Year 4 Monash University Bendigo Regional Clinical School

Year 4 Monash University Bendigo Regional Clinical School

� Definition � Assessment � First Aid � Initial management � Long-term management � Non-accidental injury � Prevention of burn injuries

� Be able to assess the extent and thickness of a burn on a child (or an adult) � Know how to dress a burn and provide analgesia appropriately � Know the principles of fluid resuscitation after a burn injury And hopefully a whole lot more!
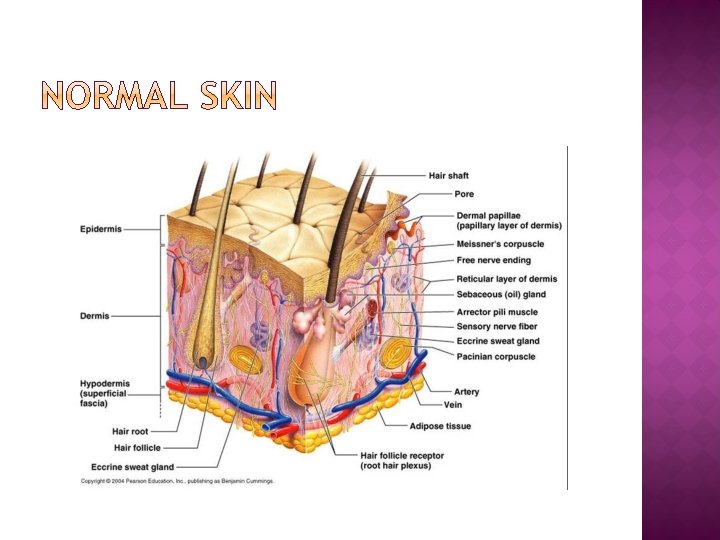

