When is IBD not necessarily the IBD you

When is IBD not necessarily the IBD you thought it was by Dr Matt W. Johnson

Topics of Discussion • Proctitis • Sigmoiditis

Proctitis • • Definition = Inflammation of the lower 15 cm of rectum = E 1 Symptoms can vary greatly, but include; - • • Painful defaecation Soreness in the ano-rectal region Sense of incomplete evacuation + Tenesmus Involuntary spasms and cramping during bowel movements Bleeding, and possibly a discharge. Involuntary straining Proximal constipation

Physical Assessment • • • Anal + Rectal erythema + oedematous mucosa Injected mucosa Ano-Rectal erosions or ulcers Blood or Mucus on stools Mucopurulent or blood-stained rectal discharge

BSG - Treatment • • 1 st Line = Topical 5 ASA 2 nd Line = Topical Steroids 3 rd Line = PO 5 ASAs or Steroids Antibiotics Immunomodulators Surgery Carter MJ. Gut 2004; 53: v 1 -v 16 on behalf of the IBD Section of the BSG Regueiro MD. Clin Gastroenterol. 2004 Oct; 38(9): 733 -40.

• IBD Differential Diagnoses Proctitis • • Non specific, self resolving Food allergy Solitary rectal ulcer syndrome Post-Infectious (eg. CDT, Campylobacter, Shigella, Escherichia