Webinar Innovations in Screening Brief Intervention Substance Use

Webinar: Innovations in Screening, Brief Intervention & Substance Use Education for Health Professionals February 25, 2015, 3 -4 pm ET

Agenda: 1) Challenges and best practices in conducting SBIRT (15 min) 2) Benefits of using virtual humans in the development and assessment of SBIRT (5 min) 3) Demo of At-Risk in Primary Care + Research results (15 min) 4) Overview of SAMHSA’s SBIRT RFA (5 min) 5) Q&A (10 min) Dr. Eric Goplerud SVP and Director Public Health Department NORC at the University of Chicago Dr. Tracy Mc. Pherson Senior Research Scientist Public Health Department NORC at the University of Chicago Ron Goldman Co-Founder & CEO Kognito

SBIRT Implementation, Benefits, and Challenges: Opportunities to Enhance Implementation and Training using Technology Tracy L. Mc. Pherson, Ph. D NORC at the University of Chicago

Presenter Tracy L. Mc. Pherson, Ph. D Senior Research Scientist Public Health Research NORC at the University of Chicago National SBIRT ATTC BIG SBIRT Initiative Adolescent SBIRT SW & Nursing Learning Collaborative Mc. Pherson-Tracy@norc. org Esap 1234@gmail. com

Agenda § Why SBIRT? § Implementing SBIRT § Challenges § Hot spots § Training Challenges, Opportunities, and Resources § Conrad Hilton Adolescent SBIRT Project

