What Every Spine Surgeon Should Know About Neurosurgical

What Every Spine Surgeon Should Know About Neurosurgical Issues… When to Refer, When Not to Worry Amer Samdani, MD Chief of Surgery Shriners Hospitals for Children Philadelphia, PA

Objectives l l Incidence and most common anomalies seen l Chiari malformation l Syrinx l Tethered cord l Split cord malformation (diastematomyelia) Patient presentations
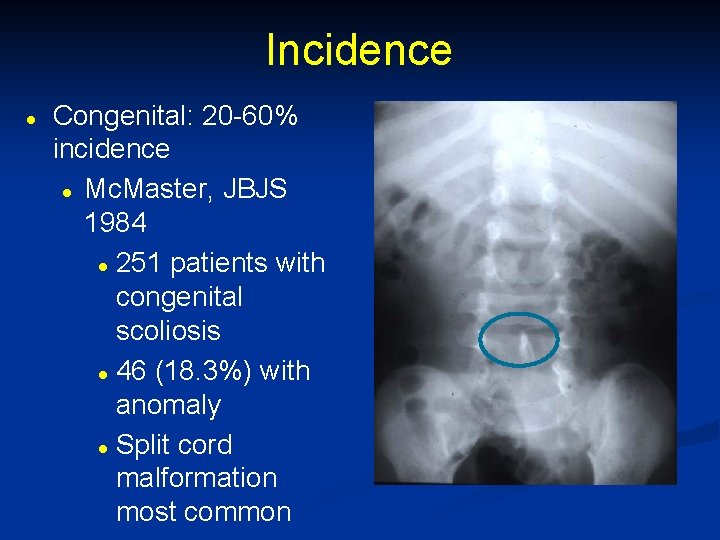
Incidence l Congenital: 20 -60% incidence l Mc. Master, JBJS 1984 l 251 patients with congenital scoliosis l 46 (18. 3%) with anomaly l Split cord malformation most common

Congenital Scoliosis: Incidence l l Shen et al, Spine 2013 l 226 patients l 43% with intraspinal anomaly l Split cord malformation most common Basu et al, Spine 2002 l 126 consecutive patients l Tethered cord most common l More common in: l Kyphosis, complex defects

Isolated Hemivertebrae Belmont et al, JBJS 2004 l l l 8 patients underwent neurosurgical intervention Only 4 had abnormal physical examination findings “. . a magnetic resonance imaging evaluation of the entire spine should be considered for all patients with congenital scoliosis, including those with an isolated hemivertebra. ”

