Whats so Special about Specialty Pharmacy What Makes

What’s so Special about Specialty Pharmacy?

What Makes a Drug "Special"

enoxaparin is classified as a specialty drug? A. True B. False

Specialty Drugs No universally accepted definition The FDA does not have a definition or a list same drug may or may not be considered a specialty drug by insurer, drug manufacturer, pharmacy, hospital, etc.

Specialty Drugs: Potential Characteristics Expensive Used to treat complex and/or rare condition Require Unique special handling administration Require high patient touch – counseling, monitoring, support, etc.

Specialty Drugs: Expensive CMS definition of a specialty drug is one with a cost of $600 or more per month. Total part D spending in 2015 for ledipasvir/sofosbuvir was $7, 030, 633, 485. 80, $92, 846. 74 per user For 2015, All Drugs with Annual Per-User Spending >$10 K for Medicare part D was $37. 9 B, 28% of total program spending Total part D spending in 2015 for enoxaparin was $316, 414, 099. 85, $777. 64 per user
Specialty Drugs: Treat Complex and Rare Conditions nusinersen Infantile spinal muscular atrophy 1 in 6, 000 to 1 in 10, 000 live births
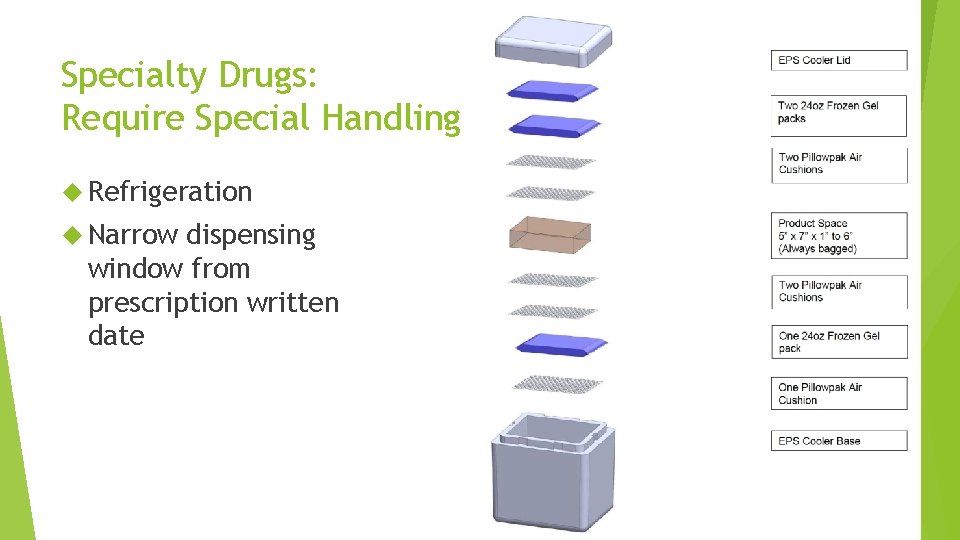
Specialty Drugs: Require Special Handling Refrigeration Narrow dispensing window from prescription written date
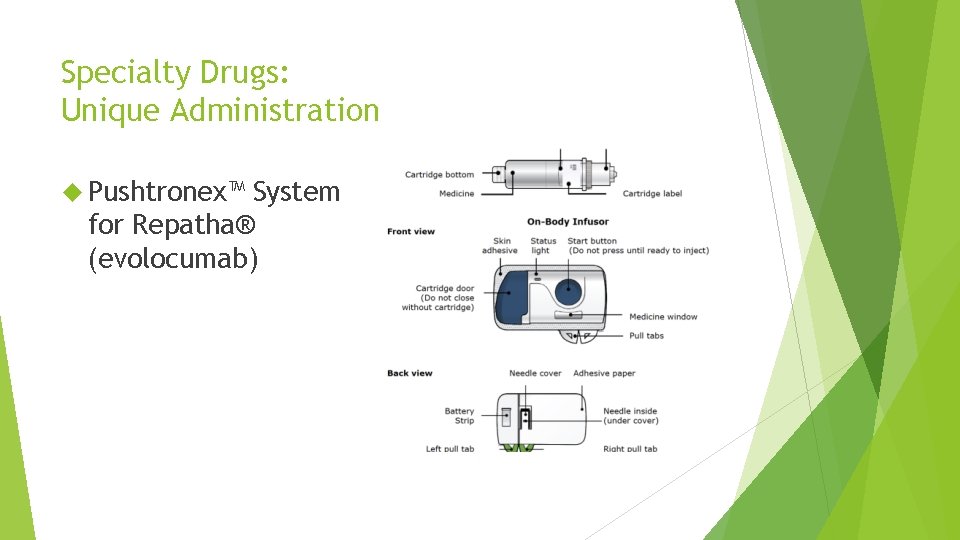
Specialty Drugs: Unique Administration Pushtronex™ System for Repatha® (evolocumab)

Specialty Drugs: Require High Patient Touch Tacrolimus May have frequent dose changes based on trough values Frequent monitoring for side effects to ensure compliance Complex billing to Medicare part B Changes in manufacturer strongly discouraged

For your Consideration Should we have a standardized definition of a specialty drug?

