YERSINIA PASTEURELLA GENUS YERSINIA Short gram negative bacilli

YERSINIA, PASTEURELLA

GENUS YERSINIA: • Short, gram negative bacilli showing bipolar staining • Three medically imp species: 1. Y. pestis- Plague 2. Y. pseudotuberculosis: rodents 3. Y. enterocolitica – enteric disaese in humans • Primary pathogens of rodents and accidentally infect man

Morphology: • Nonmotile except (Y. pseudotuberculosis & Y. enterocolitica) • Named after Alexander Yersin – discovered plague bacilli YERSINIA PESTIS • Causative agent of plague Morphology: Short, gram negative bacilli- bipolar staining SAFETY PIN APPEARENCE
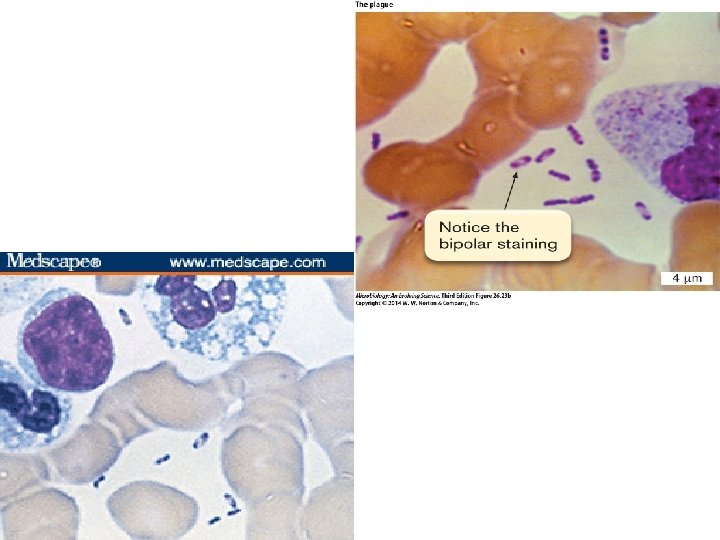

Culture: • Nutrient agar: small transparent colonies • Blood agar: non haemolytic , dark brown colonies due to absorption of haemin pigment • Mac conkey agar: Non lactose fermenting colonies • Ghee broth : organisms grown in s flask of oil or ghee a characteristic growth occurs which hangs down from the under the surface of the oil, resembling stalactites – STALACITE GROWTH

BIOCHEMICAL REACTIONS: • Ferments glucose, Mannitol and maltose with production of acid only • Catalase positive • Indole, urease, citrate, MR, VP – negative

BIOTYPES OF Y. pestis: • Based on glycerol fermentation and nitrate reduction VARIETY GLYCEROL FERMENTATIO N NITRATE REDUCTION DISTRIBUTION Y. pestis var orientalis _ + India, china, Myanmar & wild plague in USA Y. pestis var antiqua + + Justinian plague Y. pestis var mediaevalis + _ South East Russia
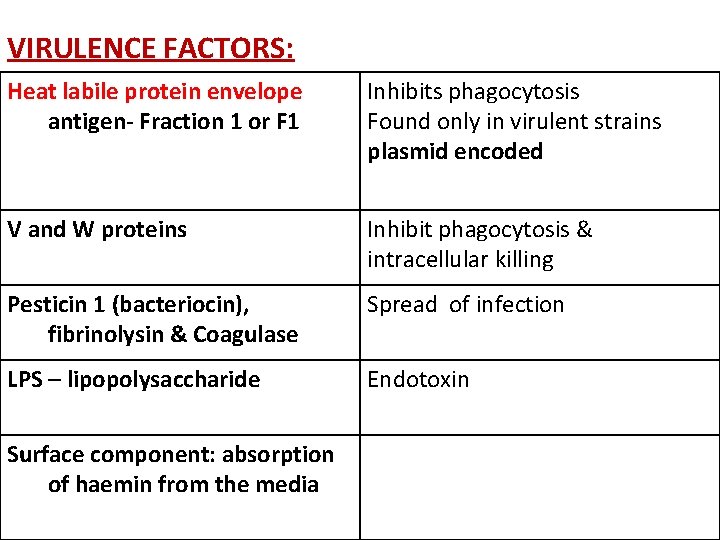
VIRULENCE FACTORS: Heat labile protein envelope antigen- Fraction 1 or F 1 Inhibits phagocytosis Found only in virulent strains plasmid encoded V and W proteins Inhibit phagocytosis & intracellular killing Pesticin 1 (bacteriocin), fibrinolysin & Coagulase Spread of infection LPS – lipopolysaccharide Endotoxin Surface component: absorption of haemin from the media

