VRE treatment options for severe infections Dr Nick











- Slides: 25

VRE - treatment options for severe infections Dr Nick Brown Addenbrooke’s Hospital, Cambridge 14 March 2013 Conflict of interest: None

Evidence biased medicine Class 0 Things I believe Class 0 a Things I believe despite the available data Class 1 Randomized controlled clinical trials that agree with what I believe Class 2 Other prospectively collected data Class 3 Expert opinion Class 4 Randomized controlled clinical trials that don’t agree with what I believe Class 5 What you believe that I don’t Bleck TP. BMJ 2000; 321: 239

VRE - treatment options for severe infections • • • Context Confounding factors Treatment options Studies of efficacy Combination therapy


Characteristics of infection with enterococci • • Rarely occur in the healthy host Majority of infections are nosocomial Bacteraemia is often polymicrobial In-hospital crude mortality is high Moellering R. J Antimicrob Chemother 1991; 28: 1 -12 Hoge CW et al. Rev Infect Dis 1991; 13: 600 -5.

‘Enterococcal bacteraemia – to treat or not to treat? ’ 81 enterococcal bacteraemias in US 50% considered clinically significant Treatment assessed for appropriateness Even non-significant bacteraemia mortality ~50% – Appropriateness of treatment made no difference Overall 51% mortality if significant – Treated appropriately = 38% – Treated inappropriately = 83% Hoge CW et al. Rev Infect Dis 1991; 13: 600 -5.

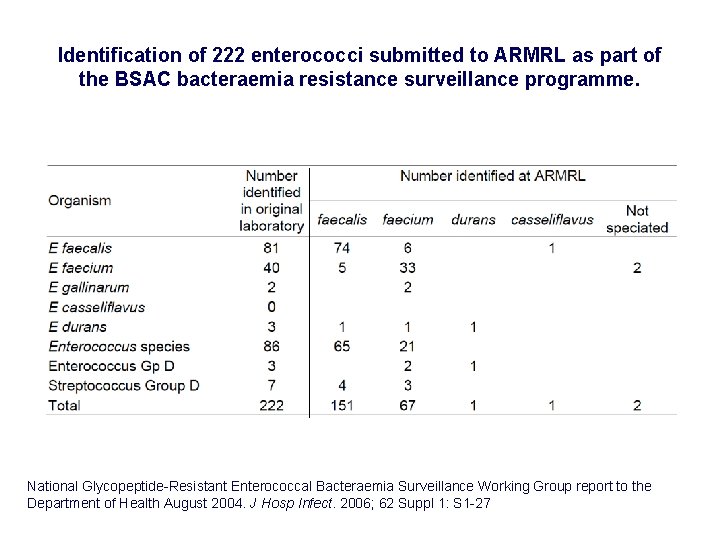
Identification of 222 enterococci submitted to ARMRL as part of the BSAC bacteraemia resistance surveillance programme. National Glycopeptide-Resistant Enterococcal Bacteraemia Surveillance Working Group report to the Department of Health August 2004. J Hosp Infect. 2006; 62 Suppl 1: S 1 -27

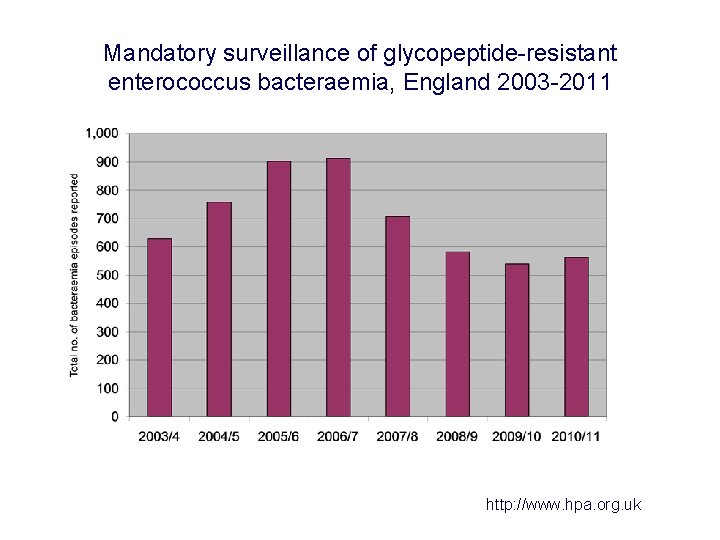
Mandatory surveillance of glycopeptide-resistant enterococcus bacteraemia, England 2003 -2011 http: //www. hpa. org. uk

