Welcome and Introductions Presented by MHSACM DMH DPHBSAS

Welcome and Introductions Presented by MHSACM, DMH, DPH/BSAS 1

Assessments 1. Assessment Group Name Affiliation Sherry Davis, Lead Bay Cove Human Services Susan Abbott Vinfen Steve Chisholm CAB Health & Recovery Dave Selden SDT Co-Facilitator North Suffolk Mental Health Porter May Advocates Presented by MHSACM, DMH, DPH/BSAS 2

2. Individualized Action Plan Group Name Affiliation Stephanie Sladen, Lead Health & Education Services Rita Barrette Department of Mental Health Jan Feingold High Point Treatment Center Jordan Oshlag SDT Co-Facilitator Community Healthlink Michael Stuart Spectrum Health Systems Presented by MHSACM, DMH, DPH/BSAS 3
3. Progress Note Group Name Affiliation Nancy Carlucci, Lead Network Health Dallas Gulley Riverside Community Care Joe Passeneau MBHP Anne Priestley Wayside Youth & Family Presented by MHSACM, DMH, DPH/BSAS 4

Thank you! • • DMH DPH/BSAS MHSACM MBHP CHD Presenters Countless volunteers Presented by MHSACM, DMH, DPH/BSAS 5

Morning Agenda MSDP Initiative Overview Compliance Jordan Oshlag Assessment Group of MSDP Processes - Form by Form, Section by Section Review with an Application Work Session Sherry Davis, Lead Susan Abbott Steve Chisholm Porter May Dave Selden Break IAP Group of MSDP Processes - Form by Form, Section by Section Review with an Application Work Session Stephanie Sladen, Lead Rita Barrette Jan Feingold Jordan Oshlag Mike Stuart Lunch Presented by MHSACM, DMH, DPH/BSAS 6

MSDP - Overview • Terms - Presented by MHSACM, DMH, DPH/BSAS 7
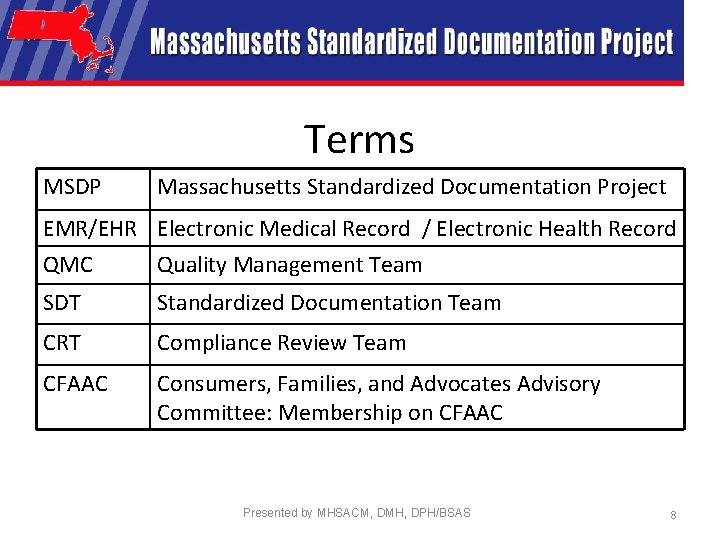

Terms MSDP Massachusetts Standardized Documentation Project EMR/EHR Electronic Medical Record / Electronic Health Record QMC Quality Management Team SDT Standardized Documentation Team CRT Compliance Review Team CFAAC Consumers, Families, and Advocates Advisory Committee: Membership on CFAAC Presented by MHSACM, DMH, DPH/BSAS 8

More terms CBFS Community Based Flexible Support Services CBHI Children’s Behavioral Health Initiative Recovery Orientated Person Centered RAC Recovery Audit Contractor Program OIG Office of the Inspector General Presented by MHSACM, DMH, DPH/BSAS 9

Paradigm Shift Presented by MHSACM, DMH, DPH/BSAS 10

New Language OLD NEW Intake, Assessment, Diagnostic Interview Treatment Plan Patient, Client, consumer CA - Comprehensive Assessment IAP – Individualized Action Plan Person Served Presented by MHSACM, DMH, DPH/BSAS 11

How did we get here Presented by MHSACM, DMH, DPH/BSAS 12

Benefits of Participating • Quality of Care Benefits – Promotes consistent assessment, planning & service documentation – Person-Centered and Strengths focus – Recovery/Resiliency focus – Promotes Information Sharing • Promotes effective collaboration with other providers & shared terminology for use by different disciplines – Less room for error; Decision support Presented by MHSACM, DMH, DPH/BSAS 13

Benefits of Participating • Business Benefits – Compliant with Federal Mandate for Electronic Health Records by 2014 & a wide variety of regulatory and payer requirements • Protection against federal audits – Wide array of funders/payers support this initiative – Enhances Measurement & Outcomes Focus Presented by MHSACM, DMH, DPH/BSAS 14

Benefits of Participating • Financial Benefits – Free training and forms – Compliant with a wide variety of regulatory and payer requirements • Some protection against federal audits – Saves time and money • Reduces redundancy in collecting information • Concurrent documentation possible – Standardized revisions and updates in future Presented by MHSACM, DMH, DPH/BSAS 15

MSDP Initiative Operational Structure Presented by MHSACM, DMH, DPH/BSAS 16

MSDP Scope of Work • The identified scope of work for the MSDP includes documentation requirements for services identified below: – All Department of Mental Health community services – Medicaid Mental Health acute services, regardless of health plan, carve out or Fee For Service status – Services purchased by the Bureau of Substance Abuse Services – Substance Abuse services purchased by Medicaid – EATS, CBATS and Supported Education and Employment Services are included in the scope of work for the project. – Programs that do not have an individual record will not be included in the scope of work (i. e. , Disaster Response, Training, Trauma Response, Consultation Programs, etc. ) Presented by MHSACM, DMH, DPH/BSAS 17

