VIET NAM CUBADNG HOI HOSPITAL QUANG BINH BNH

VIET NAM CUBA-DồNG HOI’ HOSPITAL QUANG BINH. BỆNH VIỆN HỮU NGHỊ VIỆT NAM – CUBA ÐồNG HỚI Secondary myocardial toxicity after cancer therapy. Multidisciplinary cancer management Ph. D. Dr. Jesús de los Santos Renó Céspedes Assistant Professor of Oncology and Pediatric Oncology National Oncology and Radiobiology Institute. Havana. Cuba Congress of the Vietnam Internal Medicine Association 2020 1
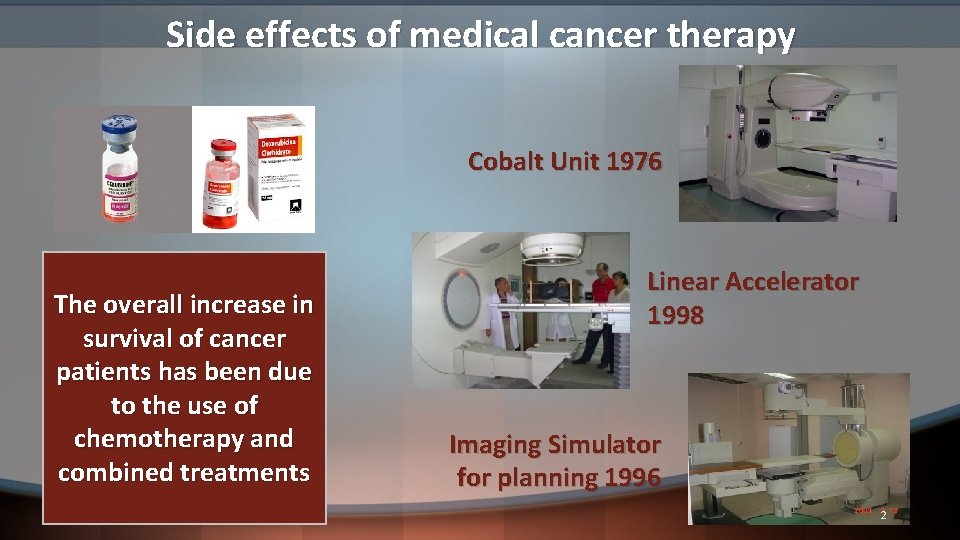
Side effects of medical cancer therapy Cobalt Unit 1976 The overall increase in survival of cancer patients has been due to the use of chemotherapy and combined treatments Linear Accelerator 1998 Imaging Simulator for planning 1996 2

Side effects of medical cancer therapy RADIATION-INDUCE HEART DISEASE These developments are nonetheless associated with emerging concerns over drug-induced cardiotoxicity. Brachytherapy HDR Cobalt 60 source 2013 Linear accelerator for Trans-Surgery Radiotherapy NOVAC-11 IORT 2014 3
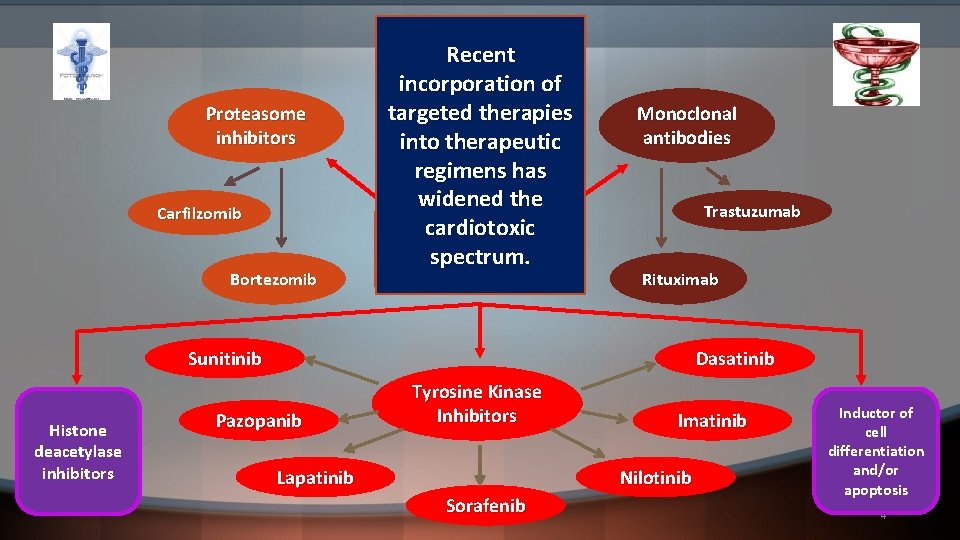
Proteasome inhibitors Carfilzomib Bortezomib Recent incorporation of targeted therapies into therapeutic regimens Hygea has widened the cardiotoxic Miscellaneous spectrum. Products Monoclonal antibodies Trastuzumab Rituximab Sunitinib Histone deacetylase inhibitors Dasatinib Pazopanib Tyrosine Kinase Inhibitors Lapatinib Imatinib Nilotinib Sorafenib Inductor of cell differentiation and/or apoptosis 4

