What is evidencebased medicine Evidence based medicine is




What is evidence-based medicine? Evidence based medicine is the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients. Sackett, et al. BMJ 1996; 312: 71 -72 salarihedayat@gmail. com

“A 21 st century clinician who cannot critically read a study is as unprepared as one who cannot take a blood pressure or examine the cardiovascular system. ” BMJ 2008: 337: 704 -705 salarihedayat@gmail. com

What is Evidence-Based Medicine? “Evidence-based medicine is the integration of best research evidence with clinical expertise and patient values” salarihedayat@gmail. com

EBM - What is it? Clinical Expertise Research Evidence Patient Preferences
Traditional medicine Experiences Pathophysiology, references, Patient value …

Practice Pradigms Old paradigm Unsystematic clinical experience Pathophysiology expertise & authoritarianism salarihedayat@gmail. com New paradigm Systematic clinical experience Pathophysiology necessary but not sufficient Rules of evidence

The 5 Steps Towards Evidence Based Practice 1. Ask the right clinical question: Formulate a searchable question 2. Collect the most relevant publications: Efficient Literature Searching Select the appropriate & relevant studies 3. Critically appraise and synthesize the evidence. 4. Integrate best evidence with personal clinical expertise, patient preferences and values: Applying the result to your clinical practice and patient. 5. Evaluate the practice decision or change: Evaluating the outcomes of the applied evidence in your practice or patient. salarihedayat@gmail. com

Background questions: 1. 2. 3. What microbial organisms can cause communityacquired pneumonia? How does pneumonia cause egophony? What is the incidence of community-acquired pneumonia? salarihedayat@gmail. com

a. s Notice that the students’ questions ask for general or “background” knowledge about pneumonia, the disorder that presumably explains much of this patient’s acute illness. salarihedayat@gmail. com

A practitioners’ questions: In this patient are any clinical findings sufficiently powerful to confirm or exclude pneumonia? In this patient is a chest radiograph necessary for the diagnosis? In this patient is the probability of Legionella infection sufficiently high to warrant considering covering this organism with the initial antibiotic choice? In this patient , do clinical features predict outcome well enough that as a “low risk” patient can be treated safely at home? salarihedayat@gmail. com

Clinical questions generally fall into two categories: Background questions have to do with general information, the “lay of the land” of a certain medical topic, or just building one’s general fund of knowledge regarding a specific topic or condition or treatment. Foreground questions have to do with addressing a specific problem for a specific patient. It can be helpful to formulate “foreground” questions into the “PICO” format. Source: Huang X, Lin J, Demner-Fushman D. Evaluation of PICO as a knowledge representation for clinical questions. AMIA Annu Symp Proc. 2006: 359 -63. PMID: 17238363 salarihedayat@gmail. com

Samples Intensive treatment in patients with type II diabetes does not decrease mortality. Intensive treatment can lower blood glucose levels in patients with type II diabetes salarihedayat@gmail. com

Clinical Questions Foreground – “What do I do for this patient? ” Patient Intervention/Investigation Comparison Intervention/Investigation Outcome (Patient-Oriented) salarihedayat@gmail. com

Question components : PICO • • What types of Participants? Interventions? Comparison? Outcomes?

Clinical Questions - “PICO” Example: In a 5 year old child with conjunctivitis (patient) will topical antibiotics (intervention) compared to no treatment (comparison) lead to quicker symptom relief (outcome)? In a 5 year old child with conjunctivitis (patient) will topical antibiotics (intervention) compared to no treatment (comparison) lead to improved cure rates (outcome)? salarihedayat@gmail. com
Patient Or Problem Acute Cough in primary care setting Intervention Comparison Outcomes
Patient Or Problem Intervention Comparison Acute Antibiotics Cough in primary care setting Outcomes
Patient Or Problem Intervention Comparison Acute Antibiotics No Cough in antibiotics primary care setting Outcomes
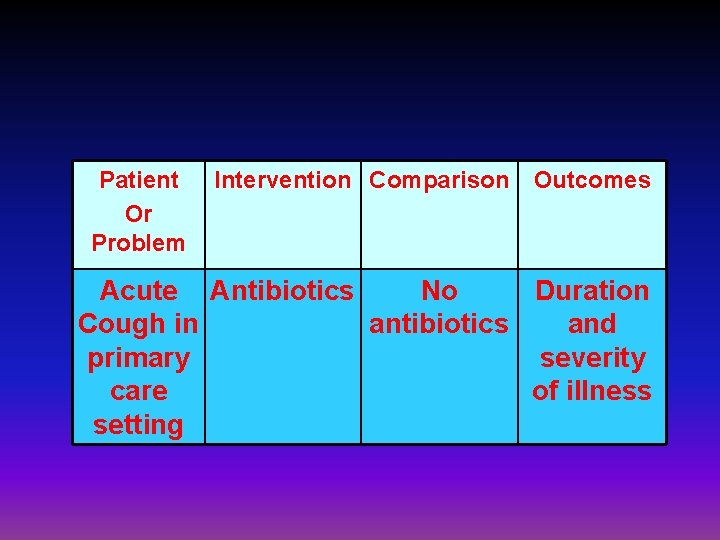
Patient Or Problem Intervention Comparison Outcomes Acute Antibiotics No Duration Cough in antibiotics and primary severity care of illness setting
Evidence-based medicine Evidence-based Medicine Gathering medical information Evaluating quality of medical information Making medical decisions using best evidence salarihedayat@gmail. com
salarihedayat@gmail. com

