What Every Surgeon Should Know About Head and

What Every Surgeon Should Know About Head and Neck Surgery David P Goldstein MD FRCSC Otolaryngology-Head & Neck Surgery Surgical Oncology University Health Network David. goldstein@uhn. on. ca

Objectives n Focus on approach to evaluation and management of a neck mass and Parotid masses n Briefly highlight key issues in diagnosis & management of following types of neck mass n Congenital disorders n n thyroglossal duct and branchial cleft cyst Salivary gland masses Carotid body tumor Squamous cell carcinoma

Differential Diagnosis n Congenital n n Inflammatory n n n Thyroglossal duct cyst Branchial cleft cyst Lymphangioma Infectious Non-infectious Neoplastic n n Primary malignancies Metastases to nodes

Approach to the Differential Diagnosis of Neck Masses Age n Location, Location n Duration of symptoms n Risk factors n Contents of neck mass n

Differential Diagnosis n n Age is a major determinant < 20 years – C I 20 – 40 years - I C > 40 years N I N N C C= congenital I= inflammatory N= neoplastic

Location n Anterior Triangle n n n Anterior- midline Posterior- SCM Inferior- clavicle Superior- mandible Posterior Triangle n n Anterior- post border of SCM Posterior- trapezius Superior- junction of SCM & trapezius Inferior- clavicle
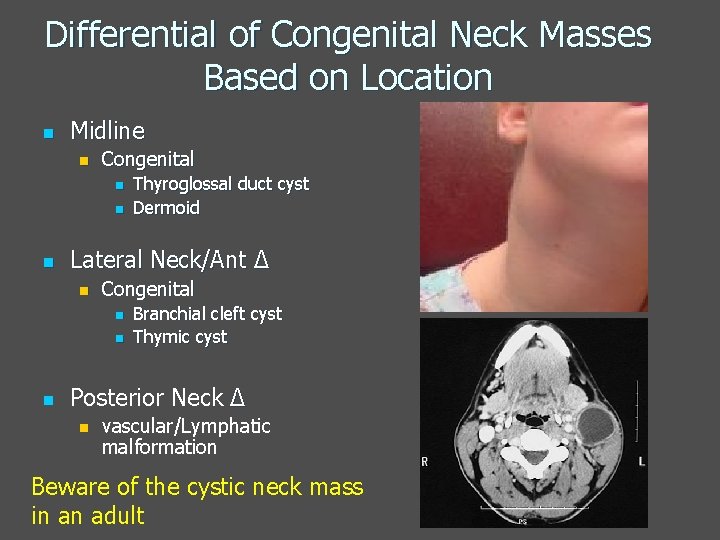
Differential of Congenital Neck Masses Based on Location n Midline n Congenital n n n Lateral Neck/Ant Δ n Congenital n n n Thyroglossal duct cyst Dermoid Branchial cleft cyst Thymic cyst Posterior Neck Δ n vascular/Lymphatic malformation Beware of the cystic neck mass in an adult

Differential Diagnosis of Neoplastic Neck Masses based on Location n Lateral Anterior Δ n Benign n Schwanomas n CBTs n Salivary gland n Malignancies n Lymphoma n Nodal metastasis n UADT n Skin n Salivary gland n Midline Anterior Δ n n Thyroid Larynx cancer n n n Direct extension Metastasis Posterior Δ n Benign n n Schwanomas Malignant n n Lymphoma Nodal metastasis n n n Skin UADT Non H & N Supraclavicular nodes (virchow nodes) - Classically represents nodal metastases from below the diaphragm

Differential Based on Growth Rate n Slow growing over years n n Tend to be benign or low grade malignancy Rapidly growing neck masses Infectious n Malignant – tend to progress over period of weeks to a few months n

Cystic Neck Mass n Congenital n n n Squamous cell cancer n n Oropharyngeal/ tonsil primary Thyroid Cancer n n n Thyroglossal duct cyst Branchial cleft cyst WDTC present with cystic mass Classically has dark brown appearance Tail of parotid masses n Warthin’s tumor

Necrotic Neck Mass n Infectious Abscess n Tuberculosis n n Malignant n Squamous cell carcinoma
Work-Up of a Neck Mass n n History Physical n n Diagnostic Imaging n n n US CT MRI PET Biopsy n n Inspection Palpation Endoscopy FNA Other n n Intraoperative endoscopy TB test

History Keep the differential diagnosis in mind n Duration & growth rate of the mass n n Associated symptoms n Malignant lesions tend to have progressive growth at more rapid rate than benign disease Dysphagia, odynophagia, otalgia, hoarseness, oral cavity pain, nasal obstruction, epistaxis n n Location n Anterior, posterior or midline Symptoms of inflammation or infection n Malignant neck masses with necrosis and skin involvement may mimic invasion n Suggests UADT malignancy B symptoms – fever, weight loss & night sweats Risk factors n n n Malignancy TB exposure Cat scratch

History n Past medical history n n n Skin cancer UADT malignancy Sarcoidosis Fungal infection Dental caries/dental work Trauma to head and neck n Family history n n Thyroid cancer Paragangliomas

History- Risk Factors for Malignancy n n Tobacco n Cigarettes, chew, betel nut, cigar Alcohol n n Viruses n n n Two together are synergistic HPV- oropharynx cancer EBV- nasopharynx cancers HIV- kaposi’s sarcoma, lymphoma Immunosupression n Transplant patients- Skin cancers, head and neck cancer Occupational n Wood working, leather work – paranasal sinus cancer

Risk Factors Cont’d n Previous head and neck cancer n n Radiation exposure n n Develop second cancer in 18% of patients Salivary gland cancers, thyroid cancer, head and neck sarcomas Autoimmune disorders n Sjogren’s syndrome n n lymphoma of salivary glands Hashimoto’s thyroiditis n thyroid lymphoma

Physical Examination n Neck mass n n n n Location Size Firmness Fixation Pulsatile Presence of other neck masses or enlarged nodes Movement with tongue protrusion Auscultate for bruits if pulsatile

