www drsarma in Prediabetes Diagnosis and Management Prof

www. drsarma. in Prediabetes Diagnosis and Management Prof. Dr. Sarma VSN Rachakonda M. D. , M. Sc. , (Canada), FCGP, FIMSA, FRCP (Glasgow), FCCP (USA). , Senior Consultant Physician, Cardio-metabolic & Chest Specialist, Visiting Professor of Internal Medicine, SBMC, FLL, i. DRF, Chennai

The Outline of the Presentation Burden, Diagnostic criteria Who should be screened Significance Prediabetes Evidence from research studies Risk Scores - Application Primary prevention of T 2 DM
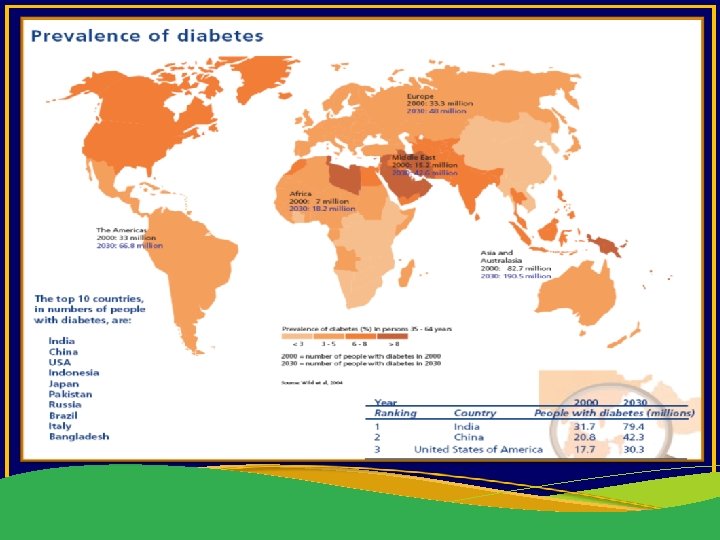

How Big is the Problem? 35% of adults over 20 years 50% of those over 65 years 79 million Americans in 2010 Double the number in India CDC. National Diabetes Fact Sheet: National estimates and general information on diabetes and Prediabetes in the United States, 2011.
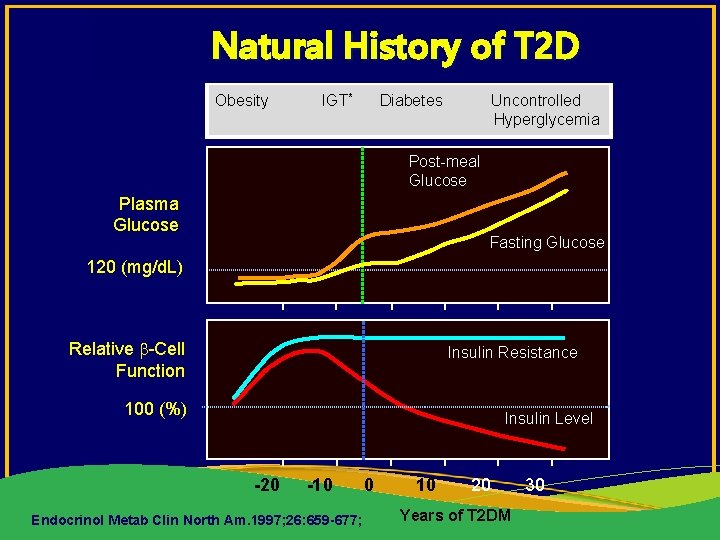
Natural History of T 2 D Obesity IGT* Diabetes Uncontrolled Hyperglycemia Post-meal Glucose Plasma Glucose Fasting Glucose 120 (mg/d. L) Relative -Cell Function Insulin Resistance 100 (%) Insulin Level -20 -10 Endocrinol Metab Clin North Am. 1997; 26: 659 -677; 0 10 20 Years of T 2 DM 30