Why SBIRT? Substance use is a public health and safety issue. Substance use has a profound impact on patients/clients and their families: • Cause or exacerbate health conditions • Poorly managed health conditions • Reduce effectiveness of medications • ER visits and excess hospital stays • Accidents and damage • Injuries and violence • Lower productivity, lost work days • Worker compensation , disability, worker turnover • Financial and legal problems • Family disruptions and relationship problems • Sexual risk-taking • Overdose and suicide
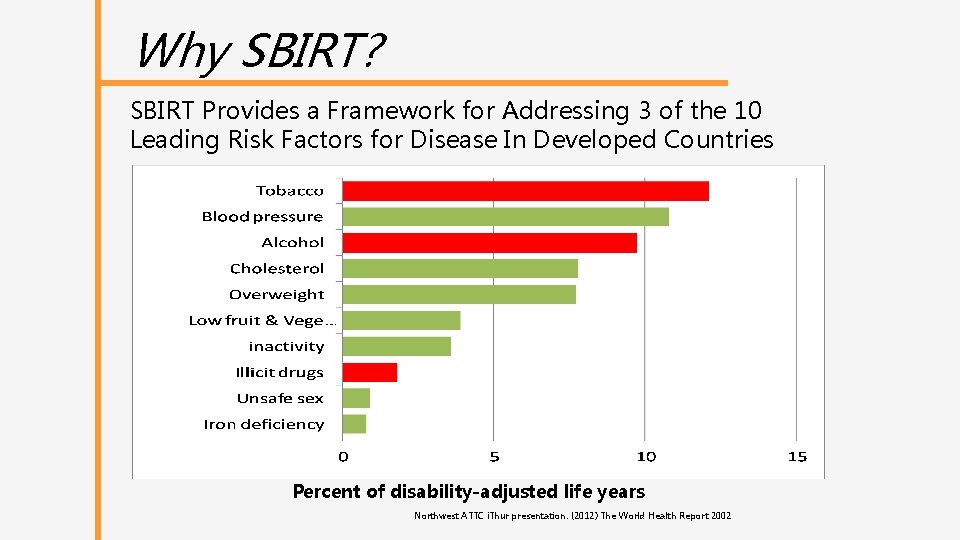
Why SBIRT? SBIRT Provides a Framework for Addressing 3 of the 10 Leading Risk Factors for Disease In Developed Countries Percent of disability-adjusted life years Northwest ATTC i. Thur presentation: (2012) The World Health Report 2002
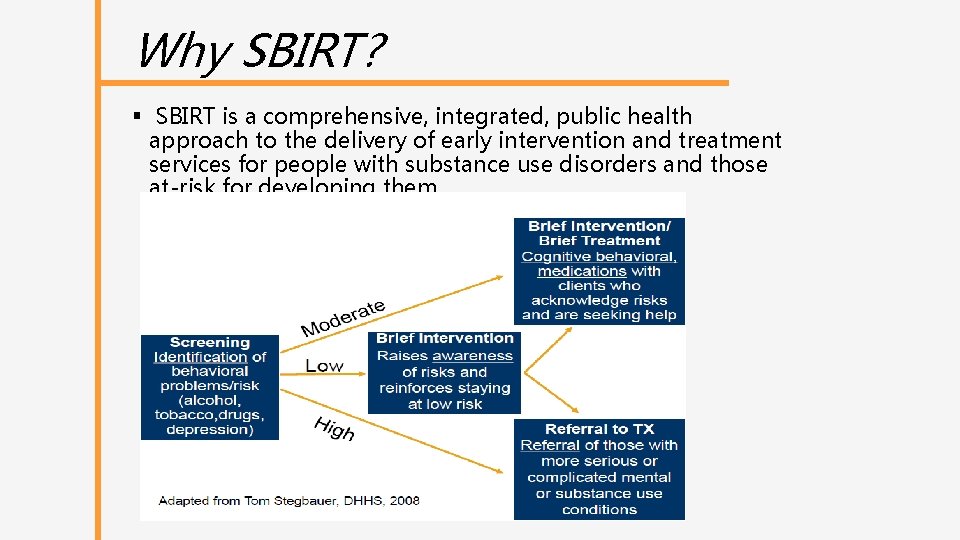
Why SBIRT? § SBIRT is a comprehensive, integrated, public health approach to the delivery of early intervention and treatment services for people with substance use disorders and those at-risk for developing them.
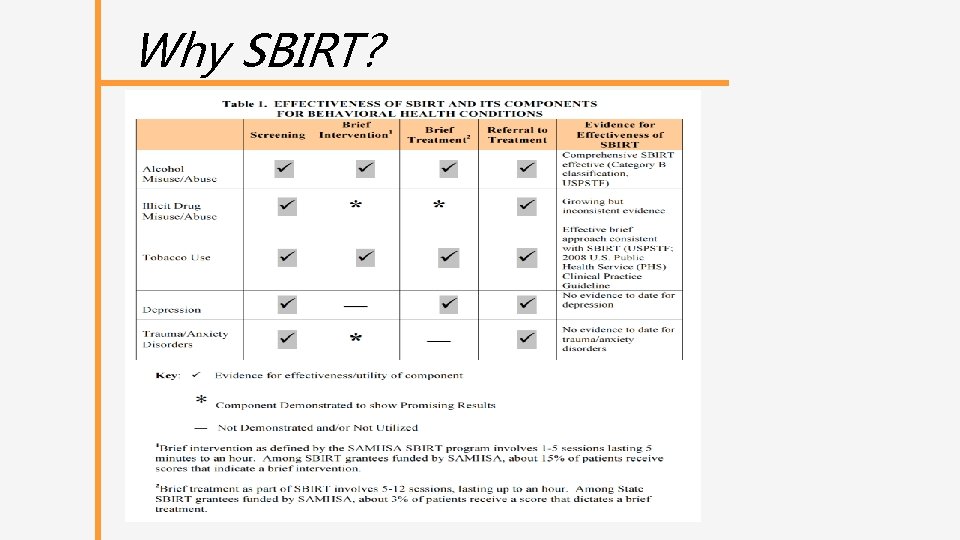

Why SBIRT?

Why SBIRT? SBIRT Aims To: • Increase early identification of patients/clients atrisk for SU problems. • Build awareness and educate patients/clients on U. S. guidelines and risks associated with SU. • Motivate those at-risk to reduce unhealthy, risky SU; and adopt health promoting behavior. • Motivate individuals to seek help and increase access to care for those with (or at risk for) a SUD. • Foster a continuum of care by integrating prevention, intervention, and treatment services.

