Week 10 GU Alterations By Teresa Hunt RN

Week 10 GU Alterations By Teresa Hunt RN, BSN University of Central Florida

Difference In Pediatrics • Infants can’t concentrate urine. • They achieve complete bladder control by 4 -5 yrs old. • Most children with acute renal failure will recover kidney function. • Shorter urethras lead to increase incidence of UTI’s. • Kidneys function is proportional to body size. Function reduced with stress.
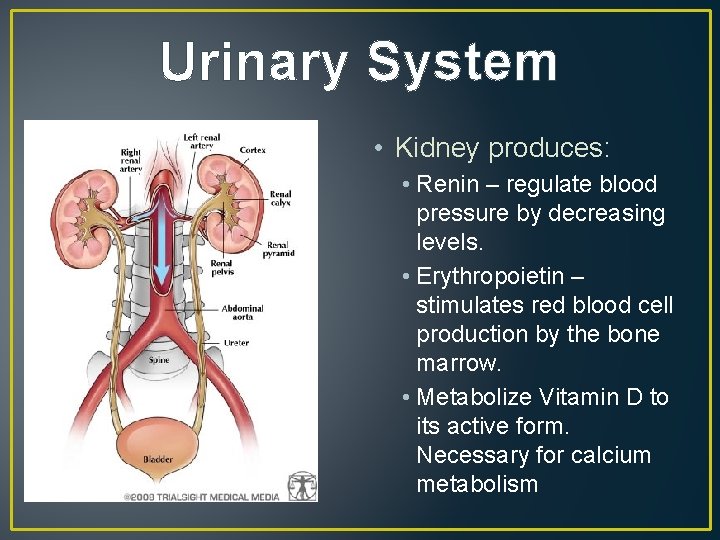
Urinary System • Kidney produces: • Renin – regulate blood pressure by decreasing levels. • Erythropoietin – stimulates red blood cell production by the bone marrow. • Metabolize Vitamin D to its active form. Necessary for calcium metabolism

Enuresis (Diurnal/Daytime) • • Holding Distance to bathroom Interruption in play Incomplete emptying Peers Overactive bladder Urgency Frequency Picture Citation: Wikihow. (n. d. ) How to manage urinary incontinence in children. Retrieved 11/15/14

Enuresis (Nocturnal/Nighttime) • Affects 15 -20% of children at 5 yrs old and spontaneously resolve. • Occurs more often in families with hx of bedwetting. • DDAVP • Wetting alarm • Fluid Restrictions • Avoid extra sugar and caffeine intake after 4 pm Picture reference: Lifestyle Theme on Genesis Framework. (2014). Bedwetting. Retrieved Nov 12, 2014.

Urinary Tract Infection (UTI) In the USA prevalence is 3%-5% in girls and 1% in boys • • • Signs and Symptoms Burning with urination Frequency and urgency Fever Abdominal discomfort Urine Analysis • Nitrates, Bacteria, Blood and WBC’s • Urine Culture • >100, 000 colonies • <100, 000 colonization Causes • Obstruction • Voiding dysfunction resulting in urinary stasis • Anatomic difference • Individual susceptibility to infection • Reflux • Sexual activity • Behavioral

UTI Treatment • Antibiotics 7 -14 days • Sulfamethoxazole – Trimethoprim • Nitrofurantoin • Cephalosporins • IM Ceftriaxone • IV • Gentamicin (aminoglycoside) • Cephalosporin • Ampicillin • Girls – wipe front to back • Cranberry juice • Prophylactic antibiotics • Same as upper left • Possible circumcision • Adhesions removal (penile/vaginal) • Behavior Modification

