WOUND HEALING INFLAMMATION OVERCOMES THE INJURY REPAIR BRINGS

WOUND HEALING INFLAMMATION OVERCOMES THE INJURY REPAIR BRINGS HEALING WOUND HEALING INVOLVES 1. PARENCHYMAL CELL REGENERATION WHERE POSSIBLE 2. MIGRATION AND PROLIFERATION OF BOTH PARENCHYMAL AND CONNECTIVE TISSUE CELLS 3. SYNTHESIS OF ECM PROTEINS

WOUND HEALING 4. REMODELLING OF PARENCHYMAL ELEMENTS TORESTORE TISSUE FUNCTION 5. REMODELLING OF CONNECTIVE TISSUE TO ACHIEVE WOUND STRENGTH

WOUND HEALING TWO TYPES OF WOUND HEALING 1. REGENERATION-DEAD CELLS REPLACED BY NEW NORMAL CELLS 2. REPAIR BY CONNECTIVE TISSUE (FIBROSIS)

REGENERATION ABILITY TO REGENERATE IS INVERSELY CORRELATED WITH THE DEGREE OF DIFFERENTIATION LABILE CELLS --CONTINUOUSELY DYING AND CONTINUOUSELY DIVIDING CELL. REGENERATION OCCURS FROM POPULATION OF STEM CELL SWITH UNLIMITED CAPACITY TO PROLIFERATE LABILE CELLS INCLUDE-SURFACE EPITHELIA, HAEMOPOIETIC CELLS, EPITHELIA LINING THE DUCTS OF EXOCRINE GLANDS, EPITHELIA OF GIT, UTERUS, FALLOPIAN TUBES, URINARY BLADDER EPITHELIUM.

REGENERATION STABLE CELLS HAVE LOW LEVEL OF REPLICATIVE CAPACITY BUT CAPABLE OF RAPID DIVISION IN RESPONSE TO INJURY STABLE CELLS INCLUDE PARENCHYMA OF SOLID GLANDULAR TISSUE LIKE LIVER, KIDNEY, PANCREAS, ENDOTHELIAL LINING OF VESSELS, FIBROBLASTS, SMOOTH MUSCLE CELLS

REGENERATION 3. PERMANENT CELLSARE TERMINALLY DIFFERENTIATED AND NONPROLIFERATIVE IN POSTNATAL LIFE. CARDIAC NUSCLE CELLS, SKELETAL MUSCLE CELLS
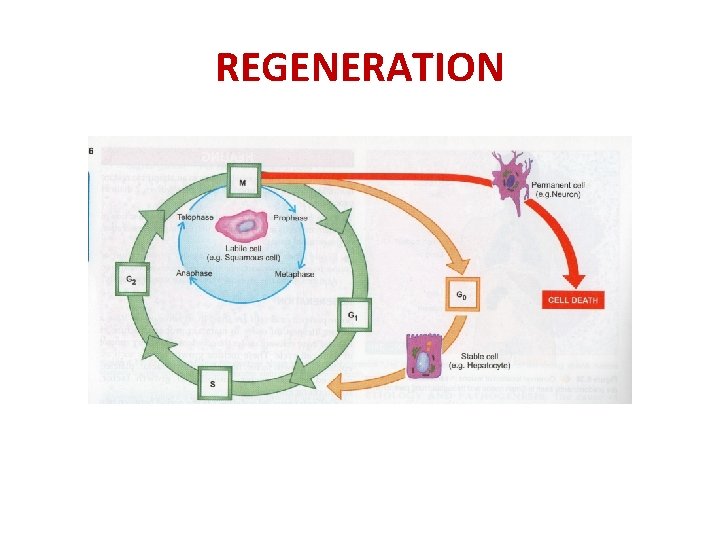
REGENERATION
REPAIR BY CONNECTIVE TISSUE ( SCAR FORMATION) 1. HEALING BY FIRST INTENTION 2. HEALING BY SECOND INTENTION

HEALING BY FIRST INTENTION -PRIMARY UNION OCCURS IN CLEAN, UNINFECTED SURGICAL INCISION SEQUENCE OF EVENTS 1. EPITHELIA REGENERATE 2. NARROW INCISIONAL SPACE IS RAPIDLY BY FIBRIN CLOTTED BLOOD

