Welcome NHS Next Stage Review Professor Mayur Lakhani













































































- Slides: 94

Welcome NHS Next Stage Review • Professor Mayur Lakhani • @BCTLLR • #LLRcares

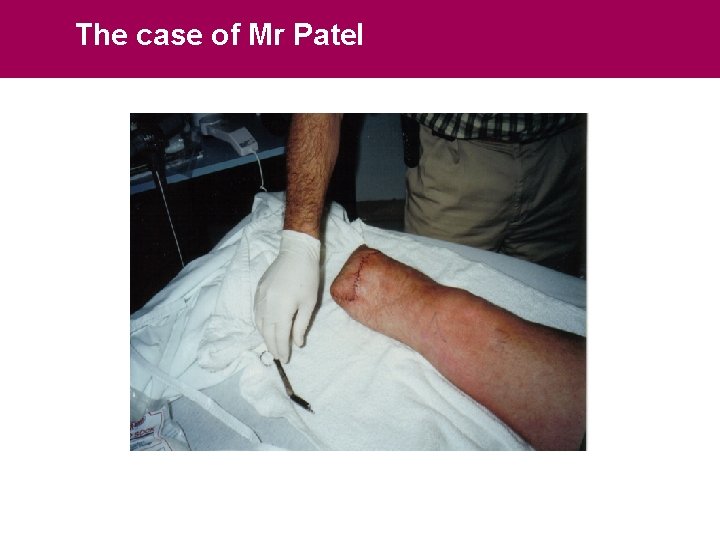
NHS Next Stage Review The case of Mr Patel

What can we learn from Mr Patel? NHS Next Stage Review PASSIVE PATIENT POOR QUALITY POOR CARE THAT COSTS MORE AND LESS EFFICIENT HOW MANY MORE EXAMPLES ARE THERE LIKE THIS? 3

• Reflect on current state of health and care in LLR • How are we responding to the challenges we face, as clinicians • Bring clarity to what we need to do next from the perspectives of clinicians NHS Next Stage Review • What does victory look like for you? • Not a talking shop- outputs that feed into the implementation plans of LLR • Ask not what the STP/LLR can do for you, but what you can do for us? 4

Purposes of Today • Thesis that leadership from the workforce is key to transformation NHS Next Stage Review • Clinicians leading change: • ‘No doctor/NHS organisation is an island’ –system and place of care • It is possible to ‘bend the curve’

NHS Next Stage Review Context • BCT STP

NHS Next Stage Review The patient experience

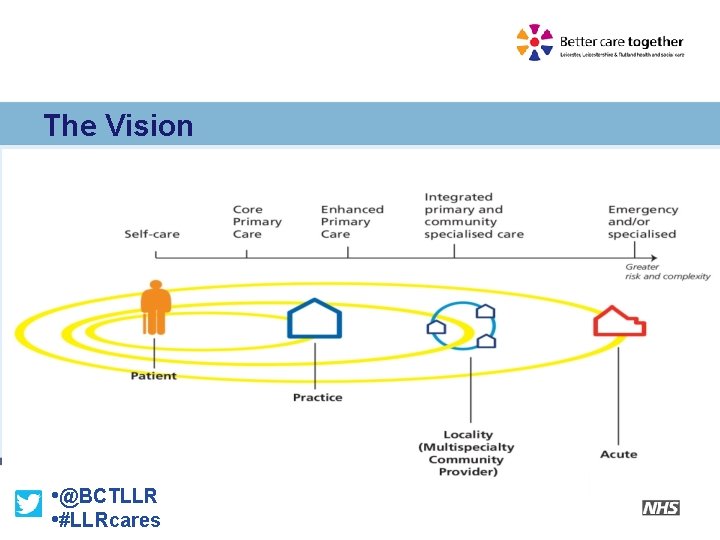
NHS Next Stage Review The Vision • @BCTLLR • #LLRcares

How the Mayo Clinic is battling burnout? • Medicine is an unhappy place right now (54. 4% in a USA study of physicians) NHS Next Stage Review • Listen, act, develop - model • Treat physicians as architects not construction workers (Dubai analogy) • Role and say in designing care delivery models, working sessions – CO-PRODUCTION

The Triple Aim of health care NHS Next Stage Review • Clinical and Population level Outcomes • Patient Experience (by designing care around patients) • Better Value – ‘the LLR pound’ • + Quadruple Aim*: A healthy and engaged workforce (to stop burnout) –*Drummond

Our LLR system and goals Dr Satheesh Kumar, Medical Director, LPT & Lisa Sharples, Head of Workforce and Organisational Development, BCT @BCTLLR #LLRcares

Shared Goals and principles – story so far… • On 6 April 2016 over 200 health and care professionals – What models of care make sense for LLR? – How will we need to work? – What support do we need?