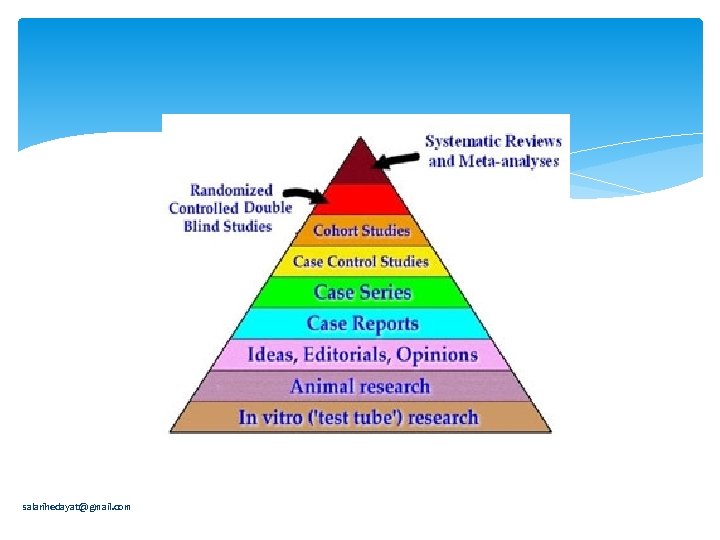
Levels of Evidence n Level 1: Randomized Clinical Trials n Level 2: Head to Head Trial or Systematic Review of Cohort Studies n Level 3: Case-Control Studies n Level 4: Case-series n Level 5: Expert Opinion salarihedayat@gmail. com
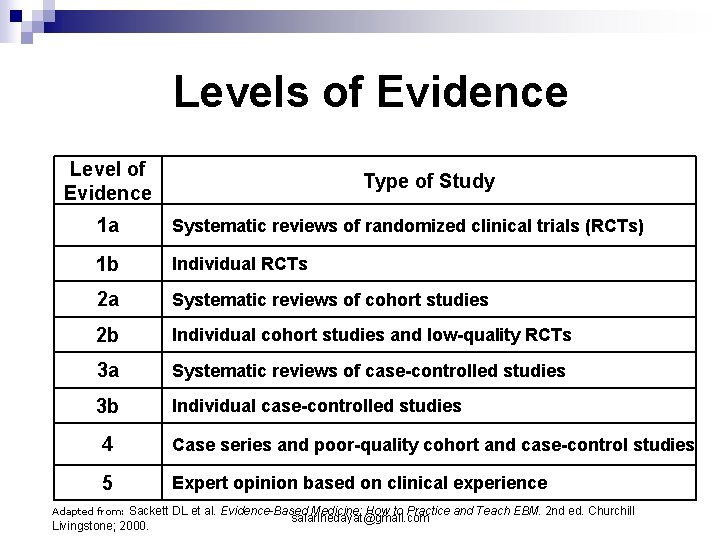
Levels of Evidence Level of Evidence Type of Study 1 a Systematic reviews of randomized clinical trials (RCTs) 1 b Individual RCTs 2 a Systematic reviews of cohort studies 2 b Individual cohort studies and low-quality RCTs 3 a Systematic reviews of case-controlled studies 3 b Individual case-controlled studies 4 Case series and poor-quality cohort and case-control studies 5 Expert opinion based on clinical experience Sackett DL et al. Evidence-Based Medicine: How to Practice and Teach EBM. 2 nd ed. Churchill salarihedayat@gmail. com Livingstone; 2000. Adapted from:

