WHO Technical Briefing seminar Geneva 01 05 November

WHO Technical Briefing seminar Geneva, 01 – 05 November 2010. Access Framework & Challenges in Medicines Supply Systems Mrs Helen Tata (WHO/EMP) 1| Helen Tata: WHO-TBS 4 November 2010
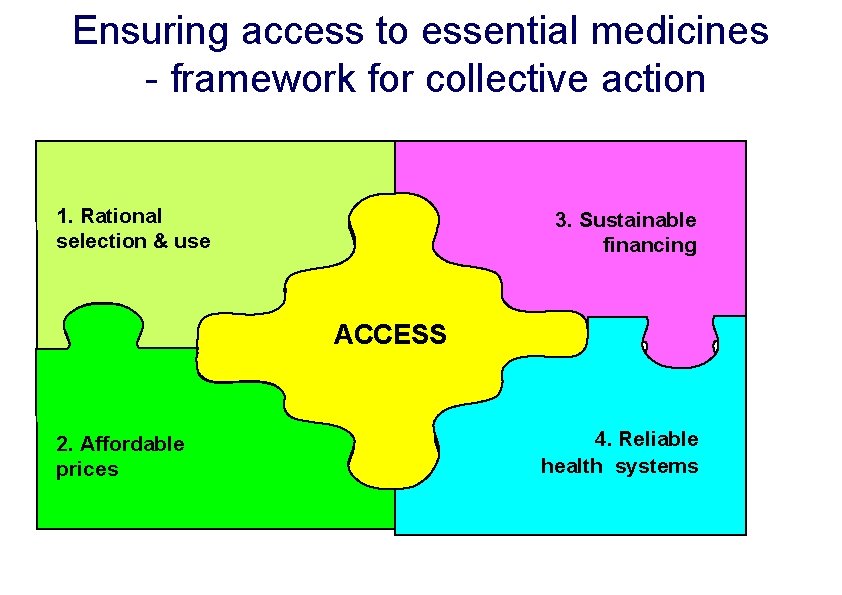
Ensuring access to essential medicines - framework for collective action 1. Rational selection & use 3. Sustainable financing ACCESS 2. Affordable prices 4. Reliable health systems
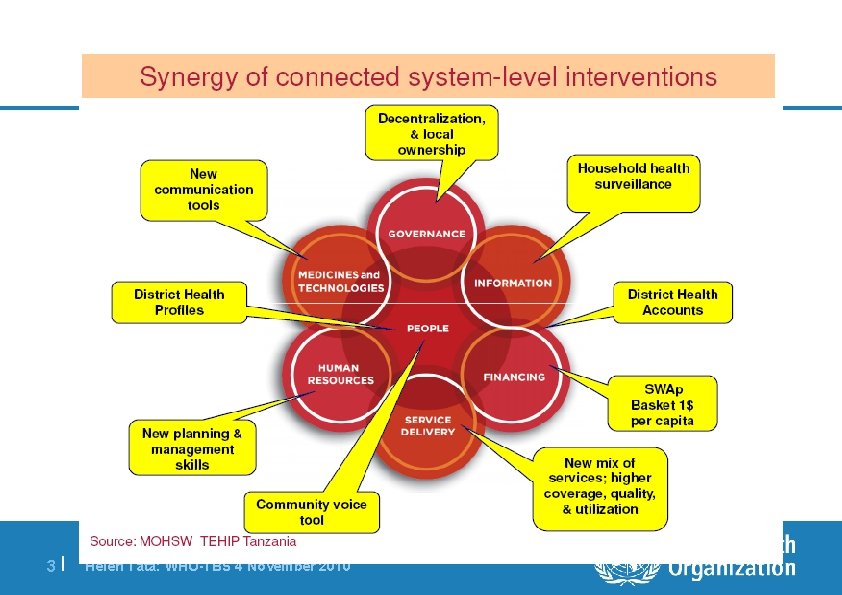
3| Helen Tata: WHO-TBS 4 November 2010

Assessment of medicines supply systems l 2007 AFRO/EDM and HQ/EMP developed tools to support countries in this activity l 1 st stage – Map partners supporting medicines procurement and distribution – Financial flows – Warehousing – Distribution l 2 nd stage l Look at issues around the medicines supply management cycle: – Selection – Procurement – Storage/stock management – Distribution – Financing – MTata: & WHO-TBS E 4 November 2010 4 | Helen