6 April outputs – what did you tell us? • “we need a single vision • “move from for integrating care” transactions to flow” • “we need ‘one system’ • “act as one workforce” language’ – its not the • “shared risk” organisation that • “integrated, multimatters” disciplinary teams” • “focus on the • “shared outcomes population and the framework” patient”

June 2016 – First draft STP • Nationally driven Health & process - identification Wellbeing of priorities in three areas Care & • Built on Better care Quality together programme and 6 April outputs Finance & • Draft shared for Efficiency feedback

September 2016 • Second large-scale engagement event – Integration models – Leadership in a systems context – LLR Way?

November 2016 – May 2017 • Interviews and focus groups system-wide – Principles of working together – How our system impacts the people of LLR – Staff induction/ introduction to the whole LLR system

Creating an introduction to our system • Introduction to our system • Using the input and • Why is our system stories we heard important through our • How we will work together engagement, we are • What we are hoping to creating a series of achieve animations • What support is available

The results – How we work Vision To become one of the best, joined up systems of health and care, with all parts working together to achieve our shared mission Core Principles One Team Person-focussed Accountable We will Work Together across organisational boundaries, collaborating, appreciating each other, seeking to understand the impact of our work on others and sharing decision making to provide best care We will Care for People – designing our system with them at the heart We will act collectively to manage risk and ensure the safety of those in our care We will aim for ‘Home First’ – care close to home, promoting independence We will anticipate obstacles and proactively resolve them Efficient (best value) We will Increase the value of LLR pound by focusing on prevention, early intervention and community based care We will continuously innovate and improve care, driving out inefficiencies and unnecessary variation, sharing resources and reducing duplication and delay

Table discussions (1) • Did we get it right? (Vision, Principles) • What works? • What would we change? • How do we get it out there? • This is your story – what • What do you need from us? should we do with it? • How will we know when it has been successful?

The results – What we will do Mission Deliver the highest possible standard of health and care services to the people of Leicester, Leicestershire and Rutland so that they can fulfil their potential and live healthy, independent lives Goals Wellbeing & Prevention Home & Community First Improve independence, Increase early detection, reduce escalation, Increase rate of reablement and reduce readmission, improve staff wellbeing, … Increase diagnostics and procedures in communities, Create a sustainable, integrated model for specialist community teams and sub -acute care Improve care quality and outcomes for Mental Health, Learning Disabilities and Cancer Responsive, 24/7 Urgent & Emergency Care A World Class Acute Sector Best Value for the LLR £ Keep people well and out of hospital The best care in a crisis Improve access and flow, reduce Length of Stay Provide care in the right setting Focus on emergency and complex, specialised care Focus complex/crisis care at 2 hospitals , reduce duplication, improve research & innovation, improve standards Reduce Inequality Improve outcomes in key conditions Sustainable financial performance Improve efficiency and innovation, Financial savings in line with plan, effective contracting, shared budget (control total), Accountable Care System

Table discussions (2) • Did we get it right? (Mission, Goals) • What works? • What would we change?

Coffee @BCTLLR #LLRcares

Systems Leadership Masterclass @BCTLLR #LLRcares

Systems Leadership Masterclass (How do you get it to work…) @BCTLLR #LLRcares

What to expect • 1 hour 15 minutes • Systems working (the reality of collaboration) • How to make it work • Leave the room thinking differently and with a thought to do something different tomorrow

Attention please… This is an interactive masterclass during which you will be doing several discussion exercises with others at your table.

Systems leadership The system needs leaders who can motivate staff and managers to work differently, across service and organisational boundaries. That is the only way to meet the needs of the growing number of people with complex and long-term conditions, many of whom rely on care and support from different services. The Kings Fund

But what does it really mean? I’m sure glad the hole isn’t in our end. . . These days are over!