HEALING BY FIRST INTENTION -PRIMARY UNION 3. DEHYDRATION AT THE SURFACE PRODUCES A SCAB TO COVER TO PROTECT HEALING SITE 4. WITHIN 24 HOURS NEUTROPHILS APPEAR AT THE INCISION MARGIN , MIGRATING TOWARD FIBRIN COLT. BASAL CELLS AT THE CUT EDGE OF EPIDERMIS UNDERGO MITOSIS ALONG WITH DEPOSITION OF BASEMENT MEMBRANE COMPONENTS
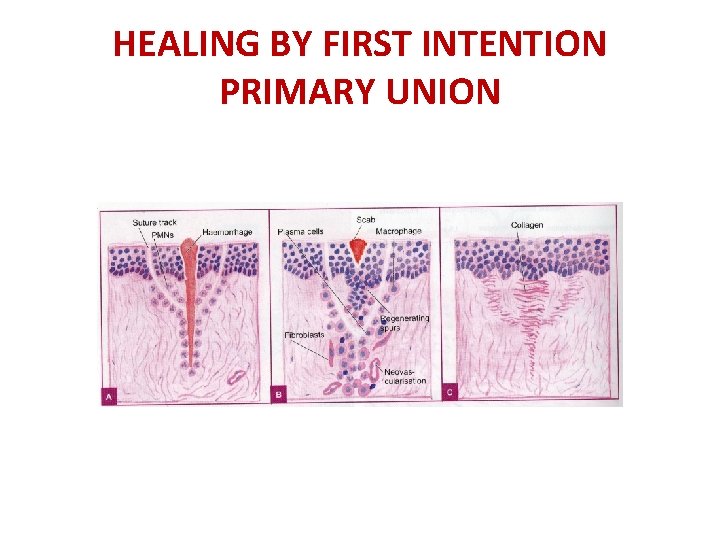
HEALING BY FIRST INTENTION PRIMARY UNION

HEALING BY FIRST INTENTION -PRIMARY UNION 5. BY 48 HOURS EPITHELIAL CELLS MEET AT THE MIDLINE BENEATH THE SCAB. , THUS FORMING A THIN CONTINUOUS EPITHELIAL LAYER. 6. BY DAY 3 NEUTROPHILS HAVE BEEN LARGELY REPLACED BY MACROPHAGES AND GRANULATION TISSUE PROGRESSIVELY INVADE THE INCISION SPACE WITH COLLAGEN FIBRE DEPOSITION. EPITHELIAL CELL PROLIFERATION CONTINUESYEILDING A THICK EPIDERMAL COVERING LAYER. COLLAGEN FIBRES ARE ORIENTED VERTICALLY

HEALING BY FIRST INTENTION -PRIMARY UNION 7. BY DAY 5 NEOVASCULARISATION REACHES IT’S PEAK. COLLAGEN FIBRES BECOME MORE ABUNDANT AND BECOME HORIZONTALLY ORIENTED TO BRIDGE THE INCISION. EPIDERMAL CELLS DIFFERENTIATE AND RECOVER IT’S NORMAL THICKNESS
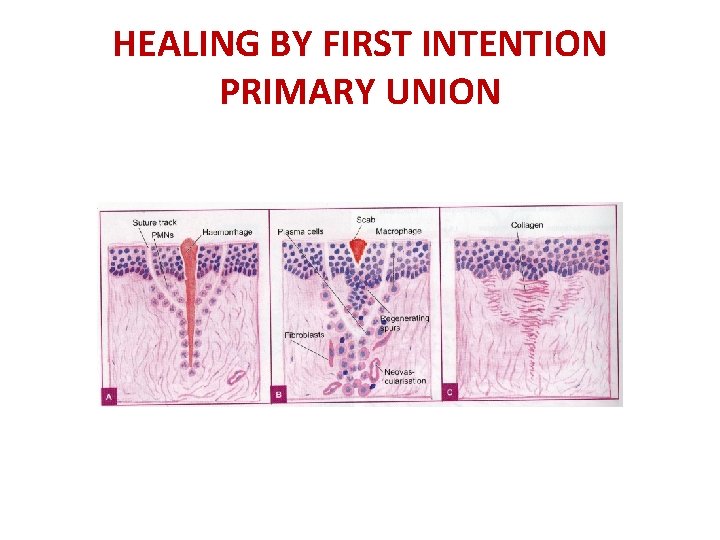
HEALING BY FIRST INTENTION PRIMARY UNION

