What can the experience of combatting tobacco addiction

What can the experience of combatting tobacco addiction tell us about better ways of addressing other addictions? Robert West University College London March 2014 1

Declaration of competing interest • I undertake research and consultancy for companies that develop and manufacture smoking cessation medicines and licensed nicotine products • I am a trustee of the charity, QUIT • I am an honorary co-director of the National Centre for Smoking Cessation and Training • My salary and most of my research is funded by Cancer Research UK 2

Overview 1. What is needed to change behaviour? 2. Interventions and policies to reduce tobacco use 3. Implications for combating other addictive behaviours 3

What is needed for behaviour to change To change the incidence of a behaviour there must be a change in one or more of. . . Capability: physical and psychological abilities underlying the behaviour Opportunity: environmental factors that stimulate or inhibit behaviour Motivation: mental processes that energise and direct behaviour … relating to the target behaviour or other behaviours that compete with or support it 4
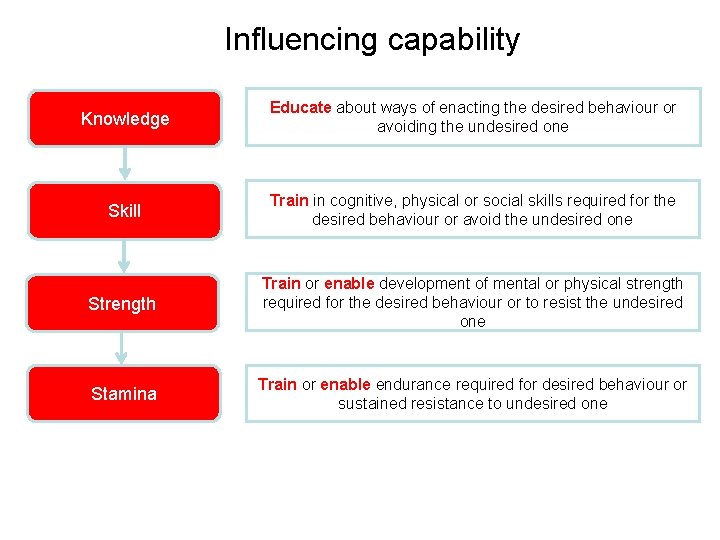
Influencing capability Knowledge Educate about ways of enacting the desired behaviour or avoiding the undesired one Skill Train in cognitive, physical or social skills required for the desired behaviour or avoid the undesired one Strength Train or enable development of mental or physical strength required for the desired behaviour or to resist the undesired one Stamina Train or enable endurance required for desired behaviour or sustained resistance to undesired one
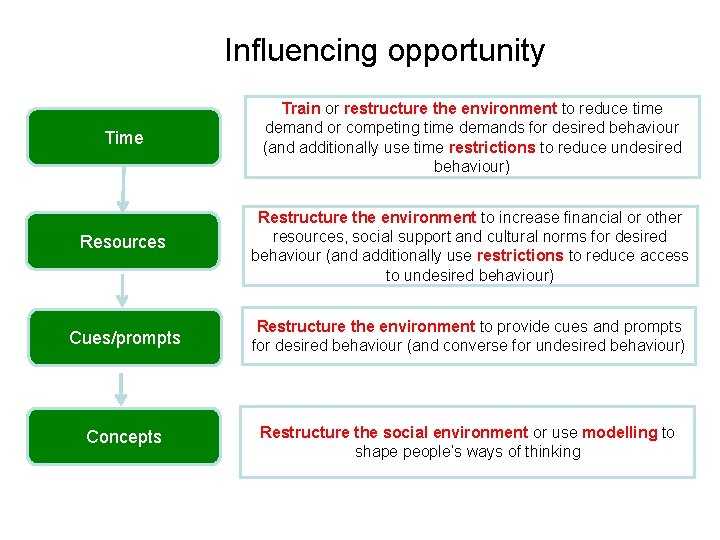
Influencing opportunity Time Train or restructure the environment to reduce time demand or competing time demands for desired behaviour (and additionally use time restrictions to reduce undesired behaviour) Resources Restructure the environment to increase financial or other resources, social support and cultural norms for desired behaviour (and additionally use restrictions to reduce access to undesired behaviour) Cues/prompts Restructure the environment to provide cues and prompts for desired behaviour (and converse for undesired behaviour) Concepts Restructure the social environment or use modelling to shape people’s ways of thinking
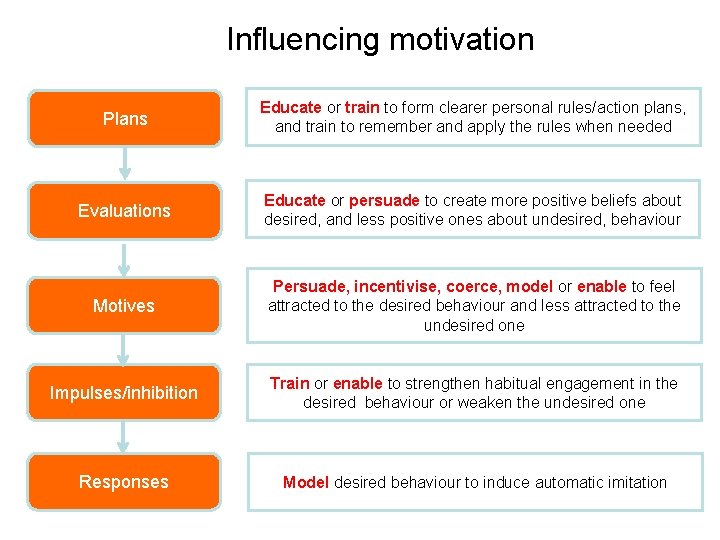
Influencing motivation Plans Educate or train to form clearer personal rules/action plans, and train to remember and apply the rules when needed Evaluations Educate or persuade to create more positive beliefs about desired, and less positive ones about undesired, behaviour Motives Persuade, incentivise, coerce, model or enable to feel attracted to the desired behaviour and less attracted to the undesired one Impulses/inhibition Train or enable to strengthen habitual engagement in the desired behaviour or weaken the undesired one Responses Model desired behaviour to induce automatic imitation

