Welcome to Seminar on Nutrition Assessment and Management









- Slides: 15

Welcome to Seminar on Nutrition Assessment and Management in Family Medicine Part-2 Meera Kaur, Ph. D, RD Assistant Professor, Family Medicine kaur@cc. umanitoba. ca

Biochemical Assessment • Blood and Urine analyses • Diagnostics and imaging 16

Review of Systems • General: appetite changes; weight loss/gain; clothes tighter/loser – weakness, fatigue, fever, chills, night sweats, – changes in sleep, daytime sleepiness – edema and/or abdominal swelling • Skin: appearance of a rash, dry skin – breaking nails, hair loss, changes in texture of hair • Neurological – confusion, memory loss, difficulty with night vision – gait change, loss of position sense, numbness, paresthesia • GI symptoms/alimentary: abdominal pain, nausea, vomiting – bowel changes- diarrhea, constipation – difficulty/pain swallowing, early satiety, indigestion, heartburn – mouth lesions- ulcers, tooth decay; sore tongue, gums 17

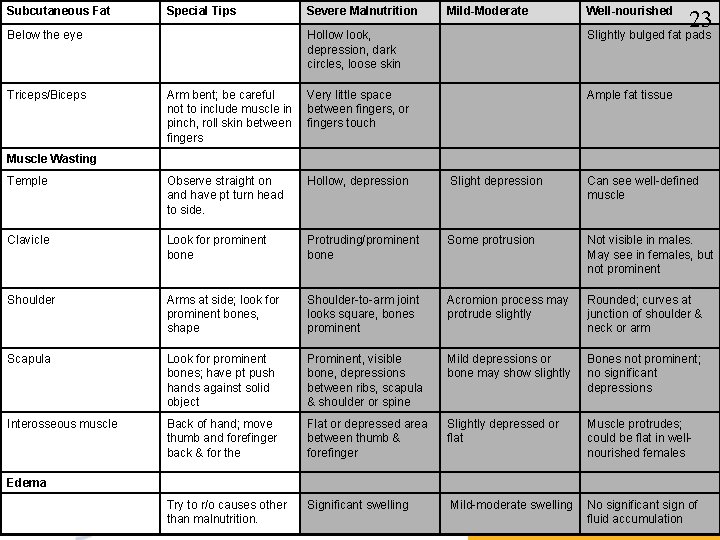
Physical Exam and Observation. Subjective Global Assessment • Assesses nutritional status based on features of the hx and physical examination. • Can easily be taught to clinicians. • Technique is reproducible – Good correlation between subjective and objective measurements. 21

nical , Subjective Global Assessment (SGA) of Nutritional Status Subjective Global Assessment (SGA) is a: status based on features of the history and physical examination a method of rating a patient's nutritional status, with subjective observations being given values on an ordinal scale. Factors assessed include weight change, appetite or anorexia, subcutaneous tissue and muscle, and GI symptoms (Mosby's Medical Dictionary, 8 th edition. © 2009, Elsevier). 22

Subcutaneous Fat Special Tips Below the eye Severe Malnutrition Mild-Moderate Well-nourished 23 Hollow look, depression, dark circles, loose skin Slightly bulged fat pads Arm bent; be careful not to include muscle in pinch, roll skin between fingers Very little space between fingers, or fingers touch Ample fat tissue Temple Observe straight on and have pt turn head to side. Hollow, depression Slight depression Can see well-defined muscle Clavicle Look for prominent bone Protruding/prominent bone Some protrusion Not visible in males. May see in females, but not prominent Shoulder Arms at side; look for prominent bones, shape Shoulder-to-arm joint looks square, bones prominent Acromion process may protrude slightly Rounded; curves at junction of shoulder & neck or arm Scapula Look for prominent bones; have pt push hands against solid object Prominent, visible bone, depressions between ribs, scapula & shoulder or spine Mild depressions or bone may show slightly Bones not prominent; no significant depressions Interosseous muscle Back of hand; move thumb and forefinger back & for the Flat or depressed area between thumb & forefinger Slightly depressed or flat Muscle protrudes; could be flat in wellnourished females Try to r/o causes other than malnutrition. Significant swelling Mild-moderate swelling No significant sign of fluid accumulation Triceps/Biceps Muscle Wasting Edema

