Western Michigan HFMA MHA Finance Policy Update Nov
















































- Slides: 55

Western Michigan HFMA MHA Finance Policy Update Nov. 18, 2015 Vickie R. Kunz, senior director, Health Finance Nathanael Wynia, director, Finance 1

Who is the MHA? • Advocacy organization representing all hospitals in Michigan. • Activities include: – State advocacy on proposed legislation, including Medicaid funding and policy activities – Federal advocacy and policy on Medicare and Medicaid issues – MHA Keystone Center – Quality Improvement and Patient Safety Initiatives – BCBSM Contract Administration Process • Unique to Michigan 2

Payer Issues • The role of the MHA is to assist in resolving systematic payer issues. • Individual hospital contracts determine terms and conditions and take precedence. • Communicate issues to Marilyn Litka-Klein or Vickie Kunz at the MHA. 3

Examples of MHA Involvement in Other Issues • Maximize federal funding in state Quality Assurance Assessment Program (QAAP) • Medicaid implementation of MI Health Link • Provide input on proposed policies and analysis of proposed and final policies. • BCBSM DRG validation audits • Auto No-Fault Insurance • CFO Forums 4

MHA CFO Forums • Changes in the Financial Landscape • • • Friday, Dec. 11 – Marquette Friday, Jan. 8 – Bay City Tuesday, Feb. 23 – Troy Wednesday, Feb. 24 – Grand Rapids Registration available at: http: //www. mha. org/docs/cfo_forum_reg_form. pdf. • Agenda includes: • Insurance Landscape • Hospital Landscape • Medicaid, Medicare and BCBSM. 5

Today’s Medicare Agenda • • Bipartisan Budget Act of 2015. Comprehensive Care for Joint Replacement (CCJR) FY 2016 Final VBP Program Adjustment Factors. 2016 Final Rule Highlights: – OPPS – HHA • Proposed Discharge Planning Requirements • Improvements - Medicare RAC Process 6

Federal Budget Agreement • Bipartisan Budget Act of 2015 - passed by Congress Oct. 30 and signed into law by President Obama Nov. 2. • Implements Medicare “site-neutral” payment reductions for new off-campus hospital outpatient departments (HOPDs). 7

Continued, Federal Budget Agreement • “New PB HOPD” defined as entity that started billing for Medicare outpatient services on/after Nov. 2, 2015. • “Off campus PB HOPD” defined as departments that are not on the main campus of a hospital and are located more than 250 yards away. • No change for existing provider-based HOPDs which will continue to be paid under Medicare OPPS. • PB HOPD = provider-based hospital outpatient department 8

Continued, Federal Budget Agreement • Jan. 1, 2017 - New or off-campus HOPDs would not be eligible for OPPS reimbursement. – Savings estimated at $9. 4 billion over 10 years. • Instead these new off-campus HOPDs would be reimbursed under other Medicare Part B payment systems: – Physician fee schedule (PFS) – Ambulatory surgery center (ASC) or – Clinical laboratory fee schedule (CLFS). 9

Continued, Federal Budget Agreement • Does your hospital/health system have projects underway that will be impacted by this change? • If so, please email Vickie Kunz at the MHA. (vkunz@mha. org). 10

Continued, Federal Budget Agreement • Extends Medicare sequester one additional year from FY 2024 to FY 2025. – Estimated Michigan hospital impact: $180 million. 11

Comprehensive Care Joint Replacement • Final rule released Nov. 16. • Implements first mandatory bundled payments program in 67 metropolitan statistical areas of U. S. effective April 1, 2016. – Includes Flint and Saginaw, Michigan • Episodes triggered by index admission assigned to MS-DRG 469 or 470. 0469 MAJOR JOINT REPLACEMENT OR REATTACHMENT OF LOWER EXTREMITY W MCC 0470 MAJOR JOINT REPLACEMENT OR REATTACHMENT OF LOWER EXTREMITY W/O MCC 12

FY 2016 Medicare VBP Program Factors • Final factors released by CMS in late October. • FY 2016 IPPS base payments reduced by 1. 75%, to fund an estimated $1. 5 billion in incentive payments from Medicare value-based purchasing program. – Up from 1. 5% payment withhold in FY 2015 • Under VBP program, eligible hospitals have the opportunity to break even or earn more or less than their contribution, depending on their total 13 performance score.

