Whole Grains and Their Effect on Colorectal Cancer


























- Slides: 27

Whole Grains and Their Effect on Colorectal Cancer Presented by Brad Grubbs, Heather Hennessey, Amber Hill, Rachel Kelley, and Ayako Tabeya

Introducing whole grains Potential benefits • Whole grain consumption is associated with decreased risk of colorectal cancer. WHY? ~ Side effects of the refining process reducing dietary fiber and whole grain content. ~ Whole grains/ dietary fibers contain anti-cancerous components: vitamins, minerals, phytochemicals

Possible Mechanisms of Prevention • Stool bulking- increased fecal bulk and decreased transit time. ~ Allowing less opportunity for fecal mutagens to interact with intestinal epithelium layers. • Dilution of bile acids and colonic carcinogens • Selenium found in whole grain suppresses abnormal cell proliferation • Fermentation produces anticarcinogenic SCFAs • Vitamin E and other antioxidants prevent the formation of carcinogens.

Developing a standard definition As of April 2014 the first standard definition of whole grains was developed, according to the American Society for Nutrition: in order to acquire sufficient whole grains, diets should include 8 g whole grains per 30 g serving while limiting fat, sodium, sugar, and calories.

Currently the average whole grain consumption for both men and women in the United States is at 22 g/day.

Types of Whole Grains In order to be classified as a whole grain, the grain must include the bran, germ, and endosperm. -Rye -Whole wheat -Barley -Oats -Quinoa

Identifying a serving size • Whole grain serving sizes ~ 1 slice of whole grain bread ~ 1 cup whole grain cereal ~ ½ cup cooked whole grains (oats)

Consumer trends and whole grains According to the whole grains council: • In 2006, 68% of surveyed individuals were trying to consume more whole grains. • In 2009 that percentage increased to 81% • Likewise, in 2006, 56% surveyed individuals were trying to reduce consumption of refined grains and in 2009 that number rose to 67%.

Reviewing the literature “Intake of whole grains from different cereal and food sources and incidence of colorectal cancer in the Scandinavian HELGA cohort. ” Hypothesis: Is high whole-grain intake with variety in quantity and sources associated with a decrease in incidence of colorectal cancer in a Scandinavian cohort?

Methods ● This large prospective cohort included 108, 000 male and female Scandinavian subjects ages 40 -63, 1, 123 of which developed colorectal cancers in the 11 yrs of follow-up ● A FFQ was used to gather whole grain data for all part subjects, and a 24 -hr food recall was obtained in addition for 8, 716 subjects. ● Data was analyzed with Cox proportional hazard models with 95% CI.

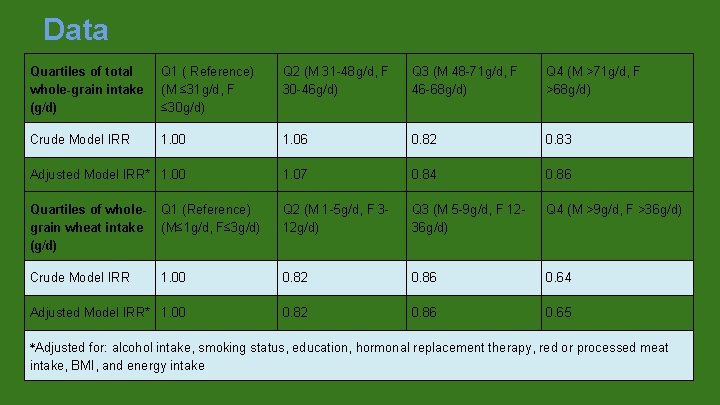
Data Quartiles of total whole-grain intake (g/d) Q 1 ( Reference) (M ≤ 31 g/d, F ≤ 30 g/d) Q 2 (M 31 -48 g/d, F 30 -46 g/d) Q 3 (M 48 -71 g/d, F 46 -68 g/d) Q 4 (M >71 g/d, F >68 g/d) Crude Model IRR 1. 00 1. 06 0. 82 0. 83 Adjusted Model IRR* 1. 00 1. 07 0. 84 0. 86 Quartiles of wholegrain wheat intake (g/d) Q 1 (Reference) (M≤ 1 g/d, F≤ 3 g/d) Q 2 (M 1 -5 g/d, F 312 g/d) Q 3 (M 5 -9 g/d, F 1236 g/d) Q 4 (M >9 g/d, F >36 g/d) Crude Model IRR 1. 00 0. 82 0. 86 0. 64 Adjusted Model IRR* 1. 00 0. 82 0. 86 0. 65 *Adjusted for: alcohol intake, smoking status, education, hormonal replacement therapy, red or processed meat intake, BMI, and energy intake

Results ● The highest whole-grain wheat intake decreased colorectal cancer by an overall IRR of 0. 81 (p-value 0. 0025). ● High total whole-grain product intake decreased the overall IRR to 0. 77 for colorectal cancer(p-value 0. 0112). ● When evaluated by site: ● In men, only colon cancer specifically showed a decrease in relation to a 50 g/d increase in whole-grains (0. 92 IRR). ● In women, only rectal cancer showed a decrease in relation to whole-grain intake (0. 53 IRR).