HEALING BY FIRST INTENTION -PRIMARY UNION 8. DURING SECOND WEEK COLLAGEN ACCUMULATION AND FIBROBLAST PROLIFERATION CONTINUES BUT LEUKOCYTEINFILTRATE, OEDEMA, AND INCREASED VASCULARITY ARE DIMINISHED.
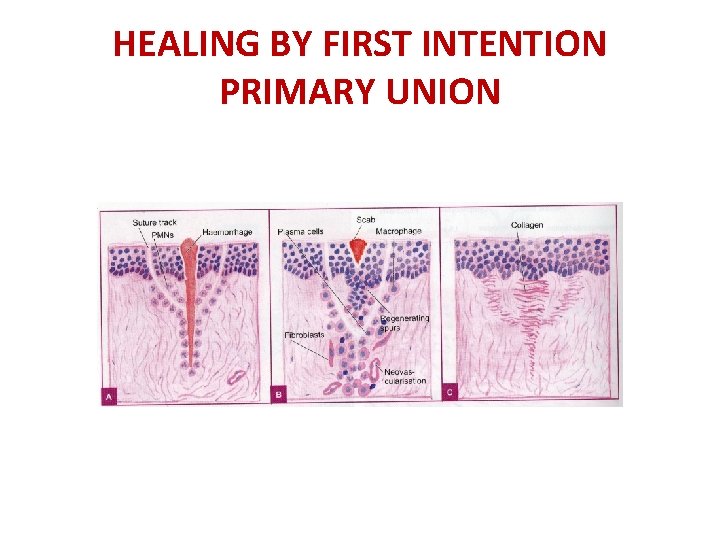
HEALING BY FIRST INTENTION PRIMARY UNION

HEALING BY FIRST INTENTION -PRIMARY UNION 9. BY THE END OF THE FIRST MONTH –SCAR COMPRISES CELLULAR CONNECTIVE TISSUE DEVOID OF INFLAMMATORY CELLS AND COVERED BY NORMAL EPITHELIA. THE TENSILE STRENGTH OF THE WOUND INCREASES WITH TIME

HEALING BY SECOND INTENTIONSECONDARY UNION CELL OR TISSUE LOSS IS MORE EXTENSIVE AS IN INFARCTION, INFLAMMATORY ULCERATION, ABSCESS, LARGE WOUNDS CHARACTERISED BY EXTENSSIVE INGROWTH OF GRANULATION TISSUE FROM WOUND MARGINS. FOLLOWED BY ACCUMULATION OF ECM AND SCAR TISSUE
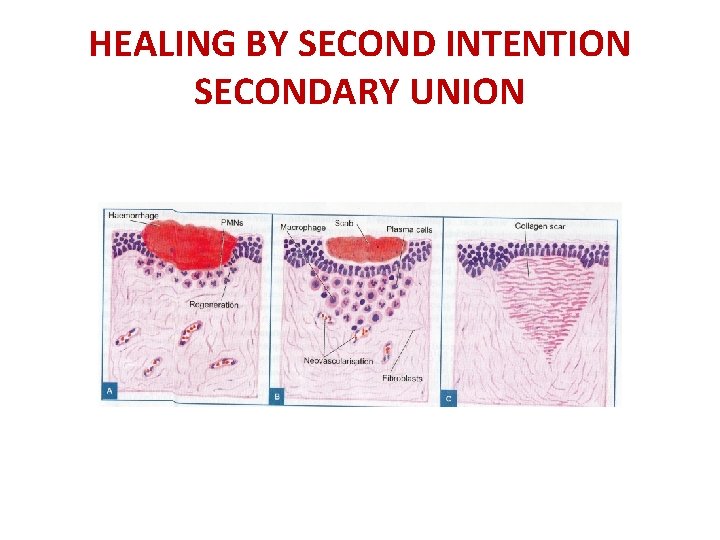
HEALING BY SECOND INTENTION SECONDARY UNION

WOUND STRENTGH CAREFULLY SUTURED WOUND HAVE 70% STRENGTH OF UNWOUDED SKIN BECAUSE OF PLACEMENT OF SUTURES WHEN SUTURES ARE REMOVED , USUALLY BY ONE WEEK WOUND STRENGTH REDUCES TO 10% OF THAT OF UNWOUDED SKIN BUT INCREASES RAPIDLY OVER NEXT 4 WEEKS WHICH IS DUE TO COLLAGEN SYNTHESIS EXCEEDING DEGRADATION DURING FIRST 2 MONTHS DUE TO CROSS LINKING AND INCREASED FIBRE SIZE