Cont. , FY 2016 Medicare VBP Program • 52 Michigan hospitals will earn more than they contribute while 35 hospitals will earn less. • Following release of measure-specific scores on Hospital Compare, the MHA will provide hospitals with an impact analysis that reflects the final VBP program impact for FYs 2015, 2016 and estimated FY 2017. • MHA will also provide an impact summary for all three Medicare quality-based programs when final data are available. 14

Medicare OPPS Final Rule Highlights • Overall rate update of negative 0. 4 percent after 2. 4% MB is reduced for 0. 7 percent point ACA reductions and 2 percentage point reduction to account for the Office of the Actuary’s previous overestimation for the amount of package lab tests. • Hospitals that do not publicly report quality measure data would be subject to statutory 2. 0 percentage point additional reduction. 15

Continued, Medicare OPPS Final Rule • 10 new comprehensive APCs – Ear, nose & throat procedures – Intraocular procedures – Gynecologic procedures – Laparoscopy – Musculoskeletal procedures – Urology and related procedures – Ancillary outpatient procedures when a patient expires. 16 – Observation services

Continued, Medicare OPPS Final Rule • New comprehensive observation services APC (C -APC-8011) will replace the existing composite extended assessment and management APC 8009. • Excludes claims with surgical procedures with status indicator “T”. • CMS will include all E/D visits as eligible services paid through C-APC 8011, rather than only the high-level E/D visits. 17

Continued, Medicare OPPS Final Rule • APC re-structuring for 9 APC clinical categories: – Airway endoscopy procedures – Diagnostic tests – Excision/biopsy and incision and drainage procedures – Gastrointestinal procedures – Imaging services – Orthopedic procedures – Skin procedures – Urology procedures and vascular procedures. 18

Two-Midnight Policy • CMS finalized its proposal that certain hospital inpatient services that do not cross two midnights may be appropriate for payment under Medicare Part A if a physician determines and documents in the medical record that the patient requires reasonable and necessary admission as an inpatient. 19

Continued, Two-Midnight Policy • Relevant factors in determining whether an inpatient admission is appropriate where patient stay is expected to be less than two midnights: – Severity of patient’s signs and symptoms – Medical predictability of adverse patient outcomes 20

Continued, Two-Midnight Policy • Quality Improvement Organizations (QIOs) rather than Recovery Audit Contractors (RACs) or Medicare Administrative Contractors (MACs) will conduct first-line medical reviews of the majority of patient status claims and educate hospitals about claims that were denied under the two-midnight policy. – Effective Oct. 1, 2015 • RACs will focus on hospitals with consistently high denial rates. 21

Continued, OPPS Final Rule • MHA will distribute an updated hospital-specific impact analysis and rule brief in the near future. • Watch for additional info regarding upcoming webinars – Joint webinar hosted by MHA and HFMA. – Data. Gen webinar 22

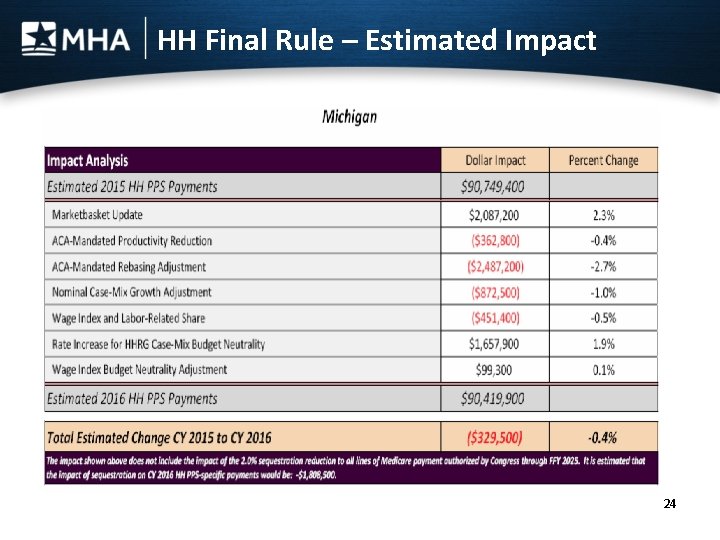
Home Health Agency Final Rule • Effective Jan. 1, 2016. • 2016 payments reduced 1. 4 percent from current payment levels. – 2. 3% Market basket update reduced by 0. 4% ACA adjustment – 0. 97% reduction for estimated case-mix growth – Third of fourth payment rebasing cut of 2. 4%. • MHA distributed an update hospital-specific impact analysis Nov. 17. 23

