Welcome to Helping Facilities Prevent Illness Absenteeism Presenter

Welcome to Helping Facilities Prevent Illness & Absenteeism Presenter: Lori Strazdas, MPH, Public Health Liaison, Clorox Healthcare

Speaker Overview Lori Strazdas, MPH Public Health Liaison, Clorox Healthcare • Lori Strazdas, MPH is a Public Health Liaison with Clorox Healthcare. • In her 12 years at Clorox, Lori has held various positions within R&D, supporting both the consumer and professional product portfolios. Her experience includes ensuring end-user product safety and regulatory compliance for EPA, FDA and CPSC regulated products, managing Clorox Healthcare sponsored epidemiological studies and providing thought-leadership for educational materials. • Prior to joining Clorox, Lori worked for the Pima County Health Department as a Communicable Disease Investigator and Epidemiologist, as well as in various clinical settings. • Lori received both her Bachelor’s in Environmental Science and Master’s in Public Health Epidemiology from the University of Arizona. She was subsequently awarded a Fulbright Scholarship to Lithuania, where she studied risk factors for stomach cancer, including the bacteria Helicobacter pilori. • She is currently a member of the American Public Health Association and Association for Professionals in Infection Control & Epidemiology.

Learning Objectives ü Learn about common infections that can spread in facilities and their impact on absenteeism and public health. ü Understand the difference between cleaning, sanitizing and disinfecting. ü Learn about new technologies and best practices to help prevent the spread of infections.

Agenda 1. Facility maintenance & infection prevention: why it matters 2. Common infections 3. The role of the environment 4. Breaking the chain of transmission: product selection, new technology and best practices 5. Conclusion & questions

Facility Maintenance & Infection Prevention WHY IT MATTERS

Why it Matters Germs that cause infectious diseases are common. They can spread in public spaces and cause: Illnesses and outbreaks • Reputational damage • Lost revenue due to facility closures, absenteeism and lost productive time • http: //www. cdc. gov/oid/docs/ID-Framework. pdf

Why it Matters Today, illness and infection have larger impacts than ever before. Infections can strike where you work, learn and play. $1, 685/employee – Average annual cost of illness to employers. http: //journals. lww. com/joem/Abstract/2003/12000/ Lost_Productive_Work_Time_Costs_From_Health. 4. aspx $400, 000 – Cost to a major university to combat a Norovirus outbreak. http: //www. issa. com/trade-shows/certification-standards/ issa-clean-standards/clean-standard-k-12/how-dirty-isyour-childsschool- infographic. html#. WCESGS 0 r. KM $14, 000 – Direct cost of hospitalization alone due to a MRSA infection. http: //www. hcup-us. ahrq. gov/reports/statbriefs/sb 35. jsp

Health Impact Norovirus leads to 1. 7 -1. 9 million outpatient visits, 56, 000 -71, 000 hospitalizations, 570 -800 deaths each year 5 -20% of Americans get the flu annually resulting in 200, 000 hospitalizations and 3, 000 -49, 000 flu-associated deaths ~1 in 6 Americans get sick, 128, 000 are hospitalized, and 3, 000 die of foodborne diseases each year https: //www. cdc. gov/foodborneburden/estimates-overview. html. http: //www. cdc. gov/flu/about/disease/us_flu-related_deaths. htm http: //www. cdc. gov/norovirus/trends-outbreaks. html

Financial Impact Roughly 60 million days of school and 50 million days of work lost because of common cold every year Flu causes ~44 million lost days of productivity, costs the U. S. more than $87 billion each year Health-related “lost productive time” costs employers $225. 8 billion per year http: //www. cleaninginstitute. org/clean_living/cleaning_for_health_some_facts. aspx. http: //www. cdc. gov/flu/about/qa/disease. htm. http: //www. cdcfoundation. org/businesspulse/flu-prevention. Walter SF et al. Journal of Occupational & Environmental Medicine. 45. 12 (2003): 1234 -1246.
Common Infections Common Colds Millions of cases in the U. S. each year: • 70 million work days missed by non-parents • 189 million school days missed by kids • 129 million work days missed by parents Economic impact of common colds costs Americans more than $40 billion annually: • $17 billion direct costs • $23 billion indirect costs http: //www. ur. umich. edu/0203/Mar 10_03/15. shtml http: //www. cdc. gov/Features/Rhinoviruses/index. html Fendrick MF et al. Arch Intern Med. 2003