Deficiency Symptoms (Fe)… • YYY 21

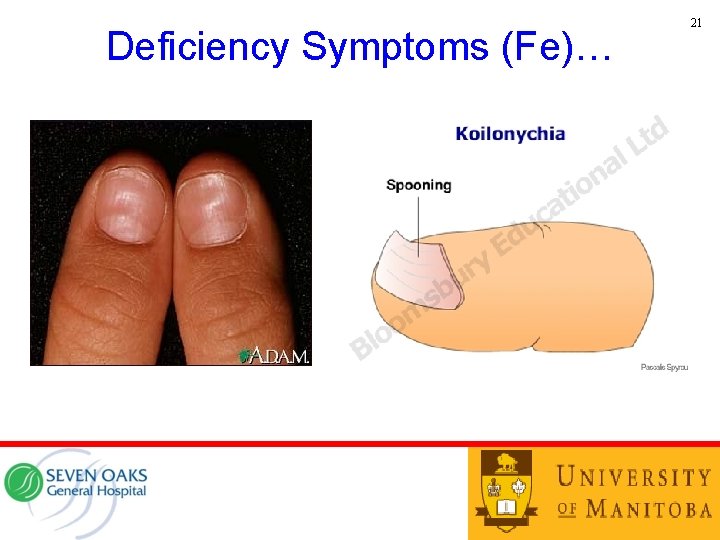
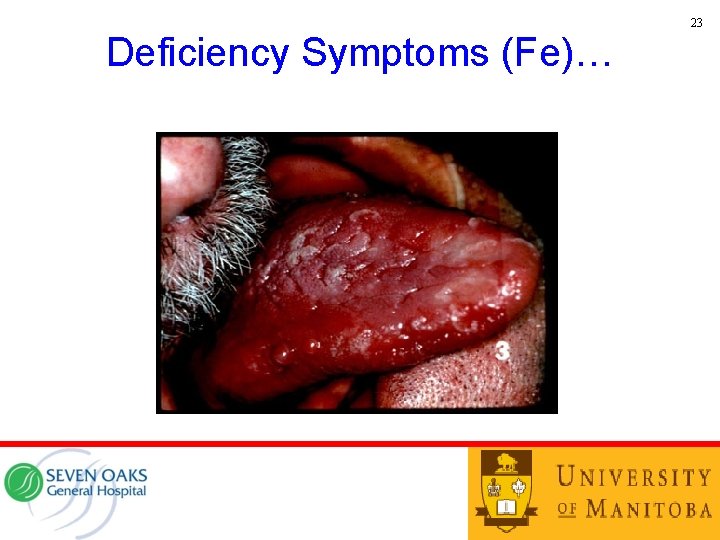
23 Deficiency Symptoms (Fe)…