� Loss of Skin or Mucosa due to Thermal, Chemical or Mechanical injury. � May extend to a variable thickness within the skin or mucosa � May extend over a variable extent � May not be visible externally �e. g. Airway burns Oesophageal burns � Outcome at site of burn depends largely on depth of burn
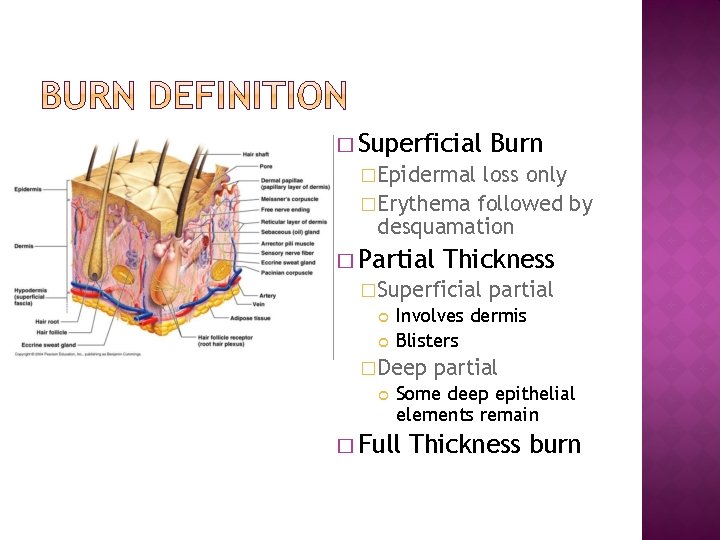
� Superficial Burn �Epidermal loss only �Erythema followed by desquamation � Partial Thickness �Superficial partial Involves dermis Blisters �Deep partial Some deep epithelial elements remain � Full Thickness burn
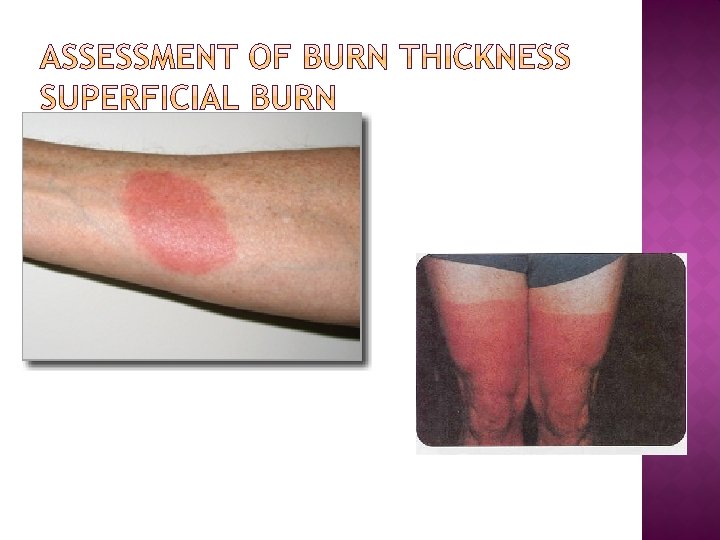
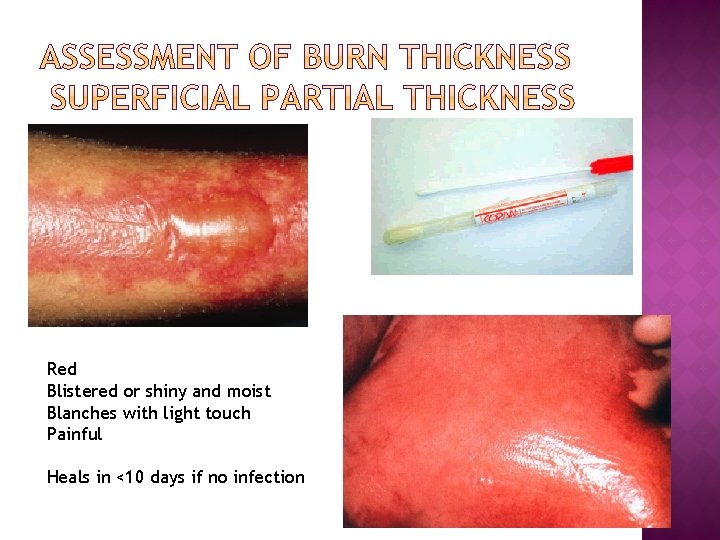
Red Blistered or shiny and moist Blanches with light touch Painful Heals in <10 days if no infection
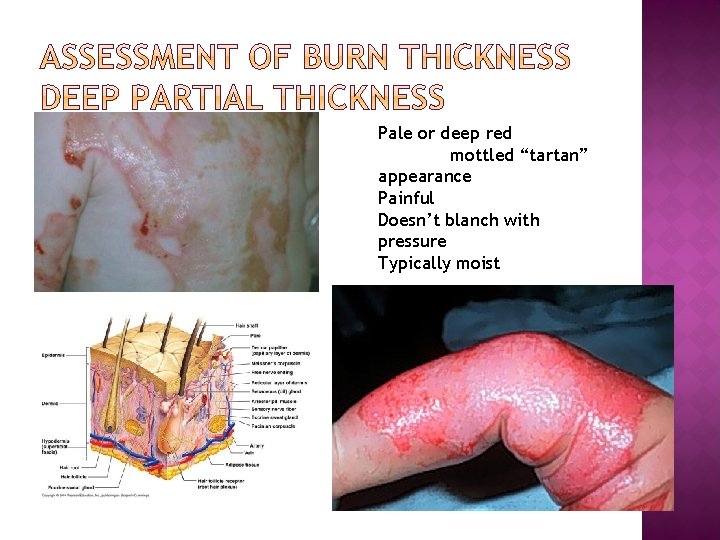
Pale or deep red mottled “tartan” appearance Painful Doesn’t blanch with pressure Typically moist
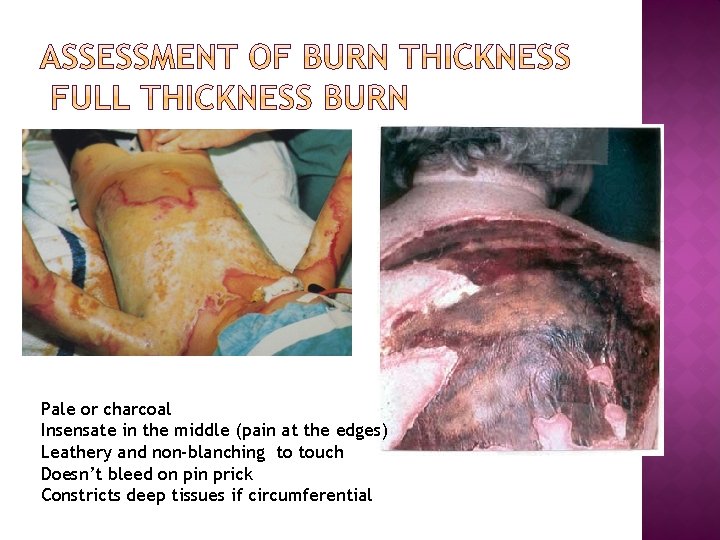
Pale or charcoal Insensate in the middle (pain at the edges) Leathery and non-blanching to touch Doesn’t bleed on pin prick Constricts deep tissues if circumferential
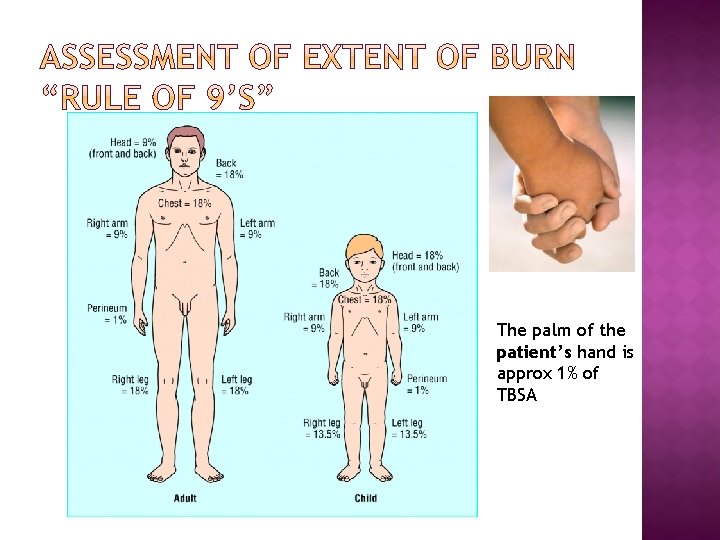
The palm of the patient’s hand is approx 1% of TBSA

