Viewing Learning Disabilities Psychotherapy Through The Lense of

Viewing Learning Disabilities Psychotherapy Through The Lense of Attachment Theoretical Perspectives and Practical Strategies Dr Kathy Mc. Kay Dr Kelly Camilleri


We don’t want to do this

We do want to do this -Share some experiences of applying attachment theory and PACE in individual therapy and systems -Ecological interventions and attachment -Look at team and organisational applications of PACE

Valorie Sinason: Secondary Handicap and its Relationship to Trauma (1986) Pivotal work • A non static and reciprocal view of ID • Highlighted vulnerability to Abuse and Trauma • Opened the door to Therapy

Pat Frankish Model • Fra • A safe Place to Live • Access to Psychological Therapy • Support for Staff • Specialist Training for Staff

Attachment • Lasting psychological connectedness between human beings

Why?

Individuation and Sense of Self

Launching Into Adulthood

Neurobiology of Attachment We are born with most of the neurons (brain cells) we will ever own but; At birth the brain is 25% of its adult weight - by the age of 2 this has increased to 75% and by age 3 it is 90% of adult weight. § § This growth is largely the result of the formation and ‘hard wiring’ of synaptic connections § Babies brains are both ‘experience expectant’ and ‘experience dependent’

Adaptation • “Neurons that fire together, wire together” Courchesne et al. , 1994 • Production and pruning enables children to fit into circumstances that surround them • Influenced by stress response -development organized around hyper arousal / dissociation
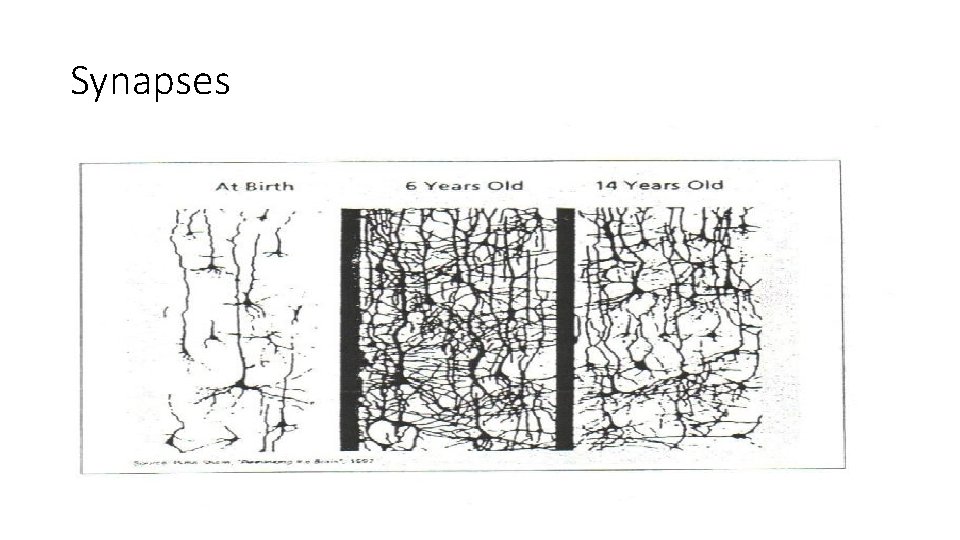
Synapses
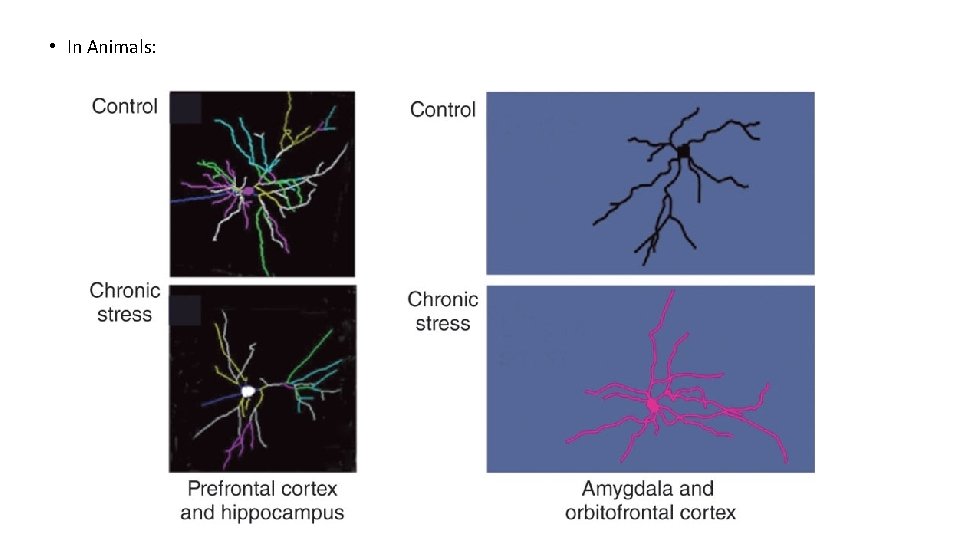
• In Animals:
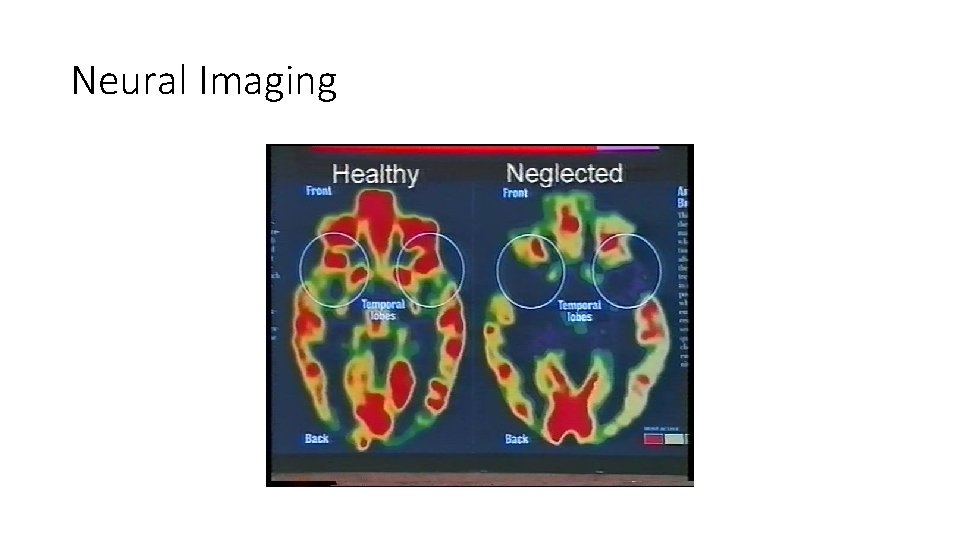
Neural Imaging

