Website www drsarma in You Tube drsarmaji channel

Website: www. drsarma. in You Tube: drsarmaji channel RHEUMATOI D ARTHRITIS Prof. Dr. Sarma. R. V. S. N M. D. (Med), M. Sc. (Canada), RCGP, FIMSA Consultant Physician and Cardio-Metabolic Specialist National Professor of Medicine Visiting Faculty – Frontier Life Line Visiting Professor of Medicine – SBMC Bio. Ed Online

Rheumatoid Arthritis (RA): Definition n Progressive, systemic, Autoimmune inflammation n Often aggressive, devastating consequences n n Unknown etiology (auto immune, ? infection, smoking) Characterized by Symmetric synovitis – Chronic Polyarthritis Joint erosions, cartilage and bone destruction Multisystem - extra-articular manifestations Onset usually slow & insidious over months In 15 to 20% may have rapid or acute Aggressive management leads to good control 2

Rheumatoid Arthritis (RA): Epidemiology n Prevalence of - 0. 8% to 2. 1% of the population n Gender predilection ratio – Women: Men – 3: 1 n Prevalence increases with age – Juvenile RA n About 40 -60% have severe disease – 3 fold mortality n Median life expectancy is shortened by 3 to 7 years n Onset mostly between ages of 35 – 60 years n Genetic – HLA-DR 1( 1*0101, 0401) – Class II HCA n Exact etiology is not known 3
