VRHA Health Information Technology Project Primary Care Conference




















- Slides: 30

VRHA Health Information Technology Project Primary Care Conference May 17, 2011

What is VRHA? • VRHA is the VT Rural Health Alliance • VRHA is a Health Center Controlled Network • VRHA is a program of Bi-State • VRHA was initially funded as a Network by the Office of Rural Health Policy (with some seed money from the State Office of Rural Health). 2

VRHA Purpose The primary purpose of VRHA is to work collaboratively on putting state and federal health policy initiatives into practice, leveraging shared resources and expertise for common benefit focused on shared missions of access to high quality health care for the medically underserved, including uninsured and underinsured, regardless of ability to pay. 3

VRHA Membership • • Bi-State Primary Care Association VT FQHCs (8) North Country Health Systems Vermont Coalition of Clinics for the Uninsured (VCCU) Vermont’s Area Health Education Center (AHEC) Network Vermont Information Technology Leaders (VITL) Vermont Program for Quality in Health Care (VPQHC) Participation in the VRHA HIT Project is limited to the eight VT FQHCs. VRHA is viewed as a “statewide” HCCN because all VT FQHCs are participating in the network. 3

National HIT Initiatives • Expansion of regional and statewide Health Information Exchange (HIE). • Development of a National Health Information Network (NHIN). • ARRA funding to drive Electronic Health Record (EHR) adoption through incentive programs and grants. • Achieve pervasive use of data to support quality improvement and accountability. • Create standards and implementation guides for a robust privacy and security infrastructure 5

Vermont HIT Initiatives • Expanding the Vermont Health Information Exchange (VHIE) to encompass data exchange between hospitals, ambulatory providers, long term care, mental health and home health. • Implementing a statewide Clinical Data Repository (CDR) to support expansion of the Vermont Blueprint for Health medical home payment reform model. • Enabling adoption of Electronic Health Records by primary care providers and critical access hospitals throughout the state through the ARRA funded Regional Extension Center. • Connecting the statewide Immunization Registry to the VHIE. 6

Project Goals • Patient data in each FQHC’s Electronic Health Record is structured, reliable, complete and reportable. • Clinical Data Repository is populated with data from all FQHCs • Clinical UDS reporting is automated in EHR or CDR • Network-wide comparative reporting is available through the CDR • HIE connectivity is implemented at each FQHC • FQHCs complete EHR implementation and achieve Meaningful Use • Workflow redesign and Continuous Quality Improvement are used to ensure lasting benefits 7

Project Participants • Eight FQHCs encompassing 36 primary care medical practices • 100+ providers • More than 100, 000 patients 8

Project Funding and Timeline • Project is funded by a $2. 2 M Health Resources and Services Administration (HRSA) grant and with over $500 K from Vermont’s HIT Fund. • Federal funds are allocated for: – Data integrity work – Data Feed to the VT Health Information Exchange (VHIE) & Clinical Data Repository (CDR) - Doc. Site – Creation of additional Doc. Site registry reports for UDS clinical data (beyond the Blueprint) – EHR templates, workflow design and training as needed • State funds are allocated for Incentive payments to health centers for achieving project goals • HRSA Grant runs through May 2012. 9

Project Outcomes – Reporting UDS Data without Chart Pulls – Blueprint Medical Home Participation – CMS Meaningful Use Incentive Payments – Data sharing with hospitals and other health care providers – Clinical Benchmarking / Networklevel QI Activities 10

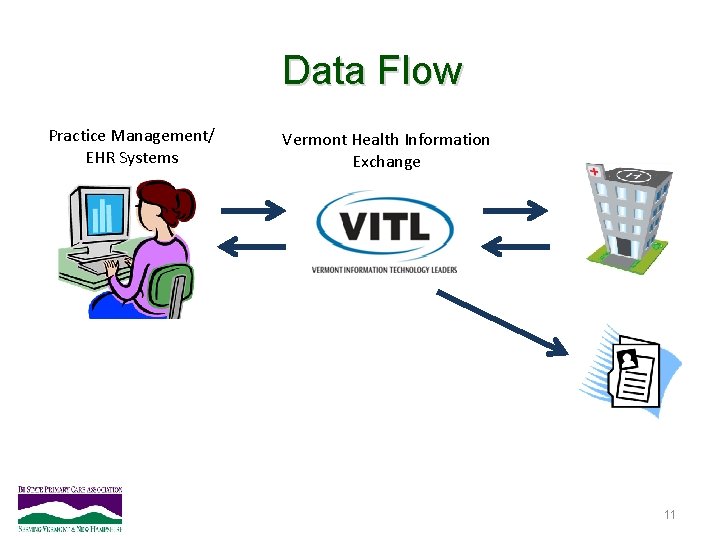
Data Flow Practice Management/ EHR Systems Vermont Health Information Exchange 11

