VITILIGO EPIDEMIOLOGY DIFFERENTIAL DIAGNOSIS AND ETIOLOGY By Sandeep

VITILIGO: EPIDEMIOLOGY, DIFFERENTIAL DIAGNOSIS AND ETIOLOGY By: Sandeep Dhand

Vitiligo is a depigmenting disorder characterized by the development of white patches in various distributions, which are due to the loss of melanocytes from the epidermis. � Alikhan provided statistical data on the treatments and symptoms of vitiligo patients. In his studies he states cases have been reported as early as 6 weeks after birth. � This article mentions one study found progression in 88. 8% of patients, more so with positive family histories, NSV, a longer duration, Koebner phenomenon, and mucous membrane involvement. �
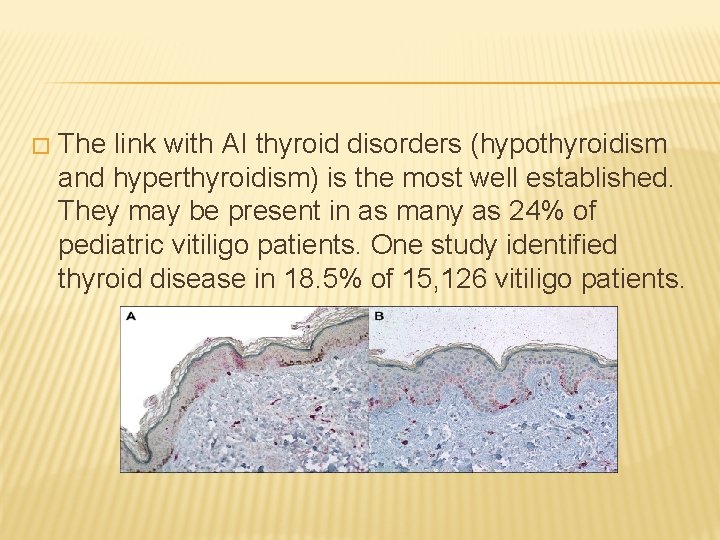
� The link with AI thyroid disorders (hypothyroidism and hyperthyroidism) is the most well established. They may be present in as many as 24% of pediatric vitiligo patients. One study identified thyroid disease in 18. 5% of 15, 126 vitiligo patients.

� The current thought is that vitiligo represents a group of heterogeneous pathophysiologic disorders with a similar phenotype � Among vitiligo patients, 20% report thyroid disease (an 8 -fold increase over the general population), particularly hypothyroidism.

� The Oxidative stress hypothesis states it is unclear why both lesional and nonlesional skin from vitiligo patients has abnormally low levels of catalase enzyme, which correlates with high H 2 O 2 levels throughout the epidermis.
-Kingo aimed to analyze changes in expression of genes involved in skin pigmentation. � With quantitative RT-PCR they measured the m. RNA expression levels of eight genes from the melanocortin system and two enzymes involved in melanogenesis.

� Expression of melanocortin receptors was increased in unaffected skin of vitiligo patients compared to healthy subjects. � The differences were statistically significant in the cases of MC 1 R (melanocortin receptor 1) and MC 4 R (melanocortin receptor 4).

� The purpose of Park’s study was to use UVB radiation exclusively on vitiligo patches of individuals affected by SV. � BIOSKIN can produce a focused beam of UV -B (microphoto-therapy) on vitiligo patches only.

� In Park’s studies it is suggested that the sera of vitiligo patients have autoantibodies mostly directed to the 65 -k. Da melanocyte surface antigen and that this antigen may play a role in the development or improvement of vitiligo. � It has been shown that concentrations of a. MSH are reduced in the epidermis of vitiligo patients which could contribute to the pathogenesis of vitiligo.
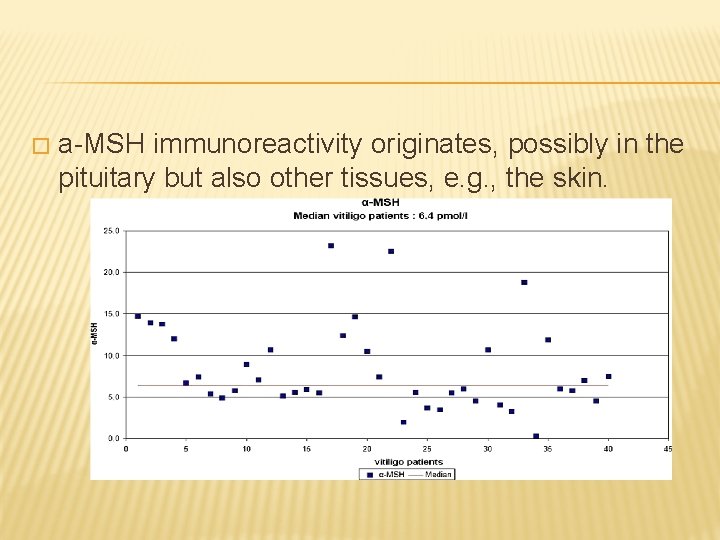
� a-MSH immunoreactivity originates, possibly in the pituitary but also other tissues, e. g. , the skin.

� Lower plasma a-MSH levels might represent an immuno-endocrine condition with higher susceptibility for the development of autoimmune depigmentation. � In conclusion, it is suggested that the sera of vitiligo patients have autoantibodies mostly directed to the 65 -k. Da melanocyte surface antigen and that this antigen may play a role in the development or improvement of vitiligo.

CITATIONS � � � Alikhan, A. (2011). Vitiligo: A comprehensive overview: Part I. Introduction, epidemiology, quality of life, diagnosis, differential diagnosis, associations, histopathology, etiology, and work-up. Journal of the American Academy of Dermatology, 65(3), 473 - 491. Kingo, K. (2007). Gene expression analysis of melanocortin system in vitiligo. Journal of dermatological science, 48(2), 113122. Lotti, T M. (1999). UV-B radiation microphototherapy. An elective treatment for segmental vitiligo. Journal of the European Academy of Dermatology and Venereology, 13(2), 102 -108. Pichler, R. (2006). Vitiligo patients present lower plasma levels of α- melanotropin immunoreactivities. Neuropeptides, 40(3), 177184. Park, Y. (1996). Identification of autoantibody to melanocytes and characterization of vitiligo antigen in vitiligo patients. Journal of dermatological science, 11(2), 111 -121.

�QUESTIONS? ? ?
- Slides: 13