HH Final Rule – Estimated Impact 24

Proposed Rule – Discharge Planning Requirements • Would require hospitals, including, critical access hospitals, long-term acute care hospitals, inpatient rehabilitation facilities and home health agencies to create discharge plans. • Alignment with current practices, with the goal of improving patient quality of care and outcomes and reducing avoidable complications, adverse events and readmissions. • Implements the Improving Medicare Post-Acute Care Transformation Act of 2014 provisions to use data on both quality and resource use measures to assist 25 patients during discharge process.

Continued, Proposed Discharge Planning Requirements • Proposed rule would apply to all inpatients and certain outpatients: – patients receiving observation services – patients undergoing surgery or other same-day procedures where anesthesia or moderate sedation is used and – Emergency department patients who have been identified as needing a discharge plan. • Requires development of discharge plan within 24 hours of admission or registration and completion of a discharge plan before patient is discharged or 26 transferred to another facility.

Continued, Proposed Discharge Planning Requirements • Hospital (including CAHs) Requirements: – Provide discharge instructions to patients who are discharged home. – Have a medication reconciliation process with the goal or improving patient safety by enhancing medication management. – Establish a post-discharge follow-up process. • Send specific medical info to the receiving facility for patients transferred to another facility. – Applies to hospitals, CAHs, LTCHs, IRFs and HHAs. • Comments due to CMS in late December. 27

Jan. 1, 2016 Medicare RAC Improvements for Hospitals • A reduction in the number of claims that the RAC may audit for providers other than physicians and suppliers. • A decrease in additional documentation request (ADR) from 2% to 0. 5% of total Medicare paid claims from previous year. • Diversification of RAC audits across all claim types for a facility, limiting the RAC’s ability to target care provided in a particular setting. • Adjustment of the ADR up or down based on provider’s claim denial rate. 28

Cont. , May 15, 2015 Medicare RAC Improvements • RAC look-back period limited to 6 months from DOS for patient status reviews in cases where hospital submits a claim within 3 months of DOS. • See Nov. 16 MHA Monday Report article. 29

Today’s Medicaid Agenda • Medicaid – Quality Assurance Assessment Program – FY 2016 Budget – Healthy Michigan Plan – Medicaid DSH – Payment Policy Changes – Managed Care Update 30

Quality Assurance Assessment Programs • Four hospital provider tax funded programs • Medicaid Access to Care Initiative (MACI) – Medicaid FFS program began in FY 2003. – Tax and payments issued quarterly • Hospital Rate Adjustment (HRA) – Through the Medicaid HMOs, started January 2007 – Tax and payments issued monthly 31

Quality Assurance Assessment Programs • Disproportionate Share Hospital (DSH) – Outpatient Uncompensated Care DSH pool started FY 2008. – Tax and payments issued annually – Subject to Step 2 recalculation and DSH audit • Psych HRA – Started FY 2010. – Tax and payments issued quarterly 32