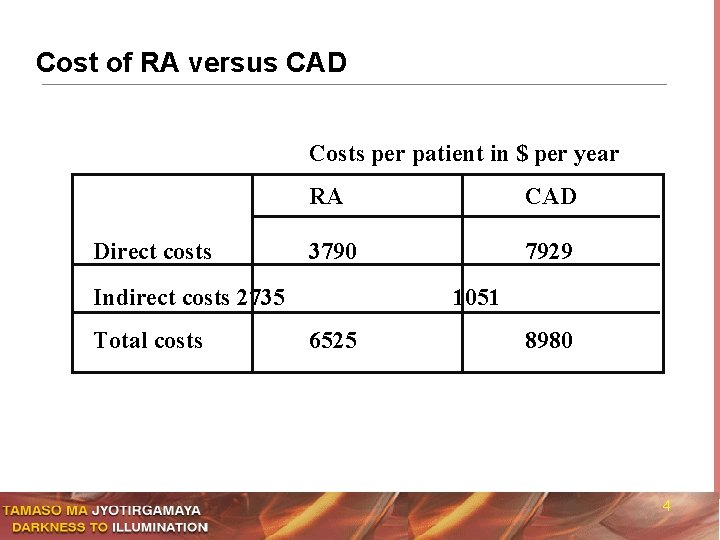
Cost of RA versus CAD Costs per patient in $ per year Direct costs RA CAD 3790 7929 Indirect costs 2735 Total costs 1051 6525 8980 4
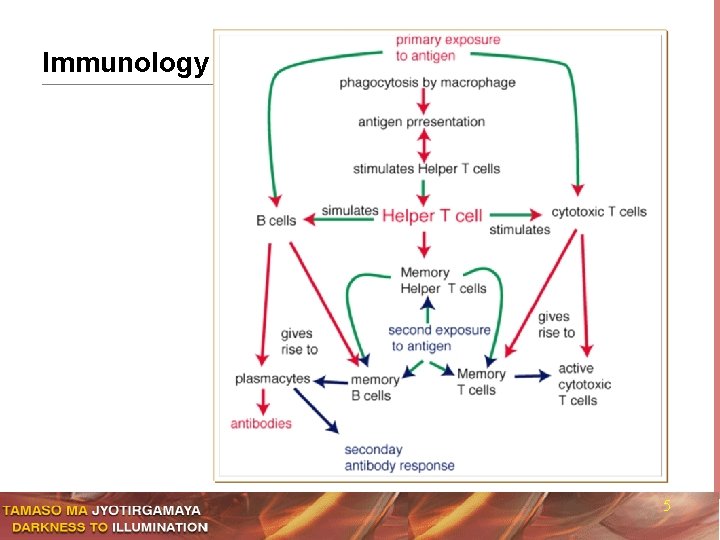
Immunology 5
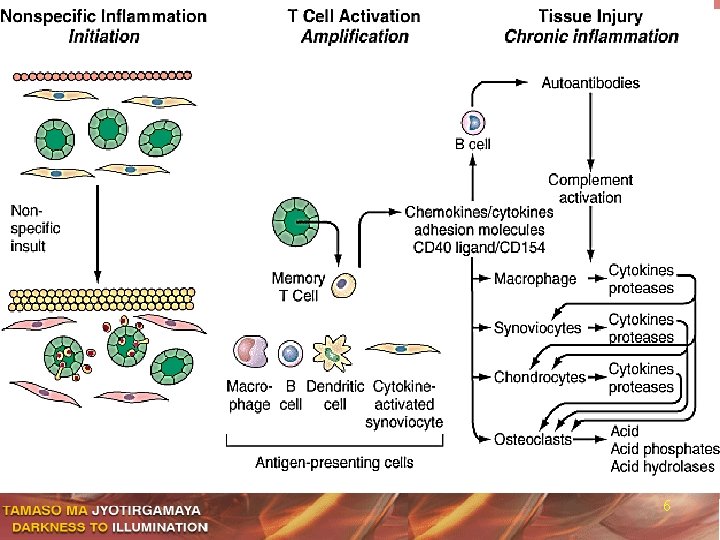
6
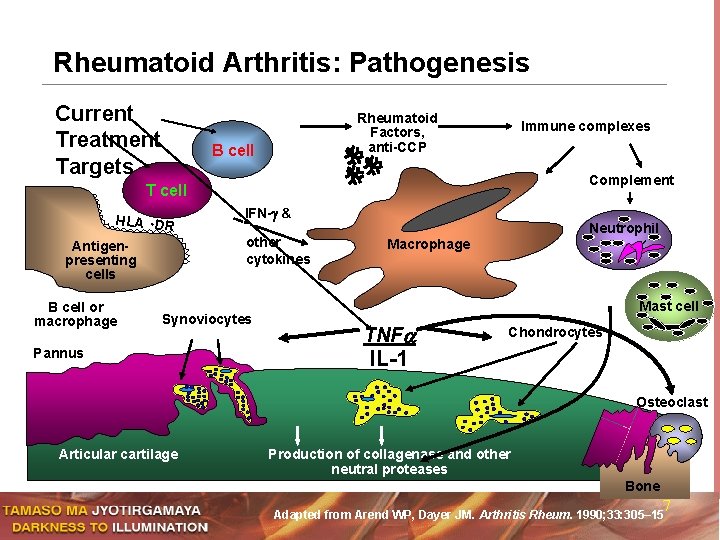
Rheumatoid Arthritis: Pathogenesis Current Treatment Targets Rheumatoid Factors, anti-CCP B cell Immune complexes Complement T cell HLA -DR other cytokines Antigenpresenting cells B cell or macrophage IFN- & Synoviocytes Pannus Neutrophil Macrophage Mast cell TNF Chondrocytes IL-1 Osteoclast Articular cartilage Production of collagenase and other neutral proteases Bone 7 Adapted from Arend WP, Dayer JM. Arthritis Rheum. 1990; 33: 305– 15
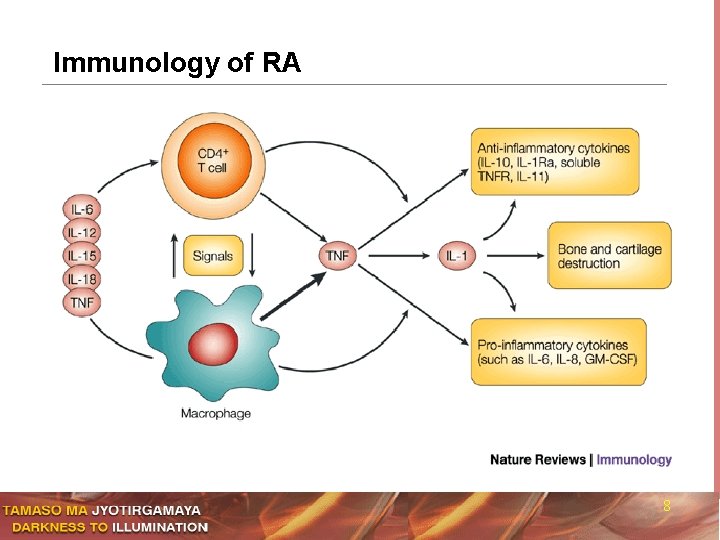
Immunology of RA 8
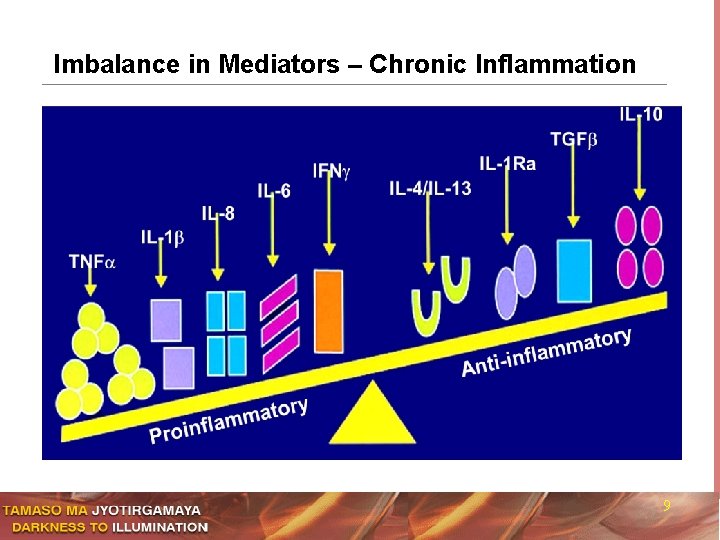
Imbalance in Mediators – Chronic Inflammation 9
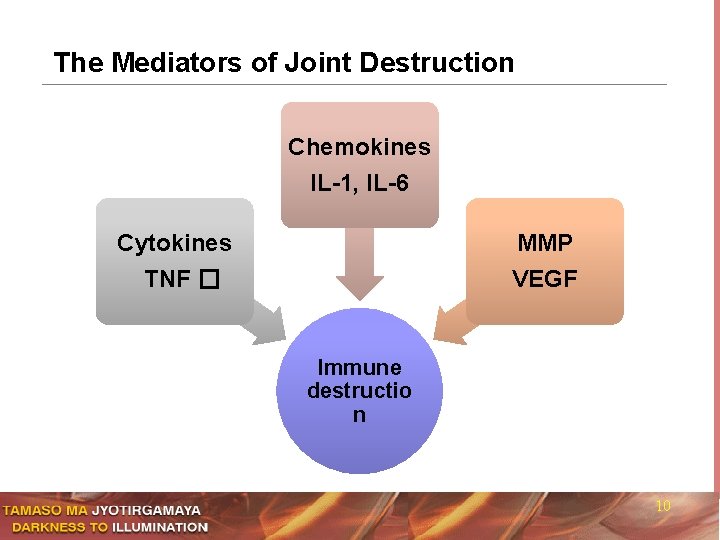
The Mediators of Joint Destruction Chemokines IL-1, IL-6 Cytokines MMP TNF � VEGF Immune destructio n 10

