WHATS UNDER YOUR SKIN Skin Care of Breast

WHAT’S UNDER YOUR SKIN? Skin Care of Breast Cancer Patients Undergoing Standard External Beam Radiation Donna M. Braunreiter RN BSN OCN MSN Student Alverno College Spring 2009, MSN 621 dmbraunreiter @ aol. com dmbraunreiter @ wi. rr. com

Objectives 1. Explain effects of external beam radiation therapy. 2. Briefly describe genetic mechanisms involved in radiation. 3. Summarize the acute physiologic mechanisms of inflammation. 4. Describe the structure and function of skin. 5. Identify breast skin changes after radiation treatment. 6. Review nursing care for breast cancer patients undergoing radiation therapy.

Directions To move to the next slide, click this To move to the previous slide, click this To return to the beginning, click this To return to the topics section, click this
RADIATION SKIN STRUCTURE AND FUNCTION GENETICS BREAST SKIN CHANGES INFLAMMATION NURSING CARE AND PATIENT EDUCATION

RADIATION Microsoft Office Clip Art 2007

Radiation Treatment • Skin reaction is the most common side effect during breast cancer radiation treatments • Over 90% of women receiving radiation for breast cancer will develop some skin changes during their course of treatment

Radiation • Interacts with all biological materials in its path • Direct and indirect damage to cells causes DNA changes • Causes many molecular responses that induce cellular mechanisms for DNA repair, cell cycle arrests, and apoptosis

Radiation • Major effect on dividing cells is reproductive death • Leaves cells unable to reproduce • Radiosensitivity of cell determines degree of injury and when it will happen

Radiation Direct Effect • DNA absorbs radiation • The atoms become ionized and damaged • Less common than indirect damage Microsoft Office Clip Art 2007

Radiation Indirect Effect • Water molecules surrounding DNA are ionized • Creates highly reactive free radicals such as hydroxyl radicals, peroxide, hydrated electrons, and oxygen radicals • These radicals interfere with DNA and cause damage and strand breakage • Common because 80% of a cell is water

Radiation Damage • Direct and indirect damage break bonds in DNA backbone • Results in loss of base, nucleotide, or one or both strands of DNA • Single-strand DNA breaks are repaired using the opposite strand as a template • Can result in mutation if not repaired correctly

Radiation Damage • Double-strand DNA breaks related to cell killing • Results in mitotic death • X-rays are sparsely ionizing and cause locally clustered damage • Leads to clinically significant events DNA Structure United States National Library of Medicine http: //ghr. nlm. nih. gov/handbook/illustrations. dnastructure. jpg

Radiation CONTROLS CANCER CELLS BY 1. Inducing apoptosis 2. Causing permanent cell cycle arrest or terminal differentiation 3. Inducing cells to die of mitotic catastrophe

Apoptosis • Programmed cell death • Radiation damage triggers signaling cascades which causes cell self-destruct mechanisms • Characteristics are nucleus fragmentation and blebbing • Tumors undergoing apoptosis have good clinical response
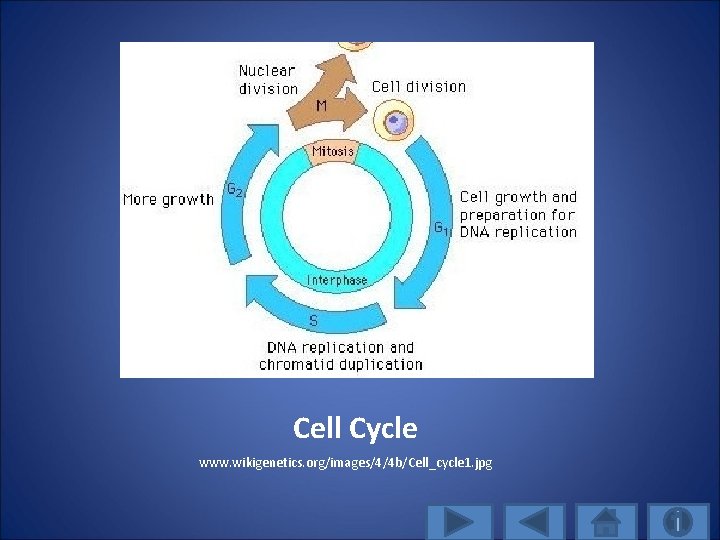
Cell Cycle www. wikigenetics. org/images/4/4 b/Cell_cycle 1. jpg

Cell Cycle Death/Terminal Differentiation (Denucleation) • Cells can arrest in any phase of cell cycle • Radiation damage mainly in G 1 and G 2 phases • Normal cells and cancer cells retaining p 53 function block in G 1 • Cancer cells with p 53 loss or mutation block in G 2 phase • G 2 arrest related to cellular repair of DNA radiation-induced DNA damage

Radiation Effects Radiosensitive • Cells renewing rapidly with little or no differentiation • Examples are skin cells, mucous membranes, and hematopoietic stem cells Radioresistant • Cells that do not divide regularly or at all and are highly differentiated • Examples are muscle cells and nerve cells