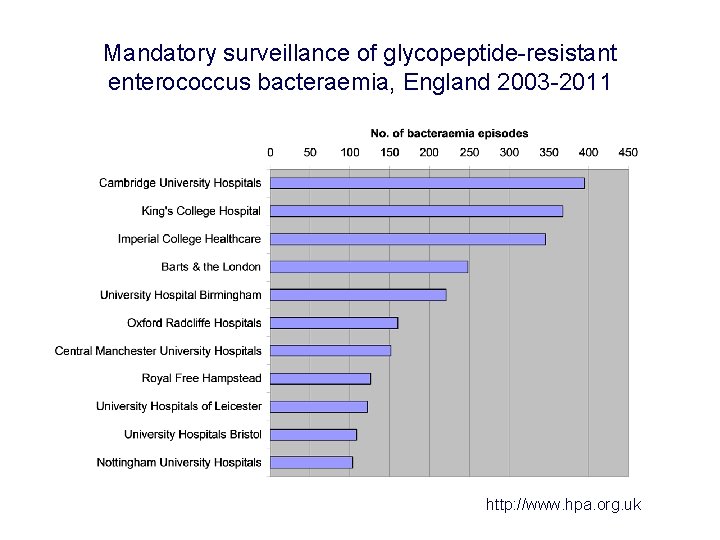
Mandatory surveillance of glycopeptide-resistant enterococcus bacteraemia, England 2003 -2011 http: //www. hpa. org. uk

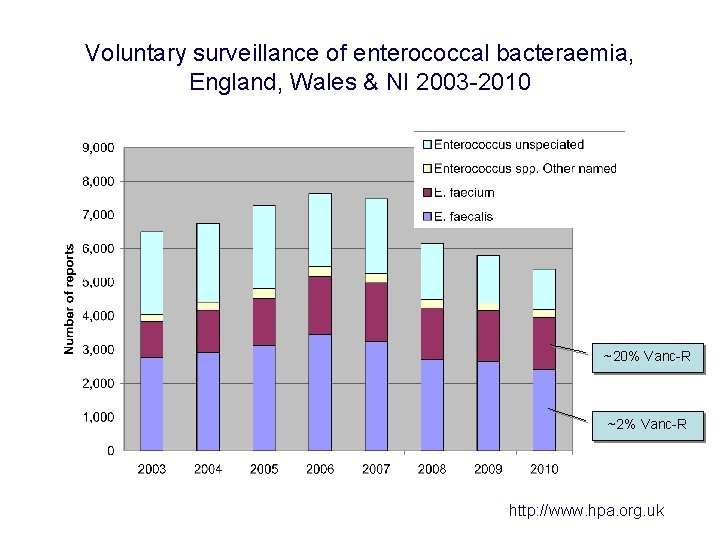
Voluntary surveillance of enterococcal bacteraemia, England, Wales & NI 2003 -2010 ~20% Vanc-R ~2% Vanc-R http: //www. hpa. org. uk

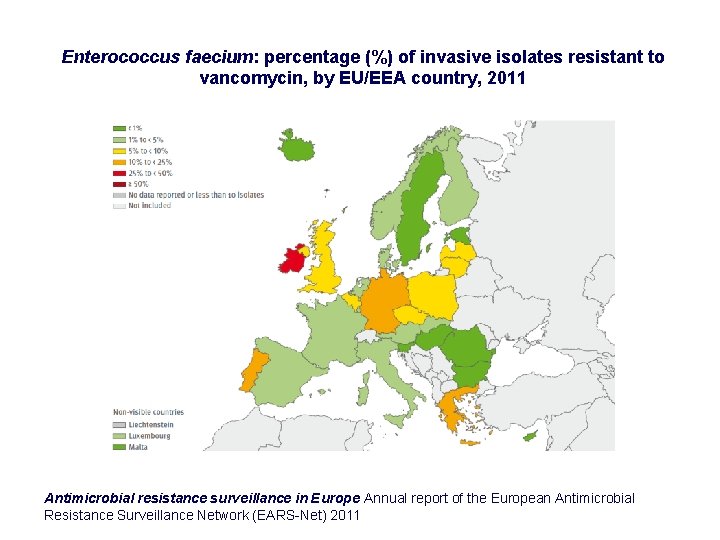
Enterococcus faecium: percentage (%) of invasive isolates resistant to vancomycin, by EU/EEA country, 2011 Antimicrobial resistance surveillance in Europe Annual report of the European Antimicrobial Resistance Surveillance Network (EARS-Net) 2011

