What is Sickle Cell Disease What is Sickle









- Slides: 37

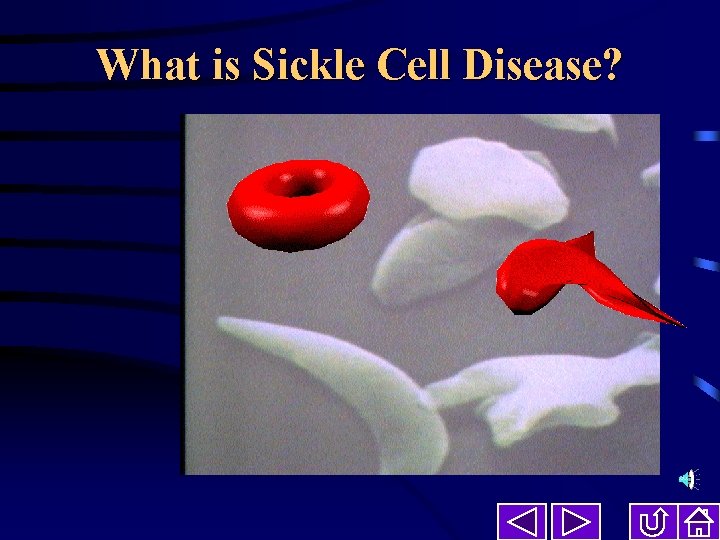
What is Sickle Cell Disease?

What is Sickle Cell Disease? • An inherited disease of red blood cells (erythocyctes) • Affects a protein inside the red blood cells called hemoglobin. • Sickle-shaped red cells interrupt blood flow by blocking small blood vessels • Tissue that has no blood flow is damaged and causes pain

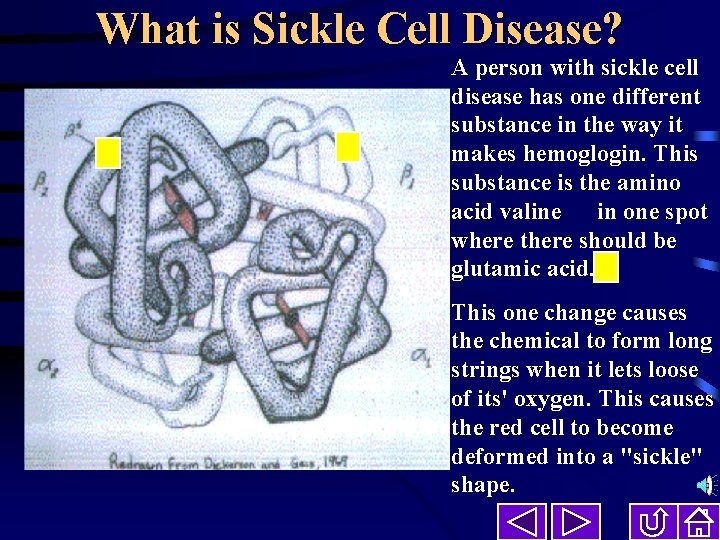
What is Sickle Cell Disease? A person with sickle cell disease has one different substance in the way it makes hemoglogin. This substance is the amino acid valine in one spot where there should be glutamic acid. This one change causes the chemical to form long strings when it lets loose of its' oxygen. This causes the red cell to become deformed into a "sickle" shape.