ADA Diagnostic Criteria for Diabetes Clinical Practice Recommendations 2010 1. A 1 C ≥ 6. 5%. The test should be performed as per NGSP method and standardized to the DCCT assay. * 2. FPG ≥ 126 mg/dl. – No caloric intake for at least 8 h. * 3. 2 -h plasma glucose ≥ 200 mg/dl OGTT performed using 75 anhydrous glucose dissolved in water. * 4. Random plasma glucose ≥ 200 mg/dl + classic symptoms of hyperglycemia or hyperglycemic crisis. * In the absence of unequivocal hyperglycemia, criteria 1– 3 should be confirmed by repeat testing
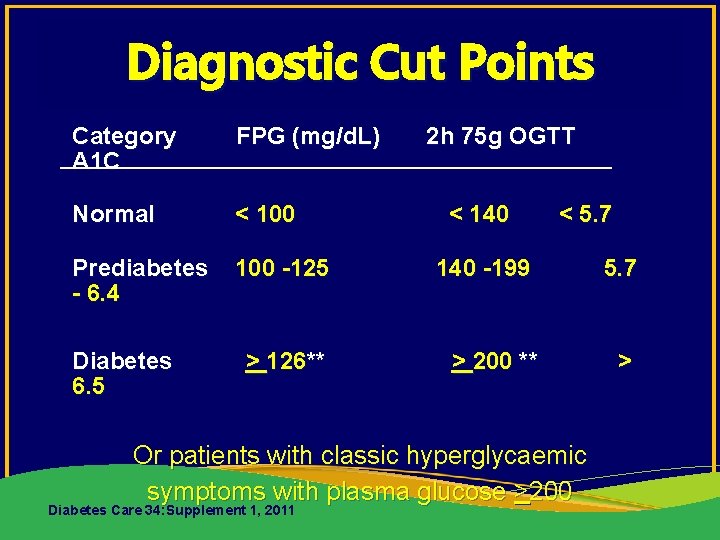
Diagnostic Cut Points Category A 1 C FPG (mg/d. L) Normal < 100 Prediabetes - 6. 4 100 -125 140 -199 5. 7 > 126** > 200 ** > Diabetes 6. 5 2 h 75 g OGTT < 140 < 5. 7 Or patients with classic hyperglycaemic symptoms with plasma glucose >200 Diabetes Care 34: Supplement 1, 2011

How is Prediabetes Diagnosed ? Categories of increased risk for diabetes Impaired Fasting Glucose [IFG] FPG of 100– 125 mg/dl Impaired Glucose Tolerance [IGT]: 2 -hour Plasma Glucose on the 75 -g Oral Glucose Tolerance Test 140– 199 mg/dl A 1 C 5. 7 – 6. 4% For all three tests, risk is continuous, extending below the lower limit of the range and becoming disproportionately greater at higher ends of the range.

Gestational Diabetes (GDM) Overnight fast 75 g OGTT • Fasting >92 mg/dl • 1 h post glucose >180 mg/dl • 2 h post glucose >153 mg/dl Any ONE abnormal value is adequate Diabetes Care 34: Supplement 1, 2011 Diabetes Care 2010; 33: 676– 682

Risk Factors for the Development of Prediabetes and Type 2 Diabetes • Age 45 or older • Overweight – BMI >25 • HT and/or on Rx for HT • Previous Prediabetes • Physical Inactivity • TG > 200, HDL < 35 • Asian or African ethnicity • Acanthosis Nigricans • Family H/o of Diabetes • Excess abdominal fat • PCOS, IR, Waist Circum • H/o GDM, CVD • Had macrosomic

Modifiable Risk Factors for T 2 DM • Obesity, Body fat distribution • Increased waist circumference • Physical inactivity • Elevated fasting and 2 hr glucose levels • Dyslipidemia and Hypertension • Smoking and Alcohol
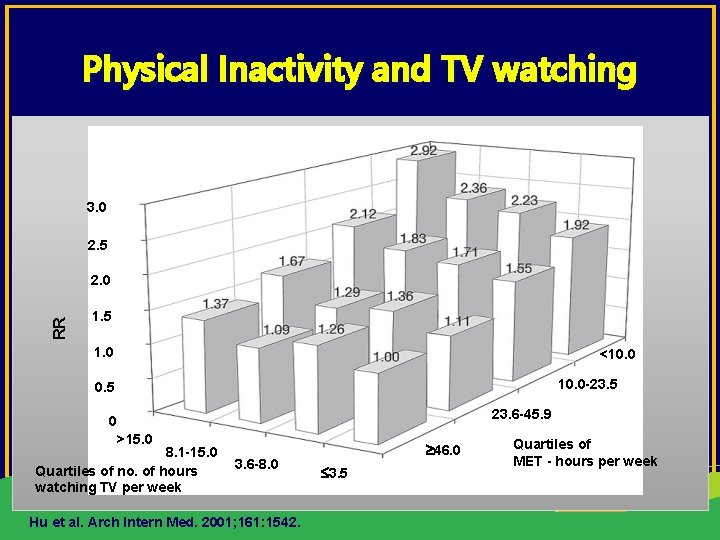
Physical Inactivity and TV watching 3. 0 2. 5 RR 2. 0 1. 5 1. 0 <10. 0 -23. 5 0. 5 23. 6 -45. 9 0 >15. 0 8. 1 -15. 0 Quartiles of no. of hours watching TV per week 3. 6 -8. 0 Hu et al. Arch Intern Med. 2001; 161: 1542. 46. 0 3. 5 Quartiles of MET - hours per week