� Remove the patient from the source of the burn � Remove hot, burnt, constrictive or contaminated clothing � Cool the burn (keeping the patient warm) � Cover the burn Clean, dry cloth �Glad wrap �


� ABC �Beware stridor in burns to face or chest � Assessment of thickness and extent of burns � ? Escharotomies � Continue First Aid, take “AMPLE” history � Debridement and Dressings � Analgesia � IV access and fluid resuscitation � Tetanus toxoid � Nutrition ? NG tube � ? Transfer to burns centre
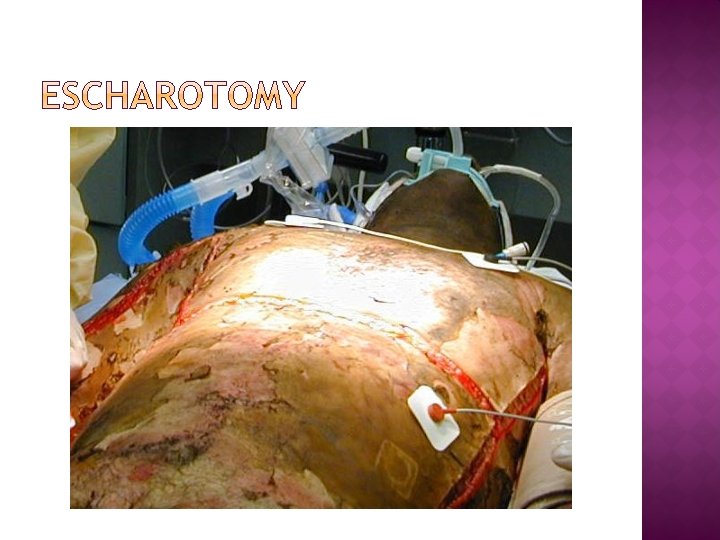
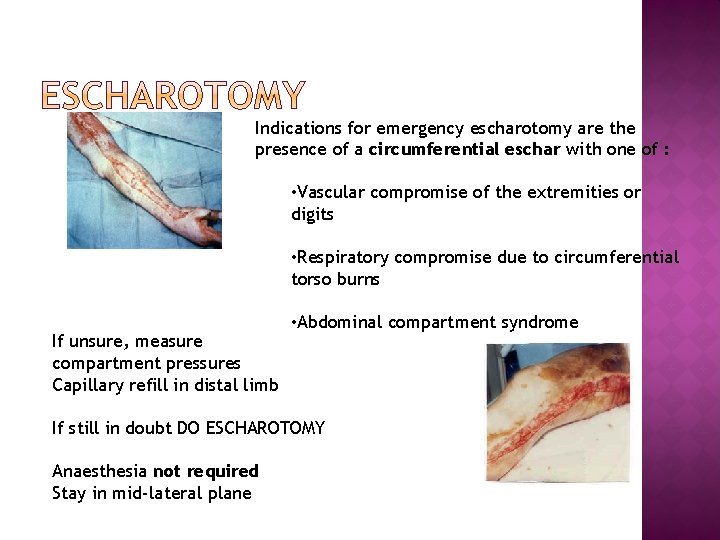
Indications for emergency escharotomy are the presence of a circumferential eschar with one of : • Vascular compromise of the extremities or digits • Respiratory compromise due to circumferential torso burns If unsure, measure compartment pressures Capillary refill in distal limb • Abdominal compartment syndrome If still in doubt DO ESCHAROTOMY Anaesthesia not required Stay in mid-lateral plane