Race to save lives l. The rush 5| Helen Tata: WHO-TBS 4 November 2010

l 6| Source: Bergis Schmidt-Ehry, GTZ Helen Tata: WHO-TBS 4 November 2010
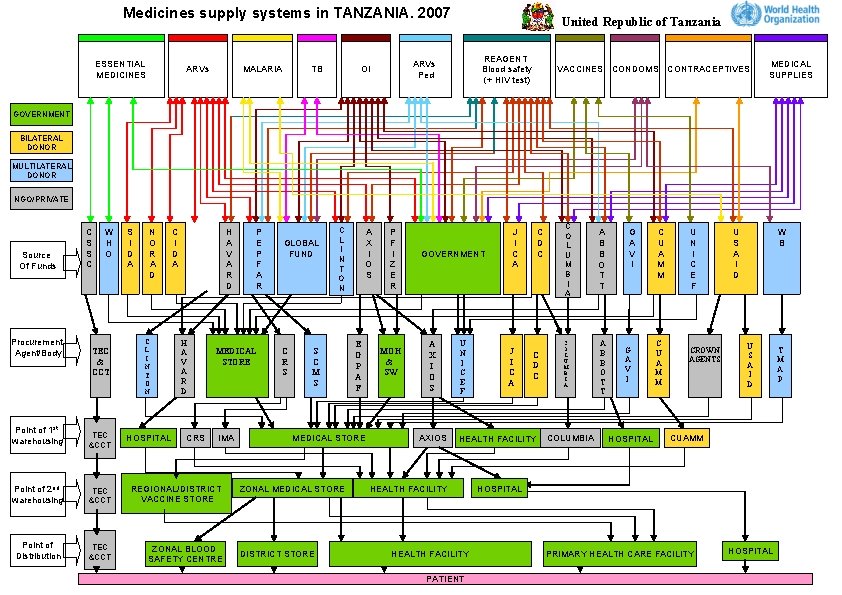
Medicines supply systems in TANZANIA. 2007 ESSENTIAL MEDICINES ARVs MALARIA TB United Republic of Tanzania REAGENT Blood safety (+ HIV test) ARVs Ped OI VACCINES CONDOMS CONTRACEPTIVES MEDICAL SUPPLIES GOVERNMENT BILATERAL DONOR MULTILATERAL DONOR NGO/PRIVATE Source Of Funds Procurement Agent/Body C S S C W H O TEC & CCT S I D A N O R A D C L I N T O N C I D A H A V A R D MEDICAL STORE Point of 1 st warehousing TEC &CCT Point of 2 nd warehousing TEC &CCT REGIONAL/DISTRICT VACCINE STORE Point of Distribution TEC &CCT ZONAL BLOOD SAFETY CENTRE HOSPITAL CRS P E P F A R IMA GLOBAL FUND C R S C L I N T O N S C M S A X I O S E G P A F MEDICAL STORE ZONAL MEDICAL STORE DISTRICT STORE P F I Z E R MOH & SW GOVERNMENT A X I O S AXIOS U N I C E F J I C A C D C HEALTH FACILITY PATIENT C O L U M B I A COLUMBIA A B B O T T G A V I HOSPITAL C U A M M U N I C E F CROWN AGENTS U S A I D W B U S A I D CUAMM HOSPITAL PRIMARY HEALTH CARE FACILITY HOSPITAL T M A P
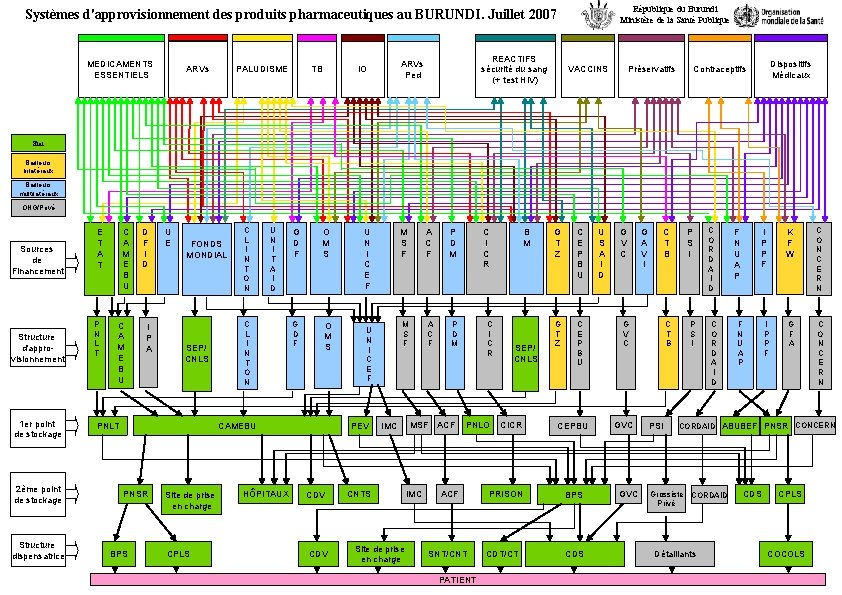
République du Burundi Ministère de la Santé Publique Systèmes d'approvisionnement des produits pharmaceutiques au BURUNDI. Juillet 2007 MEDICAMENTS ESSENTIELS ARVs PALUDISME TB REACTIFS sécurité du sang (+ test HIV) ARVs Ped IO VACCINS Préservatifs Dispositifs Médicaux Contraceptifs Etat Bailleurs bilatéraux Bailleurs multilatéraux ONG/Privé Sources de Financement Structure d'approvisionnement 1 er point de stockage 2ème point de stockage Structure dispensatrice C A M E B U E T A T P N L T C A M E B U D F I D I P A U E FONDS MONDIAL SEP/ CNLS C L I N T O N U N I T A I D C L I N T O N G D F O M S CAMEBU PNLT PNSR BPS Site de prise en charge CPLS HÔPITAUX U N I C E F PEV CDV M S F A C F P D M C I C R IMC CNTS Site de prise en charge MSF ACF IMC PNLO ACF SNT/CNT PATIENT B M SEP/ CNLS CICR PRISON CDT/CT G T Z C E P B U CEPBU BPS CDS U S A I D G V C G A V I C T B P S I G V C GVC PSI C O R D A I D F N U A P I P P F K F W C O N C E R N I P P F G F A C O N C E R N F N U A P CORDAID ABUBEF PNSR CONCERN Grossiste CORDAID Privé Détaillants CDS CPLS COCOLS