Syrinx and Chiari Malformation
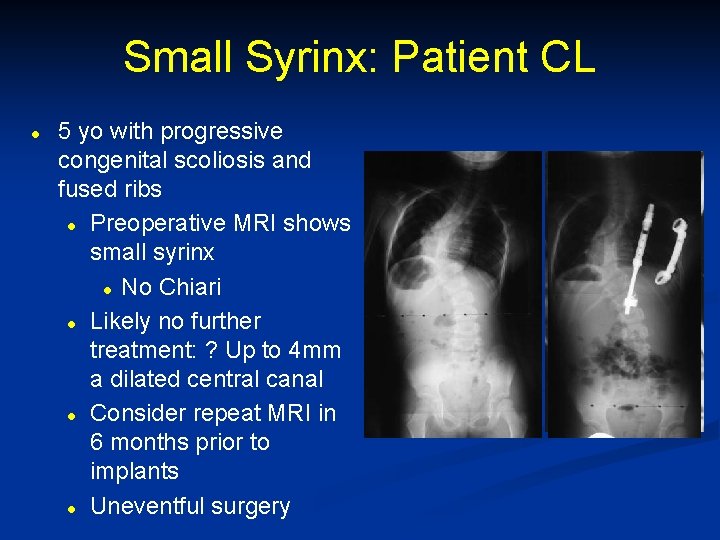
Small Syrinx: Patient CL l 5 yo with progressive congenital scoliosis and fused ribs l Preoperative MRI shows small syrinx l No Chiari l Likely no further treatment: ? Up to 4 mm a dilated central canal l Consider repeat MRI in 6 months prior to implants l Uneventful surgery
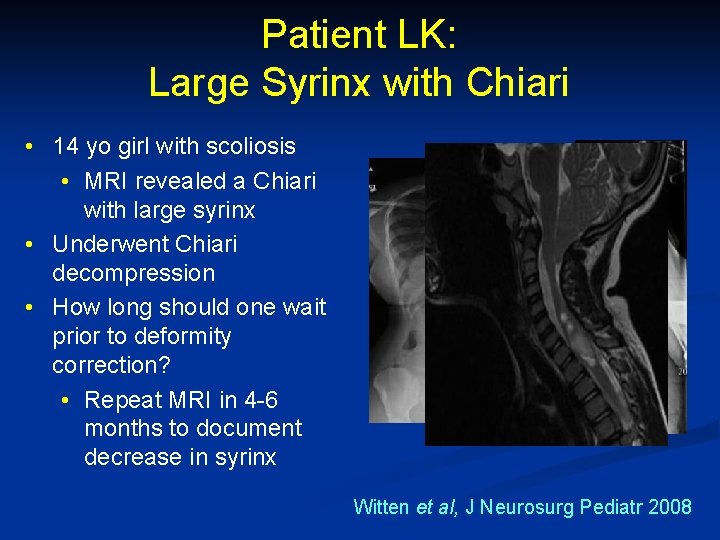
Patient LK: Large Syrinx with Chiari • 14 yo girl with scoliosis • MRI revealed a Chiari with large syrinx • Underwent Chiari decompression • How long should one wait prior to deformity correction? • Repeat MRI in 4 -6 months to document decrease in syrinx Witten et al, J Neurosurg Pediatr 2008

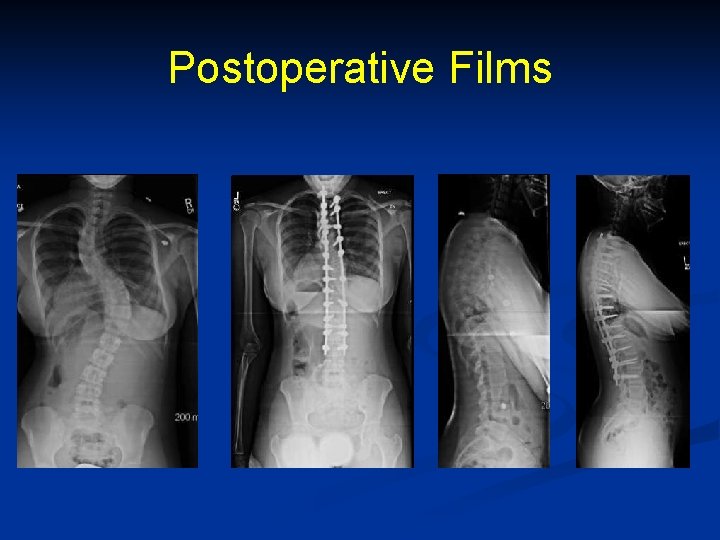
Postoperative Films

What if the syrinx does not resolve? l l Wait longer if deformity permits l Atenello et al, Neurosurgery 2008 l Median time to resolution of syrinx = 10 months Drainage of syrinx l Morbidity l Aghakhani et al, Neurosurgery 2010
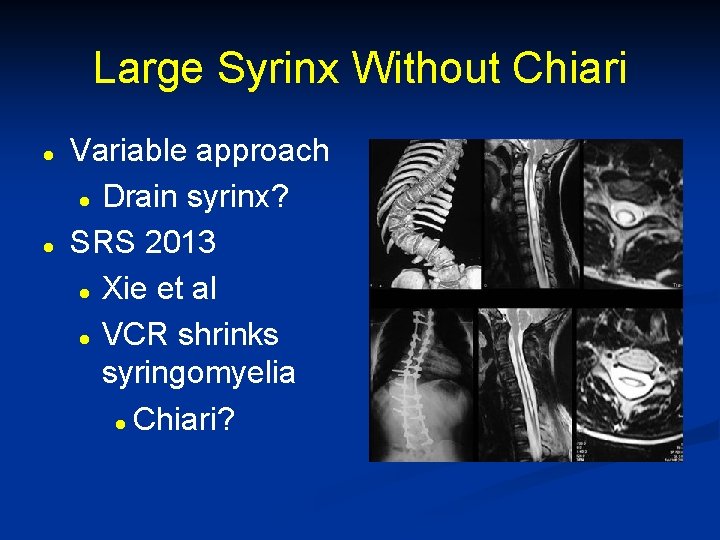
Large Syrinx Without Chiari l l Variable approach l Drain syrinx? SRS 2013 l Xie et al l VCR shrinks syringomyelia l Chiari?