Investigations n n If diagnosis of infectious or inflammatory is probable no further work up is necessary and appropriate therapy instituted Suspected inflammatory disorders may require serologic tests If there is any uncertainty in diagnosis or the suspected diagnosis is congenital or neoplastic further investigations are required When in doubt on your exam – do further investigations
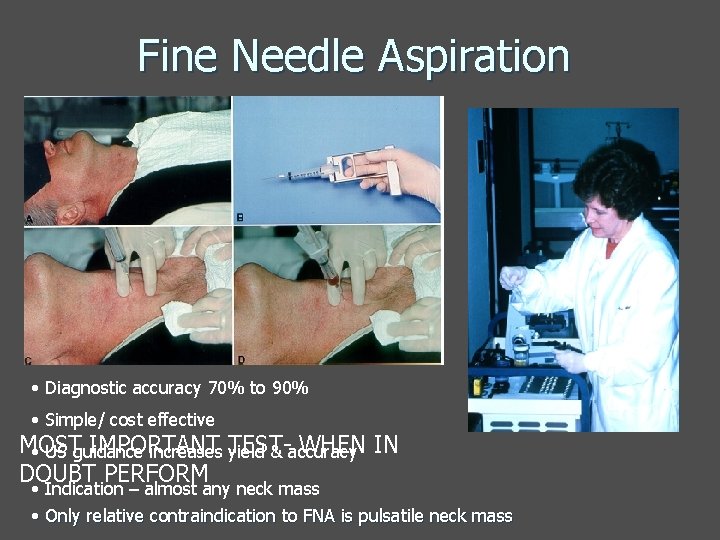
Fine Needle Aspiration • Diagnostic accuracy 70% to 90% • Simple/ cost effective MOST IMPORTANT WHEN IN • US guidance increases TESTyield & accuracy DOUBT PERFORM • Indication – almost any neck mass • Only relative contraindication to FNA is pulsatile neck mass

Fine Needle Aspiration n Diagnose most head and neck cancers n Suspect lymphoma n n Cystic neck mass n n n Send for flow cytometry Send washings Stain for thyroglobulin Still a role for FNA in infectious and inflammatory disorders n n C&S Presence of pus does not necessarily exclude malignancy n Squamous cell carcinoma can present with necrotic nodes

Open Biopsy n Almost NO role in the initial work-up of a neck mass n Contraindications n n Pulsatile masses Parotid masses Suspected malignancies and FNA not been attempted When to do n Only after work-up is completed including FNA and diagnosis is still in question n n FNA is non-diagnostic FNA is negative but not in keeping with clinical picture

Open Biopsy n Situations in which may be indicated n Lymphoma n n FNA is suspicious for lymphoma & further tissue needed Cystic neck mass FNA often inconclusive n Send cyst fluid for cytology n Do full work-up prior to open biopsy n n Imaging and panendoscopy of UADT

Open Biopsy n Incisional vs excisional biopsy n n Depends upon size, location and involvement if surrounding structures and suspected pathology Keep in mind future surgery/neck dissection n Make the incision in line with potential incision one would use if further neck surgery is required

Diagnostic Imaging n Plain films n n Limited role CXR n CT scan & MRI n n Ultrasound/Doppler n n n Useful noninvasive test Vascularity Solid vs Cystic Sensitive for adenopathy Guided FNA n n Location Relation to other structures Vascularity Bone invasion MRI for soft tissue n n n Tongue No dental artifact MRA/MRV
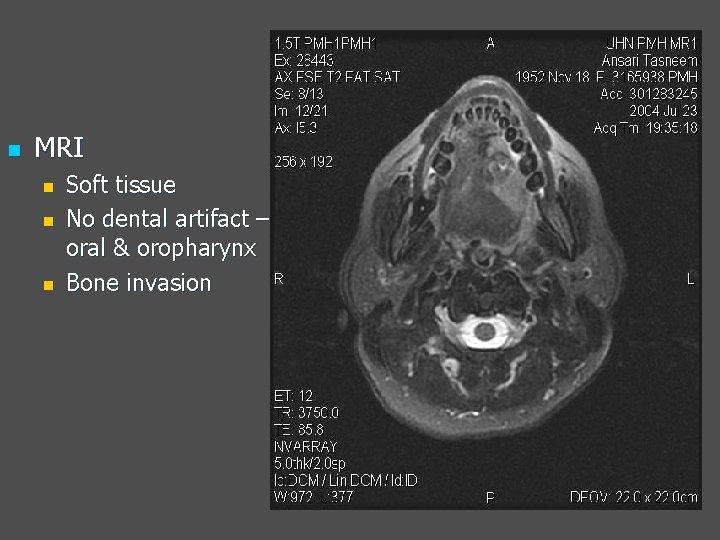
n MRI n n n Soft tissue No dental artifact – oral & oropharynx Bone invasion
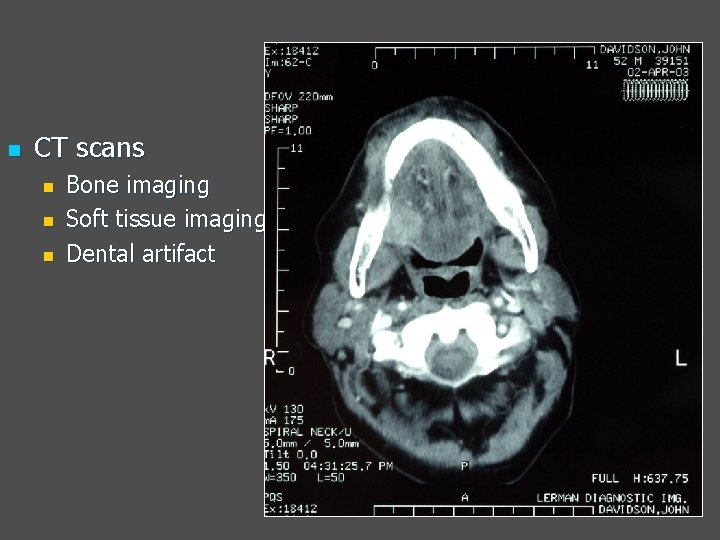
n CT scans n n n Bone imaging Soft tissue imaging Dental artifact