PLAGUE

PATHOGENESIS of PLAGUE: • Y. pestis – natural pathogen of rodents • Causes zoonotic disease – PLAGUE • Transmitted by bite of rat flea (X. cheopis) • Two natural cycles of the disease: 1. Urban plague – man & rodents 2. Sylvatic plague – wild animals & rodents
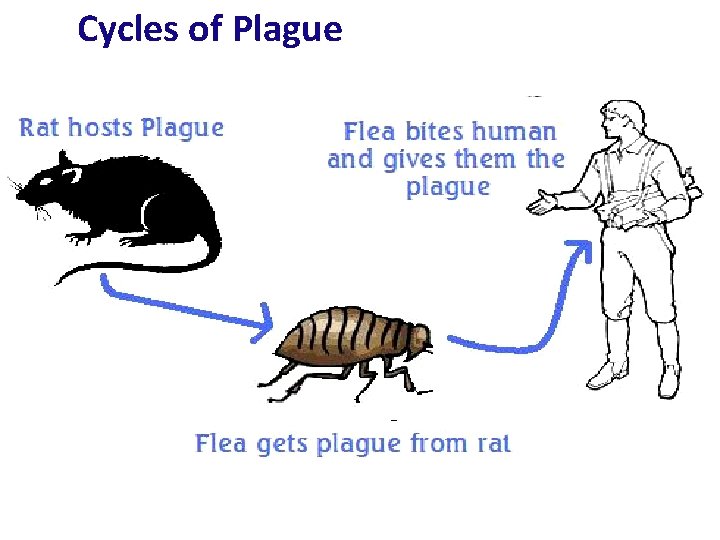
Cycles of Plague
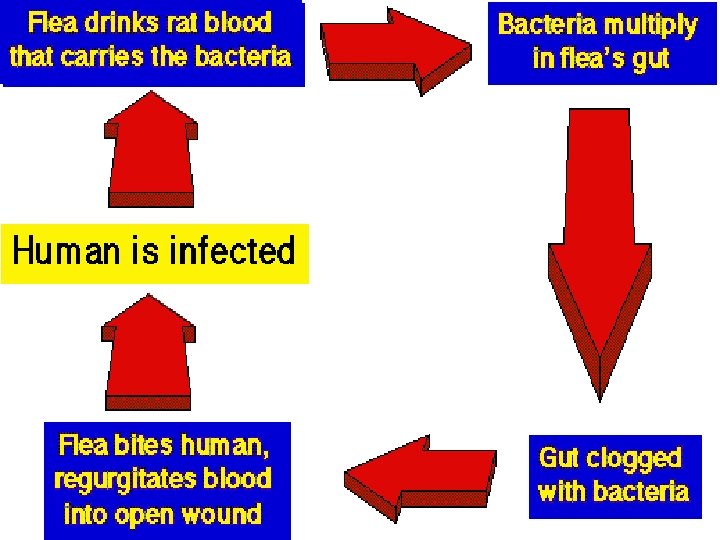

• In man plague occurs in 3 forms: 1. Bubonic plague 2. Pneumonic plague 3. Septicaemic plague BUBONIC PLAGUE: • Plague bacillus enters the body via bite of an infected rat flea on the legs. • Inguinal lymph nodes involved – bubonic plague: Lymph nodes enlarge and suppurate

• Fever chills and malaise • Bacteria reach the blood & disseminated • If not treated may progress to meningeal plague PNEUMONIC PLAGUE: • • • Highly infectious form Involving lungs producing haemorrhagic pneumonia Transmitted by droplet infection Usually secondary to bubonic plague Fever, cough with expectoration

SEPTICAEMIC PLAGUE: • Presence of bacteria in the blood • Usually complication of pneumonic or bubonic plague • Massive hemorrhage – BLACK DEATH EPIDEMIOLOGY: • • • Plague- Zoonotic disease Spread from domestic rats to man by bite of rat flea Plague – greatest killer in history of mankind Several epidemics in India – outbreak in 1994 (Maharashtra, Gujarat, Delhi, UP, MP , Karnataka)

