Wound Complications Seroma Collection of liquefied fat serum



































































- Slides: 71

Wound Complications

Seroma Collection of liquefied fat, serum, & lymphatic fluid under incision ¢ Localized, well-circumscribed swelling, pressure discomfort ¢ l No erythema, tenderness Evacuated and packed heal by secondary intention ¢ Secondary infection open wound ¢

Hematoma Ecchymotic, localized wound swelling, drainage of dark red fluid ¢ Open wound and pack if detected soon after surgery ¢ Small hematoma 2 wks after surgery may resorb ¢

Wound Dehiscence ¢ Separation of fascial layers l ¢ Evisceration of bowel Technical error, deep wound infection

Case 1 87 yo s/p repair of perforated bowel with gross stool spillage ¢ How do you close the fascia? ¢ Interrupted figure-eight good strength l Can use absorbable mesh or retention sutures to reduce tension l

Case 2 Cont. How do you close the subcutaneous tissue? ¢ Leave it open if wound clean after 5 d, then you can approximate edges ¢

…later that night ¢ Sudden drainage of large volume of clear, salmon-colored fluid… l Examine patient & wound… • probe wound with sterile applicator l Examine wound & see bowel… • cover bowel with sterile saline moistened towel O. R. STAT

Wound infection Erythema, tenderness, edema, occasional drainage ¢ Rx: open wound, free loculations, irrigate, pack ¢ l CT scan if pus emanating deep to fascia

Called for a temp of 102… ¢ Examine patient & wound l Erythema, drainage of grayish dishwater-colored fluid, what seems like necrotic fascia, mild crepitus… • O. R. STAT-rapid & expeditious debridement • clostridiomyonecrosis

Prevention of SSI Stop smoking 48 h prior, encourage weight loss, bowel prep, taper/stop immunosuppresants ¢ Prophylactic antibiotics ¢ Insert drain if gangrenous organ ¢ Delayed primary closure in contaminated field ¢

Complications of Thermal Regulation & Cardiac Complications Sumit De, M. D

Complications of Thermal Regulation • • • Hypothermia Malignant Hyperthermia Postoperative Fever Respiratory Complications Aspiration Pneumonitis Pulmonary Edema, Acute Lung Injury, ARDS • Pulmonary Embolism

Hypothermia • Causes: cold environment, paralysis, rapid resuscitation, intra-op exposed areas, irrigation • Body’s response: i. CO, i. HR, cardiac arrhythmias, icoagulation, vasoconstriction • Cardiac alterations, diuresis, hepatic & neurological dysfunction • Keep patient WARM

Malignant Hyperthermia • Exposure to inhalation agents or succinylcholine • Mostly occurs in youth • High fever, tachycardia, muscular rigidity, and cyanosis • Metabolic acidosis, hyperkalemia, hypercalcemia Management: Stop inhalation agent Cancel/conclude surgery Dantrolene, 2. 5 mg/kg Cool body Reverse met acidosis Box 14 -3, Sabiston

Post-op Fever Wind: Atelectasis – 24 -48 hrs Water (UTI) – after POD #3 Wound – after POD #3 Walking (DVT/PE/Thrombophlebitis) – POD #7 -10 Wonder drugs - Anytime

Respiratory Complications • Most post-op patients who have respiratory complications can be managed with pulmonary toilet • Two types of respiratory failure: • Type I: hypoxic – abnormal gas exchange at alveolar level (e. g. pulmonary edema, sepsis) • Type II: hypercapnia – excessive narcotic use, increased CO 2, respiratory dynamic changes , ARDS PNEUMONIA & Aspiration Pneumonitis

