Wessex PHE Centre Dr Jim OBrien Centre Director

Wessex PHE Centre Dr Jim O’Brien, Centre Director

Sender bodies The existing health organisations and functions that contributed some or all of their staff to Public Health England include: – – – – 2 Health Protection Agency National Treatment Agency Department of Health Strategic Health Authorities Primary Care Trusts Public health observatories Cancer registries National cancer intelligence network – Quality assurance reference centres (QARCS) – Specialist dental commissioners – Specialist commissioners – NHS cancer screening programme – UK national screening programmes (non-cancer)
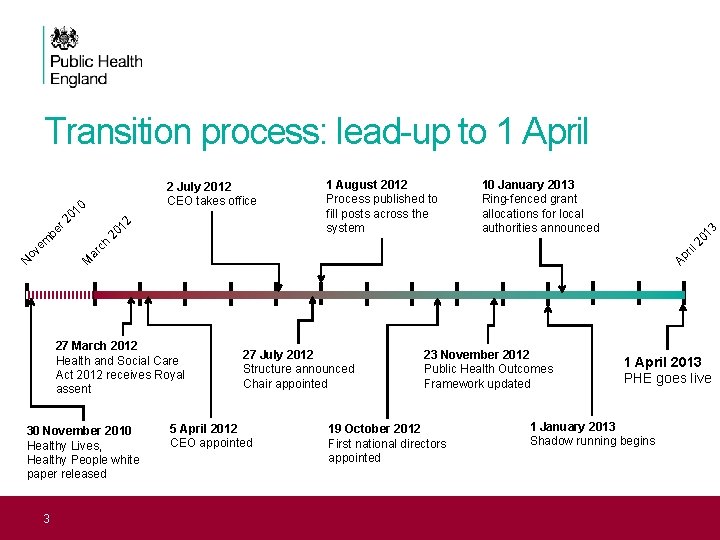
Transition process: lead-up to 1 April 13 10 January 2013 Ring-fenced grant allocations for local authorities announced ril ch 20 1 August 2012 Process published to fill posts across the system N M Ap ar ov em 20 be 12 r 2 01 0 2 July 2012 CEO takes office 27 March 2012 Health and Social Care Act 2012 receives Royal assent 30 November 2010 Healthy Lives, Healthy People white paper released 3 27 July 2012 Structure announced Chair appointed 5 April 2012 CEO appointed 23 November 2012 Public Health Outcomes Framework updated 19 October 2012 First national directors appointed 1 April 2013 PHE goes live 1 January 2013 Shadow running begins

Our priorities for 2013/14 – Sets out Public Health England’s priorities and actions for the first year of our existence – Five outcome-focused priorities – what we want to achieve – Two supporting priorities – how we will achieve it – 27 key actions to take now – The start of the conversation – a three-year corporate plan will follow 4 Prese

Mission “To protect and improve the nation’s health and to address inequalities, working with national and local government, the NHS, industry, academia, the public and the voluntary and community sector. ” 5

What we do Public Health England: – works transparently, proactively providing government, local government, the NHS, MPs, industry, public health professionals and the public with evidencebased professional, scientific and delivery expertise and advice – ensures there are effective arrangements in place nationally and locally for preparing, planning and responding to health protection concerns and emergencies, including the future impact of climate change – supports local authorities, and through them clinical commissioning groups, by providing evidence and knowledge on local health needs, alongside practical and professional advice on what to do to improve health, and by taking action nationally where it makes sense to do so 6
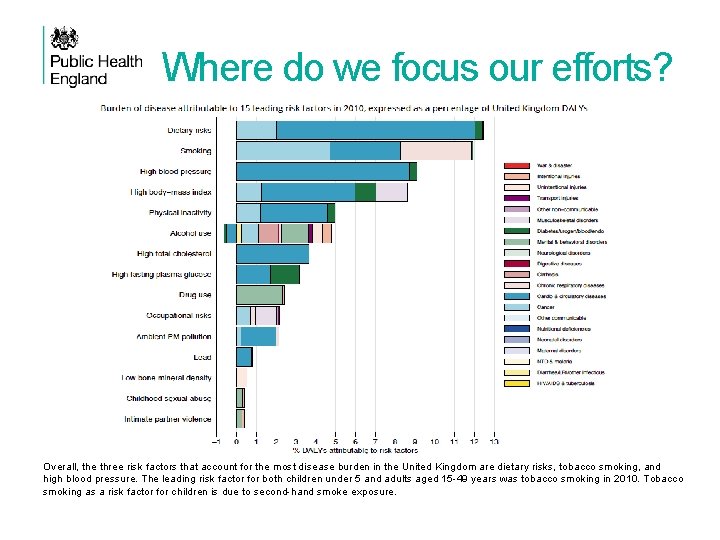
Where do we focus our efforts? Overall, the three risk factors that account for the most disease burden in the United Kingdom are dietary risks, tobacco smoking, and high blood pressure. The leading risk factor for both children under 5 and adults aged 15 -49 years was tobacco smoking in 2010. Tobacco smoking as a risk factor for children is due to second-hand smoke exposure.