Who’s On First, What’s on Second… 12

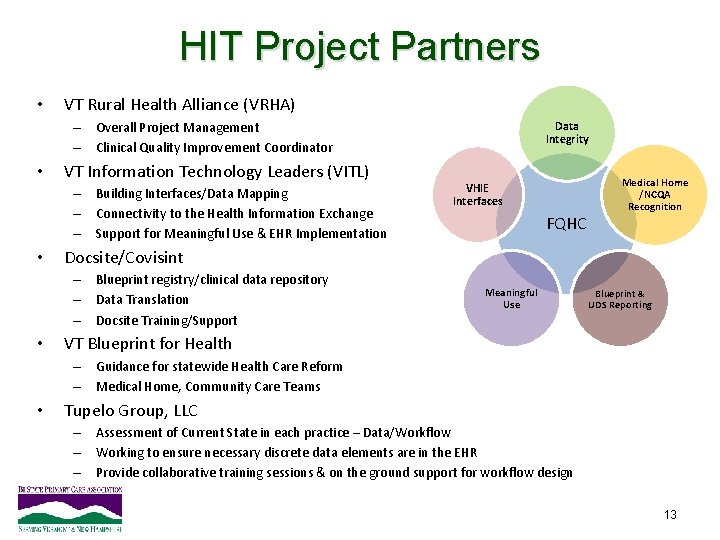
HIT Project Partners • VT Rural Health Alliance (VRHA) – Overall Project Management – Clinical Quality Improvement Coordinator • VT Information Technology Leaders (VITL) – Building Interfaces/Data Mapping – Connectivity to the Health Information Exchange – Support for Meaningful Use & EHR Implementation • VHIE Interfaces FQHC Medical Home /NCQA Recognition Docsite/Covisint – Blueprint registry/clinical data repository – Data Translation – Docsite Training/Support • Data Integrity Meaningful Use Blueprint & UDS Reporting VT Blueprint for Health – Guidance for statewide Health Care Reform – Medical Home, Community Care Teams • Tupelo Group, LLC – Assessment of Current State in each practice – Data/Workflow – Working to ensure necessary discrete data elements are in the EHR – Provide collaborative training sessions & on the ground support for workflow design 13

On The Ground Activity 14

“DATA YOU CAN TRUST ” 15

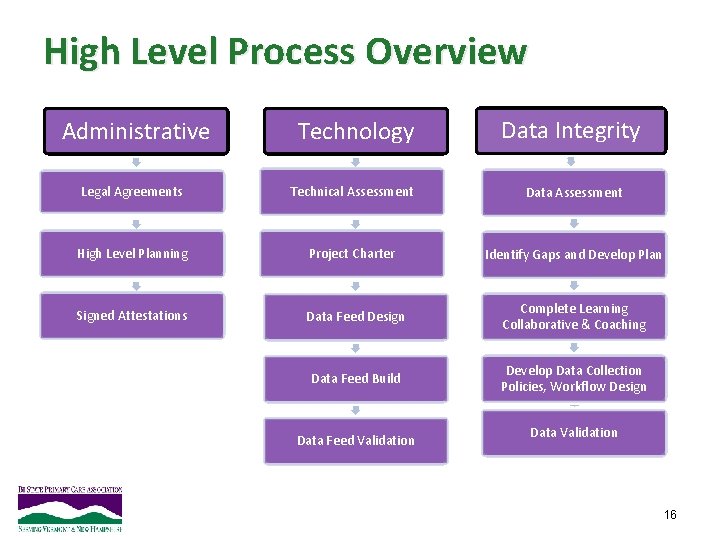
High Level Process Overview Administrative Technology Data Integrity Legal Agreements Technical Assessment Data Assessment High Level Planning Project Charter Identify Gaps and Develop Plan Signed Attestations Data Feed Design Complete Learning Collaborative & Coaching Data Feed Build Develop Data Collection Policies, Workflow Design Data Feed Validation Data Validation 16