Natural History of IGT 25% • IGT -after 10 years 25% • Normal 50% • T 2 DM
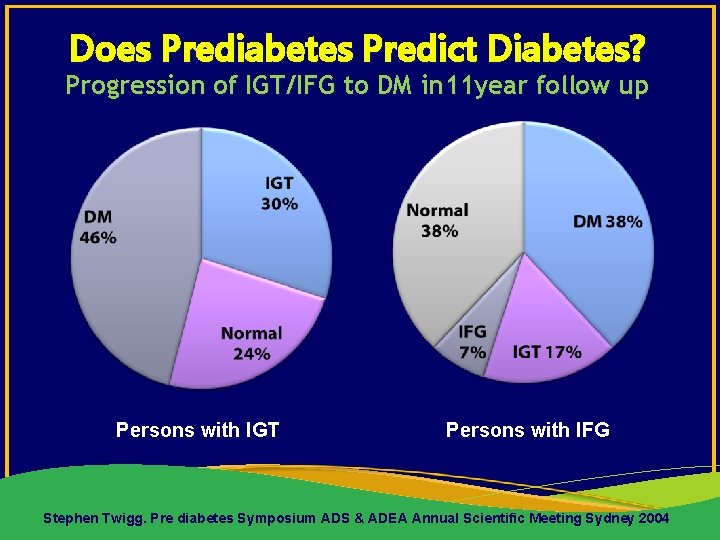
Does Prediabetes Predict Diabetes? Progression of IGT/IFG to DM in 11 year follow up Persons with IGT Persons with IFG Stephen Twigg. Pre diabetes Symposium ADS & ADEA Annual Scientific Meeting Sydney 2004
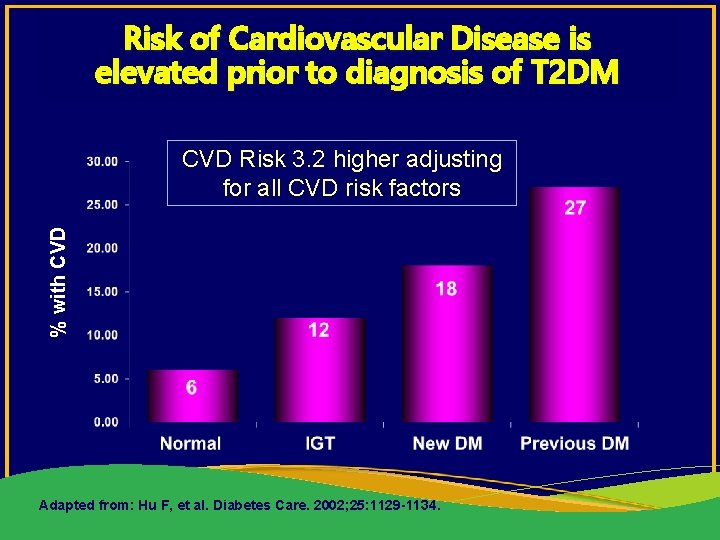
Risk of Cardiovascular Disease is elevated prior to diagnosis of T 2 DM % with CVD Risk 3. 2 higher adjusting for all CVD risk factors Adapted from: Hu F, et al. Diabetes Care. 2002; 25: 1129 -1134.
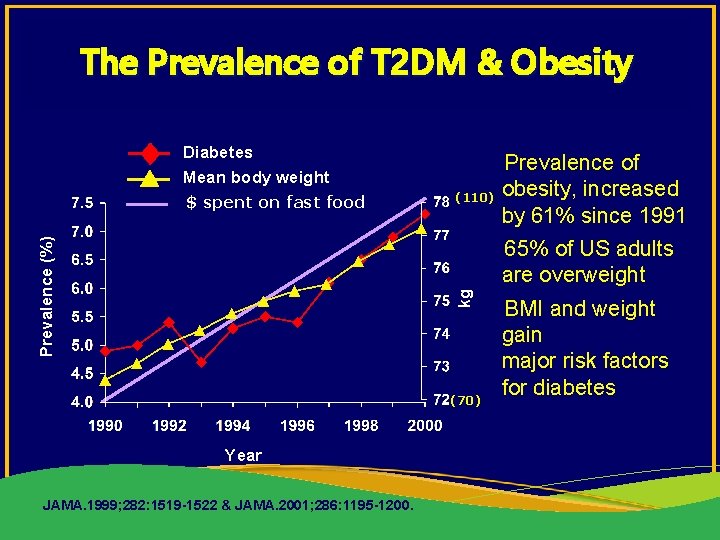
The Prevalence of T 2 DM & Obesity Diabetes Mean body weight $ spent on fast food (110) Prevalence of obesity, increased by 61% since 1991 kg Prevalence (%) 65% of US adults are overweight (70) Year JAMA. 1999; 282: 1519 -1522 & JAMA. 2001; 286: 1195 -1200. BMI and weight gain major risk factors for diabetes

What are the Health Risks Associated with Prediabetes? • Progression to diabetes: 11% of people with pre-diabetes develop T 2 DM each year (DPP) • Other studies: majority with Prediabetes develop T 2 DM in 10 years • Microvascular complications at onset of DM • 50% higher risk of CVD, CAD and Stroke