Specimen Collection Clean- Catch • Used in children that are toilet-trained. • Patient cleans with 3 castile soaps then pees a little into the toilet and then pee into the cup. • • Sterile Catheterization Used in children (<2 yrs) 5 Fr or 8 Fr Sterile Technique Need holding help! • Issues: • Girls are “fluffy” and Urethra and vagina are closely placed. • Boys uncircumcised
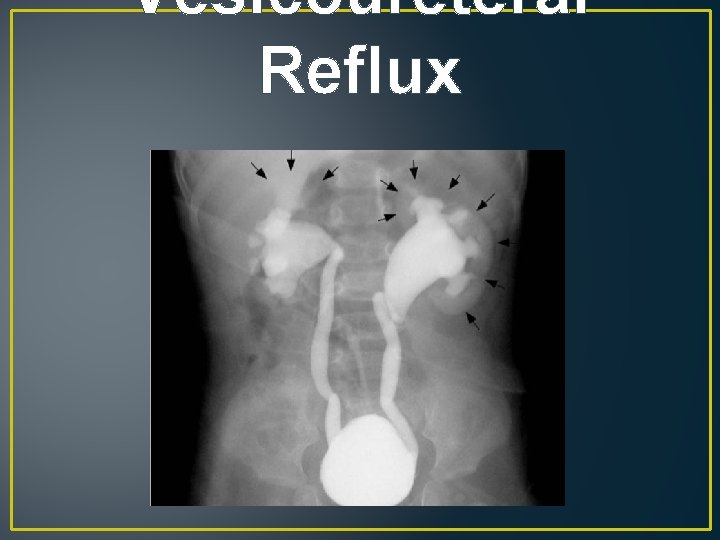
Vesicoureteral Reflux
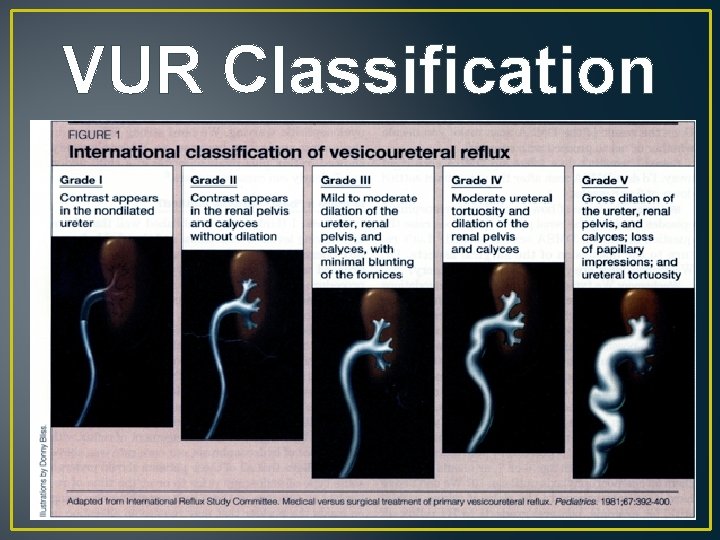
VUR Classification
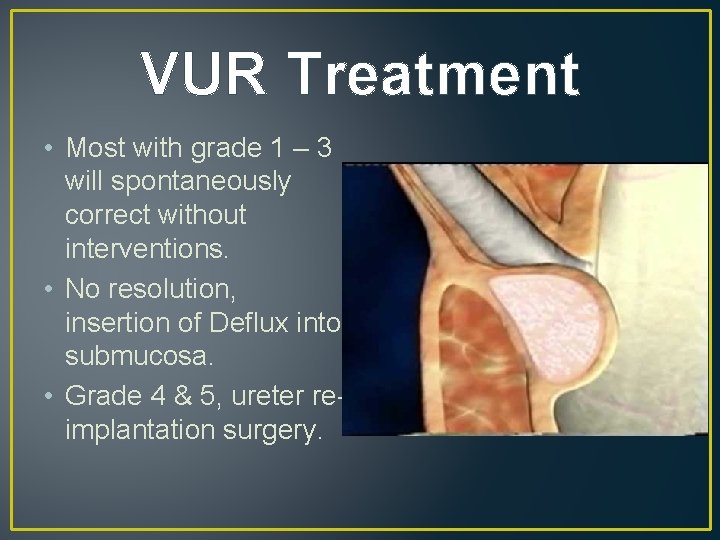
VUR Treatment • Most with grade 1 – 3 will spontaneously correct without interventions. • No resolution, insertion of Deflux into submucosa. • Grade 4 & 5, ureter reimplantation surgery.
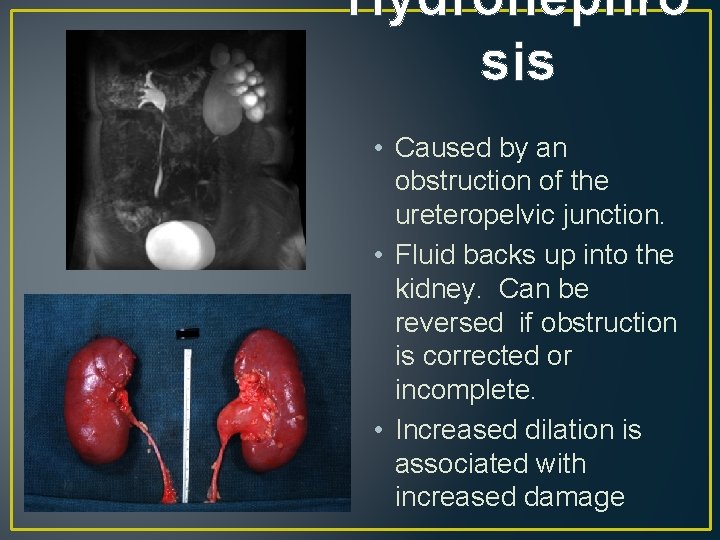
Hydronephro sis • Caused by an obstruction of the ureteropelvic junction. • Fluid backs up into the kidney. Can be reversed if obstruction is corrected or incomplete. • Increased dilation is associated with increased damage