Grade: II (Fair) • The influence of whole-grain intake on colorectal cancer may vary both by site and gender, so general recommendations are not applicable. • This population consumes significantly higher amounts of whole-grains than in the U. S: 40 g/d in males, 30 g/d in females • FFQ and 24 -hr dietary recall data collection allows for errors in data collection • Short term vs. long term whole-grain consumption

Reviewing the literature Dietary fiber and whole grain consumption in relation to colorectal cancer in the NIH-AARP diet and health study. Objective: To investigate the relationship between dietary fiber and whole grain consumption to colorectal cancer.

Methods • Large prospective cohort design of participants within the National Institute of Health- American Association of Retired Persons living in the following states: California, Florida, Louisiana, New Jersey, North Carolina, and Pennsylvania. • Diet was assessed via 124 food item FFQ of 291988 men and 197623 women between 50 -71 yo. • 2 non consecutive 24 -h recalls were administered on 1953 participants in an attempt to validate the use of the FFQ • The study defined whole grains as 1 serving = 1 slice of whole grain bread or ½ cup cooked whole grains.

Results • 2974 incidences of colorectal cancer were identified during the 5 year follow up. ~ total dietary fiber intake was not associated with colorectal cancer. (p=0. 96) • However, whole grain intake was inversely associated with colorectal cancer risk. p for trend <0. 001, CI: 95% RR: 79% • This implies that increased whole grain consumption can be associated with a modest reduced risk of colorectal cancer

Grade: II (Fair) • Given the sample size (n=489, 611 total), the length of study (5 y), and the P for trend <0. 001. This is a fairly effective study. • The evidence obtained by the study answers the question asked. However, use of the FFQ with its high level of potential error with too few 24 hr recalls to validate the data, makes this studies results less reliable. There is uncertainty attached to the conclusion because of this research design flaw.

Reviewing the literature “Dietary Fibre Intake and Risks of Cancers of the Colon and Rectum in the European prospective Investigation into Cancer and Nutrition (EPIC)” Hypothesis: Does the inverse relationship between dietary fiber intake and colorectal cancer risk remain after a mean follow up of ~11 years in European cohorts?

Methods • • • A total of 521, 448 participants (70% women), mostly aged 35 years or above were recruited between 1990 and 2000 for this large cohort study. Participants were recruited from 23 study centers in ten European countries: Denmark, France, Germany, Greece, Italy, the Netherlands, Norway, Spain, Sweden, and United Kingdom (UK). The final count after exclusions was 477, 312 participants, of which 333, 062 were women and 142, 250 were men. Dietary information over the previous 12 months was obtained at study baseline using country/center specific dietary questionnaires as well as 36, 900 participants completing a standardised computer-based single 24 -hour dietary recall. 4, 517 incident cases of colorectal cancer were documented

Results/Discussion • In calibrated models, a 13% lower (95% confidence interval: 0. 79 -0. 96, P-trend: <0. 001) colorectal cancer risk per 10 g/day increase in total fiber intake was found. • The main source of dietary fiber in most populations is accounted for in cereal fiber, so it made sense that the statistically significant 11% decrease in colorectal cancer risk per 10 g/day of cereal fiber intake was observed.

Results/Discussion (continued) • This analysis of the EPIC cohort strengthens the evidence that dietary fiber is inversely associated with colorectal cancer risk and that the association was of similar magnitude for both men and women. • The conclusion of this study summarizes that after 11 years of follow-up, this analysis confirmed the inverse associations between dietary fiber intake and colorectal cancer. Results strengthen the evidence for the recommendation of increasing the consumption of fiber rich foods for colorectal cancer prevention.

Grade: II (Fair) ● Due to the large sample size(n=477, 312, amongst 23 study centers in ten European countries), the length of the study(mean follow up of 11 y), the large number of colorectal cancer cases(4, 517), and the P-trend<0. 001 for the association between colorectal cancer risk reduction with high intake of dietary fiber. This study was effective. ● The limitations of this study mainly include that the diet was only assessed at baseline, and that dietary changes were unaccounted for during follow-up.

