Wuchereria bancrofti and Brugia malayi are filarial nematodes

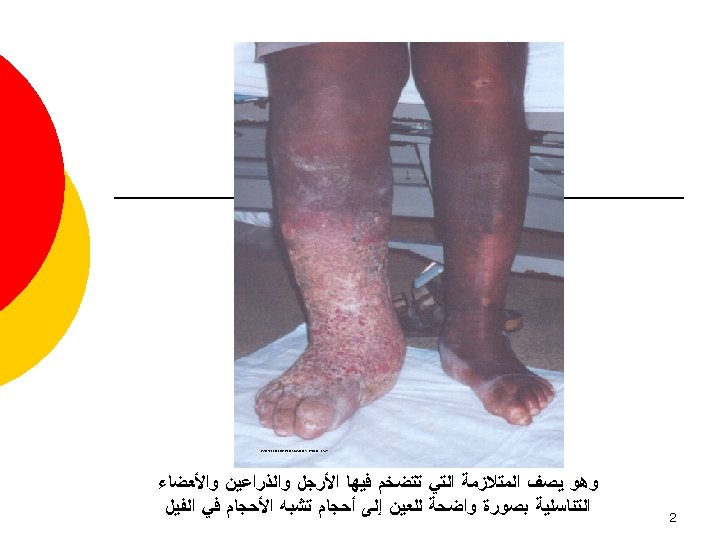

¡ Wuchereria bancrofti and Brugia malayi are filarial nematodes ¡ Spread by several species of night feeding mosquitoes ¡ Causes lymphatic filariasis, also known as Elephantiasis l Commonly and incorrectly referred to as “Elephantitis” 4

ﺍﻟﻌﺎﺋﻞ ﺍﻟﻨﻬﺎﺋﻲ ¡ Humans are the definitive host for the worms that cause lymphatic filariasis 5

Anopheles ﺍﻟﻌﺎﺋﻞ ﺍﻟﻤﺘﻮﺳﻂ ¡ Transmitted by Culex, Aedes, and Anopheles species ¡ B. malayi is transmitted by Anopheles and Mansonia species. Aedes Culex Mansonia 6

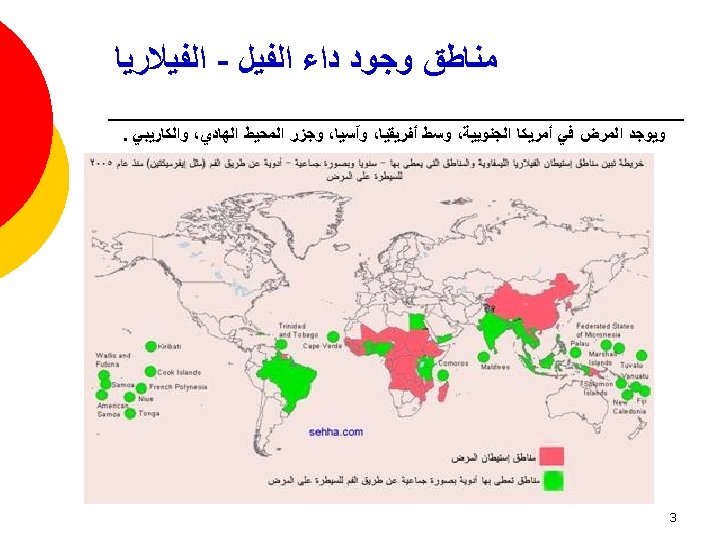
¡ Endemic in 83 countries ¡ 1. 2 billion at risk ¡ More than 120 million people infected ¡ More than 25 million men suffer from genital symptoms ¡ More than 15 million people suffer from lymphoedema or elephantiasis of the leg 7