MSDP Forms and Manual Website • Each of the MSDP 2009 version of the paper forms, eforms and manuals can be downloaded by program type at the website: • http: //www. mtmservices. org/MSDP/2009 forms. html • MSDP UPDATE Website: http: //www. mtmservices. org/MSDP-Update. html • Technical Assistance will be provided by the MSDP Leadership Team. Email at MSDPHelp@Earthlink. net Presented by MHSACM, DMH, DPH/BSAS 18

Compliance? Presented by MHSACM, DMH, DPH/BSAS 19

List of Regulators / Licensers / Accrediting Bodies - MSDP Beacon Health: • Documentation Review Tool • BHS FCHP Manual • BHS NHP Manual DHHS Regs: • DHHS Program Memo AB 03037 MH • DHHS SMD Letter Rehab Option DMA Regs: • DMA 130 CMR 429. 400: MH Center Manual • 130450 -275: Resident Regs • 130 CMR 433 -428 Docs • 130 CMR 418 -400 • 130 CMR 417: Day Tx • 130 CMR 450. 100 Presented by MHSACM, DMH, DPH/BSAS 20

List of Regulators / Licensers / Accrediting Bodies - MSDP DMH Regs: • DMH 104 CMR 28. 00 Licensing and Operations for Community Programs • 104 CMR 29. 00 Service Planning • Risk Management Policies: Informed Consent for Psychotropic Medications/ECT Therapy • Comprehensive Assessment Requirements DPH Regs: • DPH 104 CMR 27 • 105 CMR 140. 000 • 105 CMR 160 Detox • 105 CMR 161 STIIT • 105 CMR 162 SA/OT/PT • 105 CMR 750 Drug Tx Programs Presented by MHSACM, DMH, DPH/BSAS 21

List of Regulators / Licensers / Accrediting Bodies - MSDP DPH Regs (con’t): • 105 CMR 165 Halfway House • Family Substance Abuse Shelter Guidelines • Transitional Support MBHP • MBHP Audit Tool • OT/PT Perf Specs • SOAP Documentation Requirements • CBATICBAT Performance Specs • Inpatient Acute Mental Health Performance Specs • Level 4 Detox for Co-occuring Disorders Performance Specs • Medically Monitored Detox ATS Performance Specs Presented by MHSACM, DMH, DPH/BSAS 22

List of Regulators / Licensers / Accrediting Bodies - MSDP Network Health Regs: • Network Health Chart Review Tool NHIC Regs: • NHIC (L 13492) Health Behav Ass Tx • L 3159 Diag Assess • L 3162 Psycho Pharm • L 3187 ECT • L 3203 Neuro Psy Test • L 3220 Group Tx • L 3239 Ind Tx • L 3242 Interactive Ind Tx • Article 90862 • Transmit Psychotherapy Notes • Transmit Psych Tests Presented by MHSACM, DMH, DPH/BSAS 23

List of Regulators / Licensers / Accrediting Bodies - MSDP Federal Medicaid Regs: • Federal States Medicaid Manual 2500 A Doc • States Medicaid Manual 4221 Psych OTPT • States Medicaid Manual 4320 Clinic Federal Opiod Regs: • 42 CFR 812 Opiod Tx • 42 CFR 8. 1221 CFR 291 Opiod Tx JCAHO CARF COA NCQA Presented by MHSACM, DMH, DPH/BSAS 24

Documentation Linkage “The Golden Thread” Assessment Data: Diagnoses - Assessed Needs – Service Recommendations Individual Action Plan Goals Individual Action Plan Objectives Interventions and Services Progress Notes Presented by MHSACM, DMH, DPH/BSAS 25

Assessment Forms Presented by MHSACM, DMH, DPH/BSAS

Personal Information • Must be completed at the time of initial contact with the person who is seeking services. • Captures essential demographic, contact and insurance/billing information. • This form can be completed by support staff or clinical staff. Presented by MHSACM, DMH, DPH/BSAS 27

Adult Comprehensive Assessment • Complete after the Personal Information form, as the person enters services, in compliance with agency policies and funding requirements. • The Adult Comprehensive Assessment provides a standard format to assess mental health, substance use and functional needs of persons served. This Assessment provides a summary of assessed needs that serve as the basis of Goals and Objectives in the Individualized Action Plan. • A qualified clinician must complete or oversee the completion of this form after interviewing the person served, face to face. Presented by MHSACM, DMH, DPH/BSAS 28

Adult Comprehensive Assessment Specifics • Living Situation – Only need to check off one box to indicate person’s living situation • Family and Social Support History • Legal, Education, Employment, Military, etc. – May complete Addenda if additional information is needed; depends on person’s needs • Substance Use – Screening tool needed to determine if there is a substance use problem Presented by MHSACM, DMH, DPH/BSAS 29

Adult Comprehensive Assessment Specifics • Health Summary – If Physical Health Assessment has been completed, do not need to complete again here • Advanced Directives – Follow your agency’s protocols with regard to Advanced Directives • Trauma History – If Trauma is not addressed during initial intake, the Trauma Addendum is available for completion in future sessions Presented by MHSACM, DMH, DPH/BSAS 30

Adult Comprehensive Assessment Specifics • Strengths/Abilities/Resiliency – Key component of the assessment – Important shift in assessment process – Strengths-based assessments increasingly more common; used to generate goals and objectives • Interpretive Summary – This is a summary, not meant to repeat data already gathered – Answers the question: How does the data gathered in the assessment fit together and how will it be used to create an action plan? Presented by MHSACM, DMH, DPH/BSAS 31