Side effects of medical cancer therapy Knowledge of these side effects and the main risk factors associated with cardiotoxicity in cancer patients is essential for adequate monitoring and early treatment of such events in these patients. 5

Side effects of medical cancer therapy This concern is reflected in drug development with an emphasis on improved characterization of potential cardiotoxicity of new compounds during the early phases of development and designing safer drugs. 6
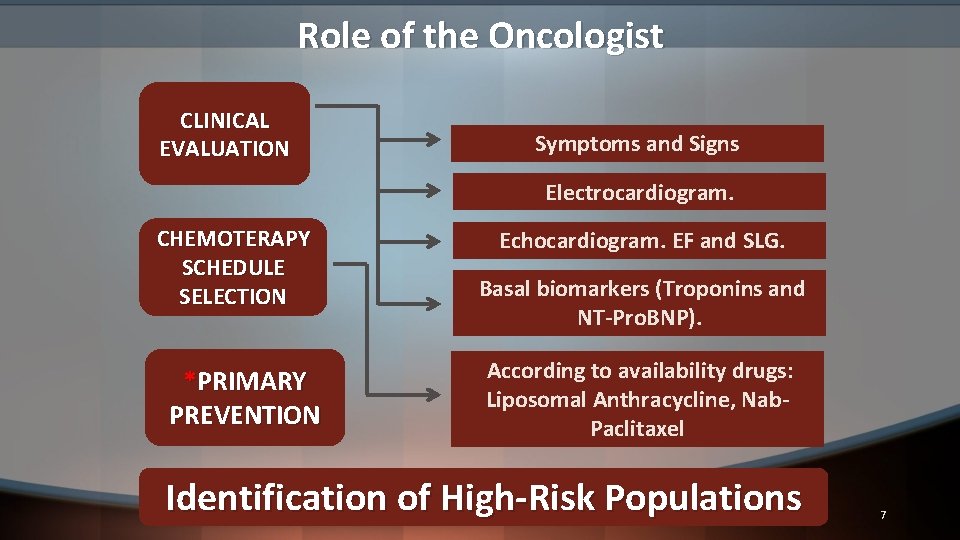
Role of the Oncologist CLINICAL EVALUATION Symptoms and Signs Electrocardiogram. CHEMOTERAPY SCHEDULE SELECTION *PRIMARY PREVENTION Echocardiogram. EF and SLG. Basal biomarkers (Troponins and NT-Pro. BNP). According to availability drugs: Liposomal Anthracycline, Nab. Paclitaxel Identification of High-Risk Populations 7

* Prevention: • Development of less cardiotoxic drugs • Identification of high risk population • Reversible cardiovascular risk factors treatment • Early cardiologist involvement • Primary prevention: Ø Dexrazoxane and ACE Inhibitors, beta-blockers. Monitoring: • LVEF evaluation if risk of left ventricular dysfunction • QTc monitoring for drugs at risk to induce QTc prolongation Early treatment: • Discontinuation if cardiotoxicity • Concomitant causes treatment • Early treatment: LVEF dysfunction. Hypertension. Coronary artery disease 8

Diagnosis of Cardiotoxicity: FIRST LEVEL CLINICAL DIAGNOSIS Survivorship: Managing Cardiac Toxicities Anecita Fadol, Ph. D, RN, FNP-BC, FAANP The University of Texas MD Anderson Cancer Center 9