Education • What is the scope for improving understanding of – the harms of smoking? – how best to stop smoking? 8
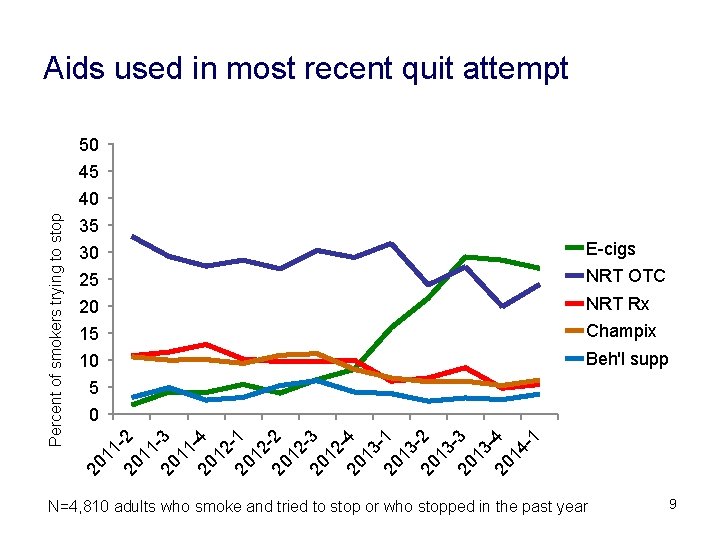
Aids used in most recent quit attempt 50 45 35 30 E-cigs 25 NRT OTC 20 NRT Rx 15 Champix 10 Beh'l supp 5 0 20 11 20 -2 11 20 -3 11 20 -4 12 20 -1 12 20 -2 12 20 -3 12 20 -4 13 20 -1 13 20 -2 13 20 -3 13 20 -4 14 -1 Percent of smokers trying to stop 40 N=4, 810 adults who smoke and tried to stop or who stopped in the past year 9

Tobacco control: education Target Scope for improvement Understanding of harmfulness of smoking Moderate Best ways of stopping smoking High Pharmacy tip: advise on best ways of stopping 10