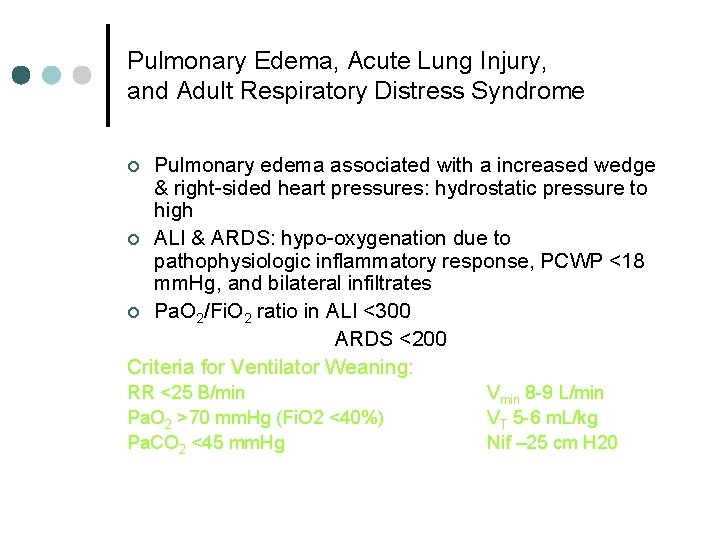
Pulmonary Edema, Acute Lung Injury, and Adult Respiratory Distress Syndrome Pulmonary edema associated with a increased wedge & right-sided heart pressures: hydrostatic pressure to high ¢ ALI & ARDS: hypo-oxygenation due to pathophysiologic inflammatory response, PCWP <18 mm. Hg, and bilateral infiltrates ¢ Pa. O 2/Fi. O 2 ratio in ALI <300 ARDS <200 Criteria for Ventilator Weaning: ¢ RR <25 B/min Pa. O 2 >70 mm. Hg (Fi. O 2 <40%) Pa. CO 2 <45 mm. Hg Vmin 8 -9 L/min VT 5 -6 m. L/kg Nif – 25 cm H 20

Pulmonary Embolism ¢ ¢ ¢ 500, 000 PEs occur annually, 100, 000 fatal Iliofemoral venous system most common source of PE; fat emboli s/p long bone fractures & air emboli s/p central lines are also well-known causes as well Signs & Sx of PE are shared with MI, PTX, PNA, and atelectasis ABG with Pa. O 2 <70 mm. Hg, T-wave inversions, and non-specific ST segment changes Severe PE: S 1 Q 3 T 3, RBBB, right-axis deviation CT angiography, Treat with HEPARIN

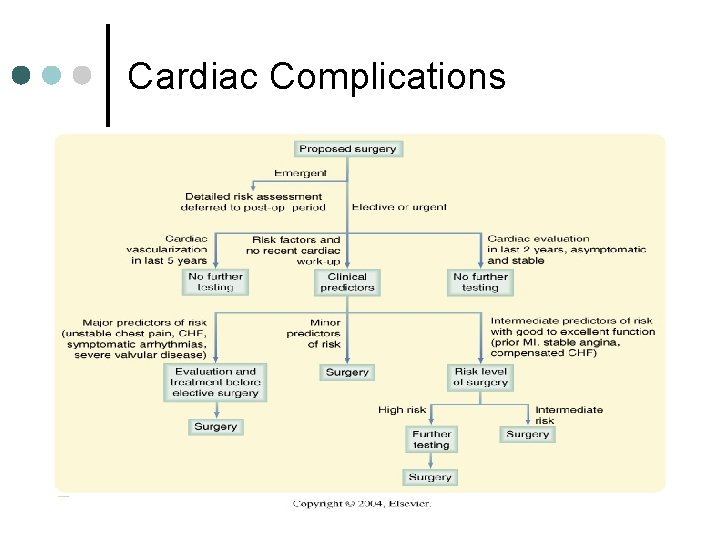
Cardiac Complications

Post-Op HTN CVA & op site bleeding are biggest concerns, especially after CEA, AAA, head & neck procedures. b-blockade Perioperative Ischemia and Infarction ~30% OR patients have CAD, perioperative MI mortality rate is ~30% compared to 12% for thiose without a surgical procedure; 8 -15% reinfarction rate for <3 mos post-MI OR patient, 3. 5% reinfarction rate for 3 -6 mos post-MI OR patient

Cardiogenic Shock ~50% or more LV mass damaged post-MI => hypoperfusion, ruptured papillary muscle, ventricular wall, aortic valvular insufficiency, mitral regurg, VSD Arrhythmias & CHF Intra-op occurrence of arrhythmias (30 sec abnl cardiac activity) is 60 -80%. Electrolyte abnormalities, medications, stress, endocrine abnormalities, and cardiac disease are main causes