Adult Comprehensive Assessment Specifics • Was outcomes tool used? – Different funders require use of different outcomes tools – May not apply to everyone – Example: CANS used for MBHP members • Inclusion of Person Served in assessment process – Important to include person/family response to recommendations – Give person option to read and sign assessment Presented by MHSACM, DMH, DPH/BSAS 32

Assessment Addenda • Addenda: Education, Employment, Legal, Military, Trauma, Substance Use (Substance Use screening must be completed) • Addenda created to shorten the length of the CA • Allows for capture of information relevant to each person served • Meets regulatory requirements of variety of funders Presented by MHSACM, DMH, DPH/BSAS 33

Addendum Example Presented by MHSACM, DMH, DPH/BSAS 34

Assessment Addenda Presented by MHSACM, DMH, DPH/BSAS 35

Assessed Needs Checklist • Functionally oriented • Captures categories other than functioning as well (Addictive Behaviors, Family and Social Support, etc. ) • Combination of clinical and rehab oriented needs to fit a variety of service models Presented by MHSACM, DMH, DPH/BSAS 36

Prioritized Assessed Needs Presented by MHSACM, DMH, DPH/BSAS 37

Adult CA Update • While receiving services persons may experience other issues or have symptoms indicating an additional mental health and/or substance use need or concern that needs to be addressed through treatment • Important to complete a CA Update form to make sure that new need is documented as an “assessed need” and incorporated into support for Goals/Objectives in the IAP Presented by MHSACM, DMH, DPH/BSAS 38

Adult CA Update • This form saves time and effort • Provides an ongoing cumulative history of assessed needs of the person served • A qualified clinician must complete or oversee the completion of this form after interviewing the person served, face-to-face • CA Update should be placed in date order on top of the CA in the chart to provide the appropriate linkage to new services if information provided indicates new services are needed Presented by MHSACM, DMH, DPH/BSAS 39

Form Components • Record the reason for the update • Enter the date of the last Comprehensive Assessment in the chart • ACA Sections for Update • Update Narrative • Signature/Credentials Presented by MHSACM, DMH, DPH/BSAS 40

Diagnosis • Official Diagnosis for the person is located (“Housed”) in the CA or in subsequent CA Updates • If there is a change to the existing Diagnosis or addition of Diagnosis it must be recorded in the CA Update • If there is no change to the diagnosis, indicate that by checking the appropriate box Presented by MHSACM, DMH, DPH/BSAS 41

Treatment Recommendations/ Assessed Needs • Document any new treatment recommendations or assessed needs • Any new recommendations/needs should be considered the basis for subsequent treatment goals and/or objectives Presented by MHSACM, DMH, DPH/BSAS 42

CA Update Process Linked to Treatment Recommendations – If the Treatment Recommendations/Assessed Needs are adequately addressed by the Treatment Recommendations/ Assessed Needs as identified in the original Diagnostic Assessment or earlier CA Updates, then check the box for “No Additional Recommendations Clinically Indicated” in the appropriate section of the CA Update – Determine if existing Goal(s) and Objective(s) address the newly identified recommendations/needs – If yes, use the Progress Note to identify the appropriate Goal and Objective and provide the interventions ordered – If NO…. Presented by MHSACM, DMH, DPH/BSAS 43

CA Update Process Linked to IAP Revision • If existing Goals, Objectives, Interventions, Services, frequency and provider types will NOT meet the person’s newly identified Treatment Recommendations/Assessed Needs, then link the newly assessed needs from the CA Update to an IAP Revision by checking “Change In IAP Required”. Update the IAP accordingly. Presented by MHSACM, DMH, DPH/BSAS 44

ASAM • To be used for person’s with identified Substance Use issues • Links to websites with more information in ACAU manual Presented by MHSACM, DMH, DPH/BSAS 45

Child/Adolescent Comprehensive Assessment • Complete after the Personal Information form, as the person enters services, in compliance with agency policies and funding requirements. • The Child/Adolescent Comprehensive Assessment (C/A CA) provides a standard format to assess the mental health, substance use, legal status and functional needs of children. This assessment provides a summary of assessed needs that serve as the basis of goals and objectives on the Individualized Action Plan. The C/A CA may be completed in concert with the Child and Adolescent Needs and Strengths (CANS) assessment. Presented by MHSACM, DMH, DPH/BSAS 46

Child/Adolescent Comprehensive Assessment • Follow agency policies and procedures when choosing to complete Child or Adult Comprehensive Assessment for transitional age youth (16 -21) • Complete the “Transition to Adulthood section for children 14. 5 years and older. • If completing the CANs assessment, complete significant history sections only. Presented by MHSACM, DMH, DPH/BSAS 47

Child/Adolescent Comprehensive Assessment Specifics • Addenda – Same addenda are used for Child/Adolescent Assessment and Adult Assessment • Sections of the assessment mirror the CANS • Each section contains assessment of current and historical functioning • Covers broad age ranges; specific instructions included in manual Presented by MHSACM, DMH, DPH/BSAS 48

Child/Adolescent Comprehensive Assessment Specifics • Transition to Adulthood – Applicable to mature minors; opt out checkbox is available Presented by MHSACM, DMH, DPH/BSAS 49

Child/Adolescent Comprehensive Assessment • Incorporation of CANS into Child/Adolescent Assessment Presented by MHSACM, DMH, DPH/BSAS 50

Child/Adolescent Comprehensive Assessment Update • Same set up as the Adult Comprehensive Assessment Update; to be used under same circumstances as ACAU. Presented by MHSACM, DMH, DPH/BSAS 51

Mental Status Exam • Use anytime to assess symptoms and behaviors. • This is a data gathering tool, with multiple uses, to assess current symptoms and behaviors. This is a component of the comprehensive assessment, or is completed as part of a risk assessment. Also it is provided as a stand-alone document. • A licensed practitioner as determined by agency policy must complete this form after interviewing the person served, face to face. Presented by MHSACM, DMH, DPH/BSAS 52