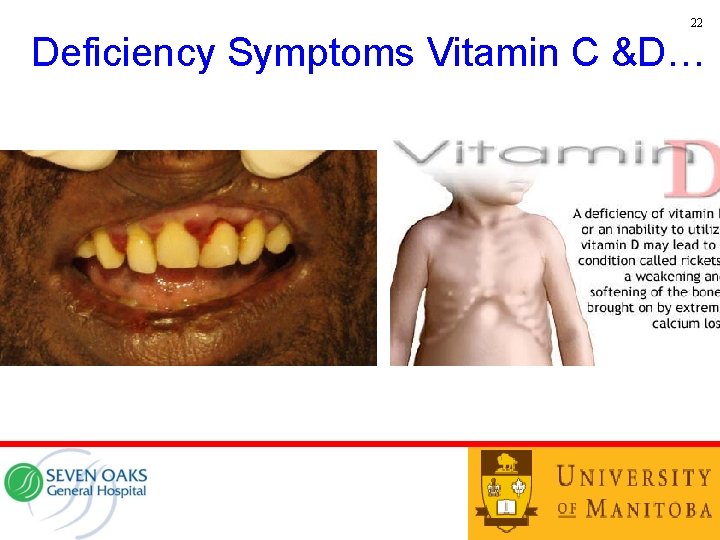
22 Deficiency Symptoms Vitamin C &D…

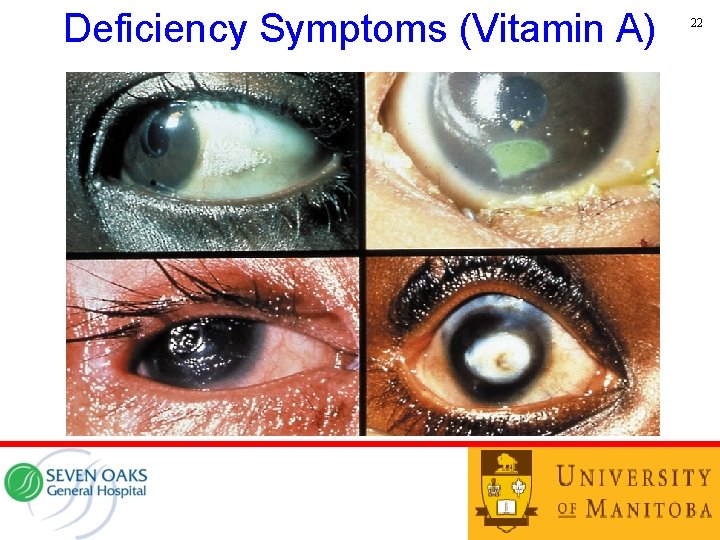
Deficiency Symptoms (Vitamin A) 22

Physical Examination in Infants, Children, and Adolescents • Determination of height, weight, and head circumference and plotting on pediatric growth charts. (www. cdc. gov/growthcharts for new growth charts) • Evaluation of growth and development over time. • 5 th to 95 th%ile is normal. • Crossing percentiles is abnormal. Dietary intake should be assessed. 24

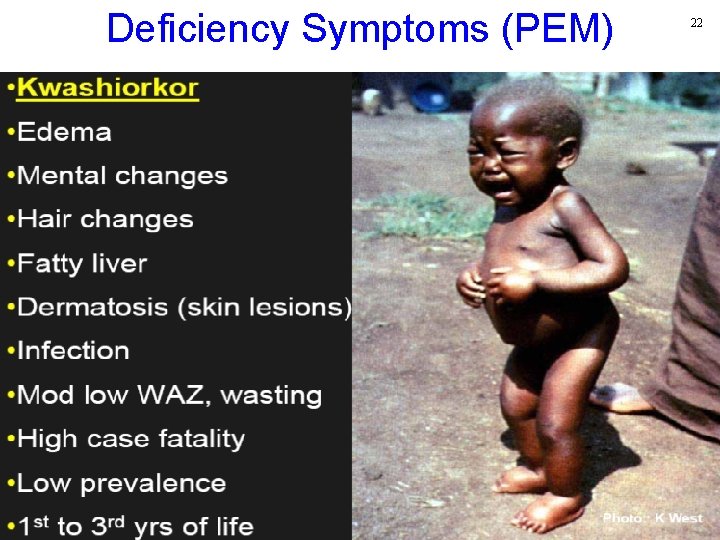
Deficiency Symptoms (PEM)… 21

Deficiency Symptoms (PEM) 22

Deficiency Symptoms (Fe) 22

Clinical Evaluation • Anemia: Hgb, Hct, MCV, TIBC, folate, vitamin B 12 • Malnutrition: serum proteins, nitrogen balance • CVD: cholesterol, lipoproteins, triglycerides • Diabetes: glucose, Hgb. A 1 C • Renal: BUN, creatinine, electrolytes • Pancreatitis: triglycerides • Malabsorption: fecal fat, hydrogen breath test • Alcoholism: thiamin, folate, B 12 25