Radiation Effects Radiosensitive • Acute effects • Damage within weeks to months of exposure • Temporary • Normal cells affected are capable of repair • Dependent upon dose-timevolume factors Radioresistant • Late effects • Damage months or years after first exposure • Permanent • Damage becomes more severe as time goes on • Dependent upon dose-timevolume factors

Radiation Effects Radiosensitive Radioresistant • Higher doses over shorter periods of time to larger volumes of tissues result in more severe acute reactions • Acute damage results from depletion of actively proliferating parenchymal or stromal cells • Characteristics are vascular dilation, local edema, and inflammation • Severity of late effects more dependent upon total dose delivered and volume if tissue irradiated • Damage to endothelial cells or connective tissues results in late effects occurring as a result of narrowing or occlusion of small vasculature and fibrosis

Radiation Effects • Acute and late side effects from radiation therapy are LOCAL and ONLY affect tissues receiving treatment • Presence and severity of acute effects can not predict late effects of radiation • Late reactions such as tissue necrosis or dense tissue fibrosis can occur independently of acute reactions

SUPINE POSITION • Most common position for breast cancer radiation therapy • MUST be used if lymph nodes need to be treated • May involve radiation exposure to heart, lungs, ribs, and contralateral breast Microsoft Office Clip Art 2007

PRONE POSITION • Used for women with larger pendulous breast, cardiac and/or pulmonary comorbidities • Possible improved dose homogeneity • Potential reduction in lung and heart irradiation Microsoft Office Clip Art 2007

Patient-Related Considerations Normal age-related changes: • thinning of the epidermis and dermis, • diminished elasticity, • decreased dermal turgor, which results in delayed healing. Nutritional status is also important for healing.

What is the effect of radiation on cells? A. Reproductive death of cells throughout the body B. Reproductive death of cells in the treated area only C. Radiation skin reactions cause internal injuries. D. Radiation helps repair DNA damage.

Wrong answer, try again. Radiation only affects the area being treated and causes damage to DNA. Click here to return to question

Correct! Radiation causes the reproductive death of cells in the treated area only.

GENETICS Microsoft Office Clip Art 2007
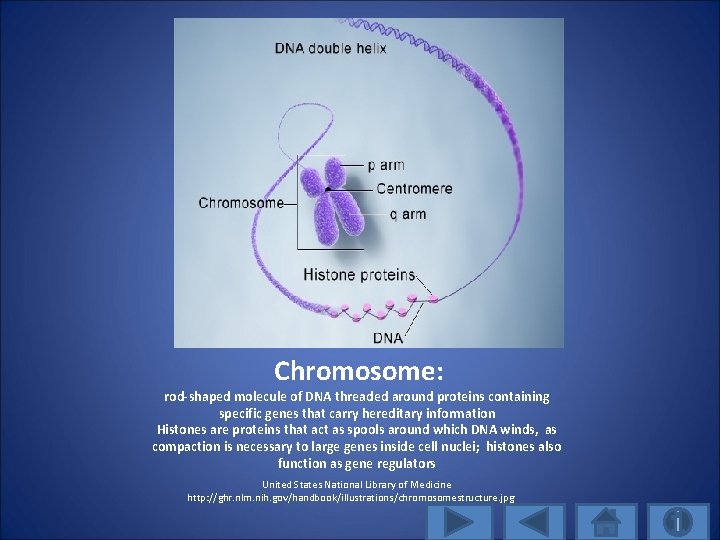
Chromosome: rod-shaped molecule of DNA threaded around proteins containing specific genes that carry hereditary information Histones are proteins that act as spools around which DNA winds, as compaction is necessary to large genes inside cell nuclei; histones also function as gene regulators United States National Library of Medicine http: //ghr. nlm. nih. gov/handbook/illustrations/chromosomestructure. jpg
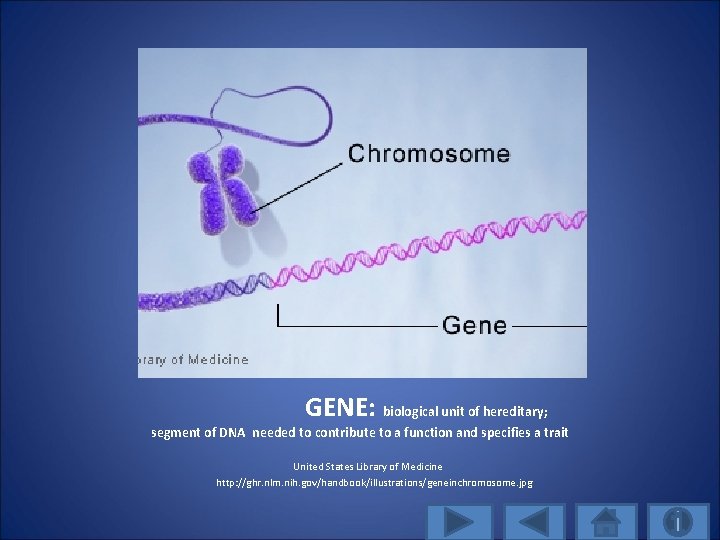
GENE: biological unit of hereditary; segment of DNA needed to contribute to a function and specifies a trait United States Library of Medicine http: //ghr. nlm. nih. gov/handbook/illustrations/geneinchromosome. jpg