“The answers to our problems do not lie within the walls of our organisations. We have to work with others to create critical mass, better services and levels of savings. That feels like the real issue at the moment… When you are in the eye of the storm it can be a difficult place, but this is still the most amazing, rewarding job”. NHS CE JUNE 2017

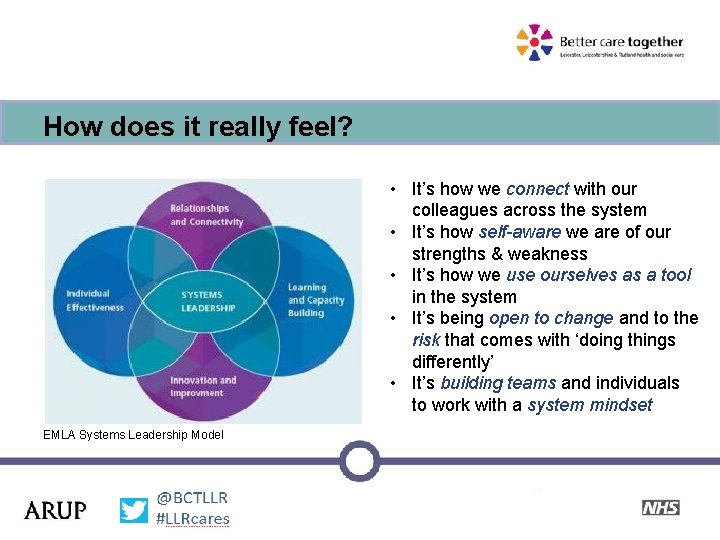
How does it really feel? • It’s how we connect with our colleagues across the system • It’s how self-aware we are of our strengths & weakness • It’s how we use ourselves as a tool in the system • It’s being open to change and to the risk that comes with ‘doing things differently’ • It’s building teams and individuals to work with a system mindset EMLA Systems Leadership Model

What skills, behaviours and attributes does a system leader need to have? @BCTLLR #LLRcares

Chief Execs on working to achieve STP aims… Leaders need: • Truth and honesty: what is happening, the reality • Authenticity • Openness • Relational fabric to anchor you – your connections • Ability to communicate within the reality of social media

Mindset Shift! @BCTLLR #LLRcares

Variability, uncertainty, complexity & ambiguity… How does it feel to work in and lead change in this environment? • • • Anxious Unstable Unclear Slow Stressful Fearful

What is needed Why don’t we like it? (if we’re honest) system What can you do? Working in new ways Feels unnatural. Our brains like habits, known processes Agility We get used to one thing and then the approach, stakeholders, rules change Pay attention to your emotions, reactions and behaviours. Working as a Loss / sacrifice Our identify, ego is threatened, we lose something valuable to us or our team. How you are feeling & your actions impact on how the system operates.

Interacting positively with emotion RAINS

Shifting our outlook Stress Positive challenge Fear Curiosity Anxiety Excitement

Collaboration is not cuddly… So what should you do? @BCTLLR #LLRcares

1. Common purpose What is your WHY • At the heart of what I do is…. • It’s not really about…. • What it’s really about is…. . [2 – 3 words only!]

2. Part a: Relate, relate (Or, connect, connect) Build relationships of both breadth and depth Ask the right questions: • Show interest in others ‘I am interested to know. . . / Would you mind sharing" • Make an in-the-moment observation “I am just aware …” • Ask a question to gain a reaction “ Is that what you really think / feel / mean. . ” • Invite others to contribute “I am sure you will be able to add more to this / Given your experience I am sure you will have a view on this. . “ • Go to a deeper level conversation “ That’s really insightful, why do say that”

2. Part b: Listen (in the right way) “Our thinking depends on the quality of our attention for each other, perhaps the most important thing we could do with our life and with our leadership is to listen to people so expertly, to give them attention so respectfully they would begin to think for themselves, clearly and afresh. ” Nancy Kline, Time to Think

3. Compassion comes first • 40% of NHS staff report that they have felt unwell due to stress • 50% say that the work stress they feel is debilitating In these conditions, we move to fight/flight, quick responses, covering our own backs

3. Compassion comes first • If we want collaborative, systems working we need first to take care of our staff • Collaboration and innovation only happens when: – We feel safe to try new things and take considered risks – We know it’s ok if not everything is a success


4. Conflict… is inevitable You are fundamentally shifting the way that your services, your organisations work There will be change, there will likely be some loss If there is never a conflict – you are not doing it right! Shifting is going to be difficult – but worth it

BUT…. There are things you can do 1. Follow points 1 -3 above (connect to purpose, relate & listen, act with compassion) 2. Set yourselves up for conflict. Create rules for engagement, what is your process when conflict raises it’s head?