Hypospadias/Epispadia s • Hypospadias occurs in 1: 250 males. • Epispadias is very rare. • May have Chordee. • May have altered urinary stream direction. • Correction not always needed. • • Picture Reference Kraft, K. H. , Shukla, A. R. , and Canning, D. A. [2010] Hypospadias. Urol. Clin. North Am. 37(2), 167– 181.
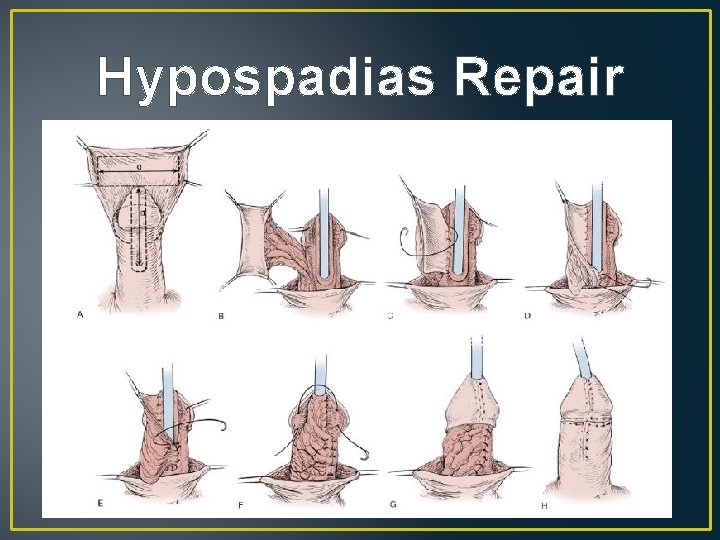
Hypospadias Repair

