WATER SOLUBLE VITAMINS Dr Greeshma Dept of Biochemistry

WATER SOLUBLE VITAMINS Dr Greeshma Dept. , of Biochemistry 1

VITAMINS: CLASSIFICATION Vitamins are micronutrients that are required for normal growth and maintainence of good health Fat soluble vitamins o vitamin A o vitamin D o vitamin E o vitamin K Water soluble vitamins - vitamin B complex - vitamin C 2

VITAMINS Characteristic Solubility Fat soluble vitamins Water soluble vitamins Organic solvent Water With lipids Requires bile salt Absorption is simple Not require bile salts Present No Liver No appreciable storage Excretion Not excreted Excreted Deficiency Manifests only when stores are depleted Manifests rapidly as there is no storage Toxicity Hyper vitaminosis Unlikely Treatment of deficiency Single large dose Regular dietary intake Digestion & absorption Carrier proteins Storage 3

VITAMINS Synonyms Chemistry Coenzyme Forms Functions Nutritional Aspects: Sources RDA Deficiency Manifestations Antivitamins 4

WATER SOLUBLE VITAMINS Vitamin B complex Thiamine (Vitamin. B 1) Riboflavin (Vitamin B 2) Niacin(Vitamin B 3) Pantothenic acid Pyridoxine (Vitamin B 6) Biotin Folic acid Cobalamin (Vitamin B 12) Vitamin C 5

WATER SOLUBLE VITAMINS Vitamin Coenzyme form Groups transferred Thiamine(B 1) Thiamine pyrophosphate(TPP) Aldehyde Riboflavin(B 2) FMN & FAD Hydrogen/electron Niacin(B 3) NAD & NADP Hydrogen/electron Pantothenic acid Co enzyme A Acyl group(Fatty acid) Pyridoxal phosphate(PLP) Amino group, CO 2 Biotin CO 2 Tetrahydrofolate(THF) 1 carbon- methyl, formyl, methenyl Methyl cobalamine methyl Pyridoxine(B 6) Biotin Folic acid Cobalamine(B 12) 6
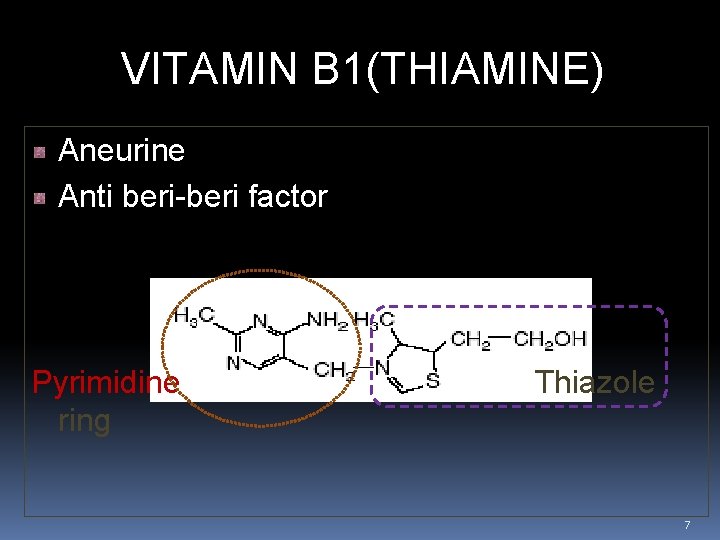
VITAMIN B 1(THIAMINE) Aneurine Anti beri-beri factor Pyrimidine ring Thiazole 7
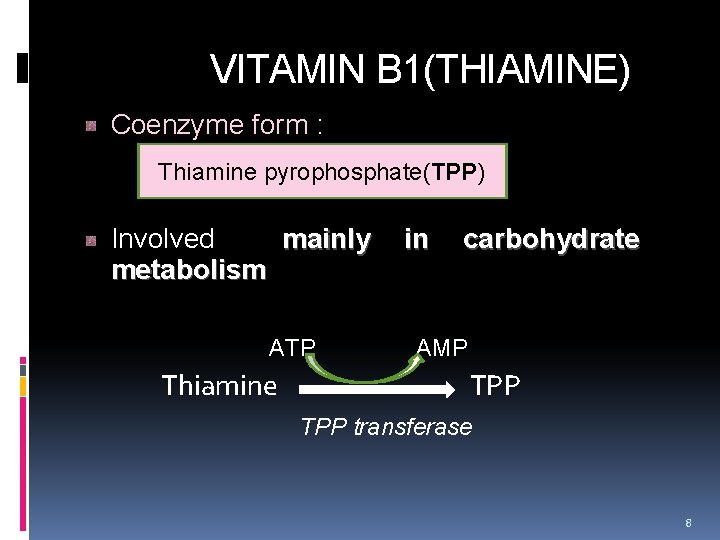
VITAMIN B 1(THIAMINE) Coenzyme form : Thiamine pyrophosphate(TPP) Involved mainly metabolism in carbohydrate ATP AMP Thiamine TPP transferase 8
VITAMIN B 1(THIAMINE) Oxidative decarboxylation reactions pyruvate dehydrogenase α-ketoglutarate dehydrogenase α-keto acid dehydrogenase Transketolase reactions in HMP pathway Neurotransmission 9

VITAMIN B 1(THIAMINE) Transketolase reaction Ribose-5 –phosphate + xylulose -5 -phosphate Transketolase-TPP Sedoheptulose-7 -phosphate+glyceraldehyde-3 phosphate 10

VITAMIN B 1(THIAMINE) Transketolase reaction Xylulose-5 -phosphate+ Erythrose-4 -phosphate Transketolase-TPP Fructose – 6 - Phosphate+Glyceraldehyde-3 -Phosphate Transfers 2 carbon units from ketose to aldose and simultaneously converts aldose to ketose Reaction generates NADPH 11
VITAMIN B 1(THIAMINE) PDH Complex Pyruvate Acetyl Co. A + CO 2 TPP, NAD, FAD, Co. ASH, Lipoic acid 12
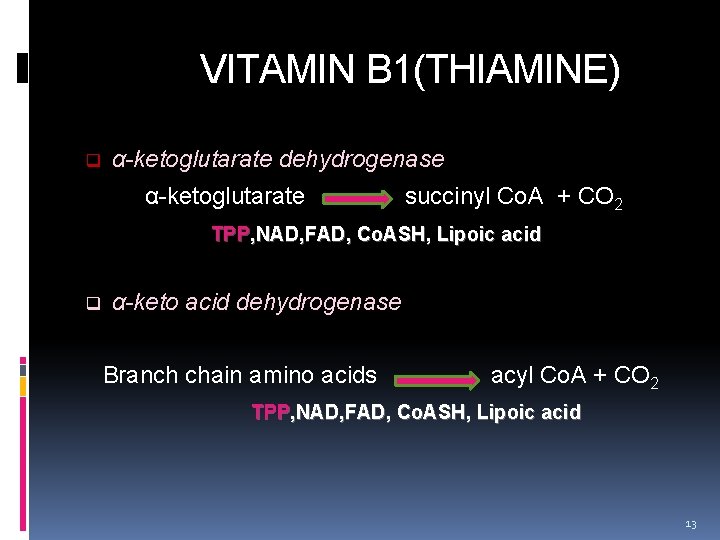
VITAMIN B 1(THIAMINE) q α-ketoglutarate dehydrogenase α-ketoglutarate succinyl Co. A + CO 2 TPP, NAD, FAD, Co. ASH, Lipoic acid q α-keto acid dehydrogenase Branch chain amino acids acyl Co. A + CO 2 TPP, NAD, FAD, Co. ASH, Lipoic acid 13

VITAMIN B 1(THIAMINE) Neurotransmission ↑acetyl choline synthesis and utilization ↑ neurotransmitter levels in brain 14