The Pulsating Neck Mass n Differential Diagnosis n n Non-vascular mass situated near carotid artery Carotid body tumor (paraganglioma) Carotid artery aneurysm Work-up n Image first n n CT with contrast or MRI If confirmed vascular mass get MRI (MRA & MRV) Avoid FNA but not end of world Incisional biopsy contraindicated

Presentation & Management of Specific Diagnosis

Thyroglossal Duct Cyst n Presentation n n May occur at any age but most common in first 2 decades of life Midline at level of hyoid to thyroid, may be off centre May have hx of infection Classic sign is rising with tongue extrusion Diagnosis n n History & Physical Imaging

Thyroglossal Duct Cyst n Cautions n n n May have papillary ca arising in thyroglossal duct cyst – rare but I perform FNA Cystic nodal metastasis from papillary thyroid ca to delphian node may have similar presentation Treatment n n Excision – sistrunk procedure (remove cyst with track up to tongue base including central portion of hyoid bone) Cosmetic and prevent recurrent infection
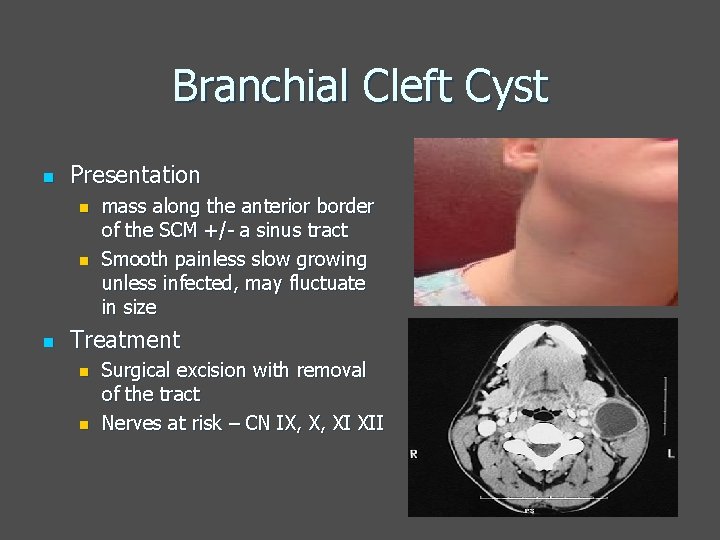
Branchial Cleft Cyst n Presentation n mass along the anterior border of the SCM +/- a sinus tract Smooth painless slow growing unless infected, may fluctuate in size Treatment n n Surgical excision with removal of the tract Nerves at risk – CN IX, X, XI XII
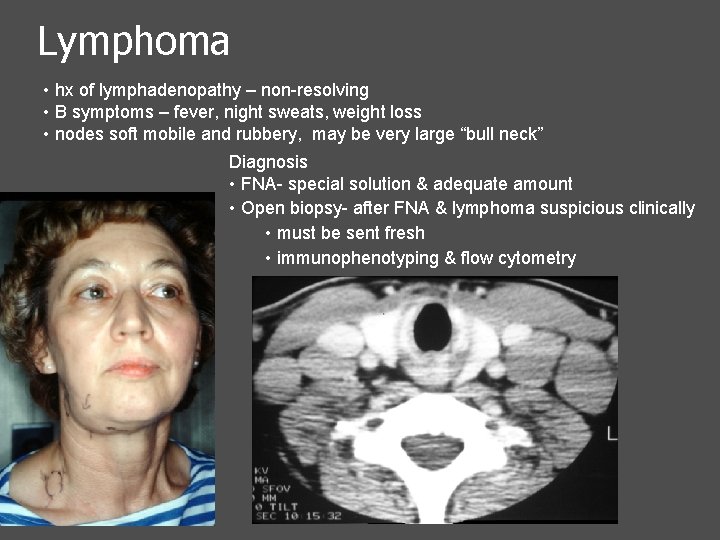
Lymphoma • hx of lymphadenopathy – non-resolving • B symptoms – fever, night sweats, weight loss • nodes soft mobile and rubbery, may be very large “bull neck” Diagnosis • FNA- special solution & adequate amount • Open biopsy- after FNA & lymphoma suspicious clinically • must be sent fresh • immunophenotyping & flow cytometry
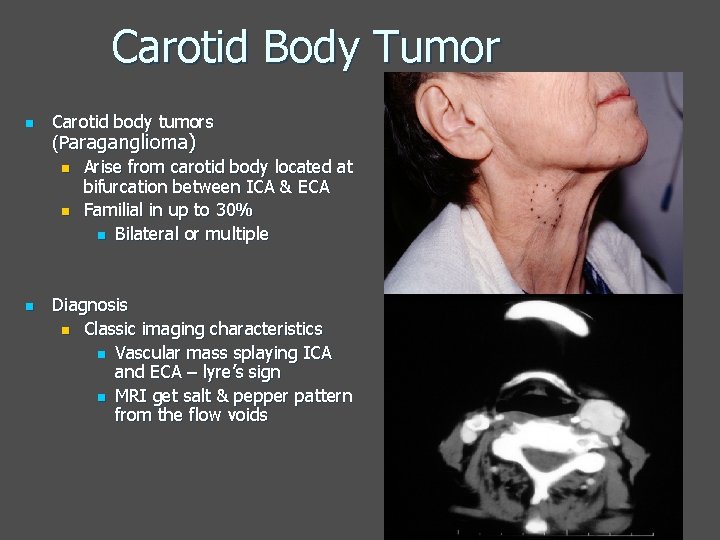
Carotid Body Tumor n n Carotid body tumors (Paraganglioma) n Arise from carotid body located at bifurcation between ICA & ECA n Familial in up to 30% n Bilateral or multiple Diagnosis n Classic imaging characteristics n Vascular mass splaying ICA and ECA – lyre’s sign n MRI get salt & pepper pattern from the flow voids