Cryptorchidism (Undescended testicles) • Occurs in 4. 5% of normal, healthy boys. • It can be unilateral or bilateral. • Usually spontaneously corrects by 6 months of life. • Found by physical exam. • Ultrasound 1 st radiological test for
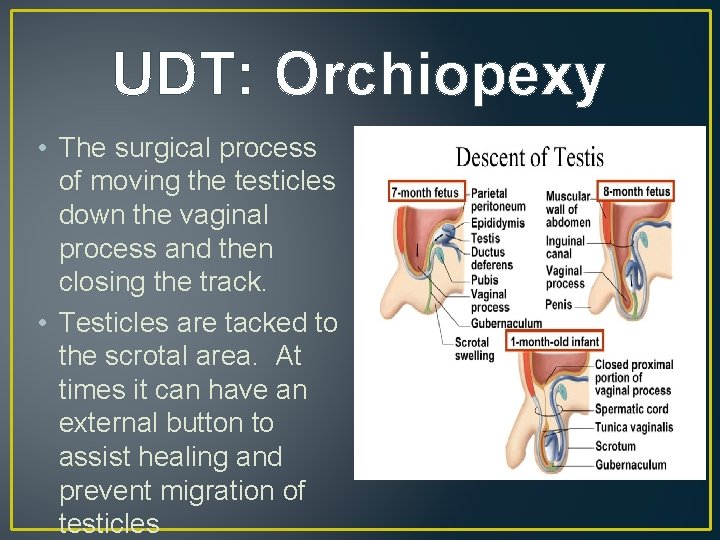
UDT: Orchiopexy • The surgical process of moving the testicles down the vaginal process and then closing the track. • Testicles are tacked to the scrotal area. At times it can have an external button to assist healing and prevent migration of testicles
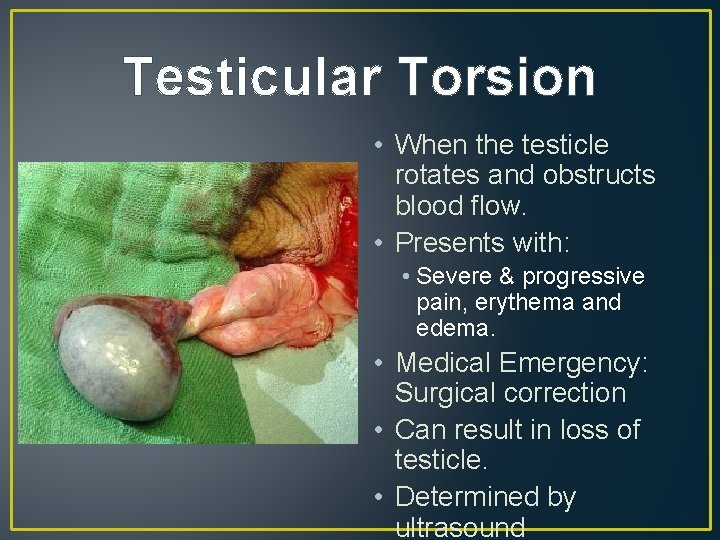
Testicular Torsion • When the testicle rotates and obstructs blood flow. • Presents with: • Severe & progressive pain, erythema and edema. • Medical Emergency: Surgical correction • Can result in loss of testicle. • Determined by ultrasound
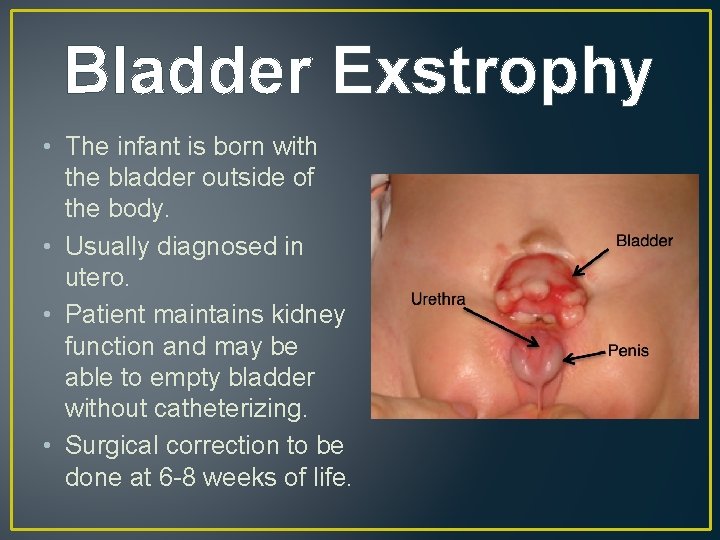
Bladder Exstrophy • The infant is born with the bladder outside of the body. • Usually diagnosed in utero. • Patient maintains kidney function and may be able to empty bladder without catheterizing. • Surgical correction to be done at 6 -8 weeks of life.
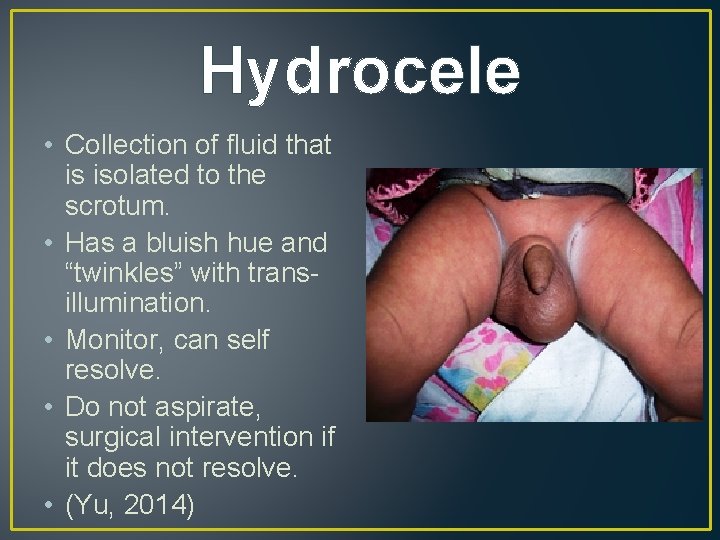
Hydrocele • Collection of fluid that is isolated to the scrotum. • Has a bluish hue and “twinkles” with transillumination. • Monitor, can self resolve. • Do not aspirate, surgical intervention if it does not resolve. • (Yu, 2014)
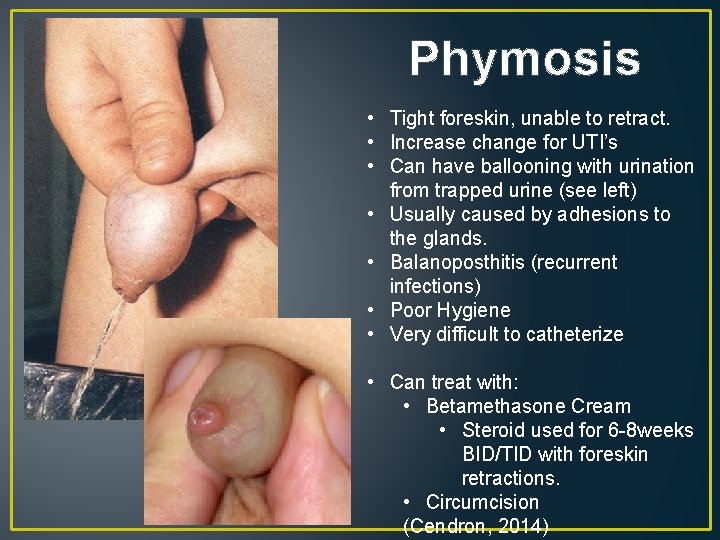