Feasibility of Preventing T 2 DM • There is a long period of glucose intolerance that precedes the development of diabetes • Screening tests can identify persons at high risk • Predicts high risk for development of diabetes • Predicts high risk for development of atherosclerotic vascular disease • There are safe, potentially effective interventions that can prevent the above modifiable risk factors such as lifestyle and pharmacologic interventions
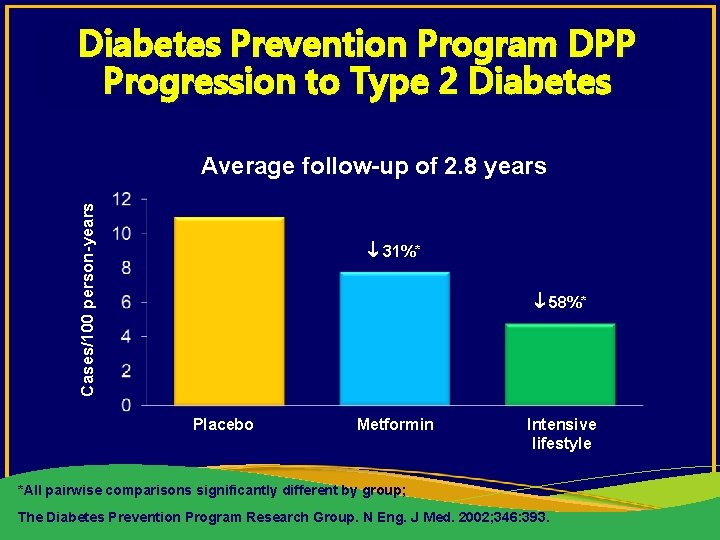
Diabetes Prevention Program DPP Progression to Type 2 Diabetes Cases/100 person-years Average follow-up of 2. 8 years 31%* 58%* Placebo Metformin Intensive lifestyle *All pairwise comparisons significantly different by group; The Diabetes Prevention Program Research Group. N Eng. J Med. 2002; 346: 393.