In a nutshell: Why SBIRT? At-risk drinking and alcohol problems are common Alcohol and other drugs significantly impact patient and public health SBIRT is proven to be effective Source – SBIRT Oregon Residency Program, 2012 Substance use is one of America’s top preventable health issues

Implementing SBIRT can be implemented in a range of settings: • Primary care • Federally Qualified Health Centers • Trauma • Drug Courts, Juvenile Justice • Emergency Department • Dental Clinics • Hospital Inpatient • HIV Clinics • Employee Assistance Programs • Colleges/Universities • Health Promotion and Wellness Programs • Peer Assistance Programs • Occupational Health and Safety, Disability Management • Community Mental Health Centers • School-based Health Centers • Addiction Treatment • Counseling/Therapy • Health Professional Training Programs

Hot Spots of SBIRT Implementation Hot Spot 1: Hospitals

Screening and Treating Acutely Ill and Injured Patients with Comorbid Substance Use Cochrane Collaboration review (Mc. Queen et al, 2011) 14 RCTs, adults and adolescents Outcomes favor BI over non-treatment controls • Significant drop in 6 month alcohol consumption • Significant drop in alcohol consumption at 9 months • Self Report at 1 year favor BI • Significantly fewer deaths at 6 months and 1 year

Salina Regional Health Center Outcomes • 199 Bed Acute Care Regional Health Center-Level III Trauma Center • 27, 000 ED presentations per year • Alcohol/Drug DRG was 2 nd most frequent re-admission Services provided ü 24 -7 coverage of ED ü Full time SUD staff on medical and surgical floors ü Warm hand off provided to all SUD/MH services ü Universal Screening and SBI beginning in 2013 • Re-admission DRG moved from 2 nd to 13 th. • 70% of alcohol/drug withdrawal LOS were 3 days or less. • 83% of SUD patients triaged in ED were not admitted. • 58% of patients recommended for further intervention attended first two appointments (warm hand off). • Adverse patient and staff incidents decreased by 60%. • CKF detox admissions increased 450% in first year. • 300% increase in commercial insurance reimbursement.

Hot Spot 2: Prenatal Screening and Case Management

Kaiser –Permanente Northern California’s Early Start Program A transformational program that is cost beneficial • Universal Screening of ALL pregnant women • Screening questionnaire • Urine toxicology (with consent) • Place a licensed mental health provider in the department of OB/GYN • Link the Early Start appointments with routine prenatal care appointments • Educate all women and providers

Rate of Preterm Delivery (<37 Weeks) Note: The rate of Preterm Delivery is 2. 1 times higher in S group than SAF (Early Start patients)
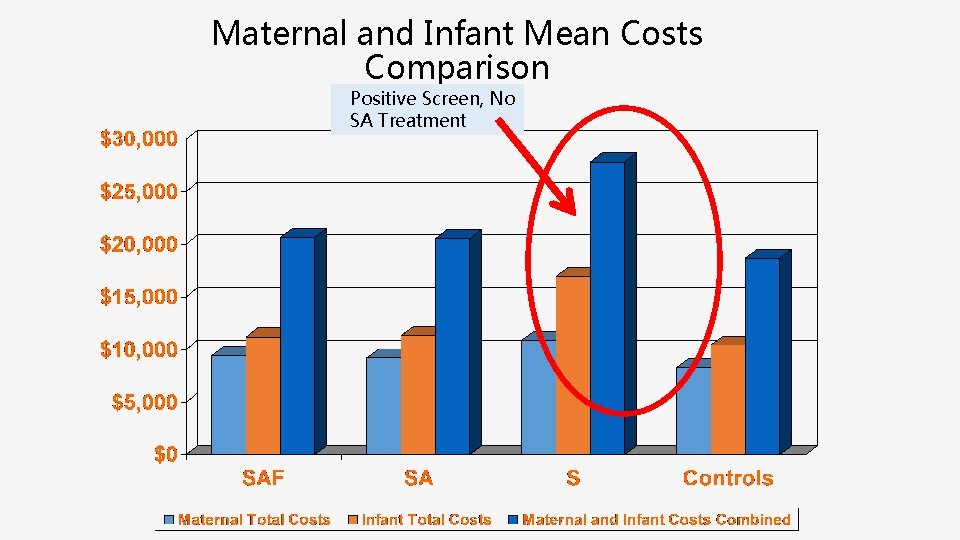
Maternal and Infant Mean Costs Comparison Positive Screen, No SA Treatment

