VWOG richtlijn vulvacarcinoom Herfst symposium VVOG Kinepolis Brugge

VWOG richtlijn vulvacarcinoom Herfst symposium. VVOG Kinepolis Brugge Frédéric Amant Namens VWOG bestuur

Tissue is the issue! • Vulvar intraepithelial disease • Squamous cell carcinoma (90%) • Verrucoid cancer • Basal cell ca • Adenocarcinoma • Paget’s disease • Bartholin gland carcinoma (40% squamous) • Melanoma • Malignant mesenchymal tumors • Metastatic
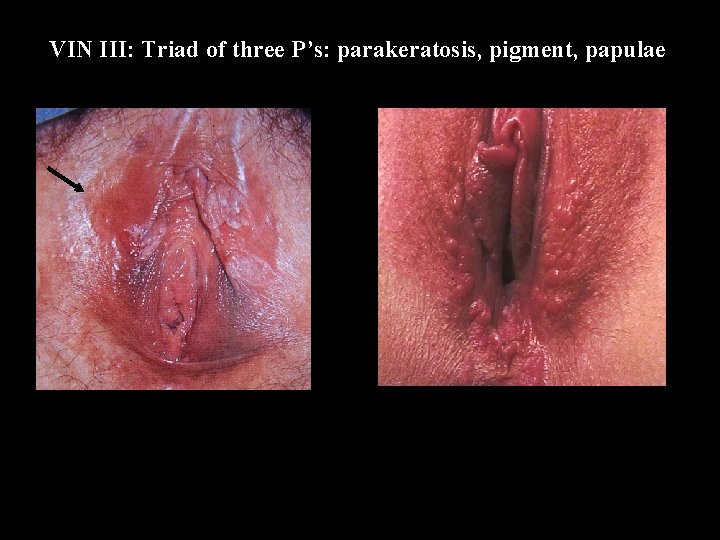
VIN III: Triad of three P’s: parakeratosis, pigment, papulae

Vulvar Intraepithelial Neoplasia • Low grade VIN: subclinical HPV infection • High grade VIN: - moderate to severe dysplasia - undisputed malignant potential - 30 -50% co-existence with vulvar ca - S/ no, pruritus, burning, pain, dysuria - R/ surgical excision (laser, cold knife)
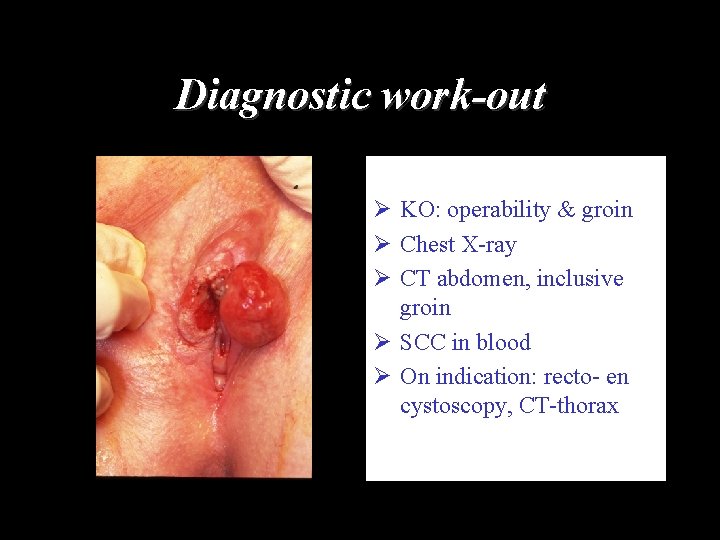
Diagnostic work-out Ø KO: operability & groin Ø Chest X-ray Ø CT abdomen, inclusive groin Ø SCC in blood Ø On indication: recto- en cystoscopy, CT-thorax