Mental Status Exam • Focus on changing commonly used “clinical” language to less clinical, more “person-friendly” language. • Examples of old vs. new language: – – – Anhedonia → Inability to perceive pleasure Homicidal ideation → Aggressive thoughts Attitude → Demeanor Compliant → Cooperative Lack of insight → Difficulty acknowledging presence of psychological problems Presented by MHSACM, DMH, DPH/BSAS 53

Risk Assessment • Used to assess risk of harm to self or others as part of a comprehensive assessment or when assessing a person in crisis. • Gathers data on relevant risk issues and severity. • Completed by a masters level clinician or a paraprofessional, under the supervision of a licensed clinician; or a licensed clinician. Presented by MHSACM, DMH, DPH/BSAS 54

Initial Psychiatric Evaluation • Complete after the Personal Information form, as the person enters services, in compliance with agency policies and funding requirements. • Used to assess the bio-psychosocial health and service needs of the person served. Components of this evaluation are included in the comprehensive assessments. Also it is provided as a stand-alone document. • This form is to be completed by a psychiatrist, CNS or other APN with credential in psychiatry and prescribing privileges. Presented by MHSACM, DMH, DPH/BSAS 55
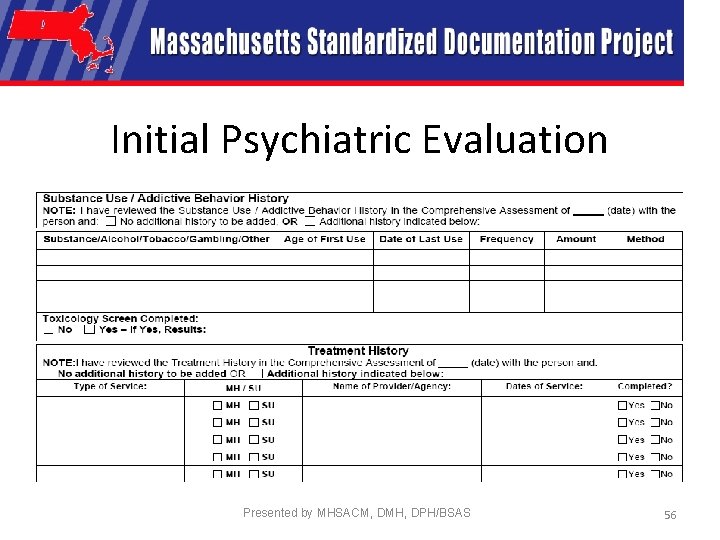

Initial Psychiatric Evaluation Presented by MHSACM, DMH, DPH/BSAS 56

Initial Psychiatric Evaluation Specifics • Designed to allow writer to indicate review of Comprehensive Assessment • Reduce redundancy for person served Presented by MHSACM, DMH, DPH/BSAS 57

Tobacco Assessment • Required for some DPH licensed programs; completed in concert with the comprehensive assessments. • Optional for other programs following agency policies. • Assesses current and past tobacco use and readiness to change. • Completed by staff following agency policy. Presented by MHSACM, DMH, DPH/BSAS 58

HIV Risk Assessment • Required for some DPH licensed programs; completed in concert with the comprehensive assessments. • Optional for other programs following agency policies. • Assesses current and past risk behaviors as well as willingness for testing and treatment. • Completed by staff following agency policy. Presented by MHSACM, DMH, DPH/BSAS 59

Physical Health Assessment • To be completed by qualified Medical Professional. Required for JCAHO certified programs and some DPH services; completed in concert with the comprehensive assessments. • Optional for other programs following agency policies. • Assess current and past medical issues of the person served that may impact current functioning. • Gathers test results that may be pertinent for functioning in the future. Presented by MHSACM, DMH, DPH/BSAS 60

Emergency Services Comprehensive Assessment Standardized assessment for use by – Emergency Service Program – Crisis Evaluation Similar to ACA, but shorter to accommodate time restraints. Clearly identifies: – Core Assessment Components – Practical Information – Level of Care Determination and Justification Presented by MHSACM, DMH, DPH/BSAS 61

Core Assessment Components • • • Presenting Concerns Substance Use/MH History Mental Status Exam Assessed Needs Checklist Prioritized Assessed Needs Clinical Formulation Presented by MHSACM, DMH, DPH/BSAS 62

Practical Information • Collateral Contacts • Current Medications Presented by MHSACM, DMH, DPH/BSAS 63

Level of Care Determination and Justification • Person Served Strengths • Disposition Presented by MHSACM, DMH, DPH/BSAS 64

Individualized Action Plan (IAP) Group Documentation Processes/Forms • Individualized Action Plan (IAP): – Expanded – Condensed – Short w/ Multiple Goals • IAP Review/Revision • Psychopharmacology Plan • IAP Detoxification • Multi-Disciplinary Team Review/Response • Transfer/Discharge Summary and Plan Presented by MHSACM, DMH, DPH/BSAS 65

Individualized Action Plan (IAP) • To promote principles of recovery, this form serves as what most of us have known as a treatment plan • The name reflects the recovery concept of shared decision making • Used to document collaboratively identified goals, objectives, and therapeutic interventions Presented by MHSACM, DMH, DPH/BSAS 66

Individualized Action Plan (IAP) • Key Functions: – Links to needs identified during the assessment phase or ongoing treatment – Serves as a tool to collaboratively build a treatment plan, which reflects both medical necessity and the desired outcomes of the person served in his or her own words – Design encourages collaboration amongst programs and across agencies Presented by MHSACM, DMH, DPH/BSAS 67

Individualized Action Plan (IAP) • Supporting a recovery focus, transition and discharge planning is advised from the earliest point in treatment possible. A section is provided on the form to assist in this process. Presented by MHSACM, DMH, DPH/BSAS 68

