Whats the SYNTAX Score all about anyway Keith
What's the SYNTAX Score all about anyway? Keith Dawkins MD FRCP FACC FSCAI Chief Medical Officer Senior Vice President Boston Scientific Corporation www. syntaxscore. com

DISCLOSURES Keith D. Dawkins, MD Salary – Boston Scientific Corporation Ownership Interest (Stocks, Stock Options or Other Ownership Interest) – Boston Scientific Corporation I intend to reference unlabeled/ unapproved uses of drugs or devices in my presentation. I intend to reference SYNTAX, TAXUS Element, PROMUS Element, TAXUS Diabetes, and EVOLUTION.

N Engl J Med 2009; 360: 961 -972
Treatment Options for CAD + +
The Interface between PCI and CABG ? CABG PCI

SYNTAX Trial Design 62 EU Sites + 23 US Sites De novo 3 VD and/or LM (isolated, +1, 2, 3 VD) Limited Exclusion Criteria Previous interventions , Acute MI with CPK>2 x, Concomitant cardiac surgery Heart Team (Surgeon & Interventional Cardiologist Amenable for both treatment options Amenable for only one treatment approach Stratification: LM and Diabetes Randomized Arms N=1800 Two Registry Arms N=1275

Left Main PCI? …CABG using IMA grafting is the ‘gold standard’ for treatment of unprotected left main disease and has proven benefit on long-term outcomes. The use of DES has shown encouraging short-term outcomes, but longterm follow-up is needed… It is likely that during the progress of their disease, many patients will benefit from a combined application of percutaneous and surgical techniques, taking advantage of the low morbidity of percutaneous methods and the established long-term benefit of surgical revascularization with arterial conduits. J Am Coll Cardiol 2006; 47: e 1 -e 121

Appropriate Revascularization? Coronary revascularization is appropriate when the expected benefits, in terms of survival or health outcomes (symptoms, functional status, and/or quality of life) exceed the expected negative consequences of the procedure. J Am Coll Cardiol 2009; 53: 530 -553
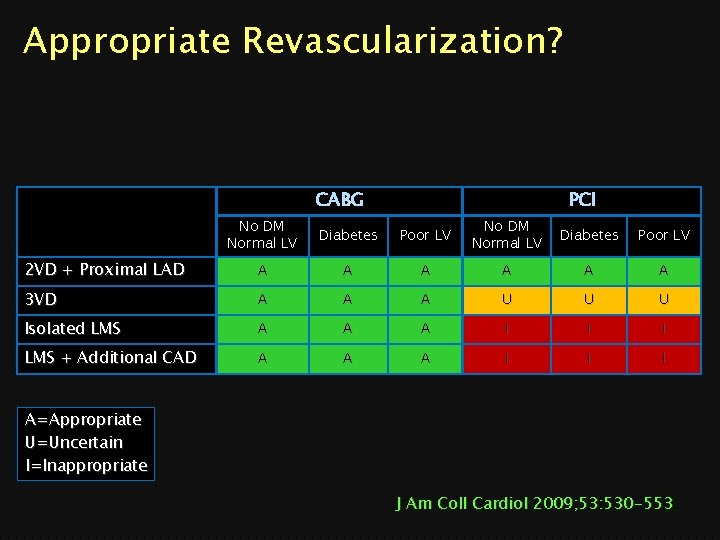
Appropriate Revascularization? CABG PCI No DM Normal LV Diabetes Poor LV 2 VD + Proximal LAD A A A 3 VD A A A U U U Isolated LMS A A A I I I LMS + Additional CAD A A A I I I A=Appropriate U=Uncertain I=Inappropriate J Am Coll Cardiol 2009; 53: 530 -553

The Ultimate Goal of the SYNTAX Score Create a prospective angiographic tool to grade complexity of coronary disease A semi-quantitative, visual score will help interventional cardiologists and surgeons be aware of the anatomical complexity to anticipate procedural difficulties and eventually predict outcomes Obtain evidence-based guidelines for selecting revascularization technique (surgery or PCI)
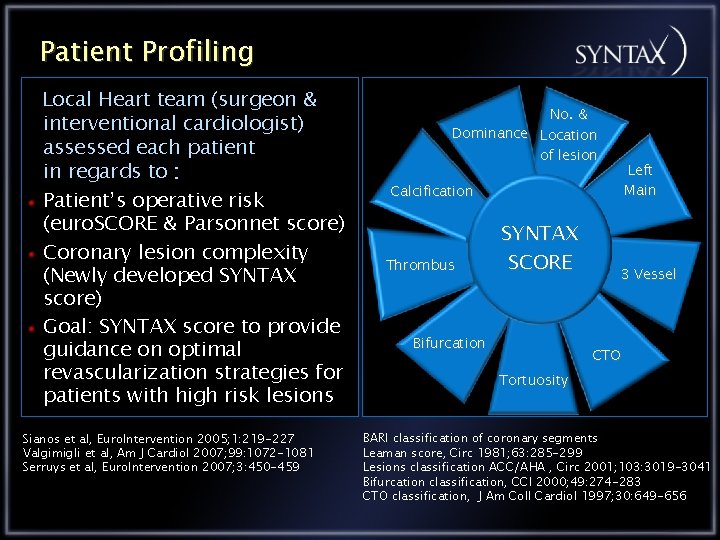

