Which Procedure Need Prophylaxis for DVT After Trauma

















- Slides: 21

Which Procedure Need Prophylaxis for DVT, After Trauma H Fanian Isfahan University of Medical Sciences

Thromboembolic Events After Trauma • Venous thromboembolic events (VTEs) are common life-threatening complications after trauma • While DVT may present clinically silent, PE is the third most common cause of death in patients that survive the first 24 hours after trauma • Increase survival of severely injured patients together with aging population may implicate an increasing risk of VTEs after trauma • • • 450, 375 patients, 1602(0. 36%) had a VTE, 998 (62. 8%) DVT, 522 (31. 7%) PE, 82 (5. 5%) both 536, 423 children after trauma, 1141 (0. 2%) VTE 2/3 of all VTE occurred during the first 3 weeks after trauma 62% cases developed VTE after hospital discharge Most trauma centre have developed protocols for VTE prophylaxis

VTE after Trauma q. Major-trauma is a hypercoagulable state often complicated by VTE & syndrome of "micro-thrombosis" q. Tissue factor & markers of thrombin generation increase q. Levels of natural anticoagulants such as antithrombin, protein C & protein S are reduced

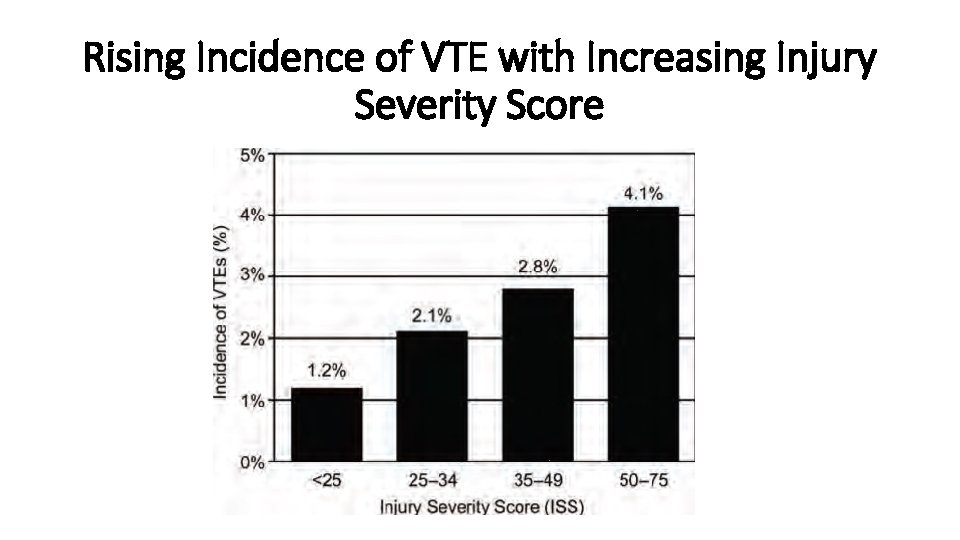
Rising Incidence of VTE with Increasing Injury Severity Score

DVT in Fractures Trauma in general & skeletal trauma in particular are strong risk factor for DVT Incidence of DVT is higher with proximal extremity fractures than with distal extremity fractures Femoral shaft 40%, tibia plateau 43%, tibia shaft 22%, tibia pilon 12. 5% Longer times before fracture fixation

VTEs & Risk Factors 1231 Patients Treated for VTE • No patient had lacked any risk factor for DVT • 11% had only one risk factor • Half of the patients had at least four risk factors Lijfering WM. BJH 2010; 149(6): 824 -33 Risk factors for venous thrombosis Many people have several of these risk factors but never develop thrombosis; others suffer from thrombosis but have none

