WEBINAR DELIVERING COMPREHENSIVE SUPPORTIVE CARE FOR PEOPLE WITH

WEBINAR: DELIVERING COMPREHENSIVE SUPPORTIVE CARE FOR PEOPLE WITH DR-TB AT FACILITY & COMMUNITY LEVELS September 30, 2019 1 Photo: D. Richardson

Webinar topics Quick review of the comprehensive supportive care framework Steps in planning implementation at the facility and community levels Success stories and advice from pilot countries Resources Q&A PHOTO: PATH • • •

Care Package guidance document • Part 1: Delivering Comprehensive Supportive Care to People with Drugresistant Tuberculosis (Practical Guide) • Part 2: Operational Toolkit – – – – Step-by-step instructions How-To guides for each element of supportive care Service Status Assessment and Planning template Rapid Systems Assessment tool Local Operational Plan template Patient Assessment and Individual Care Plan template M&E Guide http: //ghpro. dexisonline. com/resource/delivering-comprehensive-supportive-carepeople-drug-resistant-tuberculosis-0 3
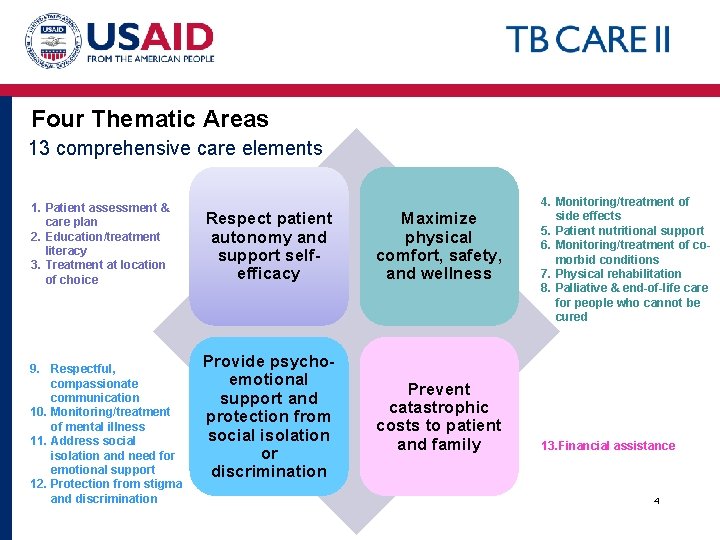
Four Thematic Areas 13 comprehensive care elements 1. Patient assessment & care plan 2. Education/treatment literacy 3. Treatment at location of choice 9. Respectful, compassionate communication 10. Monitoring/treatment of mental illness 11. Address social isolation and need for emotional support 12. Protection from stigma and discrimination Respect patient autonomy and support selfefficacy Maximize physical comfort, safety, and wellness Provide psychoemotional support and protection from social isolation or discrimination Prevent catastrophic costs to patient and family 4. Monitoring/treatment of side effects 5. Patient nutritional support 6. Monitoring/treatment of comorbid conditions 7. Physical rehabilitation 8. Palliative & end-of-life care for people who cannot be cured 13. Financial assistance 4

Operationalizing the Package Global level Agreement on four key thematic areas for comprehensive supportive care for DR-TB and the elements of supportive care for each area National or regional level Assess the current status of patient support; decide what interventions are feasible for the program to implement to cover each element for each thematic area and create an appropriate package of supportive services Local or facility level Adapt the national package to local circumstances; develop a local implementation plan with clear roles and responsibilities for delivering services Individual patient level Assess patient for needs in each thematic area and work in partnership with the patient to develop an individual care plan incorporating the available services that best meet that person's specific needs and preferences 5

Quality care for people with DR-TB • DR-TB prevention through adequate treatment of DS-TB • DR-TB prevention through infection control and contact evaluation and treatment • Quality rapid diagnostics • Trained clinicians and health workers • Free, high-quality drugs with new and shortened regimens • a. DSM and prompt treatment of side effects • Supportive care until cure • Ongoing monitoring following cure 6

Steps in implementation at local level 1. Identify and orient your local stakeholders. 2. Develop facility-specific plans for implementation. 3. Adequately prepare facility staff and community-based staff and organizations to provide person-centered supportive care. 4. Monitor your progress on at least a quarterly basis to identify what’s working, what needs changing, and what else can be done to improve performance.