VITAMIN B 1(THIAMINE) Sources Vegetarian : Outer layer of cereals – unpolished (parboiled) rice Pulses, Oil seeds, nuts and yeast Pulses nuts Animal sources: pork , liver, heart, kidney & milk RDA: 1 – 1. 5 mg/ day 15

VITAMIN B 1 DEFICIENCY Low dietary intake Intake of polished cereals Chronic alcoholism Other factors Carbohydrate rich diet Impaired intestinal absorption Excessive demand – pregnancy & lactation 16
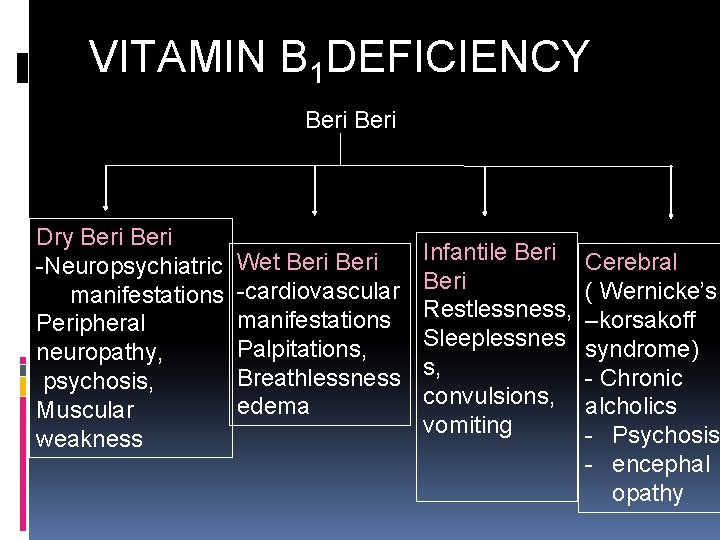
VITAMIN B 1 DEFICIENCY Beri Dry Beri -Neuropsychiatric Wet Beri manifestations -cardiovascular manifestations Peripheral Palpitations, neuropathy, Breathlessness psychosis, edema Muscular weakness Infantile Beri Restlessness, Sleeplessnes s, convulsions, vomiting Cerebral ( Wernicke’s –korsakoff syndrome) - Chronic alcholics - Psychosis - encephal opathy

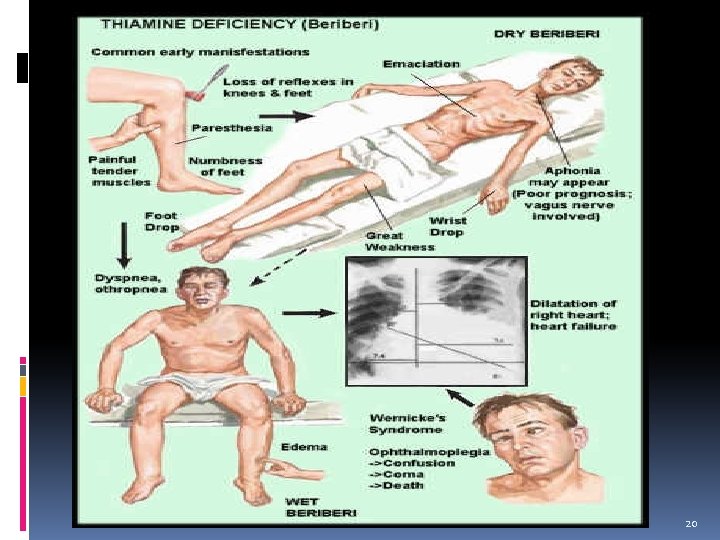
VITAMIN B 1 DEFICIENCY Beri-Beri Dry Beriberi : neuropsychiatric – peripheral neuropathy, psychosis & muscular weakness Wet Beriberi: cardiovascular breathlessness, edema – palpitation, Infantile beri-beri 18

VITAMIN B 1 DEFICIENCY Cerebral beri( Wernicke’s- Korsakoff syndrome) - In chronic alcoholics - Due to: dietary insufficiency impaired intestinal absorption Characterised by: encephalopathy, psychosis, apathy, loss of memory and nystagmus(rhythmical to-and-fro motion of the eyeballs) 19
20

VITAMIN B 1 Antivitamins: Tannin: excessive tea consumption Pyrithiamine and oxythiamine (sulfa drugsantibiotics) 21
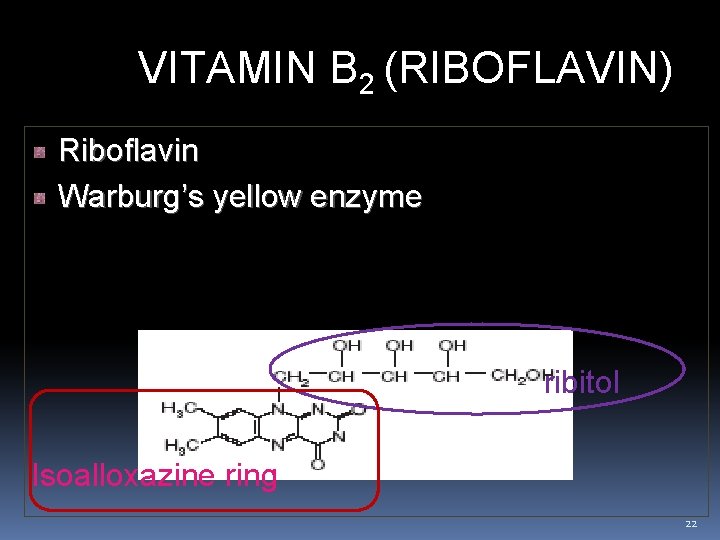
VITAMIN B 2 (RIBOFLAVIN) Riboflavin Warburg’s yellow enzyme Heat stable, Light sensitive Act as both oxidant and antioxidant ribitol Isoalloxazine ring 22
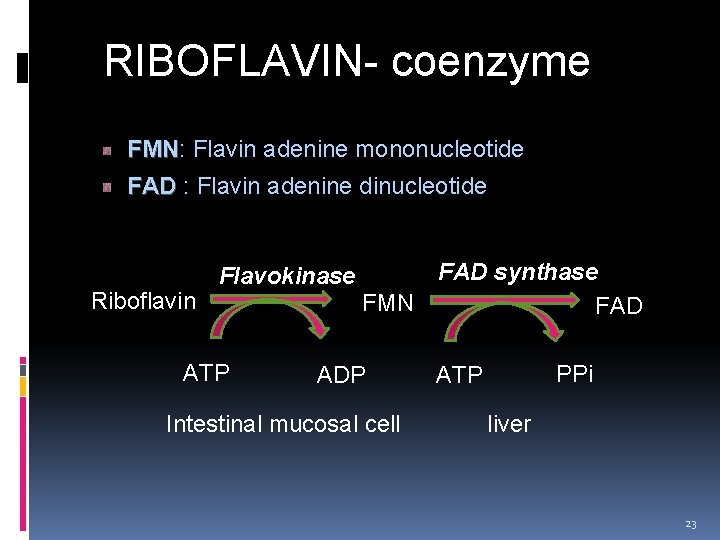
RIBOFLAVIN- coenzyme FMN: Flavin adenine mononucleotide FMN FAD : Flavin adenine dinucleotide FAD Riboflavin Flavokinase ATP FAD synthase FMN FAD ADP Intestinal mucosal cell PPi ATP liver 23