Individualized Action Plan (IAP) • A walk through of the form will demonstrate how key fields support documentation of medical necessity and linkage to identified needs, as well as a collaborative and recovery focused tool. Presented by MHSACM, DMH, DPH/BSAS 69

Individualized Action Plan (IAP) • Multiple formats are available to best meet the needs of various individuals and programs. – “Expanded” Version: provides one page per goal with ample space for writing followed by a page of objectives, which correspond with that goal – “Condensed” Version: provides space to document a goal with two objectives all on one page – “Short with Multiple Goals”: gives a user multiple condensed goal pages within one document Presented by MHSACM, DMH, DPH/BSAS 70

Individualized Action Plan (IAP) Review/Revision • This form/process was designed to document information from ongoing review(s), revision(s) of goals and objectives, and/or periodic rewrites • The IAP Review/Revision assists in minimizing duplication and maximizing the documentation of information, which demonstrates evidence and/or rationale for revision Presented by MHSACM, DMH, DPH/BSAS 71

Individualized Action Plan (IAP) Review/Revision ü Use the IAP Review/Revision form to update or modify the IAP in any of the following ways: • Revisions – to add a new goal; change goals, objectives or interventions; or change the frequency or duration of services; • Reviews - to record the progress of the person served and • Rewrites - annually, after three interim revisions, or per agency protocol, a “rewrite” of the actual IAP is warranted. This will facilitate the identification and tracking of treatment goals/objectives and progress made. Presented by MHSACM, DMH, DPH/BSAS 72

Individualized Action Plan (IAP) Review/Revision • Use both pages of the IAP Review/Revision form for either a Review or Revision; Additional goal and/or objective sheets should be added as necessary. If you are adding a new goal or objective, attach the goal and/or objective page(s) from the IAP form to the IAP Review/Revision form. • When a Rewrite is being completed, page 1 of the IAP Review/Revision should be used and the new IAP should be attached. • If a goal/objective is new and not currently supported by the most recent Comprehensive Assessment, it is important to also complete a Comprehensive Assessment Update form. Presented by MHSACM, DMH, DPH/BSAS 73

Psychopharmacology Plan • Used for persons receiving outpatient psychopharmacology services only. • Designed for ease of use and to capture all required information succinctly and accurately. Presented by MHSACM, DMH, DPH/BSAS 74

Detoxification Plan • Used for persons receiving inpatient detoxification treatment. • Modeled after the standard Individualized Action Plan and reflective of the ASAM dimensions of treatment. • Reflects and supports the short-term nature of this treatment modality. Presented by MHSACM, DMH, DPH/BSAS 75

Multi-Disciplinary Team Review/Response • As required, use this form to document the review of Individualized Action Plans and other necessary clinical documentation by a multidisciplinary team. • This form is designed to be used as a tool to provide feedback regarding required actions by the primary provider. Presented by MHSACM, DMH, DPH/BSAS 76

Transfer/Discharge Summary and Plan • Use at the time of transition or discharge, including any movement throughout the continuum of care both internal and external. • Summarize treatment, reasons for transition/discharge, and plans for referral to assist the person in following through on aftercare recommendations. Presented by MHSACM, DMH, DPH/BSAS 77

Individualized Action Plan Group Processes/Forms Application Exercise Presented by MHSACM, DMH, DPH/BSAS 78

Afternoon Agenda Progress Note Group of MSDP Processes - Form by Form, Section by Section Review with an Application Work Session Nancy Carlucci, Lead Dallas Gulley Joe Passeneau Anne Priestley Break Interplay between forms; New Goals, New Information, Updates Stephanie Sladen Implementation Strategies Jordan Oshlag Questions and Discussion Jordan Oshlag Presented by MHSACM, DMH, DPH/BSAS 79

Progress Notes Presented by MHSACM, DMH, DPH/BSAS 80

State of Behavioral Health Records in Massachusetts : 2001 Presented by MHSACM, DMH, DPH/BSAS 81

In 2001, we found isolated examples of superior documentation. Generally, however, record keeping: • • Low Priority; Poor Quality; Confusing Forms / Terminology; Multiplicity of Forms. Presented by MHSACM, DMH, DPH/BSAS 82

When Clinical Forms are Not Standardized: • Labor-Intensive Form Revision Process • Staff Training • Difficulty Reconciling Payer Requirements • Existence Of Multiple Forms, Same Facility • Frustration Presented by MHSACM, DMH, DPH/BSAS 83

Is it an exaggeration… to say that across the state, there at least 1, 000 versions of each sheet of paper, for each form? Presented by MHSACM, DMH, DPH/BSAS 84

Lack of Standardization, At What Cost? 8 most common clinical forms per OP record*: – Personal Info. Assess. (1 p) – Comp. Assessment (4 pp) – Individ. Action Plan (1 p) – Progress Note: therapy (1 p) – Progress Note: group (1 p) – MDT Review (2 pp) – Discharge Summary (1 p) – Psychopharm. Eval. (2 pp) TOTALS: *8 forms = 13 pages @ 1, 000 versions = 13, 000 pages = 26 reams = 2. 6 cases of paper 8 MSDP Forms: 1 version, 23 pages Presented by MHSACM, DMH, DPH/BSAS 85

MSDP Forms are Tools • All tools take time to learn. • They are not substitutes for professional judgment and are not perfect. • Designed to: – – – Identify Assessed Needs Decrease Confusion Fix Documentation Problems Address Risk Management Document Quality of Services Presented by MHSACM, DMH, DPH/BSAS 86

Types of Progress Notes 1. 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. Consultation Collateral Group Psychotherapy Health Care Provider Orders Intensive Services Monthly Nursing (long & short versions) Outreach Psychopharmacology-Psychotherapy Shift/Daily Services Weekly Presented by MHSACM, DMH, DPH/BSAS 87