¡ Adult: White and thread-like. Two rings of small papillae on the head. v Female: 5~10 cm in length v Male: 2. 5~4 cm and a curved tail with two copulatory spicules. para-lab by l. wafa menawi 8
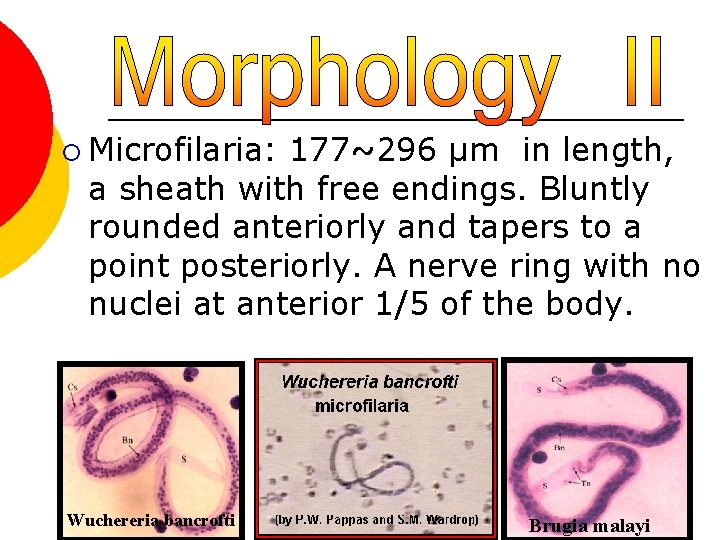
¡ Microfilaria: 177~296 µm in length, a sheath with free endings. Bluntly rounded anteriorly and tapers to a point posteriorly. A nerve ring with no nuclei at anterior 1/5 of the body. Wuchereria bancrofti para-lab by l. wafa menawi Brugia malayi 9

¡ Host: Mosqutoes (intermediate host) Human (final host) ¡ Location: Lymphatics and lymph nodes ¡ Infective stage: Infective larvae ¡ Transmission stage: Microfilariae ¡ Diagnostic stage: Microfilariae 10
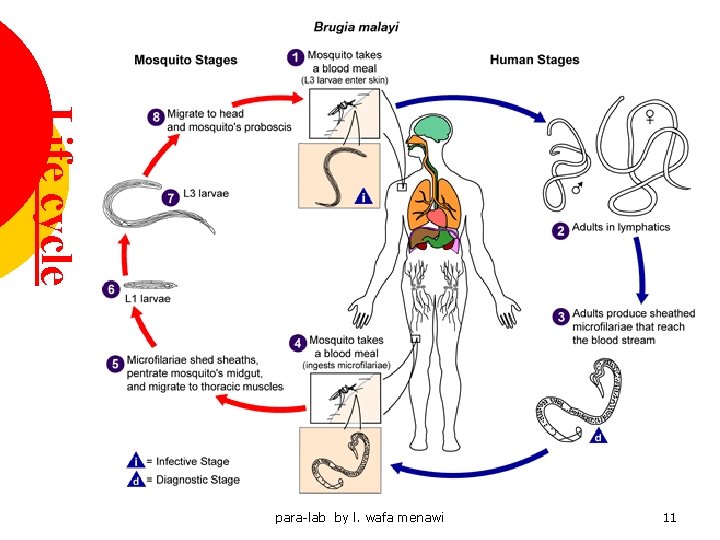
Life cycle para-lab by l. wafa menawi 11
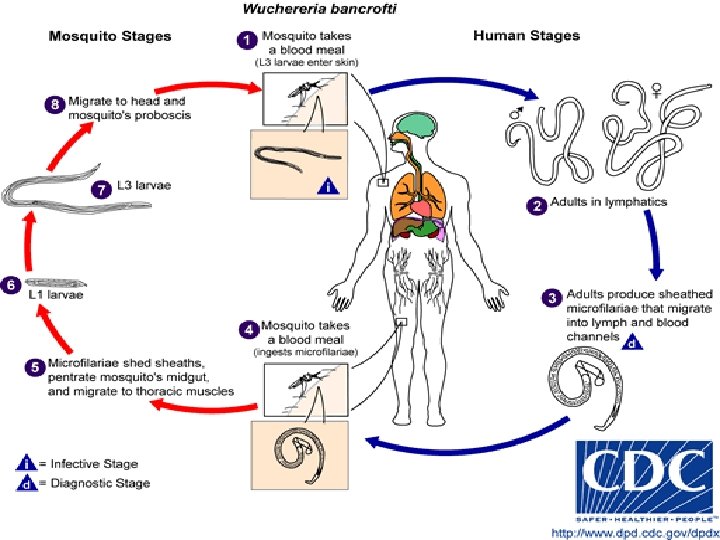
Wuchereria Life Cycle para-lab by l. wafa menawi 12