RIBOFLAVIN Enzyme cofactor for: Oxidation – reduction reactions Metabolism of lipids / carbohydrates Drug metabolism FAD transfers reducing equivalents for ATP production by oxidative phosphorylation 24
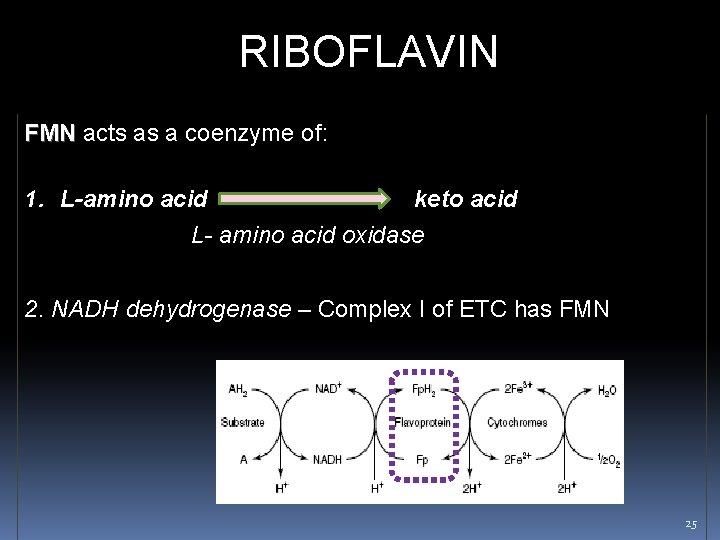
RIBOFLAVIN FMN acts as a coenzyme of: 1. L-amino acid keto acid L- amino acid oxidase 2. NADH dehydrogenase – Complex I of ETC has FMN 25
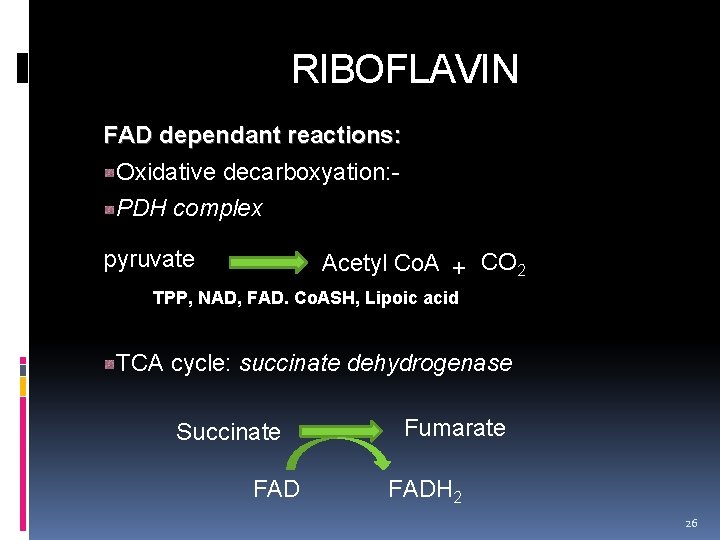
RIBOFLAVIN FAD dependant reactions: Oxidative decarboxyation: - PDH complex pyruvate Acetyl Co. A + CO 2 TPP, NAD, FAD. Co. ASH, Lipoic acid TCA cycle: succinate dehydrogenase Succinate FAD Fumarate FADH 2 26

VITAMIN B 2: SOURCES Animal: Liver Egg Kidney Meat Yeast Fish Veg: Cereals Pulses Milk Fruits Green Leafy Vegetables RDA: RDA 1. 5 mg/ day Increased in pregnancy and lactation 27
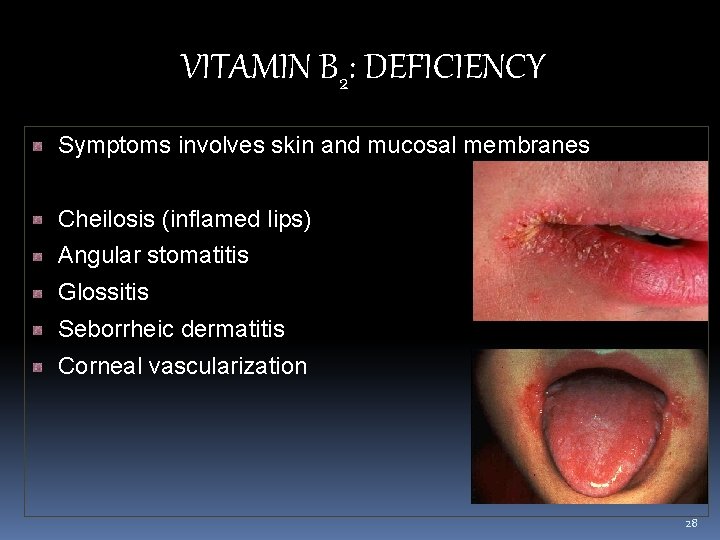
VITAMIN B 2: DEFICIENCY Symptoms involves skin and mucosal membranes Cheilosis (inflamed lips) Angular stomatitis Glossitis Seborrheic dermatitis Corneal vascularization 28

ANTIVITAMINS Isoriboflavin Galactoflavin Araboflavin 29

VITAMIN B 3: NIACIN Pellagra preventing factor of Goldberger Pyridine derivative 2 forms: Nicotinic acid & Nicotinamide 30
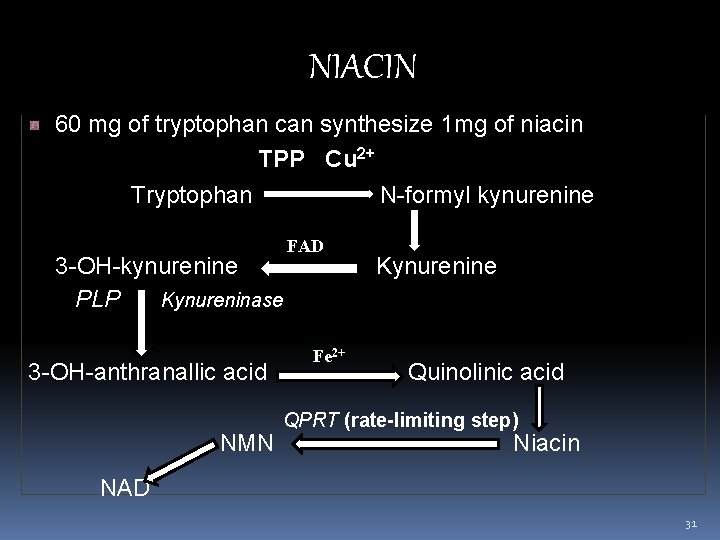
NIACIN 60 mg of tryptophan can synthesize 1 mg of niacin TPP Cu 2+ Tryptophan 3 -OH-kynurenine PLP Kynureninase 3 -OH-anthranallic acid NMN N-formyl kynurenine FADD Kynurenine Fe 2+ Quinolinic acid QPRT (rate-limiting step) Niacin NAD 31

NIACIN : COENZYME FORM Nicotinamide adenine dinucleotide (NAD+ ) Nicotinamide adenine dinucleotide phosphate (NADP + ) Functions: NAD+ collects reducing equivalents for ATP production in the mitochondria by oxidative phosphorylation. 32
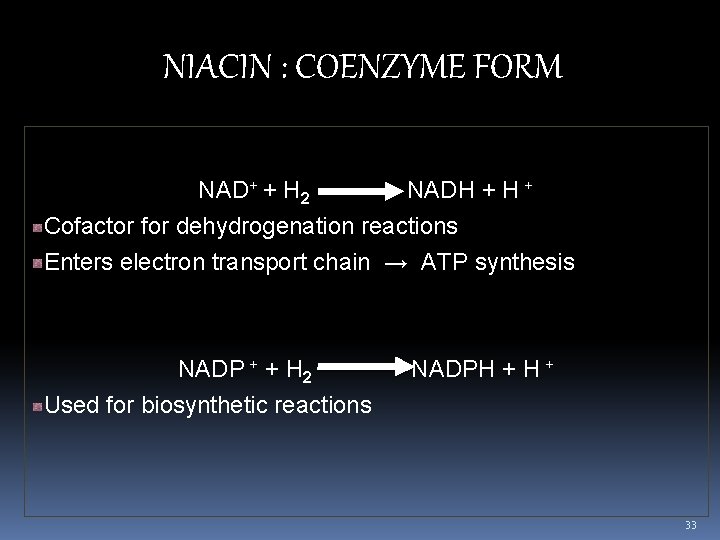
NIACIN : COENZYME FORM NAD+ + H 2 NADH + Cofactor for dehydrogenation reactions Enters electron transport chain → ATP synthesis NADP + + H 2 NADPH + Used for biosynthetic reactions 33