Discuss on tables What types of conflict are you experiencing in relation to systems leadership? @BCTLLR #LLRcares

4 habits for good negotiators @BCTLLR #LLRcares

1. Don’t neglect the other side’s problem • If you don’t understand the other side’s perspective, how will you get a solution that works? • The other side will only say yes to a proposal that meets interests better than a no-deal – you need to understand what this will be • Ask, Listen (level 3), Understand

2. Work out what is compatible (also known as shared purpose!) Your incompatible positions (A vs. B) may mask an underlying compatible interest

3. Look for differences • What matters a lot to you but little to them, is an opportunity for an easy win

4. Be aware of bias • Role bias: being over-committed to your point of view, interpreting information in self serving ways • Partisan bias: Painting your side in a positive light, while vilifying the other side

Group questions to ask when conflict arises • If we carry on as we are, what is going to happen? • What is one thing we can collectively agree on? • If we made the bold decision here, what would it be? • If the STP itself was ‘speaking’ to us, what would it tell us to do? What would it tell us to ‘get over’?

Individual questions to ask when conflict arises • What role am I playing in this conflict? • What are my emotions? (RAINS model) • How are my emotions leading me to action? Is this action the best way forward for the group?

And finally…. Looking after you @BCTLLR #LLRcares

True system working is not easy Model self compassion as well as being compassionate to others This is a tough job… thank you & keep going!! 5 ways to wellbeing (NEF)

Final reflection 1. Is collaboration an easier option that competition? 2. What are the issues involved in moving from safeguarding the organisation to doing what is right for the whole system? 3. What help do staff need to do this? 4. How will you ensure your own resilience going forwards?

https: //www. arup. com/en/publications/Promotional-Materials/Section/Arup-in-Healthcare Thank you @BCTLLR #LLRcares

Induction to Improvement Framework Professor Mayur Lakhani, Chair WLCCG & Bina Kotecha, Deputy Director of Learning and Organisational Development , UHL @BCTLLR #LLRcares

LLR Better Care Together Improvement “Portal” Setting Out Our Ambition @BCTLLR #LLRcares

LLR Improvement Portal – Our Vision • Supports system wide improvement • Consistency and standardisation of the way we enable change – using the best of the best • Better capability to engage and empower those affected by change • Centralised place for high quality system leadership development • Harnessing system expertise and building on our capacity with limited resources

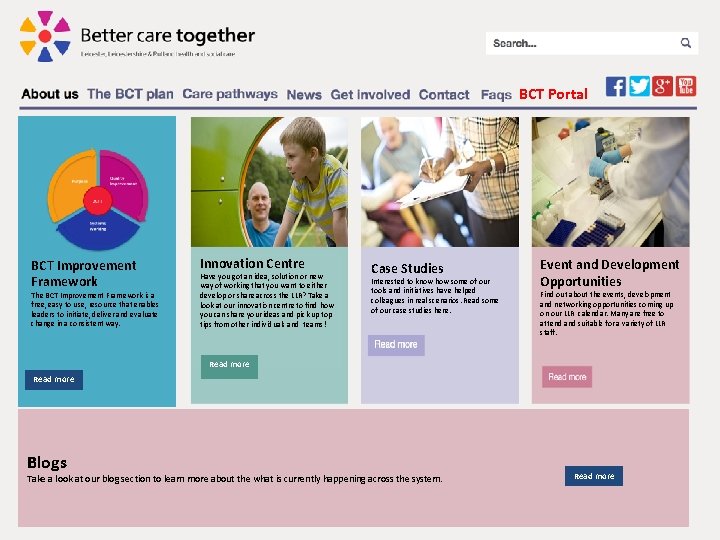
BCT Portal BCT Improvement Framework Innovation Centre The BCT Improvement Framework is a free, easy to use, resource that enables leaders to initiate, deliver and evaluate change in a consistent way. Have you got an idea, solution or new way of working that you want to either develop or share across the LLR? Take a look at our innovation centre to find how you can share your ideas and pick up top tips from other individuals and teams! Case Studies Interested to know how some of our tools and initiatives have helped colleagues in real scenarios. Read some of our case studies here. Event and Development Opportunities Find out about the events, development and networking opportunities coming up on our LLR calendar. Many are free to attend and suitable for a variety of LLR staff. Read more Blogs Take a look at our blog section to learn more about the what is currently happening across the system. Read more