Hot Spot 3: Youth and Young Adult High Risk Users

Teen and Young Adult School Health and Ambulatory Health SUD Treatment • Data were pooled from 16, 915 adolescents from 148 local CSAT-funded programs and followed quarterly for 6 to 12 months. • In 2009 dollars, adolescents averaged $3, 908 in costs to taxpayers in the 90 days before intake ($15, 633 in the year before intake). • This would be $3. 9 Million per 1, 000 adolescents served. • Within 12 months, the cost of treatment was offset by reductions in other costs producing a net benefit to taxpayers of $4, 592 per adolescent.

Hot Spot Webcasts • Kansas (Substance Use Treatment-Hospital Partnership) http: //hospitalsbirt. webs. com/partnershipsimplementing. htm • Early Start Program at Kaiser (OB/GYN) http: //hospitalsbirt. webs. com/hospitalalcoholpregnancy. htm Hear about other models: • Gosnold on Cape Cod (Addiction Treatment-Hospital Partnership) http: //hospitalsbirt. webs. com/hospitalalcoholpregnancy. htm • Southwest Virginia Community Health Systems (FQHC) http: //hospitalsbirt. webs. com/health-centers-sbirt • Cook County (Criminal Justice) http: //hospitalsbirt. webs. com/criminaljusticesbirt. htm

Challenges of Implementing SBIRT “We don’t have time. We already do 50 million things…. How can we do one more? ” “We aren’t trained to address substance use and we don’t have the resources to get our staff trained…We can’t take our staff offline. ” “Our patients have more pressing concerns than substance use. It’s not that important compared to the other issues they face like diabetes, heart disease, or depression. ”

Challenges of Implementing SBIRT • Scalability – its not a one size fits all • Facility specific – it does boil down to how will it work at each site • Common barriers – design specific & site specific • Training – all settings need initial and boosters, fidelity and proficiency monitoring in all settings, with all types of practitioners

Challenges of Implementing SBIRT Common barriers • Lack of awareness, skills, and knowledge about screening tools • Discomfort initiating discussions about AOD use/misuse • Belief of not having enough time to carry out interventions • Uncertainty about referral resources • Limited or lack of insurance company reimbursement • Negative attitudes toward substance abusers • Pessimism about the efficacy of treatment • Fear of losing or alienating patients • Lack of simple guidelines for brief intervention • Lack of education and training about the nature of addiction or addiction treatment, and how to effectively screen and

Overcoming Challenges – Prep, Prep • • • Do a strengths assessment Do a work flow analysis Define target population Develop clear practice guidelines Develop a charting/documentation protocol Develop a billing strategy Develop a data collection, storage, and analysis plan Develop a quality improvement initiative (fidelity/quality) Establish a referral network Develop a training plan (get buy-in before you train) Identify technology to facilitate practice (EHRs, tablets, e. SBI) Identify technology to facilitate training (Interactive simulations, On- Demand courses/webinars) Don’t recreate the wheel. Identify and use resources and technology that enhance what you’re doing.