CPG Clinical Practice guidelines have been defined as systematically developed statements to assist practitioner and patient decisions about appropriate health care for specific clinical circumstances. CLINICAL PRACTICE guidelines are being promoted as one strategy to assist clinical decision making to improve the effectiveness and reduce unnecessary costs of delivered health care services. salarihedayat@gmail. com

ﺍﻧﻮﺍﻉ ﺷﻮﺍﻫﺪ Primary evidence Secondary evidence Tertiary evidence (CPG) salarihedayat@gmail. com

Concepts What makes a good guideline? “Should provide extensive, critical and well-balanced information on the benefits and limitations of various interventions so that the practitioner can carefully judge individual cases” Derived from: Subcommittee of WHO. Summary of the 1993 WHO. BMJ 1993; 307: 1541 -1546 salarihedayat@gmail. com

Guidelines Purpose “To make explicit recommendations with a definite intent to influence what physicians do” salarihedayat@gmail. com
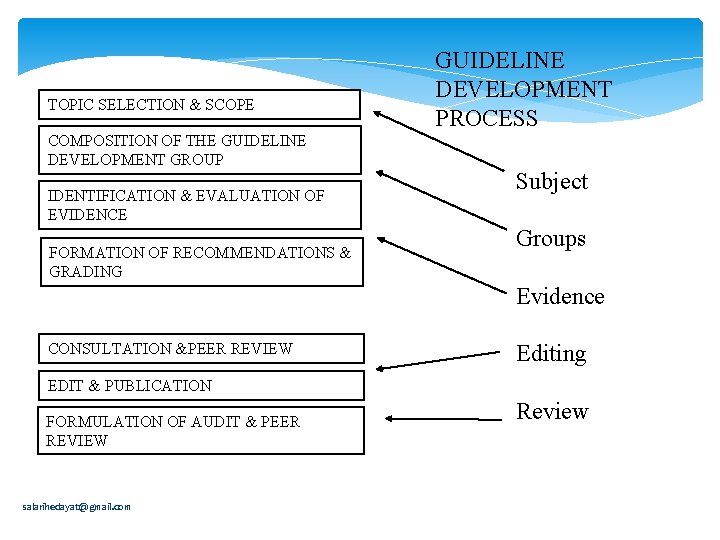
TOPIC SELECTION & SCOPE COMPOSITION OF THE GUIDELINE DEVELOPMENT GROUP IDENTIFICATION & EVALUATION OF EVIDENCE FORMATION OF RECOMMENDATIONS & GRADING GUIDELINE DEVELOPMENT PROCESS Subject Groups Evidence CONSULTATION &PEER REVIEW Editing EDIT & PUBLICATION FORMULATION OF AUDIT & PEER REVIEW salarihedayat@gmail. com Review

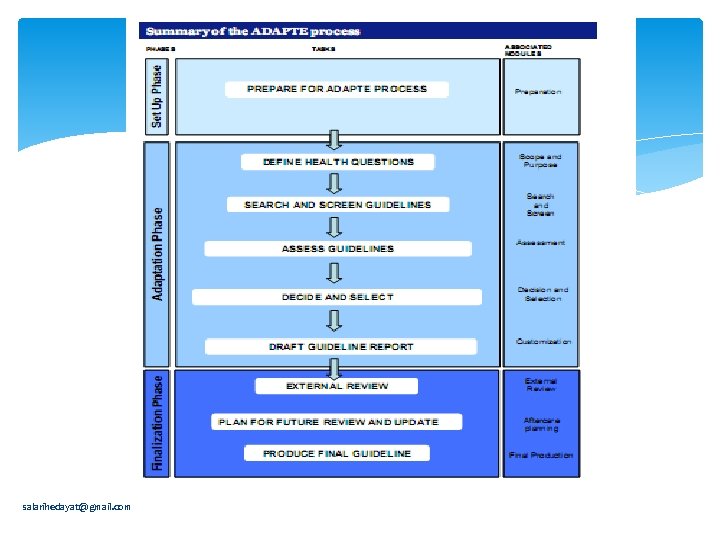
salarihedayat@gmail. com

- Slides: 34