RENAL AND URINARY TRACT COMPLICATIONS

URINARY RETENTION 6 -7 HOURS POST OP ¢ DISCOORDINATION OF TRIGONE AND DETRUSOR MUSCLES ¢ STRAIGHT CATH ¢

ACUTE RENAL FAILURE ¢ 10% PATIENTS IN PERIOP COURSE OLIGURIC <480 ML/DAY ¢ NONOLIGURIC >2 L/DAY ¢

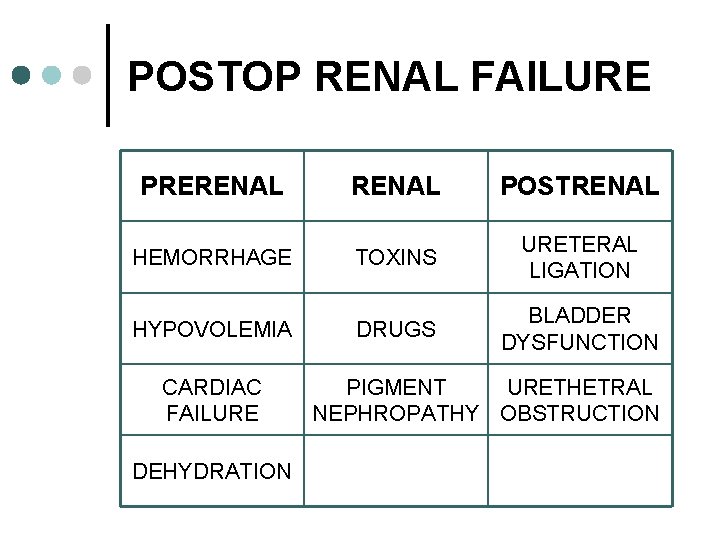
POSTOP RENAL FAILURE PRERENAL POSTRENAL HEMORRHAGE TOXINS URETERAL LIGATION DRUGS BLADDER DYSFUNCTION HYPOVOLEMIA CARDIAC FAILURE DEHYDRATION PIGMENT URETHETRAL NEPHROPATHY OBSTRUCTION

EVALUATION BUN: CR ¢ FRACTIONAL EXCRETION OF SODIUM ¢ PRERENAL FENA <1% ¢ RENAL FENA >3% ¢

CONTRAST NEPHROPATHY HYPOVOLEMIC ¢ DIABETIC VASCULOPATH ¢ HEART FAILURE ¢ ACE-I, NSAID ¢ HYDRATION ¢ MUCOMYST/ N-ACETYLCYSTEINE ¢ l 600 MG PO BID X 48 HRS Tepel M, van der Giet M, Schwarzfeld C, Laufer U, Liermann D, Zidek W: Prevention of radiographic-contrast-agent-induced reductions in renal function by acetylcysteine. N Engl J Med 343: 180– 184, 2000

RHABDOMYOLYSIS CRUSH INJURY ¢ MYOGLOBINURIC RENAL INJURY ¢ HYPERKALEMIA AND ACIDOSIS ¢ HYDRATION ¢ DIURESIS ¢ ALKALINIZATION ¢

INDICATIONS FOR HEMODIALYSIS SERUM POTASSIUM >5. 5 MEQ/L ¢ BUN >80 -90 MG/DL ¢ PERSISTENT ACIDOSIS ¢ ACUTE FLUID OVERLOAD ¢ UREMIC SYMPTOMS ¢ REMOVAL OF TOXINS ¢

METABOLIC COMPLICATIONS

ADRENAL INSUFFICIENY ¢ PRIMARY ADDISONS l INFECTIOUS l ¢ SECONDARY PITUITARY OR HYPOTHALAMIC DISEASE l CESSATION CHRONIC STEROIDS l

DIAGNOSIS BASELINE CORTISOL <15 UG/DL ¢ ACTH STIMULATION ¢ BASELINE CORTISOL l 0. 25 MG COSYNTROPIN IV l GLUCOCORTICOID l MEASURE CORTISOL AT 30 MIN l

SIADH HIGH ADH DESPITE HYPONATREMIA ¢ TRAUMA ¢ STROKE ¢ ADH PRODUCING TUMORS ¢ FLUID RESTRICTION ¢ ADMINISTRATION OF SALINE ¢ DIURETICS ¢

Gastrointestinal and Hepatobiliary Complications Harsh Jain, M. D.