SBIRT Training Face-to-face SBIRT training – Most common • Often seen as the only or best way • Varies dramatically from a 1 hour didactic presentation to 2+ day workshop • Often a “one shot deal” • One shot deals don’t allow for real world practice and ongoing feedback, coaching, or booster sessions • May not offer enough observational /vicarious learning • May offer few opportunities practice • May not offer sufficient feedback • Can be costly – to individuals or organizations • Often small training budgets limit the number of staff who can participate • Requires staff to be taken “off line” • May require staff to travel

SBIRT Training Face-to-face training can be enhanced by other learning opportunities: • Use of actors as standardized patients (can be expensive) • On-Demand courses (often free /low cost; typically underutilized/unknown) • Live and recorded webinars - specific settings, populations, or general/ overview (often free/low cost; typically underutilized/unknown) • Use of e-SBI platforms and tablet-based applications to learn, practice and facilitate SBI with patients/clients (e. g. , Radiant Interactive Behavioral Health Risk Assessment Check-up) • Use of interactive web-based patient/client simulation technology – allows user to practice competencies and receive feedback, provides boosters/refreshers, assesses skill acquisition (new state of the art technology; typically underutilized/unknown; e. g. , Kognito and Med. Respond training)
National SBIRT ATTC – SBIRT Suite of Services
On-Demand Courses • SBIRT 101 – Foundations Course • SBIRT for Adolescents Course To access courses go to: http: //ireta. org/improve-practice/addictionprofessionals/online-courses/
National SBIRT ATTC - Webinar Library http: //my. ireta. org/webinarlibrary-mobile
BIG Initiative – Live & On-Demand Webinars http: //hospitalsbirt. webs. com/webinars. htm http: //bigsbirteducation. webs. com/webinars. ht m

BIG Initiative – Learner Guides http: //bigsbirteducation. webs. com/learnersguides. htm
Interactive Tablet-based SBIRT Tools Radiant Interactive – BHRA Check-up For more information/demo contact Radiant Interactive at info@BHRACheckup. com

Interactive Virtual Patient Simulations Kognito More to come on this…

Additional Resources • SAMHSA-National Council CIHS http: //www. integration. samhsa. gov/clinical-practice/sbirt • National SBIRT ATTC http: //sbirt. ireta. org/sbirt • National ATTC Network www. attcnetwork. org • Online course for docs - http: //www. sbirttraining. com/ • Websites http: //www. oasas. ny. gov/Ad. Med/sbirt/index. cfm http: //www. improvinghealthcolorado. org/ http: //www. sbirtoregon. org/ http: //medicine. yale. edu/sbirt/index. aspx http: //www. bu. edu/bniart/sbirt-experience/sbirt-programs/ http: //www. attcelearn. org/ http: //www. motivationalinterview. org/

Integrating Adolescent SBIRT in Social Work and Nursing School Education • Conrad N. Hilton Adolescent SBIRT Grant – Launched October 2014 (3 year effort) • Overall Aim: To collaborate with schools of social work and nursing and leading professional associations to develop and test an interactive patient/client simulation training program, and to infuse adolescent SBIRT education into existing social work and nursing curriculum. • Collaborators: CSWE, CCSW, AACN, Kognito, and many others. • Learning Collaborative: Open to Schools of Social Work and Nursing launched January 2015 (Join Now!) • Visit our Website: http: //sbirt. webs. com • For More Info or to Join: Email Danielle Noriega at: Noriega. Danielle@norc. org

Conversations are Powerful Tools to Change Attitudes and Behaviors

Conversations are a social act of collaboration

Conversations are NOT: - Instruction-giving - Information delivery - Speeches - Talk that elicits no meaning

Conversations are an Integral Part of Changing Health Behaviors Individual/Environment : Medical condition Mindset Concerns Barriers to change Intrinsic motivation to change Individual Environment Behavior

Virtual Humans

“Virtual Humans are automated agents that converse, understand, reason and exhibit emotions. They possess a threedimensional body and perform tasks through dialogs with humans. ” Source: chatterbots. org

