Vulvovaginal candidiasis Learning outcomes By the end of

Vulvovaginal candidiasis

Learning outcomes • By the end of this lecture you will be • Respond to symptoms presented to your pharmacy seeking for pharmaceutical and nonpharmaceutical advice for vaginal symptoms and period pain • Understand the treatment of candidal valvovaginitis and period pain

Think of this scenario • Miss BE, 27 years old. Asked if she can buy something for thrush. Her symptoms include vaginal discharge and itch. She is embarrassed about having to answer questions and are worried that the conversation may be overheard. What would you do?

Introduction • Women often seek to buy products for feminine itching and may be embarrassed to seek advice or answer what they see as intrusive questions • Before making any recommendation it is vital to question the patient to identify the probable cause of the symptoms. • There are three type of infections accounts for most vaginal symptoms; bacterial vaginosis, candidal valvovaginitis and trichomoniasis.

Questions we must ask • Age • Vaginal candidiasis (thrush) is common in women of childbearing age • Pregnancy and diabetes are strong predisposing factors. • This infection is rare in children and in postmenopausal women because of the different environment in the vagina. • Women of childbearing age have a vaginal p. H is generally acidic (low p. H) and contains glycogen • Whilst children and menopausal women tends to be alkaline (high p. H) and does not contain large amounts of glycogen.

• The lack of oestrogen in children and postmenopausal women means this protective barrier is not present, with a consequent increased tendency to bacterial (but not fungal) infection • Women under 16 or over 60 years complaining of symptoms of vaginal thrush should be referred to their doctor

• Duration • Some women delay seeking advice from the pharmacist or doctor because of embarrassment about their symptoms. • They may have tried an OTC product or a prescription medicine already (check for this) • Symptoms (ask the patient to describe her symptoms) • Itch (pruritus) • Dermatitis, allergic or irritant dermatitis may be responsible for vaginal • It is worth asking whether the patient has recently used any new toiletries (e. g. soaps, bath or shower products). • Regular washing with warm water is all that is required to keep the vagina clean and maintain a healthy vaginal environment.

• Candidiasis (thrush) • White creamy batches , the itch associated with thrush is often intense and burning in nature. • Discharge • Vagina naturally produces a watery discharge and cervical mucus is also produced, which changes consistency at particular times of the menstrual cycle. • Watery or slightly thicker, with no associated odour. • The most common infective cause of vaginal discharge is candidiasis. • Cream-coloured, thick and curdy • Does not usually produce an unpleasant odour
• Infection leading to discharge described as yellow or greenish (Fishy odor) is more likely to be bacterial in origin, e. g. bacterial vaginosis, chlamydia or gonorrhoea. • Dysuria (pain on urination) • Dysuria may be present and scratching the skin in response to itching might be responsible, although dysuria may occur without scratching. • Sometimes the pain on passing urine may be mistaken for cystitis • Lower abdominal pain or dysuria are indications for referral because of their possible link with kidney infections

• Previous history • Recurrent thrush is a problem for some women, often following antibiotic treatment • Recurrent infections are defined as ‘four or more episodes of symptomatic candidosis annually’ • Woman who has experienced more than two attacks of thrush during the previous 6 months should be referred to the doctor. • Repeated thrush infections may indicate an underlying problem or altered immunity and further investigation is needed.

• Pregnancy • During pregnancy almost 1 in 5 women will have an episode of vaginal candidiasis. • This high incidence has been attributed to hormonal changes • Any pregnant woman with thrush should be referred to the doctor. • Diabetes • Candida is able to grow more easily in diabetic patients because of the higher glucose levels in blood and tissues • Recurrent vaginal thrush can be a sign of undiagnosed diabetes or, in a patient who has been diagnosed, of poor diabetic control.

• Oral steroids • Patients taking oral steroids may be at increased risk of candidal infection • Immunocompromised patients • Patients with HIV or AIDS are prone to recurrent thrush infection • Cancer chemotherapy are also at risk of infection.