Persuasion, incentivisation and coercion • What is the scope for increasing how much smokers – feel they want or need to stop smoking? – feel concerned about harms of smoking? – feel concerned about cost of smoking? 11
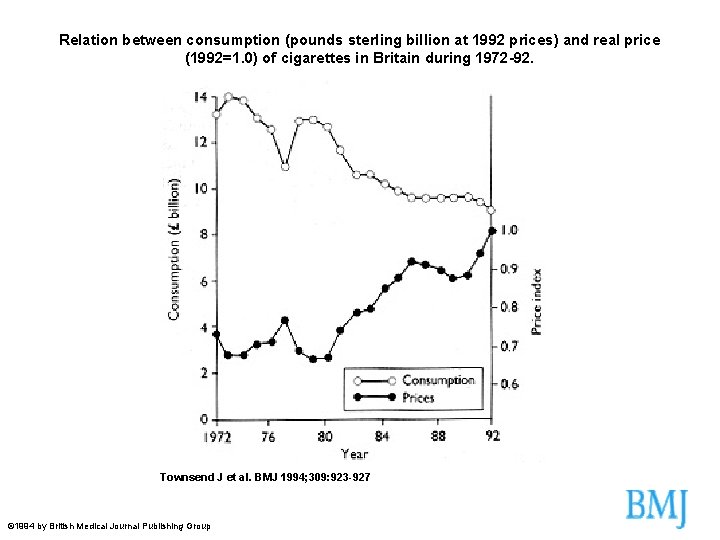
Relation between consumption (pounds sterling billion at 1992 prices) and real price (1992=1. 0) of cigarettes in Britain during 1972 -92. Townsend J et al. BMJ 1994; 309: 923 -927 © 1994 by British Medical Journal Publishing Group
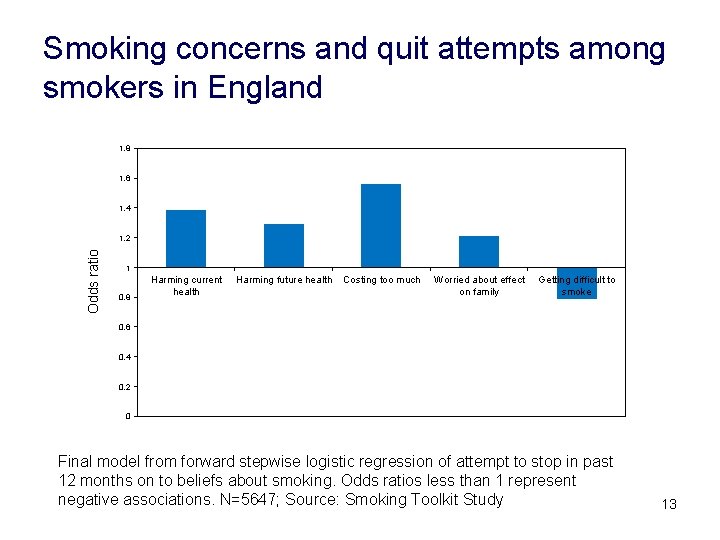
Smoking concerns and quit attempts among smokers in England 1. 8 1. 6 1. 4 Odds ratio 1. 2 1 0. 8 Harming current health Harming future health Costing too much Worried about effect on family Getting difficult to smoke 0. 6 0. 4 0. 2 0 Final model from forward stepwise logistic regression of attempt to stop in past 12 months on to beliefs about smoking. Odds ratios less than 1 represent negative associations. N=5647; Source: Smoking Toolkit Study 13
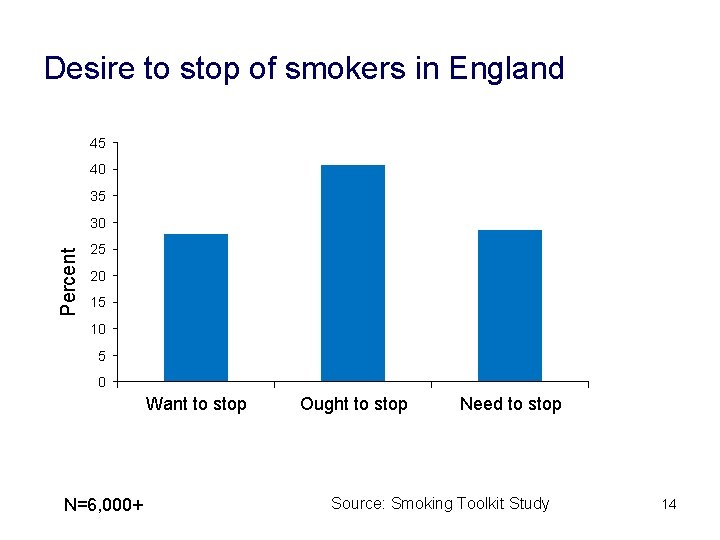
Desire to stop of smokers in England 45 40 35 Percent 30 25 20 15 10 5 0 Want to stop N=6, 000+ Ought to stop Need to stop Source: Smoking Toolkit Study 14
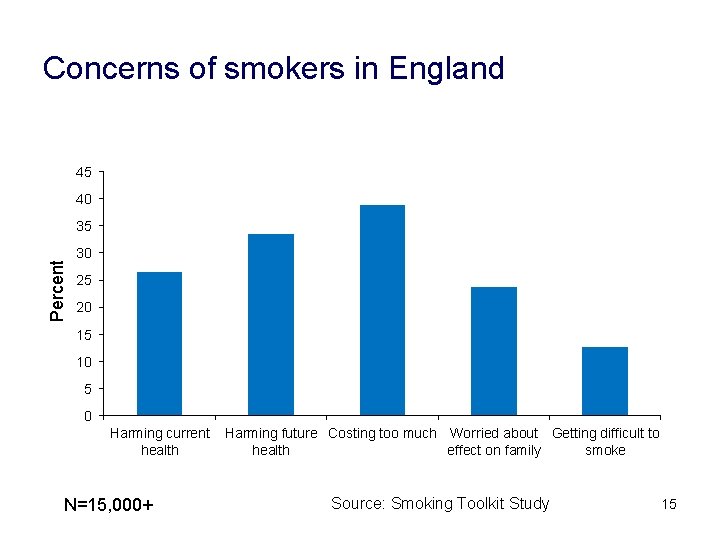
Concerns of smokers in England 45 40 Percent 35 30 25 20 15 10 5 0 Harming current health N=15, 000+ Harming future Costing too much Worried about Getting difficult to health effect on family smoke Source: Smoking Toolkit Study 15

Tobacco control: persuasion, incentivisation and coercion Target Scope for improvement Feeling of wanting to stop smoking Moderate Feeling of need to stop smoking Moderate Concern about cost of smoking Moderate Concern about health effects of smoking Moderate Concern about effect of smoking on friends and family Moderate Concern about stigma from smoking Moderate Pharmacy tip: reinforce messages about immediate benefits of quitting 16

Training • How far can we usefully improve – the planning skills needed to stop smoking? 17

Abrupt versus gradual quitting among smokers in England • Quitting abruptly: 49. 2% • Odds of success for abrupt versus gradual: 3. 2, p<0. 001 N=901. Adjusting for baseline age, gender, social grade, cigarette dependence, use of quitting aids, motivation to quit, time since quit attempt, previous quit attempts. Smoking Toolkit Study 18

Tobacco control: training Target Scope for improvement Planning skills for stopping smoking Moderate Pharmacy tip: advise smokers to stop abruptly 19