Carotid Body Tumor n n Treatment n Excision n Proximal and distal control of CA n Prepared to bypass Complications n Vascular injury n Stroke n CN injury – CN IX, X, XII
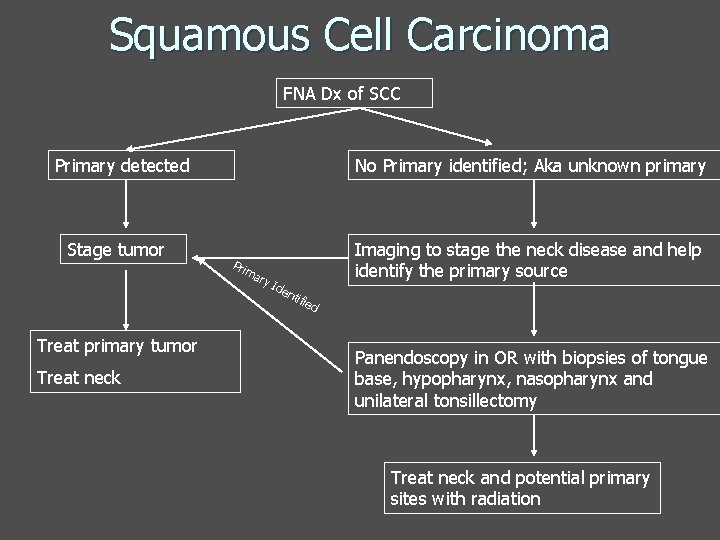
Squamous Cell Carcinoma FNA Dx of SCC Primary detected Stage tumor No Primary identified; Aka unknown primary Pri ma ry Imaging to stage the neck disease and help identify the primary source Ide nti fie d Treat primary tumor Treat neck Panendoscopy in OR with biopsies of tongue base, hypopharynx, nasopharynx and unilateral tonsillectomy Treat neck and potential primary sites with radiation

Squamous cell carcinoma General Management Principles n Staging n Hx, Px (flex scope) n Imaging n n CT Head and neck MR for tongue/tongue base Chest CT r/o synchronous primary Panedoscopy/Quadroscopy (EUA under GA) n n Esophagoscopy, Bronchoscopy, Laryngoscopy, +/- nasopharynx Used for cancers of larynx, hypopharynx and +/- oropharynx n n n Assess the extent of the tumor & surgical resectabilty Obtain biopsy specimens Assess for 2 nd primary

Squamous cell carcinoma General Management Principles n Treatment Options n n Surgery Radiation Chemotherapy Combination of both n n Rads or chemo can be given pre- or post op Treat the primary site and the cervical lymph nodes n Try and treat cervical lymph nodes with the same modality of therapy used for the primary site

How do we decide which treatment to offer n Provide the treatment that will offer the highest survival & control rate n n based on literature Early stage disease often similar Advanced disease usually combination QOL and morbidity n n n Organ preservation (larynx, hypopharynx) Preserve form and function (oropharynx Swallowing, speech, cosmesis

Goals of Treatment n Cure Local regional control n Survival n n Palliation Pain n Bleeding n Cosmesis n

Squamous cell carcinoma General Management Principles n n n Oral cavity – surgery Oropharynx (tonsil, tongue base)- radiation or chemoradiation Hypopharynx cancer – radiation or chemoradiation Larynx- transoral laser surgery for small tumors, radiation or chemoradiation for most Nasopharynx- chemoradiation or radiation

Adenocarcinoma n FNA diagnosis of adenocarcinoma in the neck – from a distant site n n Lung, breast, GI, GU May require an open biopsy to get more tissue for analysis to help identify site Image chest, abdo, pelvis Rarely treat the neck b/c metastatic disease palliative therapy to prevent obstruction of trachea or esophagus n Neck dissection - Only if primary site is controlled and patient is potentially curable
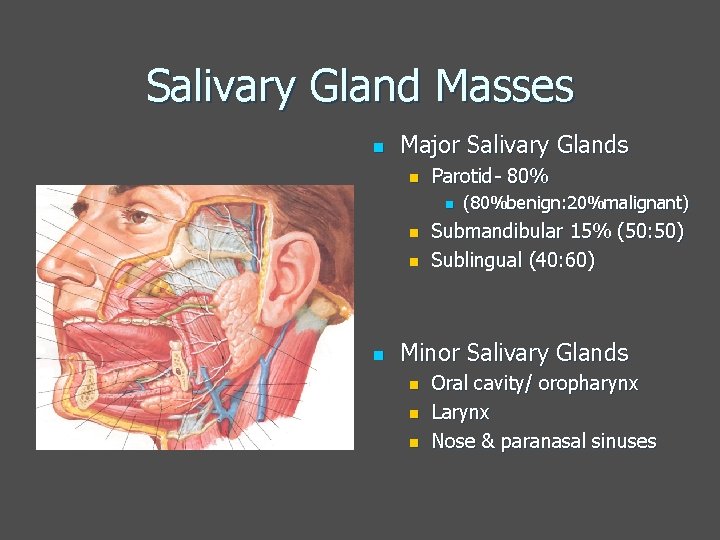
Salivary Gland Masses n Major Salivary Glands n Parotid- 80% n n (80%benign: 20%malignant) Submandibular 15% (50: 50) Sublingual (40: 60) Minor Salivary Glands n n n Oral cavity/ oropharynx Larynx Nose & paranasal sinuses
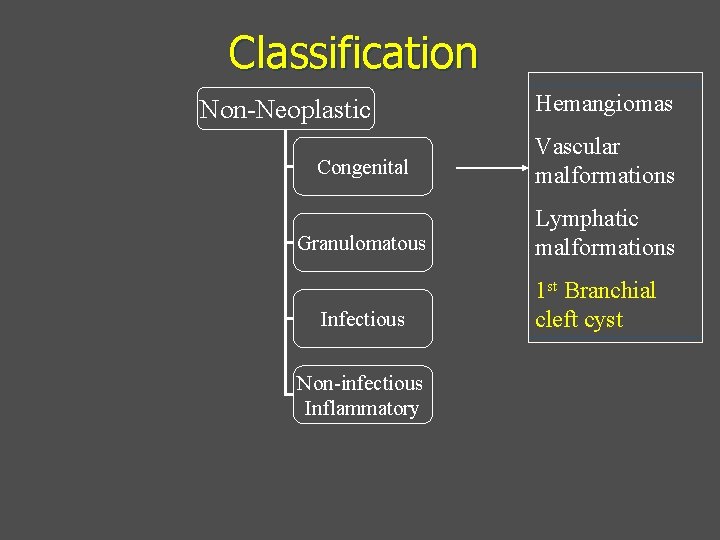
Classification Non-Neoplastic Hemangiomas Congenital Vascular malformations Granulomatous Lymphatic malformations Infectious Non-infectious Inflammatory 1 st Branchial cleft cyst
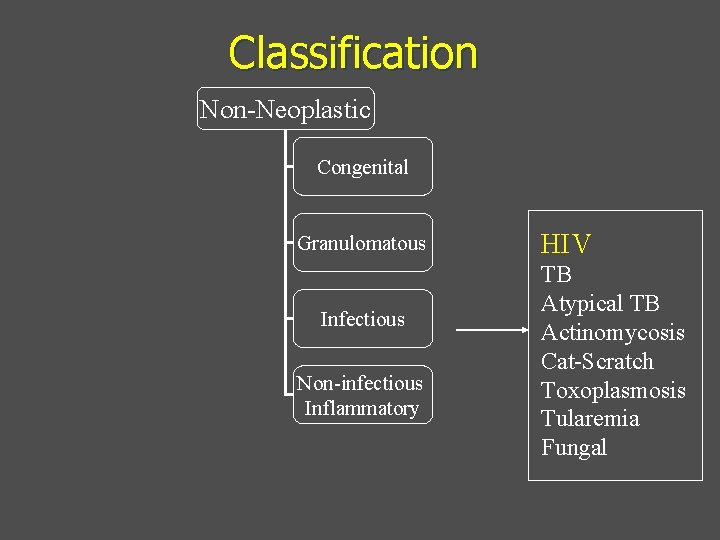
Classification Non-Neoplastic Congenital Granulomatous Infectious Non-infectious Inflammatory HIV TB Atypical TB Actinomycosis Cat-Scratch Toxoplasmosis Tularemia Fungal