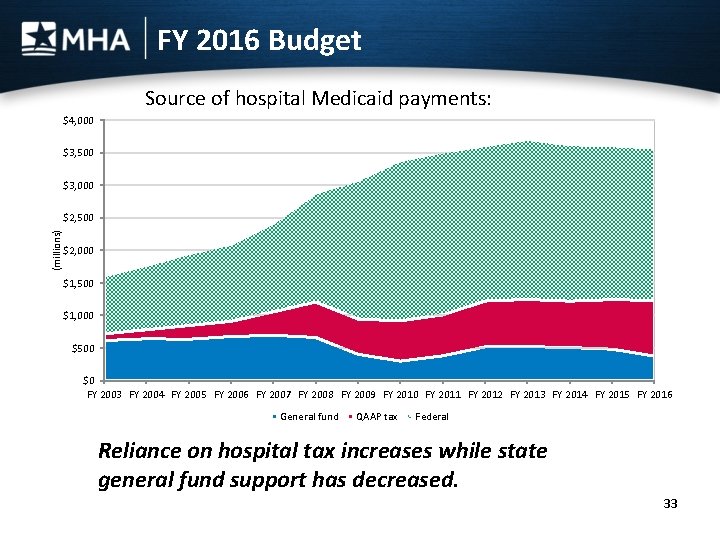
FY 2016 Budget Source of hospital Medicaid payments: $4, 000 $3, 500 $3, 000 (millions) $2, 500 $2, 000 $1, 500 $1, 000 $500 $0 FY 2003 FY 2004 FY 2005 FY 2006 FY 2007 FY 2008 FY 2009 FY 2010 FY 2011 FY 2012 FY 2013 FY 2014 FY 2015 FY 2016 General fund QAAP tax Federal Reliance on hospital tax increases while state general fund support has decreased. 33

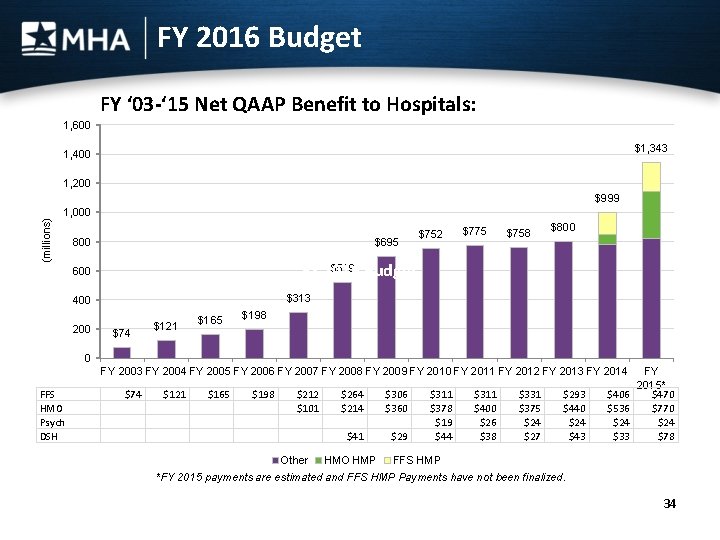
FY 2016 Budget FY ‘ 03 -‘ 15 Net QAAP Benefit to Hospitals: 1, 600 $1, 343 1, 400 1, 200 (millions) $999 1, 000 800 $695 $752 $775 $758 $800 $519 Budget FY 2016 600 $313 400 200 $74 $198 $165 $121 0 FY 2003 FY 2004 FY 2005 FY 2006 FY 2007 FY 2008 FY 2009 FY 2010 FY 2011 FY 2012 FY 2013 FY 2014 FFS HMO Psych DSH $74 $121 $165 $198 $212 $101 $264 $214 $306 $360 Other HMO HMP $41 $29 $311 $378 $19 $44 $311 $400 $26 $38 $331 $375 $24 $27 $293 $440 $24 $43 $406 $536 $24 $33 FY 2015* $470 $770 $24 $78 FFS HMP *FY 2015 payments are estimated and FFS HMP Payments have not been finalized. 34

FY 2016 Budget • FY 2016 budget maintains GF funding for Graduate Medical Education, Rural Access Pool and OB Stabilization Pool Payments at FY 2015 pre-EO levels. • FY 2016 budget includes a $93 million QAAP tax increase. • FY 2016 HRA pool target estimated at $100 million higher than FY 2015 pool. 35