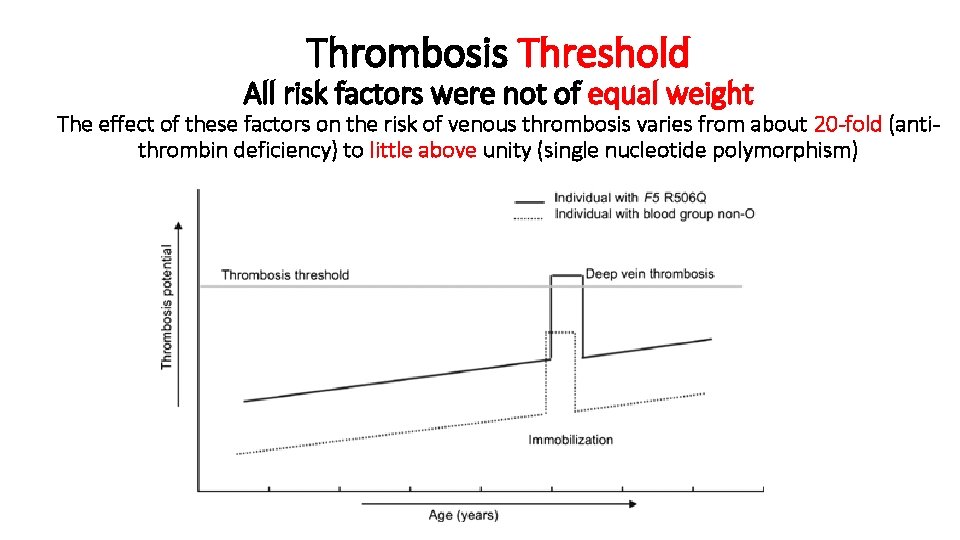
Thrombosis Threshold All risk factors were not of equal weight The effect of these factors on the risk of venous thrombosis varies from about 20 -fold (antithrombin deficiency) to little above unity (single nucleotide polymorphism)

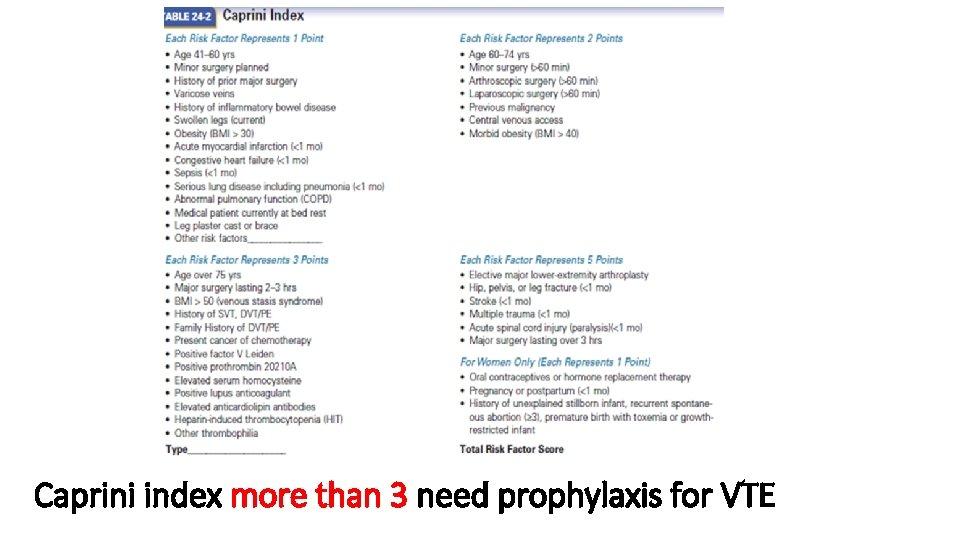
Caprini index more than 3 need prophylaxis for VTE

Caprini Venous Thromboembolism Risk Assessment Score J Vasc Surg Venous Lymphat Disord. 2016 Apr; 4(2): 153 -60. doi: 10. 1016/j. jvsv. 2015. 09. 004. Epub 2015 Nov 6. • Incidence of DVT was 2% in patients with a Caprini score of 5 to 8 • 26% in patients with scores of 9 to 11 • 65% in patients with scores of 12 to 15 • The risk for DVT was increased 18. 7 -fold for patients with scores of 9 to 11 and 98. 4 -fold for scores of 12 to 15 compared with patients with scores of 5 to 8 • Caprini score of 11 was the cutoff point (extremely high risk & need a more effective prophylactic regimen)