Phenomen which the number of microfilariae in peripherial blood is very low density during daytime, but increase from evening to midnight and reach the greatest density at 10 p. m to 2 a. m. May be related to cerebral activity and vasoactivity of pulmonary vessels. 15

• Larva deposited by mosquito bite • Travel through dermis to lymphatic vessels • Growth (approx 9 months) to mature worms(20 -100 mm long) • Worms live 5 -7 years (occasionally up to 15 years) • Mate->Microfilariae (1 st stage larva) • Females->release up to 10, 000 microfilariae/day into bloodstream • Microfilarie taken up by mosquito bite • Develop into 2 nd and 3 rd stage larva over 10 -14 days inside mosquito vector para-lab by l. wafa menawi 16
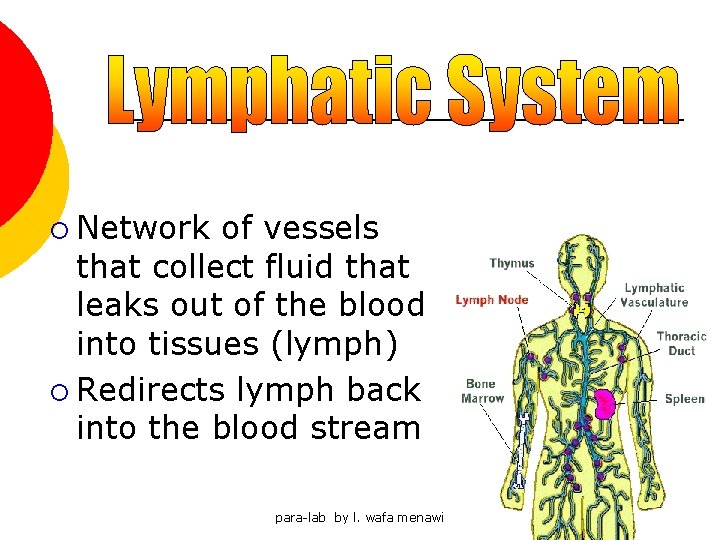
¡ Network of vessels that collect fluid that leaks out of the blood into tissues (lymph) ¡ Redirects lymph back into the blood stream para-lab by l. wafa menawi 17

• Initially asymptomatic • Symptoms develop with increasing numbers of worms • Less than 1/3 of infected individuals have acute symptoms • Clinical Course is 3 phases: • Asymptomatic Microfilaremia • Acute Adenolymphangitis (ADL) • Chronic/Irreversible lymphedema • Superimposed upon repeated episodes of ADL para-lab by l. wafa menawi 18

• Presents with sudden onset of fever and painful lymphadenopathy • Retrograde Lymphangitis • Inflammation spreads distally away from lymph node group • Immune mediated response to dying worms • Most common areas: Inguinal nodes and Lower extremities para-lab by l. wafa menawi 19

o o o o Inflammation spontaneously resolve after 4 -7 days but can recur frequently Recurrences usually 1 -4 times/year with increasing severity of lymphedema Secondary bacterial infections in edematous(elephantatic) areas Filarial fever (fever w/o lymphangitis) Tropical Pulmonary Eosinophilia Hyperresponsiveness to microfilariae trapped in lungs Nocturnal Wheezing para-lab by l. wafa menawi 20