Patient Profiling Local Heart team (surgeon & interventional cardiologist) assessed each patient in regards to : Patient’s operative risk (euro. SCORE & Parsonnet score) Coronary lesion complexity (Newly developed SYNTAX score) Goal: SYNTAX score to provide guidance on optimal revascularization strategies for patients with high risk lesions Sianos et al, Euro. Intervention 2005; 1: 219 -227 Valgimigli et al, Am J Cardiol 2007; 99: 1072 -1081 Serruys et al, Euro. Intervention 2007; 3: 450 -459 No. & Dominance Location of lesion Left Main Calcification Thrombus SYNTAX SCORE Bifurcation 3 Vessel CTO Tortuosity BARI classification of coronary segments Leaman score, Circ 1981; 63: 285 -299 Lesions classification ACC/AHA , Circ 2001; 103: 3019 -3041 Bifurcation classification, CCI 2000; 49: 274 -283 CTO classification, J Am Coll Cardiol 1997; 30: 649 -656
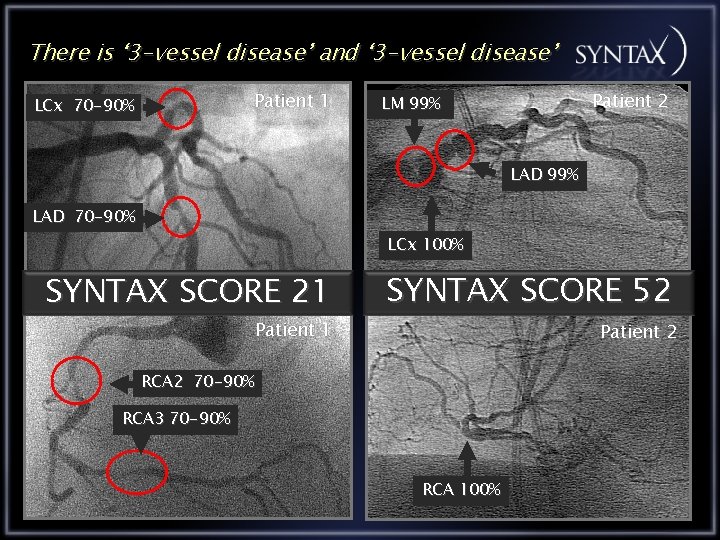
There is ‘ 3 -vessel disease’ and ‘ 3 -vessel disease’ Patient 1 LCx 70 -90% Patient 2 LM 99% LAD 70 -90% LCx 100% SYNTAX SCORE 21 Patient 1 SYNTAX SCORE 52 Patient 2 RCA 2 70 -90% RCA 3 70 -90% RCA 100%

2 y Ma 9 0 0 SYNTAX SCORE or www. syntaxscore. com

www. syntaxscore. com
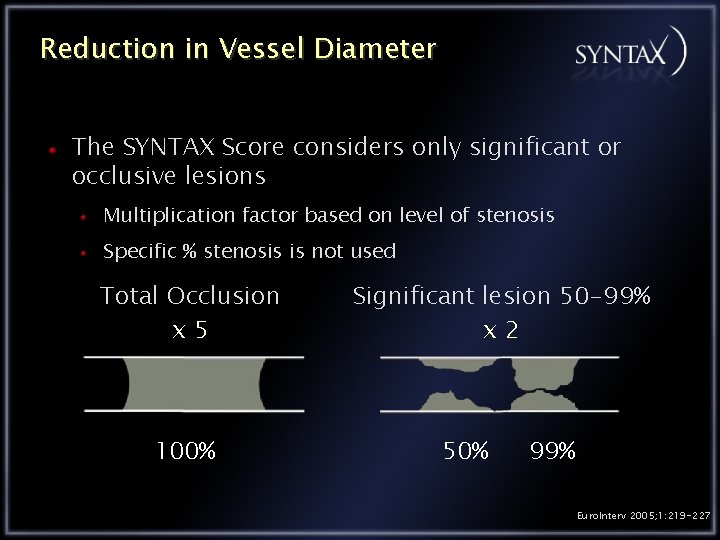

Reduction in Vessel Diameter The SYNTAX Score considers only significant or occlusive lesions Multiplication factor based on level of stenosis Specific % stenosis is not used Total Occlusion x 5 100% Significant lesion 50 -99% x 2 50% 99% Euro. Interv 2005; 1: 219 -227
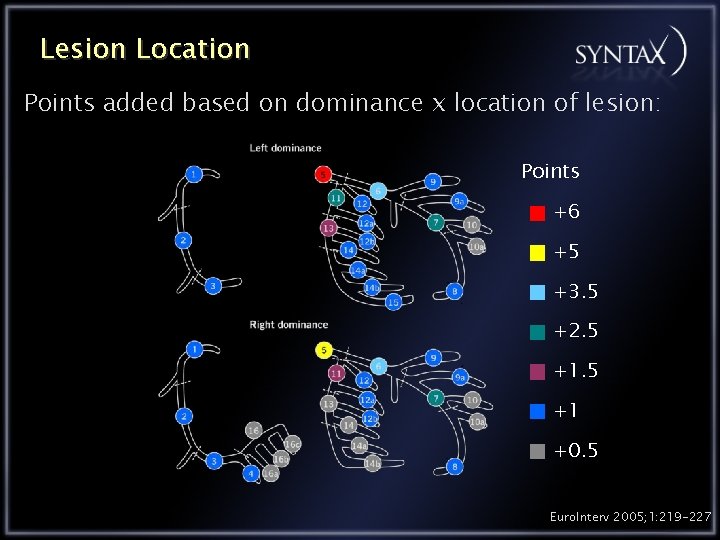
Lesion Location Points added based on dominance x location of lesion: Points +6 +5 +3. 5 +2. 5 +1 +0. 5 Euro. Interv 2005; 1: 219 -227

