Welcome to Nursing Professional Development Learning Objectives 1

Welcome to Nursing Professional Development

Learning Objectives 1. Discuss the impact of the ANA Standards of Practice, Standards of Professional Performance, and Code of Ethics on the professional performance of the Registered Nurse. 2. Describe components of the California Nurse Practice Act as it applies to the Scope of Practice for Registered Nurses. 3. Apply the California Nurse Practice Act, ANA Standards of Practice, Standards of Professional Performance, and Code of Ethics to case studies. 4. Describe the relationship of Community Medical Center’s Nursing Philosophy to the ANA Standards and the California Nurse Practice Act. 2

Nursing Leadership at Community Population health Working more efficiently Doing what is best for the patient Engaging the family Evidence-based care across the continuum Strategizing a discharge plan upon admission to provide care after the hospital 3

CMC Mission To improve the health status of the community. To promote medical education. 4

CMC Vision To serve the community as the provider, practice location, and employer of choice – establishing Community Medical Centers as a leader in clinical excellence, technological innovation, quality service, superb facilities and compassionate care. 5

Vision of Nursing at CMC To be recognized as the leader in Professional Nursing Practice, providing care in a patient-family centered environment that surpasses the expectations of everyone we serve. 6

CMC Nursing Philosophy As we provided care, we value: Safety Effectiveness Patient-Centeredness Timeliness Efficiency Equitability 7
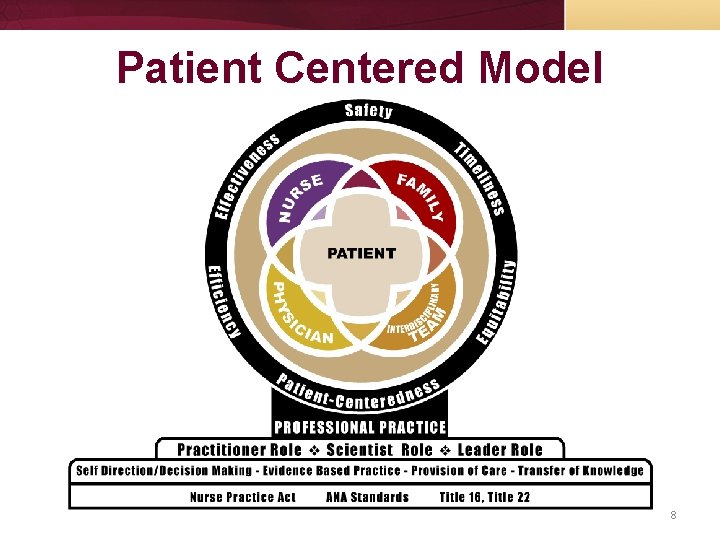
Patient Centered Model 8

Community Medical Center • The value of nursing at CMC • Nursing’s contribution to the successful outcomes at CMC • How do we measure these successful outcomes? 9

Professionalism What is a “profession”? What distinguishes someone as a “professional”? Consider the knowledge, skills, attitudes, and character traits… What is specific to NURSING? 10

From the CA Nurse Practice Act • Scientific base of knowledge • Clinical skills and training • Use of a scientific process for decision-making • Ethical practice 11

Critique the Professionalism 12

Professional Role Clarity and Competency Professional Guidelines: • ANA Standards of Practice • ANA Standards of Professional Performance • ANA Code of Ethics Legal Requirements: • California Nurse Practice Act (2725) • Title 16—Standards of Competent Performance • Title 22 § 70215—Code of Regulations (Title 22) Regulating Bodies: • CA Board of Registered Nurses • CA Department of Public Health (CDPH) • Centers for Medicare/Medicaid Services (CMS) • Joint Commission Profession Licensure Regulators 13

ANA Standards of Practice • Critical thinking model Nursing Process • Significant actions that guide our decisionmaking • Notice 5 a and 5 b • Coordination of care being delivered • Teaching to promote health and a safe environment 14

ANA Standards of Professional Performance • Behaviors and activities of a professional nurse • New Standards: • • #8: Culturally congruent practice #9: Communicating in all areas of practice #13: Integration of EBP and Research #17: Environmentally safe and healthy practice 15

ANA Code of Ethics • 9 Provisions • Respect for the person is the core principle, but not the sole obligation: • Knowledge of clinical situation • Knowledge of people involved • Knowledge of patient’s values and desires 16

Click the star for a 10 minute break.

CA Nurse Practice Act: Chapter 6, Section 2725 Nursing is defined as: Ø Dynamic field of work Ø Science is continually evolving Ø Sophisticated patient care activities Ø Practice in any setting 18

CA Nurse Practice Act: Goal of Practice The goal of nursing is to help people cope with difficulties in daily living associated with their health and illness problems. 19