The Natural Course of RA Severe RA with Deformities Early RA – Mild Disease Undifferentiated Polyarthritis 11
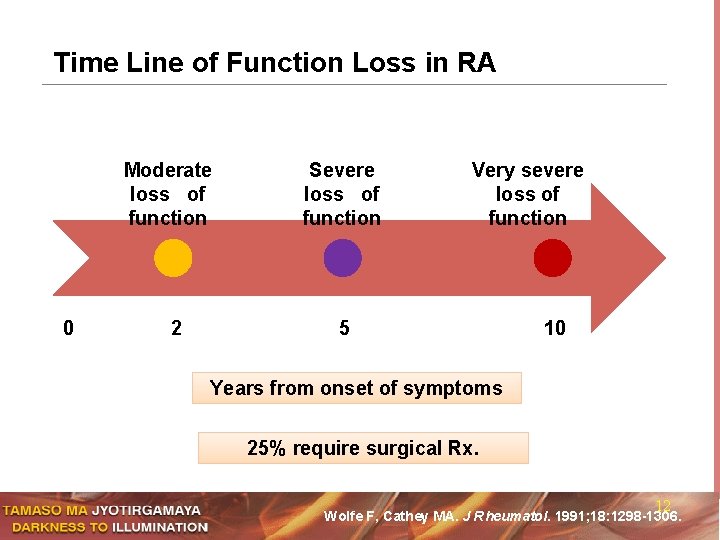
Time Line of Function Loss in RA Moderate loss of function 0 2 Severe loss of function Very severe loss of function 5 10 Years from onset of symptoms 25% require surgical Rx. 12 Wolfe F, Cathey MA. J Rheumatol. 1991; 18: 1298 -1306.

Rheumatoid Arthritis: Diagnosis - ACR Criteria n Four or more of the following criteria must be present: n Morning stiffness > 1 hour n Arthritis of > 3 joint areas of the possible 28 joints n Arthritis of hand joints (MCPs, PIPs, wrists) n Symmetric swelling (arthritis) – same joints on both sides n Serum rheumatoid factor – RA Factor (antibody to Ig. G) n Rheumatoid nodules n Radiographic changes n First four criteria must be present for 6 weeks or more 13

Rheumatoid Arthritis: Typical Involvement n Wrist joints and MCP joints - very commonly involved n Index and middle Metacarpophalangeal joints n Proximal interphalangeal joints (PIP) n Metacarpophalangeal joints (MCP) n Metatarsophalangeal joints (MTP) n Elbows, Shoulders n Knees, Ankles, Hips. Lumbosacral area is not involved n Spine: only Atlanto-axial joint (C 1– C 2), subluxation n Terminal interphalangeal (TIPS) joints are not involved 14 n
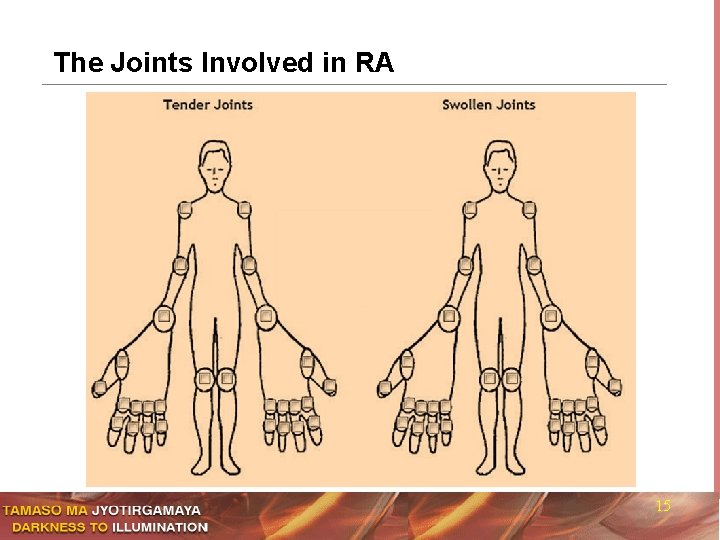
The Joints Involved in RA 15

DAS 28 (Disease Activity Scoring) for RA EULAR n Calculated using a formula that includes n Counts for tender and swollen joints – (28 joints) n General health by the patient (on a scale of 0 to 100) n A measurement of ESR or CRP n Score > 5. 1 – High disease activity, n Score 5. 1 to 3. 2 – Moderate disease activity n Score < 3. 2 – Low disease activity n Score < 2. 6 – Being in Remission n Response to Rx. – of ≥ 1. 2 – Good and < 0. 6 – Poor European League Against Rheumatism (EULAR) 16