A Collaborative Approach • 4 Waves – 2 FQHC organizations in each wave – Interdisciplinary teams from each practice/organization – 4 months of intensive data integrity work • Focus during 4 -month waves – Diabetes – Hypertension – Childhood Immunizations • Focus through May 2012 – Remainder of UDS/Blueprint measures – Clinical Outcomes 17

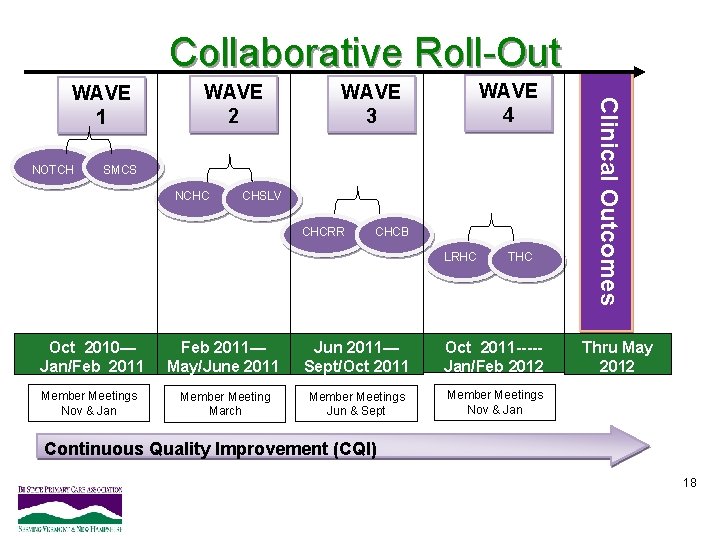
Collaborative Roll-Out NOTCH WAVE 2 WAVE 4 WAVE 3 SMCS NCHC CHSLV CHCRR CHCB LRHC THC Oct 2010— Jan/Feb 2011— May/June 2011 Jun 2011— Sept/Oct 2011 ----Jan/Feb 2012 Member Meetings Nov & Jan Member Meeting March Member Meetings Jun & Sept Member Meetings Nov & Jan Clinical Outcomes WAVE 1 Thru May 2012 Continuous Quality Improvement (CQI) 18

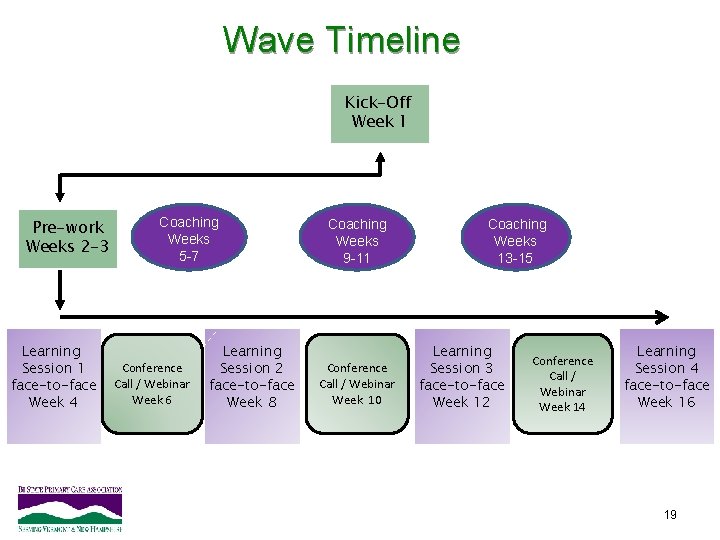
Wave Timeline Kick-Off Week 1 Pre-work Weeks 2 -3 Learning Session 1 face-to-face Week 4 Coaching Weeks 5 -7 Conference Call / Webinar Week 6 Learning Session 2 face-to-face Week 8 Coaching Weeks 9 -11 Conference Call / Webinar Week 10 Coaching Weeks 13 -15 Learning Session 3 face-to-face Week 12 Conference Call / Webinar Week 14 Learning Session 4 face-to-face Week 16 19

Beware: We will not go away when the 4 -month collaborative is over!!!

