William E Boden MD FACC FAHA Medical Therapy

William E. Boden, MD, FACC, FAHA Medical Therapy Should Work Well for Professor of Medicine, Albany Medical College Patients with Documented Ischemia Chief of Medicine, Stratton VA Medical Center Why Guideline-Directed Medical Therapy Vice-Chairman, Department of Medicine Has Altered Therapeutic Landscape Albany the Medical Center, Albany, NY Cardiovascular Research Technology 2013 Washington, D. C. February 25, 2013
An SIHD Patient with CCS 2 Angina & 1. 5 mm ST ↓ at 9. 5 min ETT Exercise Is this a benign lesion in a benign condition?

Dual Goals for Management of Stable Ischemic Heart Disease (SIHD) Prevent MI and Death (Disease Modification) Improve “Quantity of Life” Reduce Ischemia & Relieve Anginal Symptoms Improve “Quality of Life” Boden WE. Medical management of chronic coronary disease. Am J Cardiol. 2008; 101: 69 D 74 D. Gibbons RJ et al. Circulation. 2003; 107: 149 -158. http: //acc. org/qualityandscience/clinical/guidelines/stable_clean. pdf.

Pharmacologic Therapy in SIHD: 2000 Disease-Modifying Therapy Symptomatic Treatment for Angina/Ischemia Control • Aspirin • Beta-blockers w/o MI • Statins • Calcium antagonists • ACE inhibitors and/or ARBs • Nitrates • Beta-blockers Post-MI Boden WE et al. N Engl J Med. 2007; 356: 1503 -1516.

Pharmacologic Rx in SIHD: 2013… A Moving Target—and Improving! Disease-Modifying Therapy Symptomatic Treatment for Angina/Ischemia Control • Aspirin • Beta-blockers w/o MI • Thienopyridines • Calcium antagonists • Statins • Nitrates • ACE inhibitors and/or ARBs • Ranolazine • Beta-blocker Post-MI • Ivabradine (in Europe) • Aldosterone Inhibitors • ? Fibrates and Niacin Boden WE et al. N Engl J Med. 2007; 356: 1503 -1516.
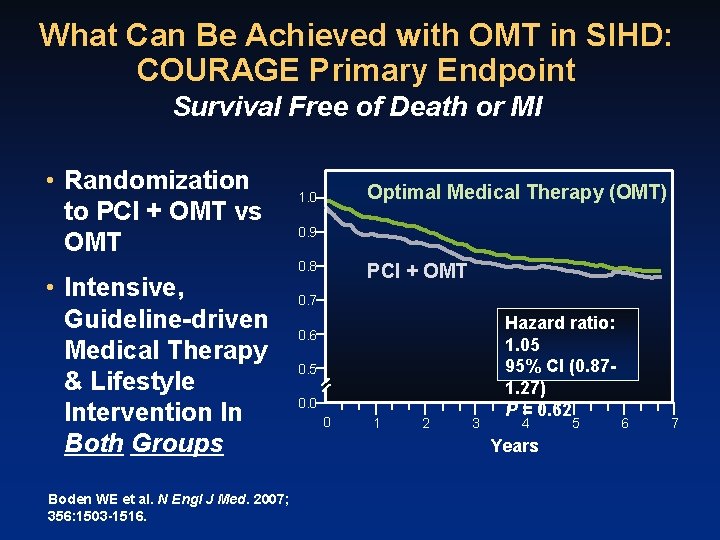
What Can Be Achieved with OMT in SIHD: COURAGE Primary Endpoint Survival Free of Death or MI • Randomization to PCI + OMT vs OMT • Intensive, Guideline-driven Medical Therapy & Lifestyle Intervention In Both Groups Boden WE et al. N Engl J Med. 2007; 356: 1503 -1516. Optimal Medical Therapy (OMT) 1. 0 0. 9 0. 8 PCI + OMT 0. 7 0. 6 0. 5 0. 0 0 1 2 3 Hazard ratio: 1. 05 95% CI (0. 871. 27) P = 0. 62 4 Years 5 6 7