CLINICAL DIAGNOSIS Others: • Electrolyte disorders: Hypomagnesemia Hypercalcemia History and physical examination: • Assess for symptoms or sings to heart failure • Asses patient’s ability to perform routine and desired activities of daily living • Look for signs volume overload Evaluated for presence of heart failure risk factors: • • • Arterial Hypertension Diabetes Mellitus Dyslipidemia Age > 65 years History of Cardiovascular comorbidities Review oncology history: Previous chemotherapy with emphasis on anthracyclic (total cumulative doses) and its received dose-limiting anthracyclic administration method. Other system therapy and/or chest Review other cardiovascular risk factors: radiation therapy • • Smoking Alcohol Obesity Family of cardiovascular cardiomyopathy or other heart disease 10
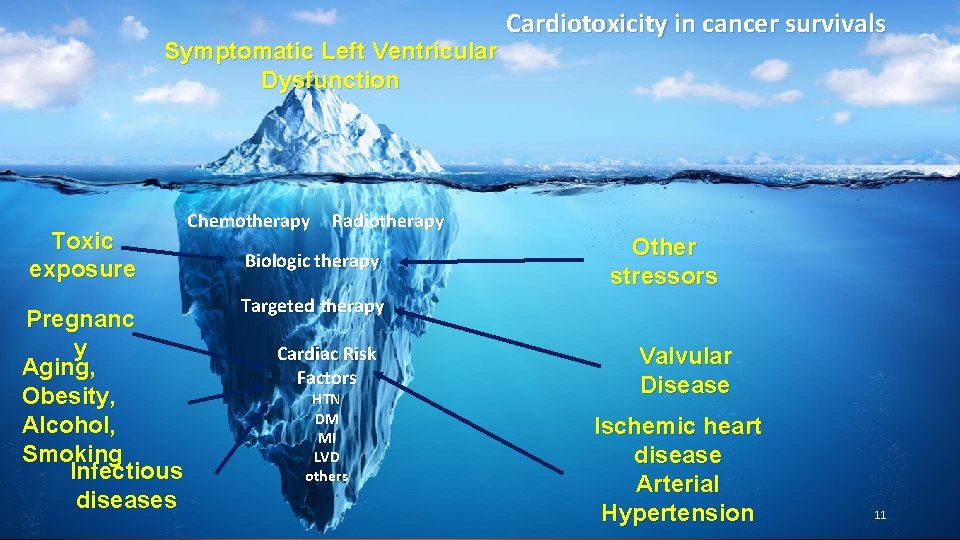
Symptomatic Left Ventricular Dysfunction Toxic exposure Pregnanc y Aging, Obesity, Alcohol, Smoking Infectious diseases Chemotherapy Cardiotoxicity in cancer survivals Radiotherapy Biologic therapy Other stressors Targeted therapy Cardiac Risk Factors HTN DM MI LVD others Valvular Disease Ischemic heart disease Arterial Hypertension 11