WOUND STRENTGH WOUND STRENGTH REACHES 70% 80% OF NORMAL BY 3 MONTHS
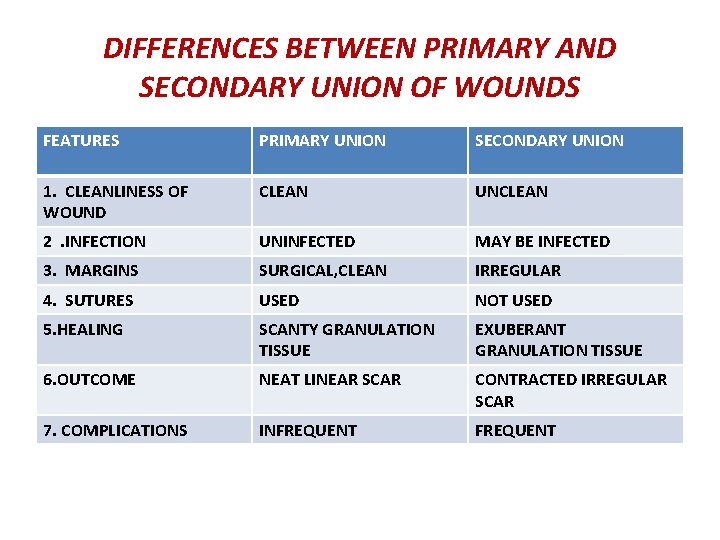
DIFFERENCES BETWEEN PRIMARY AND SECONDARY UNION OF WOUNDS FEATURES PRIMARY UNION SECONDARY UNION 1. CLEANLINESS OF WOUND CLEAN UNCLEAN 2. INFECTION UNINFECTED MAY BE INFECTED 3. MARGINS SURGICAL, CLEAN IRREGULAR 4. SUTURES USED NOT USED 5. HEALING SCANTY GRANULATION TISSUE EXUBERANT GRANULATION TISSUE 6. OUTCOME NEAT LINEAR SCAR CONTRACTED IRREGULAR SCAR 7. COMPLICATIONS INFREQUENT

COMPLICATIONS OF WOUND HEALING 1. INFECTION 2. IMPLANTATION EPIDERMOID CYST 3. PIGMENTATION 4. POOR SCAR FORMATION DUE TO INADEQUATE GRANULATION TISSUE FORMATION

COMPLICATIONS OF WOUND HEALING 5. INCISIONAL HERNIA 6. HYPERTROPHIED SCAR AND KELOID(CLAW LIKE) FORMATION, MORE SEEN IN BLACK RACE 7. EXCESSIVE CONTRACTION- DUPUYTREN’S(PALMAR) CONTRACTURE, PLANTAR CONTRACTURES 8. NEOPLASM- DEVELOPMENT OF CARCINOMA(SQUAMOUS CELL CARCINOMA) MARJOLI’S ULCER

FACTORS INFLUENCING HEALING 1. LOCAL FACTORS INFECTION POOR BLOOD SUPPLY FOREIGN BODIES MOVEMENT

FACTORS INFLUENCING HEALING IONISING RADIATION –DELAYS GRANULATION TISSUE FORMATION EXPOSURE TO ULTRAVIOLET LIGHT –FACILITATE HEALING TYPE, SIZE AND LOCATION OF INJURY ALSO DETERMINES THE HEALING PROCESS

FACTORS INFLUENCING HEALING 2. SYSTEMIC FACTORS AGE NUTRITION –DEFICIENCY OF PROTEIN, VITAMIN C AND ZINK DELAYS HEALING PROCESS DRUGS LIKE GLUCOCORTICOID, ANTIINFLAMMATORY AGENTSDELAY HEALING

FACTORS INFLUENCING HEALING SYSTEMMIC DISEASES LIKE UNCONTROLLED DIABETES, HAEMATOLOGIC ABNORMALITIES-NEUTROPHIL DEFECT, NEUTROPENIA, BLEEDING DISORDERS

HEALING IN SPECIALIZED TISSUES FRACTURE HEALING DEPENDS ON TYPE OF FRACTURE

FRACTURE HEALING 1. SIMPLE FRACTURE 2. COMPOUND FRACTURE

PRIMARY UNION OCCURS WHEN THE ENDS OF THE FRACTURE APPROXIMATED BONY UNION TAKES PLACE WITH FORMATION OF MEDULLARY CALLUS WITHOUT PERIOSTEAL CALLUS FORMATION