Hap. Epil is a new drug on the market. Which of the following would NOT make it a specialty drug? A. It must be kept below 45 degrees at all times B. It costs $150 per month C. It treats a very rare condition D. Drug is administered by injection

What makes a pharmacy a specialty pharmacy?

In order to be a specialty pharmacy, a pharmacy must be accredited by: A. The Joint Commission B. Utilization Review Accreditation Commission (URAC) C. Accreditation commission for Health Care (ACHC) D. None of the Above

The Specialty Pharmacy No universal definition Accreditation is not required to designate a pharmacy as a specialty pharmacy In the increasingly competitive specialty landscape, accreditation is becoming necessary to contend

Specialty Pharmacies – Dispense Specialty Drugs Specialty Pharmacies dispense specialty drugs. . . …. . . wait didn't we say there was no definition of a specialty drug? May also dispense non-specialty drugs May be low volume – Walgreens local specialty averaged about 50 scripts a day at one point May be high volume – Frisco central fill averages around 700 scripts per day

Specialty Pharmacies – Equipped to handle complex billing Prior Authorization Medical Billing billing multiple payers Securing financial assistance

Specialty Pharmacies – Staff may have specialized training Clinicians Viroligy, HIV training Administration Specialty training billing training

Specialized Pharmacies – Support Programs May have special programs to support patients and increase adherence Allow the pharmacy staff to closely monitor the patient Proactive care, often calling patient when refills are due May offer special services aiming to increase adherence such as delivery of medication to patient's home or doctor's office.

Specialized Pharmacies - Reporting Many specialty drugs require comprehensive reporting and the pharmacy must be equipped to handle this Reporting may be required by the manufactureer, the FDA, the patient's private insurance, medicare/medicaid, or an accrediting third party Near 0% deviation is expected in reporting completion and accuracy Revlamid® only allows 3 deviations per year before suspending access

Drug Access Restrictions and Limitations

Susie Q presents to the pharmacy with a prescription for sofosbuvir/velpatasvir. You order the drug and receive it the next day but when you bill Susie’s insurance the claim is rejected with the following message: “Pharmacy not in network. Must be filled by Hoptom Mail Order Pharmacy. Call 888888 -8888 to transfer prescription. ” sofosbuir/velpatasvir is a example of : A. A Payer Restricted Access Drug B. A Limited Distribution Drug C. Both A and B

Payer Restricted Drug Access Insurance companies may restrict access by only covering specialty medication if it is filled at a specialty pharmacy of their designation This allows the payer to more tightly control costs and negotiate prices Sometimes payers will allow first fill or an emergency fill outside the network

Limited Distribution Drugs The manufacturer limits the number of pharmacies that can obtain the drug. The FDA may mandate that a drug be LDD Manufactures may autonomously decide to limit access to certain pharmacies that can provide things like: Risk evaluations Outcomes data Special documentation Clinical expertise Support for Patients Compliance/side effect monitoring

LDD’s in the Retail Setting – Who has access? Local Access is limited: Presbyterian Specialty Pharmacy – Aubagio Walgreens at Lovelace Hospital (Towers) - Daraprim, Iressa, Lynparza, Tagrisso Walgreens at Lovelace (Journal Center) – Cosentyx, Nucala Walgreens at Presbyterian Hospital Downtown –Iressa, Lynparza, Tagrisso Most local pharmacies refer specialty scripts to a central fill or specialty partner Costco- Diplomat Specialty CVS - CVS specialty Walgreens – Walgreens specialty Wal-Mart/Sams Club – Wal-mart specialty

How does a pharmacy get LDD access? For new drugs - pharmacies work with manufactures well before drugs are even approved Negotiations for access are often started while the drug is still undergoing clinical trials A drug may come to market with limited access and then move to regular distribution To gain access to LDDs already on the market, accreditation by a 3 rd party is often required Contact the drug manufacturer directly to get information on their application process

Specialty Drug Billing

Specialty Drug Billing High Cost Prior Authorization usually required May require billing multiple payers Medicare part B may be payer Additional Financial Assistance

Prior Authorization Drug companies may have “drug access specialist” to facilitate the PA process Cover. My. Meds – “A free system that automates prior authorization requests, saving countless administrative hours on the phone and sending faxes to health plans. ” – Cover. My. Meds. com Doctor’s office’s often have their own workflow/personnel to handle prior auths –