Key Elements • Therapeutic Interventions Provided • Person’s Response to therapeutic interventions, progress and functioning • Interventions Linked to IAP interventions • New Issues • Billing Strip Presented by MHSACM, DMH, DPH/BSAS 88

Key elements Therapeutic Interventions and Person’s Response to interventions Insert sections: “Therapeutic Interventions” and “Person’s response” from Group psychotherapy Presented by MHSACM, DMH, DPH/BSAS 89

Key elements • Linkage to specific Goal(s)/Objective(s) in IAP: – Group Progress Note: Insert Goals/Object box – Monthly Progress Note: Insert Goals/Object box – Nursing Progress Note: Presented by MHSACM, DMH, DPH/BSAS 90

Key element - “New issues” Four Options: 1. “None Reported” 2. If the new issue can be resolved during the session, document in the “Person’s Response Section” 3. If the issue is already part of the Goals and Objectives, document the progress in the “Person’s Response Section” and… Presented by MHSACM, DMH, DPH/BSAS 91

Key element – “New issues” 4. When a new issue with a therapeutic need is not addressed in the IAP: • Check “CA Update Required” • Document the new issue on a Comprehensive Assessment Update as instructed in the manual. • The newly assessed therapeutic information may require a new goal, objective, therapeutic intervention or service additionally requiring use of the IAP Review/Revision form Presented by MHSACM, DMH, DPH/BSAS 92
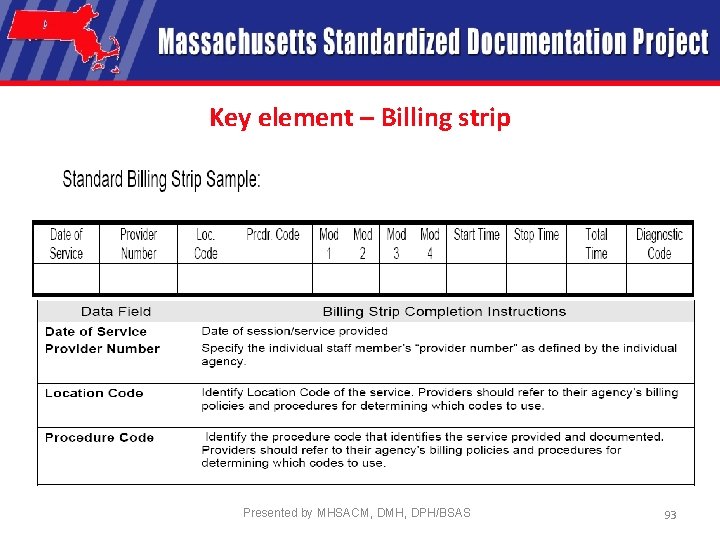

Key element – Billing strip Presented by MHSACM, DMH, DPH/BSAS 93

Medicare “Incident to” MSDP forms that contain the Medicare “Incident to” checkbox: Ø Group Psychotherapy Progress Note Ø Intensive Services Progress Note Ø Nursing Progress Notes Presented by MHSACM, DMH, DPH/BSAS 94

Psychotherapy • Use to document therapeutic interventions and person’s response to the intervention(s) during a specific contact. • Use for outpatient individual, couple, or family psychotherapy. Presented by MHSACM, DMH, DPH/BSAS 95

Group Psychotherapy • Used to document therapeutic interventions and person’s response to the intervention(s) during a specific contact. • Used for outpatient group psychotherapy. Presented by MHSACM, DMH, DPH/BSAS 96

Nursing (Long or Short) • To be completed by a LPN, RN, BSN, or MSN • Use either long or short version depending on amount of space needed. • Use as a shift note by a nurse in Detox, SOAP, or DDART program. Presented by MHSACM, DMH, DPH/BSAS 97

Nursing (Long or Short) • Nursing Progress Note Short: • Nursing Progress Note Long: Insert: Person’s Condition; No sig. changes; Notable; and changes in person’s condition grid. Presented by MHSACM, DMH, DPH/BSAS 98

Psychopharmacology Progress Note • For Pharmacological Management session by: – Psychiatrists – Advanced Practiced Registered Nurses – Clinical Nurse Specialists • Key features: – Ease of use; – Salient information; – Tracks status of core clinical data Presented by MHSACM, DMH, DPH/BSAS 99

Psychopharmacology/Psychotherapy Progress Note • For Individual Psychotherapy with Medical Evaluation and Management session by: – Psychiatrists – Advanced Practiced Registered Nurses – Clinical Nurse Specialists Presented by MHSACM, DMH, DPH/BSAS 100

Psychopharmacology/Psychotherapy Progress Note • Key features: – Ease of use; – Salient information; – Tracks status of core clinical data – Clearly indicates provision of both services Presented by MHSACM, DMH, DPH/BSAS 101

Consultation/Collateral Contact • Use for billable or non-billable face-to-face or telephonic consultation or collateral contacts. • Identifies next action step and responsible party. Presented by MHSACM, DMH, DPH/BSAS 102

Outreach Services • Use for home visits and community support interactions with the person and/or family. • Required for CRS, CSP, FST, Flex Support Programs and PACT. Insert Goals Objective Addressed as per Ind. Action Plan section Presented by MHSACM, DMH, DPH/BSAS 103

Intensive Services • Use for all individual and group services as part of CBAT, ICBAT, PHP, IOP, SOAP, and DDART. • Documents each therapeutic service during the course of the day. Presented by MHSACM, DMH, DPH/BSAS 104

Shift/Daily • Required for Child Day Services, Crisis Stabilization Unit (CSU), Detox Level III, Intensive Residential Treatment Program (IRTP), and Respite. Presented by MHSACM, DMH, DPH/BSAS 105

Monthly • Use for services requiring monthly documentation • Required for Residential Services (DMH) • Summarizes progress toward the IAP goals and significant environmental changes Insert Goal/objective Status Box Presented by MHSACM, DMH, DPH/BSAS 106