coli, Salmonella, and amebiasis) STDs (HSV, HIV, Syphilis, LGV, Gonorrhoea, Chancroid, TB) Trauma XR + Ischaemia + Drug induced (NSAIDS) Sigmoiditis • Diverticular disease associated colitis
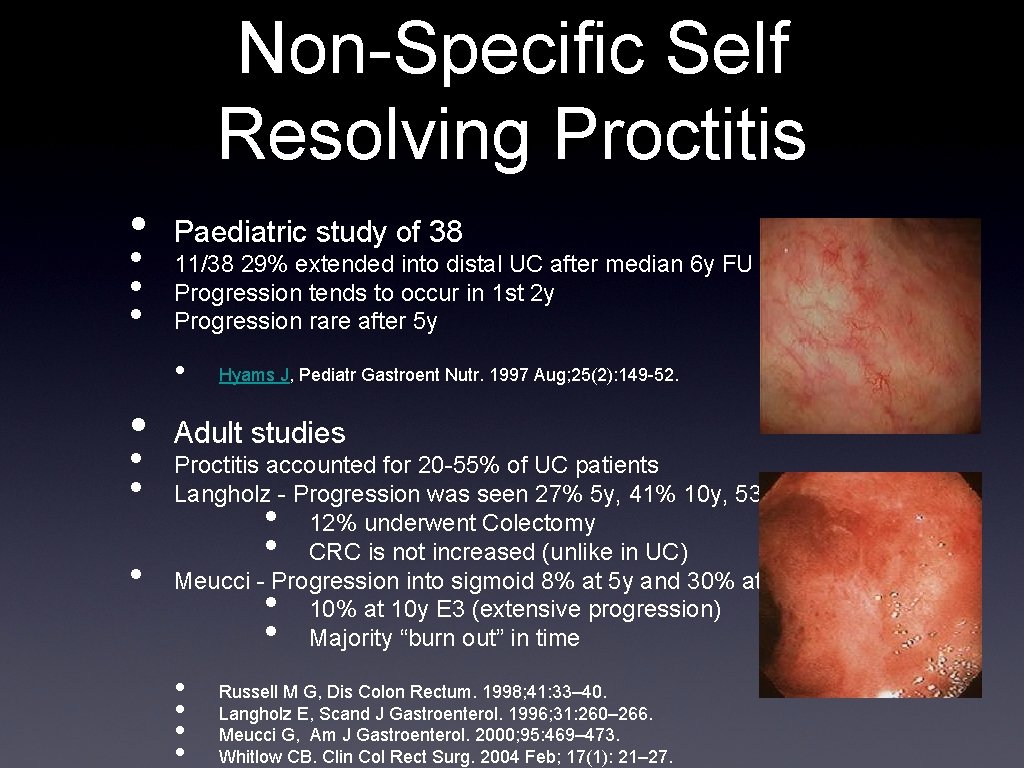
Non-Specific Self Resolving Proctitis • • Paediatric study of 38 11/38 29% extended into distal UC after median 6 y FU Progression tends to occur in 1 st 2 y Progression rare after 5 y • • • Hyams J, Pediatr Gastroent Nutr. 1997 Aug; 25(2): 149 -52. Adult studies Proctitis accounted for 20 -55% of UC patients Langholz - Progression was seen 27% 5 y, 41% 10 y, 