Classification of Risk Factors for First Thrombosis Long list of risk factors known today q Genetic (most frequently missed risk factor) q Acquired q Environmental (trauma, surgery, Immobilisation) q Mixed (mixture of such origins) q Not well established Absolute vs. relative, provoked vs. no provoked, preventable vs. no preventable, strong vs. weak

Trauma-Related Risk Factors Associated with VTE I 1. 2. 3. 4. 5. 6. 7. 8. 9. Head injury Spinal cord injury 5 points Lower-extremity fracture 5 points Pelvic fracture 5 points Patients requiring transfusion AIS (Abbreviated Injury Scale)>3 Venous injury Shock on admission (BP<90 mm Hg) Minor surgery one point, minor surgery >60 min two point, & major surgical procedure lasting 2 -3 hrs, three points but major surgery lasting over 3 hrs five points 10. Sepsis (<one mo)

Trauma-Related Risk Factors Associated with VTE II 11. Single or multiple organ failure 12. Time from injury to admission (72 hours) 13. Ventilator days >3 14. ICU admission 16. Central venous lines 17. Hypoxemia 18. ………….

Nontraumatic Risk Factors for DVT I 1. Age (41 -60 yrs one point, 60 -74 yrs two point, over 75 yrs five point) 2. Co-morbidities (diabetes, renal failure, congenital or acquired coagulation disorders & malignancies) 3. History of major surgery 4. Varicose veins 5. History of inflammatory bowel disease 6. Swollen leg >3 cm compared with asymptomatic leg 7. Obesity (BMI> 30 one point, morbid obesity, or BMI>40 two point, BMI >50 three points) 8. Acute myocardial infarction 9. Congenital heart failure(<one mo) 10. Serious lung disease including pneumonia(<one mo)

Nontraumatic Risk Factors for DVT II 11. Abnormal pulmonary function 12. Medical patient currently at bed rest 13. Stroke (<one mo) 14. History of SVT, DVT/PE 15. Family history of DVT/PE 16. Present cancer of chemotherapy 17. Positive factor V Leiden 18. Positive prothrombin 20210 A 19. Elevated serum homocysteine 20. Positive lupus anticoagulant

Nontraumatic Risk Factors for DVT III 21. Elevated anticardiolipin antibodies 22. Heparin-induced thrombocytopenia 23. Other thrombophilia 24. Oral contraceptives or hormone replacement therapy 25. Pregnancy or postpartum (<one mo) 26. History of unexplained stillborn infant recurrent spontaneous abortion (>3 mo) premature birth with toxemia or growth-restricted infant

DVT in Pelvic & Acetabular Fractures Ø Usually result from high-energy trauma, associated with injury to vascular structures and oblige prolonged immobilisation Ø Traumatic radicular lesions, limb fractures, anaesthesia, or pain, will weaken the calf pump and contribute to vascular stasis Ø Surgical techniques may promote tissue necrosis or direct vascular damage

Spinal Cord Injury • A meta-analysis by Rogers et al. found patients with spinal injury or spinal fracture to be the highest risk to develop VTE • Thromboembolic events have been reported in 70 -100% of patients with complete spinal cord injury due to complete motor paralysis • In sub-acute or chronic phase of spinal cord injury, incidence of DVT increases

Incidence of VTE in Children after Trauma Risk of VTE is low among young patients, occurring in 0. 1% of patients 12 years or younger, but increased to 0. 3% in patients aged 13 to 15 years and to 0. 8% in patients 16 years or older

Risk Factors in Children q. Central venous line (previous or existing) q. Poor perfusion q. Deep sedation q. Immobility q. Neuromuscular blockade q. Parenteral nutrition

The "High-Risk" DVT Screening Protocol for Trauma Patients- Is it Practical J. Trauma Acute Care Surg. 2015 Dec; 79(6): 970 -5 May not to be practical or cost-effective for Trauma patients

Thank You For Your Attention