Gastrointestinal complications ¢ Ileus Intestine that ceases contrancting for brief period of time (3 -5 days) l Operative manipulation, major small bowel injury, heavy narcotic use, intraabdominal infection, and pancreatitis can prolong the ileus l Past 7 days – prolonged ileus vs SBO l

Ileus vs SBO ¢ Ileus l l l ¢ SBO Distention Diffuse discomfort Hypoactive BS AXR l • Air into colon and rectum l Treat underlying cause l l l Distention Often intermittent, colicky pain Nausea, vomiting Obstipation AXR • No air into colon and rectum l May require operative therapy

SBO ¢ Causes l l l ¢ Adhesions Malignancy Hernias Diagnosis l l Flat plate and upright abdominal films CT Scan ¢ Management l l Hydration Correct electrolyte imbalances NGT Operative therapy if conservative management fails

Abdominal Compartment Syndrome ¢ Etiology l l ¢ Massive abdominal trauma Operation for massive abdominal infection Prolonged operation Pressures >25 cm. H 2 O Presentation l l Distended, tense Hypoxia Elevated airway pressure Oliguria ¢ Diagnosis l ¢ Measure intraabdominal pressures through foley cathether Treatment l l Surgical emergency Open fascial closure and re-do with temporary closure

Post op GI Bleeding ¢ Etiology l Stomach • PUD, Stress erosions, M-W tear, varices l Small intestines • AV malformations, anastomotic bleeding l Large intestines • anastomotic bleeding, diverticulosis, AV malformations, varices ¢ Management l l l l Large bore IV’s Fluids Labs NGT Correct coagulopathy Endoscopy/Colonosc opy Rarely surgery

Stomal Complications ¢ Prolapse l ¢ ¢ Stoma placement l l Necrosis l ¢ Rarely surgical problem ¢ Ischemia to skin level usually resolves Stenosis Peristomal hernia High output Bleeding l l Avoid skin folds Mobilize adequate length Through the rectus Below the anterior superior iliac crest

Pseudomembranous Colitis ¢ ¢ 1 % of patients who receive antibiotics in peri-op period Superinfection with C. Diff Secretion of exotoxin Pseudomembranes l ¢ Whitish membrane consisting of fibrin, WBC, mucus Diarrhea, cramping and dehydration ¢ ¢ Diagnosis by stool sample for exotoxin Treat with oral metronidazole or vanocmycin, IV metronidazole Sometimes disease progresses despite treatment If febrile, shock and tender __> colectomy

Anastomotic Leak ¢ Caused by l l ¢ Ischemia Tension Mismatch of the lumens Rough handling of tissues ¢ l l l ¢ Presentation l l l l Fever Abdominal pain Malaise Paralytic ileus Fullness of the area Wound dehiscence Fistula CT Scan ¢ Large fluid collection Air fluid levels in abscess cavity Free air Small leak with controlled fistula, conservative management with gut rest, TPN and antibiotics Larger leaks, or uncontrolled infection, no drainage usually require reoperation

Fistulas ¢ ¢ Abnormal communication between one hollow epithelialized organ and another epithelialized surface. Entero-cutaneous fistula l ¢ Initial erythema, abscess, and the subsequent efflux of GI contents Entero-vesical fistula l Pneumaturia or fecaluria ¢ ¢ ¢ Initial treatment includes fluids, antibiotics, protection of skin NPO, TPN Low output (<200 ml/day), consider enteral feedings Watch lytes with high output (1 -2 L/day) H 2 blockers, octreotide Foreign body, radiation, infection at fistula site, epithelialization of the fistula tract, neoplasm or, distal obstruction

Bile Duct Injuries ¢ ¢ Increased incidence after lap chole became generally accepted Presentation l ¢ Fever, RUQ Pain, malaise and occasionally jaundice ¢ ¢ ¢ Immediate CT Scan l l If fluid collection, precutaneous drainage with the drain left in ERCP ¢ Small leak and open common bile duct – stent Cystic duct injury or small leak – stent and drain Major injury or obstruction of bile duct – stenting is only supplementary to surgery Surgery l l If adequate control of leak, wait 5 -7 days Debride nonviable CBD Roux-en-Y limb to CBD Multiple drains

Neurological and ENT Complications Muhammad Irfan Saeed MD

Neurological Complications § § § Delirium, Dementia, Psychosis Seizure Disorder Stroke and Transient Ischemic attack

Delirium § High Risk Patients Elderly Prior history of Substance abuse Prior history of Psychiatric disorder Children

Causes of Acute Delirium § § § § Drug Intoxication (Alcohol, Antihistamines, Sedatives) Drug Withdrawal (Alcohol, Narcotics, Anxiolytics) Acute Cerebral Disorder (Edema, TIA, Stroke, Neoplasm) Metabolic Disturbance (Electrolyte disturbance, Hypoglycemia) Hemodynamic disturbances (Hypovolemia, MI, CHF) Infections (septicemia, UTI, Pneumonia) Respiratory Disorder (Respiratory failure, PE) Trauma (Head Injury, Burns)