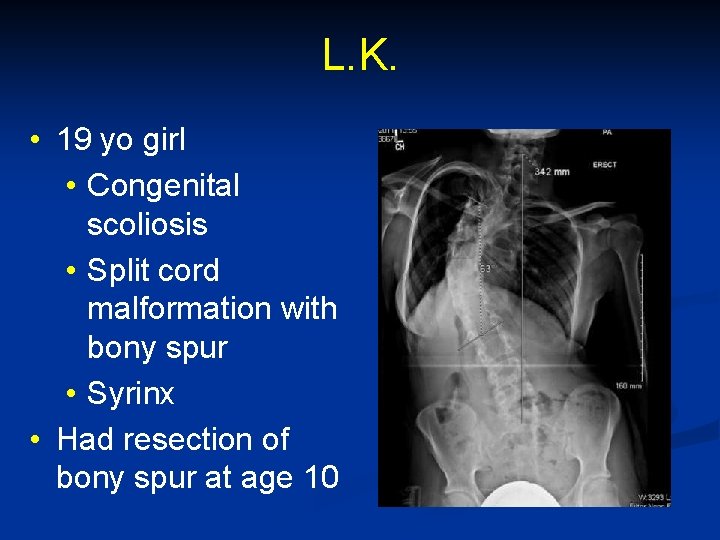
L. K. • 19 yo girl • Congenital scoliosis • Split cord malformation with bony spur • Syrinx • Had resection of bony spur at age 10
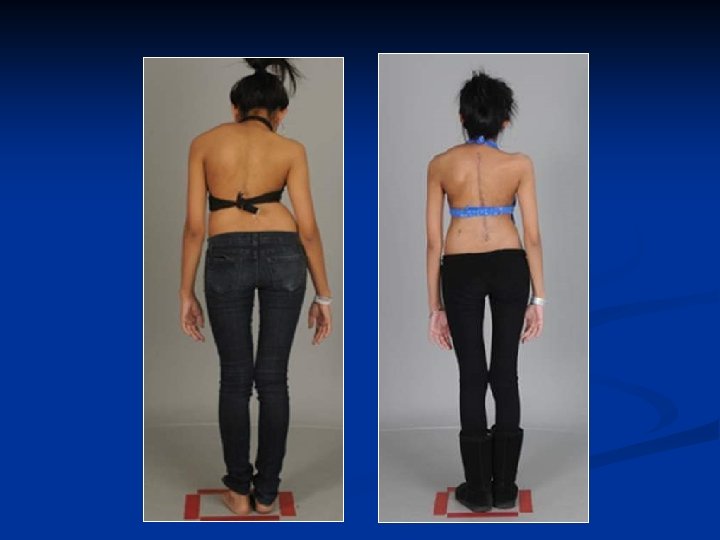
Clinical Photos
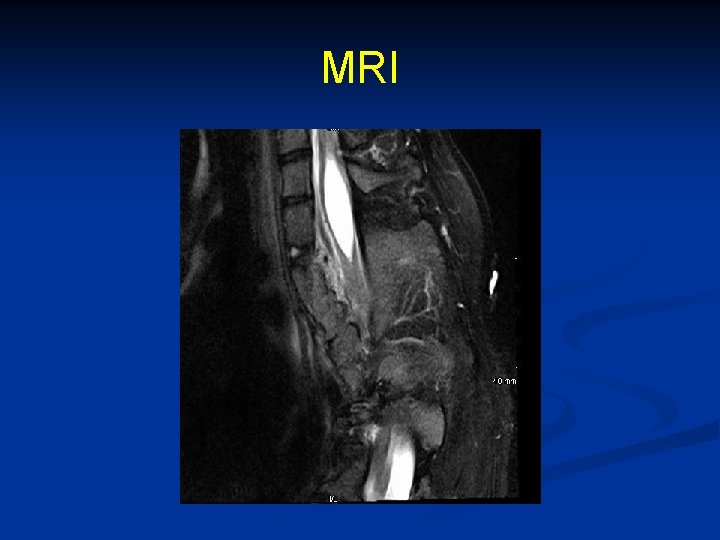
MRI Syringomyelia + Diastematomyelia
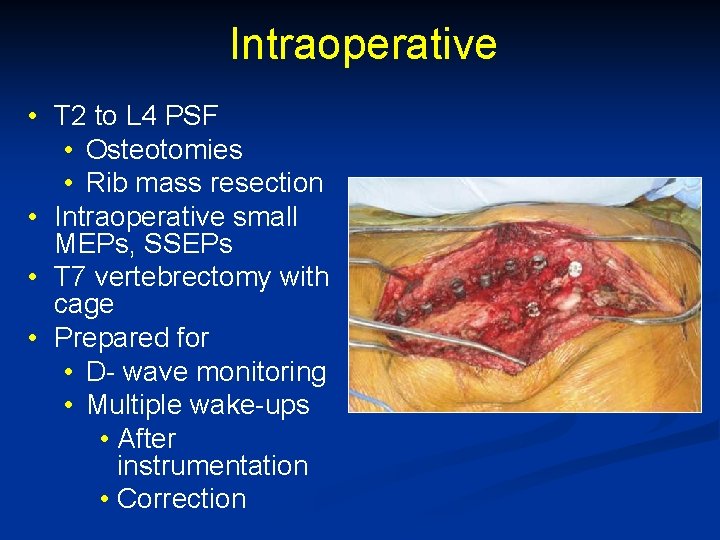
Intraoperative • T 2 to L 4 PSF • Osteotomies • Rib mass resection • Intraoperative small MEPs, SSEPs • T 7 vertebrectomy with cage • Prepared for • D- wave monitoring • Multiple wake-ups • After instrumentation • Correction