FY 2016 Budget • • • HRA Pool Target $966 million ($866 in FY 2015) HMP HRA Target $410 million ($329 in FY 2015) Psych HRA Pool continues at $45 million FY 2016 MACI pool amount not yet determined. $85 million tax-funded outpatient uncompensated care DSH pool continues into FY 2016 • Oct. 2015 HRA payments in process include a $51 million lookback adjustment for Jan. – June 36 2015

FY 2016 Budget • Reductions: • $35 million in hospital capital payments • Prospective payments based on a blend of FFS and HMO data. Proposed by MSA in late 2014; opposition by MHA and hospitals resulted in MSA not implementing for FY 2015. 37

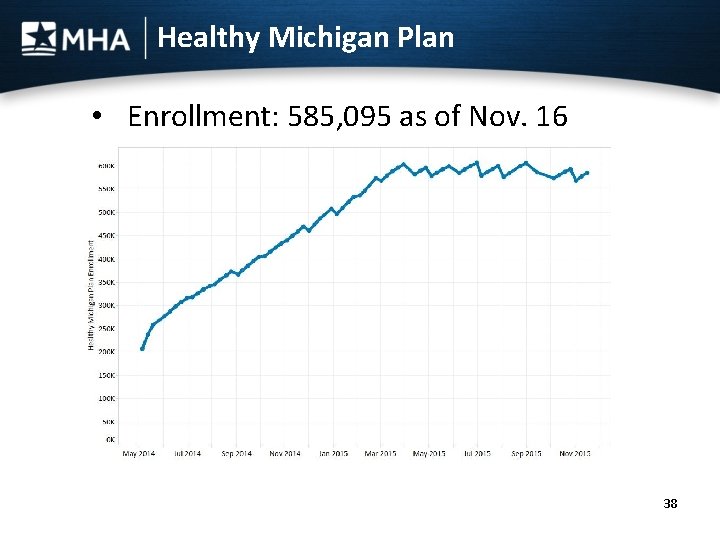
Healthy Michigan Plan • Enrollment: 585, 095 as of Nov. 16 38

Healthy Michigan Plan 39

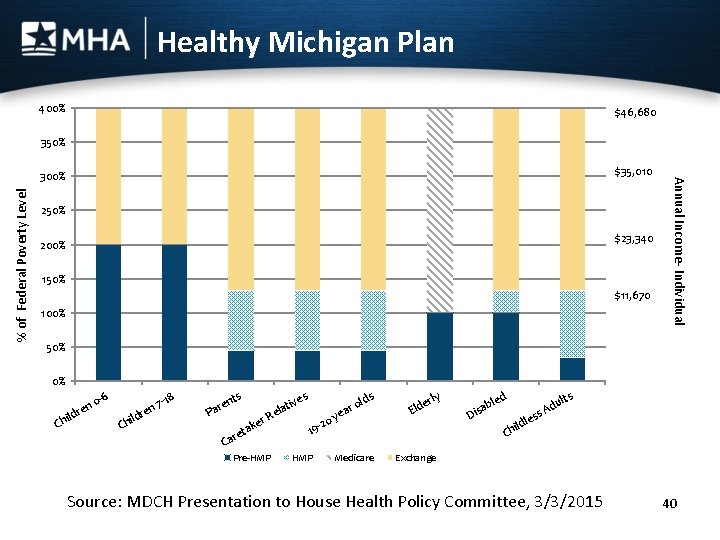
Healthy Michigan Plan 400% $46, 680 350% % of Federal Poverty Level 250% $23, 340 200% 150% $11, 670 100% Annual Income- Individual $35, 010 300% 50% 0% il n dre Ch 0 -6 Ch il n dre 8 7 -1 nts re Pa er ak ret R Ca Pre-HMP s ive t ela 20 19 HMP r yea s old Medicare y erl Eld ab Dis led les ild Ch s ult d s. A Exchange Source: MDCH Presentation to House Health Policy Committee, 3/3/2015 40