NIACIN : FUNCTION NAD+ dependent enzymes (NADH generating reactions) NADP+ dependent enzymes (NADPH generating reactions) 34

NIACIN : FUNCTION NAD dependant reactions: Pyruvate dehydrogenase Pyruvate Acetyl Co. A + CO 2 TPP, NAD, FAD. Co. ASH, Lipoic acid Glyceraldehyde-3 -phosphate dehydogenase Lactate dehydrogenase Lactate GLYCOLYSIS Pyruvate NAD+ NADH+H+ 35

NAD DEPENDANT REACTIONS α-ketoglutarate dehydrogenase Isocitrate dehydrogenase TCA Cycle Malate dehydrogenase β hydroxy acyl Co. A dehydrogenase ( β oxidation) β-OH-acyl Co. A β-ketoacyl Co. A 36
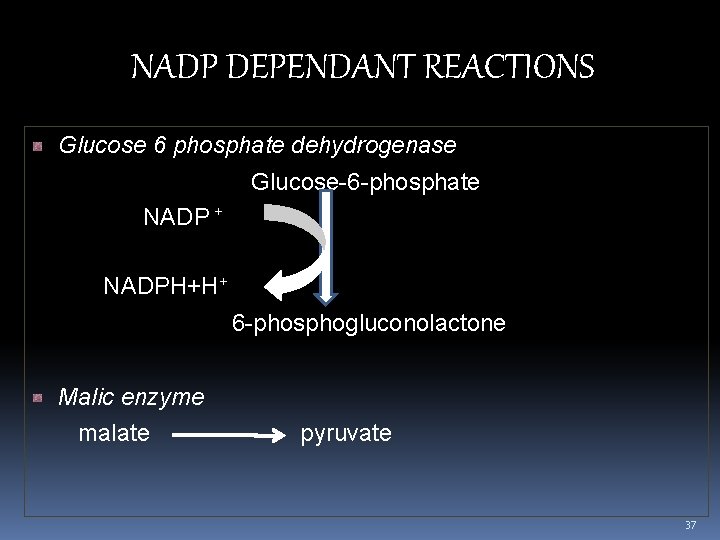
NADP DEPENDANT REACTIONS Glucose 6 phosphate dehydrogenase Glucose-6 -phosphate NADP + NADPH+H+ 6 -phosphogluconolactone Malic enzyme malate pyruvate 37

NIACIN : SOURCES Yeast Meat Legumes Liver Fish Cereals (outer coats) Peanuts Sweet potato - Niacin is formed in humans during catabolism of tryptophan. It provides only 10% of the requirement. Remainder must come from the diet Every 60 mg of tryptophan = 60 mg of tryptophan 1 mg of niacin RDA: 20 mg/day 38

NIACIN : DEFICIENCY 1. Diet poor in niacin & tryptophan - seen in populations dependant on maize as staple food. Maize deficient in tryptophan, niacin present. in bound form in maize →niacin unavailable 2. Hartnups disease: defective intestinal absorption and renal disease tubular reabsorption of tryptophan 3. Inability to convert tryptophan to niacin 39

NIACIN : DEFICIENCY Pellagra : Disease of 3 Ds( involves skin, GIT & CNS) Dermatitis: bright red erythema and increase pigmentation around neck(Casal’s necklace), ankle, feet and face exposed to sunlight Diarrhea: chronic inflammation of intestinal mucosa Dementia: degeneration of nervous tissue – irritability, inability to concentrate, poor memory 40
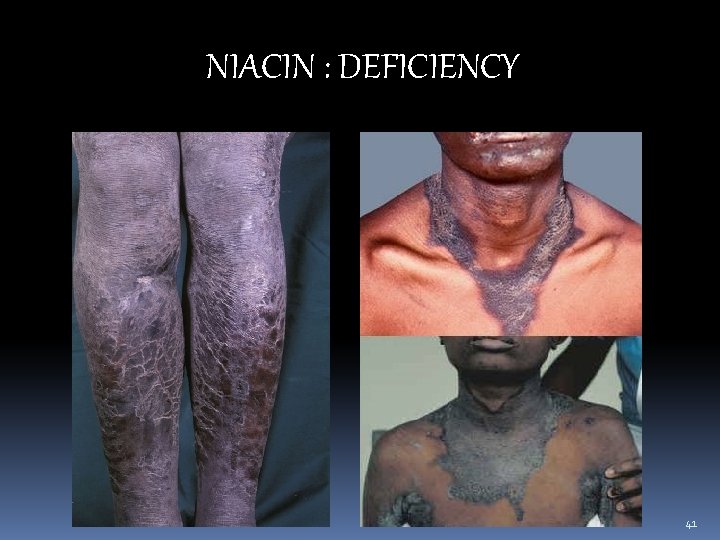
NIACIN : DEFICIENCY 41

NIACIN : ANTAGONISTS 3 Acetyl pyridine Isoniazid 42

1. Explain the following aspects of thiamine. a) Coenzyme form b) Biochemical functions/ metabolic role and c) Deficiency 2. TPP as a coenzyme in three metabolic reactions of the body. 3. Write coenzyme forms of and one reaction for each a) Niacin b) Riboflavin 4. Deficiency manifestations of Niacin. 5. Explain the biochemical basis: a) Intake of polished cereals as staple food may cause Beriberi b) Pellagra is more common in population dependent on maize as the 43 staple food
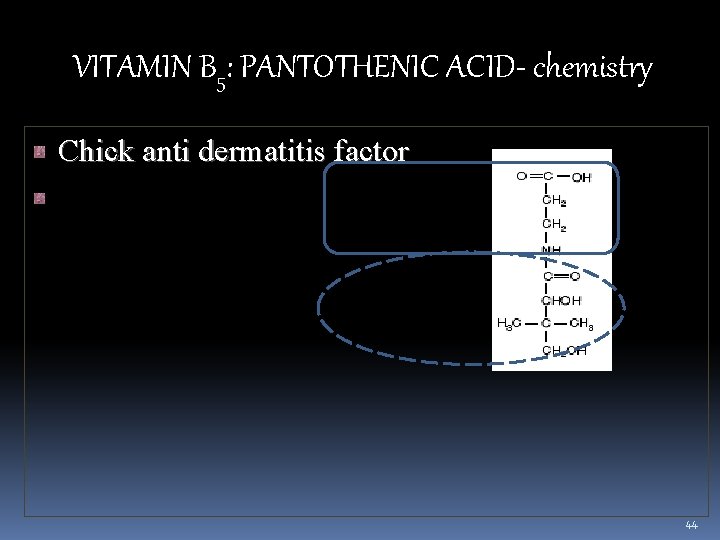
VITAMIN B 5: PANTOTHENIC ACID- chemistry Chick anti dermatitis factor 44

PANTOTHENIC ACID: active form Used in synthesizing two important acyl carriers 1. Coenzyme A ( Co. ASH) 2. Acyl carrier protein( ACP of fatty acid synthase complex) 45

PANTOTHENIC ACID: functions Coenzyme A (Co. A / Co. A-SH) Coenzyme (Co. A) participates in several enzymatic reactions of carbohydrate, lipid and amino acid metabolism Important Co. A derivatives: Acetyl Co. A, Succinyl Co. A, HMG Co. A, Malonyl Co. A, Palmityol Co. A, Propionyl Co. A Acyl carrier protein - Pantothenic acid is required for the synthesis of phosphopantotheine of fatty acid synthase complex synthase - carry acyl groups in fatty acid synthesis 46