53% 15 y 12% underwent Colectomy CRC is not increased (unlike in UC) Meucci - Progression into sigmoid 8% at 5 y and 30% at 10 y 10% at 10 y E 3 (extensive progression) Majority “burn out” in time • • Russell M G, Dis Colon Rectum. 1998; 41: 33– 40. Langholz E, Scand J Gastroenterol. 1996; 31: 260– 266. Meucci G, Am J Gastroenterol. 2000; 95: 469– 473. Whitlow CB. Clin Col Rect Surg. 2004 Feb; 17(1): 21– 27.

Allergic Proctitis • • Markedly increased number of Ig. E containing cells in the lamina propria of rectal mucosa biopsies. 8/12 were sucessfully treated with disodium cromoglycate (DSCG). The remaining 4 had mild proctitis and did not require Rx. P C Rosekrans, GUT 1980 December; 21(12): 1017– 1023. Diagnosis requires objective improvement on withdrawing suspected food Ag and recurrence with subsequent reintrduction
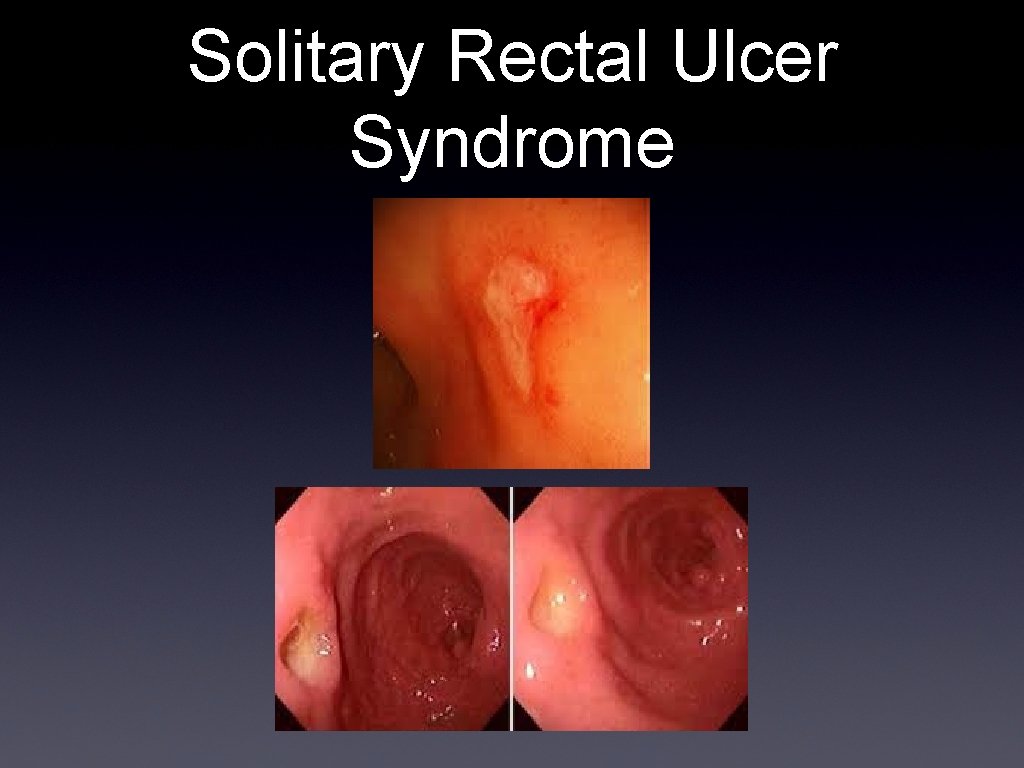
Solitary Rectal Ulcer Syndrome
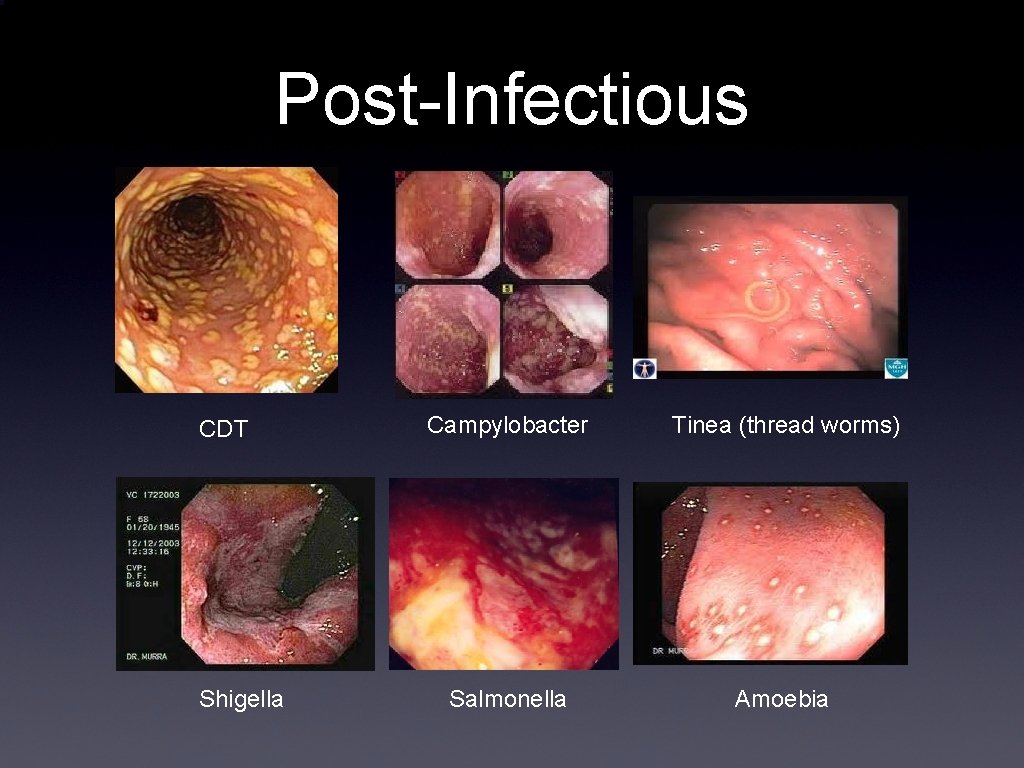
Post-Infectious CDT Shigella Campylobacter Tinea (thread worms) Salmonella Amoebia

STDs • • • 10% of S. London men have paid for sex 18% of US men have had unprotected anal sex Causes • • 45% no STDs Gonorrhoea 20% - 50% are