� Principles �Minimize opportunities for bacterial contamination/growth and invasion (debridement) �Maintain a moist wound environment �Avoid substances which are toxic to tissues which are potentially viable (some historical dressings) �Enable re-evaluation as necessary �Be cost and time effective for both staff and patient

� Minimize opportunities for bacterial growth and invasion � Remove all loose dead devascularised skin at first presentation prior to dressing � Clean with Chlorhexidine to remove gross dirt � De-roof blisters when they are no longer tense � Surgically debride deep partial and fullthickness burns at the earliest convenient opportunity
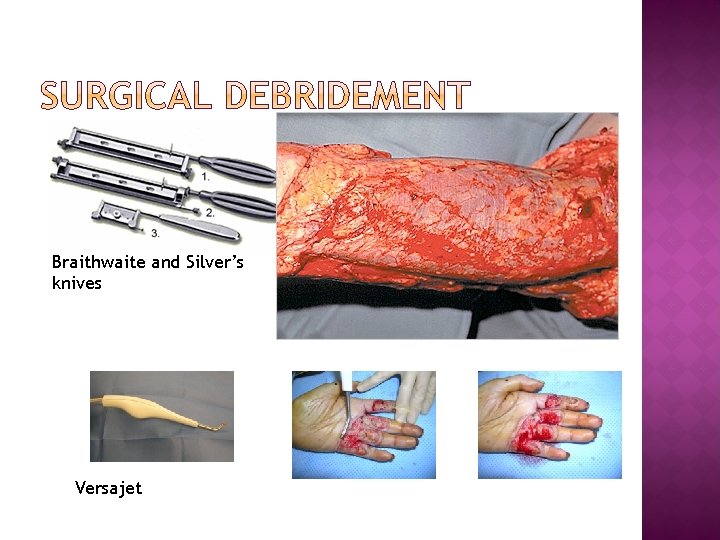
Braithwaite and Silver’s knives Versajet

� Creams, Solugel – A liquid hydrogel. Needs thorough washing off and reapplication 4 x per day. Used for face and perineum � Low Adherent dressings Mepital (silicone-based dressing) Uni-tulle/Bactigras � Silver Lotions and Gels Products Acticoat/Acticoat 7 (Needs activation by sterile water and cover with Intrasite conformable to maintain moisture) Aquacel Ag with intrasite/tegaderm over it (also needs to be moist) SSD Causes difficulty assessing burn depth and is toxic to the cornea. Appropriate for full-thickness burns (not on face) pending excision � Glad Wrap

� Scalds in children classically get deeper over the first 24 -48 hours. � Once depth is established then care plan can be developed � Assessment of burn depth requires experience and expertise � Photographs can be helpful in ED � When in doubt �Clean, dress simply, admit and review by surgical consultant in am �Call consultant surgeon to review