Radiation effect on genes 1. Ionizing radiation causes phosphorylation of histone H 2 AX (forming gamma-H 2 AX) 2. Reaction dependent on ataxia telangiectesia mutated (ATM) molecule 3. Followed by accumulation of 53 BP 1, a protein acting as central mediator for critical pathways, including phosphorylating (which conveys the DNA damage signal to) tumor suppressor protein p 53

Genetics in Radiation 4. Next, phosphorylating the ATM protein amplifies the damage signal 5. And recruits proteins critical for repair, such as the BRCA 1 and HDAC 4 6. Which allows a G 2 cycle checkpoint 7. 53 BP 1 important in double-strand DNA damage sensing, repair, and tumor suppression

Genetics in Radiation • HR (homologous repair) efficient in late S or G 2 phase when sister chromatids have replicated but not separated • Repair is cell cycle dependent • Undamaged homologous chromosome or sister chromatid or replicated chromosome is used as a template to fill in missing DNA sequences in damaged chromosome

Genetics in Radiation • Human tumor cells block in G 2 after DNA double-strand damage, when repairs are detectible, and irradiation induced G 2 checkpoint allows more time for cells to undergo HR (homologous repair) and survive radiation

Genetics in Radiation • NHEJ (nonhomologous endjoining) is where blunt ends of chromosomes severed by radiation are directly rejoined • Less cell cycle dependent • Highly mutagenic due to template-free rejoining lacks specificity of HR • Ends of different chromosomes can be rejoined, leading to chromosomal aberrations or expression of dangerous fusion proteins

p 53 Tumor Suppressor Gene • p 53 stops activity of tumors • Loss or mutation of p 53 predisposes to cancer (e. g. inheriting only one functional copy of p 53 gene from parents) • p 53 protein binds DNA and stimulates another gene to produce protein p 21 and blocks next stage of cell division • Mutant p 53 no longer binds DNA and does not interact with p 21 • Results in p 21 unable to act as a stop signal • Cells divide uncontrollably

Genetics in Radiation • Ras, Raf, and EGFR alter cellular sensitivity to radiation, but exact mechanisms unknown • Ras is a proto-oncogogene (portion of DNA that regulates normal cell proliferation and repair) • Raf is a gene coding for protein kinase • EGFR (epidermal growth factor receptor) found on surface of some cells and where epidermal growth factor binds, causing the cells to divide

What is a common gene that can lead to many cancers it is mutated or lost? A. EGFR B. p 21 C. p 53 D. Ras

Wrong answer, try again. EGFR is epidermal growth factor, Ras is a protooncogene, and p 21 is a protein influenced by p 53 and acts as a stop signal in the cell cycle. Click here to return to question
Correct! p 53

INFLAMMATION Microsoft Office Clip Art 2007

Inflammation • Reaction of vascularized tissue to local injury. • Causes are many and varied. • Commonly it results from an immune response to infection organisms. • Other causes are trauma, surgery, caustic chemicals, extremes of heat and cold, and ischemic damage to body tissues. (Porth, 2005).

Five Cardinal Signs of Inflammation 1. 2. 3. 4. 5. Redness Swelling Heat Pain Loss of function Microsoft Office Clip Art 2007

Acute Inflammation Two major components 1. VASCULAR 2. CELLULAR Inflammatory mediators, acting together or in sequence, amplify the initial response and influence its evolution by regulating the subsequent vascular and cellular responses (Porth, 2005). Microsoft Office Clip Art 2007
Vascular Stage • Constriction of small blood vessels in injured area • Vasoconstriction followed rapidly by vasodilation of the arterioles and venules • Causes the area to becomes congested and results in redness and warmth

Vascular Stage • Capillary permeability increases causes swelling, pain, and impaired function • Movement of fluid from capillaries into interstitial spaces (swelling) dilutes the offending agent • Extravasation of plasma proteins into extracellular spaces causes exudate • Blood stagnation and clotting of blood in the capillaries around the injury site; aids in localizing the spread of infectious microorganisms
Vascular Stage 1. FIRST is immediate transient response 2. SECOND is immediate sustained response which occurs with more serious injury and continues for several days and damages vessels in the area 3. THIRD is a delayed hemodynamic response, which increases capillary permeability that occurs 4 to 24 hours after injury, seen with RADIATION types of injuries
Cellular Stage • Movement of phagocytic white blood cells (leukocytes) into area of injury • Two types of leukocytes involved-granulocytes and monocytes • Requires the release of chemical mediators from sentinel cells (mast cells and macrophages) already positioned in tissues