Medicare Part B - Coverage Medicare Part B provides coverage for certain durable medical equipment supplies, prescriptions that can’t be self-administered, and certain selfadministered anti-cancer drugs

Medicare Part B - Requirements In order to use Medicare Part B benefits, the following requirements must be met: • The patient must have Medicare Part B coverage • The item must be a Medicare Part B approved item • The item must be a medical necessity as defined by Medicare (verify ICD-10 code is a covered diagnosis code)

Medicare Part B – Deductible and Co-Pays The patient must pay all costs until he/she meets the yearly Part B deductible ($166. 00 for 2016). Then Medicare pays its share and the patient pays the copay, which is typically 20% of the Medicare-approved amount for prescriptions. If the patient has a supplemental insurance or Medicaid, the deductible and copay are $0. If the patient has ONLY Medicare Part B coverage, the following copay applies: Medical and Other Services: 20% of the Medicare-approved amount for most preventative services and durable medical equipment.

Insulin Humalog Humalin Novalog Medication must be administered in a pump The Infusion pump make/model and date of purchase (mm/yyyy) on claim Medicare must have paid for the pump

Anti-Cancer: Oral Alkeran (Melphalan) Cytoxan (Cyclophosphamide) Hycamtin (Topotecan) Methotrexate (Trexall) Myleran (Busulfan) Temodar (Temozolmide) Vepisid (Etoposide) Xeloda (Capecitabine) Medication must be used for treatment of Cancer

Antiemetic: Oral Anzemet 100 mg Atarax 25 mg, 50 mg Benadryl 50 mg Compazine 5 mg, 10 mg Dexamethasone. 25 mg Emend 5 mg Kytril 1 mg Marinol 2. 5 mg, 5 mg Nabilone 1 mg Phenergan 12. 5 mg, 25 mg Thorazine 10 mg, 25 mg Tigan 250 mg Torecan 10 mg Trilafon 4 mg, 8 mg Zofran (Ondansetron) 8 mg Medication must have been ordered as a full therapeutic replacement of IV drugs. Initial dose of medication must be administered 2 hours before or 48 hours after administration of chemotherapy drug. Patient must be on chemotherapy and have a cancer diagnosis.

Immunosuppressive Cellcept 250 mg (Mycophenolate) Imuran (Azathioprine) 50 mg, 100 mg Methylprednisolone (Medrol) 4 mg Myfortic (Mycophenolic) Neoral (Sandimune/Gengraf/Cyclosporin e) 25 mg, 100 mg Prednisone 5 mg, 10 mg Prednisolone 4 mg Prograf 1 mg (Tacrolimus) Rapamune 1 mg (Sirolimus) Patient must have had a covered organ transplant Patient must have been enrolled in Medicare Part A when transplant occurred
Inhalation Albuterol 0. 083%, 0. 5% Alupent 0. 4%, 0. 6%, 5% Atrovent Broncho Saline Brovana Cromolyn Sodium Duoneb Iloprost Ipratropium Mucomyst 10%, 20% Nebupent Perforomist Proventil 0. 083%, 0. 5% Pulmicort Pulmozyme Tobramycin 6% Ventolin 0. 083%, 0. 5% Xopenex Medication must be administered in a nebulizer Patient must be diagnosed with a chronic pulmonary condition. (Conditions such as pneumonia, bronchitis, shortness of breath and cough are not covered by Medicare Part B)

Copay Assistance for Specialty Medications

Copay Assistance Cards Most copay cards are not valid for prescriptions covered by Medicare, Medicaid, or any federal/state funded program Check individual offer to verify if it can be used for patients with federal/state funded insurance You may get a paid claim, but you put yourself at risk for a chargeback Consider developing a consent form that allows you to complete enrolment on behalf of the patient. The following information should be included on the form as it is often requested to complete enrolment: Total number of people residing in the home Total combined annual income of the household

Copay Assistance Cards - Examples Drug Contact Limits Patient Activation INCIVEK (Hep C) 855 -837 -8394 Up to $10, 000/year Required Cell. Cept (Transplant) 877 -509 -2235 Up to $100 Not Required Nexavar (Oncology) 866 -639 -2827 Up to 95% of co- Required pay Ampyra(MS) 888 -881 -1918 Up to $500 Required

Grants Health. Well Foundation: 1 -800 -675 -8416 https: //healthwellfoundation 1 -866 -55 -COPAY Patient Access Network: http: //cancercarecopay. org 1 -866 -316 -7263 https: //www. panfoundation. org Cancer. Care Copayment Assistance Foundation: Patient Advocate Foundation: 1 -800 -532 -5274 http: //www. patientadvocate. org Good Days Fund: 1 -877 -968 -7233 https: //portal. mygooddays. org
- Slides: 41