SECONDARY UNION THE NATURAL COURSE OF THE FRACTURE HEALING INCLUDES 1. STABILISATION OF THE FRACTURED BONE FRAGMENTS BY PERIOSTEAL & ENDOSTEAL CALLUS FORMATION & BY FIBROCATRTILAGE DIFFERENTIATION

SECONDARY UNION 2. RESTORATION OF BONE CONTINUITY & BONE UNION BY OSSIFICATION

SECONDARY UNION 3. SUBSTITUTION OF AVASCULAR & NECROTIC AREAS BY HAVERSIAN REMODELLING 4. CORRECTION OF MALALIGNMENT BY REMODELLING

RADIOLOGICAL FEATURES 1. ABUNDANT CALLUS FORMATION 2. WIDENING OF THE FRACTURE GAP

RADIOLOGICAL FEATURES 3. SLOW DISAPPEARANCE OF THE RADIOLUCENT FRACTURE LINE DUE TO FIBROCARTILAGE MINERALISATION & BONE FORMATION 4. CALLUS FORMATION OCCURS WITHIN A FEW DAYS.

FRACTURE HEALING 5. FIRST WOVEN BONE IS FORMED WHICH FORMS CONICAL CUFF AROUND THE FRAGMENT ENDS

CALLUS FORMATION AT FIRST YOUNG COLLAGEN FIBRES ARE RANDOMLY ORIENTED, THEN GET ORGANISED INTO BUNDLES , GET ANCHORED TO THE BONE FRAGMENT ENDS,

CALLUS FORMATION THEIR DIRECTION REFLECTS THE MAIN DIRECTION OF THE TENSILE FORCES CREATED BY THE INTERFRAGMENTARY MOVEMENT

CALLUS FORMATION FIBROCARTILAGE ON THE OTHER HAND IS FORMED IN AREAS WHERE THE SIZE & SHAPE OF THE FRACTURE GAP LEADS TO COMPRESSION.

CALLUS FORMATION AS THE CONNECTIVE TISSUE & FIBROCARTILAGE THICKENS THE FRACTURE BECOMES INCREASINGLY STABLE ALLOWING A STABLE PLATFORM ON TO WHICH MINERALISATION CAN OCCUR TO FORM BONE.

FRACTURE HEALING OVER TIME THE CONNECTIVE TISSUE & FIBROCARTILAGE IS GRADUALLY RESORBED BY OSTEOCLASTS AND REPLACED BY BONE
DIFFERENT KINDS OF CALLUS & THEIR FORMATION 1. PROCALLUS FORMATION-DESCRIBED IN THE FOLLOWING STEPS. a. HAEMATOMA - BLEEDING FROM TORN BLOOD VESSELS FILLING THE FRACTURE SITE.

DIFFERENT KINDS OF CALLUS & THEIR FORMATION FIBRIN CLOT ACTS AS A FRAMEWORK FOR SUBSEQUENT GRANULATION TISSUE FORMATION.

PROCALLUS FORMATION b. LOCAL INFLAMMATORY RESPONSE AT THE SITE OF INJURY EXUDATION OF FIBRIN, POLYMORPHS & MACROPHAGES

PROCALLUS FORMATION MACROPHAGES CLEAR AWAY THE FIBRIN, RED BLOOD CELLS, INFLAMMATORY EXUDATE & DEBRIS FRAGMENTS OF NECROSED BONE ARE SCAVENGED BY MACROPHAGES & OSTEOCLASTS.

PROCALLUS FORMATION C. INGROWTH OF GRANULATION TISSUE – NEOVASCULARISATION & PROLIFERATION OF MESENCHYMAL CELLS FROM PERIOSTEUM & ENDOSTEUM –