Restriction • What further scope is there for – restrictions in availability of smoking? – restrictions in locations where smoking is permitted? 20
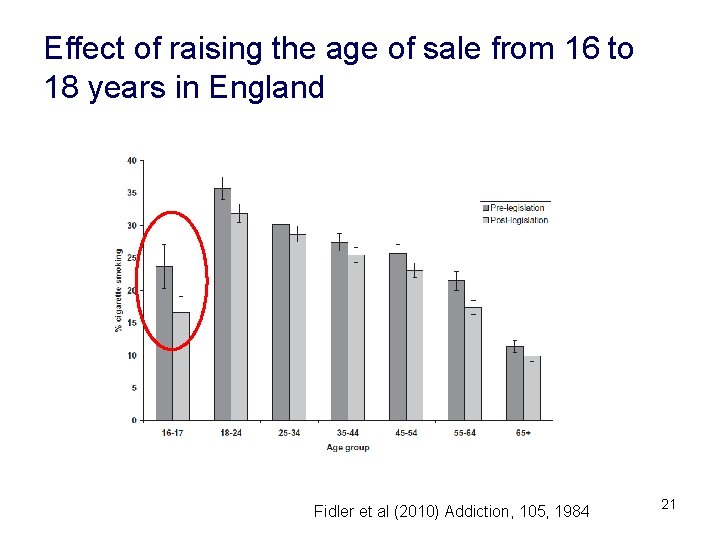
Effect of raising the age of sale from 16 to 18 years in England Fidler et al (2010) Addiction, 105, 1984 21
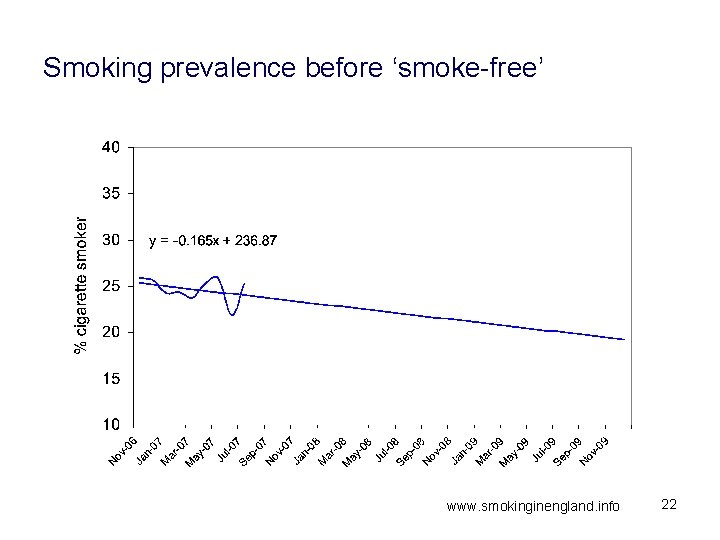
Smoking prevalence before ‘smoke-free’ www. smokinginengland. info 22
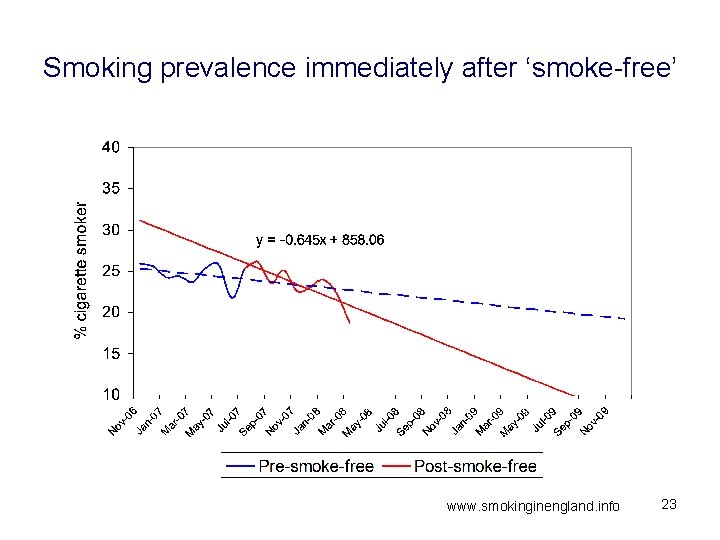
Smoking prevalence immediately after ‘smoke-free’ www. smokinginengland. info 23
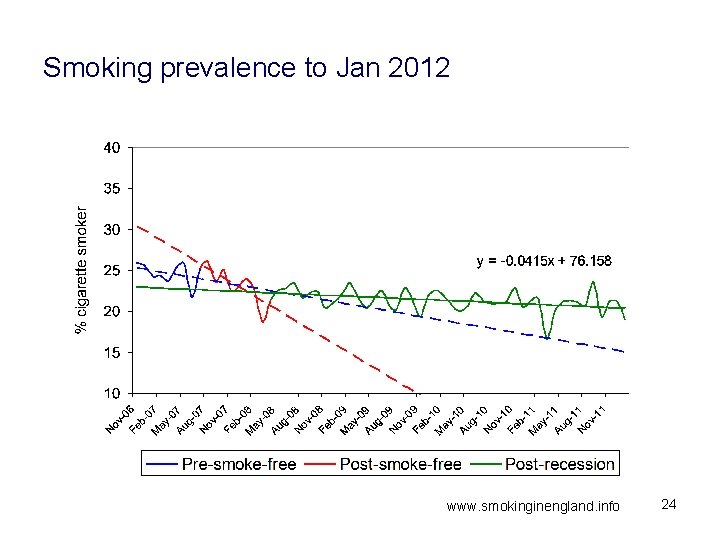
Smoking prevalence to Jan 2012 www. smokinginengland. info 24
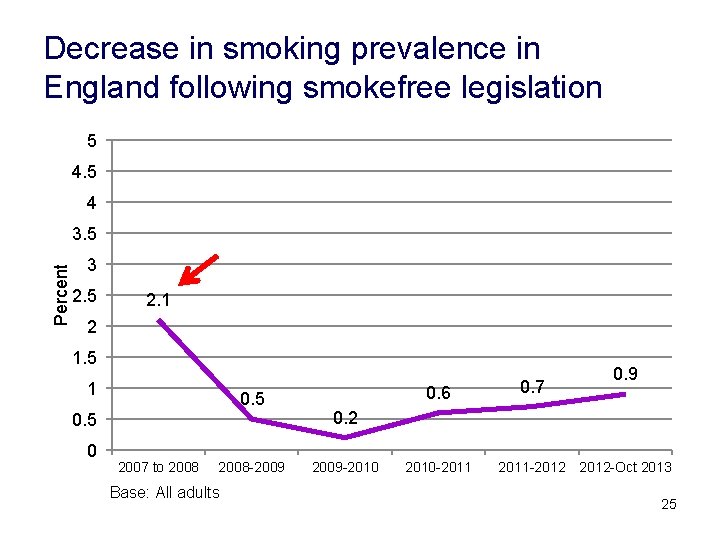
Decrease in smoking prevalence in England following smokefree legislation 5 4 Percent 3. 5 3 2. 5 2. 1 2 1. 5 1 0. 5 0 2007 to 2008 -2009 Base: All adults 0. 6 0. 7 0. 9 0. 2 2009 -2010 -2011 -2012 -Oct 2013 25