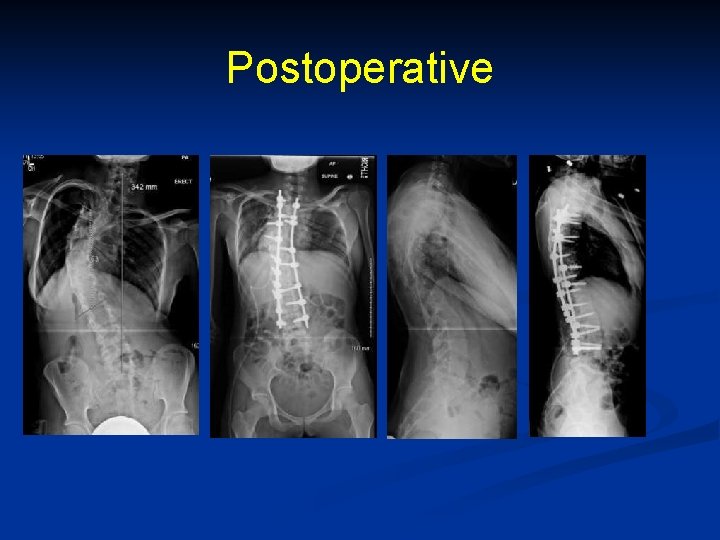
Postoperative
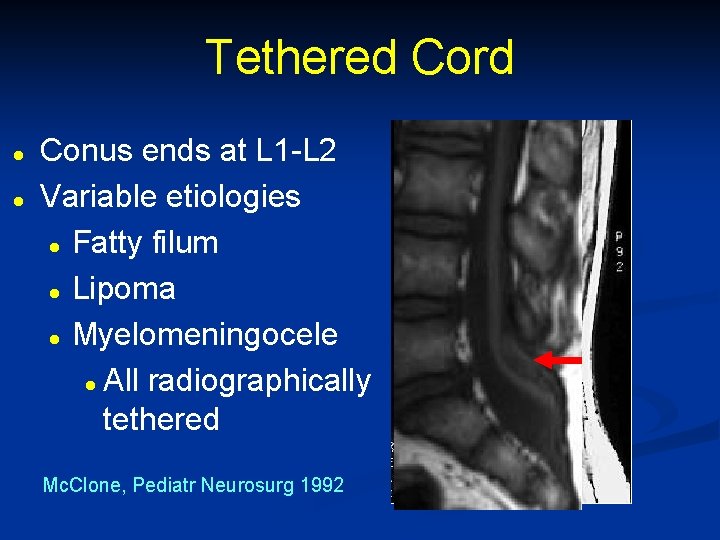
Tethered Cord l l Conus ends at L 1 -L 2 Variable etiologies l Fatty filum l Lipoma l Myelomeningocele l All radiographically tethered Mc. Clone, Pediatr Neurosurg 1992
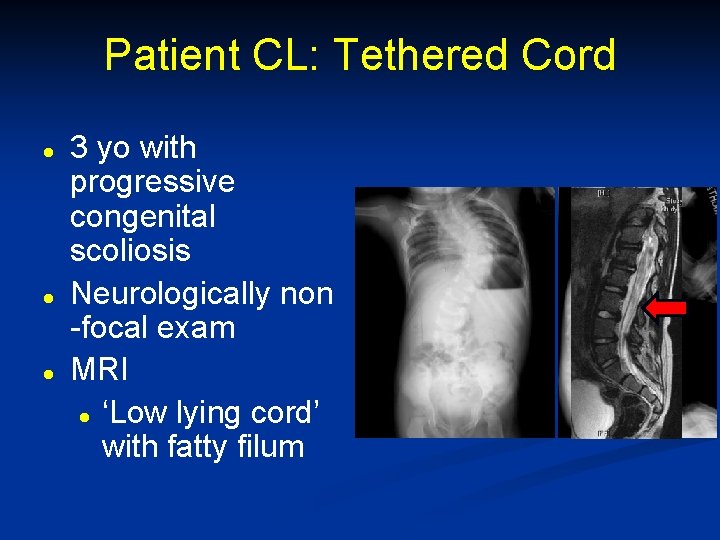
Patient CL: Tethered Cord l l l 3 yo with progressive congenital scoliosis Neurologically non -focal exam MRI l ‘Low lying cord’ with fatty filum

Fatty Filum with Low Lying Conus l l Recommend untethering l Low morbidity l Bowman et al, J Neurosurg Pediatr 2009 Family feels everything done