History & Physical Exam n n Majority of neoplasms (benign or malignant) present as asymptomatic swelling Risk factors for malignancy n Majority idiopathic Ionizing radiation Sjogren’s syndrome Lymphoma n Skin cancers n n n

Clinical Presentation of Cancers n n n Pain Fixation & invasion of surrounding structures i. e. dermis, mandible Trismus Facial nerve paralysis Adenopathy
Facial Nerve Paralysis with a Parotid Mass n n n Very rarely occurs with benign tumors 12% to 15% parotid malignancies will exhibit facial paralysis Pathologies Adenoid cystic carcinoma n Poorly differentiated carcinoma n SCC n

Lab Tests n Serology if suspect auto-immune process Biopsy n n FNA – mainstay Open biopsy n Very rarely indicated for parotid masses: AVOID in most cases

Fine Needle Aspiration n Debate about utility of FNA in parotid masses Among all H & N sites the parotid gland is associated with the highest FNA inaccuracy rates False negative rates higher then false positive n Sensitivity rates reported can be as low as 38% when comes to recognizing malignant nature of parotid masses n Diagnostic precision is difficult n Determine high vs. low grade tumors is also difficult

Why do an FNA? n Accuracy in determining benign from malignant disease n Rates of ~ 90% n It may help in planning surgery especially informed consent n It may help in timing of surgery in resource restricted climate n Change clinical approach in up to 30% of patients n Results interpreted in the face of the clinical presentation and imaging
Diagnostic Imaging n n Ultrasound n Identifying a mass n Guide FNA n Assessing adenopathy Technitium-99 m Scan n Diagnosis of Oncocytoma or Warthin’s tumor Sialography n Rarely used n Little role in routine work-up of a parotid mass CT Scan and/or MRI n Main modalities for imaging parotid neoplasms

Value of Imaging n Know what you are getting into n n n “tip of iceberg” with deep lobe involvement Approach Malignancy n Resectability n n Skull base Structures requiring resection Nodal status Facial nerve status n Adenoid cystic carcinoma- proximal portion

Common Pathologies n Benign n Pleomorphic adenoma n n Warthin’s tumor n n Malignant degeneration into carcinoma ex-pleomorphic adenoma in 2 -10% of pleomorphic adenomas 10% bilateral Malignant n n n Mucoepidermoid carcinoma Adenoid cystic carcinoma Metastases from skin cancers

Prognostic Factors with Malignancy n Histology n n n n High Grade Malignancies Older Age Pain at presentation Stage of primary tumor & nodal metastases Skin invasion Facial nerve dysfunction Peri-neural growth Positive margins
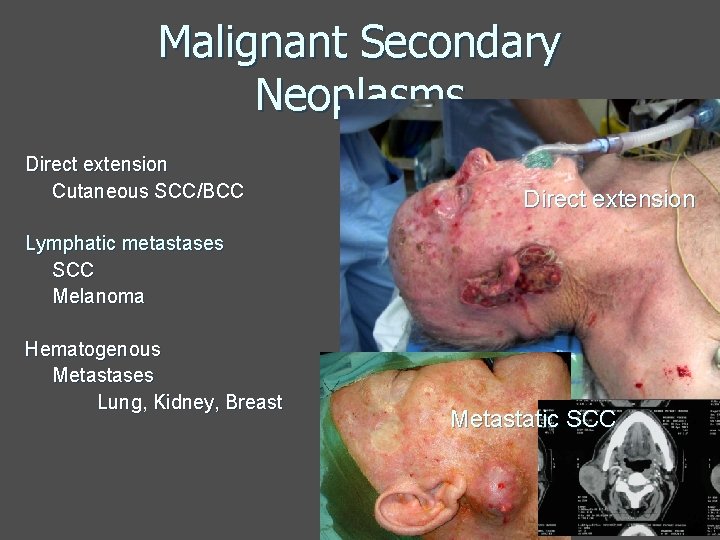
Malignant Secondary Neoplasms Direct extension Cutaneous SCC/BCC Direct extension Lymphatic metastases SCC Melanoma Hematogenous Metastases Lung, Kidney, Breast Metastatic SCC

