 4=more so than usual Item Mean Felt playing a useful part 3. 00 Able to enjoy normal day-to-day activities 3. 00 Able to face up to problems 2. 94 Feeling reasonably happy, all things considered 2. 98 Been able to concentrate on what you are doing 2. 97 99

School Issues • 83% are in school • 32% have been bullied, intimidated or pushed around – About two thirds 1 or 2 times • 16% have been in a physical fight – 70% once • 52% have had property stolen or damaged – About three quarters between 1 -3 times • Felt so sad and hopeless in past year, stopped usual activities – 7% 100

Conclusions • Research shows teens can be vulnerable to negative effects if parents have HIV/AIDS • These teens in Zimbabwe are not exhibiting high risk behavior, high stress • Many may not be aware of parental HIV; but two thirds of coping arm teens went through the teens “Aware of parental status” intervention • School tribulations may be a sign of difficulty • Teens are picked on at fairly high rates • Unfortunately, we don’t know if this is due to living with a parent with HIV, or if this is normative in Zimbabwe • Research among teens in schools to establish normative numbers for risk is needed 101

Explanations • School may be protective • Other research from Zimbabwe confirms that teens in school have low risk behavior on average • Targeting teens in schools with efficacious evidence-based HIV prevention programs may be important • Parenting is protective; most teens lived with mothers, and had good relationships with mothers 102

Explanations • These children are used to hardship, given what they have been growing up with • Zimbabwean culture is protective of children – Not discussing problems so as to not burden children • Zimbabwean culture also has family solidarity values – One does not discuss problems outside the family 103

HIV Research in Zimbabwe: Future Directions • Family Health Study continued among grandparents who end up fostering AIDS orphans • HIV prevention targeting youth 13 -19 • Neuro-cognitive effects of HIV acute infection • Other Sexually transmitted diseases (STI etiology study) – Herpes, Syphilis, Human Papillomavirus (HPV) • Male circumcision device testing • Prevention with Positives • Monitoring and evaluation of public health programs and approaches • Continued capacity building – STI Annual Workshop 104

Zimbabwe Victoria Falls – “the smoke that thunders” 105

Zimbabwe Great Zimbabwe Built 1100 – 1400 106

Zimbabwe 107

ACKNOWLEDGEMENTS Funded by: NIMH, NINR, NIAAA - Battelle Team: Terry Johnson, Bill Grady, Ed Liebow, Hunter Handsfield, Lisa Cubbins, April Greek, Diana Echeverria, Kasia Alderman, Gary Chovnick, Carolina Mejia, Susan Hauth, Kate Blessing, Burk Dowell, Peter Klein - Zi. CHIRe Team: Mufuta Tshimanga, MD, MPH, director Zichire Godfrey Woelk, Ph. D (Site PI CPOL intervention) Sally-Nyandiya Bundy (Site PI FHS intervention) Tinashe Muromo, BSc (Hon), MPhil. , Ph. C Rachel Gatsi, Office Manager Philani Moyo and Ethnography Team Reggie Mutsindiri and Nurses Team Patrick Mateta, Luanne Rodgers and Lab Team Walter Chikanya and Intervention Team Pesenai Chatikobo and Process Evaluation Team Gay Hendrikse, Admin Staff, Transcription Team, Security Team Gift Mutepfe and Driving Team - All Study Participants 108
- Slides: 108