Where do we focus our efforts?

Outcome-focused priorities 9 1. Helping people to live longer and more healthy lives by reducing preventable deaths and the burden of ill health associated with smoking, high blood pressure, obesity, poor diet, poor mental health, insufficient exercise, and alcohol 2. Reducing the burden of disease and disability in life by focusing on preventing and recovering from the conditions with the greatest impact, including dementia, anxiety, depression and drug dependency 3. Protecting the country from infectious diseases and environmental hazards, including the growing problem of infections that resist treatment with antibiotics 4. Supporting families to give children and young people the best start in life, through working with health visiting and school nursing, family nurse partnerships and the Troubled Families programme 5. Improving health in the workplace by encouraging employers to support their staff, and those moving into and out of the workforce, to lead healthier lives

Supporting priorities 10 6. Promoting the development of place-based public health systems 7. Developing our own capacity and capability to provide professional, scientific and delivery expertise to our partners

Actions 2013/14 1. Reducing preventable deaths • Support people to live healthier lives by implementing NHS Healthchecks • Accelerate efforts to promote tobacco control and reduce the prevalence of smoking • Report on premature mortality and the Public Health Outcomes Framework • Enable improved integration of care, to support local innovations to find alternatives to hospital-based care 11
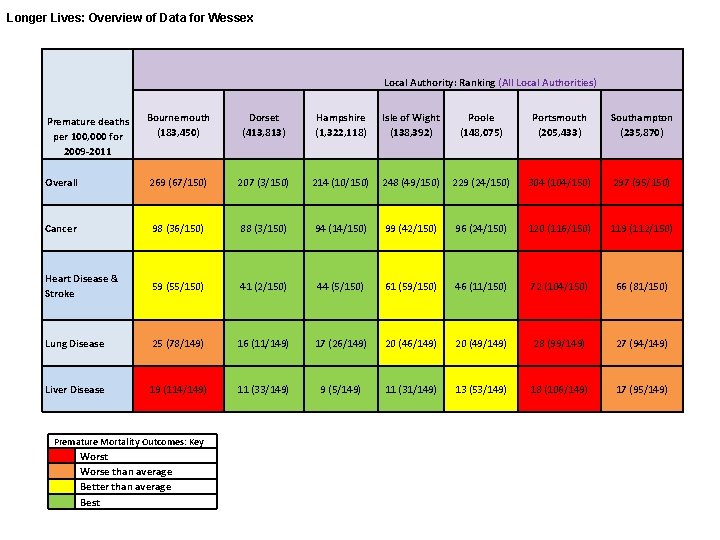