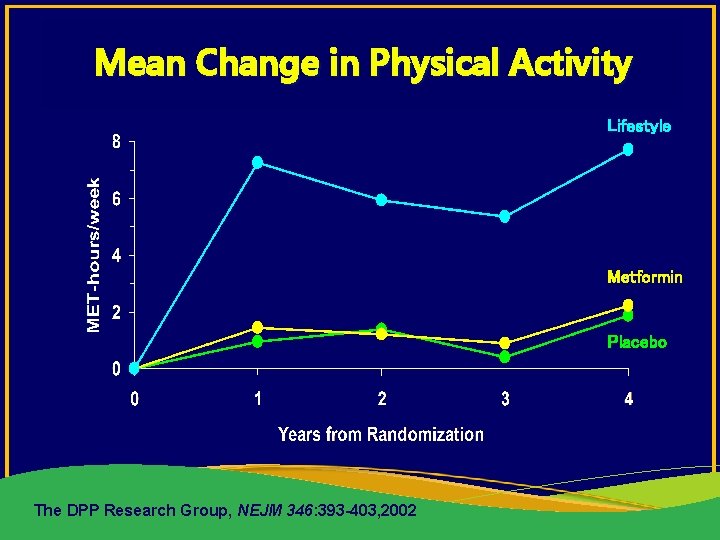
Mean Change in Physical Activity Lifestyle Metformin Placebo The DPP Research Group, NEJM 346: 393 -403, 2002
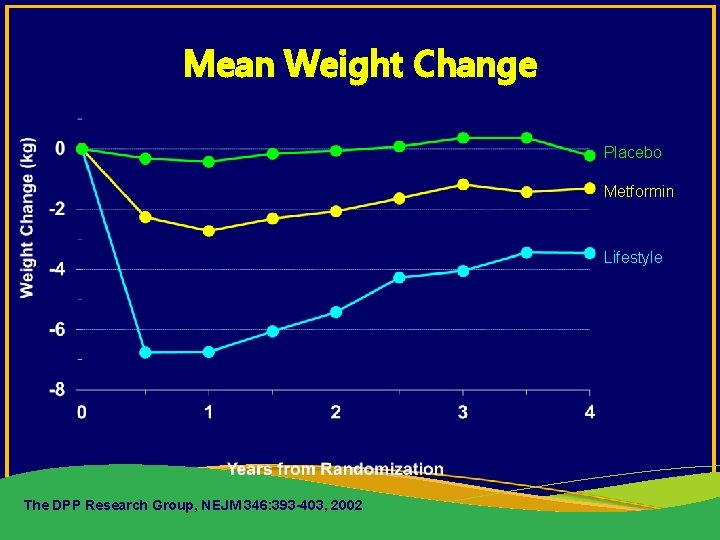
Mean Weight Change Placebo Metformin Lifestyle The DPP Research Group, NEJM 346: 393 -403, 2002
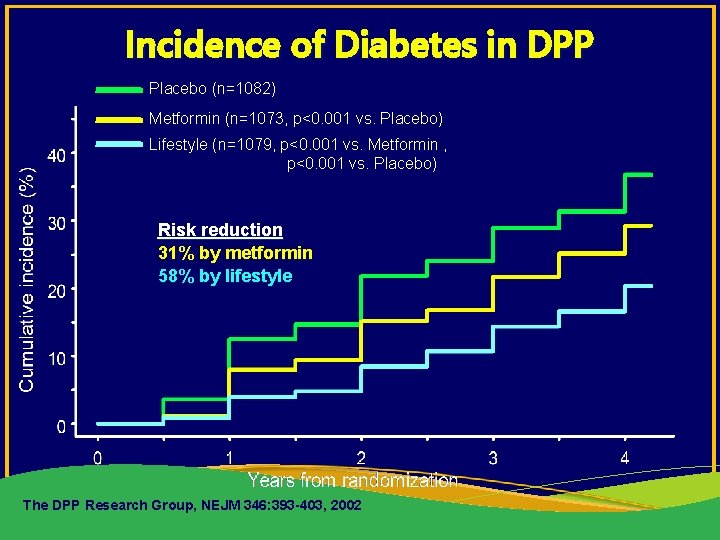
Incidence of Diabetes in DPP Placebo (n=1082) Metformin (n=1073, p<0. 001 vs. Placebo) Lifestyle (n=1079, p<0. 001 vs. Metformin , p<0. 001 vs. Placebo) Risk reduction 31% by metformin 58% by lifestyle The DPP Research Group, NEJM 346: 393 -403, 2002
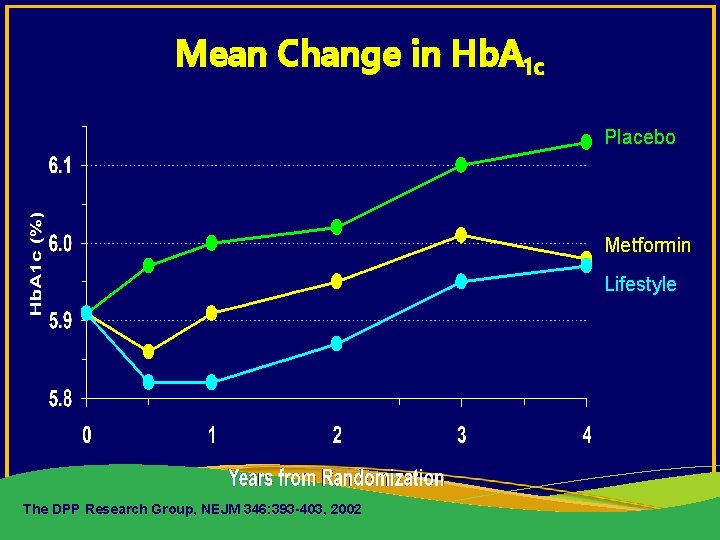
Mean Change in Hb. A 1 c Placebo Metformin Lifestyle The DPP Research Group, NEJM 346: 393 -403, 2002