Diagnosis of Cardiotoxicity: SECOND LEVEL ELECTRICAL DIAGNOSIS The initial and periodic electrocardiograms are useful for cancer treatments that are associated with increases risk of: • Arrhythmia and QT prolongation, • Brugada’s Syndrome, • Short QT syndrome, • Cathecholaminergic polymorphic syndrome and others. 12
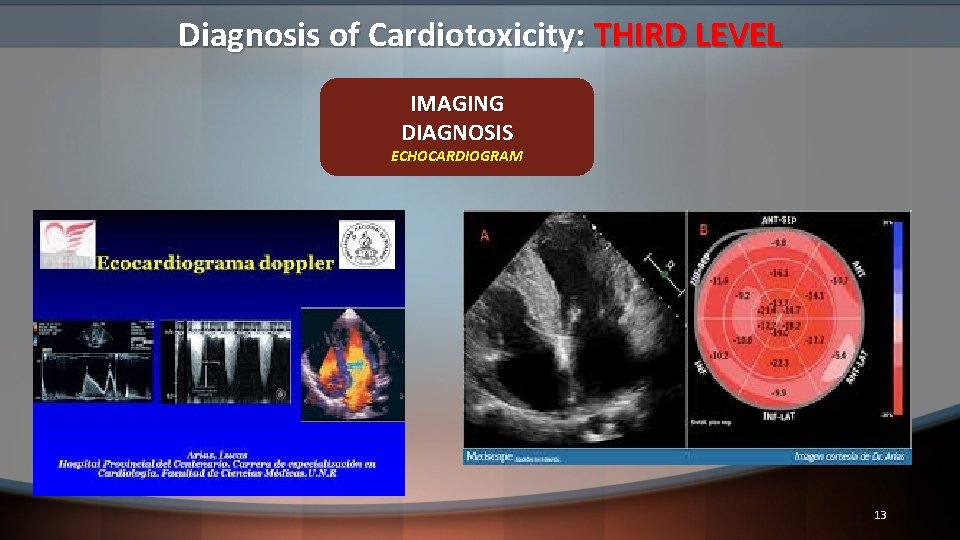
Diagnosis of Cardiotoxicity: THIRD LEVEL IMAGING DIAGNOSIS ECHOCARDIOGRAM 13
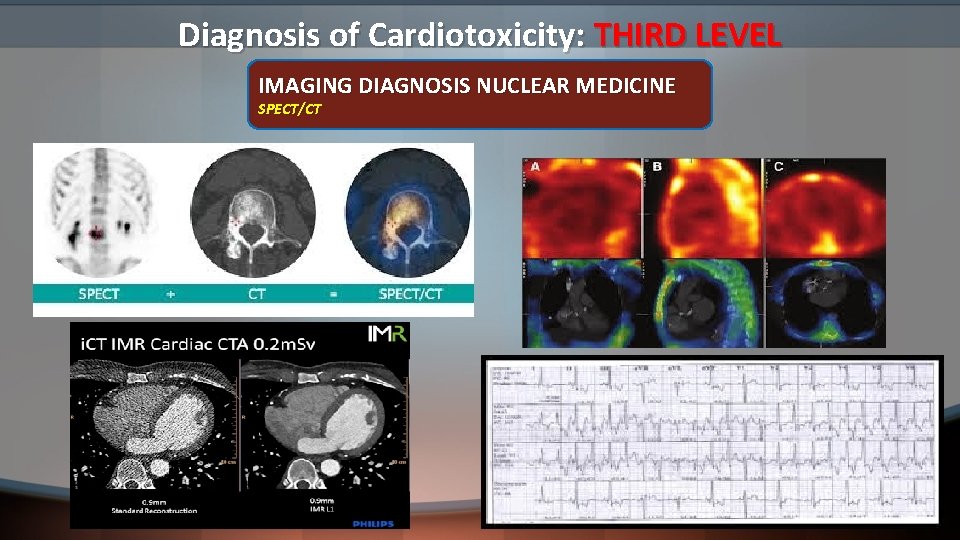
Diagnosis of Cardiotoxicity: THIRD LEVEL IMAGING DIAGNOSIS NUCLEAR MEDICINE SPECT/CT 14
Diagnosis of Cardiotoxicity: THIRD LEVEL IMAGING DIAGNOSIS NUCLEAR MEDICINE PET/CT STEM CELLS Prósper Cardoso F. et al. Stem cells to Regenerate Cardiac Tissue in Heart Failure. Rev Esp Cardiol 2003; 56(10): 935 -9 www. revespcardiol. org 15
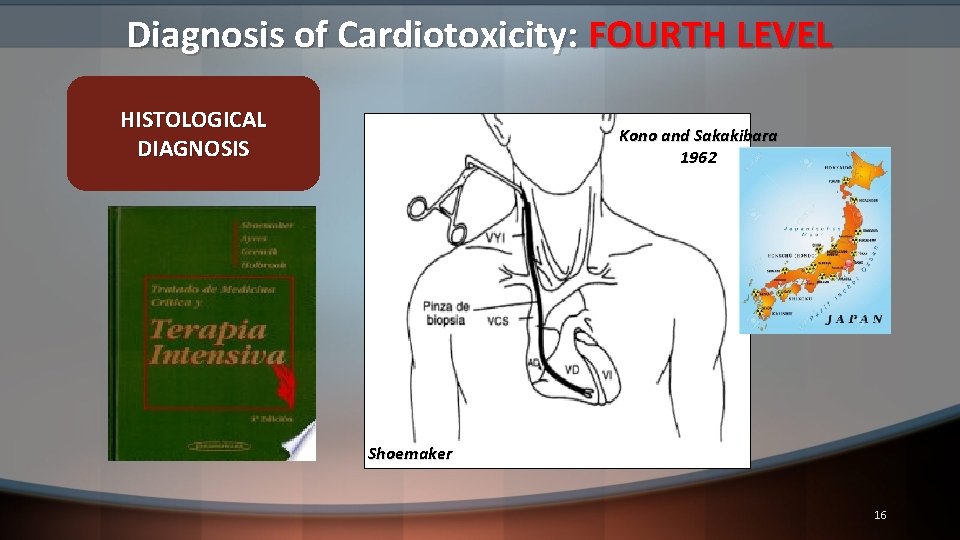
Diagnosis of Cardiotoxicity: FOURTH LEVEL HISTOLOGICAL DIAGNOSIS Kono and Sakakibara 1962 Shoemaker 16

