Visual Outcomes After Temporary Keratoprosthesis Kristin C Bains
Visual Outcomes After Temporary Keratoprosthesis Kristin C. Bains, MD Robert Phillips, MD The authors have no financial interest in the subject matter of this poster

Purpose • To evaluate visual outcomes after combined penetrating keratoplasty (PK) and vitreoretinal surgery using temporary keratoprosthesis (TKP)

Introduction • Utilized in patients with coexisting corneal and vitreoretinal pathology • Combined procedure necessary for adequate visualization intraoperatively • If combined only with PK, delay waiting for graft to clear, leading to worsening retinal pathology • Does not expose patient to risks associated with open-sky vitrectomy • Attempts to restore visual function by allowing earlier surgical intervention

Methods • IRB approval obtained • Retrospective, observational case series – CPT code 65770 – Date range: 2003 -2010 – 55 eyes of 47 patients identified • 1 corneal surgeon, multiple vitreoretinal surgeons • Included: 47 eyes of 41 patients who underwent combined TKP/PK and vitreoretinal surgery • Excluded: 8 eyes of 6 patients lost to follow-up • Previous surgeries common
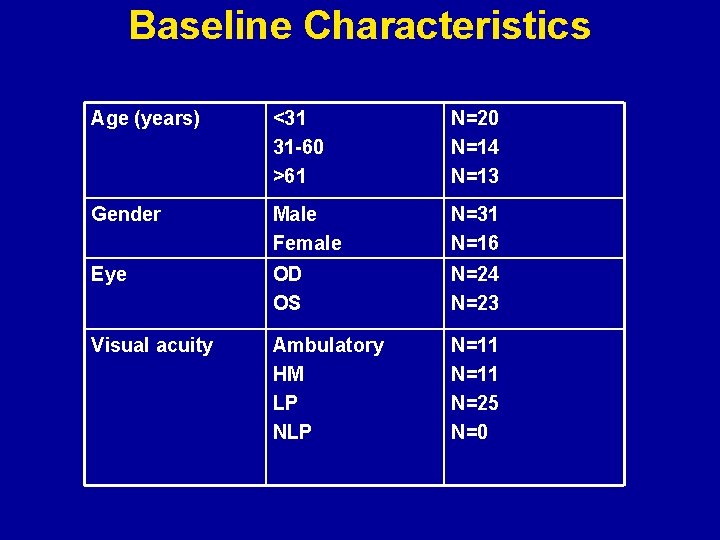
Baseline Characteristics Age (years) <31 31 -60 >61 N=20 N=14 N=13 Gender Male Female N=31 N=16 Eye OD OS N=24 N=23 Visual acuity Ambulatory HM LP N=11 N=25 N=0

Baseline Characteristics (cont. ) Cornea status Scar Rejected graft BK N=23 N=19 N=5 Retina status RD Attached Macular pucker Choroidal hemorrhage Vitritis Macular hole N=29 N=12 N=3 N=1 N=1 Comorbid ocular disease Secondary glaucoma Amblyopia Bells’ palsy Traumatic optic neuropathy Traumatic maculopathy N=11 N=3 N=1 N=2 N=1
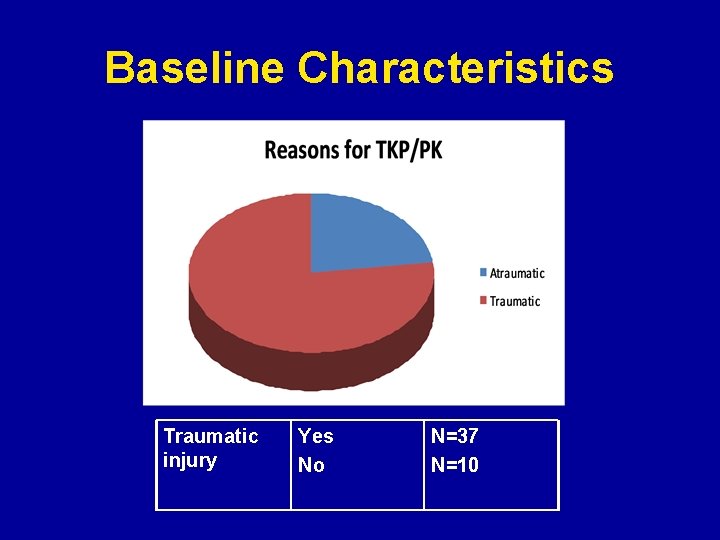
Baseline Characteristics Traumatic injury Yes No N=37 N=10
Methods • Wide-field Landers TKP • Vitreoretinal procedures – 3 port ppv – Pars plana lensectomy if indicated – Retinal reattachment • Penetrating keratoplasty

Results • Follow-up: 1 month- 67 months • Mean pt follow-up: 23. 4 months • Post-operative graft status at final follow-up • 17 clear (36. 9%) • 29 rejected • 7 repeat TKP/PK • 5 repeat PK
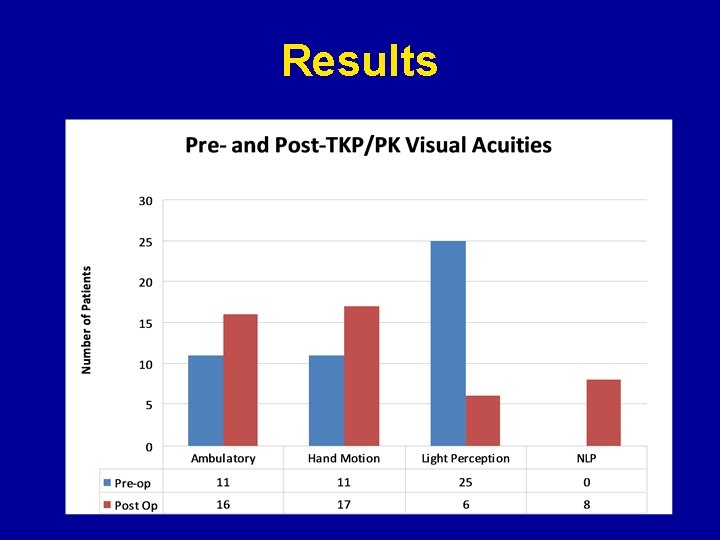
Results

Conclusions • Before combined surgery 21 eyes had BCVA of ambulatory to HM. • Post-operatively, majority of patients (32 eyes) had BCVA of ambulatory to HM. • 93. 6% of eyes (44 eyes) were retained • 2. 1% of eyes (1 eye) became phthisical

Conclusion • Tool used in management of complex disease, without which, many eyes could not be salvaged • Combined surgery is not without complications • Outcomes can be good considering complexity of pathology
- Slides: 12