Rheumatoid Arthritis – ACR Functional Classes Classification Specifications of activity levels Class I Complete ability to perform daily activities self-care, vocational and avocational Class II Ability to perform usual self-care and vocational activities; limited avocational activities Class III Ability to perform usual self-care activities; limited vocational or avocational activities Class IV Limited ability to perform usual self-care or vocational or avocational activities 17

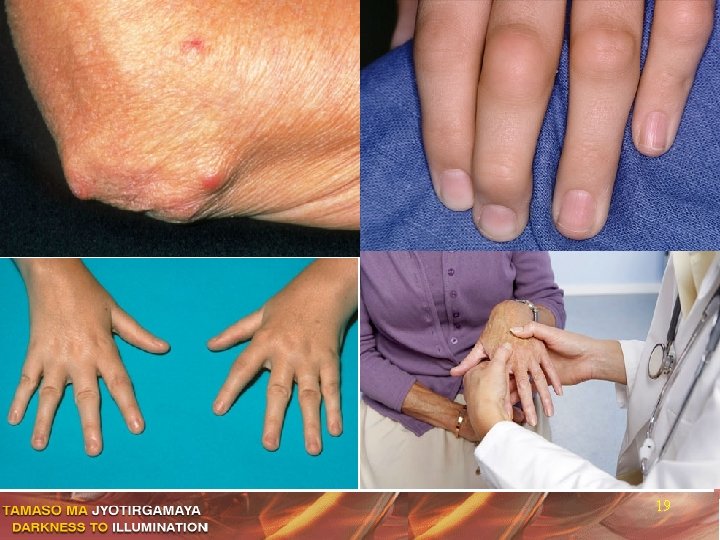
Extra Articular Manifestations of RA Systemic involvement Special Features Musculoskeletal wasting Episcleritis, Scleromalacia Tenosynovitis, Bursitis