Tobacco control: restriction Target Scope for improvement Restrictions on getting cigarettes High Restrictions on where smoking is permitted Moderate Pharmacy tip: advise on use of nicotine products when cannot smoke 26

Environmental restructuring • How much further can we go in – limiting availability of smoking? – limiting prompts and cues for smoking? – making smoking non-normative? – providing triggers for stopping smoking? 27
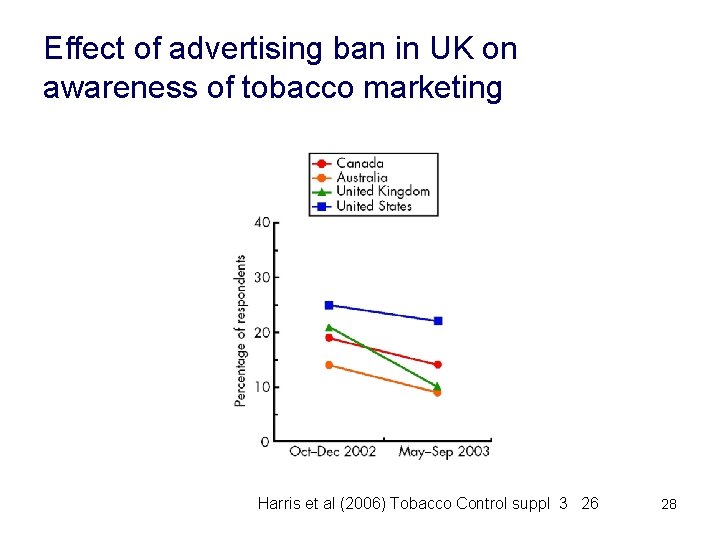
Effect of advertising ban in UK on awareness of tobacco marketing Harris et al (2006) Tobacco Control suppl 3 26 28
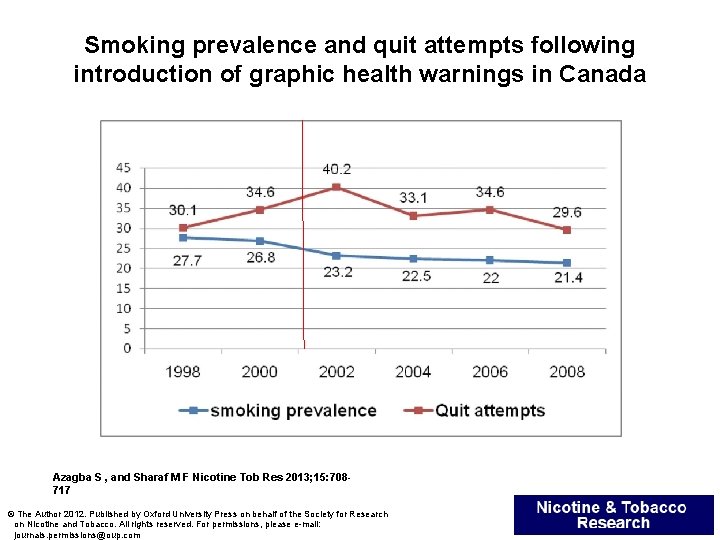
Smoking prevalence and quit attempts following introduction of graphic health warnings in Canada Azagba S , and Sharaf M F Nicotine Tob Res 2013; 15: 708717 © The Author 2012. Published by Oxford University Press on behalf of the Society for Research on Nicotine and Tobacco. All rights reserved. For permissions, please e-mail: journals. permissions@oup. com

Tobacco control: environmental restructuring Target Scope for improvement Limited availability of cigarettes High Limited prompts to smoke High-Moderate Exposure to triggers to stop smoking High-Moderate Pharmacy tip: use point of sale materials to trigger quitting 30