Assessing the DR-TB Package • Patient satisfaction – Surveyed patients – Compared responses from a baseline or control cohort with the cohort receiving the care package • Asked about satisfaction with services received and their providers • Feasibility and acceptability – Surveyed healthcare providers and managers – Asked if care package implementation was feasible, acceptable, and sustainable 8

Assessing the DR-TB Package • Treatment outcomes (are more patients cured? ) – Compared historical outcomes data with interim outcomes from the cohort receiving the care package – Measured by interim results • Higher proportion of patients completed or still on treatment at 6 -9 months • Lower proportion of deaths • Lower proportion of loss to follow-up • Higher treatment success as final outcome (determined post-pilot) 9

IMPLEMENTING AMBULATORY MDR-TB CARE THROUGH MULTIDISCIPLINARY TEAMS IN UKRAINE

Creating Multidisciplinary Teams (MDT) 1. Team approach in the treatment of MDR-TB and creation of MDT is in line with the "Strategy for Provision of Socio-Psychological Assistance to Patients with MDRTB", developed by Challenge TB project. 2. MDTs are created on the basis of an order by the oblast public health administration.

Steps required for implementation ü ü ü ü Training of hospital staff and NGOs. Preparation of orders of oblast health administration. Creation of multidisciplinary teams (MDT) Workshops for MDTs. Purchase of food packages/hygiene kits and cell phone cards. Establishment of partnership (shelters, addictiontreatment centers, and others). Regular monitoring visits.

The goal of MDT is to lower loss to follow-up, build strong adherence to treatment and retain patient on treatment till completion by providing comprehensive medical and socio-psychological person-oriented care at the ambulatory stage of treatment.
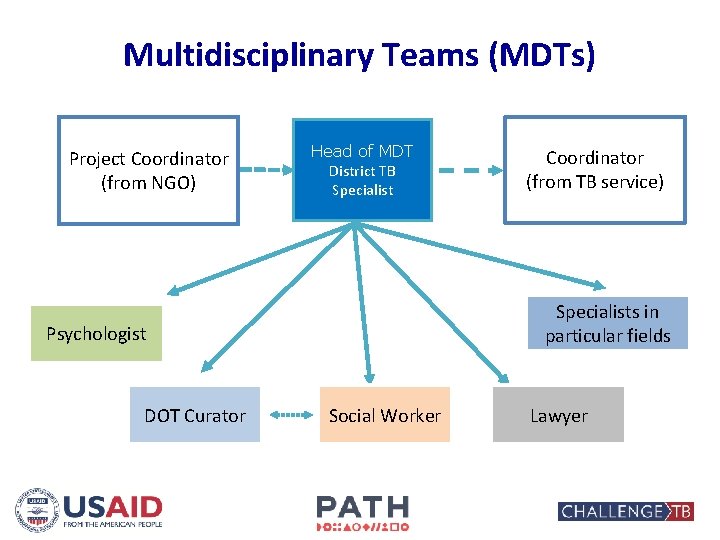
Multidisciplinary Teams (MDTs) Project Coordinator (from NGO) Head of MDT District TB Specialists in particular fields Psychologist DOT Curator Coordinator (from TB service) Social Worker Lawyer

Functions of MDTs • Comprehensive analysis of patient's health status during outpatient phase of treatment. • Provision of treatment for a patient throughout the course of ambulatory treatment. • Identification and addressing patient’s needs in socio-psychological care. • Active detection and timely management of side effects of TB drugs. • Rapid and high-quality interaction/exchange of information between DOT supervisor and other MDT members to ensure continuity of treatment. • Building partnerships and cooperation with public services. • Treatment monitoring.