A Decade Later…. DPPOS The Lancet, Oct 2009 • At end of DPP: participants 16 -session program of intensive TLC Parameter Placebo Metformin 850 mg bid TLC: MNT, PA Weight Loss <2 lbs 5 lbs 11% 7. 8% 4. 8% Diabetes at 2. 8 yrs Diabetes at 10 yrs 5 -6% Percent reduction - 18 34 Delay in diabetes - 2 yrs 4 yrs • Lifestyle group: 34% reduction in diabetes risk maintained • More favorable CV risk factors: BP and TG’s, despite fewer drugs • Benefits more pronounced in elderly: 50% reduction in age >60

The Finnish Diabetes Prevention Study Lifestyle Modifications • 522 overweight individuals with IGT randomized to – Control: diet instruction at the onset of study – Individualized advice given 7 times in the first year and every 3 months thereafter with goals of » Weight loss 5% » Reducing fat intake to <30% of energy consumption » Increasing fiber intake to 15 g/1000 kcal » Exercising at a moderate level for 30 min/d • Primary end point: Prevention of diabetes, assessed by OGTT Tuomilehto et al. N Engl J Med. 2001; 344: 1343.
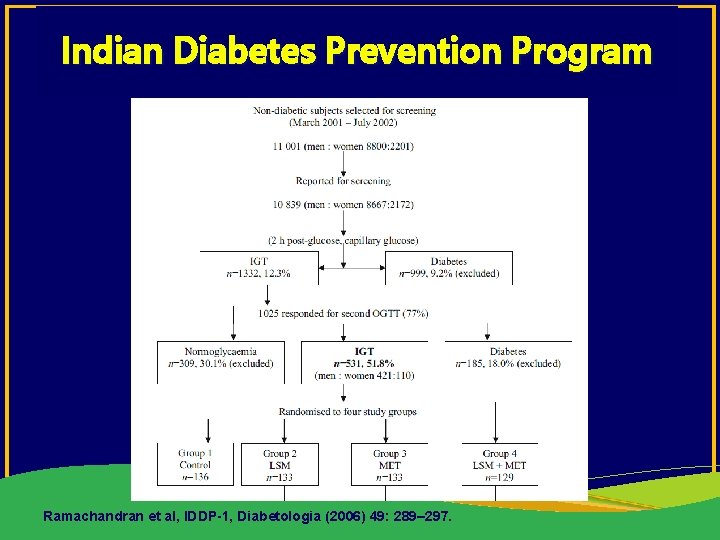
Indian Diabetes Prevention Program Ramachandran et al, IDDP-1, Diabetologia (2006) 49: 289– 297.
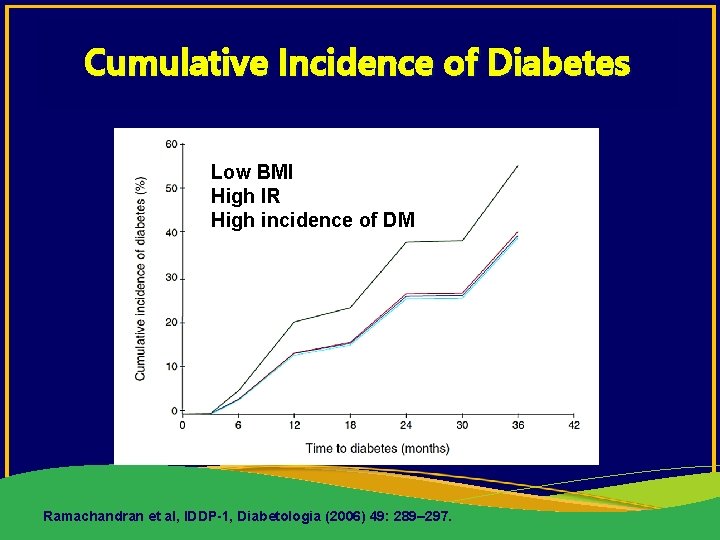
Cumulative Incidence of Diabetes Low BMI High IR High incidence of DM Ramachandran et al, IDDP-1, Diabetologia (2006) 49: 289– 297.
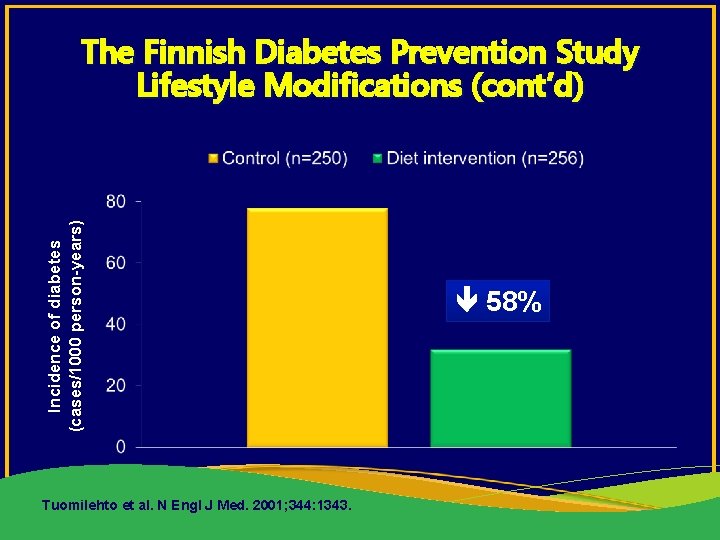
Incidence of diabetes (cases/1000 person-years) The Finnish Diabetes Prevention Study Lifestyle Modifications (cont’d) Tuomilehto et al. N Engl J Med. 2001; 344: 1343. 58%
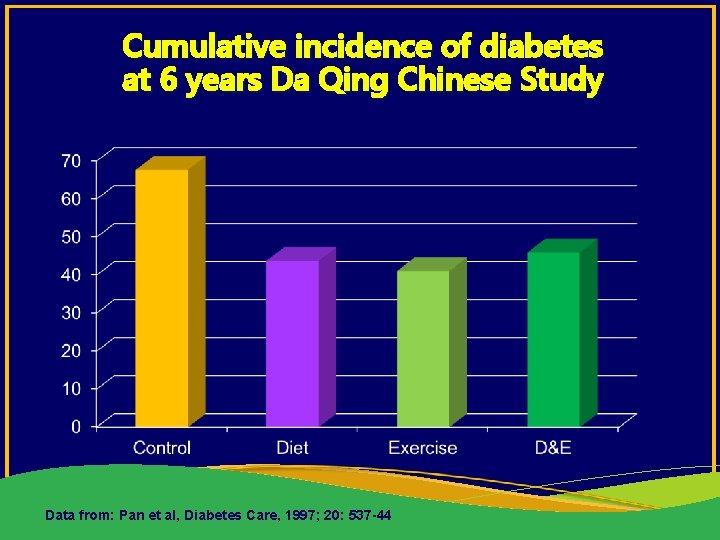
Cumulative incidence of diabetes at 6 years Da Qing Chinese Study Data from: Pan et al, Diabetes Care, 1997; 20: 537 -44