Phymosis • Tight foreskin, unable to retract. • Increase change for UTI’s • Can have ballooning with urination from trapped urine (see left) • Usually caused by adhesions to the glands. • Balanoposthitis (recurrent infections) • Poor Hygiene • Very difficult to catheterize • Can treat with: • Betamethasone Cream • Steroid used for 6 -8 weeks BID/TID with foreskin retractions. • Circumcision (Cendron, 2014)
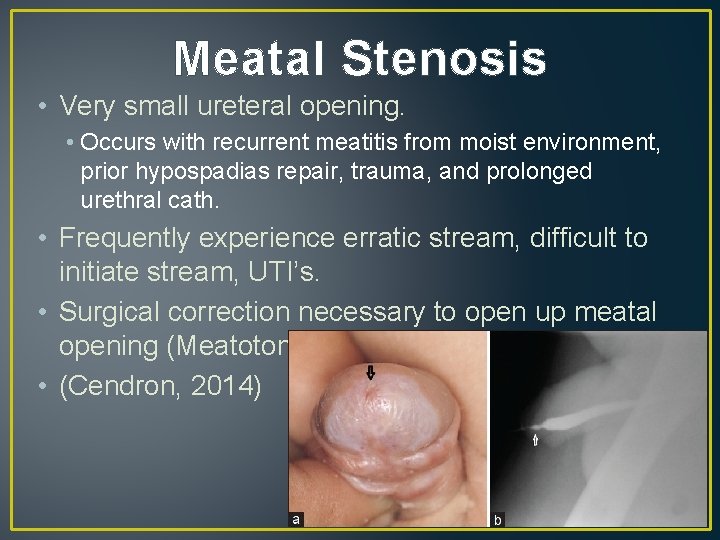
Meatal Stenosis • Very small ureteral opening. • Occurs with recurrent meatitis from moist environment, prior hypospadias repair, trauma, and prolonged urethral cath. • Frequently experience erratic stream, difficult to initiate stream, UTI’s. • Surgical correction necessary to open up meatal opening (Meatotomy). Do not dilate the urethra. • (Cendron, 2014)
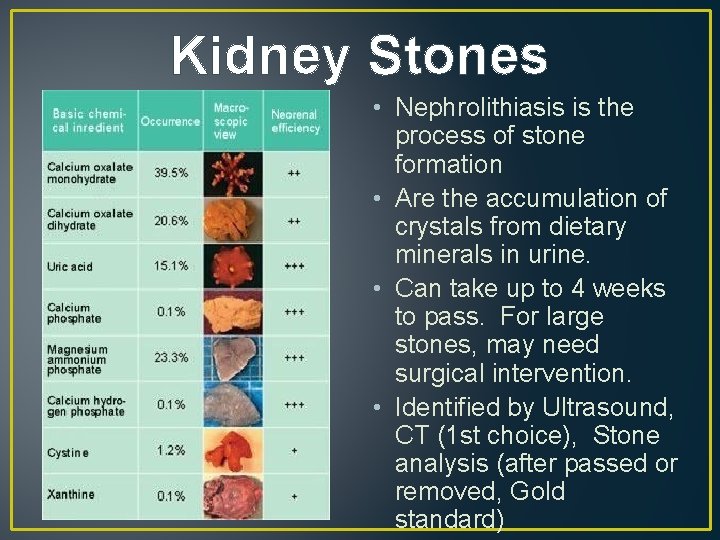
Kidney Stones • Nephrolithiasis is the process of stone formation • Are the accumulation of crystals from dietary minerals in urine. • Can take up to 4 weeks to pass. For large stones, may need surgical intervention. • Identified by Ultrasound, CT (1 st choice), Stone analysis (after passed or removed, Gold standard)
Kidney Stones, Cont. • Symptoms: • Dysurina, urinary frequency, Hematuria, Pain (flank, Lower abdomen & groin (renal Colic)), N/V, fever, UTI • Renal colic comes in waves and lasts 20 -60 min. • Uncontrolled pain must go to the ED • (Baggett, 2014) • Treatment • INCREASED FLUID INTAKE. • Decreased Salt and eggs. • Medications • Sodium citrate (increase urinary p. H, HCTZ (decrease calcium excretion), Antibiotics, Bladder relaxers (ditropan, Detrol) • Surgery: • Extracorporeal Shock Wave Lithotripsy (ESWL) • Ureteroscopy • Percutaneous
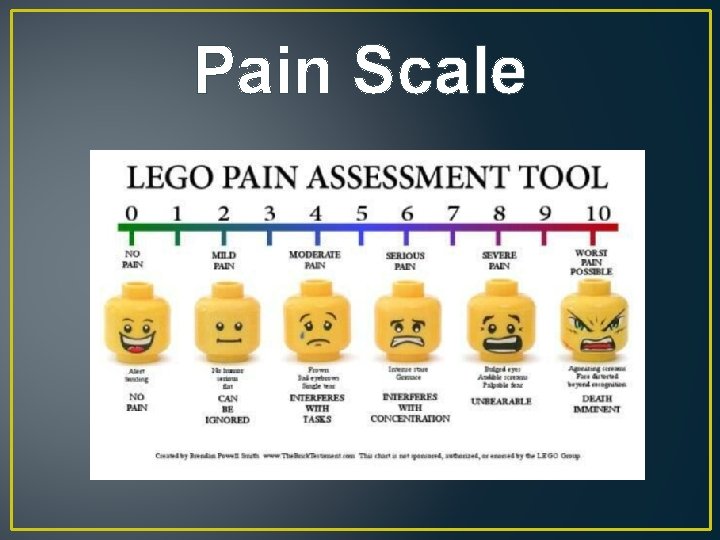
Pain Scale