Symptoms § § § Impaired memory Altered perception Altered sleep patterns Hallucinations Combativeness Confusion

Management § § § History and Physical examination (Neurological examination) Check Medication List Vitals with Pulse oximetry EKG, ABG, UA, CXR CT scan MRI

Treatment § § § Appropriate Sedation Treatment of the underlying cause Careful Observation (one to one nursing, transfer the patient to a naturally lighted room)

Delirium Tremens § § Onset usually 72 to 96 hours after alcohol cessation. Characterized by disorientation, hallucinations, autonomic lability (tachycardia, fever, HTN, diaphoresis)

Treatment § § § § Benzodiazepines Clonidine IVF Thiamine Magnesium sulphate Folate Restraints

Seizure Disorder § § Caused by paroxysmal electrical discharges from the cerebral cortex. Cause Primary Secondary

Causes § § § Primary Intracranial Tumor Hemorrhage Trauma Idiopathic § § § Secondary Metabolic Sepsis Systemic disease (epilepsy) Pharmacological agents (antidepressants, hypoglycemic agents, Lidocaine)

Symptoms and Signs § § § Convulsions Rhythmic myoclonic activity Loss of consciousness Change in mental status (lack of neurological responsiveness) Fecal and urinary incontinence Post event amnesia

Diagnostic Workup § § § § Rapid blood glucose determination Oxygen saturation CBC Chem-7 Serum calcium / magnesium Serum levels of anticonvulsants CT scan

Treatment § § § § Patient safety (airway, restraints) IV Benzodiazepines Phenytoin Carbamezapine Valproic acid Gabapentin Treat the underlying cause

Stroke and TIA § § § § One of the most devastating complication Most common causes include Advanced atherosclerotic disease of Internal carotid artery. Atrial fibrillation VSD Acute hepatic failure Excessive anticoagulation

Symptoms and Signs § § § Unilateral weakness or clumsiness Sensory loss Speech disorder Diplopia Vertigo Alteration in mental status

Diagnostic Workup § § § § Finger stick glucose Pulse oximetry CBC Chem-7 Coagulation studies CT scan of head Echocardiography Carotid ultrasound

Management § § § Depends upon type of stroke (hemorrhagic vs. Non-hemorrhagic) Supplemental oxygen and IVF Pharmacological BP reduction (Mannitol and Dexamethasone) Aspirin 325 mg orally Thrombolytic therapy in close consultation with neurologist

ENT Complications § § § Epistaxis Most frequent postoperative causes NG tube placement Endotracheal tube placement Temperature probe Pressure application for 3 -5 minutes Nasal packing for 10 -15 minutes Nasal packing for 1 -3 days Treatment of underlying cause

Sinusitis § § Often missed in postoperative period due to analgesics, antipyretics and NG tube Malaise, dull aching pain in maxillary or frontal sinus area and low grade fever CT scan of head Treatment Removal of NG tube Antibiotics Decongestants Drainage Procedure

Questions? ? ?

Question #1 ¢ Which of the following statements about tracheoinominate artery fistulas after tracheostomy is not true? A Occur within 2 -3 weeks l B Caused by excessive inflation of cuff l C Mortality of 50% l D Hyperinflation of cuff may control bleeding temporarily l

Answer!!! ¢ C Mortality is 80% Can be life threatening l Presents as exsanguinating hemoptysis (small herald bleed may be noted) l Avoid placing trach below 4 th tracheal ring l Can place finger along trach and compress artery l

Question#2 ¢ Which of the following insufflation gases for laparoscopic pneumoperitoneum can cause hypercarbia and acidosis? A Carbon dioxide l B Nitrous oxide l C Helium l D Argon l

Answer!!! ¢ A Carbon dioxide l Also associated with increases in arterial pressure, pulmonary vascular resistance, pulmonary arterial pressure. Decreases in cardiac contractility.

Question#3 ¢ A postop patient has a serum Na of 125 meq/L and blood glucose of 500 mg/dl (nl 100). What would Na level be if glucose level normal? A 120 meq/L l B 122 meq/L l C 137 meq/L l

Answer!!! ¢ C 137 meq/L l Each 100 mg/dl rise in blood glucose above normal is equivalent to a 1. 63. 0 meq/L fall in the apparent Na concentration.