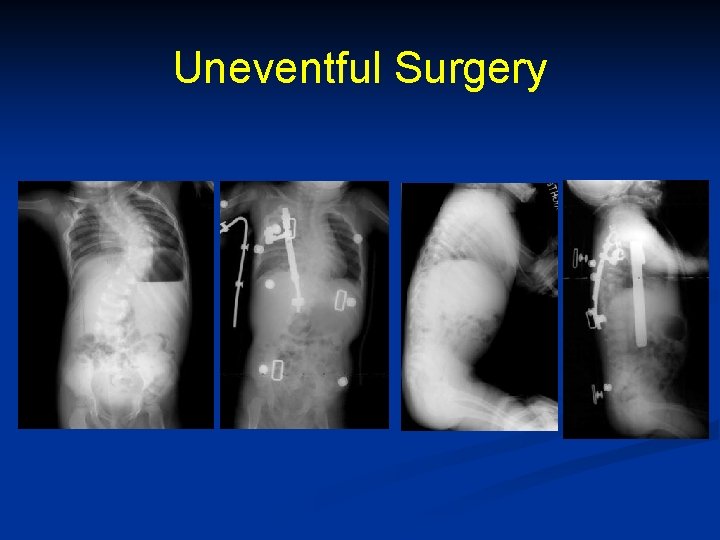
Uneventful Surgery
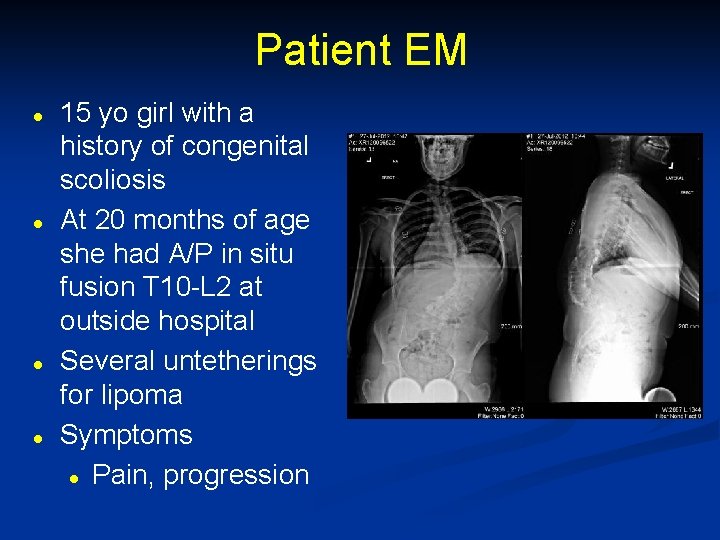
Patient EM l l 15 yo girl with a history of congenital scoliosis At 20 months of age she had A/P in situ fusion T 10 -L 2 at outside hospital Several untetherings for lipoma Symptoms l Pain, progression
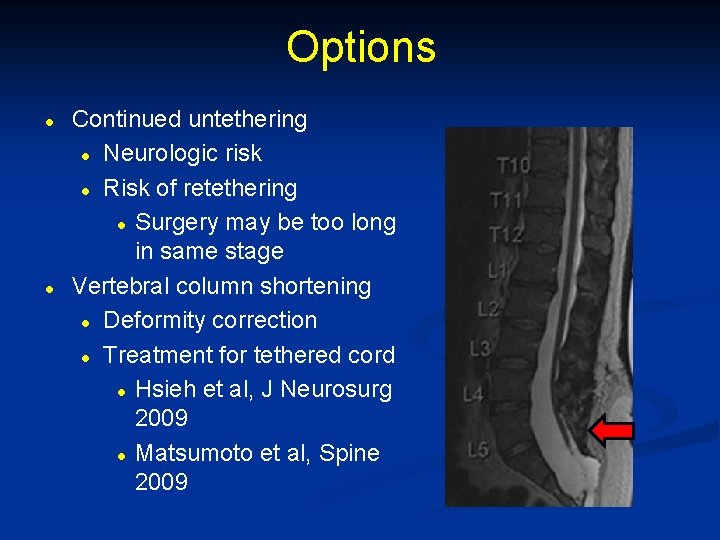
Options l l Continued untethering l Neurologic risk l Risk of retethering l Surgery may be too long in same stage Vertebral column shortening l Deformity correction l Treatment for tethered cord l Hsieh et al, J Neurosurg 2009 l Matsumoto et al, Spine 2009