Partner store within national store

National Medicines stores l

Challenges (1) l Selection: – Supply outside the EML/STG still exists – Procurement of non registered medicines in countries still exists l Quantification: – CMS not always involved in forecasting/procurement – No coordination in quantification between Mo. H, CMS, partners resulting in: • stock-outs or • overstocking • expired products – Inadequate logistic information system 11 | Helen Tata: WHO-TBS 4 November 2010

Challenges (2) l Procurement: – Managed by various partners present in country. – National system hardly involved in program procurement Storage/stock management: – Inadequate storage capacity due to lack of coordination in procurement planning – Different stock management tools for the same product originating from different partners l Distribution: – Inadequate funds for distribution. – Uncoordinated distribution between different programs leading to high operational costs for all programs. 12 | Helen Tata: WHO-TBS 4 November 2010

Challenges (3) Financing: – Funds available mainly for 3 disease programs – Other areas under funded – Financial figures not always available – Logistic support is under- funded Monitoring-Evaluation: – Each program may have a stand alone M&E – Different reporting tools – Burden of work for scare human resource at periphery high 13 | Helen Tata: WHO-TBS 4 November 2010

What can we do? 14 | Helen Tata: WHO-TBS 4 November 2010

Source: Bergis Schmidt-Ehry, GTZ 15 | Helen Tata: WHO-TBS 4 November 2010

Source: Bergis Schmidt-Ehry, GTZ 16 | Helen Tata: WHO-TBS 4 November 2010

Benefits ØPlatform for dialogue, information sharing and coordination ØJoint M & E and reporting ØReduced workload ØHealth System strengthening ØTimely delivery of medicines to target population ØCost savings 17 | Helen Tata: WHO-TBS 4 November 2010

Expectations l Adequate funding to medicines for priority disease to support distribution of all other categories of medicines l Stock management tools for medicines from various sources streamlined l No stock outs in any health facility l Un-interrupted access to medicines! 18 | Helen Tata: WHO-TBS 4 November 2010

Recap ØCoordination, dialogue, information sharing ØJoint M & E and reporting ØReduced workload ØHealth System strengthening ØTimely delivery of medicines to target population ØCost savings 19 | Helen Tata: WHO-TBS 4 November 2010

Source: Bergis Schmidt-Ehry, GTZ 20 | Helen Tata: WHO-TBS 4 November 2010
- Slides: 20