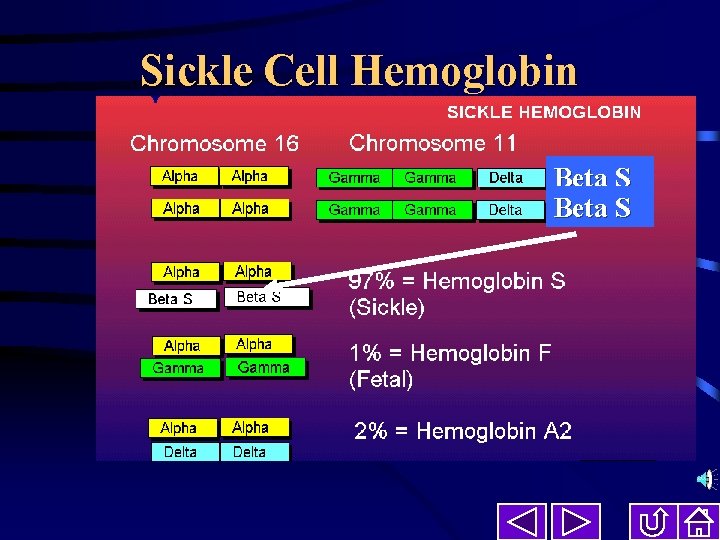
Sickle Cell Hemoglobin Beta S

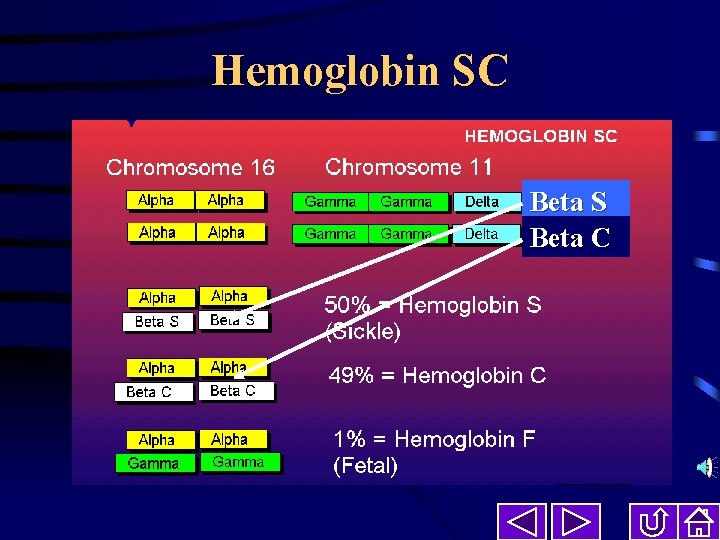
Hemoglobin SC Beta S Beta C

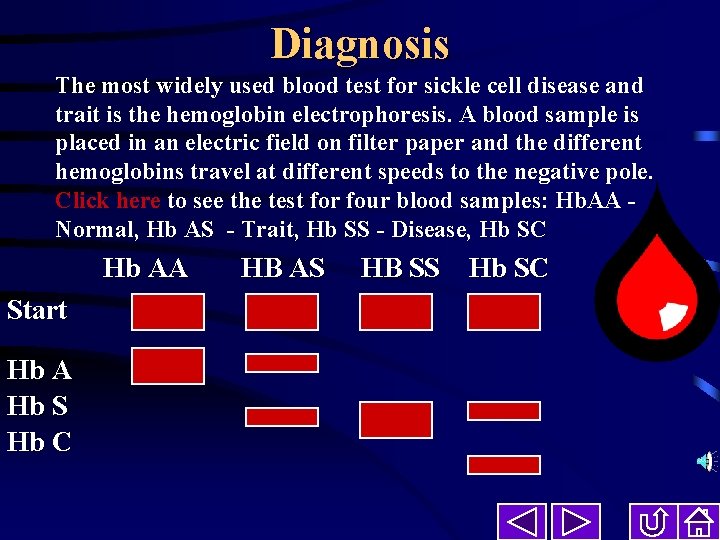
Diagnosis The most widely used blood test for sickle cell disease and trait is the hemoglobin electrophoresis. A blood sample is placed in an electric field on filter paper and the different hemoglobins travel at different speeds to the negative pole. Click here to see the test for four blood samples: Hb. AA Normal, Hb AS - Trait, Hb SS - Disease, Hb SC Hb AA Start Hb A Hb S Hb C HB AS HB SS Hb SC

Diagnosis Sickledex The presence of sickle hemoglobin can be rapidly determined by a five minute solubility test (Sickledex). This test is only helpful by excluding sickle cell disease when negative in a patient older than six months of age without severe anemia or a very high fetal hemoglobin level. It is impossible to separate sickle cell disease from trait with this test. The test is positive if 10 percent Hb S is present, making it impossible to separate sickle cell trait from individuals with disease

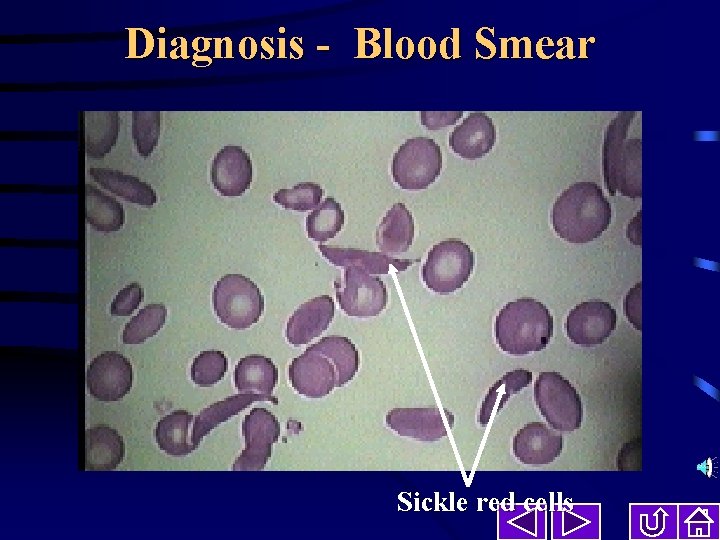
Diagnosis - Blood Smear Sickle red cells