• Oral contraceptives • oral contraceptive pill (OCP) is linked to the incidence of vaginal candidiasis; however, oral contraceptives are no longer considered a significant precipitating factor. • Antibiotics • Broad-spectrum antibiotics can predispose to candidal overgrowth. • Some women find that an episode of thrush follows every course of antibiotics they take. • The doctor may prescribe an antifungal at the same time as the antibiotic in such cases.

When to refer • • • Pregnancy or suspected pregnancy More than two attacks in the previous 6 months Previous history of sexually transmitted disease Exposure to partner with sexually transmitted disease Patient under 16 or over 60 years Abnormal or irregular vaginal bleeding/ blood staining of vaginal discharge Vulval or vaginal sores, ulcers or blisters Associated lower abdominal pain or dysuria Adverse effects (redness, irritation or swelling associated with treatment) No improvement within 7 days of treatment

Management • Uncomplicated vulvovaginal candidiasis is defined as sporadic episodes with mild symptoms in normal host. • Complicated candidiasis is defined as a vulvovaginal yeast infection that has one or more of the following characteristics: recurrent, severe, non-albicans, pregnancy, and compromised host.

Uncomplicated vulvovaginal candidiasis • Single-dose intravaginal and oral azole preparations are effective in treating vaginal candidiasis. A Cochrane review found them to be equally effective. • Intravaginal (topical ) azole antifungals, including both the imidazoles and triazoles. • Alternatively, oral therapy with fluconazole (Diflucan) can be used.

• Intravaginal (topical ) azole antifungals might be advocated over all for the limited systemic absorption and exposure usually resulting in a reduction of systemic adverse effects and drug interactions. • However, it is important to remember that although the absorption of topical agents is minimal, drug interactions (e. g. , topical azole antifungals and warfarin) have been rarely reported. In addition, local reactions such as burning or irritation may occur in some patients.
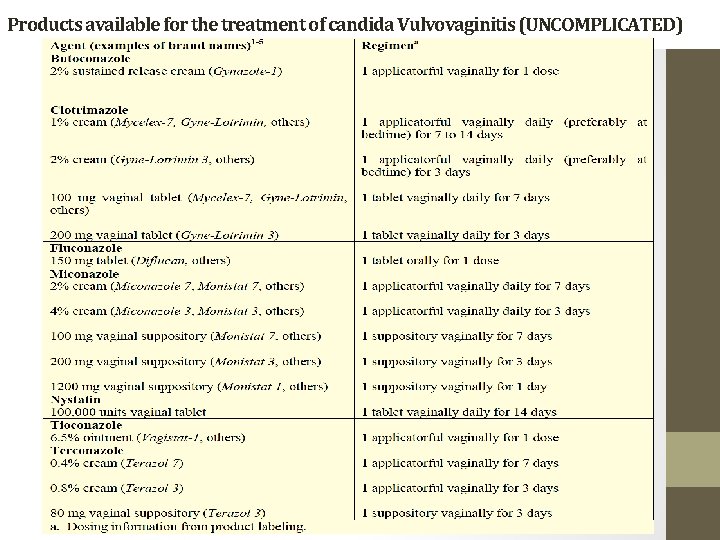
Products available for the treatment of candida Vulvovaginitis (UNCOMPLICATED)

• Topical preparations give quicker initial relief, however they may sometimes exacerbate burning sensations initially, and oral • Oral therapies are effective, but it may be 12– 24 h before symptoms improve. • In general, all of these regimens are considered similarly (80% to 90%) effective. • Chose is based on patient’s preference, cost etc. • Oral therapy could be also Itraconazole (200 mg/day for 3 days or 400 mg/day as a single use) or Ketoconazole 400 mg/day for 5 days • All Azoles are superior to nystatin