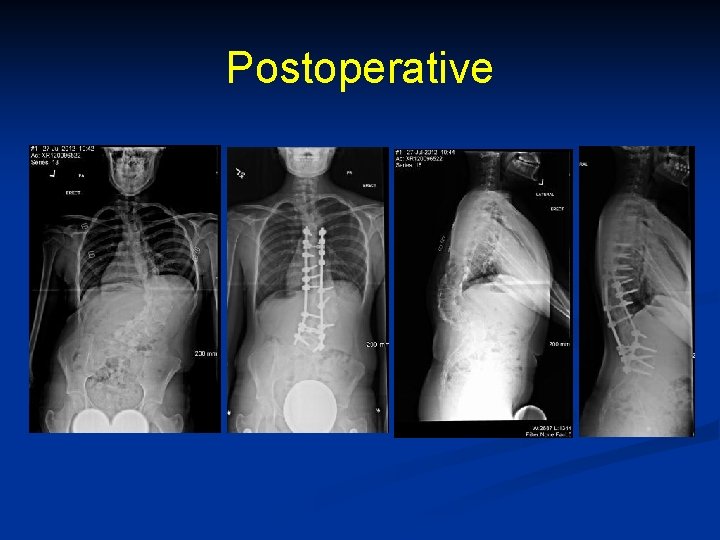
Postoperative
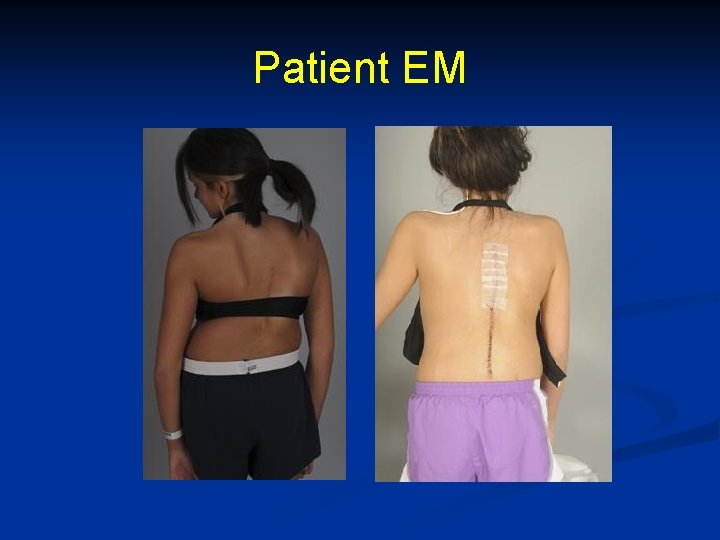
Patient EM
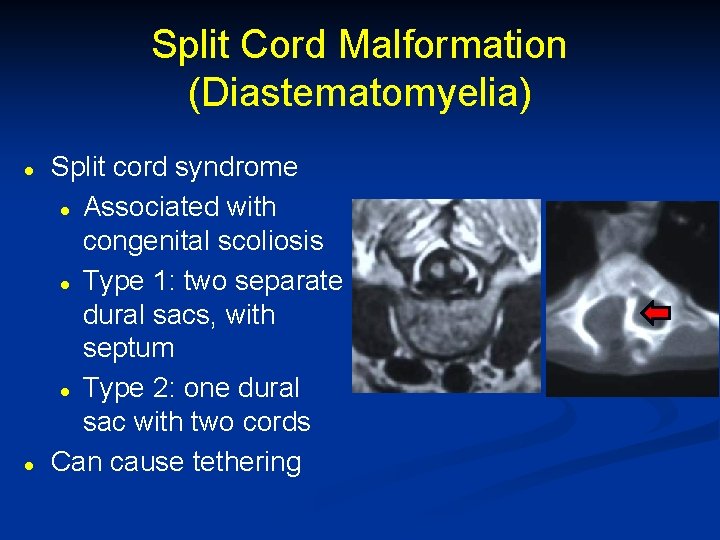
Split Cord Malformation (Diastematomyelia) l l Split cord syndrome l Associated with congenital scoliosis l Type 1: two separate dural sacs, with septum l Type 2: one dural sac with two cords Can cause tethering
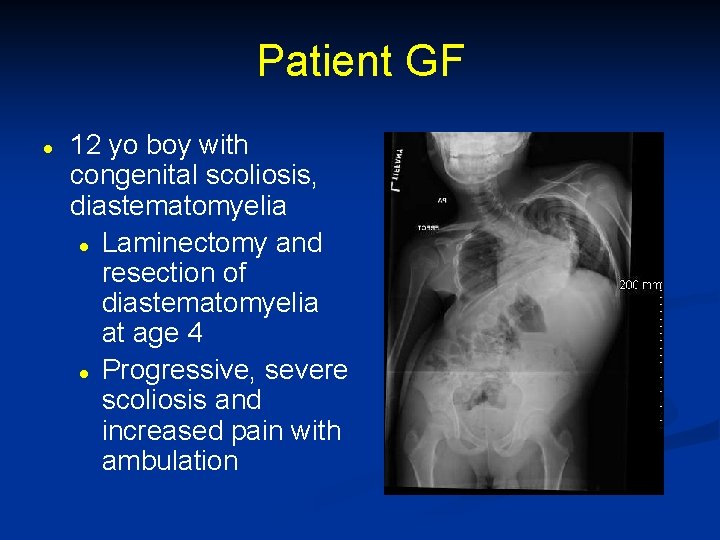
Patient GF l 12 yo boy with congenital scoliosis, diastematomyelia l Laminectomy and resection of diastematomyelia at age 4 l Progressive, severe scoliosis and increased pain with ambulation