asymptomatic Herpes 13% - Very painful Chlamydia 11% Syphillis 9% Mixed 8% BSG 2005 - Snail track ulcers, condylomata lata
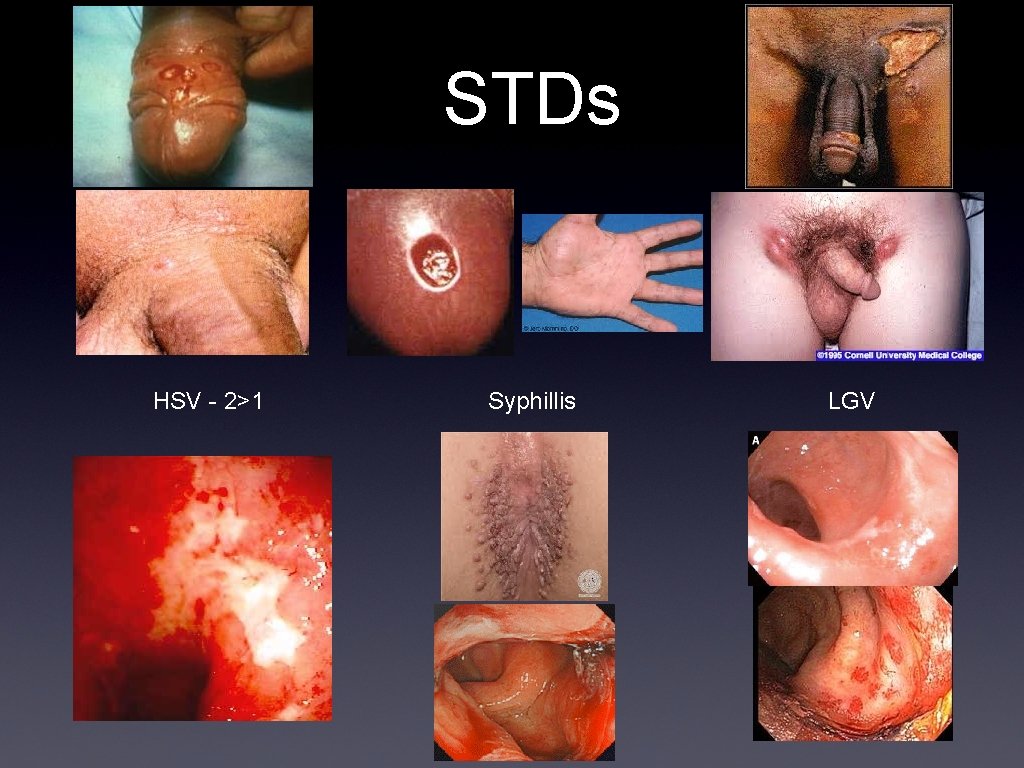
STDs HSV - 2>1 Syphillis LGV

STDs HIV Gonorrhoea Chancroid

Practicalities • • • Serology HIV 1+2 HSV + HVZ CMV Hep. B Histopathological Staining CMV PCR TB Chlamydia + LGV

STD Ix + Rx Gonorrhoea Ciprofloxacin 500 mg stat Chlamydia Doxycycline 100 mg bd + Azithromycin 1 g stat Syphillis Benzyl Penicillin HSV Aciclovir 400 mg x 5 for 10/7 Empirical Cipro 500 mg or Cefixim 400 mg stat Azithr 1 g stat or Dox 100 mg bd 1 w Aciclovir 400 mg x 5 10/7