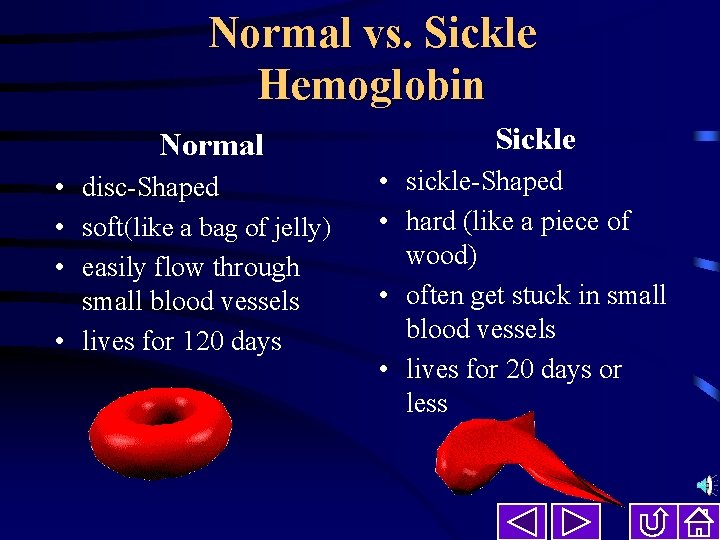
Normal vs. Sickle Hemoglobin Normal • disc-Shaped • soft(like a bag of jelly) • easily flow through small blood vessels • lives for 120 days Sickle • sickle-Shaped • hard (like a piece of wood) • often get stuck in small blood vessels • lives for 20 days or less

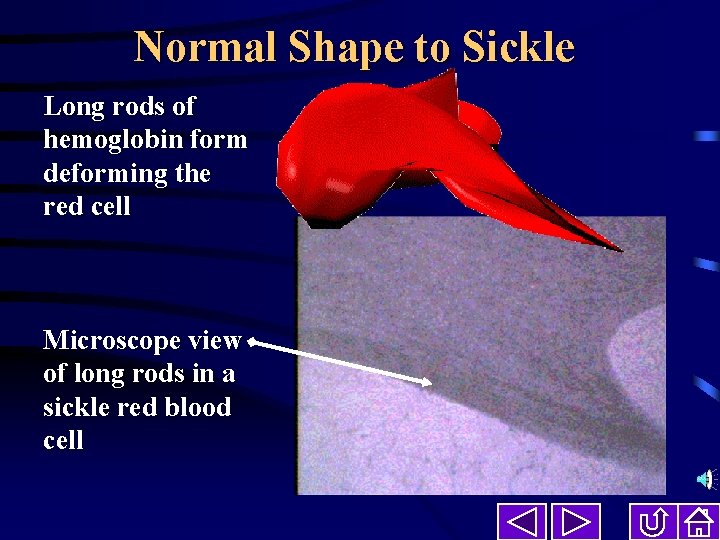
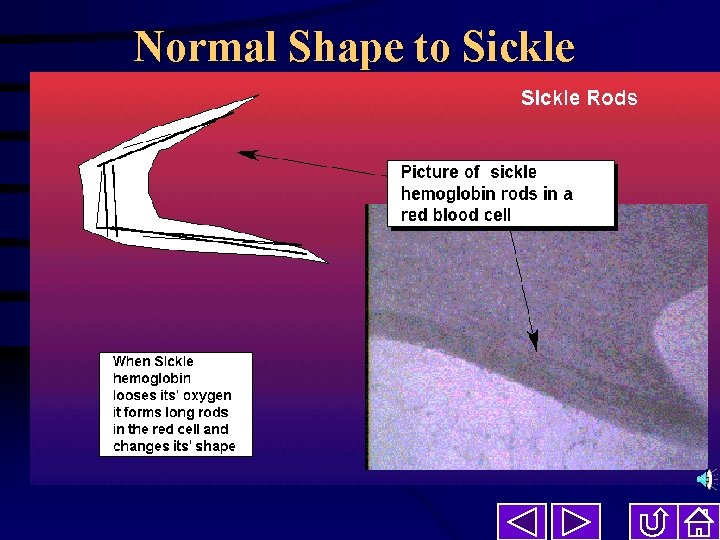
Normal Shape to Sickle Long rods of hemoglobin form deforming the red cell Microscope view of long rods in a sickle red blood cell