Treatment modalities in vulvar cancer • Stage Ia (< 1 mm depth of invasion 0% + inguin LN partial vulvectomy • Stage Ib-III (partial) vulvectomy inguinofemoral lymphadenectomy/ sentinel node procedure • Stage IVa exenteration/neoadjuvant CT/45 -65 Gy • Stage IVb palliation
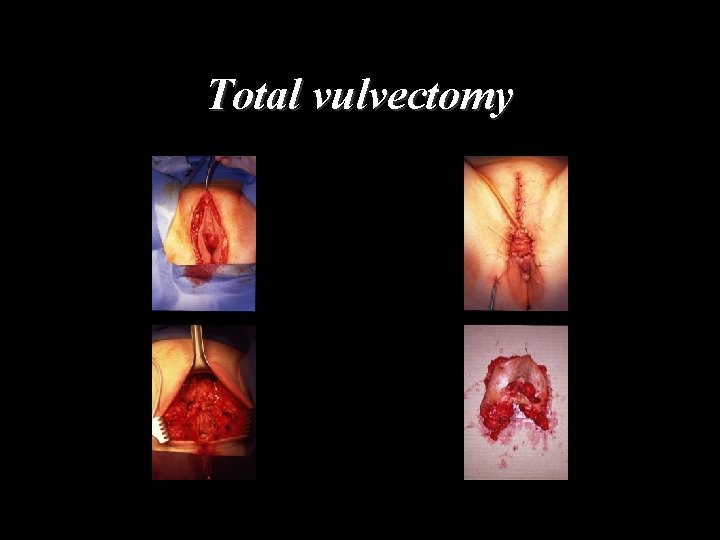
Total vulvectomy

The price of less radical surgery • Surgical tumor-free margin – > 8 mm: no vulvar recurrence, n=91 – < 8 mm: 21/44 (48%) vulvar recurrence • Heaps et al. , Gynecol Oncol 1990; 38: 309 -14 • Surgical tumor-free margin – >8 mm: no vulvar recurrence, n=39 – < 8 mm: 9/40 (22. 5%) vulvar recurrence • de Hullu et al. , Cancer 2002; 95: 2331 -8