Total Occlusions (I) Points added based on: Age >3 months or unknown Blunt occlusion +1 Bridging occlusion +1 +1 Euro. Interv 2005; 1: 219 -227
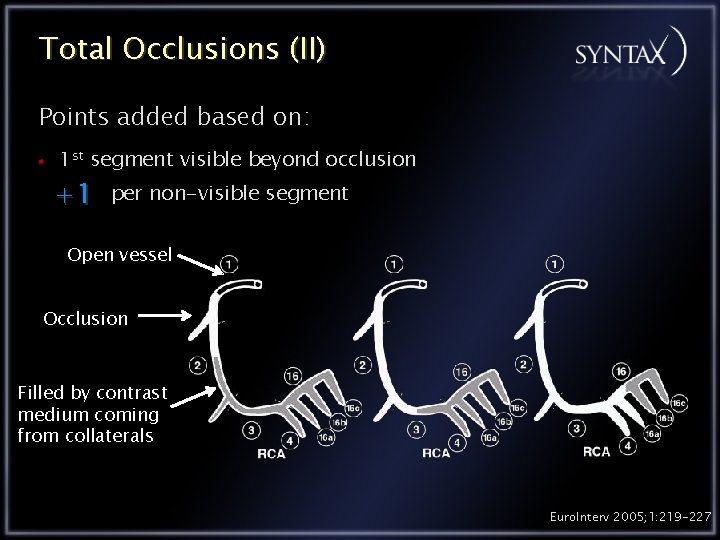
Total Occlusions (II) Points added based on: 1 st segment visible beyond occlusion +1 per non-visible segment Open vessel Occlusion Filled by contrast medium coming from collaterals Euro. Interv 2005; 1: 219 -227
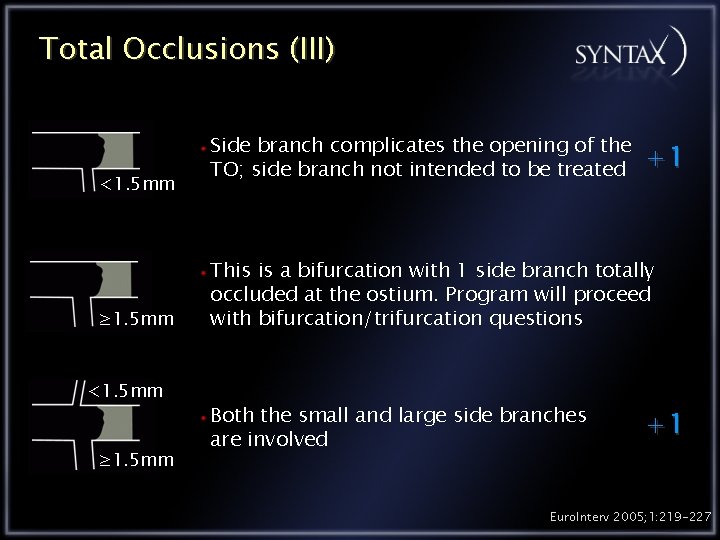
Total Occlusions (III) <1. 5 mm ≥ 1. 5 mm Side branch complicates the opening of the TO; side branch not intended to be treated +1 This is a bifurcation with 1 side branch totally occluded at the ostium. Program will proceed with bifurcation/trifurcation questions Both the small and large side branches are involved +1 Euro. Interv 2005; 1: 219 -227
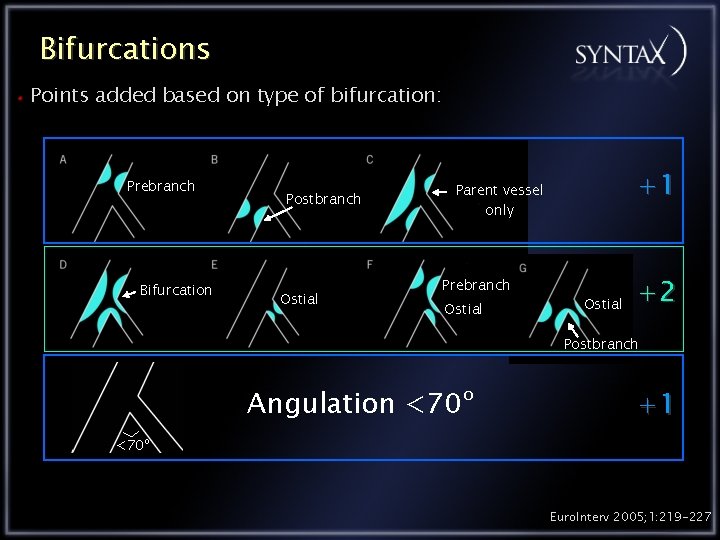
Bifurcations Points added based on type of bifurcation: Prebranch Bifurcation Postbranch Ostial +1 Parent vessel only Prebranch Ostial +2 Postbranch Angulation <70º +1 <70º Euro. Interv 2005; 1: 219 -227
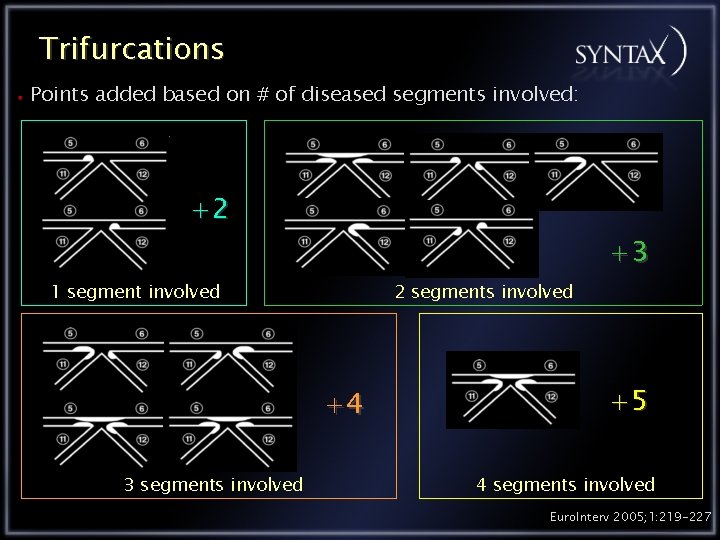
Trifurcations Points added based on # of diseased segments involved: +2 +3 1 segment involved 2 segments involved +4 3 segments involved +5 4 segments involved Euro. Interv 2005; 1: 219 -227
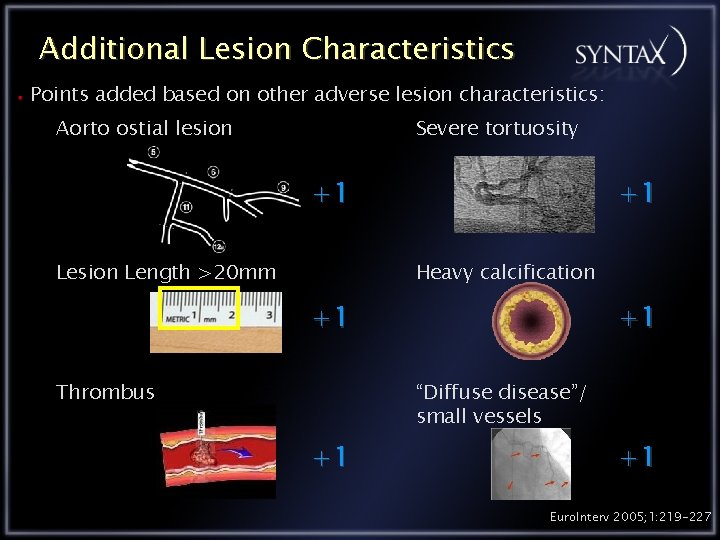
Additional Lesion Characteristics Points added based on other adverse lesion characteristics: Aorto ostial lesion Severe tortuosity +1 Lesion Length >20 mm +1 Heavy calcification +1 Thrombus +1 “Diffuse disease”/ small vessels +1 +1 Euro. Interv 2005; 1: 219 -227