Normal Shape to Sickle

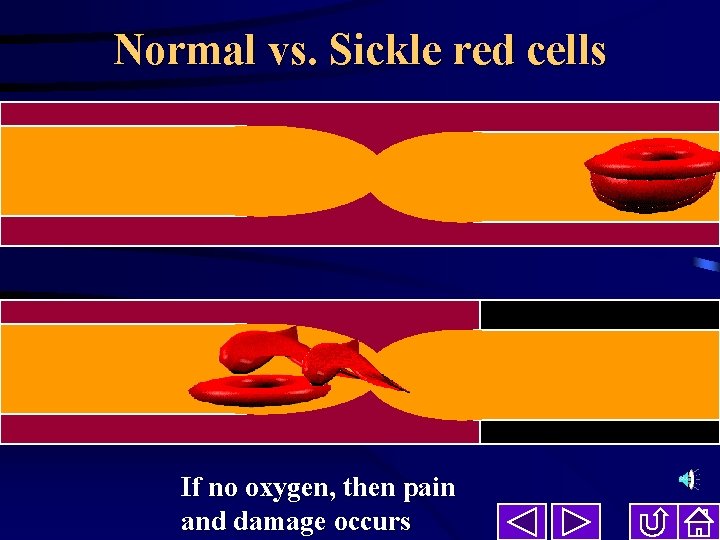
Normal vs. Sickle red cells If no oxygen, then pain and damage occurs

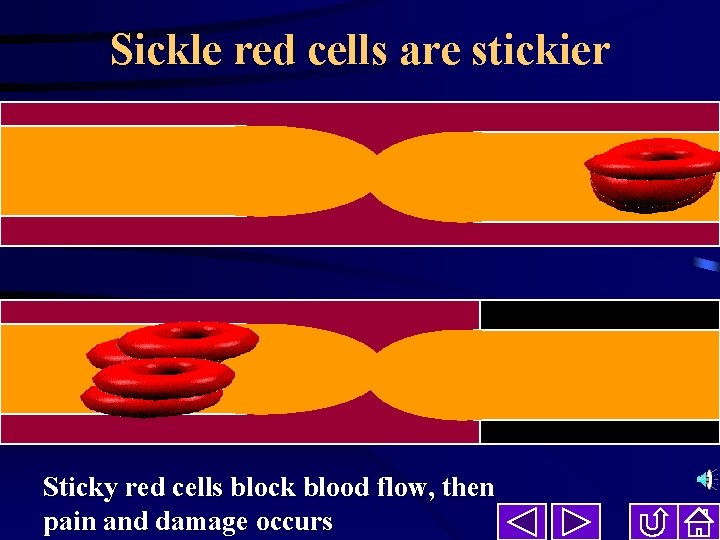
Sickle red cells are stickier Sticky red cells block blood flow, then pain and damage occurs

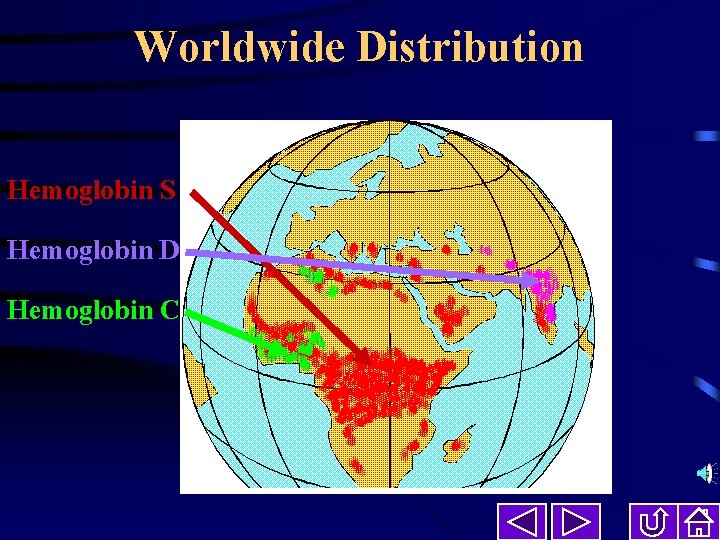
Worldwide Distribution Hemoglobin S Hemoglobin D Hemoglobin C

Worldwide Distribution Hemoglobin S Sickle Cell Disease is found in Africans, Turks, Greeks, Saudi Arabians, Egyptians, Iranians, Italians, Latin Americans and Asiatic Indians. Sickle cell disease is present in one out of four hundred African Americans in the United States. It is the most common genetic disease in this country. All new born babies should be tested at birth for sickle cell disease, so prevention can be started right away. A simple blood test can be done from the baby's blood.