Pleural effusion, Nodules Osteoporosis, Rh nodules Cervical cord compression Vasculitis, Arteritis Pericarditis, Myocarditis Mononeutitis, carpel tunnel Felty’s syndrome, Caplan’s 18
19
20
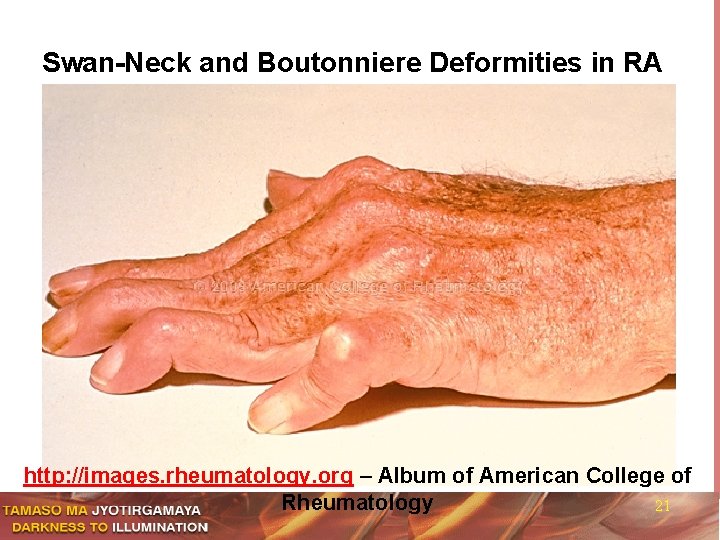
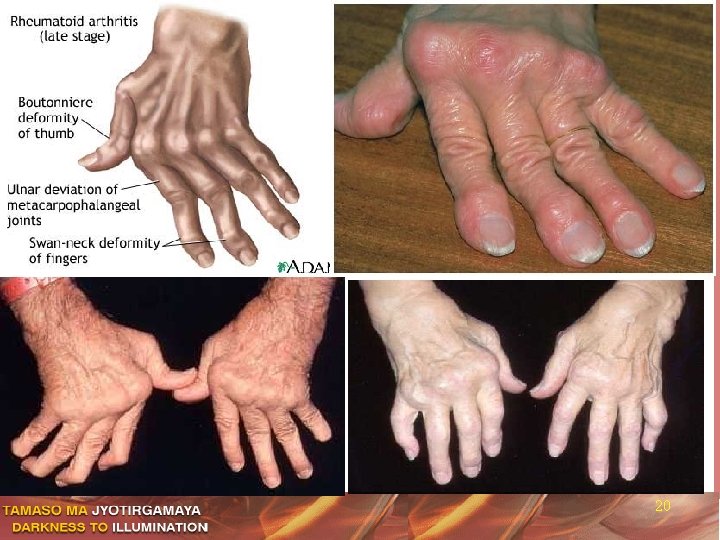
Swan-Neck and Boutonniere Deformities in RA http: //images. rheumatology. org – Album of American College of Rheumatology 21
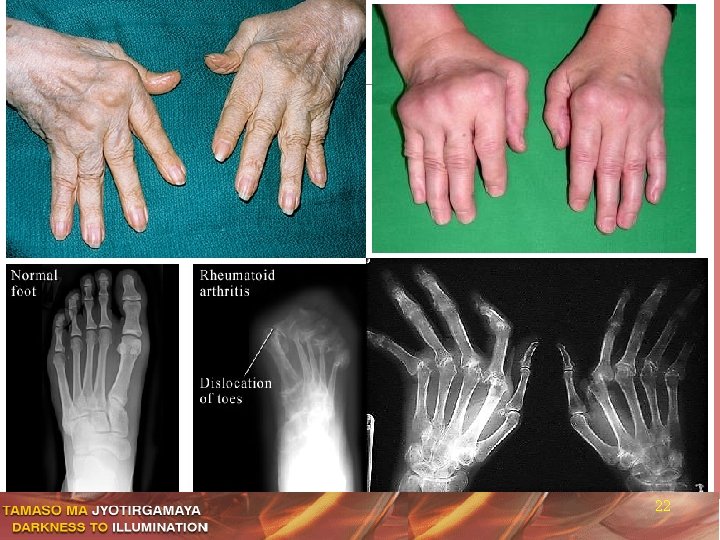
22
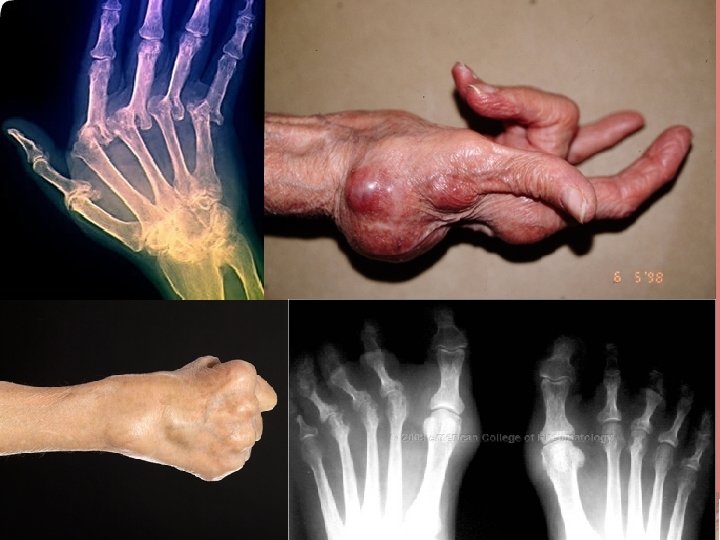
23
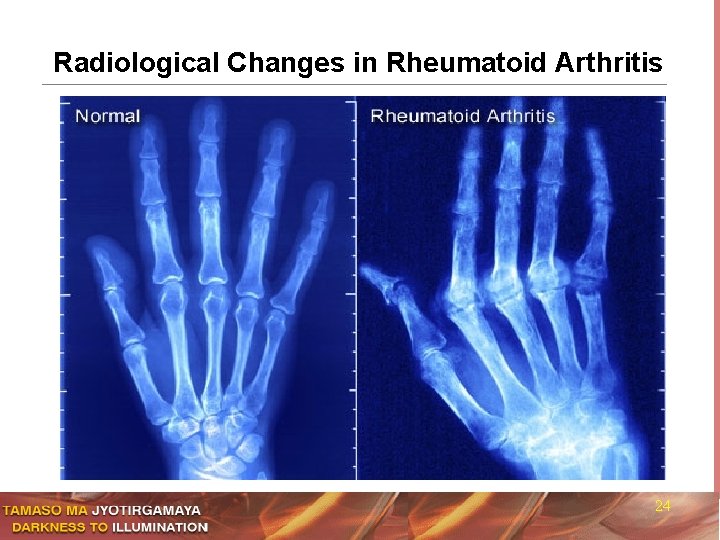
Radiological Changes in Rheumatoid Arthritis 24
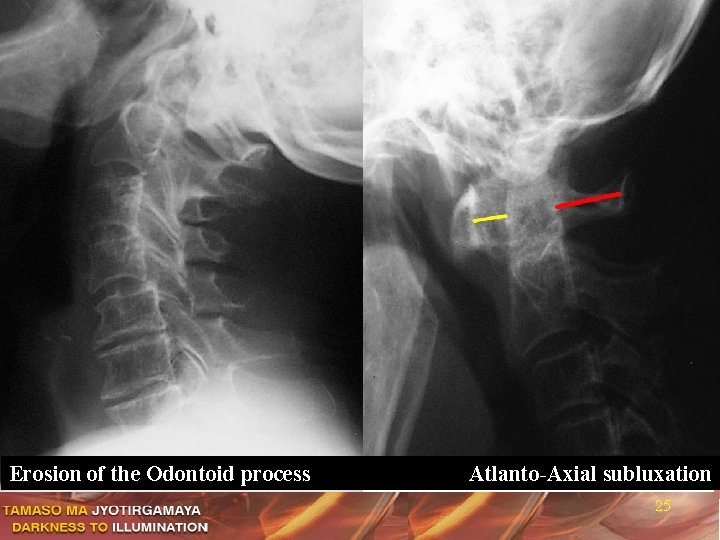
Erosion of the Odontoid process Atlanto-Axial subluxation 25