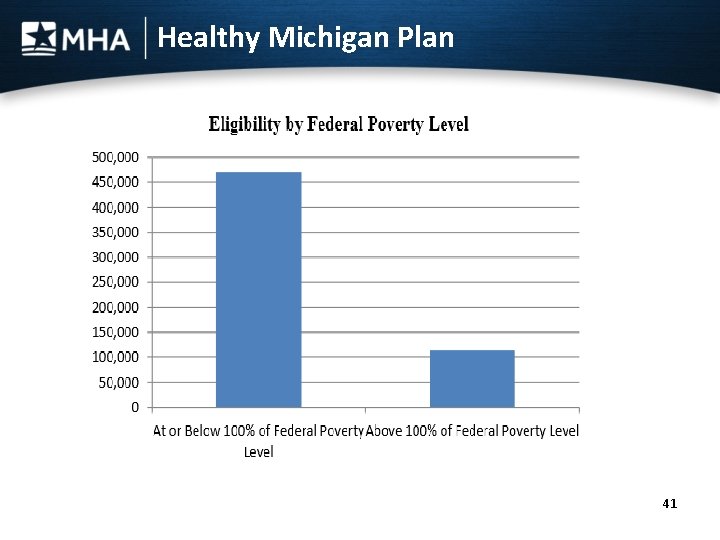
Healthy Michigan Plan 41

Healthy Michigan Plan • Waiver for cost-sharing submitted Sept. 1. • Affects individuals between 100 and 133% FPL. • State law as written requires these beneficiaries after 48 months to either: – Purchase exchange plan (eligible for tax credits) OR – Incur cost-sharing up to 7% of income to remain on HMP (can reduce contribution by participating in healthy behavior activities) 42

Healthy Michigan Plan • Waiver must be approved by Dec. 31 or HMP for all beneficiaries ends Apr. 30, 2016 • State officials in discussion with CMS • CMS concerned this could price some out of coverage • State officials optimistic CMS will approve • No alternate plan in place 43

Healthy Michigan Plan • CMS approved FY 2014 HMP MACI pool of approx. $149 million. – Payments distributed Sept. 17. – Minimal $3. 5 million QAAP tax associated with these payments for individuals that would have qualified for traditional Medicaid. • FY 2015 HMP MACI pool amount estimated at $252 million. – CMS requested that MSA recalculate this amount using a more complete claims set. 44 – Approval expected by Dec. 31.

Healthy Michigan Plan • HMP HRA payments targeted at approximately $34 million monthly • Medicaid cost report includes new forms to report HMP cost, payments, and HRA payments 45

Medicaid DSH • FY 2011: Audit complete; Step 3 payment recovery and redistribution awaiting outcome of Washington and Texas litigation • FY 2012: Step 3 (DSH audit) near complete. Draft report provided to MSA 9/30. Will be submitted to CMS by 12/31. – After accounting for CPE and ICA transactions, recoveries limited to 2 hospitals that received payments in excess of their DSH limit 46

Medicaid DSH • FY 2013 Step 2 recalculation completed; payment redistribution awaiting outcome of federal litigation • FY 2013 Step 3 (DSH audit) expected to begin in Feb. 2016. • FY 2014 Step 2 expected early 2016 • FY 2015 Step 1 payments made Sept. 24 – Payments will be recalculated in Step 2 47

Medicaid DSH • Michigan’s innovative, multi-step approach has preserved federal funding by minimizing DSH payment recoveries “States retain considerable flexibility in setting DSH State plan payment methodologies to the extent that these methodologies are consistent with section 1923(c) of the Act and all other applicable statute and regulations. Some states may determine that implementing a retrospective DSH payment methodology or a DSH reconciliation in their state plan is a reasonable way to manage its DSH allotment and ensure that payments made in excess of hospital-specific DSH limits are redistributed to hospitals that have not exceeded their limits. ” -CMS Final DSH Rule, Dec. 3, 2014 48