Impact of poor attachment These functions may be delayed, diminished or lost: ▪ ▪ ▪ ▪ Ability to learn language and to speak Understanding feelings or having words to describe them Connection between how we feel and our sensory experience Empathy Control of impulse Regulation of mood Short term memory Enjoyment NB. Consider the nature of the referral to ‘challenging behaviour’ services in LD. Often about ‘dysregulation’ (aggression, food, sleep etc. ), and issues regarding relationships with the family, staff or peers(‘clingy’, or rejecting).

Prevalence and Nature of Attachment Difficulties • Rates of LD children are not dissimilar to non LD (e. g. . 60% of non LD securely attached, cf. 50% of children with Downs Syndrome, 53% autism). • BUT - of the non-secure LD more likely to have disorganised or ‘non typical’ attachments (rates similar levels to those who are institutionalised or traumatised) - Scheungel at al (2013).

Issues Related to the Child’s Difficulties: • Impaired theory of mind - makes ‘goal directed partnership’ harder • Cues more difficult to interpret - e. g. . Infants with Downs Syndrome - ‘blunted’ - (De Schipper and Scheungel 2010) • Delayed responses in reciprocal interaction • Hospital care and early feeding difficulties as a neonate more likely (impacting on early bonding) • Delays in mobility – impact on ability to gain proximity to the parent (as an attachment behaviour) • Sensory processing difficulties (common in autism) can mean that they find touch, or certain textures/sounds, smells etc. aversive – This can include sensory stimulation provided by the care giver – can therefore find aspects of the care giving anxiety evoking and aversive • Sense of ‘shame’ – the taboo of cognitive impairments – inadequacy. Autism – (NB. Some similar features of attachment/developmental trauma and autism – Coventry Grid can help to consider this).

Experiences of Parents: • Potential grief for loss of the ‘healthy child’ – can disrupt the attachment and care-giving systems as their efforts to care for and protect their child does not lead to an improvement in the condition. • Sense of guilt for the loss of the healthy child – e. g. . if genetic, birth trauma etc. • If the parent struggles to develop an internal representation of the child’s actual abilities, rather than wished for abilities, this can impact of parenting sensitivity. (NB. Most parents DO adapt, and resolve their grief. However, social support and stress within the family needs to be considered for those who present as unresolved. )

Social Factors: • More likely to have had earlier separation – e. g. . nursery can start at an earlier age • More likely to have had multiple care givers – e. g. . respite care • More likely to have a degree of ‘institutional’ care, with multiple care givers (e. g. . residential school). • In care settings – can have a high staff turnover. • Greater risk of people with LD suffering multiple forms of abuse, increasing the risks of developmental trauma.

Dyadic Developmental Psychotherapy • Therapist and carer work together with the child. • Playful, Accepting, Curious, Empathic. • Creates an environment that facilitates healthy relationship development. • Offers increased sensitivity, availability and responsiveness. • Co-regulates emotion and co-constructs meaning. • Builds trust. • Facilitates intersubjective experience and secure attachment. • Contains anxiety and supports exploration.