Benefits of Virtual Humans Instructional Benefits: § Safe to self-disclose, experiment § Increase in engagement, openness § Decrease in transference reactions § Decrease in social evaluative threat § The challenge of the uncanny valley Other benefits: § Personalization of experience § Reduce costs of updates § “Choose your Avatar” option
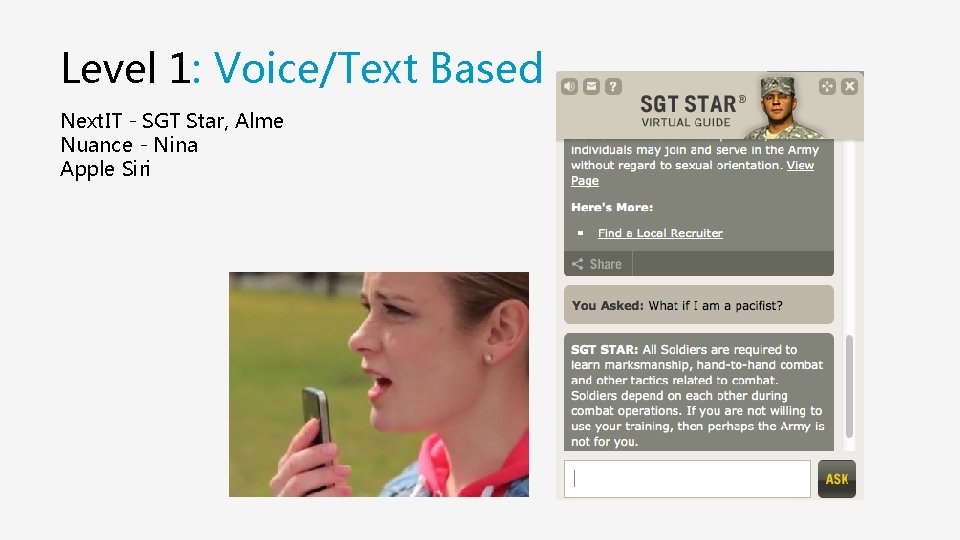
Level 1: Voice/Text Based Next. IT - SGT Star, Alme Nuance - Nina Apple Siri
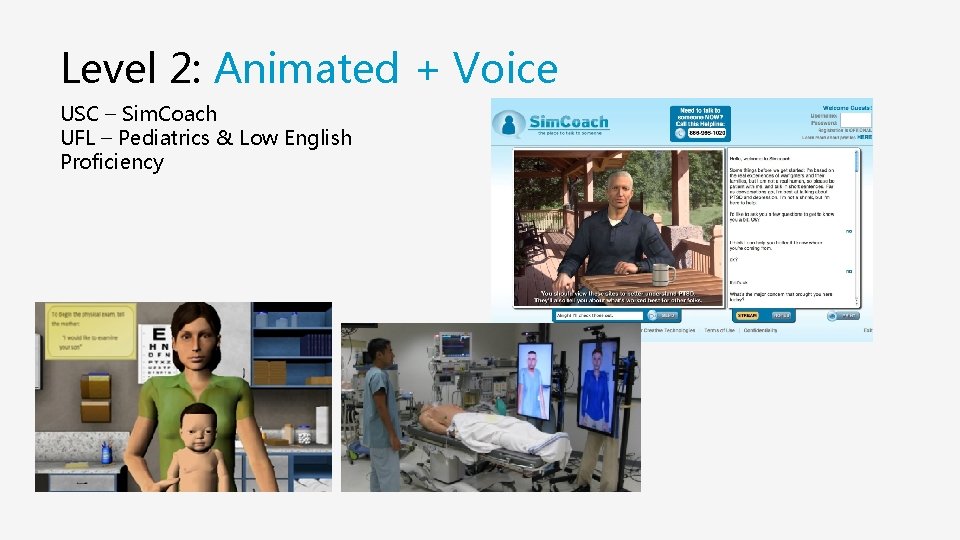
Level 2: Animated + Voice USC – Sim. Coach UFL – Pediatrics & Low English Proficiency