Assessing the Current State: Data Workbook

Data Workbook • Collaborative Effort from our partners • Purpose of Data Workbook – An assessment tool for VRHA, VITL, Blueprint and practices – Provides all information about data collection capacity and. . . – Understand what gaps there may be – Understand where we need to focus our efforts • Data Elements compiled from: – Vermont Blueprint for Health Data Dictionary for the Chronic Disease Registry (Covisint/Doc. Site) – NCQA Patient-Centered Medical Home Standards – Federal Register guidelines for Meaningful Use – CMS Physician Quality Reporting Initiative (PQRI) – Uniform Data System Clinical Measures (Added for Federally Qualified Health Centers mandated reports) • Data Elements are mapped to specific standards as applicable • Multiple Sections (7): Demographics & Scheduling, Core Data Elements, Vital Signs, Prenatal, Screening Tools, Misc. Data Elements, EHR Elements & Processes 22

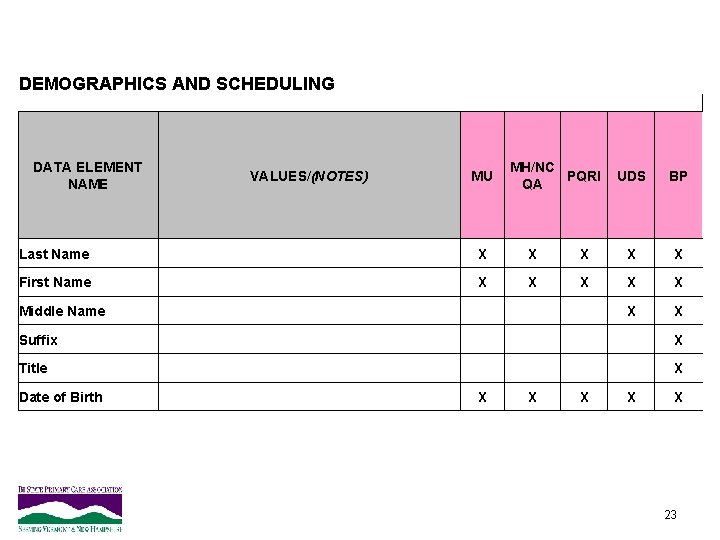
DEMOGRAPHICS AND SCHEDULING DATA ELEMENT NAME VALUES/(NOTES) MU MH/NC PQRI QA UDS BP Last Name X X X First Name X X X Middle Name X X Suffix X Title X Date of Birth X X X 23

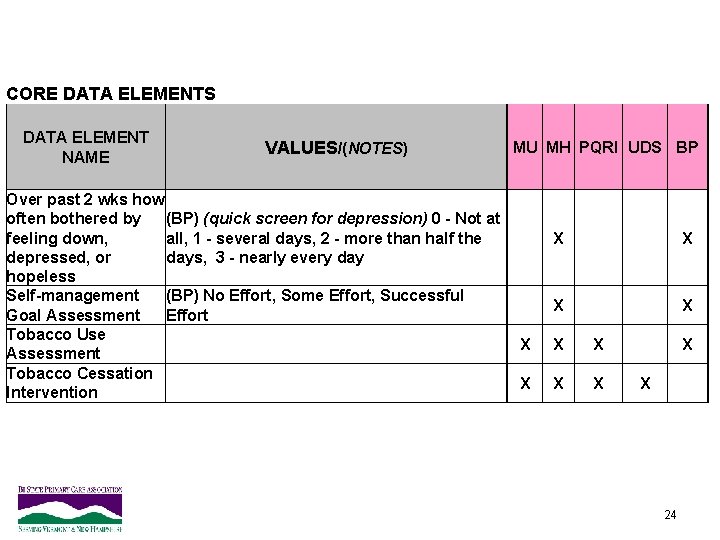
CORE DATA ELEMENTS DATA ELEMENT NAME VALUES/(NOTES) MU MH PQRI UDS BP Over past 2 wks how often bothered by (BP) (quick screen for depression) 0 - Not at feeling down, all, 1 - several days, 2 - more than half the depressed, or days, 3 - nearly every day hopeless Self-management (BP) No Effort, Some Effort, Successful Goal Assessment Effort Tobacco Use X Assessment Tobacco Cessation X Intervention X X X X X 24