Poststreptococcal Glomerulonephritis • Sudden, self-limiting, and fully resolves • Manifestations: • Hematuria (cola-colored urine), Edema (abrupt onset, mild periorbital or lower extremity), HTN, Proteinuria, usually young school aged children. • Labs: • RBCs, cast, Small Proteinurea (0 – 3+), Altered electrolytes, elevated blood urea nitrogen or creatinine levels, Elevated ASO titer or Streptozyme, decreased complement. • Management: • Supportive, Anti-hypertensives and diuretics, antibiotic treatment for active streptococcal infection, Nephrotic Syndrome • Manifestations: • Severe Proteinuria (Frothy Urine), Edema (insidious onset, massive from shift of fluid into interstitial spaces), Hypovolemia, Normotensive, Pallor, Fatigue, Usually toddler or preschool-age child. • Labs: • Protein in urine 3 -4+, Hypoalbuminemia, elevated cholesterol and triglyceride, H/H, and PLT levels. • Management: • Prednisone, diuretics, possible albumin administration, prevent infections and skin breakdown, no-added-salt diet
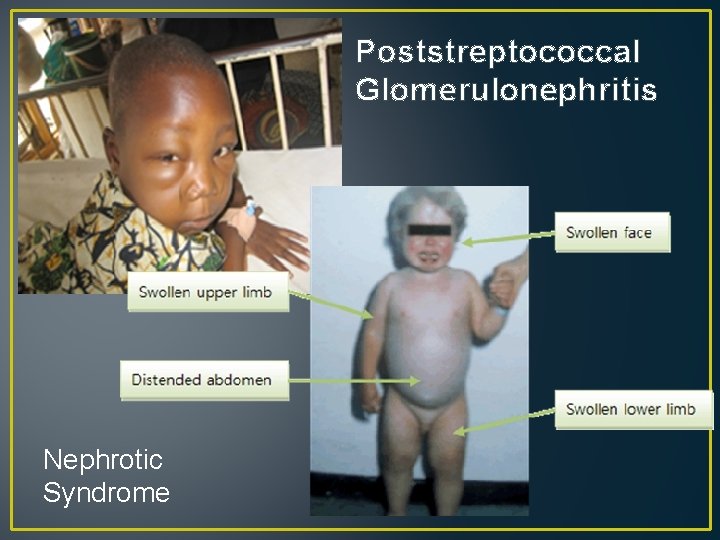
Poststreptococcal Glomerulonephritis Nephrotic Syndrome
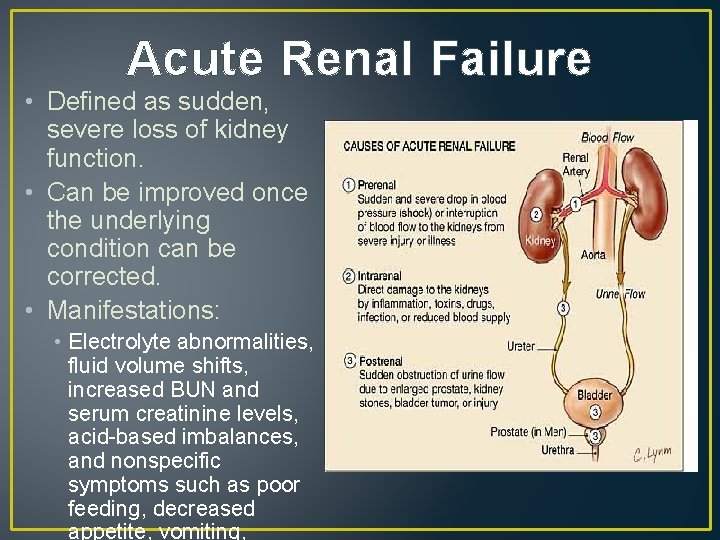
Acute Renal Failure • Defined as sudden, severe loss of kidney function. • Can be improved once the underlying condition can be corrected. • Manifestations: • Electrolyte abnormalities, fluid volume shifts, increased BUN and serum creatinine levels, acid-based imbalances, and nonspecific symptoms such as poor feeding, decreased appetite, vomiting,