Level 3: Emotionally Responsive § 3 -D, fully animated § Real-life behaviors - Individual personalities - Memory - Emotionally responsive § Adapt to players’ decisions Be interviewed by the virtual human to identify their own barriers to change and build motivation Learn how to manage health conversations with others

Demo
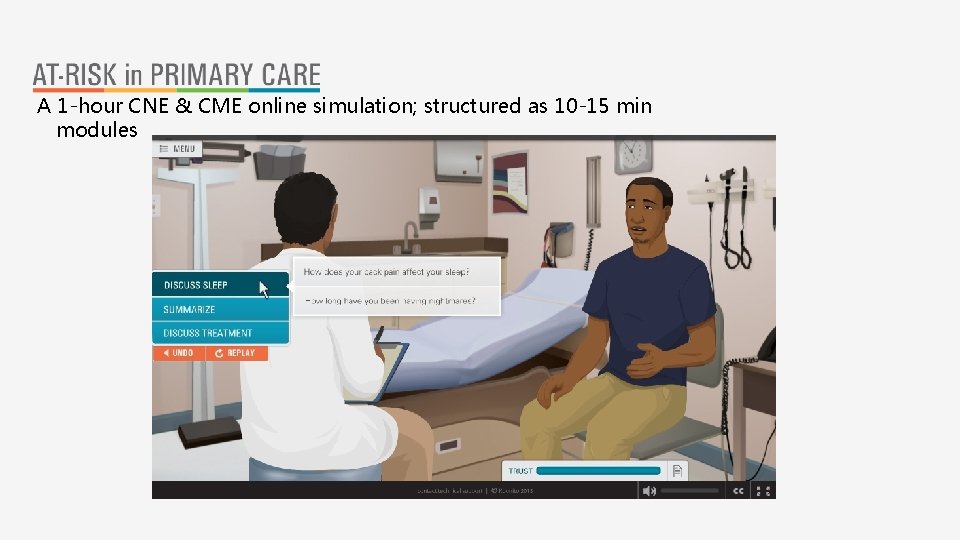
A 1 -hour CNE & CME online simulation; structured as 10 -15 min modules

Virtual Patients Level 1: Level 2: Antoine, 38 Chief Complaint: Back pain, seeking prescription renewal for pain medication Underlying Issue: PTSD Judith, 65 Chief Complaint: Arthritis Underlying Issue: Depression following retirement and loss of daughter on 9/11 Goals: Determine risk of mental health disorder Goals: Discuss results of PHQ-9 Collaboratively develop treatment plan that integrates behavioral health Build motivation to treatment adherence
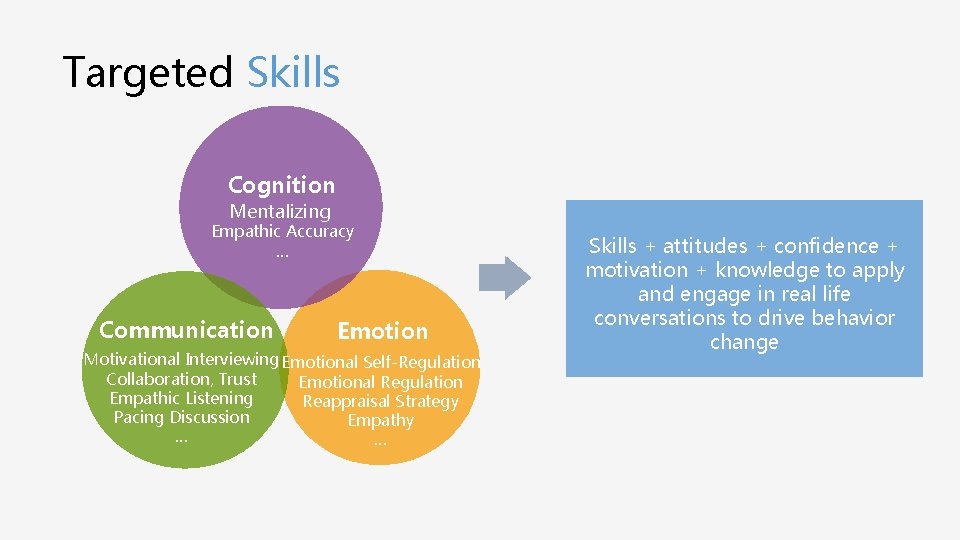
Targeted Skills Cognition Mentalizing Empathic Accuracy … Communication Emotion Motivational Interviewing Emotional Self-Regulation Collaboration, Trust Emotional Regulation Empathic Listening Reappraisal Strategy Pacing Discussion Empathy … … Skills + attitudes + confidence + motivation + knowledge to apply and engage in real life conversations to drive behavior change