Common Infections Influenza or “Flu” Cause of seasonal epidemics of disease almost every winter in the U. S. • Impacts ~ 5 -20% of Americans annually • More than 200, 000 hospitalized per year • Severity can vary widely Epidemics cost the U. S. economy $71$167 billion per year Costs parents of influenza-stricken children: • 11 -73 hours of missed work • $300 -$4, 000 in medical expenses Seasonal Influenza (Flu): CDC Study: Treating children’s flu illness costly. CDC, 21 May 2012. CDC - Seasonal Influenza (Flu) - Q & A: Preventing Seasonal Flu. Centers for Disease Control and Prevention, 1 Aug. 2013. http: //www. cdc. gov/flu/about/qa/disease. htm. Influenza. World Health Organization, Mar. 2003. Web. 10 Oct. 2016.

Common Infections Norovirus & Foodborne Illness Norovirus, sometimes called “stomach flu, ” is highly contagious • Leading cause of foodborne illness in the U. S. • Per year in the U. S. , results in: • ~800 deaths • 71, 000 hospitalizations • 19 -21 million total illnesses • ~$1. 4 billion in healthcare costs • ~$23. 5 billion in societal costs Foodborne illness is a major problem with significant impact on schools and businesses • Roughly 48 million get sick, 128, 000 are hospitalized, 3, 000 die each year Hall, A. "Norovirus disease in the United States. " Emerging Infectious Diseases. 19. 8 (2013). http: //www. jhsph. edu/news-releases/2016/the-high-cost-of-norovirus-worldwide. html http: //www. cdc. gov/foodsafety/foodborne-germs. html

Common Infections S. aureus & MRSA S. aureus, or “staph, ” is commonly carried on the skin or in the nose of healthy people MRSA is a type of S. aureus bacteria that is resistant to antibiotics • Risk is increased in activities or places that involve crowding, skin-to-skin contact, and shared equipment or supplies • Contaminated surfaces and lack of cleanliness make it easier to spread https: //www. cdc. gov/mrsa/community/index. html http: //www. cdc. gov/niosh/topics/mrsa/

Cleaning and Disinfection Why is it so important? The Role of the Environment
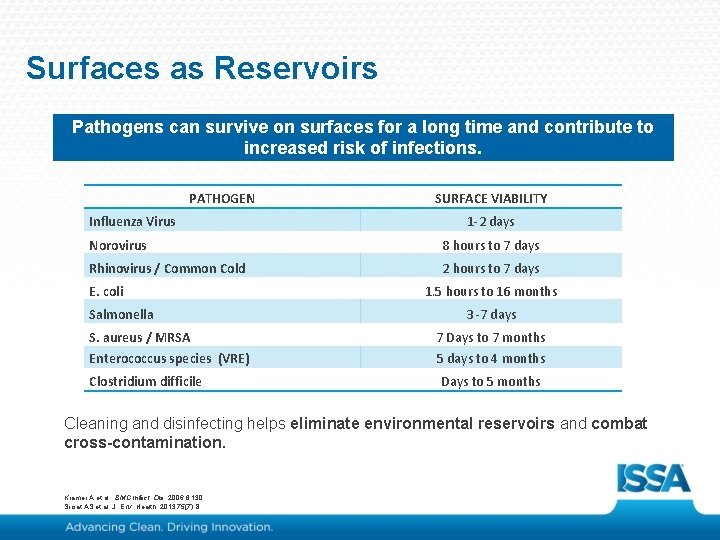
Surfaces as Reservoirs Pathogens can survive on surfaces for a long time and contribute to increased risk of infections. PATHOGEN Influenza Virus SURFACE VIABILITY 1 -2 days Norovirus 8 hours to 7 days Rhinovirus / Common Cold 2 hours to 7 days E. coli Salmonella 1. 5 hours to 16 months 3 -7 days S. aureus / MRSA 7 Days to 7 months Enterococcus species (VRE) 5 days to 4 months Clostridium difficile Days to 5 months Cleaning and disinfecting helps eliminate environmental reservoirs and combat cross-contamination. Kramer A et al. BMC Infect. Dis. 2006; 6: 130. Sirsat AS et al. J. Env. Health; 2013; 75(7): 8.
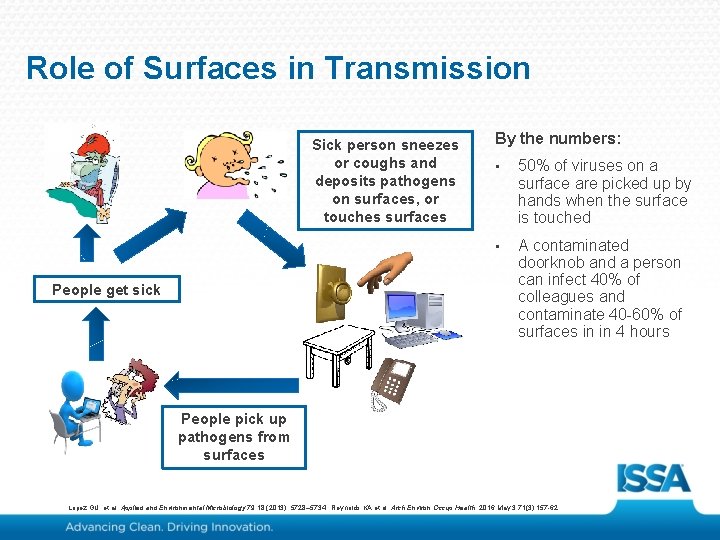
Role of Surfaces in Transmission Sick person sneezes or coughs and deposits pathogens on surfaces, or touches surfaces People get sick By the numbers: • 50% of viruses on a surface are picked up by hands when the surface is touched • A contaminated doorknob and a person can infect 40% of colleagues and contaminate 40 -60% of surfaces in in 4 hours People pick up pathogens from surfaces Lopez GU. et al. Applied and Environmental Microbiology 79. 18 (2013): 5728– 5734. Reynolds KA et al. Arch Environ Occup Health. 2016 May 3; 71(3): 157 -62.