What is an adequate resection margin? Ibrahim et al. , IGCS 2006, Santa Monica Abstract 36 • 15 consecutive patients • At least 10 mm clear margin macroscopically • Reduction of clear margin – – 15% post resection 15% tissue fixation 15% microscopically Totalling 45% reduction • 1 cm is insufficient as macroscopic margin
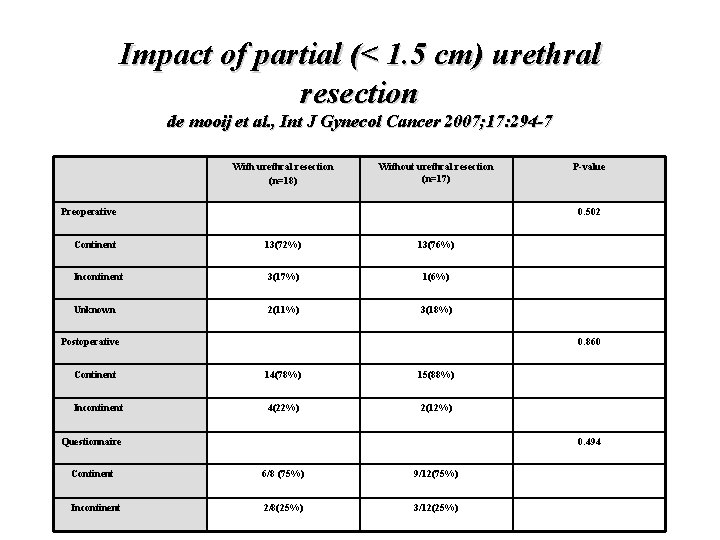
Impact of partial (< 1. 5 cm) urethral resection de mooij et al. , Int J Gynecol Cancer 2007; 17: 294 -7 With urethral resection (n=18) Without urethral resection (n=17) Preoperative P-value 0. 502 Continent 13(72%) 13(76%) Incontinent 3(17%) 1(6%) Unknown 2(11%) 3(18%) Postoperative 0. 860 Continent 14(78%) 15(88%) Incontinent 4(22%) 2(12%) Questionnaire 0. 494 Continent 6/8 (75%) 9/12(75%) Incontinent 2/8(25%) 3/12(25%)
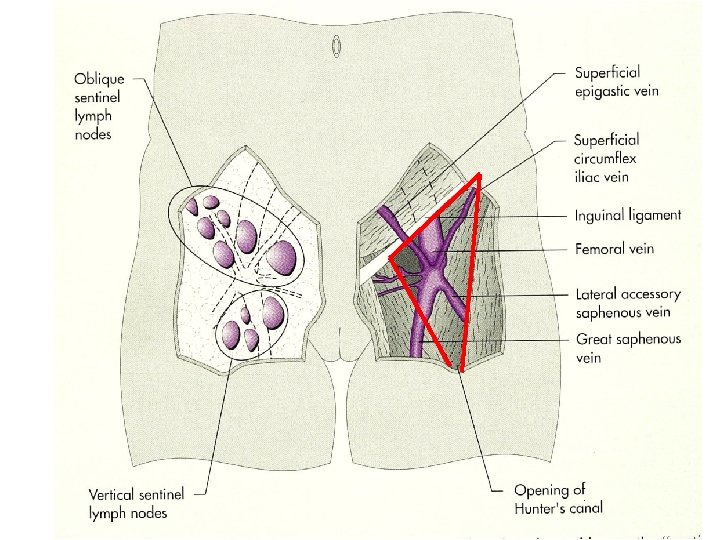
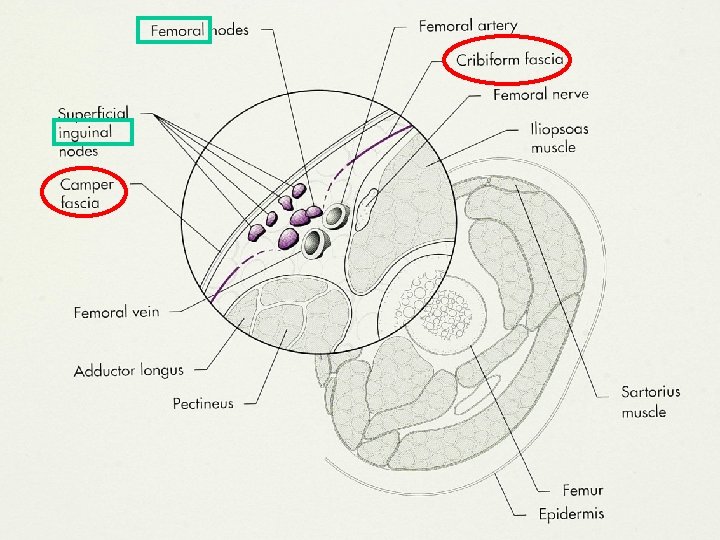
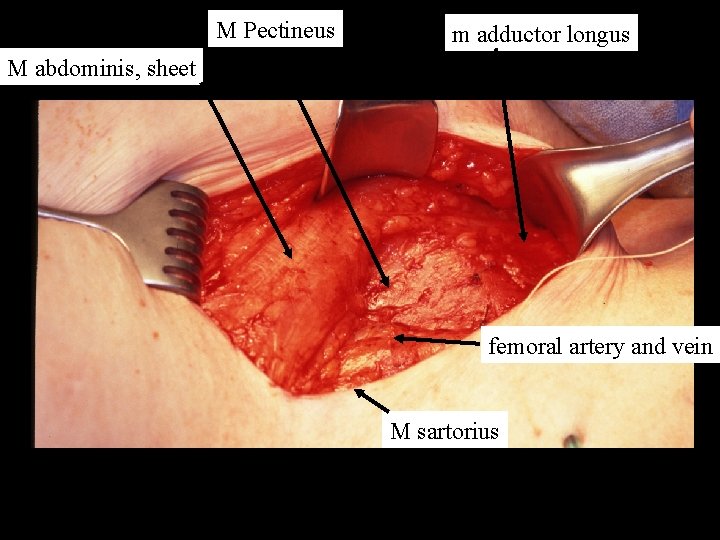
M Pectineus m adductor longus M abdominis, sheet femoral artery and vein M sartorius

Apex of the femoral triangle Femoral vein Sartorius muscle Femoral artery

Ipsilateral superficial inguinal lymphadenectomy Stehman et al. , Obstet Gynecol 1992; 79: 490 -7 Ø Prospective evaluation Ø N = 155 Ø 7. 3% inguinal recurrence rate Ø Historical control: 0% inguinal recurrence rate Recurrence rate varies from 0 -8. 6% (Berman 1989; Stehman 1992; Burke 1995; Gordinier 2003; Kirby 2005) Number of recurrences attributable to decision to leave the femoral nodes