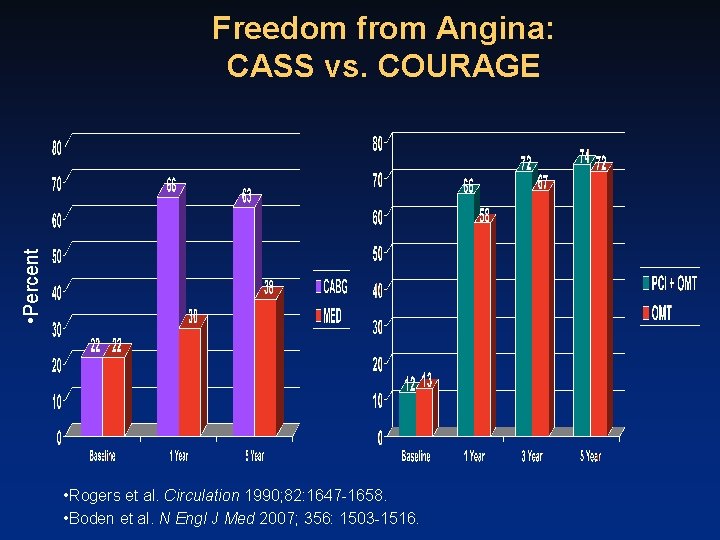
• Percent Freedom from Angina: CASS vs. COURAGE • Rogers et al. Circulation 1990; 82: 1647 -1658. • Boden et al. N Engl J Med 2007; 356: 1503 -1516.
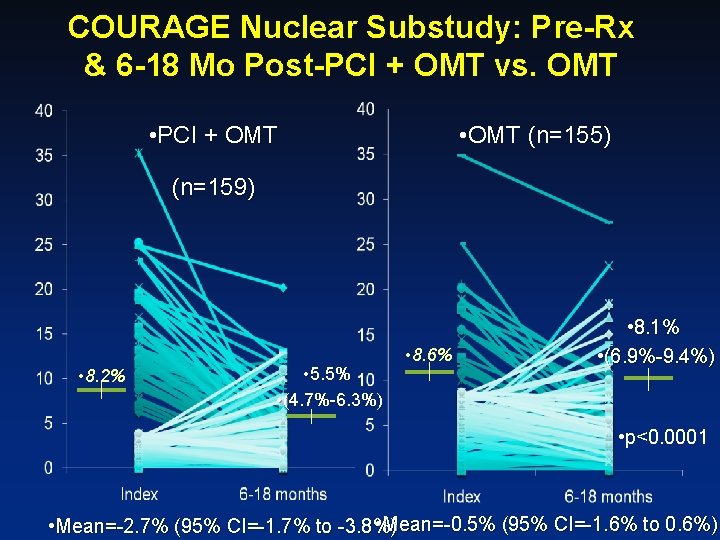
COURAGE Nuclear Substudy: Pre-Rx & 6 -18 Mo Post-PCI + OMT vs. OMT • OMT (n=155) • PCI + OMT (n=159) • 8. 2% • 5. 5% • (4. 7%-6. 3%) • 8. 6% • 8. 1% • (6. 9%-9. 4%) • p<0. 0001 • Mean=-0. 5% (95% CI=-1. 6% to 0. 6%) • Mean=-2. 7% (95% CI=-1. 7% to -3. 8%)
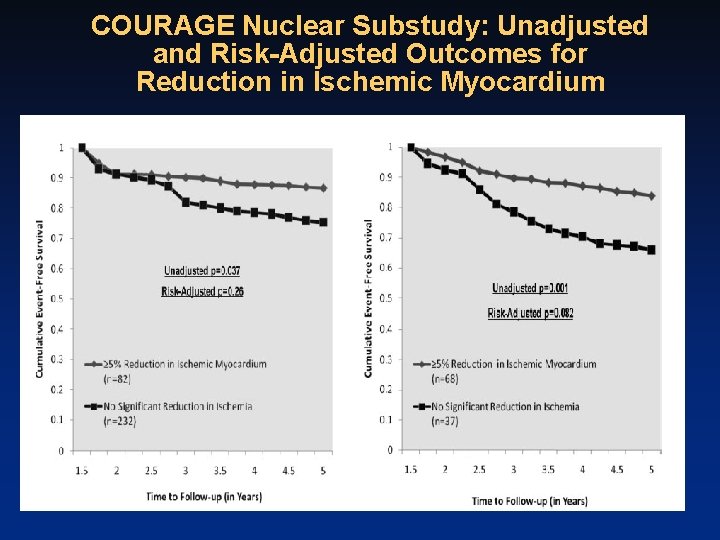
COURAGE Nuclear Substudy: Unadjusted and Risk-Adjusted Outcomes for Reduction in Ischemic Myocardium
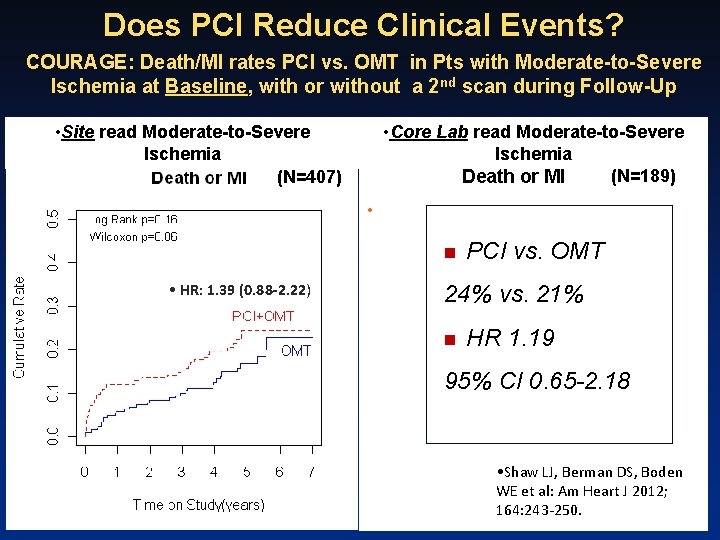
Does PCI Reduce Clinical Events? COURAGE: Death/MI rates PCI vs. OMT in Pts with Moderate-to-Severe Ischemia at Baseline, with or without a 2 nd scan during Follow-Up • Site read Moderate-to-Severe Ischemia (N=407) • Core Lab read Moderate-to-Severe Ischemia (N=189) Death or MI • n • HR: 1. 39 (0. 88 -2. 22) PCI vs. OMT 24% vs. 21% n HR 1. 19 95% CI 0. 65 -2. 18 • Shaw LJ, Berman DS, Boden WE et al: Am Heart J 2012; 164: 243 -250.