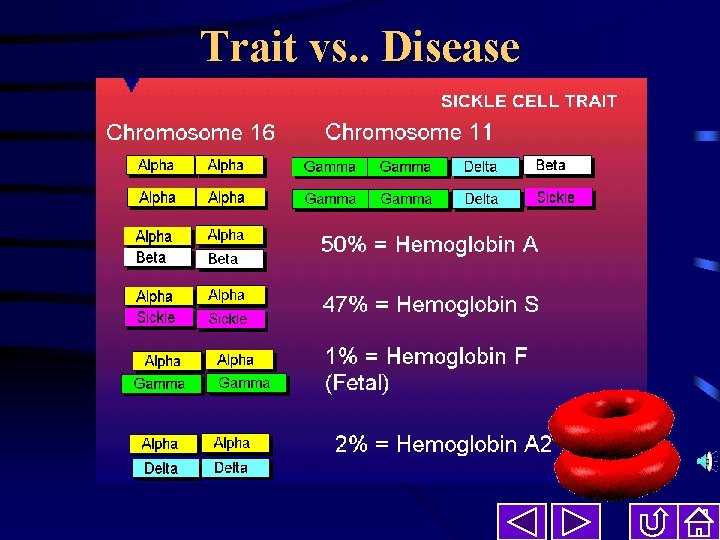
Trait vs. . Disease Sickle cell trait is present in one out of ten African Americans. About half of the hemoglobin in the red cell is sickle and the cell will exhibit sickling when under severe conditions of low oxygenation. Hematuria or blood in the urine is the most common problem. There are case reports of people with sickle cell trait having more severe sickle related problems when placed under severe conditions such as extreme pressure and low oxygen conditions. Those with trait should be advised of the risks of extreme physical activity, severe pressure changes, deep sea diving, and the possibility of hematuria.

Trait vs. . Disease

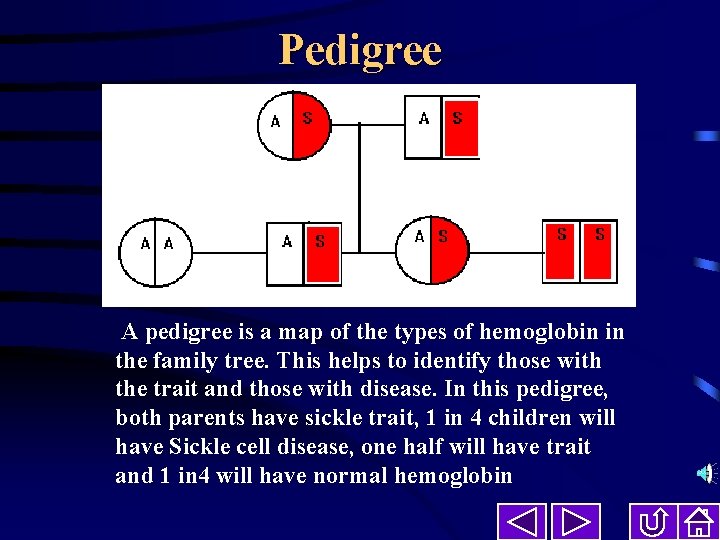
Pedigree A pedigree is a map of the types of hemoglobin in the family tree. This helps to identify those with the trait and those with disease. In this pedigree, both parents have sickle trait, 1 in 4 children will have Sickle cell disease, one half will have trait and 1 in 4 will have normal hemoglobin

Pedigree AA AS AS SS There are two genes for hemoglobin, one of which is inherited from each parent. If one normal gene and one abnormal gene is passed on by each parent, only half of the hemoglobin produced will be abnormal and the individual will be a carrier of the abnormal gene. This is commonly referred to as having the trait of the disease.

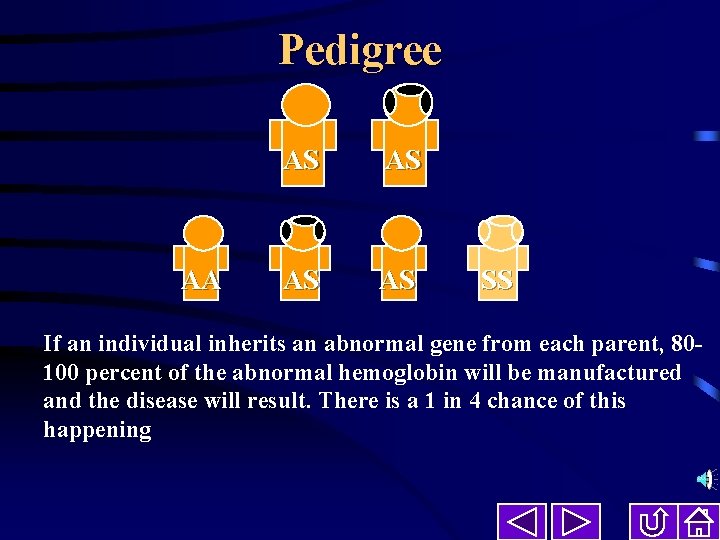
Pedigree AA AS AS SS If an individual inherits an abnormal gene from each parent, 80100 percent of the abnormal hemoglobin will be manufactured and the disease will result. There is a 1 in 4 chance of this happening

Managing Sickle Cell • • • Fluids Antibiotics Rest Pain Medication Prevention of infections Healthy lifestyle

Complications From Sickle Cell Disease • Sickle cells become trapped and destroyed in the spleen causing Splenic Sequestion • Shortage of red blood cells or anemia • Pain episodes • Stroke or Brain Damage • Kidney failure • Pneumonia or Chest Syndrome • Increased Infections