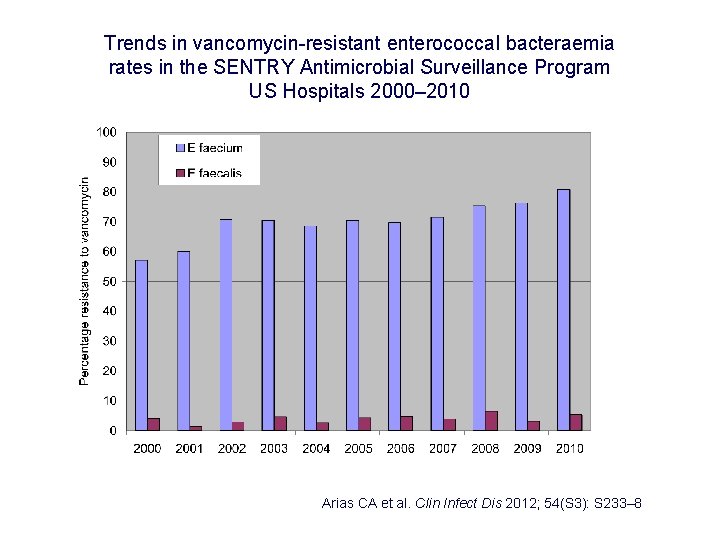
Trends in vancomycin-resistant enterococcal bacteraemia rates in the SENTRY Antimicrobial Surveillance Program US Hospitals 2000– 2010 Arias CA et al. Clin Infect Dis 2012; 54(S 3): S 233– 8


Treatment options for invasive infection due to VRE The main contenders • • • Penicillin/amoxicillin +/- aminoglycoside Linezolid Daptomycin (Quinupristin-dalfopristin) Tigecycline Have been used at some point (usually as part of combination) • Teicoplanin • Chloramphenicol • Tetracycline • Rifampicin • Fosfomycin • Quinolones Not quite here yet • • Oritavancin Dalbavancin (new oxazolidonones) (Cephalosporins with enhanced Gram positive activity) No specific recommendations in AHA, ESCMID or BSAC endocarditis guidelines

Combination therapy reported in the literature (note - data on efficacy are extremely limited and conflicting evidence of synergy or antagonism have been reported for some combinations) • • • ampicillin + quinupristin-dalfopristin ampicillin + quinolone quinupristin-dalfopristin + doxycycline + rifampicin quinupristin-dalfopristin + minocycline + chloramphenicol daptomycin + ampicillin +/- gentamicin daptomycin + gentamicin + rifampicin daptomycin + tigecycline ampicillin + ciprofloxacin + tetracycline ciprofloxacin + gentamicin + rifampicin ceftriaxone + vancomycin + gentamicin fosfomycin + ceftriaxone …and more…

Comparative data on treatment outcome • • • Retrospective review 113 VRE bacteraemia Nebraska, USA 1993 -2005 112 E. faecium, 1 E. faecalis All isolates ampicillin-resistant and HLGR Overall mortality 37. 2% Univariate analysis significant advantage to linezolid Advantage disappeared when underlying factors taken into account Crude mortality QPD (n=20) LZD (n=71) OTHER (n=22) 13 (65%) 18 (25%) 11 (50%) P= 0. 002 1 (1. 4%) 5 (23%) P=0. 10 Directly due to VRE 5 (25%) Erlandson KM et al. Clin Infect Dis 2008; 46: 30 -6.

