Workers Compensation Drug Formulary The Basics Louisiana WCAC

Workers Compensation Drug Formulary: The Basics Louisiana WCAC August 2015 Ken Eichler; Director Regulatory & Outcome Initiatives Work Loss Data Institute / ODG ken@worklossdata. com 917 -270 -3921

Improving Quality of Care & Outcomes l Improving the way opioids are prescribed through clinical practice guidelines can ensure patients have access to safe, effective treatment while reducing the number of people who misuse, abuse, or overdose from these powerful drugs. l Informing agencies, providers, and medical/professional organizations about evidence-based practices that can improve patient outcomes. Content source: Centers for Disease Control and Prevention, National Center for Injury Prevention and Control, Division of Unintentional Injury Prevention Page last updated: June 12, 2014 2

Workers Compensation Research Institute http: //www. wcrinet. org/whats_new. html l 3 New WCRI Publications – WCRI Medical Price Index for Workers' Compensation, Sixth Edition (MPI-WC) – Impact of a Texas-Like Formulary in Other States – Interstate Variations in Use of Narcotics, 2 nd Edition – Longer-Term Use of Opioids, 2 nd Edition – Higher costs of doctor-dispensed drugs draw state reform efforts
Impacts of Texas Adoption of ODG Guidelines & Formulary Ø 2014 Workers Compensation Research Institute Study “Impact of a Texas-Like Formulary in Other States” http: //www. wcrinet. org/whats_new. html Ø 70 % Reduction in Non-Formulary Prescriptions Ø Physicians infrequently substitute formulary drugs for non-formulary drugs. Ø Ø 4 Medical/drug costs both down 30% (opioid costs down 81%) NASI Study: Texas new lowest cost state in the U. S.
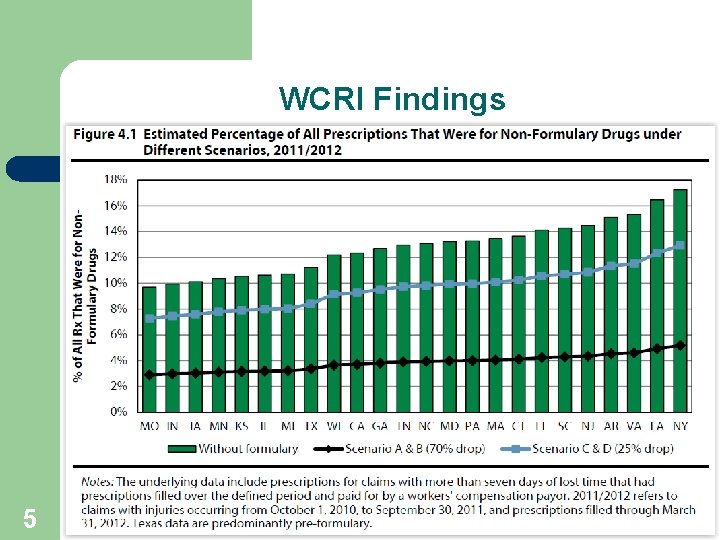
WCRI Findings 5

Workers Compensation Versus Group Health Coverage GROUP HEALTH “YOU GET WHAT YOU PAY FOR” • • 6 Coverage is purchased for pre-set defined services and benefits on a plan & premium specific, by option basis. Cost based with predefined set benefits, coverage, co-pays and deductibles knowingly purchased and factored into premium pricing. Insurer costs and profits are factored into determination of Covered Services and Formulary. Minimal opportunity to address case specific needs & variences.

Workers Compensation Versus Group Health Coverage WORKERS COMPENSATION “MEDICALLY APPROPRIATE & CAUSALLY RELATED” • • • 7 Coverage affords treatment & services required to restore the Patient to MMI and/or ongoing care as medically necessary. Evidence Based reflecting medical appropriateness; NOT costs, discounts, rebates or incentives from providers, manufacturers and distributors. “Traditionally” consistent coverage for all Workers on a jurisdictional basis without co-pays or deductibles paid by the Injured Worker.

All Formularies Are Not A Good Fit for Workers Compensation • EBM Based versus Business Model Based • Workers Comp versus Group Health • Ease of use by all Stakeholders, decreasing the need for pre-authorization • 8 • Use in the Authorization, Utilization Review and Appeals processes Integration into Claims & PBM programs/systems

Evidence Based Medicine (EBM) Guidelines & Formularies Can Afford: 9 Ø Safeguards for Patients against risky, questionable and inappropriate care and prescription medications Ø User friendly framework to address Patient & case specific needs Ø Improved Patient outcomes, quality of life and function Ø Decreased disabilities, substance abuse, overdoses & deaths Ø Identification of “pre-approved” care and medications versus those requiring expedited pre-authorization with substantiation of need, thereby DECREASING the volume of UR & IMR Ø Improved reserve setting, cost containment and MSA’s

EBM Formularies Empower Medical Providers 10 Ø Decrease adversarial relationship with Patients and enable Physicians to “Just Say No” Ø Expedite authorizations and medical reviews Ø Consider the picture within the picture; the specific drug versus the alternative drug options versus the alternatives to drugs.