Cellular Stage: Granulocytes divided into three types neutrophils, eosinophils, and basophils. 1. Neutrophils are primary phagocytes; arrive within 90 minutes to injury site; contain enzymes and antibacterial substances that destroy and degrade engulfed particles.
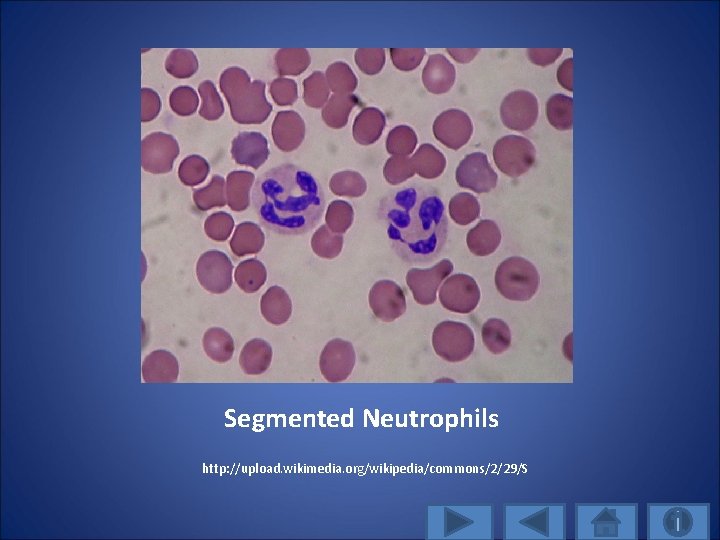
Segmented Neutrophils http: //upload. wikimedia. org/wikipedia/commons/2/29/S

Cellular Stage: Monocytes • Mononuclear phagocytes are largest of white blood cells • Last 3 to 4 times longer than granulocytes and survive longer in the tissues. • Help to destroy agent, aid in signaling processes of specific immunity, and help to resolve inflammatory process. • Arrive by 24 hours and at 48 hours monocytes and macrophages are predominant cells at injury site • Engulf larger and greater quantities of foreign materials and migrate to lymph nodes.

Phases of Acute Inflammation Response MARGINATION Leukocytes increase adhesion molecules, slow migration, and move along periphery of blood vessels

Phases of Acute Inflammation Response EMIGRATION Leukocytes pass through capillary walls and migrate into tissue spaces

Phases of Acute Inflammation Response CHEMOTAXIS Leukocytes in tissues guided by cytokines, bacteria, and cell debris

Phases of Acute Inflammation Response PHAGOCYTOSIS Neutrophils and macrophages engulf and degrade bacteria and debris Phagocytosis http: //upload. wikimedia. org/. . . /180 px-Phagocytosis 2. png

Inflammatory Mediators CYTOKINES Polypeptide products of various cell typesmostly lymphocytes and macrophages modulate functions of other cell types COLONY-STIMULATING FACTORS directs growth of immature marrow precursor cells INTERLEUKINS (Ils) INTERFERONS (Ifs) TUMOR NECROSIS FACTOR

Inflammation with Chemical Mediator INFLAMMATORY RESPONSE Swelling, redness, and tissue warmth (vasodilation and increased capillary permeability) CHEMICAL MEDIATOR Histamine (fast acting and causes dilatation and increased permeability of capillaries), Prostaglandins, Leukotrienes, Bradykinin, Platelet-activating factor (attracts neutrophils)

Inflammation with Chemical Mediators INFLAMMATORY RESPONSE Tissue Damage CHEMICAL MEDIATOR Lysomomal enzymes and products released from neutrophils, macrophages, and other inflammatory cells

Inflammation with Chemical Mediators INFLAMMATORY RESPONSE CHEMICAL MEDIATOR Pain Prostaglandins Bradykinins

Inflammation with Chemical Mediator INFLAMMATORY RESPONSE Leukocytosis CHEMICAL MEDIATOR Interleukin-1 Other Cytokines

What are the five major signs of inflammation? A. Redness, pus, fever, pain, and swelling B. Pain, swelling, numbness, tingling, and cold C. Heat, pain, swelling, pus, and loss of function D. Redness, swelling, heat, pain, and loss of function

Wrong answer, try again. Click here to return to question

Correct! Redness, swelling, heat, pain, and loss of function.