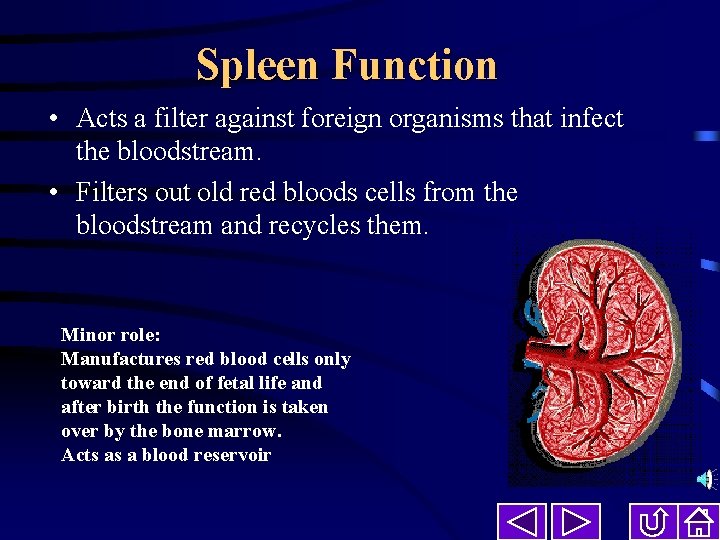
Spleen Function • Acts a filter against foreign organisms that infect the bloodstream. • Filters out old red bloods cells from the bloodstream and recycles them. Minor role: Manufactures red blood cells only toward the end of fetal life and after birth the function is taken over by the bone marrow. Acts as a blood reservoir

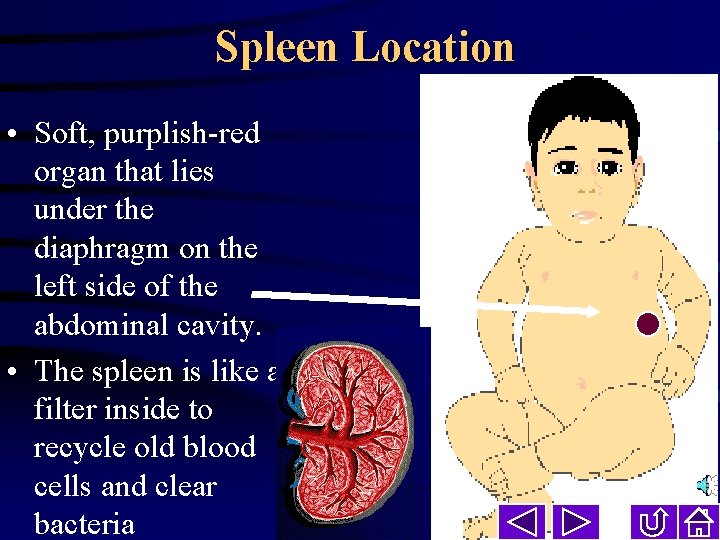
Spleen Location • Soft, purplish-red organ that lies under the diaphragm on the left side of the abdominal cavity. • The spleen is like a filter inside to recycle old blood cells and clear bacteria

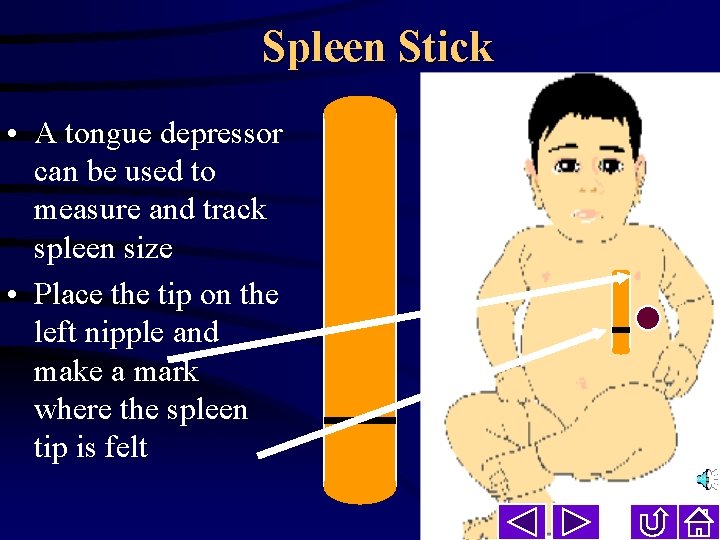
Spleen Stick • A tongue depressor can be used to measure and track spleen size • Place the tip on the left nipple and make a mark where the spleen tip is felt