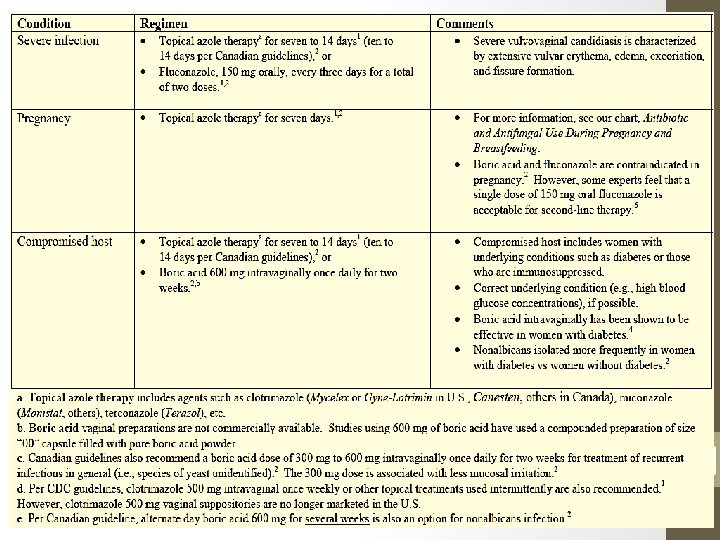
Complicated case • The treatment varies depending on the undelaying cause of complication • In pregnant women with diagnosed vulvovaginal candidiasis, topically administered azole therapy (butoconazole, clotrimazole, miconazole) for seven days is recommended. • Women with underlying conditions such as uncontrolled diabetes or those receiving corticosteroid therapy often do not respond to short-course therapies, and more prolonged therapy (e. g. , seven to 14 days of therapy) is necessary. • E. g. Fluconazole 150 mg (two days given 3 days apart) • Non –albicans candida respond to intravaginal terconazole (Fluconazole poor activity against Non –albicans)

Treatment of Complicated Yeast Infections 21
22

Otherapies ( student presentations) • Boric acid • Oral lactobacillus and lactobacillus containing yogurt • Local anesthetics such as benzocaine (Vagisil cream, others)

Practical tips to respond to vaginal thrush • The pharmacist should make sure that the patient knows how to use the product. An effective way to do this is to show the patient the leaflet instructions. • Oral fluconazole should not be recommended during pregnancy or for nursing mothers because it is excreted in breast milk. • Requests for a named product may be an attempt to avoid discussion. However, a careful response is needed to ensure that the product is appropriate.

Practical tips to respond to vaginal thrush • Men may be infected with Candida without showing any symptoms • Expert opinion is that male partners without symptoms should not be treated, this remains an area of debate. • Symptomatic males with candidal balanitis (penile thrush) and whose female partner has vaginal thrush should be treated. • An azole cream can be used twice daily, applied under the foreskin for 6 days. Oral fluconazole can also be used.

Responding to period pain (Dysmenorrhoea) • It has been estimated that as many as one in two women suffer from dysmenorrhoea (period pains). • Up to one in ten of those affected will have severe symptoms, which necessitate time off school or work. • Pharmacists should remain aware that discussing menstrual problems is potentially embarrassing for the patient and should therefore try to create an atmosphere of privacy.

• Primary dysmenorrhoea is defined as pain in the absence of pelvic disease, whereas secondary dysmenorrhoea refers to pain, which may be due to underlying disease. • Secondary dysmenorrhoea is most common in women aged over 30 years and is rare in women aged under 25 years. • Common causes of secondary dysmenorrhoea include endometriosis or PID. Primary dysmenorrhoea is uncommon after having children.

• Previous history • Dysmenorrhoea is often not associated with the start of menstruation (menarche). This is because during the early months (and sometimes years) of menstruation, ovulation does not occur. • Anovulatory cycles are usually, but not always, pain free and therefore women sometimes describe period pain that begins after several months or years of pain-free menstruation.

Timing and nature of pains Primary dysmenorrhoea • Primary dysmenorrhoea classically presents as a cramping lower abdominal pain that often begins during the day before bleeding starts. • The pain gradually eases after the start of menstruation and is often gone by the end of the first day of bleeding. Mittelschmerz is ovulation pain which occurs midcycle, at the time of ovulation. The abdominal pain usually lasts for a few hours, but can last for several days and may be accompanied by some bleeding.