Example Case: Patient 2 (I) RCA 100% Lesion 1 • Segment 1: 1 x 5 • Age T. O. is unknown • + Blunt stump • + side branch • First segment visualized by contrast: 4 • +Tortuosity • +Heavy calcification • +Length Lesion 1 Score: 5 1 1 1 3 2 2 1 16
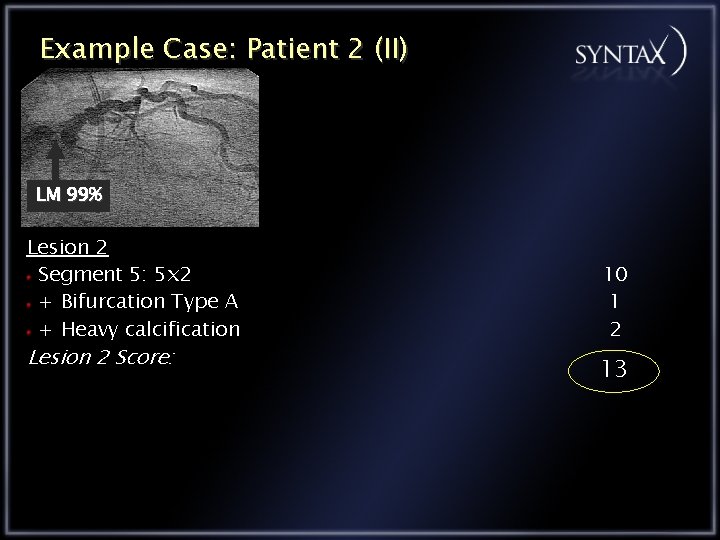
Example Case: Patient 2 (II) LM 99% Lesion 2 Segment 5: 5 x 2 + Bifurcation Type A + Heavy calcification Lesion 2 Score: 10 1 2 13
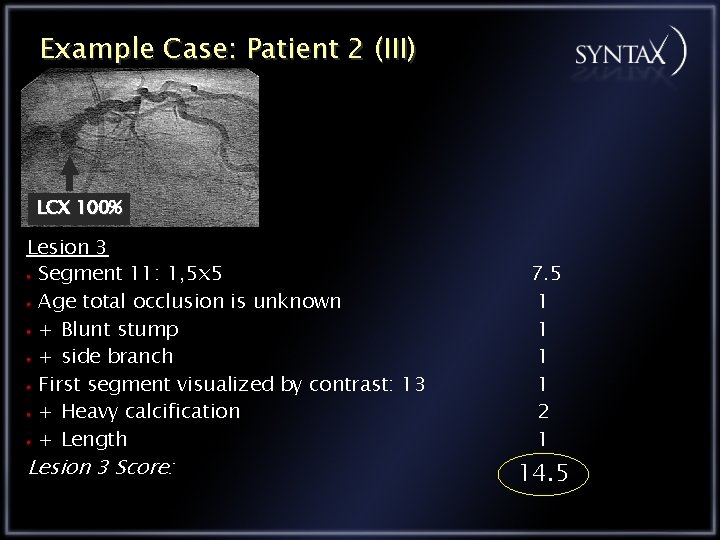
Example Case: Patient 2 (III) LCX 100% Lesion 3 Segment 11: 1, 5 x 5 Age total occlusion is unknown + Blunt stump + side branch First segment visualized by contrast: 13 + Heavy calcification + Length Lesion 3 Score: 7. 5 1 1 2 1 14. 5
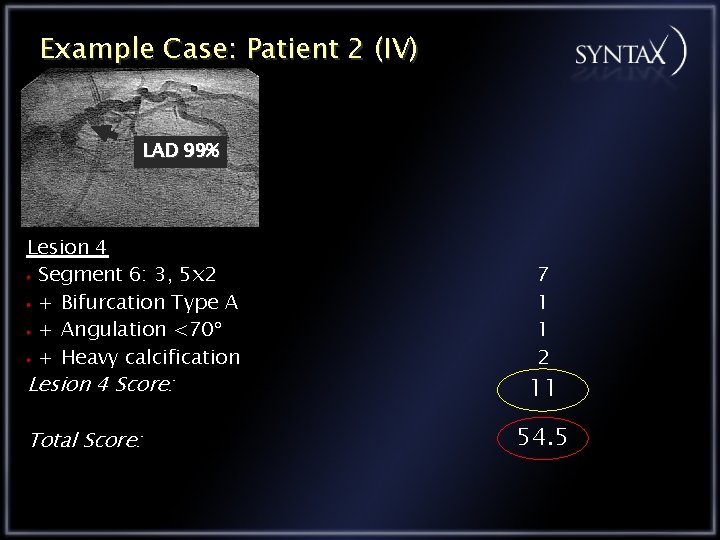
Example Case: Patient 2 (IV) LAD 99% Lesion 4 Segment 6: 3, 5 x 2 + Bifurcation Type A + Angulation <70 + Heavy calcification Lesion 4 Score: Total Score: 7 1 1 2 11 54. 5
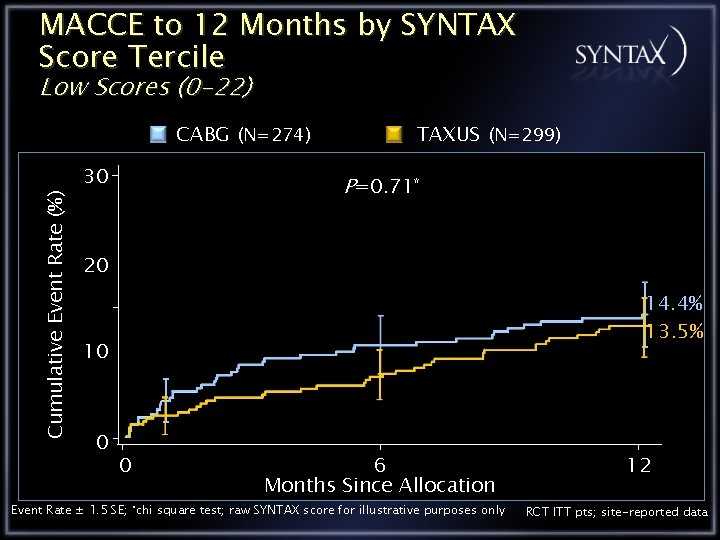
MACCE to 12 Months by SYNTAX Score Tercile Low Scores (0 -22) Cumulative Event Rate (%) CABG (N=274) 30 TAXUS (N=299) P=0. 71* 20 14. 4% 13. 5% 10 0 0 6 Months Since Allocation Event Rate ± 1. 5 SE; *chi square test; raw SYNTAX score for illustrative purposes only 12 RCT ITT pts; site-reported data
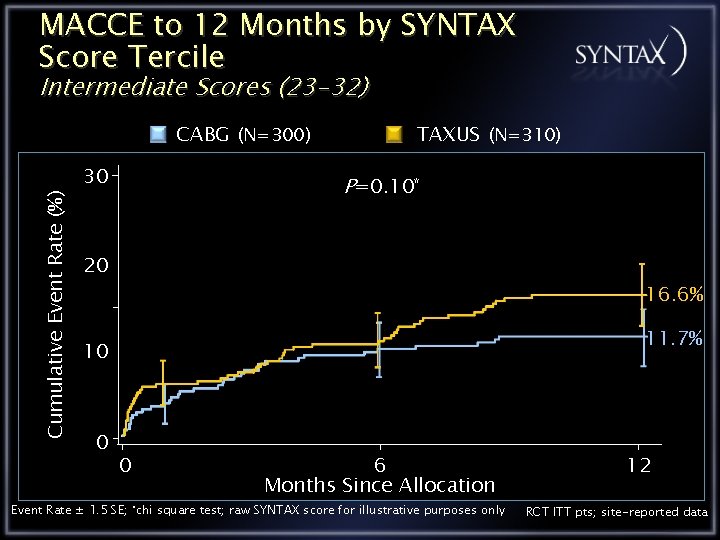
MACCE to 12 Months by SYNTAX Score Tercile Intermediate Scores (23 -32) Cumulative Event Rate (%) CABG (N=300) 30 TAXUS (N=310) P=0. 10* 20 16. 6% 11. 7% 10 0 0 6 Months Since Allocation Event Rate ± 1. 5 SE; *chi square test; raw SYNTAX score for illustrative purposes only 12 RCT ITT pts; site-reported data
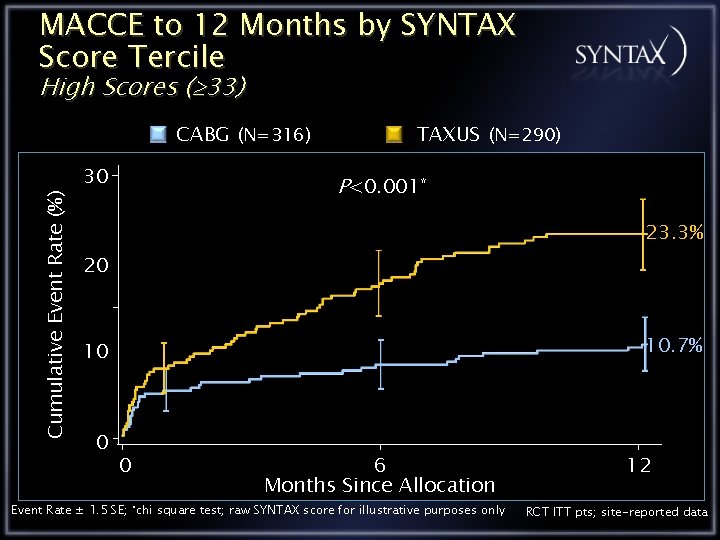
MACCE to 12 Months by SYNTAX Score Tercile High Scores ( 33) Cumulative Event Rate (%) CABG (N=316) 30 TAXUS (N=290) P<0. 001* 23. 3% 20 10. 7% 10 0 0 6 Months Since Allocation Event Rate ± 1. 5 SE; *chi square test; raw SYNTAX score for illustrative purposes only 12 RCT ITT pts; site-reported data
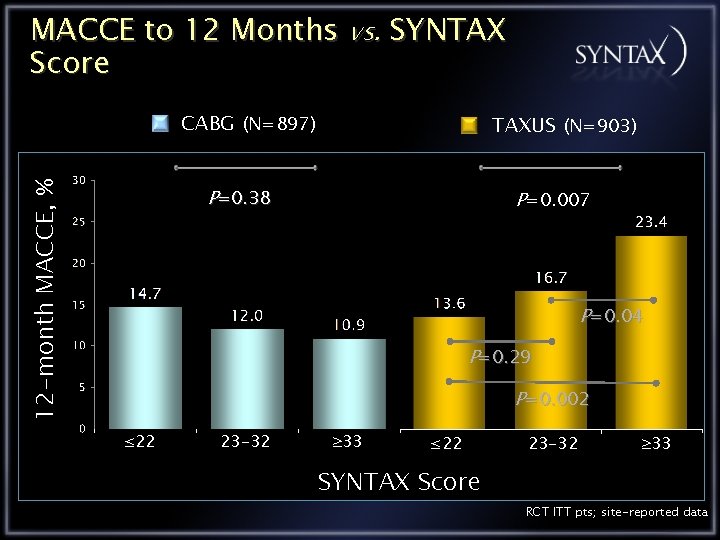
MACCE to 12 Months vs. SYNTAX Score 12 -month MACCE, % CABG (N=897) TAXUS (N=903) P=0. 38 P=0. 007 P=0. 04 P=0. 29 P=0. 002 ≤ 22 23 -32 33 SYNTAX Score RCT ITT pts; site-reported data