o Lymphedema o Mostly LE and inguinal, but can affect UE and breast Initially pitting edema, with gradual hardening of tissues hyperpigmentation & hyperkeratosis Genitalia Hydroceles o o para-lab by l. wafa menawi 21

o Renal involvement Chyluria lymph discharge into urine o Loss of fat and protein hypoproteinemia & anemia o Hematuria, proteinuria from ? immune complex nephritis o o Secondary bacterial/fungal infections para-lab by l. wafa menawi 22
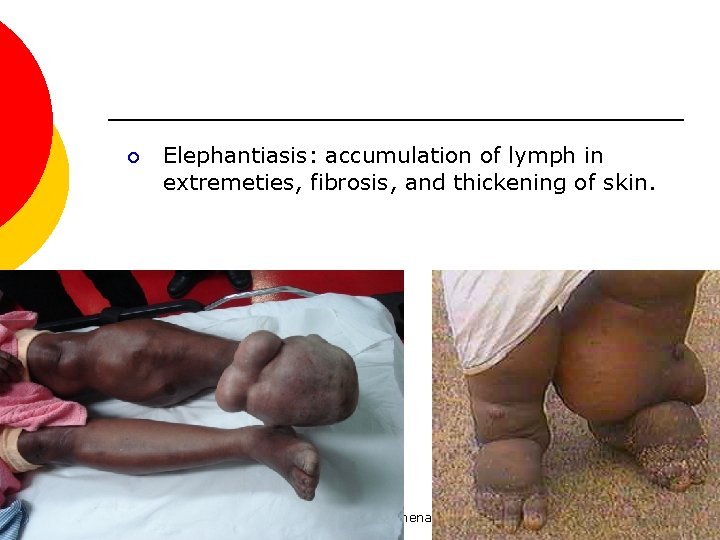
¡ Elephantiasis: accumulation of lymph in extremeties, fibrosis, and thickening of skin. para-lab by l. wafa menawi 23
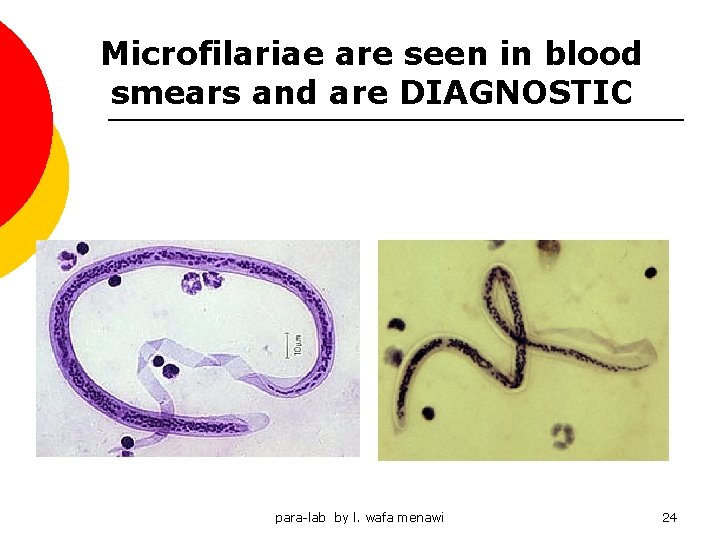
Microfilariae are seen in blood smears and are DIAGNOSTIC para-lab by l. wafa menawi 24
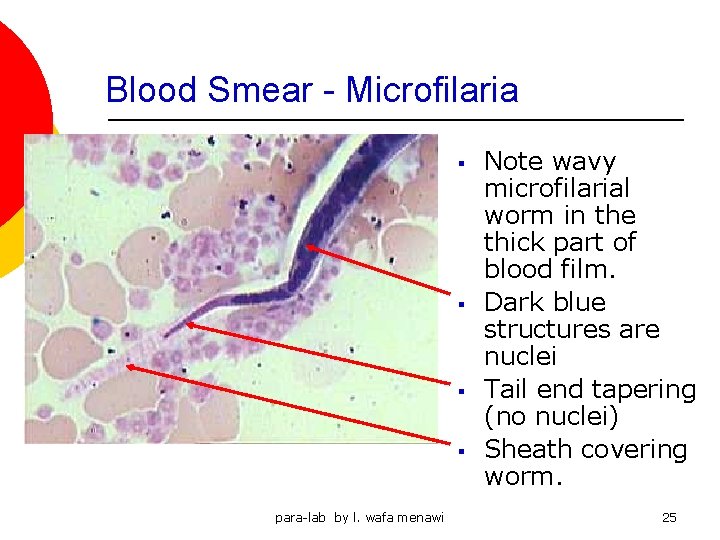
Blood Smear - Microfilaria § § para-lab by l. wafa menawi Note wavy microfilarial worm in the thick part of blood film. Dark blue structures are nuclei Tail end tapering (no nuclei) Sheath covering worm. 25