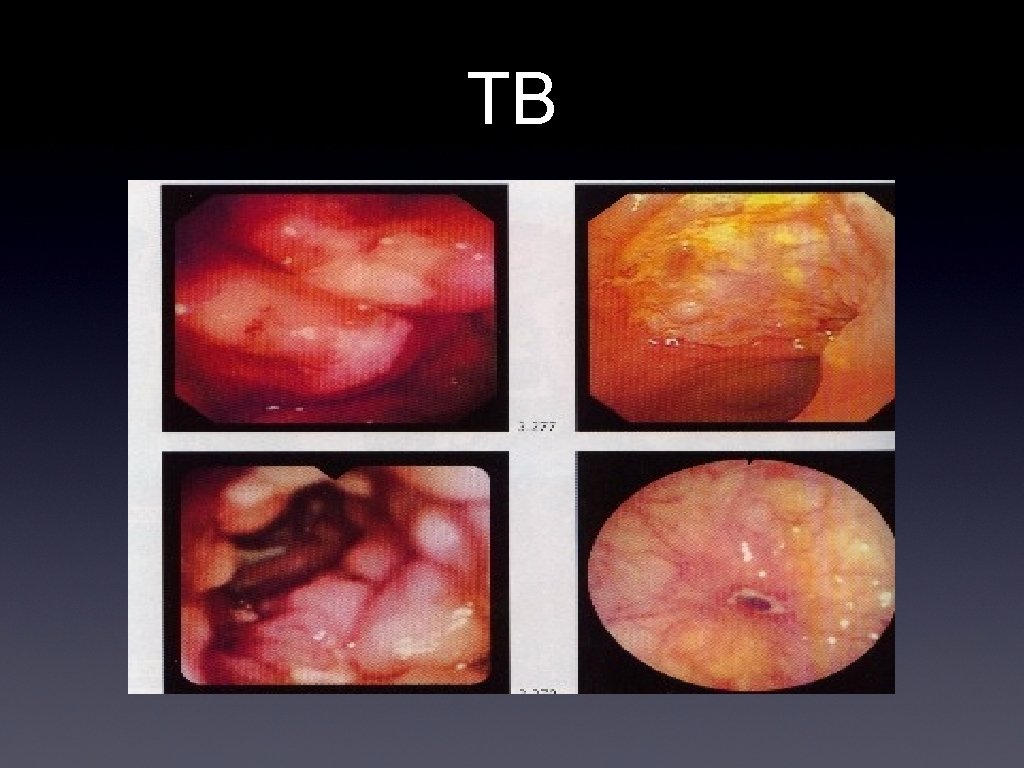
TB
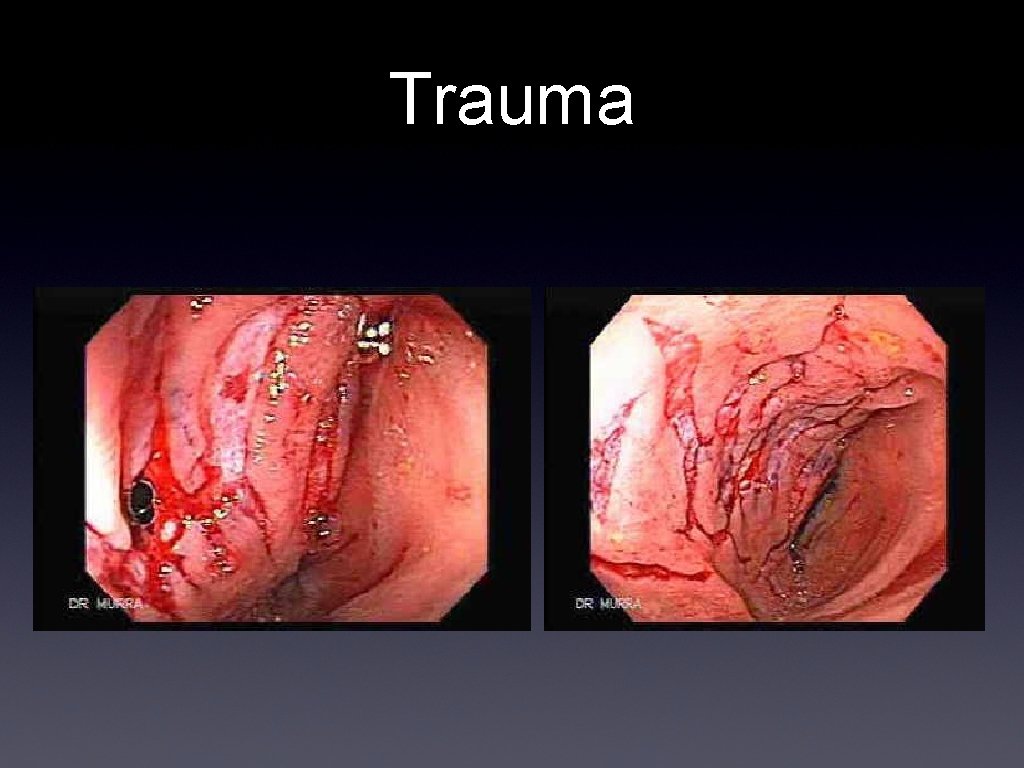
Trauma

XR - Radiation Proctography
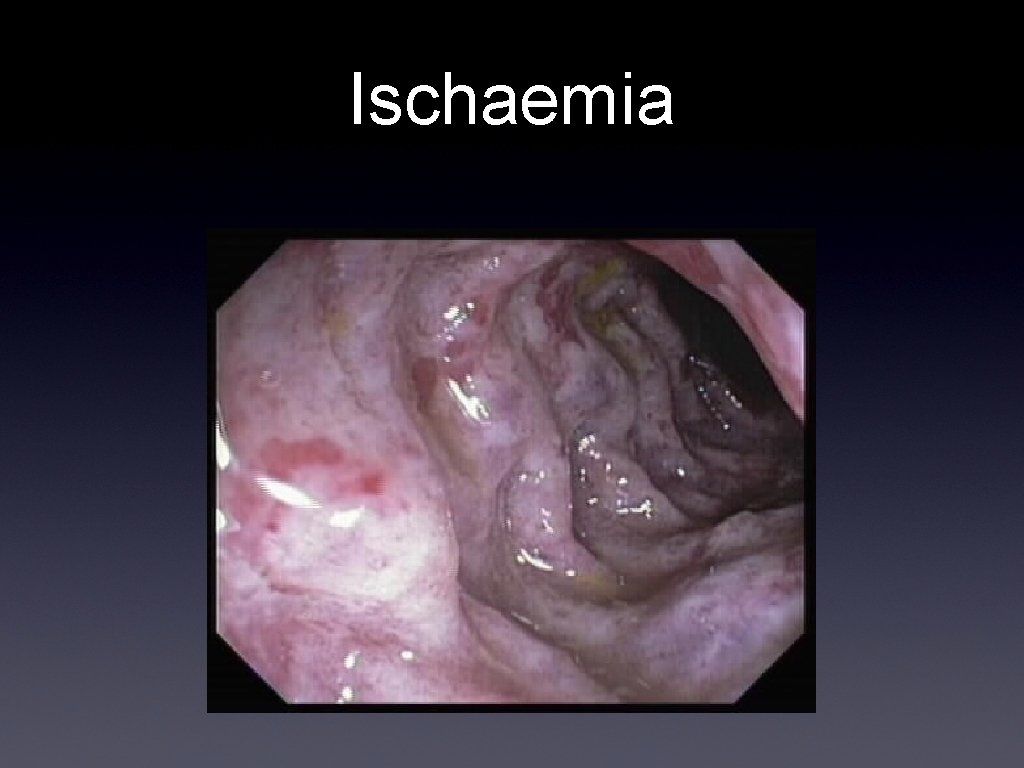
Ischaemia
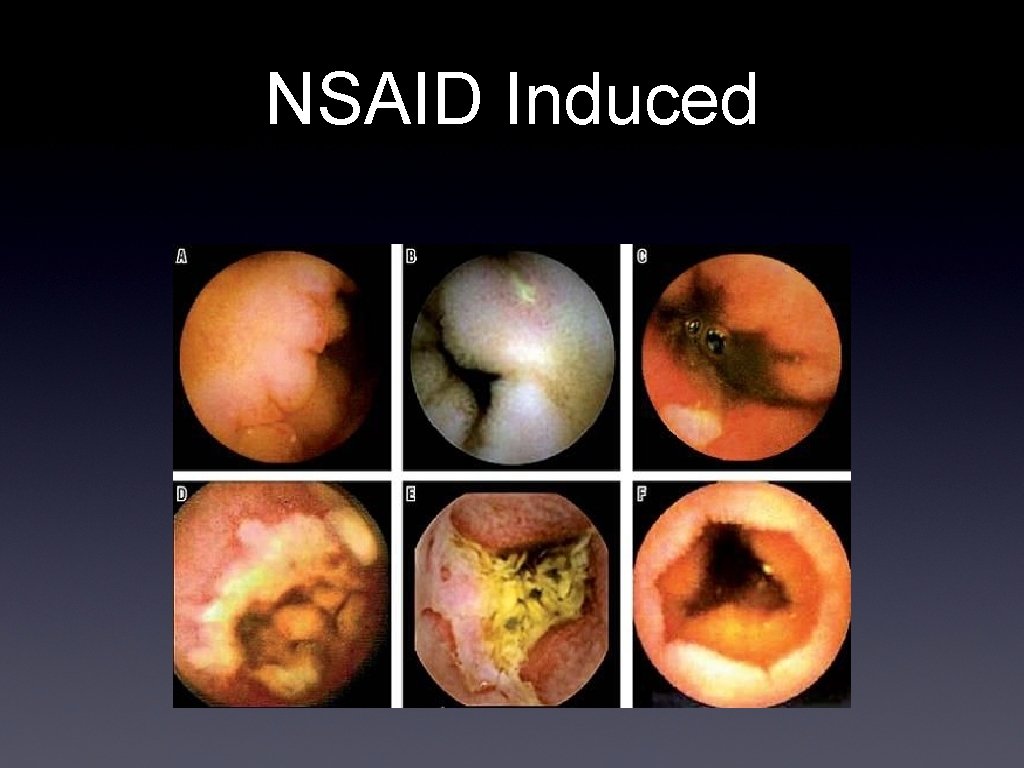
NSAID Induced

Sigmoiditis

• • • DD associated Colitis An immunologically mediated process Typically it does not effect the rectum Can proceed the development of the diverticulae by several years Many patients respond to treatment directed toward diverticulitis A subset of patients require immunosuppressive therapy and /or surgery