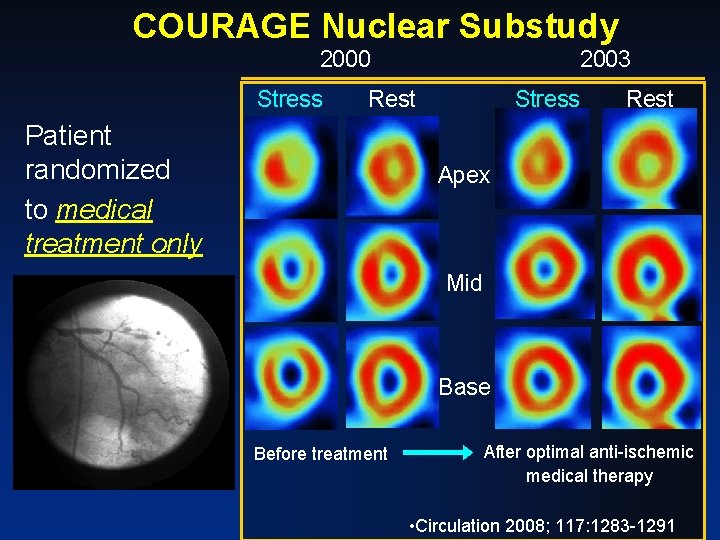
COURAGE Nuclear Substudy 2000 Stress 2003 Rest Patient randomized to medical treatment only Stress Rest Apex Mid Base Before treatment After optimal anti-ischemic medical therapy • Circulation 2008; 117: 1283 -1291
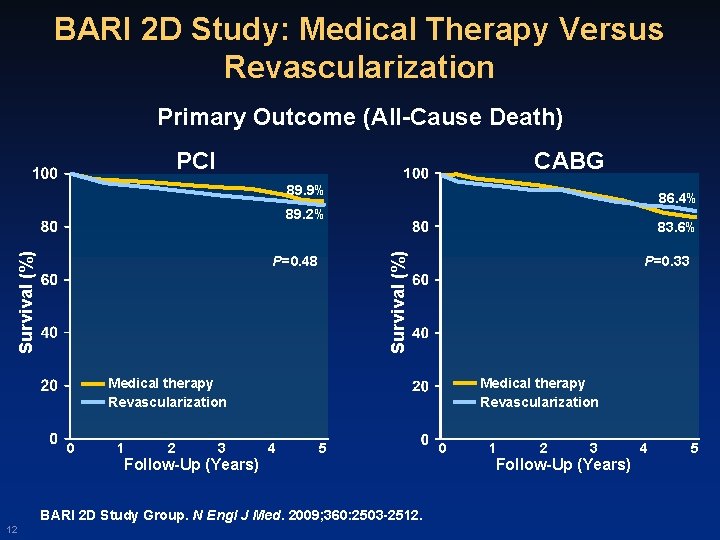
BARI 2 D Study: Medical Therapy Versus Revascularization Primary Outcome (All-Cause Death) CABG PCI 89. 9% 86. 4% 83. 6% Survival (%) 89. 2% P=0. 48 P=0. 33 Medical therapy Revascularization 0 1 2 3 4 5 Follow-Up (Years) BARI 2 D Study Group. N Engl J Med. 2009; 360: 2503 -2512. 12 0 1 2 3 Follow-Up (Years) 4 5
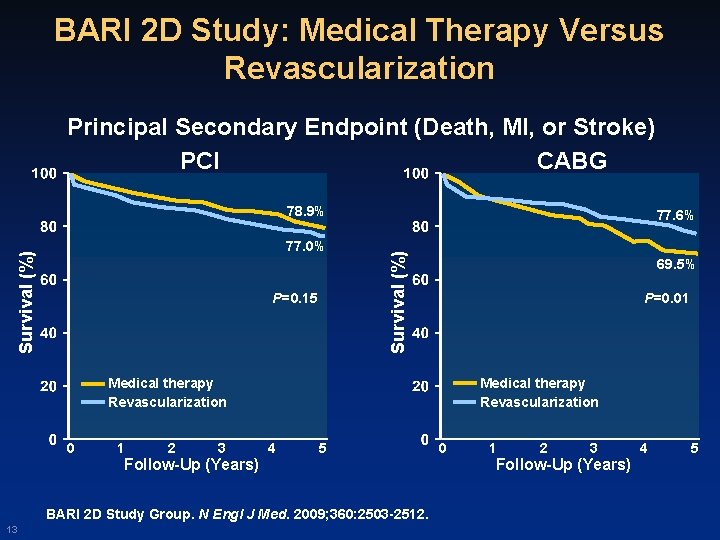
BARI 2 D Study: Medical Therapy Versus Revascularization Principal Secondary Endpoint (Death, MI, or Stroke) CABG PCI 78. 9% P=0. 15 Survival (%) 77. 0% 77. 6% 69. 5% P=0. 01 Medical therapy Revascularization 0 1 2 3 4 5 Follow-Up (Years) BARI 2 D Study Group. N Engl J Med. 2009; 360: 2503 -2512. 13 0 1 2 3 Follow-Up (Years) 4 5

1. 2. De Bruyne BD et al. N Engl J Med. 2012 (published online Aug. 28) Boden WE et al. N Engl J Med. 2012 (published online Aug. 28)
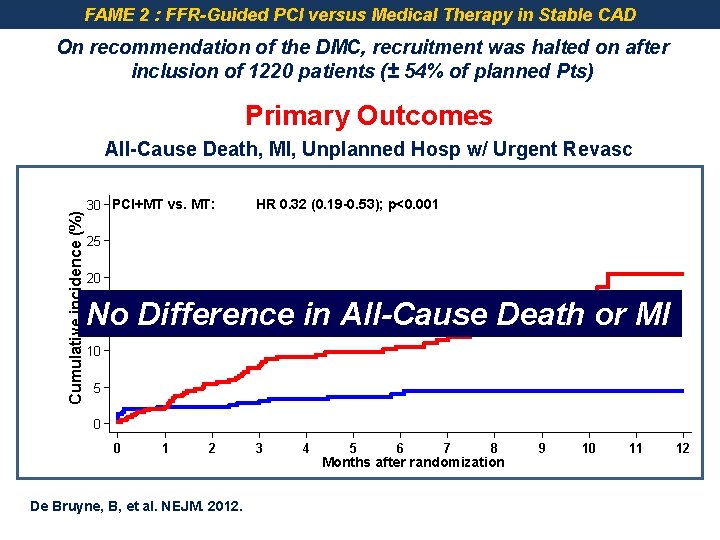
FAME 2 : FFR-Guided PCI versus Medical Therapy in Stable CAD On recommendation of the DMC, recruitment was halted on after inclusion of 1220 patients (± 54% of planned Pts) Primary Outcomes Cumulative incidence (%) All-Cause Death, MI, Unplanned Hosp w/ Urgent Revasc 30 PCI+MT vs. MT: HR 0. 32 (0. 19 -0. 53); p<0. 001 25 20 15 No Difference in All-Cause Death or MI 10 5 0 0 1 2 De Bruyne, B, et al. NEJM. 2012. 3 4 5 6 7 8 Months after randomization 9 10 11 12