PROCALLUS FORMATION THUS A SOFT TISSUE CALLUS IS FORMED WHICH JOINS THE ENDS OF FRACTURED BONE WITHOUT MUCH STRENGTH
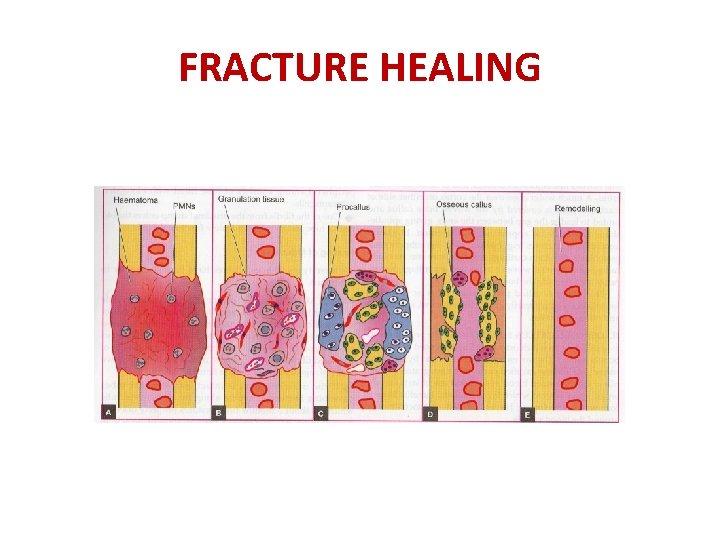
FRACTURE HEALING
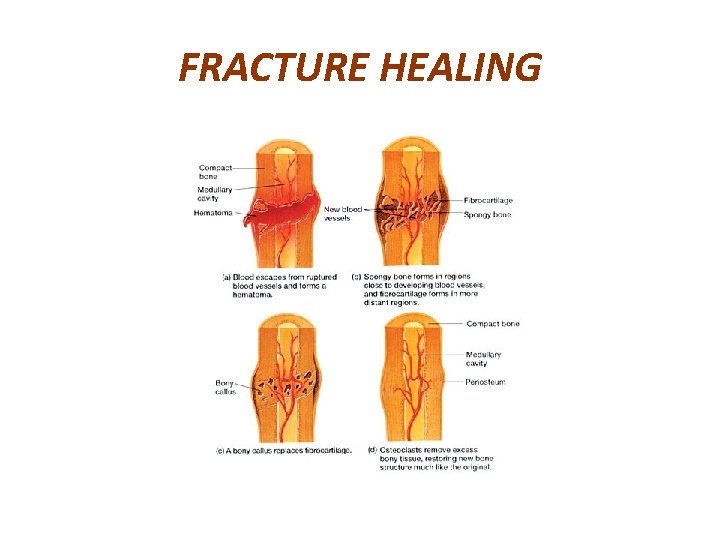
FRACTURE HEALING

PROCALLUS FORMATION d. CALLUS COMPOSED OF WOVEN BONE AND CARTILAGE – STARTS WITHIN FIRST FEW DAYS.

PROCALLUS FORMATION CELLS OF INNER LAYER OF THE PERIOSTEUM HAVE OSTEOGENIC POTENTIAL & LAY DOWN COLLAGEN AS WELL AS OSTEOID MATRIX IN THE GRANULATION TISSUE

PROCALLUS FORMATION THE OSTEOID UNDERGOES CALCIFICATION & IS CALLED WOVEN BONE CALLUS WHICH BRIDGE THE GAP BETWEEN THE ENDS GIVING SPINDLE SHAPE OR FUSIFORM APPEARANCE TO THE UNION
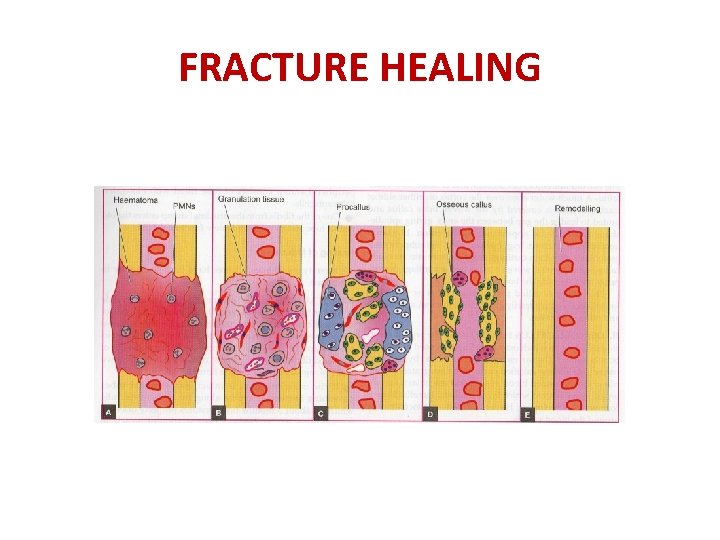
FRACTURE HEALING
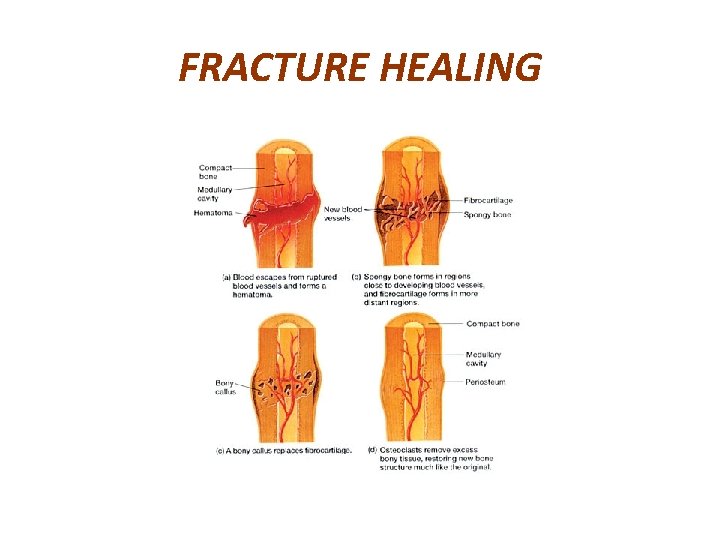
FRACTURE HEALING