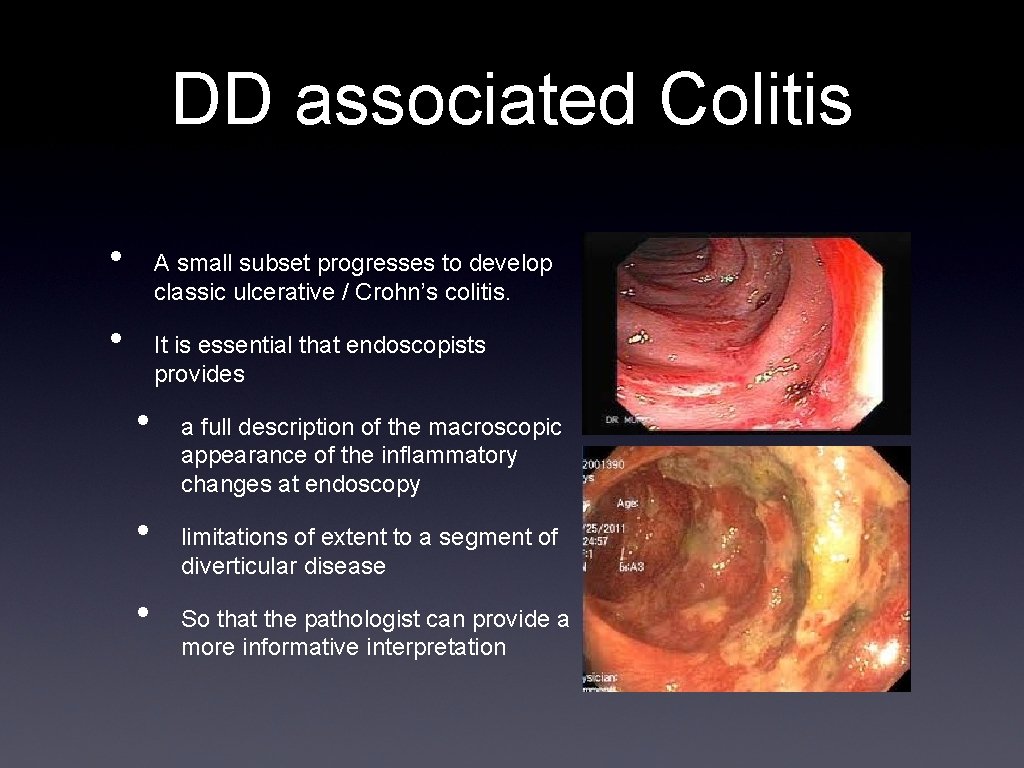
DD associated Colitis • A small subset progresses to develop classic ulcerative / Crohn’s colitis. • It is essential that endoscopists provides • • • a full description of the macroscopic appearance of the inflammatory changes at endoscopy limitations of extent to a segment of diverticular disease So that the pathologist can provide a more informative interpretation
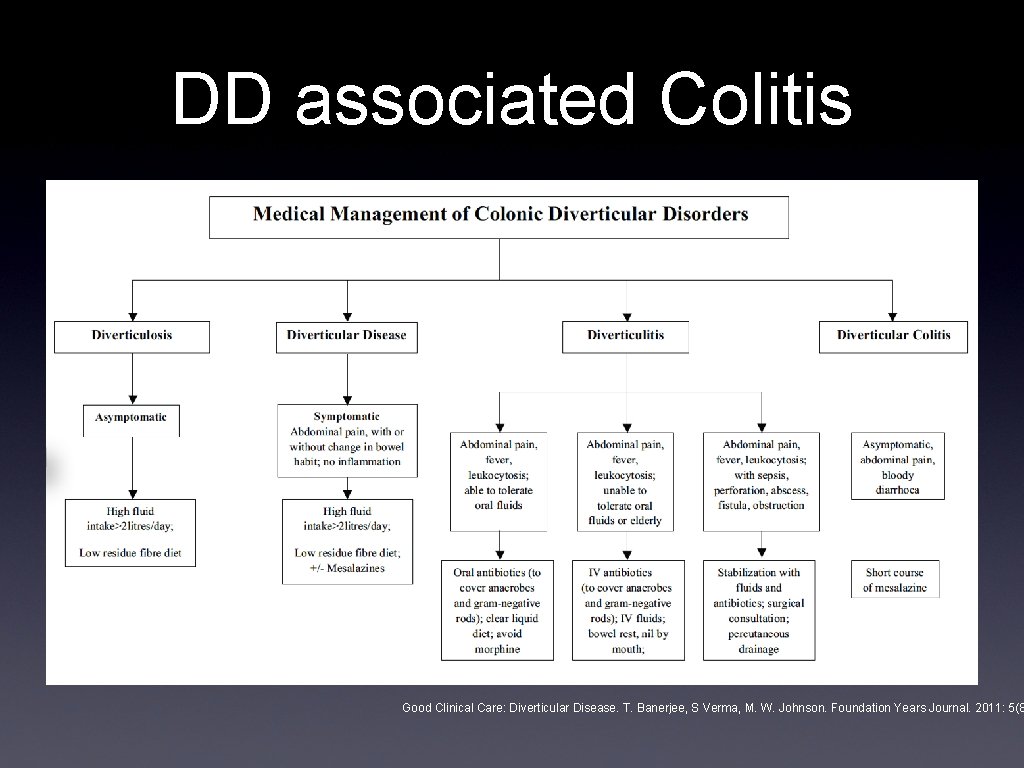
DD associated Colitis Good Clinical Care: Diverticular Disease. T. Banerjee, S Verma, M. W. Johnson. Foundation Years Journal. 2011: 5(8
- Slides: 24