NAVIGATOR Study Effect of Nateglinide & Valsartan on Incidence of T 2 DM and CV Events - 9306 persons with IGT, CVD or CV risk followed for 5 years • Nateglinide: A postprandial glucose-lowering approach; incidence of diabetes 36% vs. 34%; composite CV outcome 14. 2% vs. 15. 2%; increased the risk of hypoglycemia • Valsartan: incidence of diabetes 33. 1% vs. 36. 8% (RR 14%); 38 fewer cases per 1000 pts treated for 5 years; no reduction in rate of CV events NEJM online, March 14, 2010

Prevention Studies in People with IGT Downstream strategies • Lifestyle interventions – Da Qing : Diet and Exercise – Malmo study : Diet and exercise – Finish Diabetes Prevention Study Lifestyle – DPP (Diabetes Prevention Study) Lifestyle, MF (Glitazone) • Lifestyle interventions with pharmacological agents – FHS (Fasting Hyperglycaemia Study) Healthy Living & SU – EDIT (Early Diabetes Intervention Study): Acarbose and MF – STOP NIDDM : Acarbose

How to Ascertain the Risk ? • Low Risk - 3 to 9 points • Maintain healthy wt. • High Risk 10+ points • Regular exercise • High risk for diabetes • Keep it up regularly • Medical evaluation • Take steps to improve score
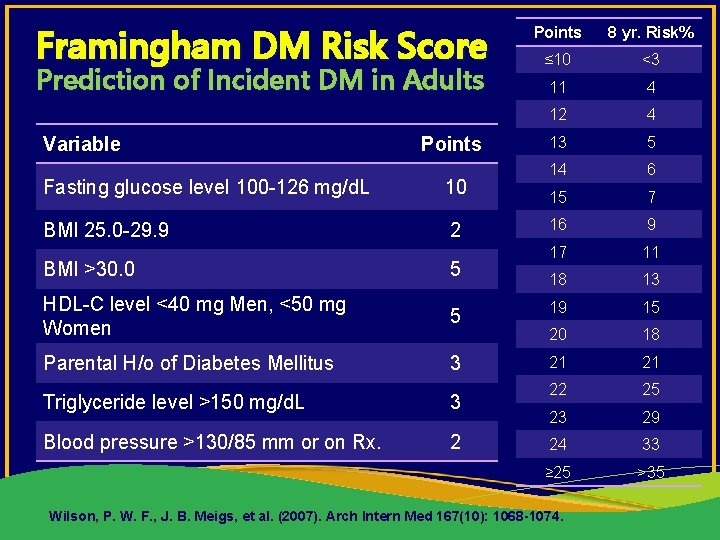
Framingham DM Risk Score Prediction of Incident DM in Adults Variable Points Fasting glucose level 100 -126 mg/d. L 10 BMI 25. 0 -29. 9 2 Points 8 yr. Risk% ≤ 10 <3 11 4 12 4 13 5 14 6 15 7 16 9 17 11 18 13 BMI >30. 0 5 HDL-C level <40 mg Men, <50 mg Women 5 19 15 20 18 Parental H/o of Diabetes Mellitus 3 21 21 22 25 23 29 24 33 ≥ 25 >35 Triglyceride level >150 mg/d. L 3 Blood pressure >130/85 mm or on Rx. 2 Wilson, P. W. F. , J. B. Meigs, et al. (2007). Arch Intern Med 167(10): 1068 -1074.
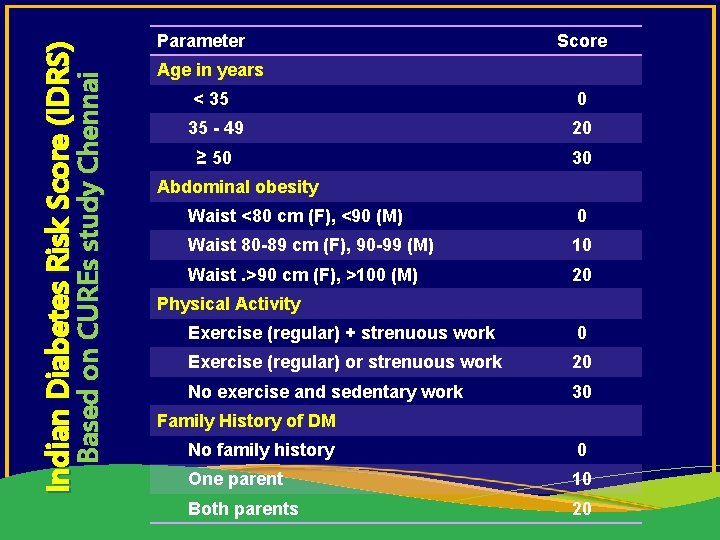
Based on CUREs study Chennai Indian Diabetes Risk Score (IDRS) Parameter Score Age in years < 35 0 35 - 49 20 ≥ 50 30 Abdominal obesity Waist <80 cm (F), <90 (M) 0 Waist 80 -89 cm (F), 90 -99 (M) 10 Waist. >90 cm (F), >100 (M) 20 Physical Activity Exercise (regular) + strenuous work 0 Exercise (regular) or strenuous work 20 No exercise and sedentary work 30 Family History of DM No family history 0 One parent 10 Both parents 20