Requirements for Effective MDTs • Clear roles and performance of obligations by MDT members. • Leadership of rayon TB specialist. • Flexible attitude to work. • Provision of quality DOT. • Rapid information exchange between DOT supervisor, social worker and rayon TB specialist regarding treatment interruptions, occurrence of exacerbations, and adverse reactions to TB drugs. • Tailoring of the services provided to individual needs of patient. • Active interaction with TB service supervisor.
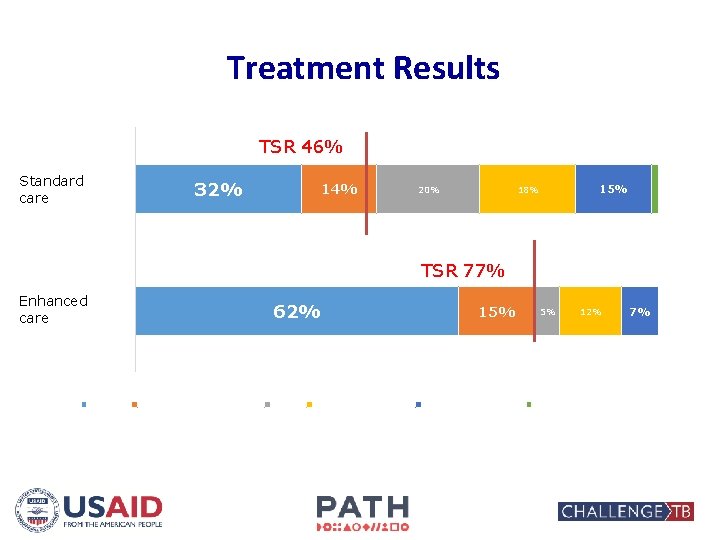
Treatment Results MDR-TB cohort, Jan 2015 - Mar 2016 TSR 46% Standard Non CTB patients care 32% 14% 20% 15% 18% 1% TSR 77% Enhanced CTB patients care 62% 0% Cured 10% 20% Treatment competed 30% Died 15% 40% 50% Treatment failed 60% 70% Lost to follow-up 5% 80% 12% 90% Transferred out 7% 0% 100%

Challenges and solutions CHALLENGES • The patient assessment tool is too long, health care workers at the hospital do not always understand who and how to fill it, and how to explain to patients why this questionnaire is needed. • Competition among NGOs and Red Cross for patients who need SPS. • Lack of motivation of some social workers to provide SPS. SOLUTIONS • • • Train medical providers and adapt the tool in consultation with users. Develop specific criteria for patients' recruitment for SPS and appoint a supervisor from TB service. Monitor NGO work carefully and provide positive feedback; interview supported patients to verify services provided

Success Factors • Situation assessment, analysis of patients' needs, reasons for loss to follow -up (in-depth interviews with patients and health care workers) • Provision of social and psychological support (SPS) primarily to patients with risk factors for loss to follow-up (effective use of resources). • Coordination and implementation of support algorithm /roles and responsibilities by all the services (TB services, primary health care services, and NGOs), adapted to local conditions in each region. • Special pre-implementation training for current NGO staff in the principles of patient-centered approach, algorithm for providing SPS, and skills of effective counseling. • Periodically conducted workshops for MDTs to ensure patient-centered approach, facilitate effective cooperation of partners, review challenging cases and share experiences.

Success Factors (2) • Timely adjustment of the SPS activities depending on the treatment status and changes in patient's needs. • Commitment and leadership of TB service providers (monthly meetings of OTBD Head doctor with all TB/HIV-service NGOs) (Mykolaiv). • TB service coordinator for each region to ensure the provision of SPS to patients with risk of loss to follow-up, monitor the results of their treatment in the register, keep records of all patients receiving SPS to avoid duplication of services.