Enablement • How much further can we help to – limit drives and impulses to smoke? – help smokers with self-regulation? 31
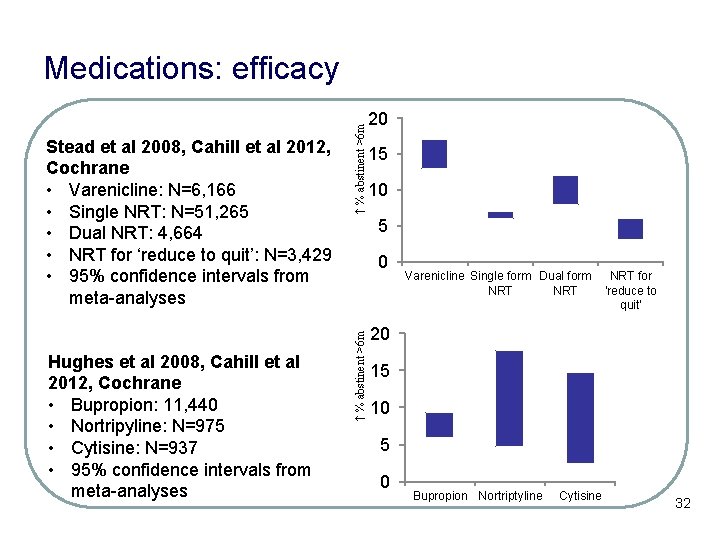
Hughes et al 2008, Cahill et al 2012, Cochrane • Bupropion: 11, 440 • Nortripyline: N=975 • Cytisine: N=937 • 95% confidence intervals from meta-analyses 20 15 10 5 0 ↑ % abstinent >6 m Stead et al 2008, Cahill et al 2012, Cochrane • Varenicline: N=6, 166 • Single NRT: N=51, 265 • Dual NRT: 4, 664 • NRT for ‘reduce to quit’: N=3, 429 • 95% confidence intervals from meta-analyses ↑ % abstinent >6 m Medications: efficacy Varenicline Single form Dual form NRT NRT for 'reduce to quit' 20 15 10 5 0 Bupropion Nortriptyline Cytisine 32
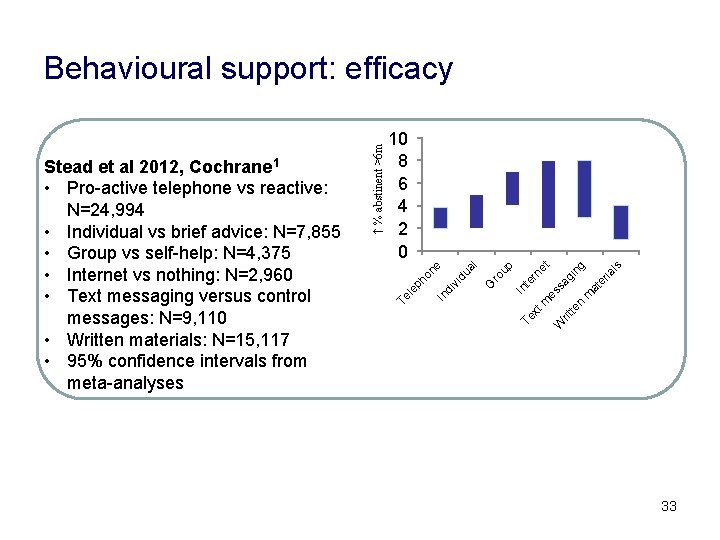
W rit te n m at er ia l s in g ag es s rn et xt m In te Te G ro up al id u di v In le p ho n e 10 8 6 4 2 0 Te Stead et al 2012, Cochrane 1 • Pro-active telephone vs reactive: N=24, 994 • Individual vs brief advice: N=7, 855 • Group vs self-help: N=4, 375 • Internet vs nothing: N=2, 960 • Text messaging versus control messages: N=9, 110 • Written materials: N=15, 117 • 95% confidence intervals from meta-analyses ↑ % abstinent >6 m Behavioural support: efficacy 33

Tobacco control: enablement Target Scope for improvement Effectiveness of stop smoking medicines Moderate Effectiveness of alternative nicotine products High-moderate Effectiveness of stop smoking advice/support Moderate Access to stop smoking medicines High-moderate Access to stop alternative nicotine products High-moderate Access to behavioural support High-moderate Pharmacy tip: offer specialist support and expert advice for quitting 34