Breaking the Chain of Transmission Product selection, new technology and best practices for preventing illness and absenteeism

Selecting the Right Products What’s the Difference? Cleaning Sanitization Disinfection • Manual or mechanical removal of organic and inorganic soil and debris from surfaces and equipment • Reduction of bacterial contaminants to safe levels as judged by public health requirements • Destruction of pathogenic and other types of microorganisms, most often accomplished using chemical agents Sterilization • Validated process used to render a product free of all forms of viable microorganisms Product label may contain the following information: • Cleaner • Detergent • • EPA registration number Non-food contact sanitizer “Kills 99. 9% of germs” Food-contact sanitizer • • EPA registration number Disinfectant Cleaner Disinfectant “Kills 99. 999% of germs” • Sterilant • FDA regulated *Adapted from Rutala WA, Weber DJ; Healthcare Infection Control Practices Advisory Committee. Guideline for Disinfection and Sterilization in Healthcare Facilities, 2008.

Selecting the Right Product Kill Claims Does it kill the most prevalent pathogens? • Select the product that is EPA-registered to kill the most prevalent pathogens Kill Time How quickly does it kill prevalent pathogens? • Select the product with fastest kill times (contact times) to ensure the product can disinfect quickly Wet Time Are the kill times less than or equal to its wet time? • Select the product that can keep surfaces visibly wet for the longest kill time (contact time) on its label Other Do its other attributes meet your facility’s needs? • Select the product that is easy to use, which will help your staff achieve compliant usage and keep themselves, building occupants and patrons safe Rutala & Weber. Selection of the ideal disinfectant. Infect. Control Hosp. Epidemiol. 2014, 35 (7), 855– 865.

Selecting the Right Products Ready-to-use products can improve overall efficiency: • • • No mixing necessary Standardized dilution Reduced user error • Pre-saturated wipes: • One-step cleaning and disinfection • Minimize cross-contamination • Many sizes available Surface Compatibility • • Disinfectants should be tough on germs, not surfaces and equipment Don’t compromise between efficacy and surface compatibility – look for products that offer both Saito, R et al. American Journal of Industrial Medicine 58. 1 (2015): 101– 111.