Weekly • Use to document therapeutic interventions over the course of a week and the person’s response to the interventions. • Required for Psychiatric Day Treatment and Transitional Support Services (TSS). Insert Type of Program and Services provided this week boxes Presented by MHSACM, DMH, DPH/BSAS 107

Healthcare Provider Orders • Use when a person is either living in a DMH-funded program or is receiving DMH-funded Supported Housing Services. • Serves as ongoing communication tool amongst providers. • Can be used in outpatient behavioral health settings as the progress note for a medication visit. • Ensures thorough and current medication list. 2. Self Medication Training Plan Presented by MHSACM, DMH, DPH/BSAS 108

Questions for the Progress Note Sub-Group Presented by MHSACM, DMH, DPH/BSAS 109

Interplay Between Forms • Progress Notes – New goals/Objectives/Issues • IAP Updates/Revisions • CA Update form Presented by MHSACM, DMH, DPH/BSAS 110

MSDP Implementation Strategies Presented by MHSACM, DMH, DPH/BSAS 111

The Change Rules Have Changed… • Behavioral healthcare community providers are facing an increased emphasis on delivering services that support rehabilitation/recovery, outcome based quality services, compliance, performance based funding, and change management requirements like no other time in our industry’s history. • The MSDP Documentation Process is a SOLUTION… Presented by MHSACM, DMH, DPH/BSAS 112

Change Challenges That Require Active Leadership… • Quality Improvement Process Focus (QI) – Typically Supports Lack of Forward Movement/ Attainment – Process based discussions of the need to change Vs. • Continuous Quality Improvement Solution Focus (CQI) – Implies Movement Forward/Action Has Happened to Provide Continuous Improvement Presented by MHSACM, DMH, DPH/BSAS 113

Key CQI Pre-Implementation Evaluation Areas 1. 2. 3. 4. How many styles/processes of Diagnostic Assessments, Service/Action Plans, Progress Notes, etc. are currently being used by staff in the Organization? What is the level of “ownership” in the current processes/documentation models? Emotional response level from staff when faced with change needs Willingness/support of Senior Managers to move forward Presented by MHSACM, DMH, DPH/BSAS 114

Key CQI Pre-Implementation Evaluation Areas 5. Assess core competency levels of direct care staff regarding: • Ability for staff to provide a more focused/objective information gathering/recording model/clinical formulation. • Level of narrative intensity in current documentation model versus focused check off/short narrative is critical through structured MSDP Clinical Tools • EHR Conversion: Computer hardware and software skills for electronic recording of documentation Presented by MHSACM, DMH, DPH/BSAS 115

Top Eight MSDP Implementation Challenges 1. Change Itself… Change is hard “We’ve always done it another way. ” “I like my way better. ” Individualized documentation perspectives and professional pride – Lack of understanding of WHY we should change – Big changes might affect competencies of some staff – Concern that the MSDP forms will not keep up with accreditation changes – – Presented by MHSACM, DMH, DPH/BSAS 116

Top Eight MSDP Implementation Challenges 2. Training costs/Learning curve/Productivity issues – Initially it takes more time to use new forms – Don’t know where to find info or where to put info in the forms – New forms might alter some internal processes – Training is needed to adapt to new forms system Presented by MHSACM, DMH, DPH/BSAS 117

Top Eight MSDP Implementation Challenges 3. Lack of commitment by top management – Perception that this is something we have to do, that this is being done to us, rather than looking for how it helps us. – Focus on rules, requirements and mandates – Lack of recognition of the changing business climate (increased scrutiny) – Focus on the perception that this will cost us money to implement, not seeing the potential for saving $$ Presented by MHSACM, DMH, DPH/BSAS 118

Top Eight MSDP Implementation Challenges 4. Forms don’t accommodate everyone’s current way of doing business – Asking clinicians to code billing strips on Progress Notes – Person Served name and # at the top of page, not the bottom – Some info on CA we’ve always put on Demographic form or Health History form, etc. – At first, clinical staff disagreed with the CA Presented by MHSACM, DMH, DPH/BSAS 119

Top Eight MSDP Implementation Challenges 5. New processes – Lack of understanding of important linkages necessary in the documentation – A CA Update and IAP Review/Revision processes are not understood – Lack of recognition that new forms will require some processes to be changed or reinvented – Need to look at whole system of documentation rather than just pieces and focus on integration of services and documentation Presented by MHSACM, DMH, DPH/BSAS 120

Top Eight MSDP Implementation Challenges 6. Technology issues – Investments in current systems – Costs to make changes in current systems – Forms don’t accommodate our existing business model; need to be integrated into how we do business Presented by MHSACM, DMH, DPH/BSAS 121

Top Eight MSDP Implementation Challenges 7. Issues with the forms themselves – – Not enough space to write on the forms No lines in the text boxes We can’t change the forms They are not in our local software which I know and love (They are in WORD!) Presented by MHSACM, DMH, DPH/BSAS 122

Top Eight MSDP Implementation Challenges 8. Incorporating a recovery culture – Shifting from a culture of doing for persons served to a culture of empowering persons served – Lack of understanding what recovery/ resiliency is – Lack of understanding the Medicaid rehabilitation option Presented by MHSACM, DMH, DPH/BSAS 123

Acceptance Levels of Change Process • Keep in mind the stages of acceptance of change staff typically go through with this process: 1. 2. 3. 4. 5. Denial Negotiation Anger (Blaming) Drop Out Acceptance of the need to change Presented by MHSACM, DMH, DPH/BSAS 124