� Cool the burn (but not the patient) � Cover the burn (once it has been cleaned and loose skin debrided) � Distraction (play therapist/video games) � Analgesic ladder �Topical Lignocaine gel to aid gentle debridement �Oral Paracetamol +/- codeine or endone �Parenteral IV (Not IM or SC as absorption is unpredictable and risk under and overdose in the same patient)

� Try and avoid burnt tissue �Difficult to secure �Risk of tight bandages with burn swelling � Consider need for “different” routes �Saphenous vein cutdown �Intraosseous needle �Central lines

� � Various “formulas” Maintenance fluid 4 ml/kg/hour to 10 kg � 2 ml/kg/hr 10 -20 kg � 1 ml/kg/hr >20 kg � � Water and sugar and Na and K Replacement of Existing burn losses FROM THE TIME OF THE BURN � Approx 4 ml/kg/%burn/24 hrs (excluding 1 st degree burn) N. Saline or Hartmann’s solution � 50% of replacement given in first 8 hours post-burn, � Remainder over next 16 hours post burn � � Replacement of anticipated on-going burn losses � � Consider possibility of Inc K from burnt tissue Ongoing re-assessment of intravascular volume i. e. IDC and hourly urine measures aim for 1 ml/kg/hr minimum in children � Consider myoglobinuria from burnt muscle in deep burns or ischaemic muscle �

� Tetanus �Burns toxoid are tetanus prone wounds � Nutrition �Nutrition requirements increase according to the size of the burn �For burns >10% will need nutitional supplementation. Consider use of NGT � Maintaining � Role Blood Glucose Levels of Antibiotics �(there isn’t one unless…. . )

� Full-thickness (third-degree) burns over 5% BSA Partial-thickness (second-degree) burns over 10% BSA � Any full-thickness or partial-thickness burn involving critical areas (e. g. , face, hands, feet, genitals, perineum, skin over any major joint), as these have significant risk for functional and cosmetic problems � Circumferential burns of the thorax or extremities � Significant chemical injury, electrical burns, lightning injury, coexisting major trauma, or presence of significant preexisting medical conditions � Presence of inhalation injury

� Skin Grafting � Temporary skin substitutes � Skin culture � Scar management � Scar contractures and scar hypertrophy
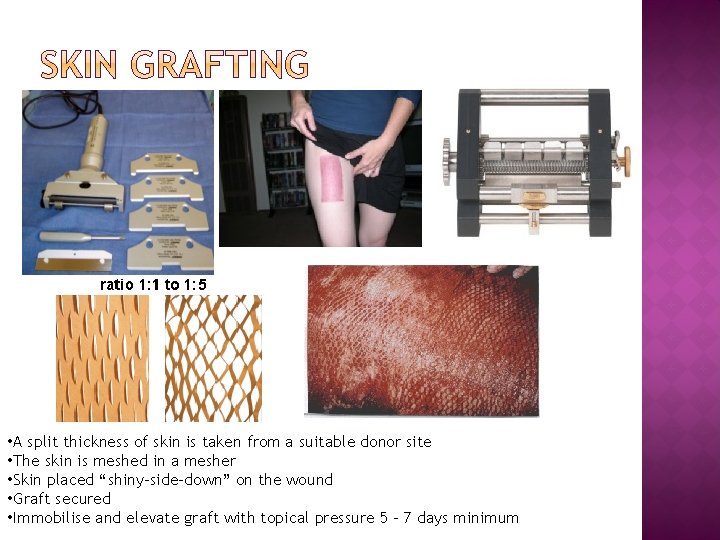
• A split thickness of skin is taken from a suitable donor site • The skin is meshed in a mesher • Skin placed “shiny-side-down” on the wound • Graft secured • Immobilise and elevate graft with topical pressure 5 – 7 days minimum

� “Classic” Cases �Cigarette burns �Perineal burns �Hot water in the bath �Burns with identifiable “brand” impression e. g. iron � Considerations �Implausible story that is inconsistent �Other signs of injuries of different ages �Other presentations with serious injury/ingestions/drowning etc

� Consider burn demographic � Home safety � Role of change in escalating risk for burn injury �Developmental �Seasonal �Location/Carers

� Electrical burns � Blast injury � Caustic ingestion � Carbon monoxide poisoning

� Burns largely preventable � Early action mitigates the severity of the outcome � Close follow-up and attention to detail is vital � Team care is important � If you don’t know ASK
- Slides: 33