PANTOTHENIC ACID: Sources Whole cereals Legumes Egg yolk Liver yeast Also synthesized by bacterial flora in the intestine RDA: 10 mg/day 47

PANTOTHENIC ACID: DEFICIENCY It is rare in humans ( due to widespread distribution of the vitamin) Gopalan’s Burning foot syndrome seen in prisoners of war and during famine manifested as: -Painful burning sensations(Paresthesia) in feet -Staggering gait -impaired coordination & sleep disturbance 48

VITAMIN B 6: PYRIDOXINE Three compounds derived from pyridine show vitamin B 6 activity. Pyridoxine Pyridoxal Pyridoxamine 49

VITAMIN B 6: PYRIDOXINE Active form of vitamin B 6 Pyridoxal phosphate Pyridoxal kinase Pyridoxal Pyridoxal phosphate(PLP) ATP ADP 50

PLP FUNCTIONS Proteinmetabolism: transamination decarboxylation transulfuration deamination Lipid metabolism sphingomyelin synthesis Carbohydrate metabolism glycogenolysis gluconeogenesis Heme synthesis 51

PLP DEPENDANT REACTIONS Transamination Amino acid 1 + Ketoacid 2 Amino acid 2 + Ketoacid 1 Example: PLP Alanine + α- Ketoglutarate Pyruvate + Glutamate Alanine transaminase 52

PLP DEPENDANT REACTIONS Decarboxylation - Glutamate decarboxylase glutamate gamma amino butyric acid(GABA) PLP (inhibitory neurotransmitter) - Histidine decarboxylase PLP histidine histamine (mediator of allergic reactions) 53

PLP DEPENDANT REACTIONS Tryptophan decarboxylase tryptophan serotonin(neurotransmitter) PLP Serine decarboxylase Serine ethanolamine PLP Catecholamine synthesis Dopa decarboxylase DOPA Dopamine PLP 54

PLP DEPENDANT REACTIONS In Lipid metabolism Sphingomyelin synthesis palmitoyl Co. A + serine 3 -ketosphingonine Carbohydrate metabolism Gluconeogenesis: through transamination reactions Glycogenolysis: Phosphorylase glycogen glucose-1 -phosphate PLP 55
PLP DEPENDANT REACTIONS Trans Sulfuration Reaction Cystathionine synthase Homocysteine + serine cystathionine PLP Cystathionase Cystathionine Homoserine + cysteine PLP B 6 deficiency : ↑ homocysteine cardiovascular disease 56

PLP DEPENDANT REACTIONS Heme synthesis : ALA synthase Glycine + Succinyl Co. A σ amino levulinic acid B 6 deficiency: anemia 57

PYRIDOXINE : SOURCES Egg, fish, meat milk, (rich sources) Beans, nuts, wheat, yeast, green leafy vegetables RDA: 1 -2 mg/day 58

PYRIDOXINE: DEFICIENCY Deficiency of vitamin B 6 may occur - During lactation - In alcoholics - During isoniazid therapy Neurological symptoms: Depression, irritability, nervousness, mental confusion and convulsions. ( decreased synthesis of GABA, serotonin, epinephrine and norepinephrine, as PLP is involved in their synthesis). PLP is involved in the synthesis of sphingolipids, so B 6 deficiency demyelination of nerves peripheral neuritis neurological manifestation 59
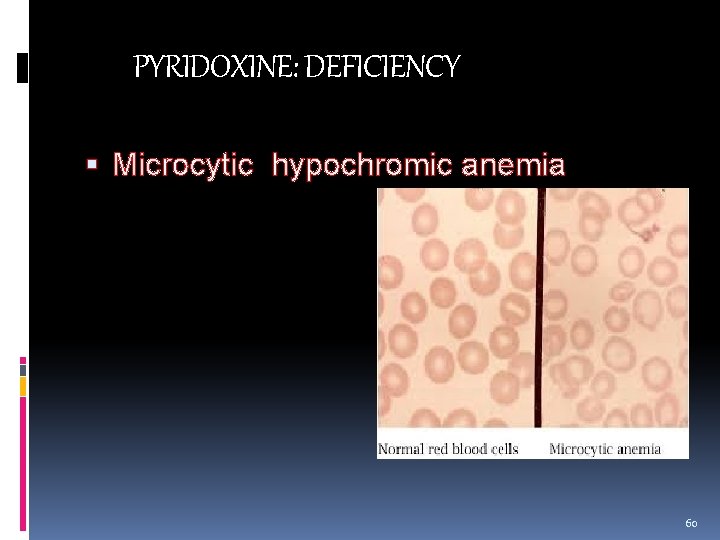
PYRIDOXINE: DEFICIENCY Microcytic hypochromic anemia 60

PYRIDOXINE - ANTIVITAMINS Isoniazid Deoxypyridoxine Methoxypyridoxine 61

VITAMIN B 7: BIOTIN Sulfur containing vitamin Anti egg white injury factor/Vitamin H Synthesized by intestinal flora Coenzyme for carboxylases 62
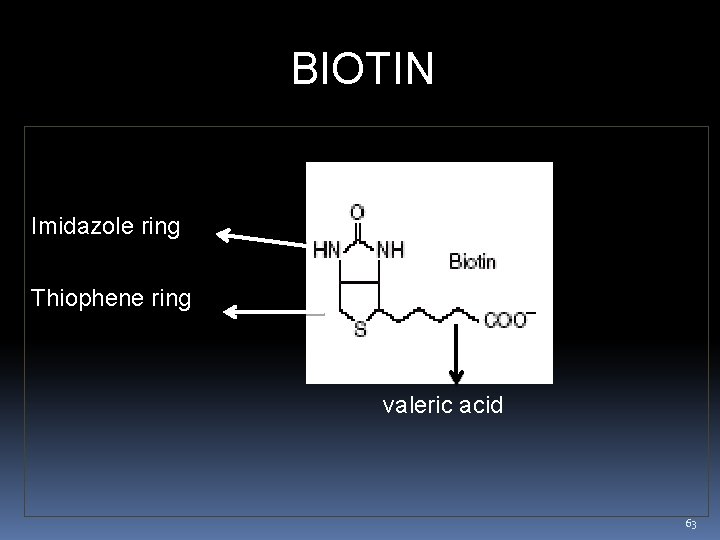
BIOTIN Imidazole ring Thiophene ring valeric acid 63

BIOTIN DEPENDANT REACTIONS Coenzyme for carboxylases Require energy from hydrolysis of ATP Biotin Substrate Biotin+CO 2 Carboxylated substrate ATP ADP+Pi 64
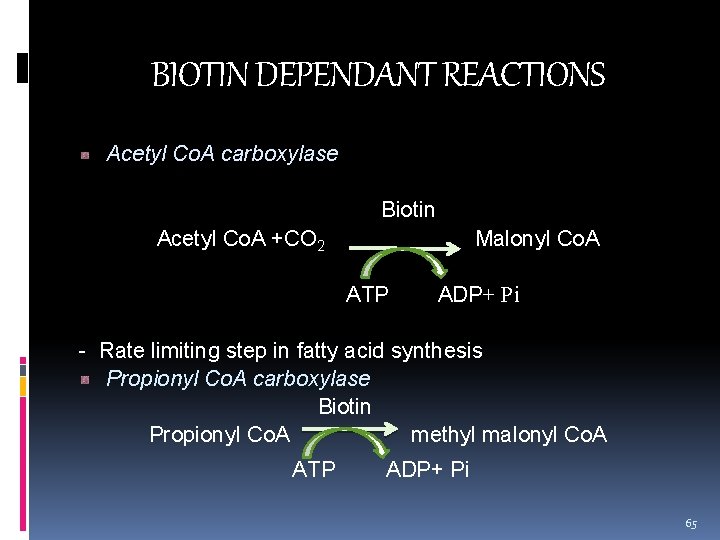
BIOTIN DEPENDANT REACTIONS Acetyl Co. A carboxylase Biotin Acetyl Co. A +CO 2 Malonyl Co. A ATP ADP+ Pi - Rate limiting step in fatty acid synthesis Propionyl Co. A carboxylase Biotin Propionyl Co. A methyl malonyl Co. A ATP ADP+ Pi 65