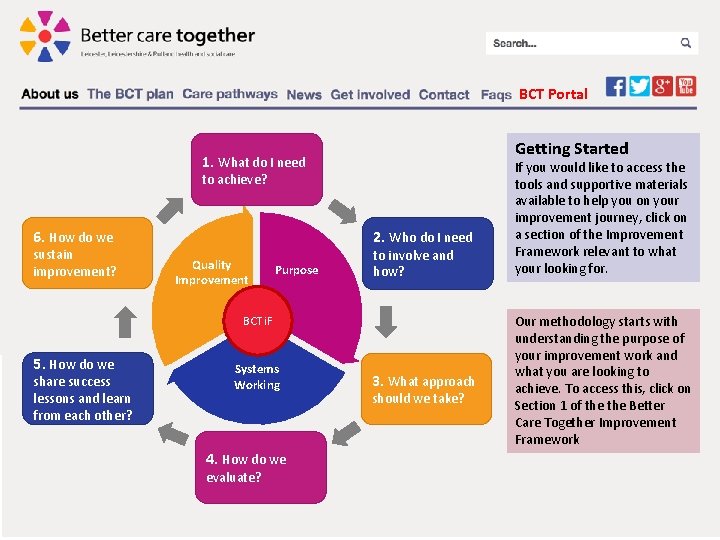
BCT Portal Getting Started 1. What do I need to achieve? 6. How do we sustain improvement? 2. Who do I need Quality Improvement Purpose to involve and how? BCTi. F 5. How do we share success lessons and learn from each other? Systems Working 4. How do we evaluate? 3. What approach should we take? If you would like to access the tools and supportive materials available to help you on your improvement journey, click on a section of the Improvement Framework relevant to what your looking for. Our methodology starts with understanding the purpose of your improvement work and what you are looking to achieve. To access this, click on Section 1 of the Better Care Together Improvement Framework

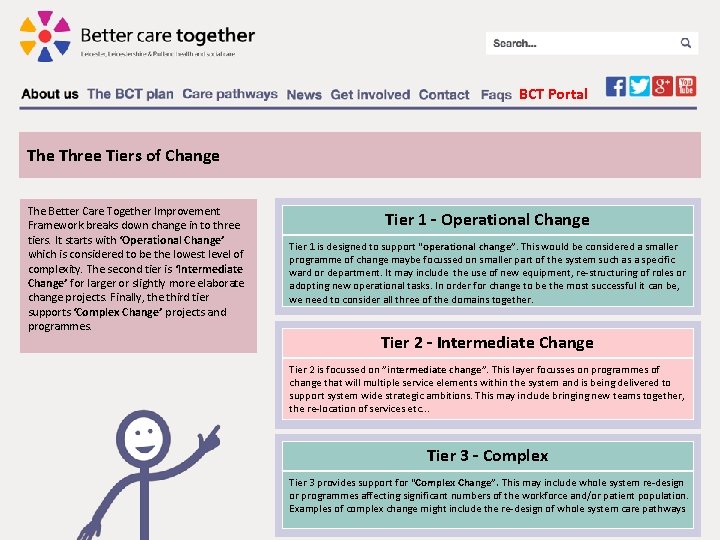
BCT Portal The Three Tiers of Change The Better Care Together Improvement Framework breaks down change in to three tiers. It starts with ‘Operational Change’ which is considered to be the lowest level of complexity. The second tier is ‘Intermediate Change’ for larger or slightly more elaborate change projects. Finally, the third tier supports ‘Complex Change’ projects and programmes. Tier 1 – Operational Change Tier 1 is designed to support "operational change”. This would be considered a smaller programme of change maybe focussed on smaller part of the system such as a specific ward or department. It may include the use of new equipment, re-structuring of roles or adopting new operational tasks. In order for change to be the most successful it can be, we need to consider all three of the domains together. Tier 2 – Intermediate Change Tier 2 is focussed on ”intermediate change”. This layer focusses on programmes of change that will multiple service elements within the system and is being delivered to support system wide strategic ambitions. This may include bringing new teams together, the re-location of services etc. . . Tier 3 – Complex Tier 3 provides support for “Complex Change”. This may include whole system re-design or programmes affecting significant numbers of the workforce and/or patient population. Examples of complex change might include the re-design of whole system care pathways