Consider Treatment Options l l 11 Isolated Treatments & Medication is a small but costly and potentially dangerous piece of the treatment plan puzzle. Look at the picture within the picture; i. e. - the specific drug versus the alternative drug options versus the alternatives to drugs.

Scope of the Drug Formulary 12 l FDA Orange Book: FDA Approved Drug Products with Therapeutic Equivalence Evaluations l Front line recommendations versus required pre-authorization l Compounds l Access by Class, Generic, Brand & NDC Code l Opioid MED (Morphine Equivalent Dose) Calculators
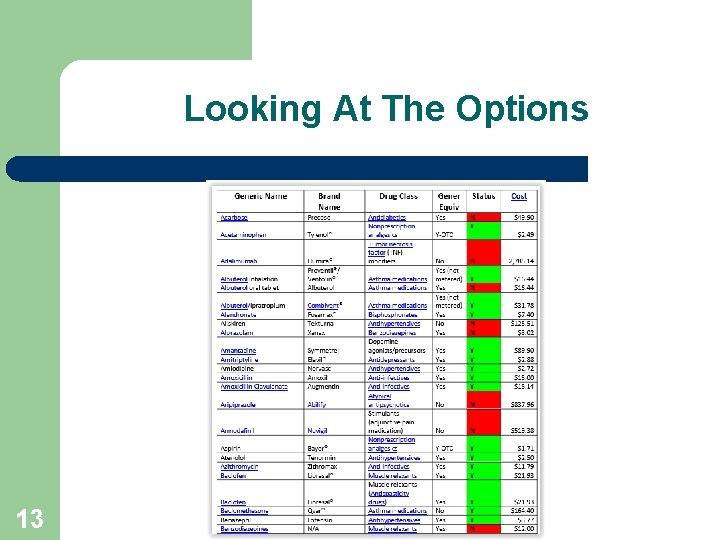
Looking At The Options 13

NDC ADVISOR “Look-up” Tool 14

NDC ADVISOR Recommendation with Hyperlinks to Supporting Evidence 15

Excerpt of Evidence Based Supporting Documentation with Hyperlinks This topic is covered under multiple headings. See more specific entries, as follows: Opioids, criteria for use; Opioids for chronic pain; Opioids for neuropathic pain; Opioids for osteoarthritis; Opioids, cancer pain vs. nonmalignant pain; Opioids, dealing with misuse & addiction; Opioids, dosing; Opioids, indicators for addiction; Opioids, long-acting; Opioids, long-term assessment; Opioids, pain treatment agreement; Opioid provider outreach; Opioids, psychological intervention; Opioids, specific drug list; Opioids, screening for risk of addiction (tests); Opioids, state medical boards guidelines; Detoxification; Substance abuse (tolerance, dependence, addiction); Urine Drug Testing (UDT) in patient-centered clinical situations; Weaning of medications; Implantable drug-delivery systems (IDDSs); Methadone; Buprenorphine; Rapid detox; Testosterone replacement for hypogonadism (related to opioids); Opioid hyperalgesia; Opioid-induced constipation treatment; & Opioids, specific drug list. Opioid drugs are also referred to as opiate analgesics, narcotic analgesics, or schedule C (II -IV) controlled substances. Opioid analgesics are a class of drugs (e. g. , morphine, codeine, and methadone) that have a primary indication to relieve symptoms related to pain. Opioid drugs are available in various dosage forms and strengths. They are considered the most powerful class of analgesics that may be used to manage both acute and chronic pain. These medications are generally classified according to potency and duration of dosage duration. Overall Classification: Pure-agonists: include natural and synthetic opioids such as morphine sulfate (MS Contin®), hydromorphone (Dilaudid®), oxymorphone (Numorphan®), levorphanol (Levo-Dromoran®), codeine (Tylenol w/Codeine 3®), hydrocodone (Vicodin®), oxycodone (Oxy. Contin®), methadone (Dolophine HCl®), and fentanyl (Duragesic®). This group of opioids does not have a ceiling effect for their analgesic efficacy nor do they antagonize (reverse) the effects of other pure opioids. (Baumann, 2002) Morphine is the most widely used type of opioid analgesic for the treatment of moderate to severe pain due to its availability, the range of doses offered, and its low cost. 16

Morphine Equivalent Dose Calculator 17

Nearly 15, 000 people die every year of overdoses involving prescription painkillers. In 2010, 1 in 20 people in the US (age 12 or older) reported using prescription painkillers for nonmedical reasons in the past year. 18 Enough prescription painkillers were prescribed in 2010 to medicate every American adult around-the clock for a month.