USAID TUBERCULOSIS SOUTH AFRICA PROJECT Implementing the DR-TB Care Package at Facility and Patient Level
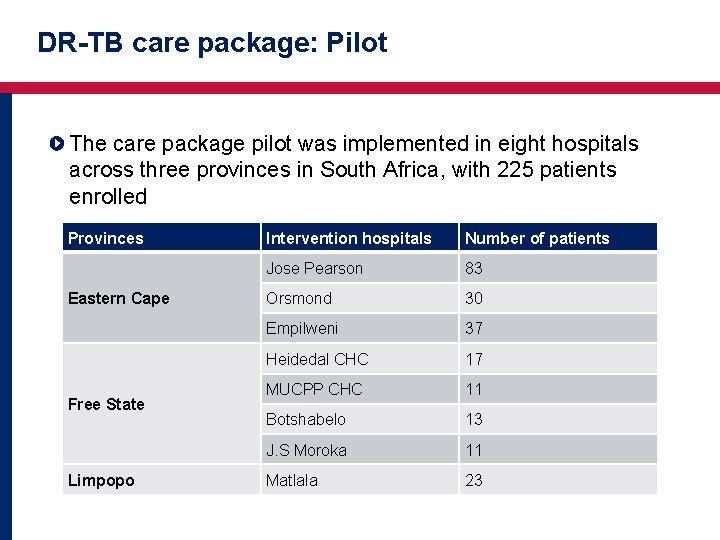
DR-TB care package: Pilot The care package pilot was implemented in eight hospitals across three provinces in South Africa, with 225 patients enrolled Provinces Eastern Cape Free State Limpopo Intervention hospitals Number of patients Jose Pearson 83 Orsmond 30 Empilweni 37 Heidedal CHC 17 MUCPP CHC 11 Botshabelo 13 J. S Moroka 11 Matlala 23

Essential elements of the DR-TB care package Clinical evaluation Has the HCW asked you if you have any other preexisting medical conditions e. g. HIV, hypertension, heart disease, diabetes, epilepsy, mental illness, renal disease or pregnancy? Health education Has the HCW educated you about TB and HIV? Nutrition Psychosocial support Has the HCW advised or counselled you on the types of food you must eat and how to eat while on treatment? Has the HCW referred you for counselling for anxiety or depression? Contact management Infection control Economic support Has the HCW screened and tested members of your household for TB? Has the HCW educated you on how to control TB infection in your home, such as opening doors and windows? Are you receiving a social grant? / Has the HCW provided you with transport assistance for check-up and follow-up appointments?
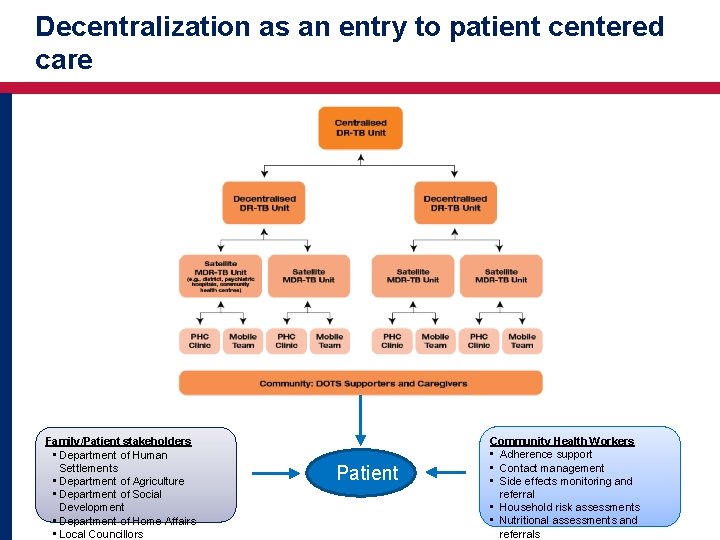
Decentralization as an entry to patient centered care Family/Patient stakeholders • Department of Human Settlements • Department of Agriculture • Department of Social Development • Department of Home Affairs • Local Councillors Patient Community Health Workers • Adherence support • Contact management • Side effects monitoring and referral • Household risk assessments • Nutritional assessments and 24 referrals