PROCALLUS FORMATION IN THE POORLY IMMOBILISED FRACTURES eg- THE SUBPERIOSTEAL OSTEOBLASTS MAY FORM CARTILAGE AT THE FRACTURE SITE.

PROCALLUS FORMATION THIS STAGE IS CALLED PROVISIONAL OR PROCALLUS FORMATION & IS ARBITRARILY DIVIDED INTO EXTERNAL, INTERMEDIATE & INTERNAL PROCALLUS

OSSEOUS CALLUS FORMATION THE PROCALLUS ACTS AS A SCAFFOLDING ON WHICH OSSEOUS CALLUS COMPOSED OF LAMELLAR BONE IS FORMED
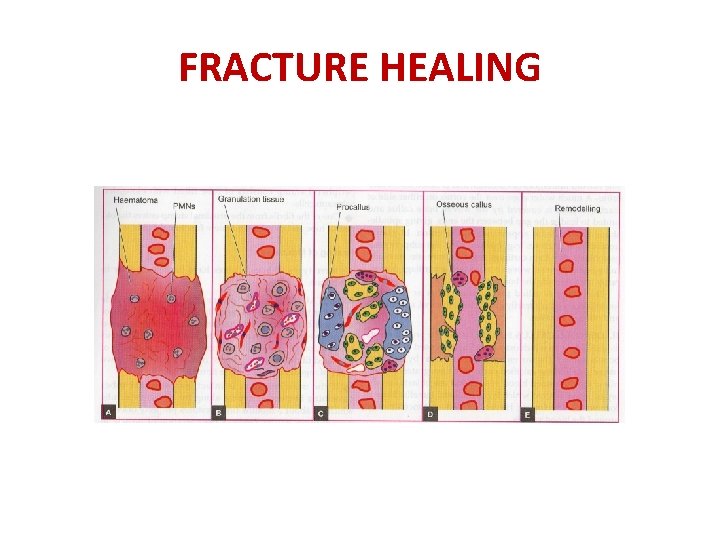
FRACTURE HEALING
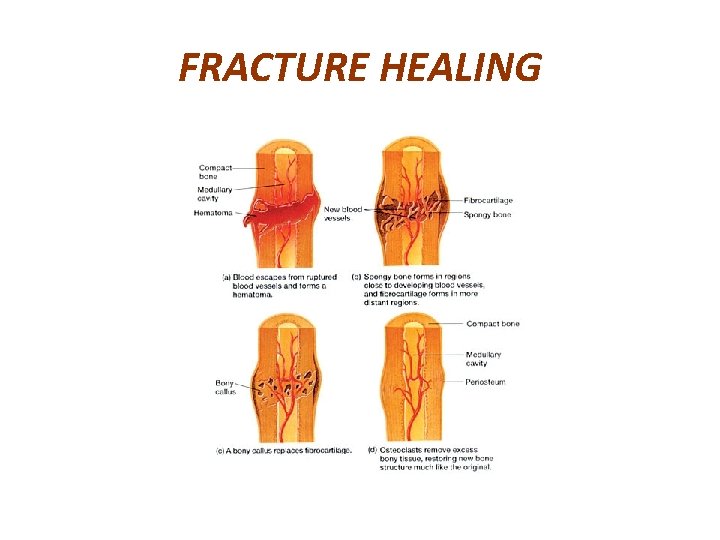
FRACTURE HEALING
OSSEOUS CALLUS FORMATION THE WOVEN BONE IS CLEARED AWAY BY INCOMING OSTEOCLASTS & THE CALCIFIED CARTILAGE DISINTEGRATES, IN THEIR PLACE NEWLY FORMED BLOOD VESSELS