SKIN STRUCTURE AND FUNCTION Microsoft Office Clip Art 2007

SKIN • Largest organ of the body • Receives approximately one-third of heart’s oxygenated blood • Body’s FIRST defense mechanism
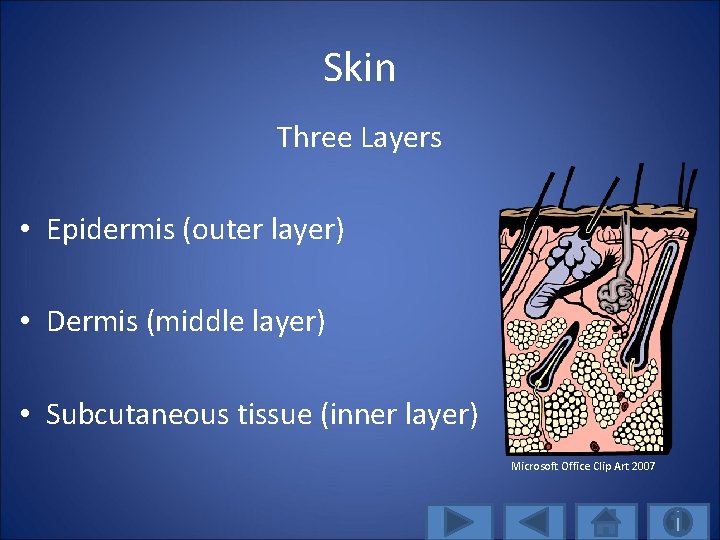
Skin Three Layers • Epidermis (outer layer) • Dermis (middle layer) • Subcutaneous tissue (inner layer) Microsoft Office Clip Art 2007
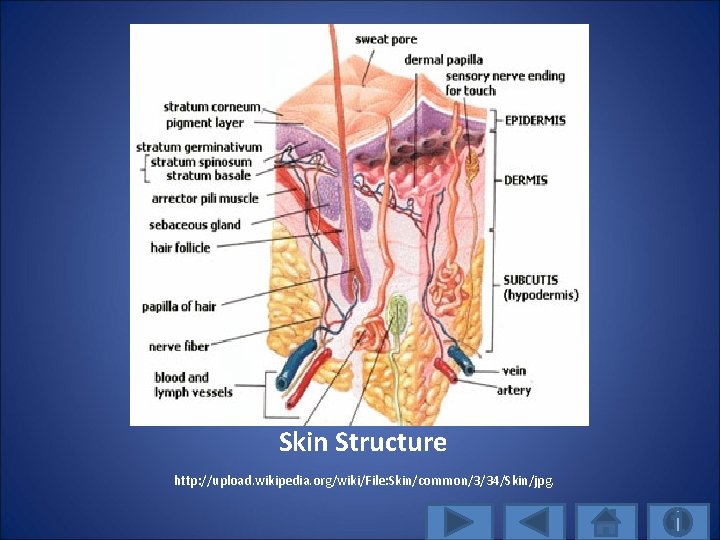
Skin Structure http: //upload. wikipedia. org/wiki/File: Skin/common/3/34/Skin/jpg.

Epidermis 1. Multi-layered and impermeable 2. Outer layer that forms a resistant cover and permeability barrier of varying thickness 3. Renews itself continuously through cell division in deepest (basal) layer 4. Undergoes keratinization to produce scales that are shed from outer layer 5. Avascular and receives nutrients from dermis

Epidermal Layers 1. Stratum corneum is outermost layer composed of flattened dead cells and is about 25% of total thickness 2. Stratum granulosum is thin transitional layer 3. Stratum spinosum (squamous cell) is viable layer made up of mainly post-mitotic cells 4. Basal cell layer is viable and deepest layer where majority of cell division occurs
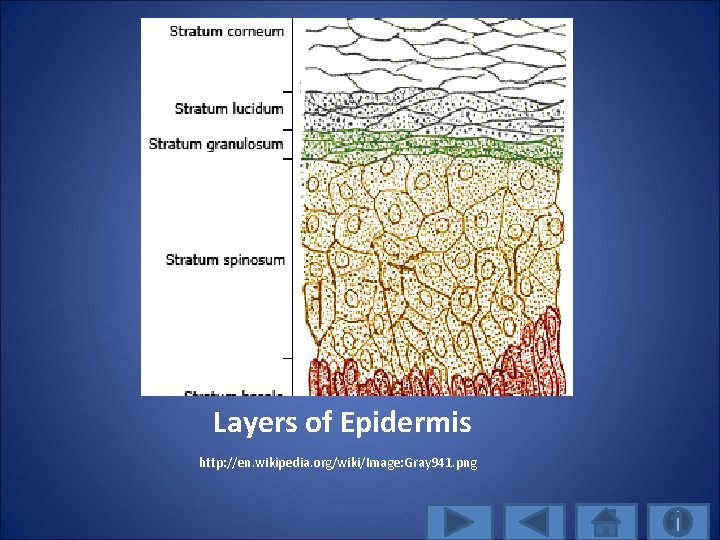
Layers of Epidermis http: //en. wikipedia. org/wiki/Image: Gray 941. png

Terminal Transition in Epidermis 1. Half the cells produced in basal layer undergo mitosis 2. After dividing, cells leave basal cell layer and enter stratum spinosum and then stratum granulosum 3. This is where the cells flatten, lose organelles, and become mature, keratininized cells of the stratum corneum 4. Cells detach and desquamate, but are continually replaced by cells produced in basal layer (turnover process is 30 days)