Blood Parameters in RA n Acute Phase Reactants (APR ) n C-Reactive Protein (CRP) - > 4 mg% n It is the single most useful marker ESR is raised > 30 mm – other confounders n Ceruloplasmin n Haptoglobin (Hp) n n Leukocytosis, Nutrophilia n Normocytic normochromic anemia n Thrombocytosis 26

Synovial Fluid in RA n No need in general for joint aspiration n Required to exclude other causes of arthritis n Inflammatory arthritis picture n Turbid fluid with reduced viscosity n Increased protein content n Decreased glucose content n WBC count from 2, 000 to 50, 000/ l n PMNLs predominate n Total compliment, C 3 and C 4 are markedly 27

Rheumatoid Factor (RA Factor) n Developed by Eric Waller in 1937 – Rose Waller Test n Agglutinating Abs - Latex particle agglutination assay n Isotype specific enzyme immunoassays – New technique n n Antibodies to Fc portion of our own Ig. G - These Abs are Ig. M Positive in 5% of normal persons and in only 70 -80% of RA n Low specificity (false +ves) & low sensitivity (false –ves. ) n It is not a screening or Dx. tool – More a prognostic tool n It is negative in 30% cases of RA – Sero negative RA n RF are commonly seen other disease – see next slide 28

Positive Rheumatoid Factor is seen in: Disease Frequency Advanced Rheumatoid Arthritis 100% Rheumatoid Arthritis (over all) 70% Sjögren's syndrome 90% Systemic Lupus Erythematosis (SLE) 30% Sub acute bacterial endocarditis (SABE) 40% Tuberculosis 15% Old Age 20% Normal healthy individuals 5% 29

Anti-CCP Antibody Test in RA (ACPA) n Antibodies to Cyclic Citrullinated Peptides (anti-CCP) n Similar sensitivity for RA (70%) n Specificity for RA (>95%) better than RA Factor n In early polyarthritis anti-CCP are useful for Dx. n Anti-CCP are associated with more severe disease n They spell a poor prognosis and rapid progression n They may be positive in asymptomatic patients years before the onset of symptoms 30

Serology in Rheumatoid Arthritis Test RA Factor is Ig. M Antibody to the Fc portion of the Ig. G Anti CCP: Antibodies to Cyclic Citrullinated Peptides 31

Differential Diagnosis of RA n Connective tissue diseases - Scleroderma and SLE n Fibromyalgia, Palindromic Rheumatism n Infectious endocarditis, Acute Rheumatic Fever n Poly articular gout n Polymyalgia Rheumatica n Sarcoidosis, Hemochromatosis n Sero negative spondylo arthropathies n n Reactive arthritis - evaluate for psoriasis, Reiter’s, IBD Still’s disease, Thyroid disease, Viral arthritis 32

Rheumatoid Arthritis v/s Osteoarthritis Feature Rheumatoid Arthritis Osteoarthritis Pathology Autoimmune Degenerative Age Any age – usually 35+ Increases with age Joints involved Small joints MCP, PIP Large joints, TIP Spine (Axial) C 1 -C 2 - Subluxation Lumbosacral Extra articular Many systemic effects Few systemic effects Course Rapidly progressive Slowly progressive Disability Highly disabling Mild to moderate 33
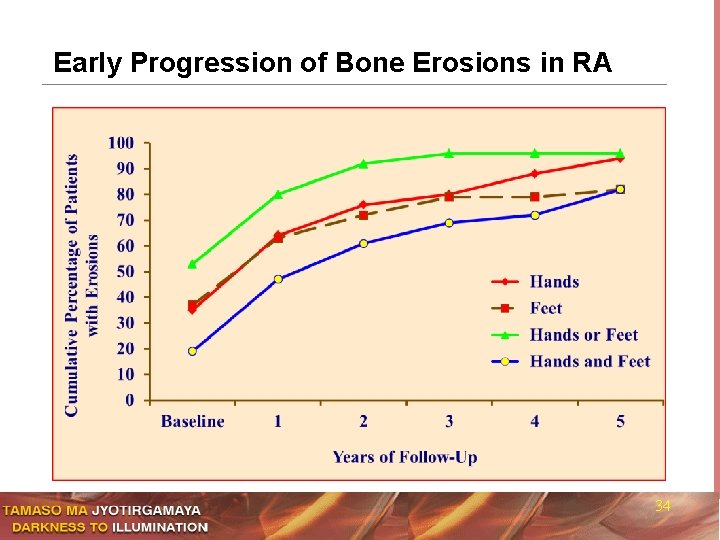
Early Progression of Bone Erosions in RA 34

Rheumatoid Arthritis: Predictors of Prognosis n Presence of > 20 inflamed joints n Markedly elevated ESR n Radiographic evidence of bone erosions n Higher class of functional disability n Persistent inflammation; comorbidities n Advanced age of onset n Low socio-economic status, low education level n HLA-DR *0401 or DR *0404 40%-85% of RA pts unable to work in 8 n Presence of rheumatoid nodules 10 years n High titers of RA Factor and anti CCP 35

Rheumatoid Arthritis: Complications n Carpal tunnel syndrome, n Baker’s cyst, Subcutaneous nodules, n Systemic Vasculitis, n Sjögren’s syndrome, n Peripheral neuropathy, n Cardiac and pulmonary involvement, n Felty’s syndrome, and anemia n Risk of lymphomas three times greater n Risk of infection due to disease and treatment 36

Goals of Therapy 1. Relief of pain 2. Reduction of inflammation 3. Protection of articular structures 4. Maintenance of functional activity 5. Control of systemic involvement 6. Slow the progression of disease 7. Increase the over all quality of life 37

Non Pharmacological Management n Rest n Exercise n Flexibility/stretching n Muscle conditioning n Cardiovascular/aerobic n Diet n Weight management n Physical and occupational therapy 38

Therapeutic Window of Opportunity n n Erosive changes occur early in disease Even a brief delay of therapy can have a significant impact on disease parameters years later n Early DMARD treatment to arrest progression n MTX is the sheet anchor – Combination of DMARDs n Bridge the gap initially with NSAID and GC n Biologics only for refractory case – with caution; cost n Surgical treatment options in selected patients O’Dell JR. Arthritis Rheum. 2002; 46: 283 -285. Van der Heijde DM. Br J Rheum. 1995; 34 (suppl 2): 74 -78.