Longer Lives: Overview of Data for Wessex Local Authority: Ranking (All Local Authorities) Premature deaths per 100, 000 for 2009 -2011 Bournemouth (183, 450) Dorset (413, 813) Hampshire (1, 322, 118) Isle of Wight (138, 392) Poole (148, 075) Portsmouth (205, 433) Southampton (235, 870) Overall 269 (67/150) 207 (3/150) 214 (10/150) 248 (49/150) 229 (24/150) 304 (104/150) 297 (95/150) Cancer 98 (36/150) 88 (3/150) 94 (14/150) 99 (42/150) 96 (24/150) 120 (116/150) 119 (112/150) Heart Disease & Stroke 59 (55/150) 41 (2/150) 44 (5/150) 61 (59/150) 46 (11/150) 72 (104/150) 66 (81/150) Lung Disease 25 (78/149) 16 (11/149) 17 (26/149) 20 (49/149) 28 (99/149) 27 (94/149) Liver Disease 19 (114/149) 11 (33/149) 9 (5/149) 11 (31/149) 13 (53/149) 18 (106/149) 17 (95/149) Premature Mortality Outcomes: Key Worst Worse than average Better than average Best
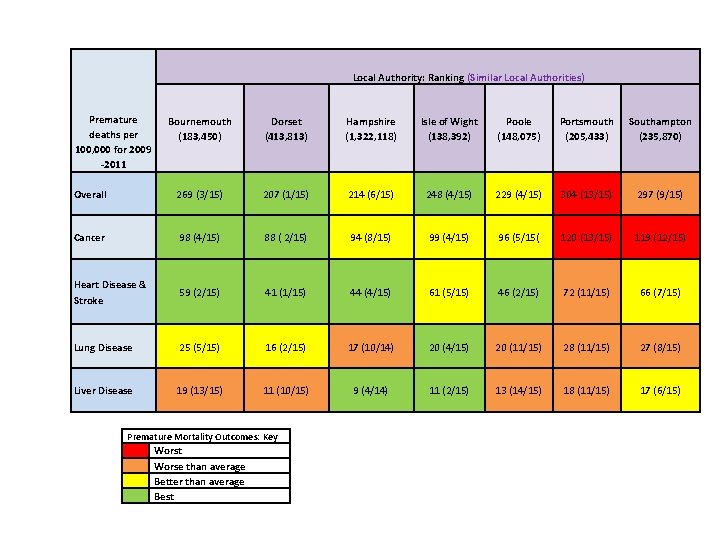
Local Authority: Ranking (Similar Local Authorities) Premature deaths per 100, 000 for 2009 -2011 Bournemouth (183, 450) Dorset (413, 813) Hampshire (1, 322, 118) Isle of Wight (138, 392) Poole (148, 075) Portsmouth (205, 433) Southampton (235, 870) Overall 269 (3/15) 207 (1/15) 214 (6/15) 248 (4/15) 229 (4/15) 304 (13/15) 297 (9/15) Cancer 98 (4/15) 88 ( 2/15) 94 (8/15) 99 (4/15) 96 (5/15( 120 (13/15) 119 (12/15) Heart Disease & Stroke 59 (2/15) 41 (1/15) 44 (4/15) 61 (5/15) 46 (2/15) 72 (11/15) 66 (7/15) Lung Disease 25 (5/15) 16 (2/15) 17 (10/14) 20 (4/15) 20 (11/15) 28 (11/15) 27 (8/15) Liver Disease 19 (13/15) 11 (10/15) 9 (4/14) 11 (2/15) 13 (14/15) 18 (11/15) 17 (6/15) Premature Mortality Outcomes: Key Worst Worse than average Better than average Best

Actions 2013/14 3. Protecting the country’s health • Reverse the current trends so that we reduce the rates of tuberculosis infections • Lead the gold standards for current vaccination and screening programmes • Tackle antimicrobial resistance (AMR) • Develop and implement a national surveillance strategy 14