Factors in Decision Making n Patient factors n n Age Co-morbidities Patient’s concerns Tumor Factors n Histology n n Benign vs malignant Do you have a diagnosis & how certain are we Growth rate Risk factors for malignancy

Surgery n n Majority can be managed with a superficial parotidectomy Subtotal parotidectomy n n Involvement of deep lobe Parotidectomy and transcervical approach to parapharyngeal space tumours

Surgical Complications n n n n Temporary VII nerve paresis=21% Frey’s syndrome=6% Infection=3. 6% Hematoma=2. 7% Hypertrophic scar=2. 4% Seroma=0. 8% Salivary fistula=0. 4%

Indications for Post-operative Radiotherapy n n n High grade cancers Recurrent cancers Gross or microscopic residual disease Regional lymph node metastases Evidence of locally advanced tumors

Thyroid Cancer
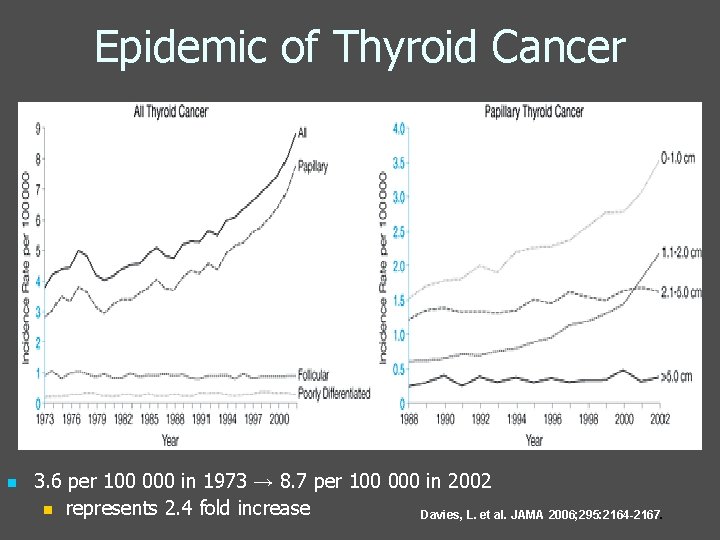
Epidemic of Thyroid Cancer n 3. 6 per 100 000 in 1973 → 8. 7 per 100 000 in 2002 n represents 2. 4 fold increase Davies, L. et al. JAMA 2006; 295: 2164 -2167.

Thyroid Malignancies n Well-Differentiated Carcinomas (80 -85%) Papillary Thyroid Carcinoma (PTC) n Follicular Thyroid Carcinoma (FTC) n n Medullary Thyroid Carcinoma (5 -10%) Anaplastic Thyroid Carcinoma (5 -10%) Other malignancies Lymphomas n Distant Metastases n

Well-Differentiated Thyroid Carcinoma n Papillary Thyroid CA n n n 75 -80% of thyroid carcinomas Frequently Multifocal Dx on FNA or FS Common Nodal Dz Infrequent Distant Dz Slightly Better Prognosis n Follicular Thyroid CA n n n n 5 -10% of all thyroid carcinomas more aggressive natural history Solitary Lesion Dx on final path Infrequent Nodal Dz Common Distant Dz Slightly Worse Prognosis
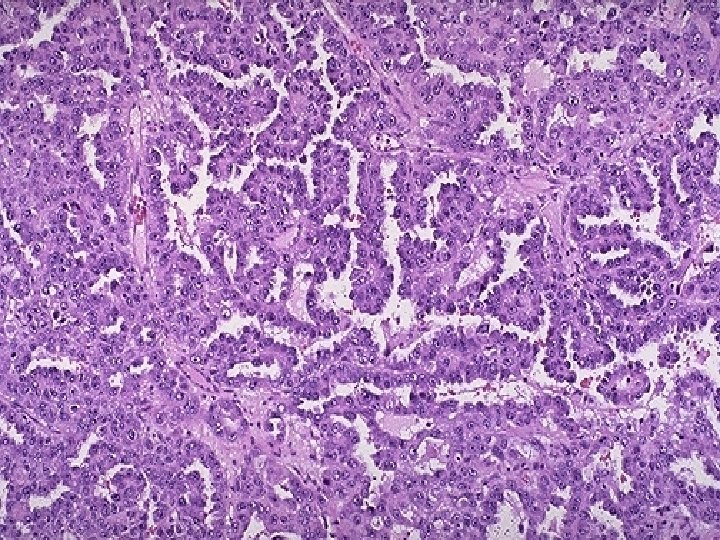
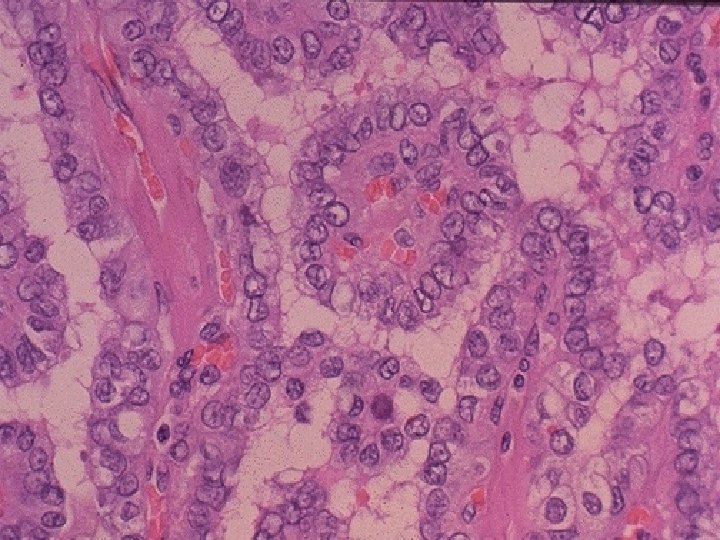
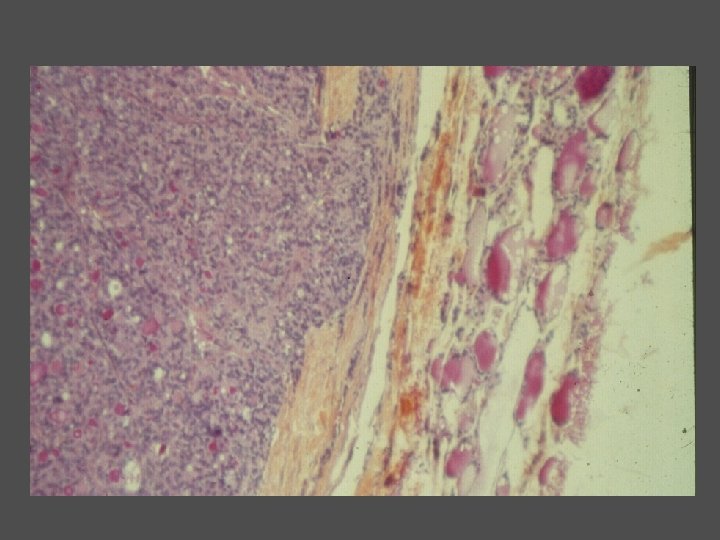