Overall Conclusion • If you are not reaching the recommended amount of fiber or whole grains, increasing your intake would be beneficial in decreasing colorectal cancer risk. • There are discrepancies in the research, however the overall conclusion is that fiber/whole grains will reduce risk from 11 -40%

Overall Grading Grade II: Fair Pros Cons • Large sample sizes • Most showed an inverse association • Not all conclusions showed an inverse association • Two variables: fiber and whole grains • High fiber diets also exercised more and was more educated • Used Food Frequency Questionnaires

Public Health Recommendation We recommend increased daily intake of dietary fibers as a method to moderately decrease the risk of colorectal cancer, especially colon cancer, in both men and women. The Dietary Guidelines for Americans 2010 recommends men age 50 or younger should eat at least 38 grams of fiber per day, men older than 50 years old should eat at least 30 grams a day. For women, age 50 or younger should eat at least 25 grams a day, while women older than 50 year old should eat at least 20 grams a day. These recommendations can be achieved by adding 3 -5 servings of whole grains (48 -80 grams) with other dietary fiber sources, such as beans, fruits, and vegetables.

References Bingham S, Day N, Luben R, Ferrari P, Slimani N, Norat T. Dietary fibre in food and protective against colorectal cancer in the european prospective investigation into cancer and nutrition (EPIC): an observational study. The Lancet. 2003; 361: 1496 -1501 Egeberg R, Olsen A, Loft S, Christensen J, Johnsen NF, Overvad K, and Tjonneland A. Intake of wholegrain products and risk of colorectal cancer in the Diet, Cancer and Health cohort study. BRIT J CANCER. 2010; 103: 730 -734 Ferruzzi M, Jonnalagadda S, Liu S, et al. Developing a Standard Definition of Whole-Grain Foods for Dietary Recommendations: Summary Report of a Multidisciplinary Expert Roundtable Discussion. American Society for Nutrition. 2014; 5: 164 -176. doi: 10. 3945/an. 113. 005223 Fuchs C, Giovannucci E, Colditz G, et al. Dietary fiber and the risk of colorectal cancer and adenoma in women. N Engl J Med 1999; 340: 169 -76 Kyro, Cecilie, Olsen, Anja, Landberg, Rikard, et al. (2013). Plasma alkylresorcinols, biomarkers of whole-grain wheat and rye intake, and incidence of colorectal cancer. Journal of the National Cancer Institute, 106: 1, 1 -9. Retrieved April 10, 2014 from the world wide web: http: //jnci. oxfordjournals. org. ezproxy. library. oregonstate. edu/content/106/1/djt 352 Kyro, Cecilie, Skeie, Guri, Loft, Steffen, et al. (2013). Intake of whole grains from different cereal and food sources and incidence of colorectal cancer in the Scandinavian HELGA cohort. Cancer Causes Control, 24, 1363 -1374. Retrieved April 10, 2014 from the world wide web: http: //www. ncbi. nlm. nih. gov/pubmed/23624874

Larsson S, Giovannucci E, Bergkvist L, Wolk A. Whole grain consumption and risk of colorectal cancer: a population-based cohort of 60 000 women. British Journal of Cancer. 2005; 92: 1803 -1807. Mc. Cullough M, Robertson A, Chao A, Jacobs E, Stampfer M, Jacobs D, Diver W, Calle E, Thun M. A Prospective Study of Whole Grains, Fruits, Vegetables, and Colon Cancer Risk. Cancer Causes and Control. 2003: 14: 959 -970. Schatzkin A, Mouw T, Park Y, Subar AF, Kipnis V, Hollenbeck A, Leitzmann MF, Thompson FE. Dietary fibre and whole grain consumption in relation to colorectal cancer in the NIH-AARP diet and health study. Am J Clin Nurr. 2007; 85: 1353 -1360 Uchida K, Kono S, Terasaka R, et al. Dietary fiber, source foods and colorectal cancer risk: The Fukuoka Colorectal Cancer Study. Scand J Gastroentero 2010; 45: 1223 -1231 U. S. Department of Agriculture and U. S. Department of Health and Human Services. Dietary Guidelines for Americans, 2010. 7 th Edition, Washington, DC: U. S. Government Printing Ofice, December 2010. Whole Grain Council. 2013. http: //wholegrainscouncil. org/newsroom/whole-grain-statistics Williams DC, Satina JA, Adair LS, Stevens J, Galanko J, Keku TP, and Sandler RS. Dietary Patterns, Food Groups, and rectal cancer risk in Whites and African Americans. Cancer Epidem Biomar. 2009; 18: 1552 -1561 Wakai K, Date C, Fukui M, Tomakoshi K, Watanabe Y, Hayakawa N, et. al. (2007). Dietary Fiber and Risk of Colorectal Cancer in the Japan Collaborative Cohort Study. Cancer Epidemiol. Biomarkers Prev. (4): 668 -75