Dermis 1. 2. 3. 4. Tough and durable middle layer 1 -3 mm thick Gives skin strength, elasticity, and softness Protects deeper structures from injury Contains blood vessels that regulate body temperature and provide nourishment to epidermis; also contains nerves, hair follicles and various glands 5. Interacts with epidermis during wound repair

Subcutaneous Tissue 1. 2. 3. 4. 5. Composed mostly of adipose tissue Cushion to physical trauma Insulator to temperature change Energy reservoir Nerves, blood vessels, and lymphatics run through it

Functions of Skin 1. 2. 3. 4. 5. PROTECTION - MOST IMPORTANT! Regulation of body temperature Sensory perception Vitamin D production Provides an active system of immunologic defense (dermal lymphocytes, mast cells, mononuclear phagocytes, Langerhans cells) 6. Excretion

Skin First line of defense against bacteria and foreign substances, physical trauma, heat, or rays Microsoft Office Clip Art 2007 Protection works by: (1) eccrine gland sweating (2) insulation by the skin and subcutaneous tissue (3) regulation of cutaneous blood flow (vasoconstriction and vasodilation) (4) muscle activity (shivering)

What is the major function of the skin? A. Vitamin D Production B. Sensory perception. C. Regulation of body temperature. D. Protection

Wrong answer, try again. Click here to return to picture

Correct! Protection.

BREAST SKIN CHANGES Microsoft Office Clip Art 2007

Radiation Changes • Reflect injury occurring mostly in the epidermis • Primary target for acute radiation skin reactions is the basal cell layer • Entire epidermis turns over in 30 days

Radiation Changes • Early erythema within few hours after radiation and subsides after 24 -48 hours • Inflammatory response from histamine-like substances that cause dermal edema from the permeability and dilatation of capillaries

Radiation Changes • Main erythematous reaction occurs 3 -6 weeks after radiation begins and is due to a varying severity loss of epidermal basal cells • Basal cell density changes with higher doses of radiation • Reddening of the skin due to a secondary inflammatory reaction or hyperemia

Radiation Changes • Higher radiation doses reduce number of mitotic cells and increase in degenerate cells • When cells are not being reproduced at the same rate in the basal cell layer and the normal migration of cells to stratum corneum continues, epidermis is denuded in time equal to natural turnover (30 days)

Dry Desquamation • If enough numbers of clonogenic cells (cells giving rise to a clone of cells) remain to replace injured cells, there is atypical thickening of the stratum corneum • The populations of the basal-layer stem cells become depleted in the radiation treated area • This can result in dry flaking, scaling, and itching in the treated area
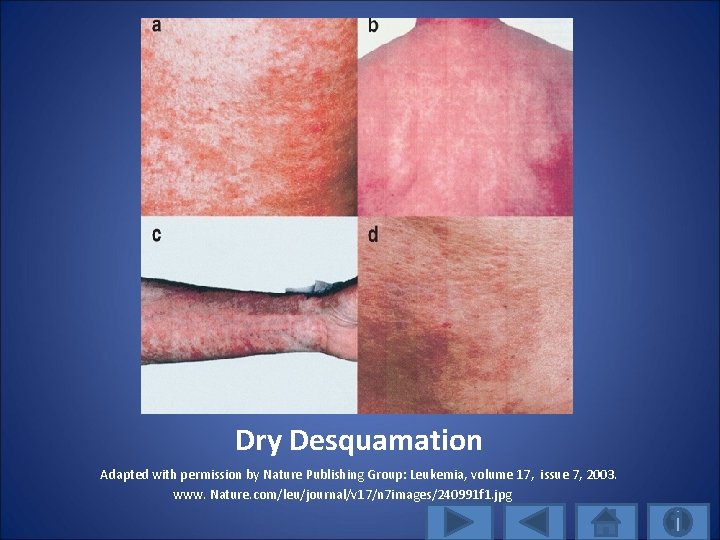
Dry Desquamation Adapted with permission by Nature Publishing Group: Leukemia, volume 17, issue 7, 2003. www. Nature. com/leu/journal/v 17/n 7 images/240991 f 1. jpg