OSSEOUS CALLUS FORMATION OSTEOBLASTS INVADE LAYING DOWN OSTEOID WHICH IS CALCIFIED. LAMELLAR BONE IS FORMED BY DEVELOPING HAVERSIAN SYSTEM CONCENTRICALLY AROUND THE BLOOD VESSELS

REMODELLING DURING THE FORMATION OF LAMELLAR BONE, OSTEOBLASTIC LAYING & OSTECLASTIC REMOVAL ARE TAKING PLACE, REMODELLING THE UNITED BONE ENDS, WHICH AFTER SOMETIME IS INDISTINGUISHABLE FROM NORMAL BONE.

REMODELLING THE EXTERNAL CALLUS IS CLEARED AWAY COMPACT BONE IS FORMED IN PLACE OF INTERMEDIATE CALLUS BONE MARROW DEVELOPS IN PLACE OF INTERNAL CALLUS
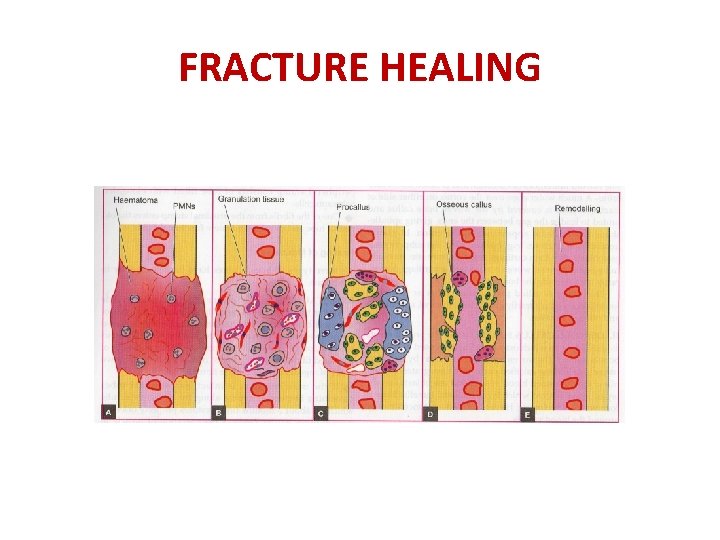
FRACTURE HEALING
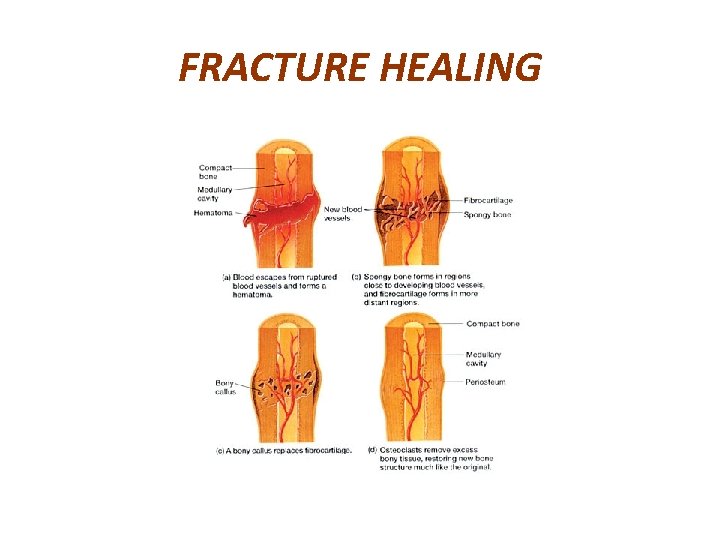
FRACTURE HEALING

COMPLICATIONS OF FRACTURE HEALING 1. FIBROUS UNION – INSTEAD OF OSSEOUS UNION IF IMMOBILISATION OF FRACTURED BONE IS NOT DONE 2. PSEUDOARTHROSIS- OCCATIONALLY A FALSE JOINT MAY DEVELOP AT THE FRACTURE SITE

COMPLICATIONS OF FRACTURE HEALING 3. NONUNION –IF SOFT TISSUE IS INTERPOSED BETWEEN THE FRACTURED ENDS 4. DELAYED UNION- CAUSES AREINFECTION, INADEQUATE BLOOD SUPPLY, POOR NUTRITION, MOVEMENT & OLD AGE
- Slides: 68