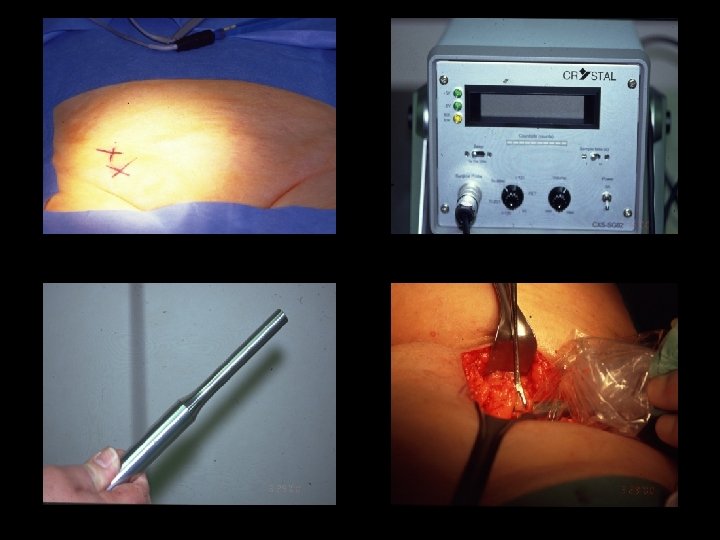
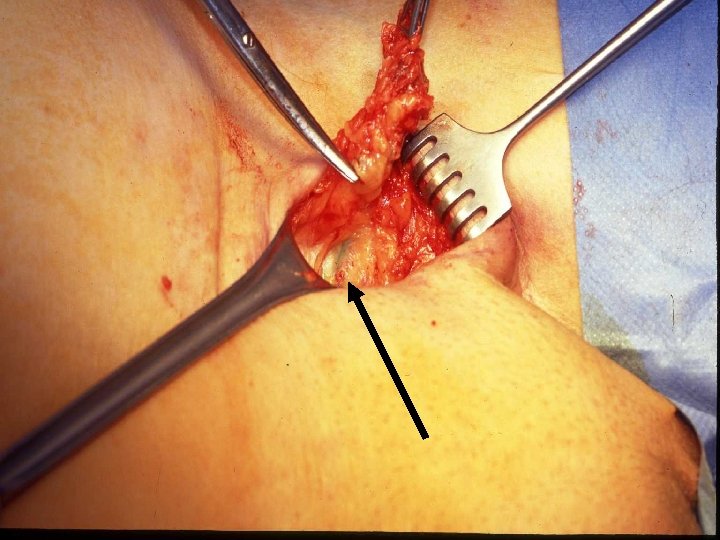
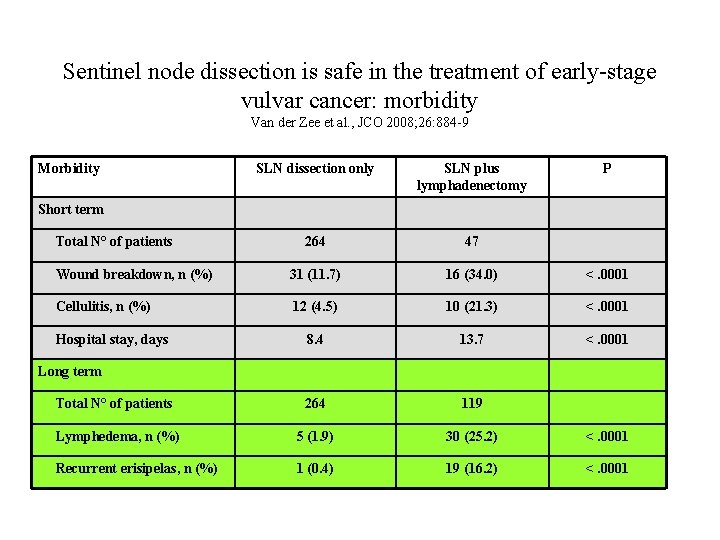
Sentinel node dissection is safe in the treatment of early-stage vulvar cancer: morbidity Van der Zee et al. , JCO 2008; 26: 884 -9 Morbidity SLN dissection only SLN plus lymphadenectomy P 264 47 Wound breakdown, n (%) 31 (11. 7) 16 (34. 0) <. 0001 Cellulitis, n (%) 12 (4. 5) 10 (21. 3) <. 0001 8. 4 13. 7 <. 0001 Total N° of patients 264 119 Lymphedema, n (%) 5 (1. 9) 30 (25. 2) <. 0001 Recurrent erisipelas, n (%) 1 (0. 4) 19 (16. 2) <. 0001 Short term Total N° of patients Hospital stay, days Long term
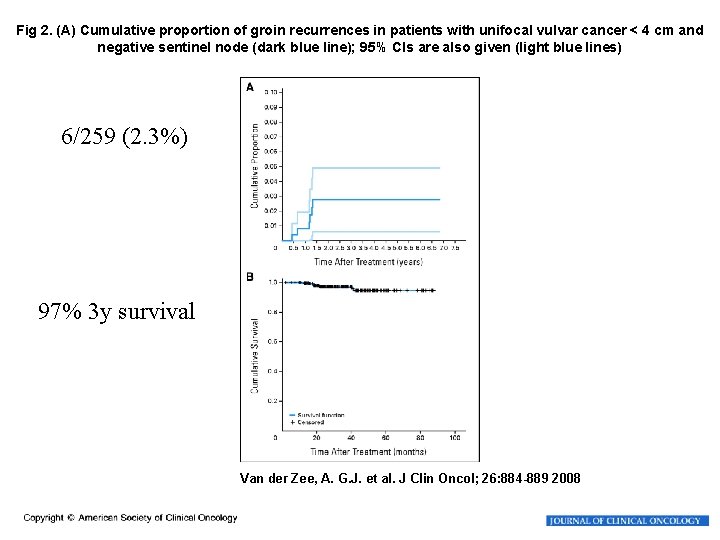
Fig 2. (A) Cumulative proportion of groin recurrences in patients with unifocal vulvar cancer < 4 cm and negative sentinel node (dark blue line); 95% CIs are also given (light blue lines) 6/259 (2. 3%) 97% 3 y survival Van der Zee, A. G. J. et al. J Clin Oncol; 26: 884 -889 2008