Multi-disciplinary core teams Provincial road shows were conducted to get buy in from stakeholders Multidisciplinary team of participants included: CEOs from pilot hospitals Provincial managers DR-TB nurses Dieticians Facility clinicians Social workers HIV Counsellors Auxiliary Workers Project funded NGOs USAID TB South Africa Project funded NGOs

Capacity building and service provision Core teams Basic TB training Nutrition training Interpersonal communication and counselling Orientation on conducting household risk assessments Patients & family members TB education TB treatment adherence Nutrition education Cough hygiene & etiquette Patient and family counselling

Tools used for the DR-TB care package Quality of care assessment Patient file / chart review Household risk assessment

Community education approach through dialogues and community radio sessions The Project engaged with community radio stations in the pilot districts for weekly TB education slots. Topics were based on thematic areas of the package Eastern Cape: Nqubela (KQ 97 FM) 130 000 listeners Free State: Motheo (88. 5 FM ) 74 000 listeners Limpopo: Thabantsho (91. 0 FM) 20 000 listeners Community dialogues were implemented to address issues of stigma and discrimination TB patient sharing his experience of DR-TB treatment from Matlala Hospital A social worker facilitating a community radio session

Psychosocial support for patients Psychosocial interventions by the social workers Psychological counselling for patients and family members Support to apply for ID documents Assistance to apply for social grants Support to access food packages Support to access community housing/relocation to new areas DR-TB patients tending to their vegetable gardens to supplement their own diet
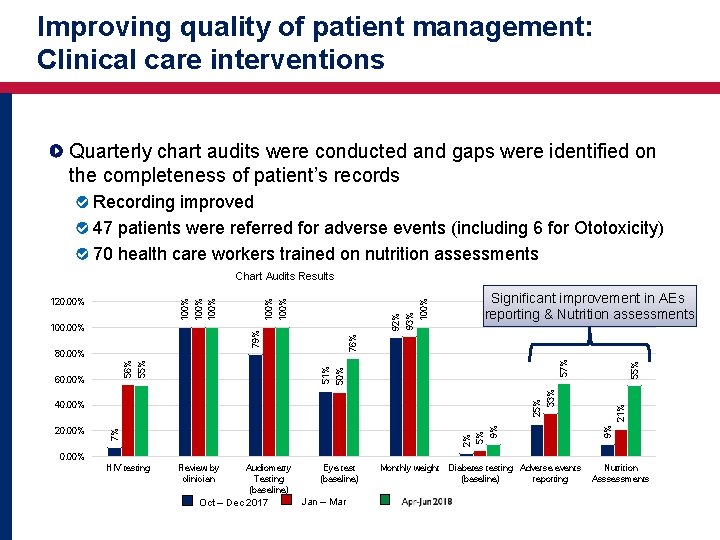
Improving quality of patient management: Clinical care interventions Quarterly chart audits were conducted and gaps were identified on the completeness of patient’s records Recording improved 47 patients were referred for adverse events (including 6 for Ototoxicity) 70 health care workers trained on nutrition assessments 55% 21% 9% 9% 5% 2% 20. 00% 7% 40. 00% 33% 25% 51% 57% 76% 100% Significant improvement in AEs reporting & Nutrition assessments 50% 55% 56% 80. 00% 60. 00% 93% 92% 100% 79% 100. 00% 100% 120. 00% 100% Chart Audits Results 0. 00% HIV testing Review by clinician Audiometry Testing (baseline) Oct – Dec 2017 Eye test (baseline) Jan – Mar Monthly weight Diabetes testing Adverse events (baseline) reporting Nutrition Asssessments