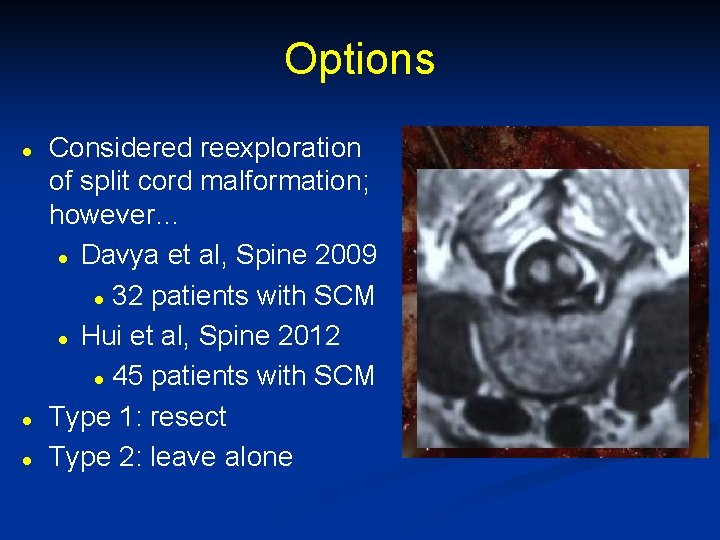
Options l l l Considered reexploration of split cord malformation; however… l Davya et al, Spine 2009 l 32 patients with SCM l Hui et al, Spine 2012 l 45 patients with SCM Type 1: resect Type 2: leave alone
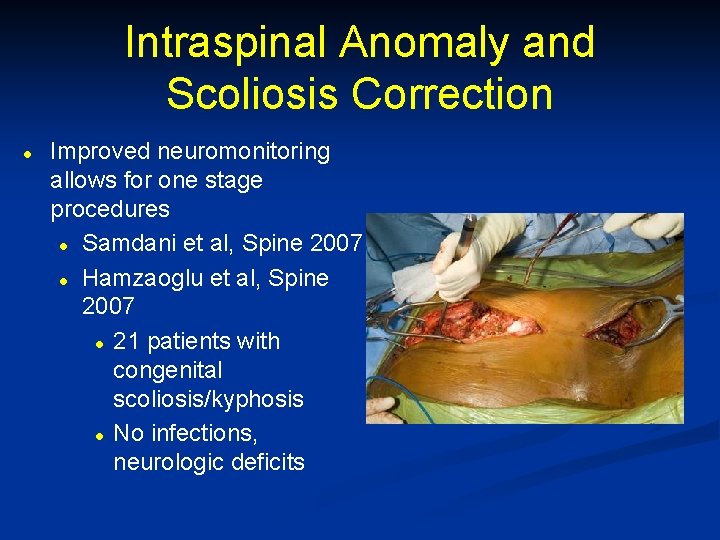
Intraspinal Anomaly and Scoliosis Correction l Improved neuromonitoring allows for one stage procedures l Samdani et al, Spine 2007 l Hamzaoglu et al, Spine 2007 l 21 patients with congenital scoliosis/kyphosis l No infections, neurologic deficits

Congenital Scoliosis and Neurologic Risk l l Hwang et al, JNS Pediatr 2013 Possible reasons l ? Vascular anomalies to spinal cord l Vitale et al, JBJS 2010 l Cardiopulmonary comorbidity risk factor l Mik et al, “Diminished spinal cord size associated with congenital scoliosis of the thoracic spine, ” JBJS 2009

Summary l l l Small syrinx without Chiari can likely be left alone, although a repeat MRI to demonstrate nonprogression should be considered Split cord malformation type 2 may not need to be treated prior to congenital spine deformity For complex anomalies spinal cord shortening may be safest
- Slides: 32