Medicaid Payment Policy • Effective July 1, the MSA implemented a short stay rate for specific diagnosis codes in non-surgical cases. – Claim includes a qualifying diagnosis code based on MSA policy – Outpatient claim includes observation revenue code (762) – Inpatient or outpatient claim does not include surgical revenue code (36 x) or cardiac cath revenue code (481) – Inpatient discharge of same day or next day • Rate of $1, 314 applies to Medicaid FFS cases and non-contracted HMO cases – Rate is inclusive of operating and capital – Same rate paid to hospitals regardless of hospital determination of inpatient or observation status. – If patient meets criteria for inpatient admission, patient days will be counted for Medicare DSH purposes. • List of applicable ICD-10 Codes released in final policy Sept. 1. 49

Medicaid Payment Policy Effective Oct. 1, the MSA implemented several policy changes: • Statewide DRG rate, adjusted for area wage index – one rate for PPS hospitals and another rate for CAHs – Budget-neutral statewide; individual hospital impact may vary. – Adjusted rates available on MDHHS website. • APR-DRGs, simultaneously with ICD-10. • Hospital-specific capital rates developed using a blend of FFS and HMO data. • Rates and relative weights will be updated annually on Oct. 1. 50

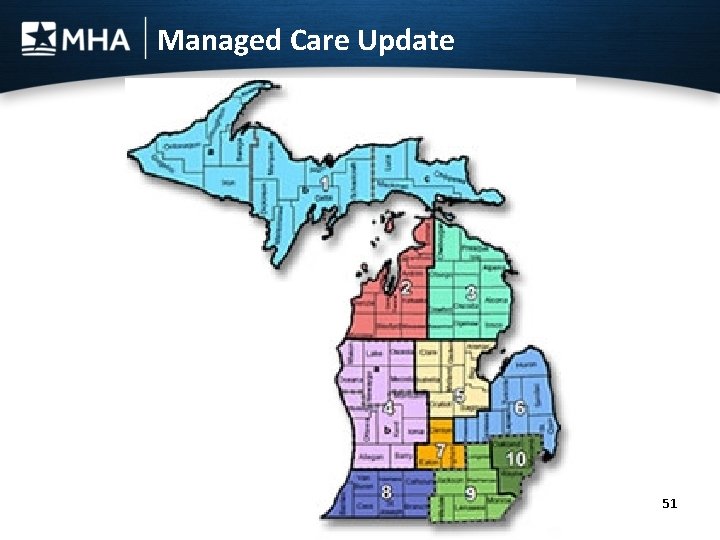
Managed Care Update 51

Managed Care Update • Service areas will be Gov. Snyder’s 10 prosperity regions. • Coverage will include MIChild • Effective Jan. 1, 2016 for five years with extensions available • Oct. 16 - Awards announced • Oct. 30 – Appeals filed • Nov. 14 – Response to appeals • Nov. 17 – State Administrative Board Meeting 52

Managed Care Update “Tentative” final results • Region 4 (Grand Rapids): – BCBSM, Mc. Laren, Meridian, Molina, Priority, UHC • Region 8 (Kalamazoo): – Aetna, Mc. Laren, Meridian, Molina, Priority, UHC • Region 7 (Lansing): – Aetna, Mc. Laren, Meridian, Molina • Appeal status: Meridian and Molina in, UHC out • PHP (Region 7) and HAP (Southeast Michigan) denied appeal at State Admin. Board 11/17. 53

MHA Resources • Monday Report is available FREE to anyone and is distributed via email each Monday morning. – Go to website and select “Newsroom”, then Monday Report • MHA Monday Report – electronic publication issued weekly • Request password if you don’t have one. – Email Donna Conklin at dconklin@mha. org to obtain MHA member ID number • Advisory Bulletins – Extensive communications available only to MHA members, as needed. (Require password to obtain from website). • Hospital specific mailings as needed for various impact analyses, etc. • Periodic member forums • See mha. org for other resources. • Monthly Financial Survey (MFS) provides free benchmarking of financial and utilization statistics. 54

? ? ? Questions? ? ? Vickie Kunz Senior Director (517) 703 -8608 vkunz@mha. org Nathanael Wynia Director (517) 703 -8625 nwynia@mha. org Michigan Health & Hospital Association 110 W. Michigan Avenue, Suite 1200 Lansing, MI 48933 55