Household risk assessments Patient factors Elements assessed Contact TB screening Hygiene and infection control measures Out of 581 household contacts, 27 were found to have TB and were started on treatment Living conditions factors Elements assessed Ventilation (open windows & doors) Access to water and sanitation Six families whose living conditions were found to be dire were relocated to new homes / areas Before intervention After intervention
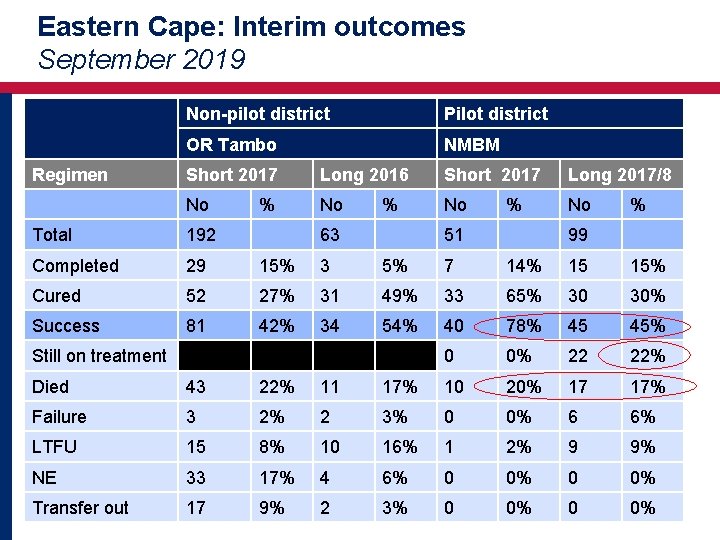
Eastern Cape: Interim outcomes September 2019 Non-pilot district Pilot district OR Tambo NMBM Regimen Short 2017 Long 2016 Short 2017 Long 2017/8 No % Total 192 63 51 99 Completed 29 15% 3 5% 7 14% 15 15% Cured 52 27% 31 49% 33 65% 30 30% Success 81 42% 34 54% 40 78% 45 45% Still on treatment 0 0% 22 22% Died 43 22% 11 17% 10 20% 17 17% Failure 3 2% 2 3% 0 0% 6 6% LTFU 15 8% 10 16% 1 2% 9 9% NE 33 17% 4 6% 0 0% Transfer out 17 9% 2 3% 0 0% 32

Lessons learned and recommendations Implementation of the DR-TB care package requires a multi disciplinary team (social workers, dietitians, nurses, doctors, optometrists, nutritionists, community health workers and others) Multidisciplinary teams are essential for patient management Clear referral pathways for comorbid disease management and mental health Management of patients from point of diagnosis to treatment completion Holistic management and support for patients Conducting regular chart reviews improves quality of clinical care and serves to strengthen the health system e. g. Timely monitoring and management of adverse events Timely ART initiation for co-infected patients Timely nutritional assessments

Lessons learned and recommendations Case management through social workers assists in addressing comprehensive needs of patients and supports the breaking down of barriers in service provision Social workers play a key advocacy role for patients as they link patients to service delivery interventions Supported patients to apply for ID documents and social grants Mobilized community members to support patients Supported patients with housing issues Provided nutritional support to patients – linkages with Department of Agriculture Community based stakeholders are critical to the success of addressing stigma and supporting patients with adherence support

Acknowledgements United States Agency for International Development (USAID) USAID Core Team (Dr A. Golubkov, Dr L. Adams and Dr H. Lam and Ms. D. Richardson) South African National Department of Health Eastern Cape Provincial Department of Health Free State Provincial Department of Health Limpopo Provincial Department of Health Multidisciplinary core teams DR-TB patients and their family members

“…we had our own dreams about how to provide patient care and to address…stigma and the high interruption rate…now, the patient-centered DRTB package has made those dreams a reality…” Doctor at Matlala Hospital, Limpopo Province, South Africa
- Slides: 36