Medullary Thyroid Carcinoma n n n C - cell/parafollicular cell origin May be sporadic/nonfamilial (80%) or familial (20%) Familial forms n Medullary thyroid carcinoma alone • MEN 2 A (Sipple’s) n • MEN 2 B n n MTC, Pheochromcytoma, Hyperparathyroidism MTC, Pheochromocytoma, Mucosal Neuromas, Mutations on chromosome 10 for the RET protooncogene Regional lymph node metastases - 50% Distant metastases
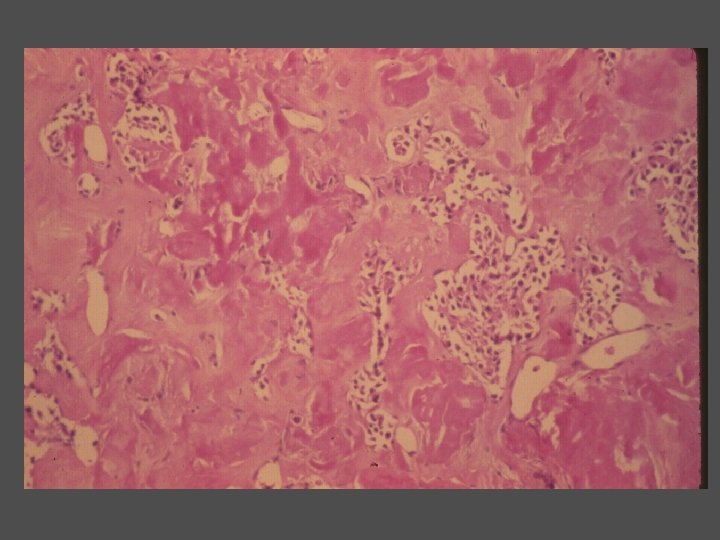

Medullary Thyroid Carcinoma n Diagnosis / Screening Pentagastrin Stimulation with measurement of calcitonin levels • Ret proto-oncogene screening Patients who screen positive should undergo early thyroidectomy Early intervention has resulted in 85% DFS at 15 -20 years Serum calcitonin levels are used as a tumor marker in follow-up • n n n

Medullary Thyroid Carcinoma n Treatment • • • n exclude pheochromocytoma total thyroidectomy central compartment lymphadenectomy elective lateral neck dissection for patients with palpable thyroid disease therapeutic lateral neck dissection for patients with palpable neck disease Treatment • • Adjuvant external beam radiation may be used to enhance locoregional control The role of chemotherapy remains to be defined

Anaplastic Carcinoma n n n Rare tumor noted for its rapid growth and nearly uniform lethal nature Typically develops in a pre-existing well differentiated thyroid carcinoma or a goiter Poor prognostic factors n n Advanced age Presence of regional or distant metastases
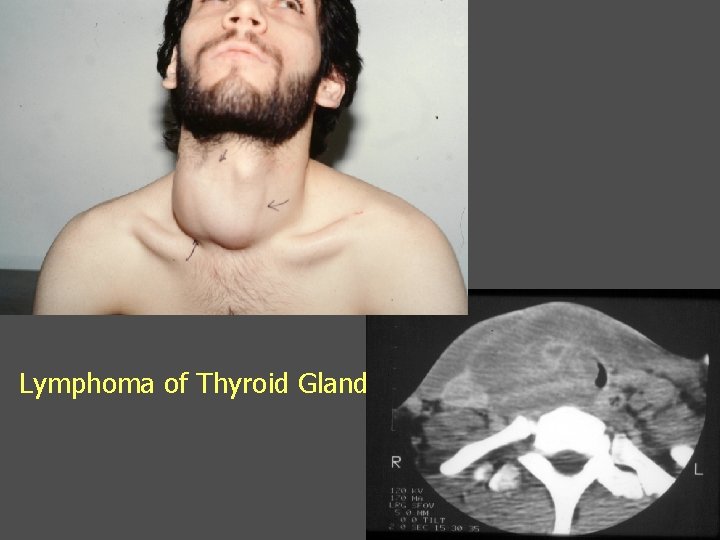
Lymphoma of Thyroid Gland

Thyroid Nodules n n n Approximately 95% of thyroid nodules are benign 4 -7% of adults have thyroid nodules Women > men Likelihood of malignancy=5% Malignancy in clinically apparent nodules=20%