Sentinel node dissection is safe in the treatment of early-stage vulvar cancer: quality control at each step Van der Zee et al. , JCO 2008; 26: 884 -9 Injection of radioactive tracer Interpretation of lymphoscintigram Surgeon: 10 patients/year/surgeon Pathology: experience with ultrastaging
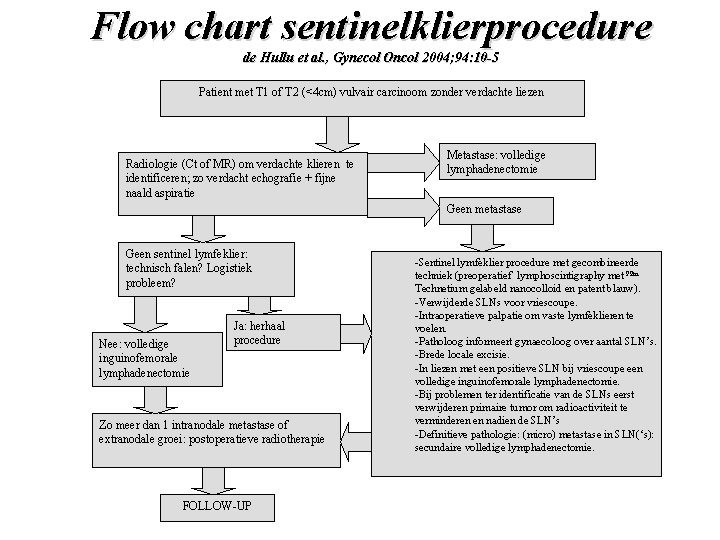
Flow chart sentinelklierprocedure de Hullu et al. , Gynecol Oncol 2004; 94: 10 -5 Patient met T 1 of T 2 (<4 cm) vulvair carcinoom zonder verdachte liezen Radiologie (Ct of MR) om verdachte klieren te identificeren; zo verdacht echografie + fijne naald aspiratie Metastase: volledige lymphadenectomie Geen metastase Geen sentinel lymfeklier: technisch falen? Logistiek probleem? Nee: volledige inguinofemorale lymphadenectomie Ja: herhaal procedure Zo meer dan 1 intranodale metastase of extranodale groei: postoperatieve radiotherapie FOLLOW-UP -Sentinel lymfeklier procedure met gecombineerde techniek (preoperatief lymphoscintigraphy met 99 m Technetium gelabeld nanocolloid en patent blauw). -Verwijderde SLNs voor vriescoupe. -Intraoperatieve palpatie om vaste lymfeklieren te voelen. -Patholoog informeert gynaecoloog over aantal SLN’s. -Brede locale excisie. -In liezen met een positieve SLN bij vriescoupe een volledige inguinofemorale lymphadenectomie. -Bij problemen ter identificatie van de SLNs eerst verwijderen primaire tumor om radioactiviteit te verminderen en nadien de SLN’s -Definitieve pathologie: (micro) metastase in SLN(‘s): secundaire volledige lymphadenectomie.

Indications for postop radiochemotherapy of the groin and ipsilateral hemipelvis Vulvar Inguinofemoral > 4 cm Ø < 8 mm resection margin Significant lymfatic permeation Macrosc + nodes 2 microscopic nodes
- Slides: 23