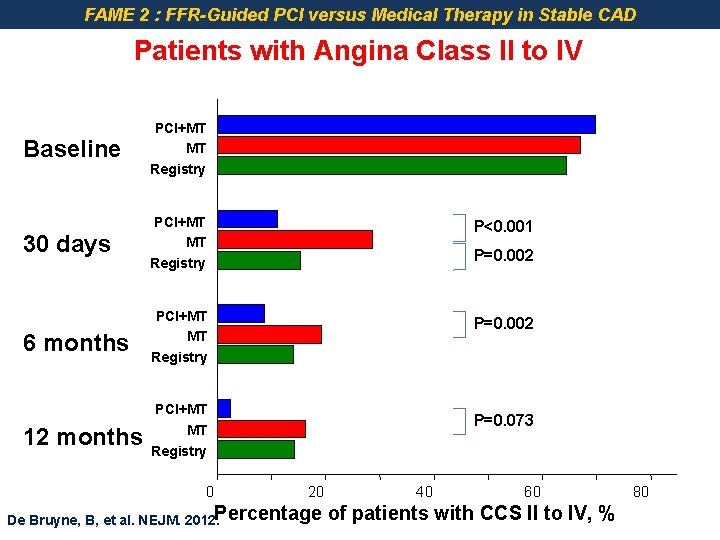
FAME 2 : FFR-Guided PCI versus Medical Therapy in Stable CAD Patients with Angina Class II to IV Baseline PCI+MT MT Registry 30 days PCI+MT MT Registry 6 months PCI+MT MT Registry 12 months PCI+MT MT Registry P<0. 001 P=0. 002 0 P=0. 002 P=0. 073 20 De Bruyne, B, et al. NEJM. 2012. Percentage 40 60 of patients with CCS II to IV, % 80

Limitations of FAME 2 Trial 1 • Only 888 of a planned 1, 600 stable CAD patients were randomized to FFRguided PCI vs. OMT (55% of projected initial sample size) • Trial was stopped early by DSMB due to benefit in FFR-guided stenting group for the composite primary endpoint, but this was driven solely by a lower rate of urgent revasc. rate (1. 6%) in the PCI pts compared to pts on OMT alone with no difference in death or MI • Mean follow-up was only 7 months (projected mean follow-up=24 months), which was too short a time for even restenosis to emerge in PCI pts • In an unblinded trial, an endpoint such as “urgent revasc” (which did not mandate either ECG ischemia or (+) c. Tn. T) could have introduced MD bias • Only 98 patients were followed longer than 12 months, after which there were 0 deaths in either group, and only 2 MIs (both in the PCI group) • OMT was not rigorously used to achieve treatment targets for BP, LDL, Hb. A 1 c, etc. , as in COURAGE 1. Boden WE: Which Is More Enduring: FAME or COURAGE? N Engl J Med. 2012 (published online Aug. 28)

How Superior is PCI to OMT for Angina Relief In the Modern Era of Contemporary Medical Therapy?