End Stage Renal Disease (ESRD) • Defined as an irreversible loss of kidney function that usually occurs over months to years. • Usually caused by congenital anomalies such as obstruction, VUR, and Renal Dysplasia. • Dialysis or kidney transplantation when • Manifestations: • Electrolyte abnormalities, fluid volume shifts (dehydration or fluid overload), acid-base imbalance, renal osteodystrophy (rickets), anemia, poor growth, HTN, fatigue, decreased appetite, poor feeding, N/V and neurologic symptoms from waste accumulation in the blood.

Reference • Boston Childrens Hospital (2014). Treatment forbladder exstrophy and epispadias in children. Kids. MD Health Topics. Retrieved from http: //www. childrenshospital. org/healthtopics/conditions/b/bladder-exstrophy-andepispadias/treatments • Cendron, M. (2014). Circumcision and circumcision revision. Essential Pediatric Urology for the Pediatric Care Clinician. Boston Children’s Hospital Urology Convention. • Chowdhury, P. , Nayak, P. , Mallick, S. , Gurumurthy, S. , Deepak, D. & Mossadeq, A. (January-March 2014). Single stage ventral onlay buccal mucosal graft urethroplasty for navicular fossa stricures. Indian Journal of Urology. 30 (1). 17 -22 • Yu, R. (2014). Module III: Pediatric andrology: Swollen scrotum (Hydrocele). Essential Pediatric Urology for the Pediatric Care Clinician. Boston Children’s Hospital Urology Convention.

Reference Cont. • Baggett, A. (2014). What are kidney stones? . Boston Children’s Urology Department.
- Slides: 30