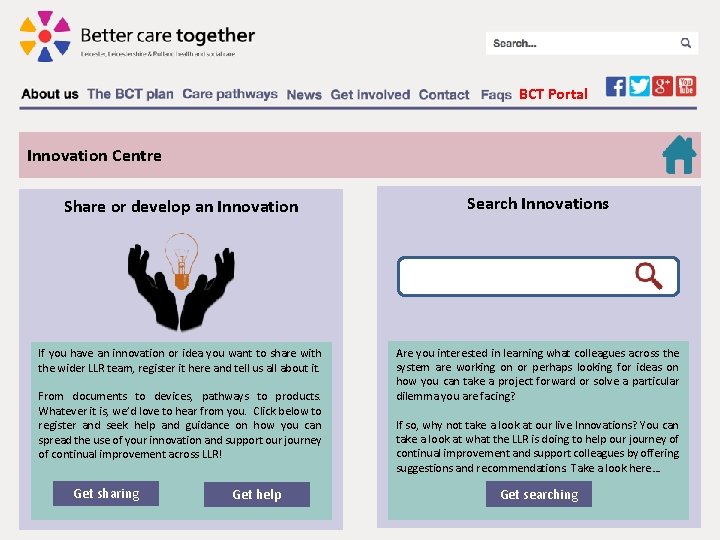
BCT Portal Innovation Centre Share or develop an Innovation Search Innovations If you have an innovation or idea you want to share with the wider LLR team, register it here and tell us all about it. Are you interested in learning what colleagues across the system are working on or perhaps looking for ideas on how you can take a project forward or solve a particular dilemma you are facing? From documents to devices, pathways to products. Whatever it is, we’d love to hear from you. Click below to register and seek help and guidance on how you can spread the use of your innovation and support our journey of continual improvement across LLR! Get sharing Get help If so, why not take a look at our live Innovations? You can take a look at what the LLR is doing to help our journey of continual improvement and support colleagues by offering suggestions and recommendations. Take a look here… Get searching

BCT Portal Case Studies Welcome to our case studies page… Here you can read some of the specific workforce related case studies that have been inspired or delivered as a result of our strategic plans and ambitions to work more collaboratively. All our case studies are reflective of real work and efforts that have been undertaken by teams and individuals across the LLR System Read More

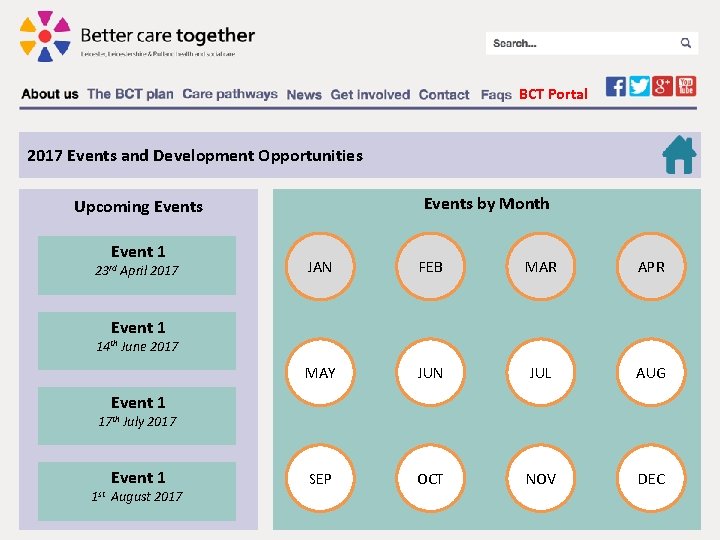
BCT Portal 2017 Events and Development Opportunities Events by Month Upcoming Events Event 1 23 rd April 2017 JAN FEB MAR APR MAY JUN JUL AUG SEP OCT NOV DEC Event 1 14 th June 2017 Event 1 17 th July 2017 Event 1 1 st August 2017

BCT Portal Blog Page Interested in writing blog? If you work within LLR and are interested in sharing an experience, a point of view or want to share something about an exciting project you’re working on, we’d love to hear from you…. Blog 1 Blog 2 by General Manager, UHL by Director of Finance, West Leicestershire CCG Blog 3 Blog 4 I’d like to blog by Office Manager Rutland County Council by Head Engineer East Midlands Ambulance Service