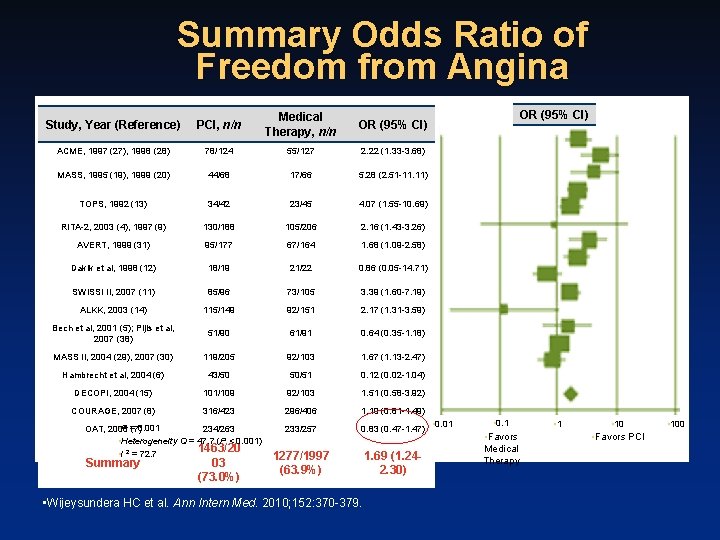
Summary Odds Ratio of Freedom from Angina Study, Year (Reference) PCI, n/n Medical Therapy, n/n OR (95% CI) ACME, 1997 (27), 1998 (28) 78/124 55/127 2. 22 (1. 33 -3. 68) MASS, 1995 (19), 1999 (20) 44/68 17/66 5. 28 (2. 51 -11. 11) TOPS, 1992 (13) 34/42 23/45 4. 07 (1. 55 -10. 69) RITA-2, 2003 (4), 1997 (9) 130/188 105/206 2. 16 (1. 43 -3. 26) AVERT, 1999 (31) 95/177 67/164 1. 68 (1. 09 -2. 58) Dakik et al, 1998 (12) 18/19 21/22 0. 86 (0. 05 -14. 71) SWISSI II, 2007 (11) 85/96 73/105 3. 39 (1. 60 -7. 19) ALKK, 2003 (14) 115/149 92/151 2. 17 (1. 31 -3. 59) Bech et al, 2001 (5); Pijls et al, 2007 (38) 51/90 61/91 0. 64 (0. 35 -1. 18) MASS II, 2004 (29), 2007 (30) 119/205 92/103 1. 67 (1. 13 -2. 47) Hambrecht et al, 2004 (6) 43/50 50/51 0. 12 (0. 02 -1. 04) DECOPI, 2004 (15) 101/109 92/103 1. 51 (0. 58 -3. 92) COURAGE, 2007 (8) 316/423 296/406 1. 10 (0. 81 -1. 49) 233/257 0. 83 (0. 47 -1. 47) 1277/1997 (63. 9%) 1. 69 (1. 242. 30) • P =(7)0. 001 OAT, 2006 234/263 • Heterogeneity Q = 47. 7 (P < 0. 001) 1463/20 • I 2 = 72. 7 Summary 03 (73. 0%) • Wijeysundera HC et al. Ann Intern Med. 2010; 152: 370 -379. OR (95% CI) • 0. 01 • 0. 1 • Favors Medical Therapy • 10 • Favors PCI • 100
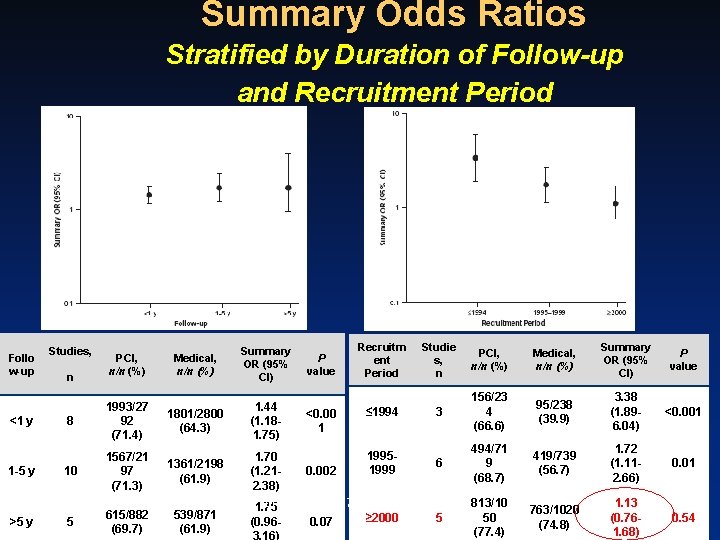