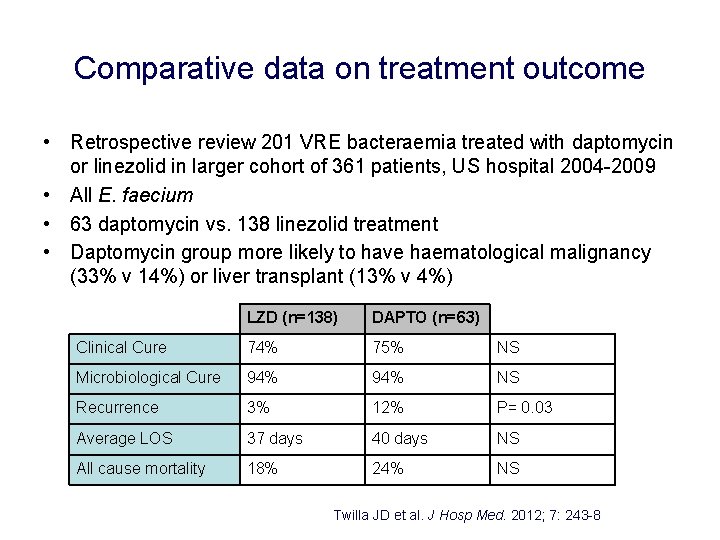
Comparative data on treatment outcome • Retrospective review 201 VRE bacteraemia treated with daptomycin or linezolid in larger cohort of 361 patients, US hospital 2004 -2009 • All E. faecium • 63 daptomycin vs. 138 linezolid treatment • Daptomycin group more likely to have haematological malignancy (33% v 14%) or liver transplant (13% v 4%) LZD (n=138) DAPTO (n=63) Clinical Cure 74% 75% NS Microbiological Cure 94% NS Recurrence 3% 12% P= 0. 03 Average LOS 37 days 40 days NS All cause mortality 18% 24% NS Twilla JD et al. J Hosp Med. 2012; 7: 243 -8

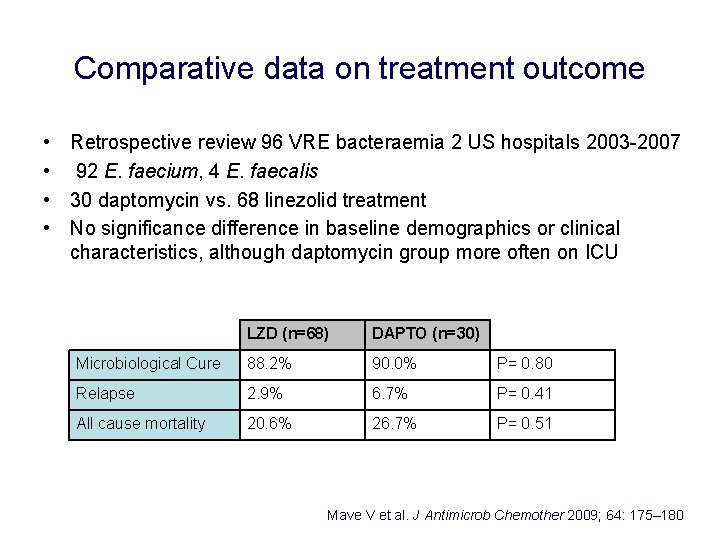
Comparative data on treatment outcome • Retrospective review 96 VRE bacteraemia 2 US hospitals 2003 -2007 • 92 E. faecium, 4 E. faecalis • 30 daptomycin vs. 68 linezolid treatment • No significance difference in baseline demographics or clinical characteristics, although daptomycin group more often on ICU LZD (n=68) DAPTO (n=30) Microbiological Cure 88. 2% 90. 0% P= 0. 80 Relapse 2. 9% 6. 7% P= 0. 41 All cause mortality 20. 6% 26. 7% P= 0. 51 Mave V et al. J Antimicrob Chemother 2009; 64: 175– 180