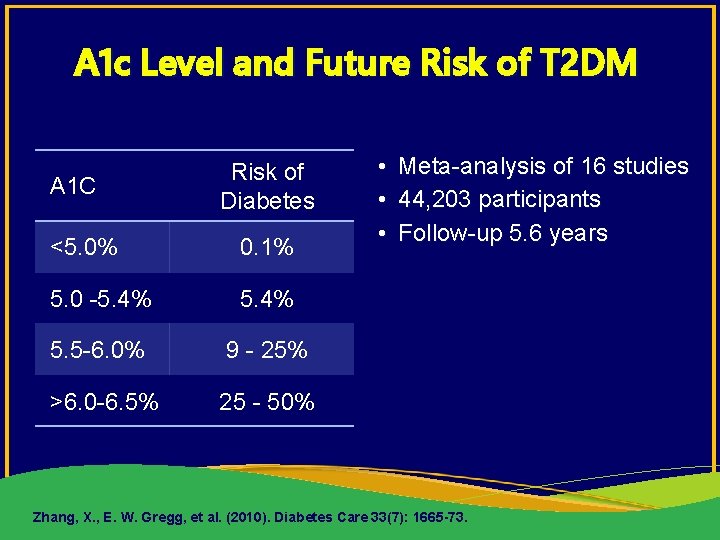
A 1 c Level and Future Risk of T 2 DM A 1 C Risk of Diabetes <5. 0% 0. 1% 5. 0 -5. 4% 5. 5 -6. 0% 9 - 25% >6. 0 -6. 5% 25 - 50% • • • Meta-analysis of 16 studies 44, 203 participants Follow-up 5. 6 years Zhang, X. , E. W. Gregg, et al. (2010). Diabetes Care 33(7): 1665 -73.
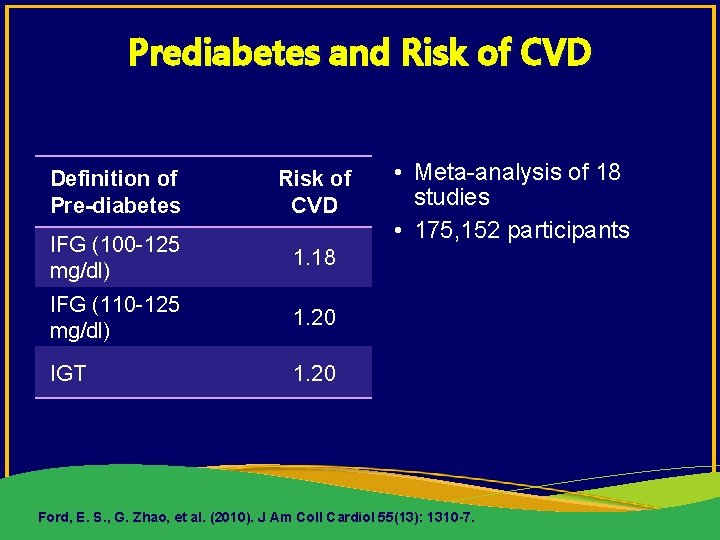
Prediabetes and Risk of CVD Definition of Pre-diabetes Risk of CVD IFG (100 -125 mg/dl) 1. 18 IFG (110 -125 mg/dl) 1. 20 IGT 1. 20 • Meta-analysis of 18 studies • 175, 152 participants Ford, E. S. , G. Zhao, et al. (2010). J Am Coll Cardiol 55(13): 1310 -7.

ADA Consensus Statement Preventive treatment in high risk individuals with Prediabetes • In addition to lifestyle modification, the following individuals should be considered for treatment with metformin: – those who have both IFG and IGT, and – at least one additional risk factor (age < 60, BMI ≥ 35, F H/o of diabetes, TGs, HDL, or A 1 C > 6% Diabetes Care 2007

Prevention of Diabetes Recommendations to reduce risk of type 2 diabetes – Regular physical activity – Interventions to reduce obesity » Waist circumference, » body weight and body mass index (BMI) » identify individuals for weight management program – Individuals at risk should have dietary intake assessed and receive individualised dietary advice and continued diet advice Evidence Based Guideline for the Prevention of Type 2 Diabetes. Australian Government NHMRC www. diabetesaustralia. com. au

Prevention of Diabetes Recommendations to reduce risk of type 2 diabetes – Identification of women with GDM would allow: » Postnatal clinical interventions in those with diabetes » Option to use preventive methods to the risk of DM – Diet and exercise education in children should include » Parental involvement » Behavioral techniques Evidence Based Guideline for the Prevention of Type 2 Diabetes. Australian Government NHMRC www. diabetesaustralia. com. au

Prescription pad

Thank you all
- Slides: 41