Summary Odds Ratios Stratified by Duration of Follow-up and Recruitment Period Follo w-up <1 y Studies, n 8 PCI, n/n (%) 1993/27 92 (71. 4) Medical, n/n (%) Summary OR (95% CI) 1801/2800 (64. 3) 1. 44 (1. 181. 75) P value <0. 00 1 Recruitm ent Period Studie s, n PCI, n/n (%) Medical, n/n (%) Summary OR (95% CI) P value ≤ 1994 3 156/23 4 (66. 6) 95/238 (39. 9) 3. 38 (1. 896. 04) <0. 001 6 494/71 9 (68. 7) 419/739 (56. 7) 1. 72 (1. 112. 66) 0. 01 5 813/10 50 (77. 4) 763/1020 (74. 8) 1. 13 (0. 761. 68) 0. 54 19951567/21 1. 70 1361/2198 1999 1 -5 y 10 97 (1. 210. 002 (61. 9) (71. 3) 2. 38) • Wijeysundera HC et al. Ann Intern Med. 1. 75 2010; 152: 370 -379. 615/882 539/871 ≥ 2000 >5 y 5 (0. 960. 07 (69. 7) (61. 9)

Why PCI Does Not Reduce Long-Term Events in Stable CAD “Revascularization fixes the lesion and the segment, but not the artery or the patient; OMT reduces clinical

Why Scientific Evidence Supports OMT as an Appropriate Initial Approach to SIHD Patient Management • • • 16 RCTs in 8, 820 patients (including COURAGE, BARI-2 D, & FAME-2) show no difference in death, MI, stroke, or other “hard” CV events between PCI and OMT Aggressive medical therapy & lifestyle intervention without initial PCI can be implemented safely in the majority of SIHD patients— 1/3 of whom may require a symptom-driven procedure over 7 years of F/U, but 2/3 of whom may not require even a first revascularization. This approach incurs no penalty with respect to death, MI, ACS, or need for CABG Although routine PCI + OMT provides some advantages in angina/physical limitation/QOL, these differences are numerically small, not durable, and achieved only at an unattractive cost for chronic disease management
- Slides: 22