Results: Primary Care Setting Longitudinal Study with 516 Health Professionals in 6 States (N=87 matched pairs) Goal of Simulation: Increase screening for depression and substance abuse within primary care settings, integration of behavioral health, and treatment adherence by such patients Method: Empowering physicians and nurses with the skills and motivation to engage in challenging screening and brief intervention conversations with patients that exhibit signs of Participants: 19% physicians, 55% nurses, 8% Nurse Practitioners, 14% depression and substance use disorders. Medical Students, 7% Nursing Students, 26% male, 82% Caucasian, 12% Hispanic, 13% African American. 58% in NYC, 31% North Dakota, 11% in Arizona, Oklahoma, Virginia. Study Design: Participants completed pre-training, post-training, and a 3 month follow up surveys. Surveys asked a range of Likert scale and openended questions to determine changes in skills, attitudes, and behavioral intent. 2015. Kognito. All Rights Reserved. Do Not Share without Kognito Approval

Results: Primary Care Setting Quality of Learning Experience • 94% reported that the simulation was well constructed and easy to use • 79% reported that it was relevant to their patient population to a “great extent” or “very great extent” • 84% reported that the simulated conversations with virtual humans were helpful to a “great extent” or “very great extent” in learning effective conversation tactics to increase patient engagement, trust, and adherence to treatment plans • 81% reported that the simulated conversations with virtual humans were, to a Overall Satisfaction “great extent” or “very great extent, ” realistic representations of • 84% said the simulation was at their skill level (16% said it was above their conversations they skill level) have with their patients • 95% reported that they will recommend it to their colleagues

Results: Primary Care Setting Changes in knowledge and Skill Study found statistically significant (p<. 05) and sustainable increase at follow-up in learners’ knowledge and skill to: • • • Identify risk factors and warning signs of mental health disorders Screen patients for symptoms of a mental health disorder Discuss treatment options Engage in collaborative decision making about treatment plans Build intrinsic motivation in patients to adhere to the suggested treatment plans Behavior Change At 3 -month follow-up, as a result of taking the simulation: • 62% reported increases in the number of patients they screened • 57% reported increases in discussions with patients about treatment options • 52% reported that they engaged more frequently in collaborative decision-making about treatment pla

Questions & Answers Dr. Eric Goplerud SVP and Director Public Health Department NORC at the University of Chicago 301 -634 -9525 Goplerud-Eric@norc. org Dr. Tracy Mc. Pherson Senior Research Scientist Public Health Department NORC at the University of Chicago Ron Goldman Co-Founder & CEO Kognito 757 -427 -1028 Mc. Pherson-Tracy@norc. org 212 -675 -9234 ron@Kognito. com Demos: www. kognito. com

Extra Slides

Approach: Immersive Learning Conversations Science Driven and Research Proven Neuroscience Social Cognition Adult Learning Theory ` Virtual Humans with Real-Life Behaviors Individual personalities Memory Emotionally Responsive
Kognito’s Virtual Humans - Process 3 -D Modeling Behavior/Emotion Library
Kognito’s Virtual Humans - Process Embedded in 3 -D Environment Virtual Human Controller
- Slides: 59