Key Challenges To Address before Implementation of MSDP Forms Begins 1. 2. 3. The trainer needs to believe in the MSDP documentation process and come across to the staff that way – Select Trainers that really believe MSDP process is a positive change. Be aware of individualized documentation perspectives and professional pride Be aware big change may affect the competency of some staff – Plan ahead to provide core competency training (i. e. , Motivational Interviewing, Objective Recording Using Structured Form Process, etc. ) Presented by MHSACM, DMH, DPH/BSAS 125

Key Challenges To Address before Implementation of MSDP Begins 4. 5. 6. Change is hard for some to accept – may need to provide an enhanced Coaching/Mentoring Supervision Model during implementation Management of an agency needs to feel confident and support the documentation processes if the agency is going to implement– need buy in of top management Initially will need to do a closer review of quality of notes and clinical forms Presented by MHSACM, DMH, DPH/BSAS 126

Some Identified Solution Focus Areas to Assist Focus on MSDP Forms are a “Tool not a rule”. As a tool it can address compliance and audit concerns. 2. Focus on what MSDP documentation can do FOR staff instead of what it will do TO staff. Look for the potential benefits. Talk about the benefits. Continue to remind staff that MSDP documentation: 1. – Meets all three national accreditation standards (JCAHO, CARF and COA) – Provides available documentation solution without having to develop local form design efforts – Prepares us to move towards electronic medical records 3. Senior management/leadership need to be visibly proactive about the MSDP forms. Communicate, communicate, communicate. Share “learnings”, “aha’s” and success stories Presented by MHSACM, DMH, DPH/BSAS 127

Some Identified Solution Focus Areas to Assist in Implementation of MSDP Forms 4. 5. 6. Be proactive about training and re-training needs (i. e. , schedule additional core competency support). Provide coaching sessions on documentation. Develop and provide to staff a written implementation plan including a change management strategy. Whether you decide to implement one form at a time or a group of forms (i. e. Progress notes), or all the forms at once, be planful about the approach. Provide training and support. Develop post implementation monitoring and coaching plans. Tie monitoring to CQI efforts. Presented by MHSACM, DMH, DPH/BSAS 128

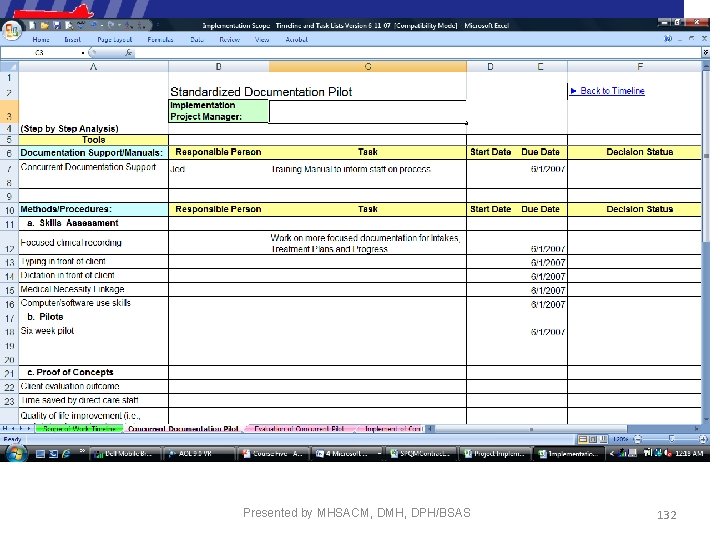
Some Identified Solution Focus Areas to Assist in Implementation of MSDP Forms 7. 8. 9. With staff, look at processes that could be improved and how the transition to MSDP forms can help improve them. View MSDP implementation as an opportunity to take a look at the things that are problematic in your system and perhaps make changes. Use MSDP data for internal process Improvements. Try the MSDP e-forms. Talk to your software vendor about integrating the forms into your systems (Several vendors are in the process). Try each form at least 7 times and then keep track of issues, problems, suggestions for improvement. Presented by MHSACM, DMH, DPH/BSAS 129

Implementation Timeframes and Supports • Establish a completion date before the initiative begins. • Develop a full implementation plan with action work plans to ensure operational readiness. • Recommend a pre-announced evaluation process to ensure all feedback regarding implementation process is given consideration Presented by MHSACM, DMH, DPH/BSAS 130
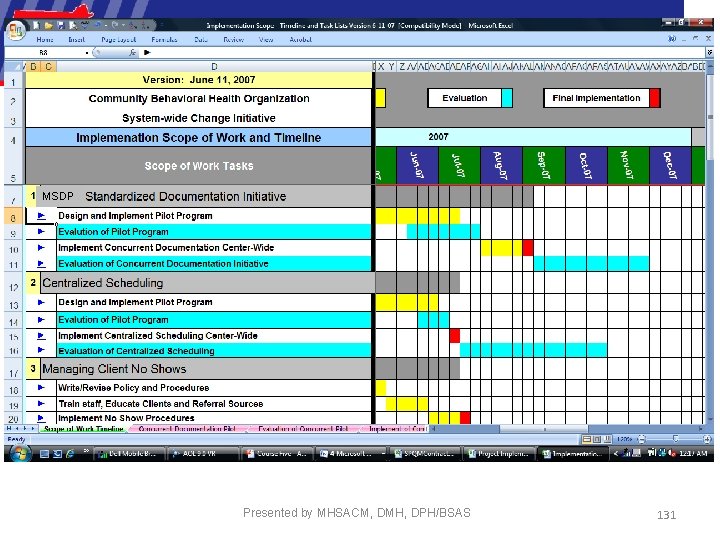
MSDP Presented by MHSACM, DMH, DPH/BSAS 131
Presented by MHSACM, DMH, DPH/BSAS 132

Resources • • How to start Integration Planning Help: – MSDPHelp@Earthlink. net Presented by MHSACM, DMH, DPH/BSAS 133

Questions and Discussion Presented by MHSACM, DMH, DPH/BSAS 134
- Slides: 134