Moist Desquamation • If new cell proliferation is inadequate, there is exposed dermis with oozing of serum • Repopulation of the basal cell layer of epidermis after irradiation is mainly from surviving clonogenic cells (cells giving rise to a clone of cells) within the irradiated area • If the treated area is completed denuded of clonogenic epithelial cells, then healing results from division and migration of viable cells from skin around the irradiated area
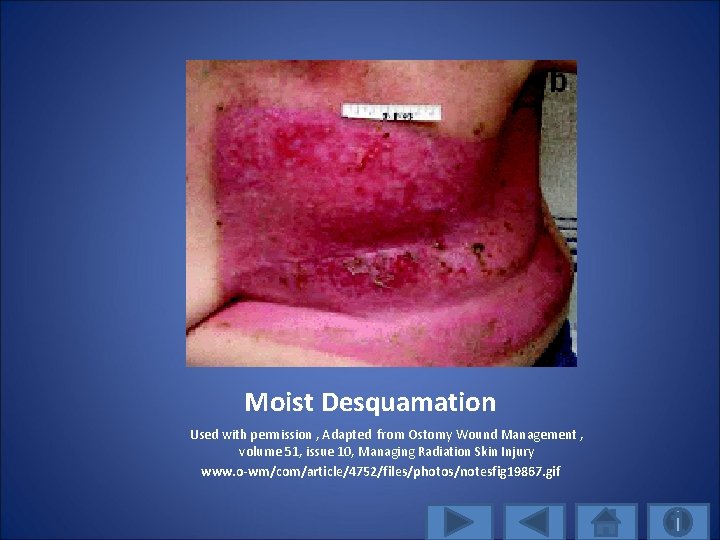
Moist Desquamation Used with permission , Adapted from Ostomy Wound Management , volume 51, issue 10, Managing Radiation Skin Injury www. o-wm/com/article/4752/files/photos/notesfig 19867. gif

Acute Skin Reactions ERYTHEMA Redness that outlines treatment field and intensifies as treatment continues Increased skin temperature Edema Follows after 2 -3 weeks after standard fractionated radiation and resolves 20 -30 days after last treatment

Acute Skin Reactions DRY DESQUAMATION Dryness Flaking Peeling Pruritus Following 3 -4 weeks of standard fractionated radiation and resolves 1 -2 weeks after completion of treatments

Acute Skin Reactions HYPERPIGMENTATION Tanned appearance Following 2 -3 weeks of standard fractionated therapy and is usually resolved in 3 months to 1 year after treatment but may be chronic

Acute Skin Reactions MOIST DESQUAMATION Bright erythema Sloughing skin Exposed dermis Serous exudate Pain

Acute Skin Reactions MOIST DESQUAMATION Can occur with radiation or with trauma or friction and most recovery usually 2 -4 weeks after completion of treatment SKIN REGROWTH New skin is smooth, pink, thin, and dryer Depends upon severity but usually is complete 2 -3 months after therapy

Late Skin Reactions PHOTOSENSITIVITY Enhanced erythema over skin exposed to UV radiation from sun and tanning bed/booths Begins during treatment and is lifelong

What develops after 3 -4 weeks of radiation with symptoms of dry, flaking, and peeling skin? A. Dry desquamation B. Erythema C. Moist desquamation D. Hyperpigmentation

Sorry, wrong answer. Click here to return to question

Yes! Dry desquamation.

NURSING CARE AND PATIENT EDUCATION Microsoft Office Clip Art 2007

Nursing Care • Perform skin assessment before radiation treatments, at least weekly during treatments, 1 month following completion of treatment, and each follow-up appointment. • Initial assessment includes the patient’s present skin condition, preexisting skin disorders, medical conditions, medications, age-related factors, and nutritional status. • Consistency in assessment and documentation is important.

Patient Instructions • Use gentle soaps ONLY, such as Dove or Ivory, which do not contain additives • Use a moisturizing lotion on the treatment area twice a day • Expose the treated area to the air as much as possible • Do not wear underwire bras • Do not wear tight-fitting clothing that rubs or binds underneath the breast

Patient Instructions • Wear a comfortable bra. Wear cotton t-shirts underneath your bra to absorb moisture. • Drink 8 -10 glasses of water a day. • Eat well-balanced meals and maintain your weight during treatment. • Continue with your normal daily activities.

Patient Instructions • Sexual activity may continue during treatment. You are not radioactive and there are no dangers to your partner. • Avoid extreme temperatures to the affected area. Do not use water bottles, heating pads, sun lamps, ice bags, etc. • Avoid exposing your skin to the sun, as the sun and sun rays are an additional form of radiation to the skin. Always apply sunscreen with SPF or 15 before sun exposure.

Patient Instructions • Do not apply tape or adhesive bandages to the treated area. • Speak with your nurse about deodorant use • Continue with the range of motion exercises for your arm and shoulder. • Report any pain or swelling to your doctor or nurse.

Breast Skin Products Cleanser and moisturizer Given to every breast cancer patient being treated with radiation Have patients use twice a day

Breast Skin Products Healing ointment and skin protectant Used for dry desquamation Apply to affected area

Breast Skin Products MOIST DESQUAMATION Topical aluminum acetate packets (astringent) mixed with normal saline Gently debride area and apply solution to area for 20 minutes; rewet every 10 minutes and repeat once a day Apply hydrocolloid dressing over affected area and secure Do NOT use hydrocolloid dressing 4 hours before treatment

What is the recommended treatment for every radiation patient? A. Soap and water once a day B. Apply cleanser and moisturizer twice a day on the affected area C. Apply a hydrocolloid over the treated area D. Encourage daily sun exposure.