• 2002 outbreak in Shimla • Scattered natural foci still exist: Kolar, Bead- Lathur belt in Maharashtra, Shimla and Uttaranchal LAB DIAGNOSIS: Specimens; • • • Pus/ fluid aspirated from infected lymph nodes Sputum / blood in pneumonic plague Blood in septicemic plague Splenic tissue- postmortem CSF in meningeal plague
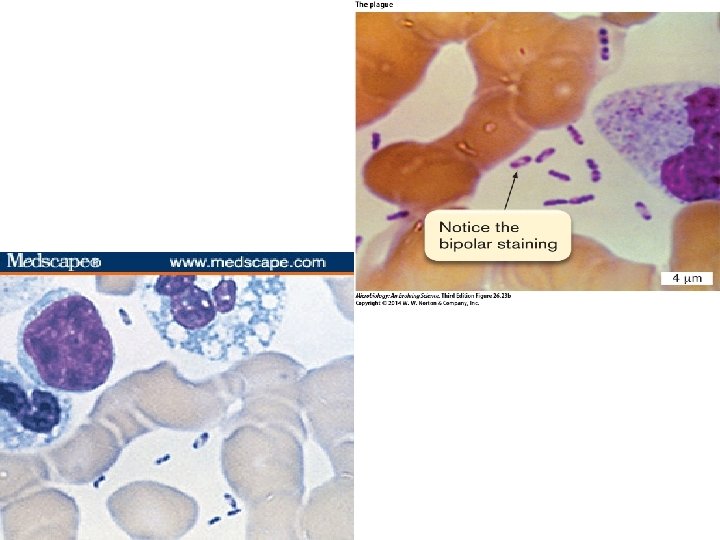

Direct microscopy: • Gram stain- gram negative coccobacilli • Methylene blue stain- bipolar staining (WAYSON stain) Culture: Blood agar: incubated at 270 C Biochemical tests for identification On ghee broth- stalactite growth Animal inoculation: • • Rats injected s/c with exudates from lymph nodes. Animals die in 2 -5 days. Postmortem reveals- regional lymph nodes congested. Bacteria found in spleen, heart blood etc

Antigen detection: • F 1 glycoprotein antigen – detected in aspirated fluid by ELISA or immunoflourescence Serological tests: • Detection of antibodies to F 1 antigen by CFT PCR: rapid & sensitive for diagnosis of plague in clinical samples

TREATMENT: • Tetracycline –drug of choice • Streptomycin, Chloramphenicol, kanamycin can be used VACCINE: • Killed vaccine: whole bacterial culture antigen of plague bacillus • Live vaccine: prepared from 2 avirulent strains of Y. pestis CHEMOPROPHYLAXIS: • Close contacts – tetracycline 500 mg 6 th hrly for one week.

YERSINIA ENTEROCOLITICA – gastroenteritis • Transmission – fecal contamination, domestic animals • water • milk – meat

– Found worldwide – Found in pigs, cats and dogs – Human also infected by ingestion of contaminated food or water – Some infections result from eating contaminated meat – Is able to survive refrigerator temperatures (can use “cold enrichment” to isolate)

Human disease are of three types: 1. Self limiting gastroenteritis/ enterocolitis in young children 2. Mesenteric adenitis and inflammatory terminal ileitis in older children ( mimics appendicitis) 3. Systemic disease seen in adults: bacteremia, meningitis, arthralgia, erythema nodosum

• Lab diagnosis: isolation of bacteria from feces on Mac conkey agar or on selective media using cold enrichment • Biochemical identification • GNB motile at 250 C, non motile at 370 C

Yersinia pseudotuberculosis – Pathogen of rodents, particularly guinea pigs – Septicemia with mesenteric lymphadenitis, similar to appendicitis – Motile at 220 C

• • PASTEURELLA MULTOCIDA Non motile, gram negative bacilli Oxidase positive Indole positive Does not grow on Mac. Conkey media Found in the respiratory tract of dogs, cats and cattle Human infections – rare Wound sepsis following animal bites, meningitis following head injury , pneumonia, etc Treated with tetracycline, streptomycin & penicillin

FRANCISELLA TULARENSIS • Causative agent of tularemia: infection of rodents originally described in Tulare county, California • Human infection by: Direct contact with infected rodents or tick bites or ingestion of contaminated food/ water or by aerosols • Minute, capsulated, GNB • Intracellular parasite: fastidious growth requirement: Francis blood dextrose cystine agar

• Human tularemia: local ulceration with lymphadenitis, a typhoid like fever with glandular enlargement • Respiratory disease: • Highly infectious disease • Diagnosis by culture or inoculation into guinea pigs • Abs detection • An attenuated vaccine is available: administered by scarification to individuals at high risk of infection
- Slides: 28