Helping smokers to help themselves by bring the science of stopping to smokers www. smokefreeformula. com 35
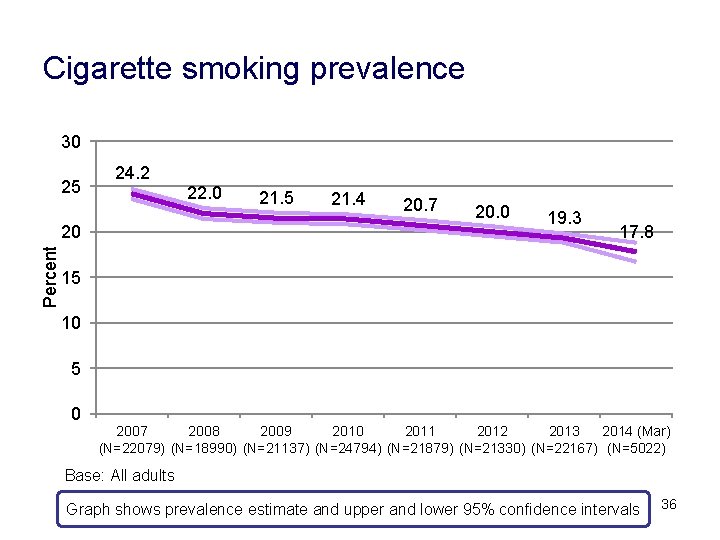
Cigarette smoking prevalence 30 25 24. 2 Percent 20 22. 0 21. 5 21. 4 20. 7 20. 0 19. 3 17. 8 15 10 5 0 2007 2008 2009 2010 2011 2012 2013 2014 (Mar) (N=22079) (N=18990) (N=21137) (N=24794) (N=21879) (N=21330) (N=22167) (N=5022) Base: All adults Graph shows prevalence estimate and upper and lower 95% confidence intervals 36
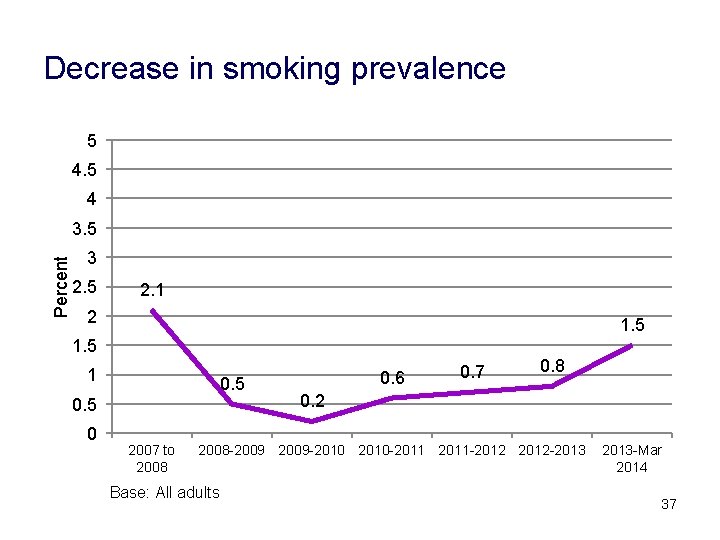
Decrease in smoking prevalence 5 4 Percent 3. 5 3 2. 5 2. 1 2 1. 5 1 0. 5 0 2007 to 2008 0. 6 0. 7 0. 8 0. 2 2008 -2009 -2010 -2011 -2012 -2013 Base: All adults 2013 -Mar 2014 37
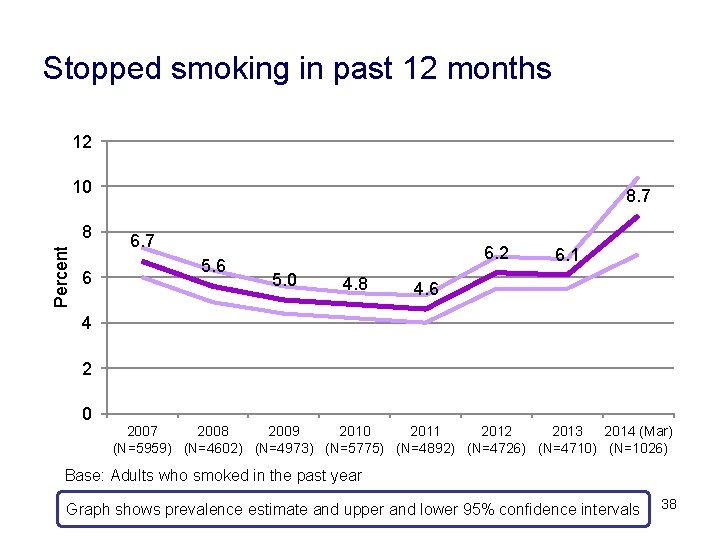
Stopped smoking in past 12 months 12 10 Percent 8 6 8. 7 6. 7 5. 6 6. 2 5. 0 4. 8 6. 1 4. 6 4 2 0 2007 2008 2009 2010 2011 2012 2013 2014 (Mar) (N=5959) (N=4602) (N=4973) (N=5775) (N=4892) (N=4726) (N=4710) (N=1026) Base: Adults who smoked in the past year Graph shows prevalence estimate and upper and lower 95% confidence intervals 38
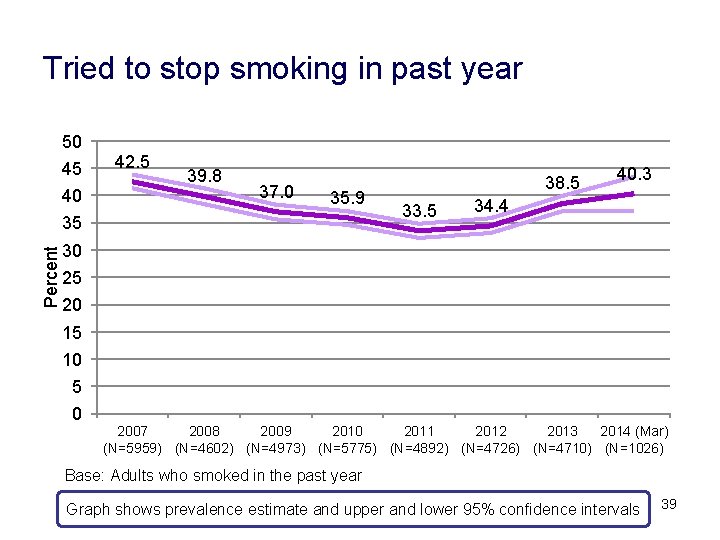
Tried to stop smoking in past year 50 45 40 42. 5 39. 8 37. 0 35. 9 Percent 35 38. 5 33. 5 40. 3 34. 4 30 25 20 15 10 5 0 2007 2008 2009 2010 2011 2012 2013 2014 (Mar) (N=5959) (N=4602) (N=4973) (N=5775) (N=4892) (N=4726) (N=4710) (N=1026) Base: Adults who smoked in the past year Graph shows prevalence estimate and upper and lower 95% confidence intervals 39
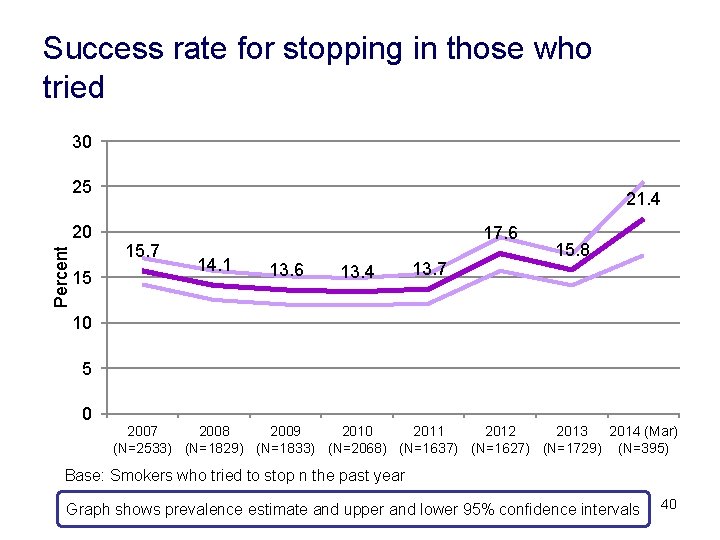
Success rate for stopping in those who tried 30 25 Percent 20 15 21. 4 15. 7 17. 6 14. 1 13. 6 13. 4 13. 7 15. 8 10 5 0 2007 2008 2009 2010 2011 2012 2013 2014 (Mar) (N=2533) (N=1829) (N=1833) (N=2068) (N=1637) (N=1627) (N=1729) (N=395) Base: Smokers who tried to stop n the past year Graph shows prevalence estimate and upper and lower 95% confidence intervals 40
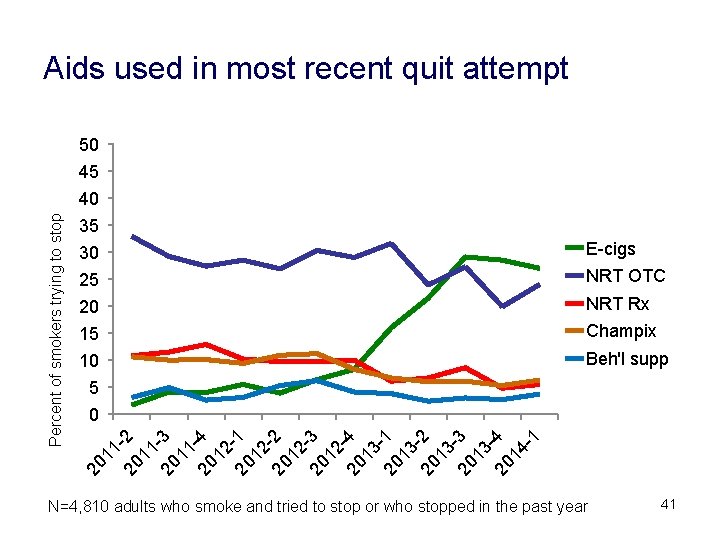
Aids used in most recent quit attempt 50 45 35 30 E-cigs 25 NRT OTC 20 NRT Rx 15 Champix 10 Beh'l supp 5 0 20 11 20 -2 11 20 -3 11 20 -4 12 20 -1 12 20 -2 12 20 -3 12 20 -4 13 20 -1 13 20 -2 13 20 -3 13 20 -4 14 -1 Percent of smokers trying to stop 40 N=4, 810 adults who smoke and tried to stop or who stopped in the past year 41