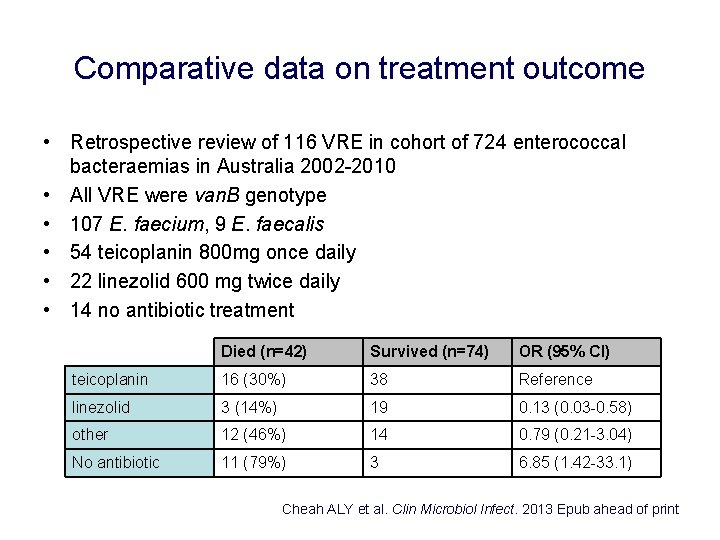
Comparative data on treatment outcome • Retrospective review of 116 VRE in cohort of 724 enterococcal bacteraemias in Australia 2002 -2010 • All VRE were van. B genotype • 107 E. faecium, 9 E. faecalis • 54 teicoplanin 800 mg once daily • 22 linezolid 600 mg twice daily • 14 no antibiotic treatment Died (n=42) Survived (n=74) OR (95% CI) teicoplanin 16 (30%) 38 Reference linezolid 3 (14%) 19 0. 13 (0. 03 -0. 58) other 12 (46%) 14 0. 79 (0. 21 -3. 04) No antibiotic 11 (79%) 3 6. 85 (1. 42 -33. 1) Cheah ALY et al. Clin Microbiol Infect. 2013 Epub ahead of print

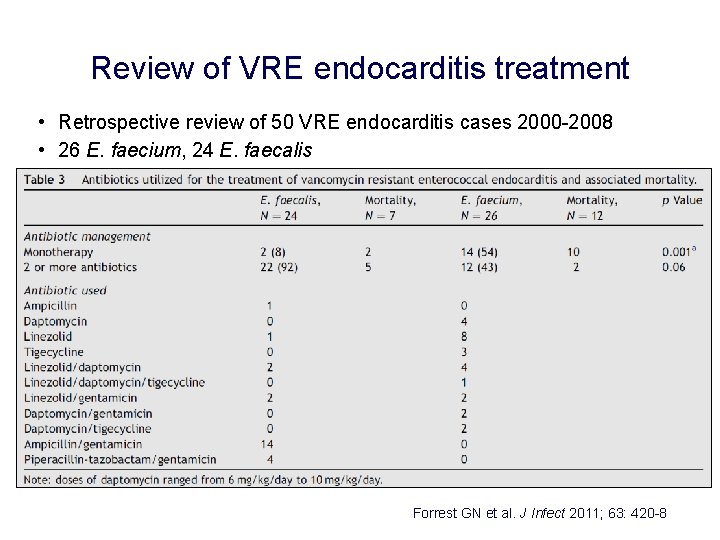
Review of VRE endocarditis treatment • Retrospective review of 50 VRE endocarditis cases 2000 -2008 • 26 E. faecium, 24 E. faecalis Forrest GN et al. J Infect 2011; 63: 420 -8

Dose of daptomycin • Evaluation of 31 patients receiving daptomycin for VRE bacteraemia • Many had factors contra-indicating use of linezolid • 2 cases of endocarditis Factors associated with good outcome: • Older age • Disease other than haematological malignancy • Dose of daptomycin >6 mg/kg/day Grim SA et al. J Antimicrob Chemother 2009; 63: 414 -6