Sorry, incorrect. Try again. Click here to return to the question

Yes! Apply cleanser and moisturized twice a day to the affected area.

Case Study Mrs. K is a breast cancer patient who has received radiation to her left breast for the past 4 weeks. She is complaining of increasing pain and her left breast is bright red in color, with sloughing skin and a serous exudate. What is the name of this skin condition caused by radiation? What would be the nurse’s actions and interventions?

Case Study Moist desquamation. The nurse would apply an aluminum acetate solution for 20 minute and gently debride the area. A hydrocolloid dressing would then be placed over this area and secured. The patient would be given instructions about this treatment once a day. Pain management will be addressed.

References Abeloff, M. D. , Armitage, J. O. , Niederhuber, J. E. , Kastan, M. B. , & Mc. Kenna, W. G. (2004). Clinical oncology (3 rd ed. ). Philadelphia, PA: Elsevier, Inc. Bruner, D. W. , Bucholtz, J. D. , Iwamoto, R. , & Strohl, R. (Eds. ) (1998). Manual for radiation oncology nursing practice and education. Pittsburgh, PA: Oncology Nursing Society. Fox, S. I. (1996). Human physiology (5 th ed. ). Dubuque, IA: Wm. C. Brown Publishers. Groenwald, S. L. , Frogge, M. H. , Goodman, M. , & Yarbro, C. H. (1993). Cancer nursing: Principles and practice (3 rd ed. ). Boston, MA: Jones & Bartlett. Hill, S. (2008). Managing radiation skin injury. Ostomy Wound Management, 51(10), 1 -2. Retrieved May 13, 2009, from, http: //www. o-wn. com/article/4752. Mahon, S. M. (Ed. ). (2007). Breast cancer. Pittsburgh, PA: Oncology Nursing Society. Milojkovic, D. , Short, K. , Salisbury, J. R. , creamer, D. , du Vivier a. W. P. , & Mufti, G. J. (2003). Dose-limiting dermatological toxicity secondary to imatinib mesylate (STI 571) in chronic myeloid leukaemia. Leukemia, (17), 1414 -1416. Retrieved May 13, 2009, from http: //nature. com/leu/journal/v/17/n 7/full/24024991 a. html. Microsoft Clip Art 2007 retrieved on various dates in April and May of 2009, from http: //office. Microsoft. com/en-us/clipart/default. aspx.

National Human Genome Research Institute (n. d. ). Chromosome. Retrieved May 12, 2009, from http: //www. genome. gov/Hyperion/DIR/VIP/Glossary/Illustration/chromosome. cf m? key=chromosome. Otto, S. E. (2001). Oncology nursing (4 th ed. ). St. Louis, MO: Mosby, Inc. Porth, C. M. (2005). Pathopphysiology: Concepts of altered health status (7 th ed. ). Philadelphia, PA: Lippincott, Williams & Wilkins. Singer, M. (1992). The Ras gene and cancer. Winding your way through DNA. Symposium conducted at the University of California. San Francisco. Retrieved May 13, 2009, from http: //www/accessexcellence. or/RC/AB/BA/Ras_Gene_and Cancer. php. United States National Library of Medicine (n. d. ). DNA structure. Genetics home reference: Your guide to understanding genetic conditions. Retrieved May 9, 2009, from http: //ghr. nlm. nih. gov/handbook/illustrations/dnastructure. . United States National Library of Medicine (n. d. ). Chromosome structure. Genetics home reference: Your guide to understanding genetic conditions. Retrieved May 13, 2009, from http: //ghr. nlm. nih. gov/handbood/illustrations/chromosomestructure. United States National Library of Medicine (n. d. ). Genetics home reference: Your guide to understanding genetic conditions. Retrieved May 13, 2009, from http: //ghr. nlm. nih. gov/handbood/illustrations/genein chromosome.

White, J. , & Joiner, M. C. (2006). Toxicity from radiation in breast cancer. In W. Small Jr. , & G. E. Woloschack (Eds. ). , Radiation toxicity: A practical guide. Springer Science + Media Business, Inc. Wikigenetics (n. d. ). The cell cycle. Retrieved May 9, 2009, from wikigenetics. org/index. php. /The_Cell_Cycle. Wikimedia Commons (n. d. ). Segmented neutrophils. Retrieved May 14, 2009, from http: //commons. wikimedia. org/wiki/File: Segmented_neutrophils. jpg. Wikimedia Commons (n. d. ). Skin. Retrieved May 13, 2009, from http: //commons. wikimedia. org/wiki/File: Skin. jpg. Wikimedia Commons (n. d. ). Skin layers. Retrieved May 13, 2009, from http: //commons. wikimedia. org/wiki/File: Skinlayers. png. Wikipedia (n. d. ). Phagocytosis. Retrieved May 14, 2009, from http: //en. wikipedia. org/wiki/Phagocyte.

Good Job Microsoft Office Clip Art 2007
- Slides: 113