Actions 2013/14 6. Promoting place-based public health systems • Make the business case for promoting wellbeing, prevention and early intervention as the best approaches to improving health and wellbeing • Partner NHS England to maximise the NHS’ impact on improving the public’s health • Implement the public health workforce strategy and develop the PHE workforce • Ensure that we use data and information across the public health system to demonstrate value for money 15
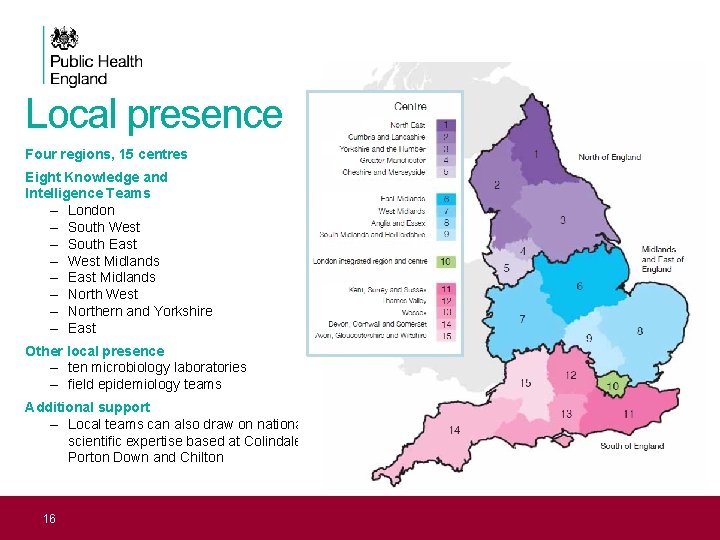
Local presence Four regions, 15 centres Eight Knowledge and Intelligence Teams – London – South West – South East – West Midlands – East Midlands – North West – Northern and Yorkshire – East Other local presence – ten microbiology laboratories – field epidemiology teams Additional support – Local teams can also draw on national scientific expertise based at Colindale, Porton Down and Chilton 16

Local focus 15 CENTRES – Led by a senior public health professional – Deliver services and advice around the three domains of public health – Ensure quality and consistency and responsiveness of centres’ services and advice – Support local government and local NHS action to improve and protect health and reduce inequalities with intelligence and evidence – Support transparency and accountability of the system – Assurance of emergency planning and response Deliver the local input to emergency preparedness, resilience and response – Workforce development – Contribute to the national public health agenda – 17 4 REGIONS

Public health outcomes framework To improve and protect the nation’s health and wellbeing and improve the health of the poorest, fastest Outcome 1) Increased healthy life expectancy – taking into account health quality as well as length of life 1 Improving the wider determinants of health 2 Health improvement Outcome 2) Reduced differences in life expectancy between communities (through greater improvements in more disadvantaged communities) 3 Health protection 4 Healthcare and public health preventing premature mortality 19 indicators, including: 24 indicators, including: 7 indicators, including: 16 indicators, including: • Children in poverty • People with mental illness or disability in settled accommodation • Sickness absence rate • Statutory homelessness • Fuel poverty • Excess weight • Smoking prevalence • Alcohol-related admissions to hospital • Cancer screening coverage • Recorded diabetes • Self-reported wellbeing • Air pollution • Population vaccination coverage • People presenting with HIV at a late stage of infection • Treatment completion for tuberculosis • Infant mortality • Mortality from causes considered preventable • Mortality from cancer • Suicide • Preventable sight loss • Excess winter deaths 18
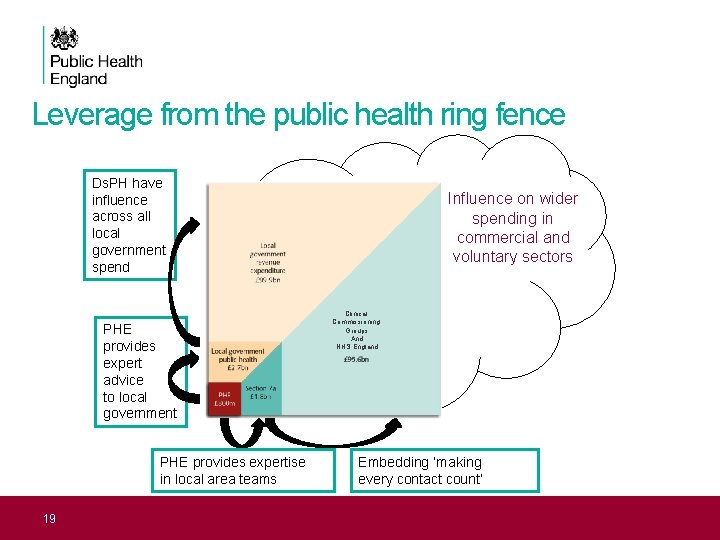
Leverage from the public health ring fence Ds. PH have influence across all local government spend PHE provides expert advice to local government PHE provides expertise in local area teams 19 Influence on wider spending in commercial and voluntary sectors Clinical Commissioning Groups And NHS England Embedding ‘making every contact count’
- Slides: 19