Drug Overdoses in the USA: 2012 l l l 19 Leading cause of injury death, exceeding motor vehicle traffic crashes or firearms 117% increase from 1999 to 2012 account for 9 out of 10 poisoning deaths 114 people died daily as a result of an overdose 6, 748 people were treated in emergency departments (ED) daily for the misuse or abuse of drugs; approximately 2. 5 million
Drug Overdoses in the USA: 2012 l 41, 502 drug overdose deaths 33, 175 (79. 9%) unintentional 5, 465 (13. 2%) suicidal intent 80 (0. 2%) homicides 2, 782 (6. 7%) undetermined intent l 20 Some deaths include more than one type of drug 22, 114 (53%) were related to pharmaceuticals 16, 007 (72%) involved opioid analgesics 6, 524 (30%) involved benzodiazepines

Drug Overdoses in the USA: 2011 l Drug misuse and abuse caused about 2. 5 million emergency department (ED) visits – – – 21 1. 4 million were related to non-medical use of pharmaceuticals. 501, 207 visits related to anti-anxiety and insomnia medications 420, 040 visits were related to opioid analgesics

Female Overdoses in the USA Nearly 48, 000 women died of prescription painkiller overdoses between 1999 and 2010. Deaths from prescription painkiller overdoses among women have increased more than 400% between 1999 and 2013, compared to 265% among men. 22

Child Drug Overdoses in the USA 23 l Between 2004 and 2005, an estimated 71, 000 children (18 or younger) were seen in EDs each year because of medication overdose (excluding self-harm, abuse and recreational drug use). l Among children under age 6, pharmaceuticals account for about 40% of all exposures reported to poison centers.

Who Consumes the Prescribed Drugs? l Over 50% of prescribed medications are consumed by individuals other than those they have been prescribe for. l Points of access other than Prescribers: – – – 24 l The generous helping hand The medicine cabinet Let’s “party” Guns get locked up, but medications do not.

How do they get the drugs? l l l 25 Studies show that over 80% of patients get what they want…drugs, testing, referrals, etc. Why don’t docs “Just Say NO”? Over 80% of narcotics are prescribed by less than 10% of the prescribers. Legitimate injured workers in need of meds Injured workers bolstering their claims Drug seekers – need vs. addiction vs. diversion
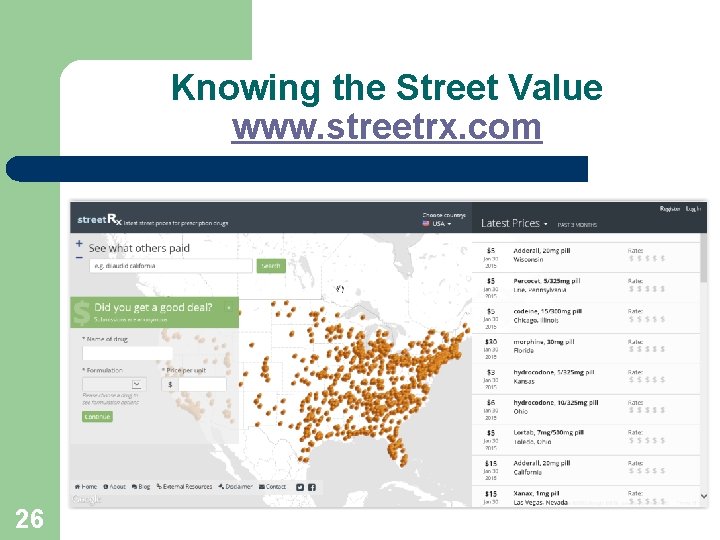
Knowing the Street Value www. streetrx. com 26

The Soaring Cost of the Opioid Economy New York Times: June 22, 2013 The stronger the opioid, the higher the expense. Average claim cost without use of opioids: $13, 000 Cost with short-acting opioid like Percocet: $39, 000 Cost with long-acting opioid like Oxy. Contin: $117, 000 27
The Soaring Cost of the Opioid Economy New York Times: June 22, 2013 28 l Between 2001 and 2008, narcotics prescriptions as a share of all drugs used to treat workplace injuries jumped 63 percent. l In California, workplace insurers spent $252 million on opioids in 2010, which represented about 30 percent of all prescription costs; in 2002, opioids accounted for 15 percent of drug expenditures.

Louisiana “Regulatory Review” Complementary ODG Trial Access URL: www. odgtreatment. com Username: LAWCAC Passcode: ODG 29

THANK YOU FOR THE OPPORTUNITY TO PRESENT Ken Eichler Director, Regulatory & Outcome Initiatives Work Loss Data Institute / ODG ken@worklossdata. com 917 -270 -3921 30
- Slides: 30