- Sharing expertise across the system - Building upon the best of what is already out there and adopting a consistent approach to change - Championing an integrated, systems way of doing things - Opportunity to create some head space to share, learn and innovate - Well embedded improvement systems already in place in organisations where significant investment has been made - Varying levels of engagement and exposure to systems work - Lots of variation around how change is led and managed - Cultural differences in the way we work

The Big Questions – Table Discussion and Actions

The Big Questions – Priorities for Action What will we collectively achieve over the next 12 months? Consider the following points: • The ambition we have set out • Where we are now, the opportunities this presents and the challenges we need to overcome • Where we should focus our efforts, to have the biggest impact? Discuss at your table for 20 minutes and agree on your top 3 ‘priorities for action’ and ‘what will be different’ in 12 months time … remember to highlight any quick wins

Next Steps – BCT Improvement Framework • Consolidate and theme your feedback on ‘priorities for action’, ‘what will be different’ and ‘quick wins’. • We hope you are interested in taking forward and progressing our change and improvement ambition across LLR – Let us know if you would like to join our Steering or Task & Finish Groups or be one of our future Innovation and Improvement Champions Key to success is everyone sharing ownership and playing their part!

Randomised Coffee Trial Fiona Mc. Namee, Organisational Development Lead, LPT @BCTLLR #LLRcares

Randomised Coffee Trial • Check out your number on your badge • Check out which corner of the room you need to move to – when we are ready to start

• Attention • 3 minutes each way to tell your story • No interruptions, positive body language, nodding and pure listening

• Introduce yourself • Who inspired/influenced you to come and work in health and care in LLR? • What improvements would you like to see in the future?

Lunch @BCTLLR #LLRcares

Welcome back Professor Mayur Lakhani @BCTLLR #LLRcares

Context/ tiger team Dr Matthew Metcalfe @BCTLLR #LLRcares

Report of the Tiger Team for developing alternative clinical models to support the bed capacity risk within the STP @BCTLLR #LLRcares

Aim of the Group The ‘Tiger Team’, comprised of senior clinicians and other professional leaders across LLR, met over the course of four Tuesday evenings to seek alternative solutions to the ‘bed gap’. The key objectives of the Tiger team were: • To identify a cohort of patients who could be cared for in community hospital beds or in the community for a) urgent care and b) planned [elective care] • To suggest how medical support/cover for this could be provided • To suggest how clinical competency and skills gaps will be addressed • To outline a pathway and access routes and timelines for implementation • An initial exploration of the quality impact of the proposed solutions including any potential un-intended consequences

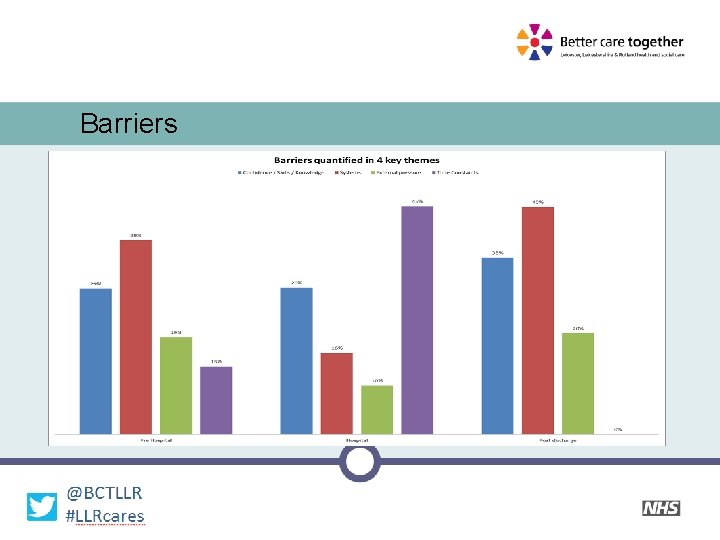
Barriers ‘Barriers’ were seen as the being the biggest obstacle to a sustainable health system, posing a two fold threat to: 1) Risk of deliverability of previously identified plans 2) Inability to extend and push plans in order to close the bed gap Discussion gave a rich picture with barriers grouped into four main categories across pre-hospital, hospital and post-discharge care. These four categories were: • • Confidence/Skills/Knowledge Systems External pressure Time Constraints