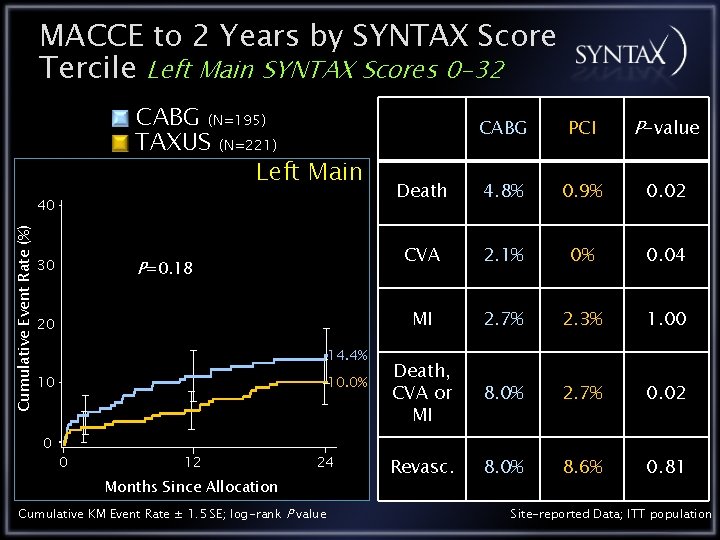
MACCE to 2 Years by SYNTAX Score Tercile Left Main SYNTAX Scores 0 -32 CABG (N=195) TAXUS (N=221) Left Main Cumulative Event Rate (%) 40 30 P=0. 18 20 14. 4% 10. 0% 10 0 0 12 24 Months Since Allocation Cumulative KM Event Rate ± 1. 5 SE; log-rank P value CABG PCI P-value Death 4. 8% 0. 9% 0. 02 CVA 2. 1% 0% 0. 04 MI 2. 7% 2. 3% 1. 00 Death, CVA or MI 8. 0% 2. 7% 0. 02 Revasc. 8. 0% 8. 6% 0. 81 Site-reported Data; ITT population
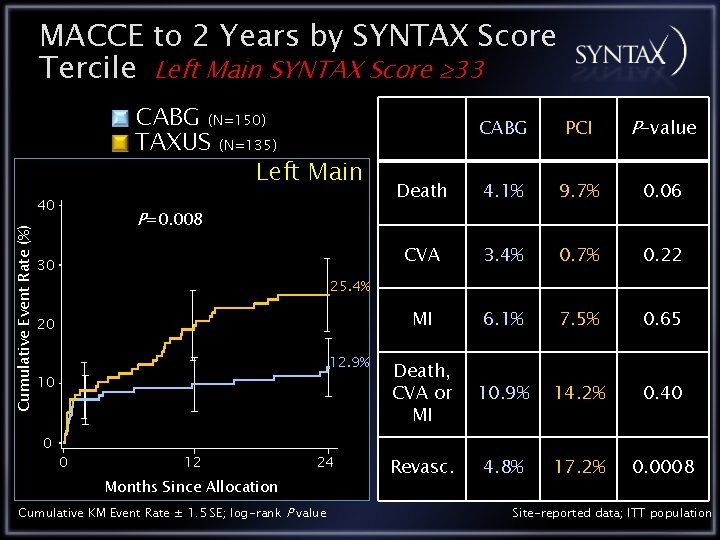
MACCE to 2 Years by SYNTAX Score Tercile Left Main SYNTAX Score 33 CABG (N=150) TAXUS (N=135) Left Main Cumulative Event Rate (%) 40 PCI P-value Death 4. 1% 9. 7% 0. 06 CVA 3. 4% 0. 7% 0. 22 MI 6. 1% 7. 5% 0. 65 Death, CVA or MI 10. 9% 14. 2% 0. 40 Revasc. 4. 8% 17. 2% 0. 0008 P=0. 008 30 25. 4% 20 12. 9% 10 0 CABG 0 12 24 Months Since Allocation Cumulative KM Event Rate ± 1. 5 SE; log-rank P value Site-reported data; ITT population
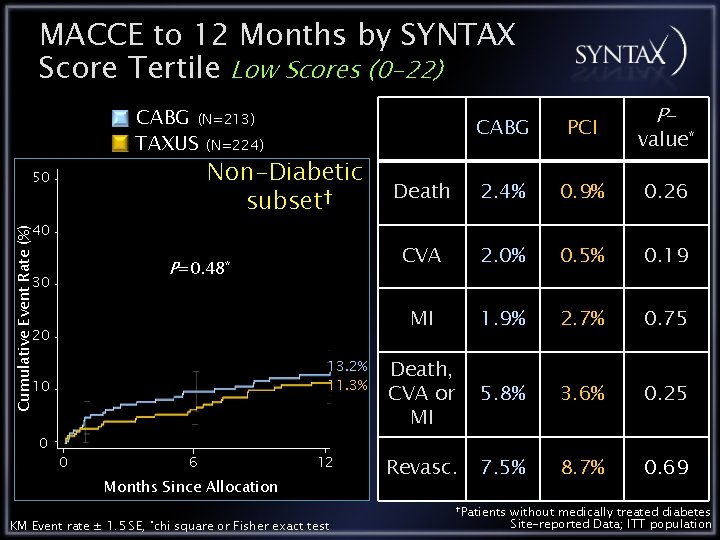
MACCE to 12 Months by SYNTAX Score Tertile Low Scores (0 -22) CABG (N=213) TAXUS (N=224) Non-Diabetic subset† 50 Cumulative Event Rate (%) 40 P=0. 48* 30 20 13. 2% 11. 3% 10 0 0 6 12 Months Since Allocation KM Event rate ± 1. 5 SE, *chi square or Fisher exact test P- CABG PCI Death 2. 4% 0. 9% 0. 26 CVA 2. 0% 0. 5% 0. 19 MI 1. 9% 2. 7% 0. 75 Death, CVA or MI 5. 8% 3. 6% 0. 25 Revasc. 7. 5% 8. 7% 0. 69 †Patients value* without medically treated diabetes Site-reported Data; ITT population
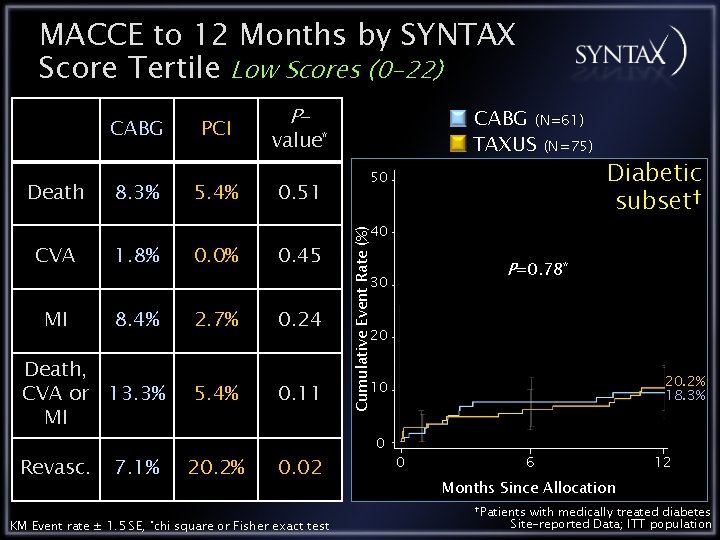
MACCE to 12 Months by SYNTAX Score Tertile Low Scores (0 -22) Death CVA 8. 3% 1. 8% PCI 5. 4% 0. 0% P- CABG (N=61) TAXUS (N=75) value* 0. 51 0. 45 50 P=0. 78* 30 MI 8. 4% Death, CVA or 13. 3% MI Revasc. 7. 1% KM Event rate ± 1. 5 SE, *chi 2. 7% 5. 4% 20. 2% 0. 24 0. 11 0. 02 square or Fisher exact test Diabetic subset† 40 Cumulative Event Rate (%) CABG 20 20. 2% 18. 3% 10 0 0 6 12 Months Since Allocation †Patients with medically treated diabetes Site-reported Data; ITT population
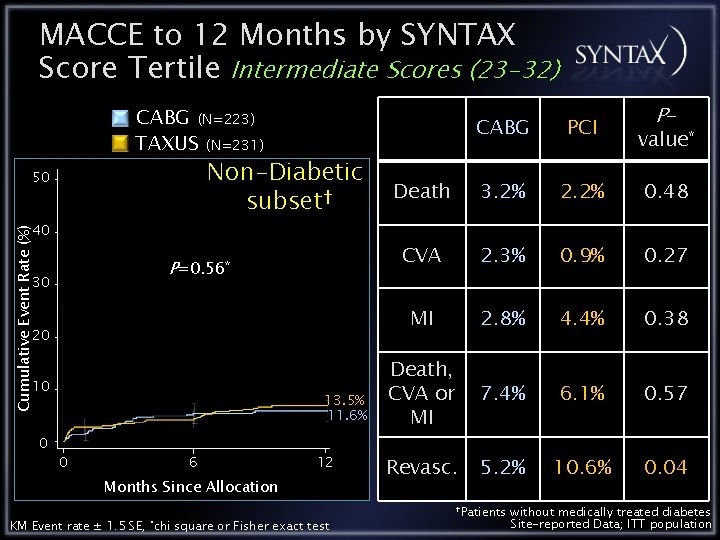