What about other addictive behaviours? • Should policies follow tobacco control? – Run mass media campaigns – Promote brief advice from health professionals – Impose moderately high duty and control illicit supply – Partially stigmatise use – Permit widespread sale – Impose legal age of sale – Restrict marketing – Restrict locations where can be used – Require warning labels on packets – Provide treatments to aid cessation 42
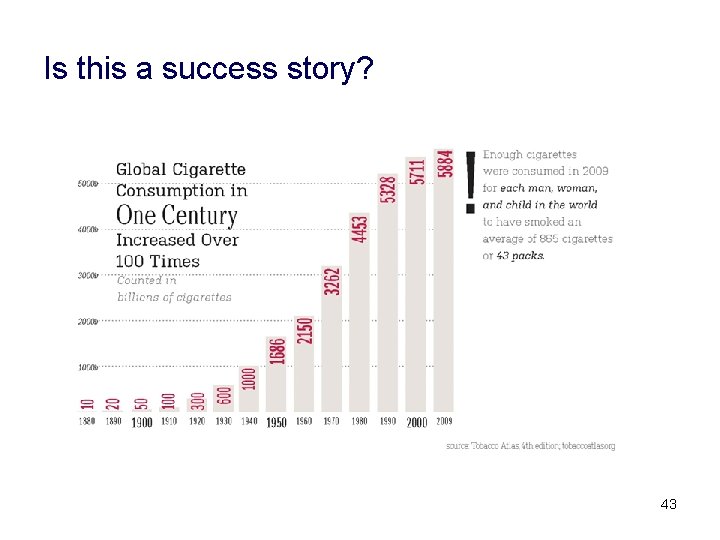
Is this a success story? 43
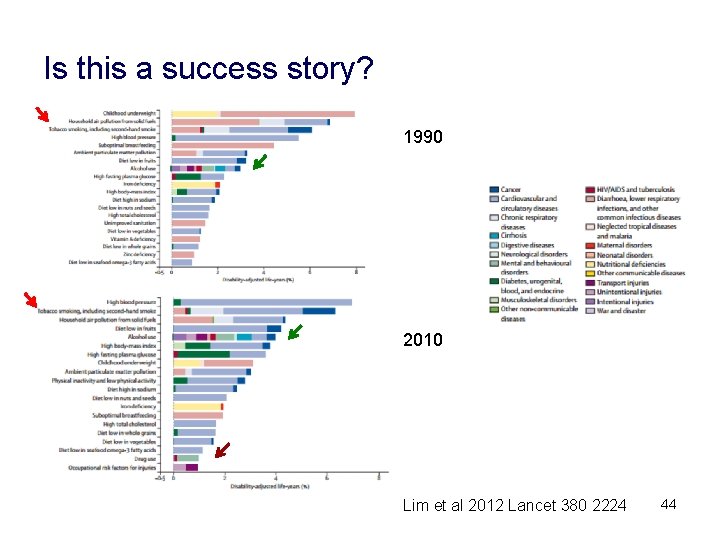
Is this a success story? 1990 2010 Lim et al 2012 Lancet 380 2224 44

Conclusions • Tobacco control is probably not a great example of how to combat a lethal addictive behaviour • Most of the potential levers of change to combat tobacco use is being applied in most of society at best to a moderate degree • Pharmacy can do more to reach more smokers with expert professional advice on: – best ways of stopping – how to use medicines effectively – where feasible, providing specialist support 45

Commercial interests and political indifference 46

Tobacco control policies 47
- Slides: 47