Attachment based care Focus on experience related to the persons history, dates, situations Can use (and support) direct care givers to develop sensitive secure attachments Get to know the inside them, think about what is needed Gives permission to nurture Planning for transitions and changes Accepts need for control - including things like visual planners to help security though support to ‘hold in mind’. • Provide experiences to combat sense of being worthless and bad. • Shame/rage • Platform to understand behavioural distress • • •

Reciprocal Conversations • Truly listening, so the person feels understood, can reduce escalation, even when there are different views • Reflective conversation includes both affect and reflective components (talking and genuine listening) • Carers must feel safe to participate in reciprocal conversation i. e. when authority is questioned, in conversation, not getting angry and insisting on compliance • Empathise with distress, including that caused by imposed or natural consequences (e. g. . ‘I’d feel upset too, if I was told I couldn’t go swimming’) • Ensure that conflict does not impact on the worth of the person or the relationship (avoid shaming) (Hughes, 2009)

Shame • Shaming experiences (e. g. . Removal of possessions/ privileges / attachment figure through ‘time out, being told he has done something wrong’) reinforce his sense of himself as inherently ‘bad’. • Confirms his sense of the world around him as hostile, unsafe and uncaring.

PACE Playfulness, Acceptance, Curiosity, Empathy • Creates a safe sanctuary to be together • Helps the person feel more connected to the carer • Avoids power struggles • Supports development of empathy • Supports emotional regulation • Describing and recognising what is happening for them, emotionally, in a regulated way.

Playfulness • Most parents intuitively maintain infants attention through playfulness • Laughter great antidote to shame and fear • Humor helps develop another perspective on events • Playfulness has no agenda • Admit mistakes, not take ourselves to seriously • Keep an open mind NB. Playfulness is different to sarcasm which can be shameful, and it is NOT making light of painful feelings, or acting silly due to our own anxiety.

Examples of Playfulness for Tom (pseudonym) o Allow his ‘play’ o Enjoy him! o Join him in his fantasy world – parallel play until he invites you in o Use his language – e. g. . “Looks like that man who told you off thinks he is the Commander in Chief today!!”

Acceptance • Unconditional acceptance - value him – see him as important • Only behaviour is subject to evaluation and guidance, judgment and criticism (I like you – I don’t like the behaviour) • Feelings are not judged, only destructive behaviours associated with the feelings • Acceptance does not mean permissiveness • May disagree with a choice but accept the intention behind the choice (e. g. , understand that they were angry, or trying to be accepted by friends, etc. when they did something stupid – doesn’t make the behaviour acceptable) • Understand meaning of behaviour before reacting

Examples of Acceptance For Tom • “Wow, you must be really angry if you want to hit him” • “You hate him ‘cos he won’t let you have the dog lead…and you really wanted it …. ” • “I get that you are really upset that the man told you not to do …. x… let’s work out a way to deal with that and sort it out”. • “It made you so cross you never want to go there again…. But Tom I think you deserve to go there as you had such as good time…” • ‘No wonder you wanted to hurt him if you thought that he did it on purpose…’

Obstacles to Acceptance Your own anger/embarrassment - giving energy at time of behaviour is more likely to entrench the behaviour “Do they accept and care for me as I am? ”

Examples of Curiosity For Tom • “I’m wondering what that is about… could it be that you were upset by what the man said in the shop” • “I’m noticing that you seem to be getting cross when I told your mum about …x. . Did it feel like I was telling you off? ” (This can lead onto acceptance – e. g. . ‘no wonder you felt cross at me, if you thought I was telling you off’).

Empathy • ‘Feeling with’ the person • Feeling compassion for their struggles • Empathy provides parental/adult ‘safe’ presence, which assists the person to regulate • Eventually allows the person to acknowledge deeper feelings of fear/ sadness/hurt/anger, without fearing judgement. • Empathy does not mean rescuing or fixing (Hughes, 2009)

Examples of Empathy For TOM • “I’m really sorry that happened Tom” • “I’m sorry if it felt like I was telling you off…. That must have felt horrible” • “That must have been really hard” • The carer, on returning home, to talk to mum in front of Tom, about an event in a way that shows that they understood his feelings/experience (e. g. . ‘X happened. . and Tom ran out because he was so frightened when the man shouted, because Tom thought the man might hurt him… and Tom does not know me well enough yet, to know that I won’t let anyone hurt him”.

References • Attachment in Intellectual and Developmental Disability: A Clinician's Guide to Practice and Research (2016). Wiley Series • Bombèr, L. H. (2007) Inside I’m Hurting: Practical Strategies for Supporting Children with Attachment Difficulties in Schools. London: Worth Publishing. • Cozolino, L. (2013) The Social Neuroscience of Education: • Dan Hughes, Jonathan Baylin, Daniel Siegal (2012). Brain based parenting: The neuroscience of caregiving for healthy attachment. Norton • Kim Golding, Dan Hughes (2012). Creating Loving Attachments. Kingsley
- Slides: 35