MACCE to 12 Months by SYNTAX Score Tertile Intermediate Scores (23 -32) CABG (N=223) TAXUS (N=231) Non-Diabetic subset† 50 Cumulative Event Rate (%) 40 P=0. 56* 30 20 10 0 13. 5% 11. 6% 0 6 12 Months Since Allocation KM Event rate ± 1. 5 SE, *chi square or Fisher exact test P- CABG PCI Death 3. 2% 2. 2% 0. 48 CVA 2. 3% 0. 9% 0. 27 MI 2. 8% 4. 4% 0. 38 Death, CVA or MI 7. 4% 6. 1% 0. 57 Revasc. 5. 2% 10. 6% 0. 04 †Patients value* without medically treated diabetes Site-reported Data; ITT population
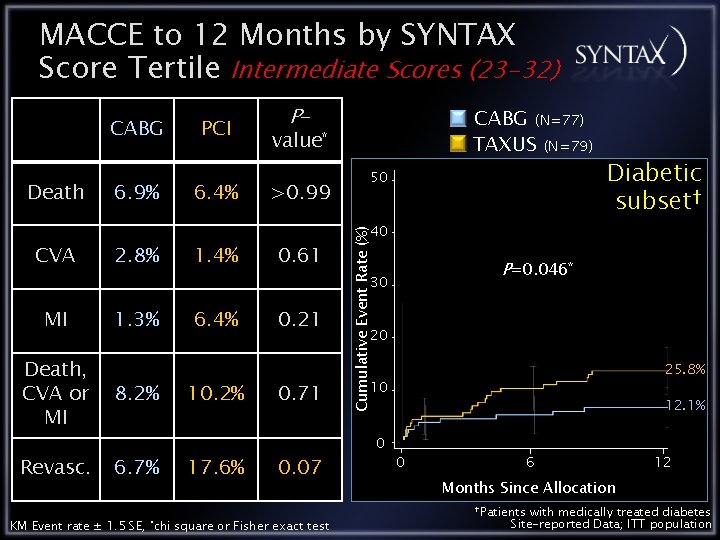
MACCE to 12 Months by SYNTAX Score Tertile Intermediate Scores (23 -32) Death CVA 6. 9% 2. 8% PCI 6. 4% 1. 4% P- CABG (N=77) TAXUS (N=79) value* >0. 99 0. 61 50 P=0. 046* 30 MI 1. 3% Death, CVA or MI 8. 2% Revasc. 6. 7% KM Event rate ± 1. 5 SE, *chi 6. 4% 10. 2% 17. 6% 0. 21 0. 71 0. 07 square or Fisher exact test Diabetic subset† 40 Cumulative Event Rate (%) CABG 20 25. 8% 10 0 12. 1% 0 6 12 Months Since Allocation †Patients with medically treated diabetes Site-reported Data; ITT population
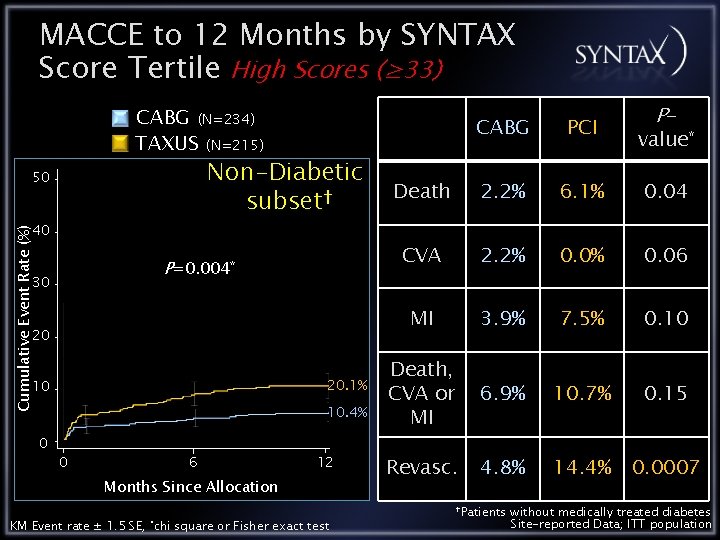
MACCE to 12 Months by SYNTAX Score Tertile High Scores (≥ 33) CABG (N=234) TAXUS (N=215) Non-Diabetic subset† 50 Cumulative Event Rate (%) 40 P=0. 004* 30 20 20. 1% 10 10. 4% 0 0 6 12 Months Since Allocation KM Event rate ± 1. 5 SE, *chi square or Fisher exact test P- CABG PCI Death 2. 2% 6. 1% 0. 04 CVA 2. 2% 0. 06 MI 3. 9% 7. 5% 0. 10 Death, CVA or MI 6. 9% 10. 7% 0. 15 Revasc. 4. 8% 14. 4% 0. 0007 †Patients value* without medically treated diabetes Site-reported Data; ITT population
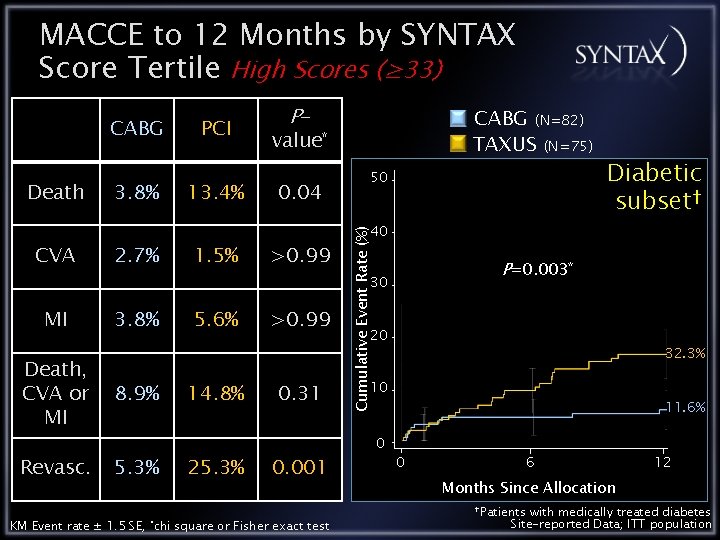
MACCE to 12 Months by SYNTAX Score Tertile High Scores (≥ 33) Death CVA 3. 8% 2. 7% PCI 13. 4% 1. 5% P- CABG (N=82) TAXUS (N=75) value* 0. 04 >0. 99 50 P=0. 003* 30 MI 3. 8% Death, CVA or MI 8. 9% Revasc. 5. 3% KM Event rate ± 1. 5 SE, *chi 5. 6% 14. 8% 25. 3% >0. 99 0. 31 0. 001 square or Fisher exact test Diabetic subset† 40 Cumulative Event Rate (%) CABG 20 32. 3% 10 0 11. 6% 0 6 12 Months Since Allocation †Patients with medically treated diabetes Site-reported Data; ITT population
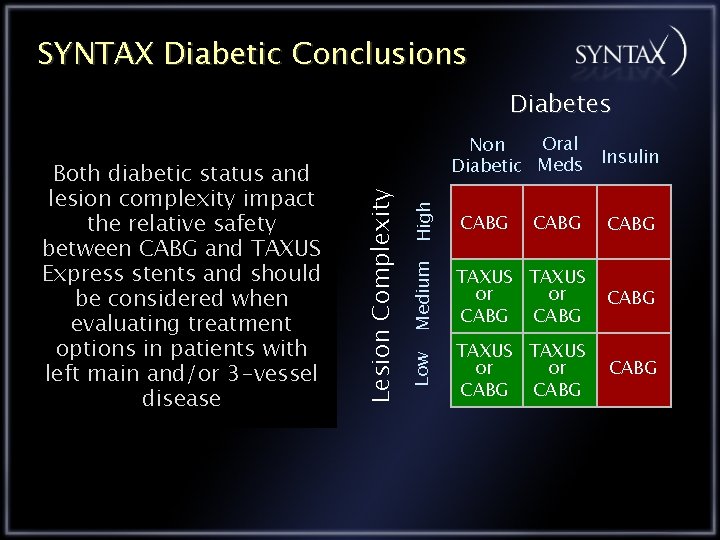