BIOTIN DEPENDANT REACTIONS Pyruvate carboxylase Biotin Pyruvate + CO 2 oxaloacetate ATP ADP+ Pi Substrate for TCA cycle Rate limiting enzyme in gluconeogenesis 66

BIOTIN: SOURCES widely distributed Liver Yeast Peanuts Soyabeans Milk Egg yolk Vegetables( tomato, carrot, cabbage, cucumber) intestinal bacteria can synthesise biotin RDA: 30 – 100μg/ day RDA 67

BIOTIN: DEFICIENCY Prolonged use of antibiotics High consumption of raw eggs cause deficiency Manifestations Dermatitis(erythematous rash: face) Atrophic glossitis Anorexia Neurological symptoms: hallucination, depression, lethargy, Hyperesthesia, Muscle pain 68

BIOTIN ANTAGONIST Avidin Present in egg white binds with biotin Prevent the absorption of biotin deficiency • Boiling of egg neutralize the inhibitory activity 69

BIOTIN - Antivitamins Avidin Desthiobiotin Biotin sulphonic acid 70

1. Biochemical functions of Pantothenic acid. 2. Co-enzyme functions of Pyridoxal phosphate 3. Explain the biochemical basis: a)B 6 deficiency can cause niacin deficiency. b) Administration of pyridoxine along with isoniazide in anti-tubercular treatment. 4. Name the anti-egg white injury factor, its source and coenzyme function. 71

VITAMIN B 9: FOLIC ACID Involved in one-carbon metabolism nucleotide synthesis growth reduction in homocysteine levels Most common vitamin deficiency Commonly supplemented during pregnancy 72
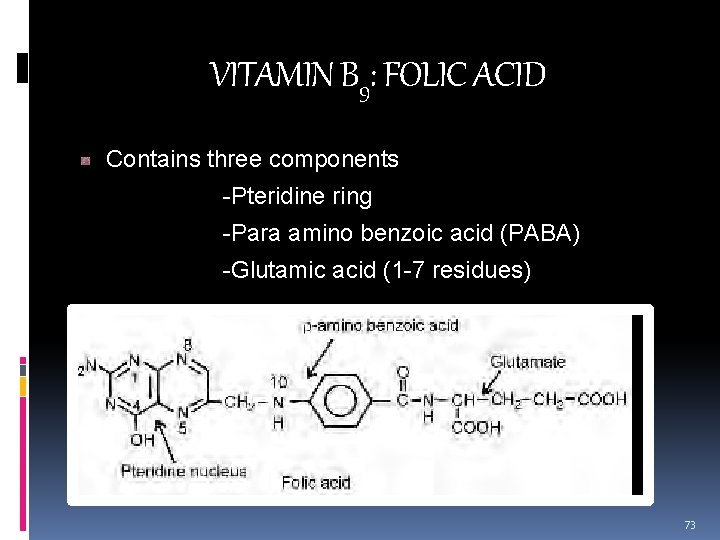
VITAMIN B 9: FOLIC ACID Contains three components -Pteridine ring -Para amino benzoic acid (PABA) -Glutamic acid (1 -7 residues) 73
![FOLIC ACID Tetrahydrofolate Coenzyme (active) form Folate reducatse Folic acid NADPH+H+ [THF] Folate reducatse FOLIC ACID Tetrahydrofolate Coenzyme (active) form Folate reducatse Folic acid NADPH+H+ [THF] Folate reducatse](http://slidetodoc.com/presentation_image_h/e6c02c18735d03c549c27f17e9a80a89/image-74.jpg)
FOLIC ACID Tetrahydrofolate Coenzyme (active) form Folate reducatse Folic acid NADPH+H+ [THF] Folate reducatse Dihydrofolate THF NADP+ NADPH+H+ NADP+ 74

FOLIC ACID: FUNCTIONS Actively involved in one carbon metabolism • Carrier of one carbon units – Formyl (-CHO) Formimino (-CH=NH) Methenyl (-CH=) Methylene (-CH 2 -) Hydroxymethyl (-CH 2 OH) Methyl (-CH 3) Bind with THF @ N 5 & / N 10 of pteroyl structure 75

FOLIC ACID: FUNCTIONS Group carrier Formyl N 5 -formyl-THFA N 10 -formyl-THFA Formimino N 5 -formimino-THFA Methenyl N 5, N 10 -methenyl-THFA Methylene N 5, N 10 –methylene-THFA Methyl N 5 -methyl-THFA Hydroxymethyl N 10 -hydroxymethyl-THFA 76

FOLIC ACID: FUNCTIONS 1. THF accepts 1 C unit from amino acid & donates it for synthesis of amino acid & nucleic acids N 10 -formyl THF nucleotide synthesis contributes to 2 nd carbon atom of purine ring N 5 N 10 -methylene-THF glycine, serine, thymidylate synthesis N 5, N 10 -methenyl-THF nucleotide synthesis Contributes to 8 th carbon of purine ring N 5 –methyl-THF Predominate form donates methyl group through S-adenosyl methionine (SAM) → transmethylation reactions 77

FOLIC ACID – One carbon metabolism 78

FOLIC ACID: FUNCTIONS 2. Folic acid prevents neural tube defects that occur during fetal development. 3. Folic acid is effective in lowering plasma homocysteine concentration in patients with coronary homocysteine artery disease. 79

FOLIC ACID: SOURCES Sources: abundant in green leafy vegetables(spinach, cauliflower) Yeast, liver, egg, vegetables, cereals, pulses and oil seeds, Beans, peas RDA: 200µg/day 400µg/day in pregnancy 80

Causes of Folate deficiency Insufficient dietary intake malabsorption Increased demand- pregnancy and lactation Administration of antifolate drugs 81