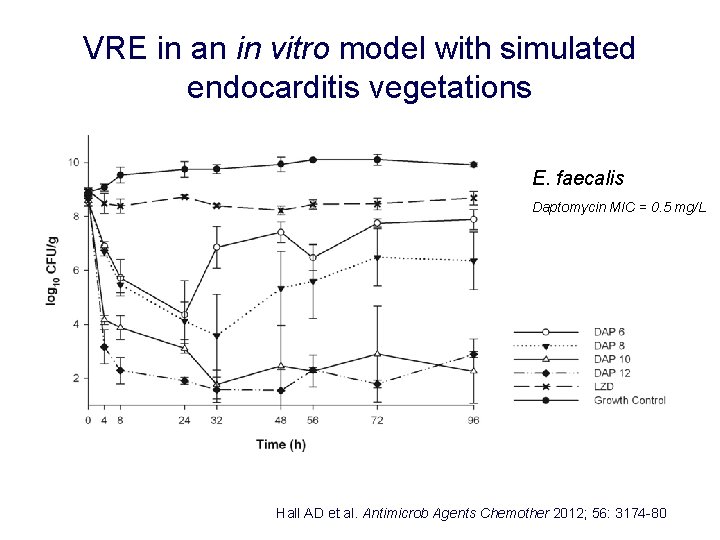
VRE in an in vitro model with simulated endocarditis vegetations E. faecalis Daptomycin MIC = 0. 5 mg/L Hall AD et al. Antimicrob Agents Chemother 2012; 56: 3174 -80

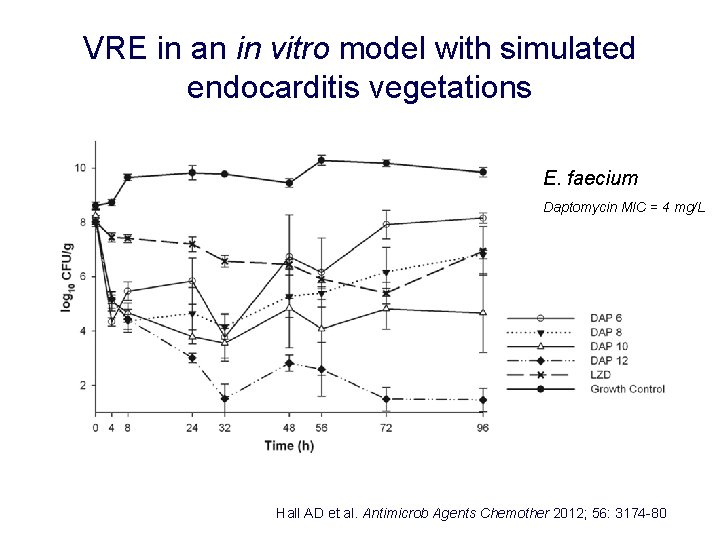
VRE in an in vitro model with simulated endocarditis vegetations E. faecium Daptomycin MIC = 4 mg/L Hall AD et al. Antimicrob Agents Chemother 2012; 56: 3174 -80

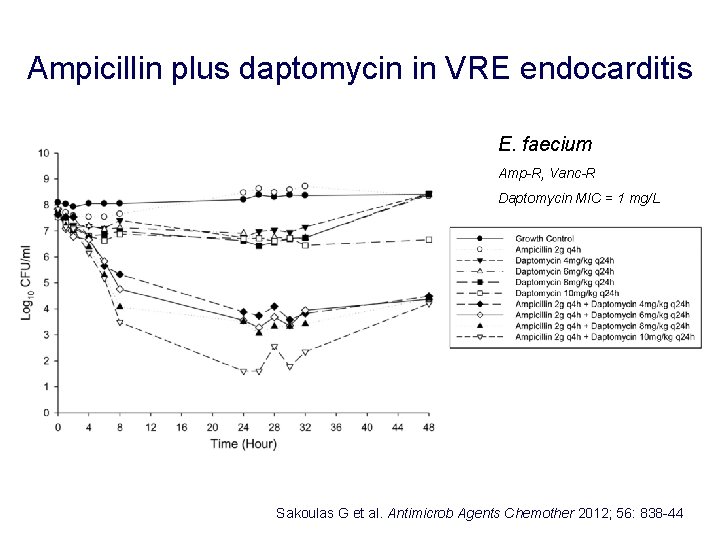
Ampicillin plus daptomycin in VRE endocarditis E. faecium Amp-R, Vanc-R Daptomycin MIC = 1 mg/L Sakoulas G et al. Antimicrob Agents Chemother 2012; 56: 838 -44

Summary • No good evidence to show which treatment option should be used for bacteraemia due to VRE • Beta-lactam plus aminoglycoside combinations are still considered optimal where susceptibility allows • Some evidence of efficacy of both linezolid and daptomycin as single agents • Higher doses of daptomycin may have better efficacy • Combination therapy may be better for severe infection, such as endocarditis, but further data needed