SYNTAX Diabetic Conclusions Diabetes High CABG Medium TAXUS or or CABG Low Lesion Complexity Both diabetic status and lesion complexity impact the relative safety between CABG and TAXUS Express stents and should be considered when evaluating treatment options in patients with left main and/or 3 -vessel disease Oral Non Insulin Diabetic Meds TAXUS or or CABG

Post SYNTAX PCI 6% CABG or PCI 28% CABG 66% Results of the SYNTAX trial suggest that 66 % of all patients are still best treated with CABG, however, for the remaining patients PCI is an excellent alternative to surgery at least for one year

? s e in l e id u G e h t e g n a h C to e Tim Circ Cardiovasc Intervent 2009; 2: 59 -68
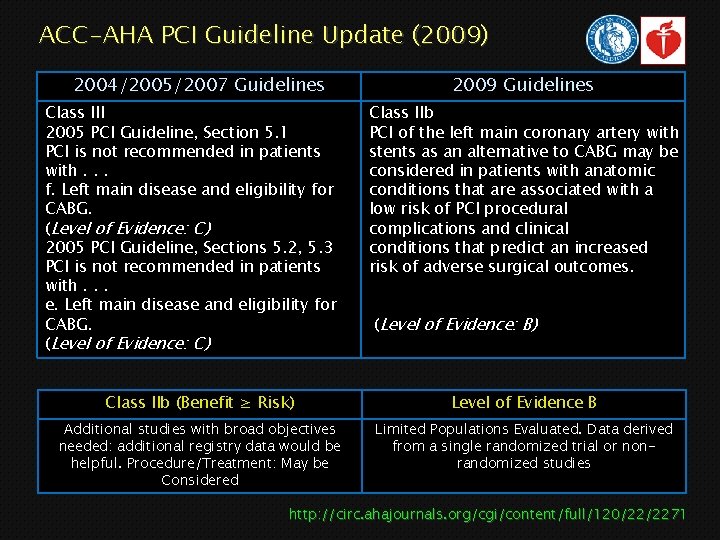