FOLIC ACID: MANIFESTATION Megaloblastic anemia Homocysteinuria Neural tube defects GIT manifestations: Vomiting, Diarrhea, Abdominal pain Anorexia, Weakness, Fatigue 82
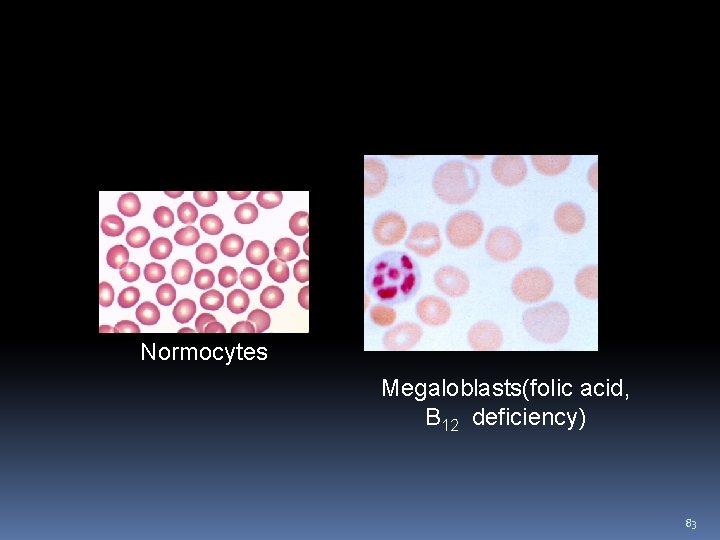
Blood picture in anemia Normocytes Megaloblasts(folic acid, B 12 deficiency) 83
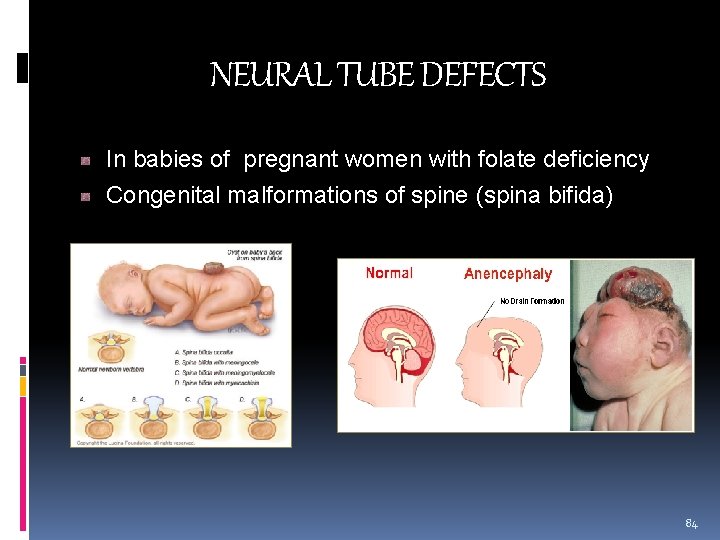
NEURAL TUBE DEFECTS In babies of pregnant women with folate deficiency Congenital malformations of spine (spina bifida) 84
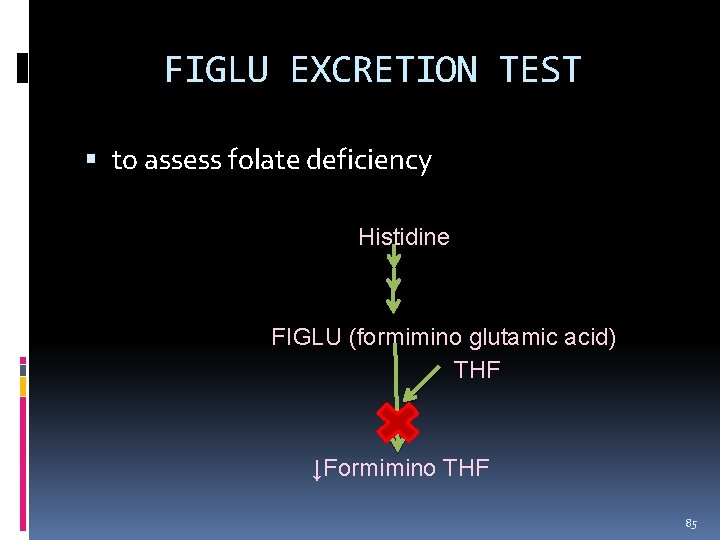
FIGLU EXCRETION TEST to assess folate deficiency Histidine FIGLU (formimino glutamic acid) THF ↓Formimino THF 85

FOLIC ACID: ANTIVITAMINS Sulfonamides- # synthesis of PABA in bacteria – used as antibiotic Methotrexate- # folate reductase →↓DNA synthesis & mitosis→ Anticancer Rx- leukemia 86

VITAMIN B 12: COBALAMIN Extrinsic factor of castle(EF) Extrinsic factor of castle Antipernicious anemia factor Contains cobalt No plant sources 87

VITAMIN B 12: COBALAMIN Pyrrole rings + Cobalt + Imidazole + R CORRIN ring+ Imidazole +R COBALAMIN +R • R group: Cyanide – Cyanocobalamin Hydroxyl – Hydroxy cobalamin Methyl - Methylcobalamin Adenosyl -- Adenosylcobalamin 88

VITAMIN B 12: COBALAMIN Active form of vitamin B 12 1. Methyl cobalamin(major form present in blood) 2. Deoxy adenosylcobalamin ( storage form) 89
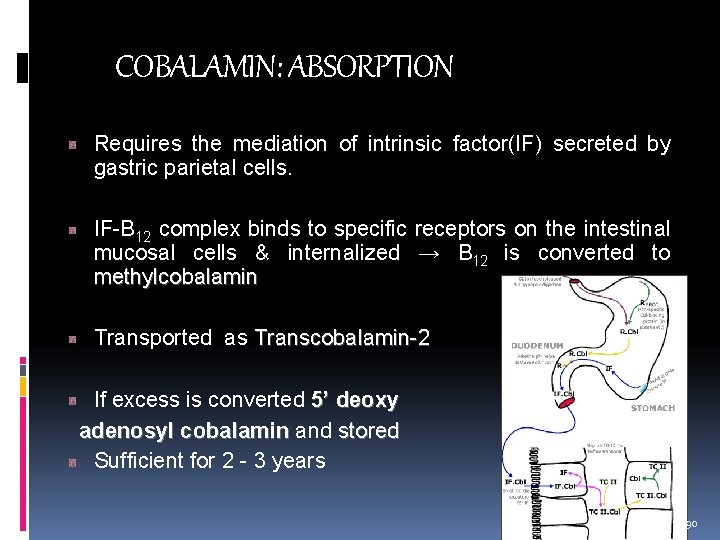
COBALAMIN: ABSORPTION Requires the mediation of intrinsic factor(IF) secreted by gastric parietal cells. IF-B 12 complex binds to specific receptors on the intestinal mucosal cells & internalized → B 12 is converted to methylcobalamin Transported as Transcobalamin-2 If excess is converted 5’ deoxy adenosyl cobalamin and stored cobalamin stored Sufficient for 2 - 3 years 90
COBALAMIN: STORAGE Unlike other water soluble vitamins, vitamin B 12 is stored in the liver and other tissues Whole liver contains about 2 mg of B 12, which is sufficient for 2 -3 years. 91
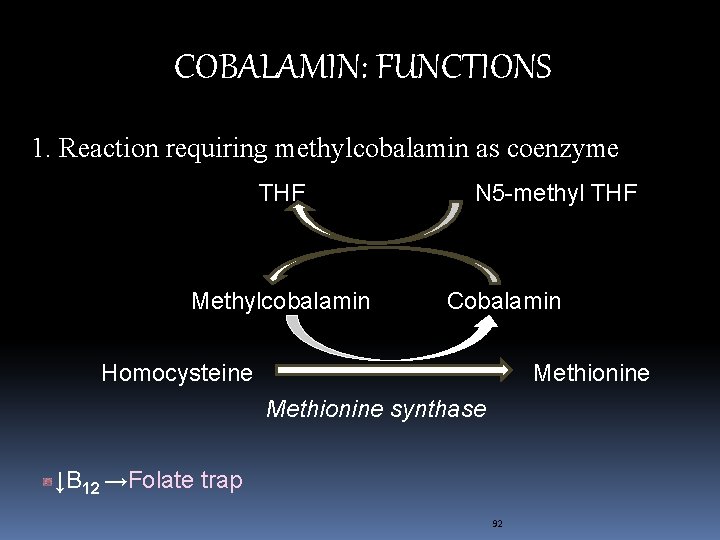
COBALAMIN: FUNCTIONS 1. Reaction requiring methylcobalamin as coenzyme THF Methylcobalamin N 5 -methyl THF Cobalamin Homocysteine Methionine synthase ↓B 12 →Folate trap 92

COBALAMIN: FUNCTIONS 2. Reactions requiring deoxyadenosylcobalamin as coenzyme Methyl malonyl Co. A isomerase Methyl malonyl Co. A Succinyl Co. A 3. Required for myelin sheath formation and proper functioning of nervous system 93

COBALAMIN: SOURCES Only animal source – Liver Meat Fish Egg Curd (lactobacillus) RDA: 1 -2µg/day RDA: 94
COBALAMIN: DEFICEIENCY CAUSES Lack of IF - common cause- Auto antibodies against parietal cells (Pernicious anemia) Malabsorption - Gastrectomy, Ileal resection Prolonged antibiotic therapy Reduced intake- elderly people, Pregnancy 95