Secondary dysmenorrhoea • The pain of secondary or acquired dysmenorrhoea may occur during other parts of the menstrual cycle and can be relieved or worsened by menstruation. • Such pain is often described as a dull, aching pain rather than being spasmodic or cramping in nature. Often occurring up to 1 week before menstruation, the pain may get worse once bleeding starts. • The pain may occur during sexual intercourse. • Secondary dysmenorrhoea is more common in older women, especially in those who have had children. • In pelvic infection, a vaginal discharge may be present in addition to pain. • If, the pharmacist suspects secondary dysmenorrhoea, the patient should be referred to her doctor further investigation.

Endometriosis • Endometriosis mainly occurs in women aged between 30 and 45 years, but can occur in women in their twenties. • The womb (uterus) has a unique inner lining surface (endometrium). In endometriosis, pieces of endometrium are also found in places outside the uterus. These isolated pieces of endometrium may lie on the outside of the uterus or ovaries, or elsewhere in the pelvis. • The pain usually begins up to 1 week before menstruation and both lower abdominal and lower back pain may occur. • The pain may also be non-cyclical and may occur with sexual intercourse (dyspareunia). • Endometriosis may cause subfertility. Diagnosis can be confirmed by laparoscopy.

• Other symptoms • Women who experience dysmenorrhoea will often describe other associated symptoms. These include nausea, vomiting, general GI discomfort, constipation, headache, backache, fatigue, feeling faint and dizziness. • oral contraceptives • Women taking oral contraceptives usually find that the symptoms of dysmenorrhoea are reduced or eliminated altogether. Any woman presenting with the symptoms of dysmenorrhoea and who is taking OCP is probably best referred to the doctor further investigation.

When to refer • • Presence of abnormal vaginal discharge Abnormal bleeding Symptoms suggest secondary dysmenorrhoea Severe intermenstrual pain (mittelschmerz) and bleeding Failure of medication Pain with a late period (possibility of an ectopic pregnancy) Presence of fever

Management • If the pain of primary dysmenorrhoea is not improved after two cycles of treatment; refer to the doctor • NSAIDs (Ibuprofen, diclofenac and naproxen) • NSAIDs can be considered the treatment of choice for dysmenorrhoea, provided they are appropriate for the patient (i. e. the pharmacist has questioned the patient about previous use of aspirin, and history of GI problems and asthma). • Paracetamol has little or no effect on the levels of prostaglandins involved in pain and inflammation and so it is theoretically less effective for the treatment of dysmenorrhoea than either NSAIDs or aspirin.

• Hyoscine, a smooth muscle relaxant, is marketed for the treatment of dysmenorrhoea on theoretical basis that the antispasmodic action will reduce cramping. In fact, the dose is so low (0. 1 -mg hyoscine) that such an effect is unlikely.

Role play • BB is a neighbor of your pharmacy , a university aged girl , she asked for something to treat thrush? You walk with Her to a quiet area of your pharmacy where your conversation will not be overheard. Initially, she was resistant to your involvement, asking why you need to ask all these personal questions. How you would respond?

After you have explained that you are required to obtain information before selling these products and that, in any case, you need to be sure that the problem is thrush and not a different infection, she seemed happier. She has not had thrush or any similar symptoms before but described her symptoms to her sister who made the diagnosis. • The worst symptom is itching. • BB described small quantities of a cream-coloured discharge. • She is not taking any medicines and does not have any existing illnesses or conditions. What would d you recommend to her?
Role play • Na. Na, is a young woman aged about 26 years, who asks your • advice about painful periods. • What to do?

• From your questioning, you find that Na. Na has lower abdominal pain and sometimes backache, which starts several days before her period begins. Her menstrual cycle used to be very regular, but now tends to vary; sometimes she has only 3 weeks between periods. The pain continues throughout menstruation and is quite severe. She has tried taking aspirin, which did not have much effect. • What would you recommend?
- Slides: 39