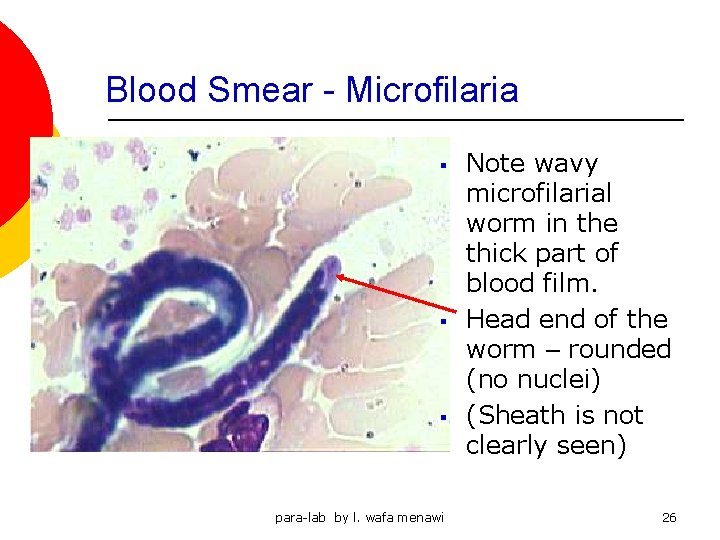
Blood Smear - Microfilaria § § § para-lab by l. wafa menawi Note wavy microfilarial worm in the thick part of blood film. Head end of the worm – rounded (no nuclei) (Sheath is not clearly seen) 26
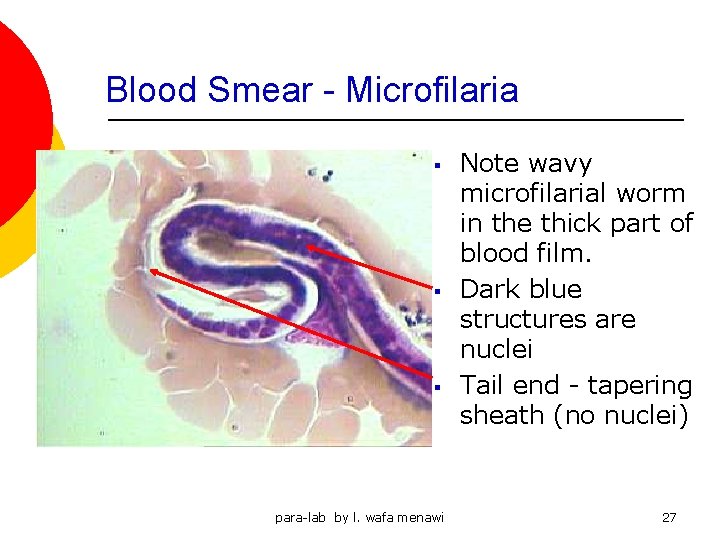
Blood Smear - Microfilaria § § § para-lab by l. wafa menawi Note wavy microfilarial worm in the thick part of blood film. Dark blue structures are nuclei Tail end - tapering sheath (no nuclei) 27
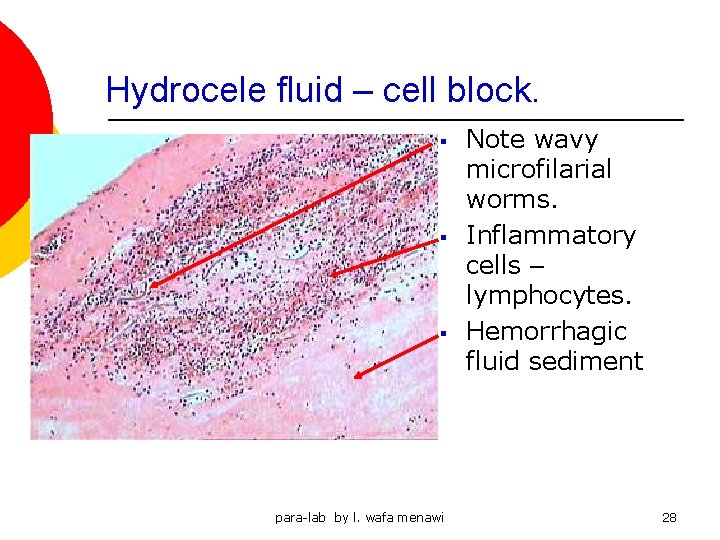
Hydrocele fluid – cell block. § § § para-lab by l. wafa menawi Note wavy microfilarial worms. Inflammatory cells – lymphocytes. Hemorrhagic fluid sediment 28
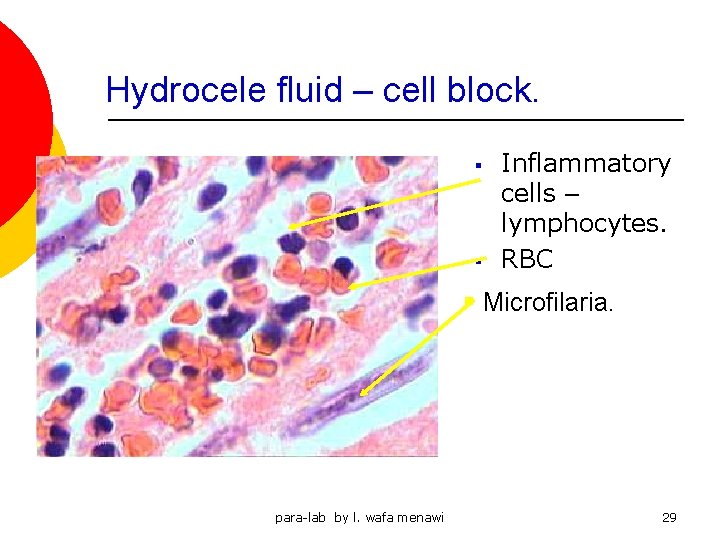
Hydrocele fluid – cell block. § § Inflammatory cells – lymphocytes. RBC § Microfilaria. para-lab by l. wafa menawi 29

¡ As with malaria, the most effective method of controlling the spread of W. bancrofti and B. malayi is to avoid mosquito bites ¡ The CDC recommends that anyone in at-risk areas: ¡Sleep under a bed net ¡Wear long sleeves and trousers ¡Wear insect repellent on exposed skin, especially at night 30

¡ Covering water-storage containers and improving waste-water and solid -waste treatment systems can help by reducing the amount of standing water in which mosquitoes can lay eggs. ¡ Killing eggs (oviciding) and killing or disrupting larva (larviciding) in bodies of stagnant water can further reduce mosquito populations. 31

¡ Treatment of filariasis involves two components: ¡ Getting rid of the microfilariae in people's blood ¡ Maintaining careful hygiene in infected persons to reduce the incidence and severity of secondary (e. g. , bacterial) infections. 32

AL mareed A. A Ph. D student at KSU 33
- Slides: 33