Therapeutic Window of Opportunity n n Erosive changes occur early in disease Even a brief delay of therapy can have a significant impact on disease parameters years later Surgical Treatment will be mandated in n Early DMARD treatment to arrest progression 25% n MTX is the sheet anchor – Combination of DMARDs n Bridge the gap initially with NSAID and GC n Biologics only for refractory case – with caution; cost n Surgical treatment options in selected patients O’Dell JR. Arthritis Rheum. 2002; 46: 283 -285. Van der Heijde DM. Br J Rheum. 1995; 34 (suppl 2): 74 -78.

Medical Management – Drug Classes NSAIDs – Cox-1 & Cox-2 inhibitors Glucocorticoids – Prednisolone, MP IAS – Intra articular steroids DMARDs – MTX, SSZ, HCQ, CQ Immunosuppressive Rx. – AZT, Leflunomide, CS Cytotoxic agents – Cyclophosphamide Biologics – TNF-�antibodies, IL-1 R antagonist Old drugs – Gold salts, D-Penicillamine 41

NSAIDS in RA n NSAIDs COX 1 COX 2 Constituent pathway Inducible pathway Renal and GI homeostasis Inflammation Selective COX 2 Inhibitors n Improved GI tolerability n Reduced effects on RBF n No effect on platelets n n n Called as COXIBs May have adverse effect on heart Celecoxib Etoricoxib Meloxicam 42

NSAID Class of Drugs Non Selective NSAIDs used as analgesics n Ibuprofen n Ketorolac n Ketoprofen n Aspirin (NSAID) n Diclofenac Selective COX-2 n Aceclofenac n Celecoxib, Etoricoxib n Piroxicam n Meloxicam n Lornaxicam Analgesics n Naproxen n Tramadol n Indomethacin n Paracetamol 43

Pros and Cons of NSAID Therapy PROS n n n Effective control of inflammation and pain Effective reduction in swelling CONS n n n Improves mobility, flexibility, range of motion n Improve quality of life n Relatively low-cost Does not affect disease progression GI toxicity common Renal complications (eg. Irreversible renal insufficiency, papillary necrosis) n Hepatic dysfunction n CNS toxicity 44

Pros and Cons of Corticosteroid Therapy PROS n n n Anti-inflammatory and immunosuppressive effects Can be used to bridge gap between initiation of DMARD therapy and onset of action Intra-articular steroid (IAS) injections can be used for individual joint flares CONS n n Does not conclusively affect disease progression Tapering and discontinuation of use often unsuccessful Low doses result in skin thinning, ecchymoses, and Cushingoid appearance Significant cause of steroidinduced osteopenia 45

Methotrexate (MTX) n n n n n MTX is given 10 to 30 mg orally, IM, or SC per week It is DHF reductase inhibitor – Supplemental folic acid The clinical improvement takes one to two months Nausea, diarrhea; mouth ulcers; rash, alopecia; Abnormal LFT Rare: low WBC & platelets; pneumonitis; sepsis; liver disease; EBV related lymphoma; CBC, creatinine, and LFTs monthly for six months, then every one to two months; repeat AST or ALT in two to four weeks if initially elevated, and adjust dose as needed; Rapid onset (six to 10 weeks); tends to produce more sustained results over time than other DMARDs and lowers all-cause mortality; Can be used when cause of polyarthritis uncertain; Often combined with other DMARDs like Leflunomide, SSZ, HCQ 46
Changing Paradigm of Treatment Evolving paradigm Current Treatment Traditional DMARDs • Early Aggressive Rx. • Biological • Combination treatment 47
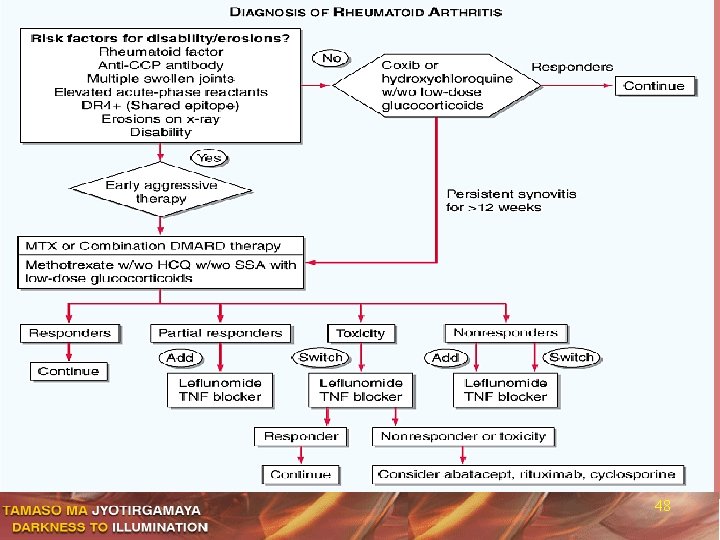
48
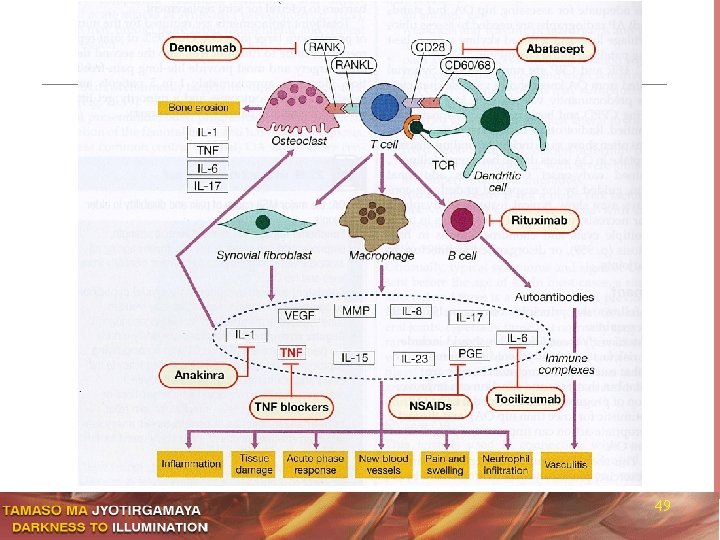
49
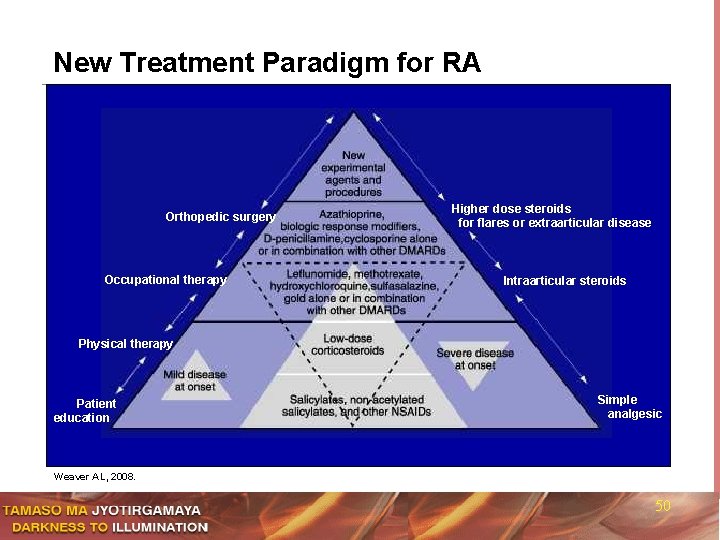
New Treatment Paradigm for RA Orthopedic surgery Occupational therapy Higher dose steroids for flares or extraarticular disease Intraarticular steroids Physical therapy Patient education Simple analgesic Weaver AL, 2008. 50