New Technology Electrostatic technology enables superior coverage of trusted solutions

Electrostatic Spray Technology was created in the 1930 s to improve spray deposition • In the 1940 s, the automobile industry implemented the technology for paint coating • In the 1980 s, the agricultural industry started using sprayers to help reduce pesticidal drift

Electrostatic Spraying is a System …. . Not just a Device

Clorox® Total 360® System Combines electrostatic technology with trusted Clorox® products to quickly and easily provide superior coverage of surfaces even outside line-of-sight. Electrostatic sprayer: • Delivery system for superior coverage • Force stronger than gravity attracts solutions to surfaces Disinfecting & sanitizing solutions: • Clorox® Total 360™ Disinfectant Cleaner 4 • Clorox® Anywhere® Hard Surface Sanitizing Spray

Clorox® Total 360® System The Clorox® Total 360® System helps keep facilities healthier while also saving time, money and labor * Compared with a trigger spray • Saves time: Works up to 4 x faster* • Saves labor: Covers up to 18, 000 ft 2/hour • Saves money: Uses up to 65% less solution*

Clorox® Total 360® System How it works: o Electrostatic technology enables superior coverage of Clorox® trusted solutions in hard to reach places —the side, underside, and backside of surfaces.

Clorox® Total 360® System Device and Solution Designed and tested as a system against three critical criteria: Micro-efficacy & Performance Residue Micro-efficacy • Norovirus, Cold & Flu viruses, MRSA (2 min) • Eliminates tough odors Residue • No wiping required • Minimal residue Worker Flow • Immediate re-entry Worker Flow Micro-efficacy • Hard surface sanitizer (1 min) • Food contact sanitizer (2 min) Residue • No wiping/rinsing required • Minimal residue Worker Flow • Immediate re-entry time

How to Protect Your Facility During cold and flu season and all year Implementing Best Practices FIGHT ABSENTEEISM 28

Best Practices: Compliance Key Barriers What can help? Cleaning protocols not followed Ready-to-use products Electrostatic technology Product misuse Training and support Incomplete product coverage Clear roles and responsibilities Time constraints Purpose is critical Buy-in Protocols and check-lists Monitoring

Best Practices: Hard Surfaces Tips for preventing the spread of the common cold, flu and norovirus: Bathrooms Surfaces • Clean surfaces from clean to dirty • Clean regularly to remove visible soil • Disinfect high-touch surfaces daily • Use bleach or another EPA-registered disinfectant that is approved to kill influenza and norovirus • Employ electrostatic spray technology for superior surface coverage https: //www. cdc. gov/features/norovirus/ • Clean and disinfect surfaces regularly using a bleach solution or EPA-registered disinfectant that is approved to kill flu and norovirus • Employ electrostatic spray technology for superior surface coverage Things to Remember • Always follow product label instructions • • for dilution (if necessary), application and contact time Use PPE when necessary Increase frequency of cleaning and disinfection during outbreaks Throw disposable cleaning items away after use Wash hands properly and regularly http: //www. cdc. gov/flu/school/cleaning. htm http: //www. flu. gov/planning-preparedness/hospital/influenzaguidance. html#

Best Practices: Soft Surfaces Some pathogens can survive on soft surfaces for as long as three months. Improve soft surface sanitization with three simple steps: 1. Routinely launder washable items and soft surfaces in your facility. 2. Use an EPA-registered product to kill bacteria on soft surfaces between laundering and on soft surfaces that cannot be laundered. 3. Encourage good hand hygiene practices by staff during and between routine cleanings.

Best Practices: Preventing Cross Contamination Cleaning tools and equipment can become contaminated during the cleaning process. Staff should regularly clean and disinfect or replace tools and equipment. Dirty cloths, sponges and mops can spread viruses and bacteria to anything else they come in contact with. Make sure there always enough clean items available for use. Focus on high-touch surfaces and objects such as counter tops, urinals, toilets, door knobs, toilet handles, stall locks, etc. , to help prevent cross-contamination.

Encourage Healthy Habits To help slow the spread of flu, the first line of defense is getting vaccinated. Cough or sneeze into a tissue or your elbow to prevent the spread of illness -causing germs. Regularly wash hands with soap and warm water, especially after sneezing or coughing, touching used tissues or using the bathroom. Stay home when sick to avoid spreading germs throughout the environment and to others.

Conclusion & Questions For more information and resources, visit www. Clorox. Professional. com. 34
- Slides: 34