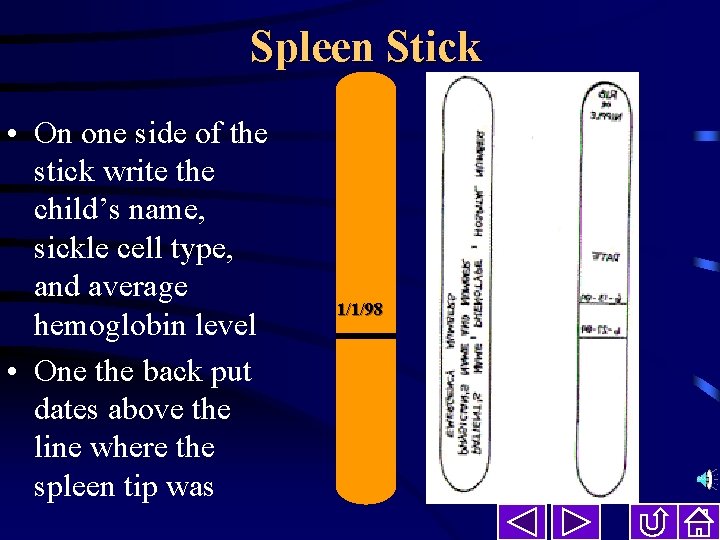
Spleen Stick • On one side of the stick write the child’s name, sickle cell type, and average hemoglobin level • One the back put dates above the line where the spleen tip was 1/1/98

What is Splenic Sequestion • Sudden trapping of blood within the spleen • Usually occurs in infants under 2 years of age • May be associated with fever, pain, and respiratory symptoms. • Circulatory collapse and death can occur in less than thirty minutes.

Treatments For Splenic Sequestion • Intravenous fluids • Blood transfusion as necessary • Spleen removal or splenectomy

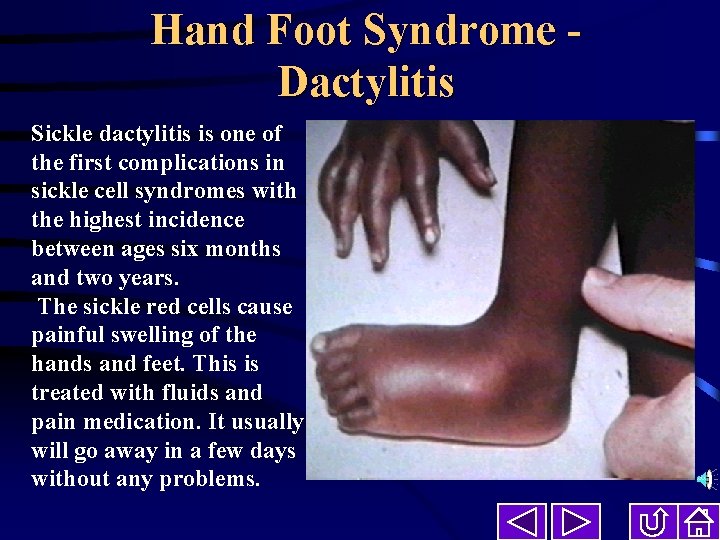
Hand Foot Syndrome Dactylitis Sickle dactylitis is one of the first complications in sickle cell syndromes with the highest incidence between ages six months and two years. The sickle red cells cause painful swelling of the hands and feet. This is treated with fluids and pain medication. It usually will go away in a few days without any problems.

Kidney damage starts very early and progresses throughout life causing complications in many individuals with sickle syndromes. The kidneys may not filter normally, passing protein and/or excessive amounts of water.

Bone Pain More prolonged and constant pain can be seen with bone infarction, sickle arthritis, and aseptic necrosis of the femur or humerus. With chronic pain, non-steroidal anti-inflammatory medications should be used. TENS units, relaxation techniques, occupational and physical therapy approaches may be useful in reducing pain and maintaining a good lifestyle.

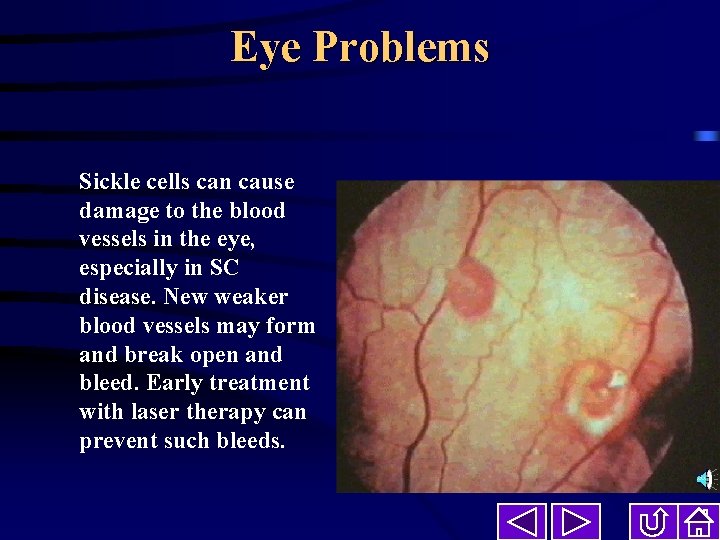
Eye Problems Sickle cells can cause damage to the blood vessels in the eye, especially in SC disease. New weaker blood vessels may form and break open and bleed. Early treatment with laser therapy can prevent such bleeds.