Biological Agents in RA n n n TNFα antagonists n Adalimumab (Humira) n Etanercept (Enbrel) n Infliximab (Remicade) Interleukin-1 antagonist n Anakinra (Kineret) Suppressors of T-Cell activation n n Abatacept (Orencia) Anti B-Cell monoclonal antibody n Rituximab (Rituxan) 51
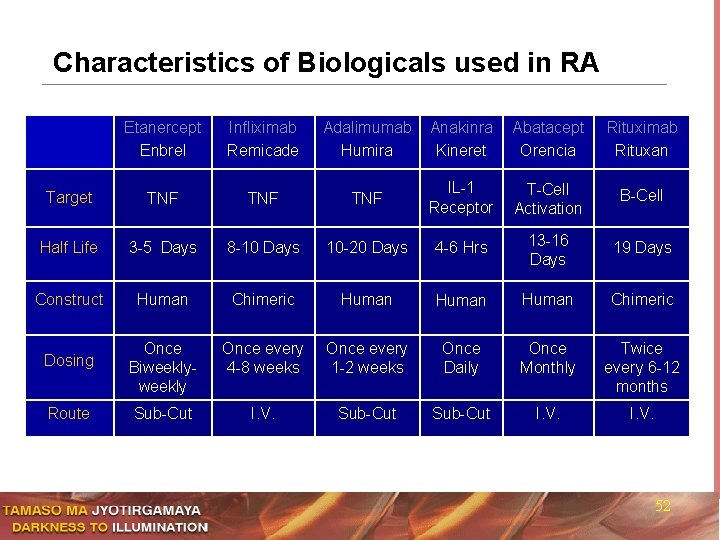
Characteristics of Biologicals used in RA Etanercept Enbrel Infliximab Remicade Adalimumab Humira Anakinra Kineret Abatacept Orencia Rituximab Rituxan Target TNF TNF IL-1 Receptor T-Cell Activation B-Cell Half Life 3 -5 Days 8 -10 Days 10 -20 Days 4 -6 Hrs 13 -16 Days 19 Days Construct Human Chimeric Human Chimeric Dosing Once Biweekly Once every 4 -8 weeks Once every 1 -2 weeks Once Daily Once Monthly Twice every 6 -12 months Route Sub-Cut I. V. 52

Biologics: Relative Contraindications n Active Hepatitis B Infection n Multiple sclerosis, optic neuritis n Active serious infections n Chronic or recurrent infections n Current neoplasia n History of TB or evidence of Koch’s n Congestive heart failure (Class III or IV) 53

Safety Considerations of Biologicals n n Serious Infections Opportunistic infections (TB) n Malignancies/lymphoma n Demyelination n Hematologic abnormalities n Administration reactions n Congestive heart failure n Hepatic n n Autoantibodies and drug induced lupus Vaccination 54

www. drsarma. in THANK YOU ALL Bio. Ed Online
- Slides: 55