Work-up of Thyroid Nodule n History n n n exposure to ionizing radiation family history of thyroid carcinoma or other endocrine neoplasms (MEN syndromes) Physical examination n Vocal cord paralysis Fixed and firm Cervical nodes

Investigations n n FNA Thyroid U/S TSH No role for calcitonin, thyroglobulin and thyroid scintigraphy in the initial work-up
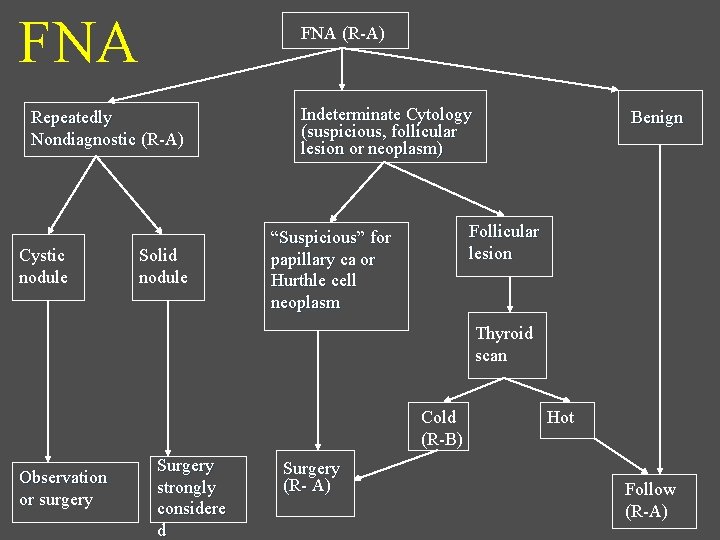
FNA (R-A) Repeatedly Nondiagnostic (R-A) Cystic nodule Solid nodule Indeterminate Cytology (suspicious, follicular lesion or neoplasm) Benign Follicular lesion “Suspicious” for papillary ca or Hurthle cell neoplasm Thyroid scan Cold (R-B) Observation or surgery Surgery strongly considere d Surgery (R- A) Hot Follow (R-A)

Risk-group Definitions AGES n A – age (> 40) n G – grade n E – extent of tumor n n extrathyroidal invasion distant metastases n S – size n Other TNM & MACIS AMES n A – age(M>40, F>50) n M – metastases (distant) n E – extent of tumor n S – size
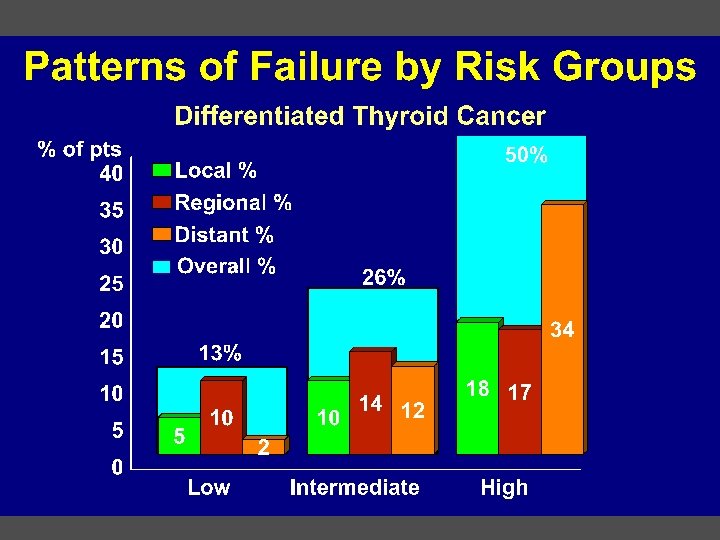

Treatment n Surgery n n Post-operative External beam Post-operative radioactive iodine thyroid suppression radiation screening

Total vs Less than Total Thyroidectomy n n Eliminates all cancer and potential cancer (up to 50% CL) Allows RAI Allows monitoring with thyroglobulin Deals with tall cell and insular Ca & prevents transformation of PTC to anaplastic ca n n No compelling evidence for survival advantage Difficult for RAI Thyroglobulin not possible Spares the parathyroids & RLN

Hemi vs Total Thyroidectomy n Low risk disease n n Controversial R. R decreased with total thyroidectomy Some studies shown no difference High risk patients n n Local & regional RR lower in total thyroidectomy Possibly improved cause specific survival

Complications of Thyroidetcomy n Hypoparathyroidism n n Temp vs Permanent Recurrent Laryngeal Nerve Injury n n Unilat vs bilat Temp vs Perm

Complications n Post-operative hematoma n n Concern re: airway Prevent obstruction with incomplete strap muscle reapprox inferiorly Drains do not prevent Management Airway emergency n Open at bedside if patient in resp distress n To OR n

Neck Management n n Clinically negative neck no neck dissection Nodal metastases at presentation n n Do not adversely affect survival Does increase risk of locoregional recurrence 80% of nodal metastases are central compartment Lateral ND only if clinically positive nodes or identified intra-op n n Functional neck dissection level II-V Spare IJV, SCM, CN XI, cervical plexus

Radioactive Iodine n n n Agent - I 131 Effect Goal of therapy n n Scan Thyroid ablation Therapeutic Complications n n Short term Long term

Radioactive Iodine n n Only useful in cases of well differentiated thyroid malignancies Results n n Overall efficacy difficult to clearly delineate Studies have shown decreased locoregional recurrences and increased survival in some series Less efficacious in unresectable disease Pulmonary metastases respond better than bony metastases

Thyroid Nodules in Pregnancy n Uncertainty if nodules in pregnancy are more likely to be malignant than those found in non-pregnant women n n No population based studies Recommendations (C) n FNA unless low TSH n Malignancy- follow with U/S n Significant growth by 24 wks gestation n n Remains stable or diagnosed in 2 nd half of pregnancy n n surgery can be performed at that time point surgery may be performed after delivery Low TSH n if persists after 1 st trimester n thyroid scan after pregnancy
- Slides: 88