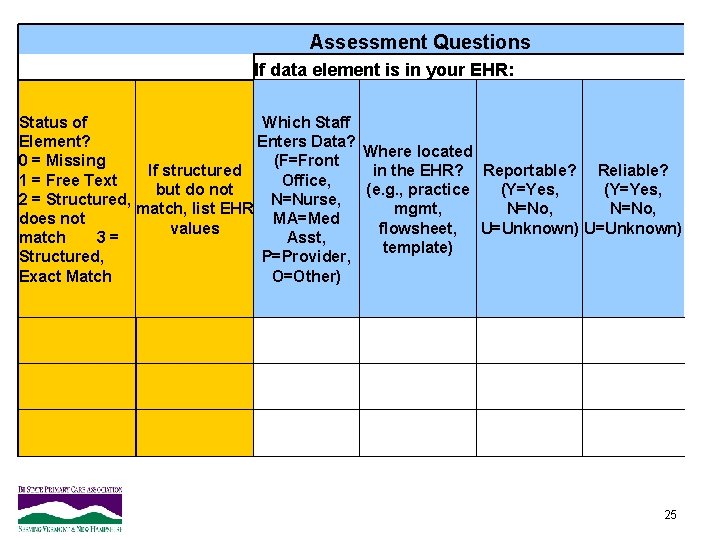
Assessment Questions If data element is in your EHR: Status of Which Staff Element? Enters Data? Where located 0 = Missing (F=Front in the EHR? Reportable? Reliable? If structured 1 = Free Text Office, but do not (e. g. , practice (Y=Yes, 2 = Structured, N=Nurse, mgmt, match, list EHR N=No, does not MA=Med values flowsheet, U=Unknown) match 3 = Asst, template) Structured, P=Provider, Exact Match O=Other) 25

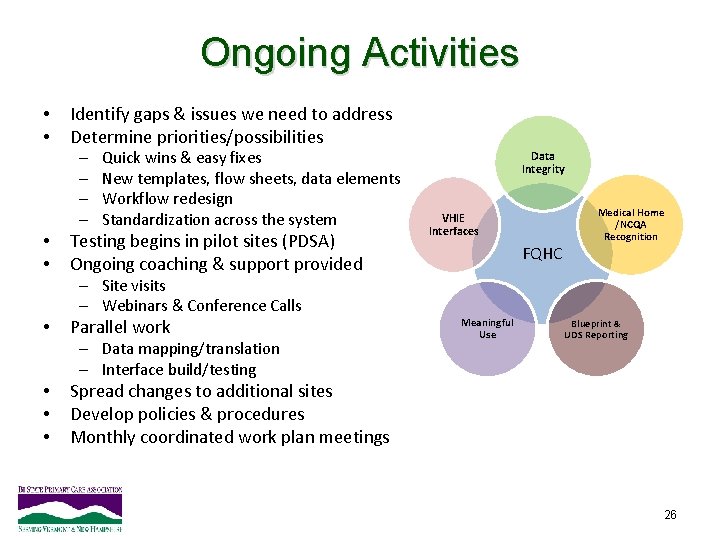
Ongoing Activities • • Identify gaps & issues we need to address Determine priorities/possibilities – – • • Quick wins & easy fixes New templates, flow sheets, data elements Workflow redesign Standardization across the system Testing begins in pilot sites (PDSA) Ongoing coaching & support provided Data Integrity VHIE Interfaces FQHC Medical Home /NCQA Recognition – Site visits – Webinars & Conference Calls • Parallel work – Data mapping/translation – Interface build/testing • • • Meaningful Use Blueprint & UDS Reporting Spread changes to additional sites Develop policies & procedures Monthly coordinated work plan meetings 26

Good News The first phase of grant incentive payments is underway. . . four FQHCs are ready to receive funds! 27

A Few Lessons Learned… • • • Strong clinical champions & leaders among staff Standardization is key to data integrity Engage EHR vendors early Many EHRs are not ready for UDS Reporting Multiple Activities Underway – Meaningful Use updates – Medical Home/NCQA Scoring Readiness • Cart before the horse… • Data translation; time consuming now and into the future • Practices benefit from ongoing training on their EHR’s & report writing capability • Monthly coordinated work plan calls with partners 28

Challenges and Successes Challenges • Complexity – Multiple EHRs – Many players • Technology Change – VITL HIE Infrastructure transition • Evolving reporting requirements and data standards Successes • FQHC team members engaged • Forward momentum maintained • Cooperation from partners and technology vendors 29

Bonnie Walker Tupelo Group, LLC (802)865 -2700 bonniewalker@tupelogroup. com Elise Ames H. I. S. Professionals, LLC (413)634 -5720 eames@hispros. com 30