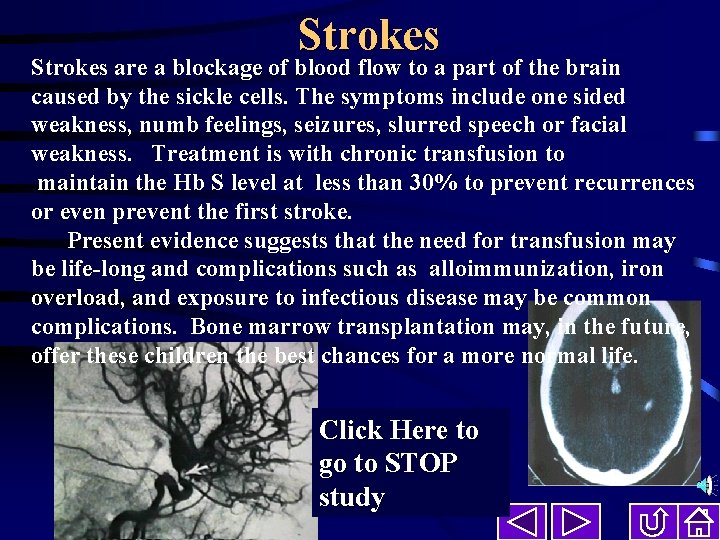
Strokes are a blockage of blood flow to a part of the brain caused by the sickle cells. The symptoms include one sided weakness, numb feelings, seizures, slurred speech or facial weakness. Treatment is with chronic transfusion to maintain the Hb S level at less than 30% to prevent recurrences or even prevent the first stroke. Present evidence suggests that the need for transfusion may be life-long and complications such as alloimmunization, iron overload, and exposure to infectious disease may be common complications. Bone marrow transplantation may, in the future, offer these children the best chances for a more normal life. Click Here to go to STOP study

Anemia - Jaundice Anemia or a low red blood cell count, is lifelong, starting in the first year of life. The average red cell life is reduced from a normal of 120 days down to an average of 10 to 20 days in sickle cell anemia. This produces anemia, a high reticulocyte count, and a bone marrow factory that is producing 3 to 4 times more red cells than normal. Other problems related to the anemia are yellow eyes or jaundice (elevated indirect bilirubin), which later in childhood and early adult life can cause gallstones

Acute Chest Syndrome Pneumonias or infections in the lung, and acute chest syndrome, caused by sickling red cells blocking blood vessels in the lung, are the most common complications. Infections are treated with antibiotics and acute chest is treated with blood transfusions It’s hard to tell the two apart so both treatments are used

Priapism is the painful erection of the penis caused by sickling red cells. This complication usually has an onset at age 5 to 35. It often occurs as a severe episode requiring hospitalization following multiple episodes of short duration termed stuttering. Onset in the early morninga waking the patient is common. Treatment includes pain relief, hydration, exchange transfusion, and surgical shunt procedures.

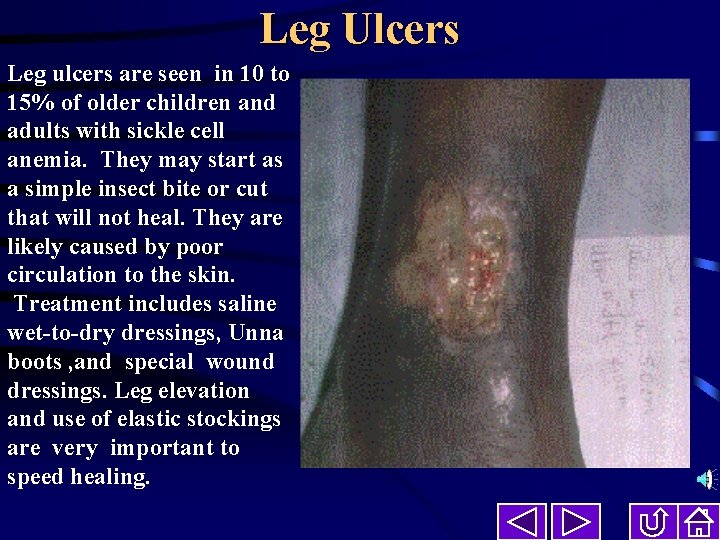
Leg Ulcers Leg ulcers are seen in 10 to 15% of older children and adults with sickle cell anemia. They may start as a simple insect bite or cut that will not heal. They are likely caused by poor circulation to the skin. Treatment includes saline wet-to-dry dressings, Unna boots , and special wound dressings. Leg elevation and use of elastic stockings are very important to speed healing.