Barriers

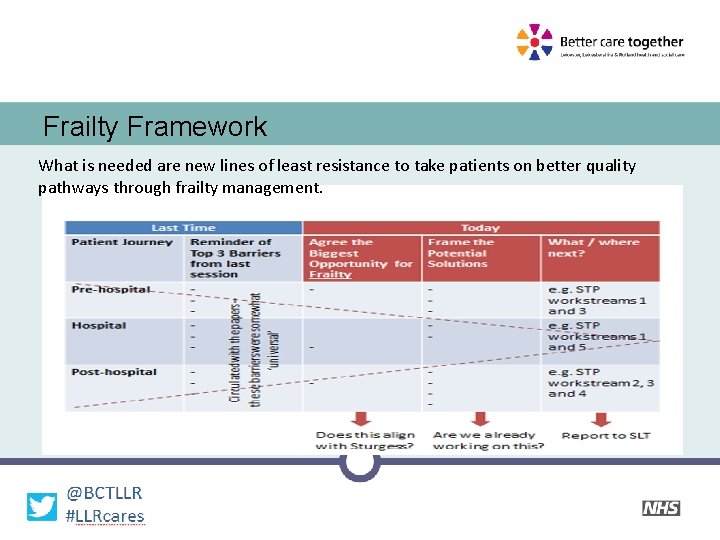
Frailty Framework What is needed are new lines of least resistance to take patients on better quality pathways through frailty management.

Top 3 barriers to reducing bed base through better management of frailty Pre-hospital 1. Better recognition of frailty 2. Diagnostic uncertainty 3. Supportive services in community Hospital 1. Supporting Frailty – ED – Back to community 2. Multiple handoffs 3. Varying discharge thresholds Post Discharge 1. Identification of high readmissions 2. Discharge summary 3. Capability

Top 3 barriers to reducing bed base through better management of frailty Pre-hospital 1. Recognition of frailty - Educational tools / expectations, act on diagnosis, 2. Supportive services in community - knowledge of what’s out there Hospital 1. Multiple handoffs - Navigator role (like learning disabilities), face to face / digital staff interactions, clinician overseeing whole pathway 2. Varying discharge thresholds -Training or complex discharge planning, early recognition of End of Life Post Discharge 1. Identification of high readmissions - frailty pathway, early clinical review, seamless pathway / team based/moving expertise across the pathway 2. Capability - specialist support /education training for generalists

Whole system solutions Moving beyond a silo approach to putting in pace a whole system approach to frailty. Key elements: • development of a frailty pathway, moving from episodic care to longitudinal care of the frail. • Needs: • early recognition and diagnosis • a navigator role to guide patients and public from end to end • a lead clinician from start to finish drawing on real or virtual specialist support when needed • early consideration and triggering of the end of life pathway as soon as appropriate. The intention would be the creation of a single frailty MDT, including social care and community support.

Planned Care – early thoughts • Same methodology applied rapidly to planned care. Potential scope for further work on: • • • Overarching piece of work for what is done for feet and ankles. Scope for rationalisation Hernia hub Menorrhagia pathway (UHL –> 1°) Pre- referral - Self care and expectations Focus on areas where there is clinical appetite and challenging (i. e. only accepting risk) Increase volume where already doing things in community • • • Diagnostics in 1°/Community (cross boundary referrals) Left shift – limited bed opportunity more clinic space/theatre capacity etc. Managing demand a key enabler Addressing variability in referral quality Advice and guidance/PRISM/ triage

Next steps Urgent care Individual points need cross checking against existing STP plans: - are they covered off already? -do they go as far as clinician appetite would suggest they would want to go? - where it goes further what would that mean in terms of beds? Where whole systems approaches solutions are being proposed (ie a single frailty MDT) this needs further consideration and working up. Planned care Further work needed on initial points raised

Workshop @BCTLLR #LLRcares

Workshop Urgent Care Premier Room – Dr Dick Hurwood & Dr Jay Banerjee Mental Health Exhibition Hall – Dr Peter Miller & Dr Peter Cannon Home First Club Suite – Jon Wilson and Carmel O’Brien

Coffee @BCTLLR #LLRcares

Plenary reflections Professor Mayur Lakhani @BCTLLR #LLRcares

Plenary reflections 15 minutes table discussions: • What do we need to do next? • I wish we could use BCT to allow me/my team to do _____ differently • What are things that get in the way – What do we need to do to overcome them?