ACC-AHA PCI Guideline Update (2009) 2004/2005/2007 Guidelines Class III 2005 PCI Guideline, Section 5. 1 PCI is not recommended in patients with. . . f. Left main disease and eligibility for CABG. (Level of Evidence: C) 2005 PCI Guideline, Sections 5. 2, 5. 3 PCI is not recommended in patients with. . . e. Left main disease and eligibility for CABG. (Level of Evidence: C) 2009 Guidelines Class IIb PCI of the left main coronary artery with stents as an alternative to CABG may be considered in patients with anatomic conditions that are associated with a low risk of PCI procedural complications and clinical conditions that predict an increased risk of adverse surgical outcomes. (Level of Evidence: B) Class IIb (Benefit ≥ Risk) Level of Evidence B Additional studies with broad objectives needed: additional registry data would be helpful. Procedure/Treatment: May be Considered Limited Populations Evaluated. Data derived from a single randomized trial or nonrandomized studies http: //circ. ahajournals. org/cgi/content/full/120/22/2271

Summary The SYNTAX score is a new, innovative tool to describe the complexity of vasculature The raw SYNTAX score is a good predictor of MACCE PCI patients with low and intermediate SYNTAX scores have similar 12 -month MACCE rates to CABG patients 12 -month MACCE rates in CABG patients are comparable between patients with high or low SYNTAX scores Increasing SYNTAX scores (and lesion complexity) are related to increased adverse outcomes in PCI, whereas outcomes of CABG are independent of SYNTAX score

Future Projects Discussions around integrating the SYNTAX Score software into cath lab systems Consideration of producing a PDA/i. Phone version of the syntaxscore. com website Development of a Clinical Syntaxscore to include limited non-anatomic variables (e. g. diabetes) Integrating the SYNTAX Score with the euro. SCORE Adding the SYNTAX outcomes at years 3 -5 to the SYNTAX Score website

QUESTIONS ?
- Slides: 45