COBALAMIN: MANIFESTATIONS 1. Megaloblastic anemia – d/t folate trap 2. Neurological disorders→non availability of methionine→defective myelin sheath→, demyelination & neurological lesions 3. Homocystinuria 4. Methyl malonic aciduria 96
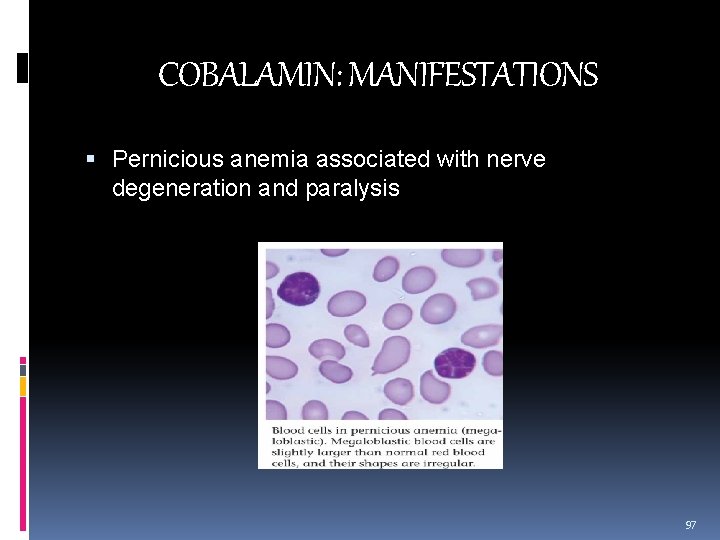
COBALAMIN: MANIFESTATIONS Pernicious anemia associated with nerve degeneration and paralysis 97

1. Describe the coenzyme forms and functions of folic acid. 2. Name two folate antagonists and their therapeutic use. 3. FIGLU excretion test 4. Explain the biochemical basis: a) Viamint B 12 deficiency may lead to megaloblastic anemia. b) B 12 deficiency can cause methyl malonyl aciduria. c) Surgical removal of stomach causes pernicious anemia. 98

VITAMIN C (ascorbic acid) - The structure of ascorbic acid closely resembles that of a hexose. - It is a strong reducing agent. The reducing property of vitamin C depends on the double bonded carbons (enediol). - L-ascorbic acid undergoes oxidation to form dehydroascorbic acid and this reaction is reversible. 99

VITAMIN C : FUNCTIONS Antioxidant function Maintaining iron or copper in the reduced state- Absorption of iron Hydroxylation reactions Prevention of formation of methemoglobin Synthesis of collagen, Epinephrine, Bile acids Immune functions Helps in wound healing 100

VITAMIN C : FUNCTIONS 1. Antioxidant function Inactivates toxic oxygen free radicals Prevent lipid peroxidation Prevent oxidation of LDL Protect lens proteins from free radical damage 101

VITAMIN C : FUNCTIONS 2. Collagen formation Collagen is a constituent of ground substance of bone, teeth, capillaries and scar tissue Vitamin C is required for hydroxylation of proline and lysine residues (post translational modification) in proto-collagen → helps in crosslinking & forms mature collagen 102
VITAMIN C : FUNCTIONS Vitamin C dependent hydroxylases Prolyl hydroxylase Proline Hydroxyproline Lysyl hydroxylase Lysine Hydroxylysine hydroxylase Protocollagen collagen (immature) vitamin C (mature) 103

VITAMIN C : FUNCTIONS Tyrosine metabolism 3. Norepinephrine synthesis Dopamine β- hydroxylase Dopamine norepinephrine vitamin C 4. Degradation of tyrosine p-hydroxyphenyl pyruvate oxidase p-hydroxyphenylpyruvate homogenisate vitamin C 104

VITAMIN C : FUNCTIONS 5. Tryptophan metabolism tryptophan hydroxylase Tryptophan 5 -hydroxy tryptophan serotonin vitamin C 105

VITAMIN C : FUNCTIONS 6. Bile acid synthesis 7α-hydroxylase cholesterol 7α- hydroxycholesterol bile acids Vitamin C 7. Steroid hormone synthesis Hydroxylation reactions in adrenal cortex needs vitamin C(corticosteroid synthesis) 106

VITAMIN C : FUNCTIONS 8. Reduces cataract formation 9. Role in iron absorption Vitamin C facilitates by reducing Fe 3+ to Fe 2+ form 10. Regeneration of hemoglobin Met Hb 11. Immunological function enhances synthesis of immunoglobulins( antibodies) increases Phagocytic action of leucocytes. 107

VITAMIN C : SOURCES Gooseberry(amla), Citrus fruits, Cabbage-type vegetables - Broccoli Strawberries, Tomatoes, Papayas, Mangoes Milk is a poor source RDA: 75 mg/day RDA 108

VITAMIN C : DEFICIENCY Cause: - Intake of foods devoid of fresh fruits and vegetables Manifestations: Scurvy - Due to 1. Formation of defective collagen 2. Low absorption of iron 109
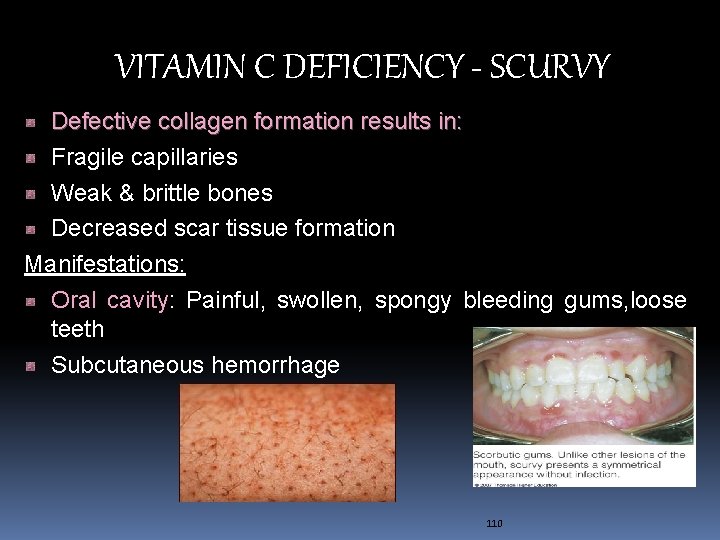
VITAMIN C DEFICIENCY - SCURVY Defective collagen formation results in: Fragile capillaries Weak & brittle bones Decreased scar tissue formation Manifestations: Oral cavity: Painful, swollen, spongy bleeding gums, loose teeth Subcutaneous hemorrhage 110
VITAMIN C DEFICIENCY - SCURVY Bone: frequent fractures Infections &Delayed wound healing Low iron absorption results in Microcytic hypochromic anemia 111

Antivitamins - naturally occurring or synthetic substances, which interfere with biological functions of vitamins. - cause deficiency symptoms similar to those observed when the corresponding vitamin is absent. 112

Antivitamins Mechanism of action of antivitamins: in one of the 3 ways: 1. The antagonist can cleave the vitamin and render it inactive. (e. g. : raw fresh water fish) contain the enzyme thiaminase which cleaves thiamine molecule. 2. Some substances can complex with the vitamins eg: avidin, (present in raw egg white) can bind with biotin and make it unavailable. 113

Antivitamins 3. Substances which have structural similarity to vitamins act as competitive inhibitor. eg dicoumarol, sulphonamides 114

Antivitamins Applications/Uses: - serve as research tools in animal experiments to generate defined vitamin deficiency states with minimal disturbance of other components of the diet. - Some of these have clinical uses. E. g. : Dicoumarol, as an anticoagulant. Methotrexate, an anticancer agent 115

1. Functions of Ascorbic acid 2. Explain the biochemical basis: a) Vitamin C deficiency may result in bleeding gums, frequent fractures and delayed wound healing. b) Vitamin C facilitates iron absorption in the intestines. 3. What are anitivitamins? Give their significance with two examples. 116

117
- Slides: 117