CA Nurse Practice Act: Responsibilities Powerful Decision Authority: Use substantial amount of scientific knowledge and technical skill to: ü Observe ü Determine abnormalities ü Determine and implement plans of action 20
Scope of Practice Dependent Independent Inter. Dependent 21
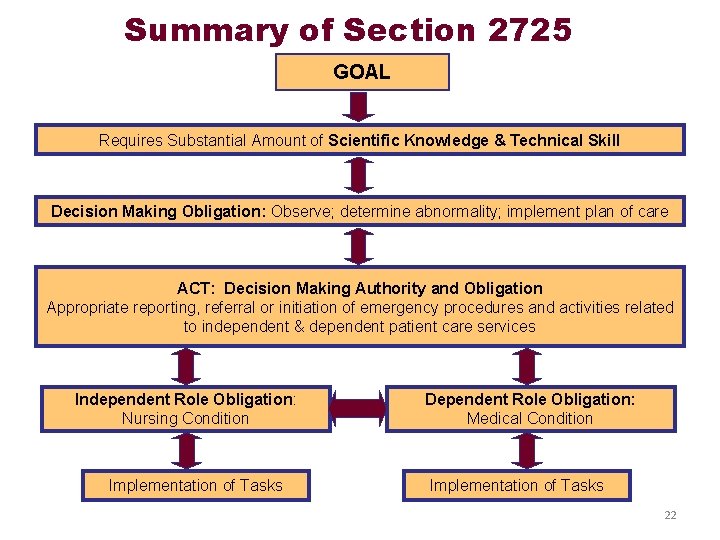
Summary of Section 2725 GOAL Requires Substantial Amount of Scientific Knowledge & Technical Skill Decision Making Obligation: Observe; determine abnormality; implement plan of care ACT: Decision Making Authority and Obligation Appropriate reporting, referral or initiation of emergency procedures and activities related to independent & dependent patient care services Independent Role Obligation: Nursing Condition Implementation of Tasks Dependent Role Obligation: Medical Condition Implementation of Tasks 22

CCR: Title 16 • Incompetent vs. Competent Performance • Nursing process • Delegation to subordinates • Patient advocacy • Patient education 23

CA ADC: Title 22 § 70215 Planning and Implementation of Patient Care: • Nursing Process • Documentation and communication of assessment findings • Delegation • Patient Education • Collaboration with patient and interprofessional team • Patient advocacy 24

5 Rights of Delegation Right Task Right Circumstances Right Person Right Directions & Communication Right Supervision & Evaluation 25

Role-Based Patient Care Skills List • CA Nurse Practice Act is non-prescriptive • Role-based skill assignment is determined by facility in collaboration with BRN • Refer to policy #11979—Role-Based Patient Care by Scope of Practice 26

Group Discussions • Your group will be provided a scenario of a nurse whose license has been suspended or revoked. • Discuss how various aspects of the supporting documents have been violated. • Be prepared to present your group’s comments to the class. 27

Click the star for a 10 minute break.

The following is a true story. This sentinel event happened within Community Medical Centers.

Case Study • Mrs. S is a 75 y. o. admitted to the ED with c/o of respiratory distress, tachypnea, SOB and tachycardia. • Sp. O 2 of 90% on 5 L/min of O 2 • Using accessory muscles, speaking 2 -3 word sentences, inspiratory wheezing with circumoral cyanosis 30

Case Study • History of vocal cord cancer, COPD, CHF, atrial fib. , heart valve replacement due to CAD, and pacemaker implantation. • Admitted to med/surg with remote telemetry for atrial fib. with RVR, pneumonia and CHF • Vital Signs: HR 82, RR 26, BP 140/64, Sp. O 2 93% on 6 L/min O 2 via NC 31

Case Study • Day 2 of admission: The on-call physician orders Coumadin 5 mg PO q. HS for on-going atrial fib. • Hospitalist physician returns on Monday • Unclear what handoff occurred between the physicians 32

Case Study • Day 4 of admission: Dietician charted that Coumadin education was provided • Pharmacist made note re: alert for drug interaction and the need for labs • Pt receiving Amiodarone, Levaquin, and Coumadin Does this change the RN’s plan? 33

Case Study • Day 7 of admission: RN notes petechia on pt’s arms at 1930 h • MAR noted pt receiving Coumadin at 2100 h • MD called at 1945 h for an order for PT/INR • Critical results: PT=167. 1 and INR > 20 What should the nurse’s next action include? 34

Case Study • RN notified the physician of lab values at 2045 h • New orders: Vitamin K 10 mg IM; hold Coumadin; and CBC in AM Is this appropriate care? What is best for the patient? What should the nurse do? 35

Case Study • During night shift pt developed smear of blood in bowel movement, a nosebleed, headache, and pain level of 5/10 Should the nurse be concerned? What should the nurse do? 36

Case Study • Second call was placed to the MD at 0615 h, and an order was obtained for a PT/INR. • New labs: PT=148. 7 and INR=20 What should the nurse discuss during shift change? 37

Case Study • 0900 h patient was unresponsive and the Rapid Response Team was called • Transferred to Progressive Care Unit • 2 units PRBCs and FFP were transfused • Pt developed respiratory insufficiency, transferred to ICU and was intubated 38

Case Study • CT scan results: large parenchymal hemorrhage with extensive mass effect and transverse herniation • Pt was removed from life support and allowed to die with family by her side. What could have been done to prevent this situation? 39

Calling the Physician Urgent, emergent, or unstable situations: • Wait no longer than five minutes in between attempts • No physician contact after the third attempt? 1. Activate chain of command procedures. 2. Call Rapid Response Team or Code Blue as appropriate. 40

Using SBAR 41

Chain of Command Policy #11895 • Patient Concern • Nurse / Physician: • Private physician • Residency program • Regular business hours • After hours

5 -P Systematic and comprehensive delivery of Hand-off: information when reporting to the next • Covers patient identifiers caregiver. • Name, age, gender, room number, MRN, language, weight, problem Patient list, code status Precaution • Covers what is expected to be different or unusual about this patient • Isolation, fall risk, allergies, cultural/spiritual needs, diet, abuse, sitters, hearing/cognitive problems Problem • Covers things that are different or unusual about this pt or condition • Unusual V/S, I&Os, labs, EKG, x-rays, case management, stability Plan Purpose • Covers the patient’s diagnosis, treatment plan, and next steps • Active orders, pending procedures/tests, medications, IVs • Covers the rationale for the plan of care • MRSA, immunizations, discharge planning, care plan, summary of goals, patient education status
- Slides: 43