26 diseases ware studied 17

PATHOPHYSIOLOGY OF CARDIOTOXICITY The histopathological study has demonstrated rupture and loss of cardiac myofibrils, mitochondrial edema and structural alterations in cellular endoplasmic reticulum, producing all this myocyte vacuolization and subsequent loss of functionality. With intermediate doses of anthracyclines, the damage is partial. With high doses the damage is total leading to myocyte necrosis and its loss González Barón 18

Spain Cuba Argentina Spain Portugal Mexico Chile 19

Rule of the Cardio - Oncology Teamwork PROTECTION 20

Cardio-Oncology involves comprehensive and continuous care for cancer patients. What does a Cardio-Oncology unit offer? Promote effective communication and decision-making channels among professionals involved in cancer treatment. 1 Stratify the CV risk of the Onco-hematological patient. Develop protocols for prevention, diagnosis and early treatment as well as follow-up of cardiovascular complications. 3 2 Facilitate oncological treatment and avoid interruptions in the administration of antitumor treatment. 4 Register and evaluate the results in health and quality of care and coordinate research protocols. Promote training programs for professionals involved in the care of patients with cancer and CV disease. 6 5 21

Cardiology and Oncology Departments WORKING TOGETHER 22

Cardiology and Oncology Department: Teamwork HOW TO START A CARDIO-ONCOLOGY PRACTICE DEVELOP INDIVIDUAL RELATIONSHIPS AND UNDERSTAND THE NEEDS WORK AS A TEAM UNDERSTAND WHAT YOU CAN OFFER AND DELIVER 23

Cardiology and Oncology Department: Teamwork 24

Cardiology and Oncology teamwork for clinical trials 25

Project of Cardio/Oncology Unit Clinical Trial Protocol 26
Ethical aspect: Logo of Cardio/Oncology Unit in Viet Nam Cuba-Dồng Hoi’ Friendship Hospital BỆNH VIỆN HỮU NGHỊ VIỆT NAM – CUBA ÐồNG HỚI NATIONAL CARDIOVASCULAR AND CARDIO/SURGERY INSTITUTE NATIONAL ONCOLOGY AND RADIOBIOLOGY INSTITUTE 27

28
Finding in Case Presentations 29
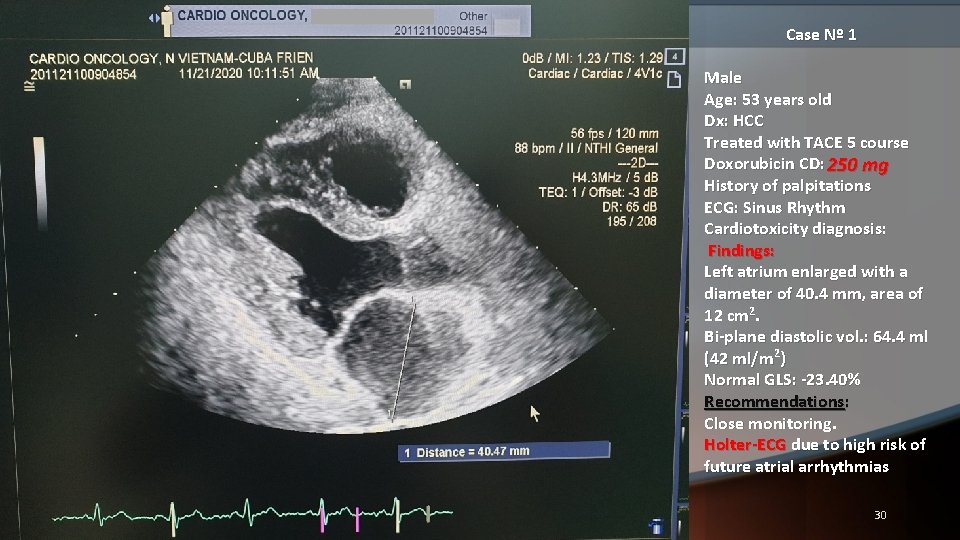
Case Nº 1 Male Age: 53 years old Dx: HCC Treated with TACE 5 course Doxorubicin CD: 250 mg History of palpitations ECG: Sinus Rhythm Cardiotoxicity diagnosis: Findings: Left atrium enlarged with a diameter of 40. 4 mm, area of 12 cm 2. Bi-plane diastolic vol. : 64. 4 ml (42 ml/m 2) Normal GLS: -23. 40% Recommendations: Close monitoring. Holter-ECG due to high risk of future atrial arrhythmias 30
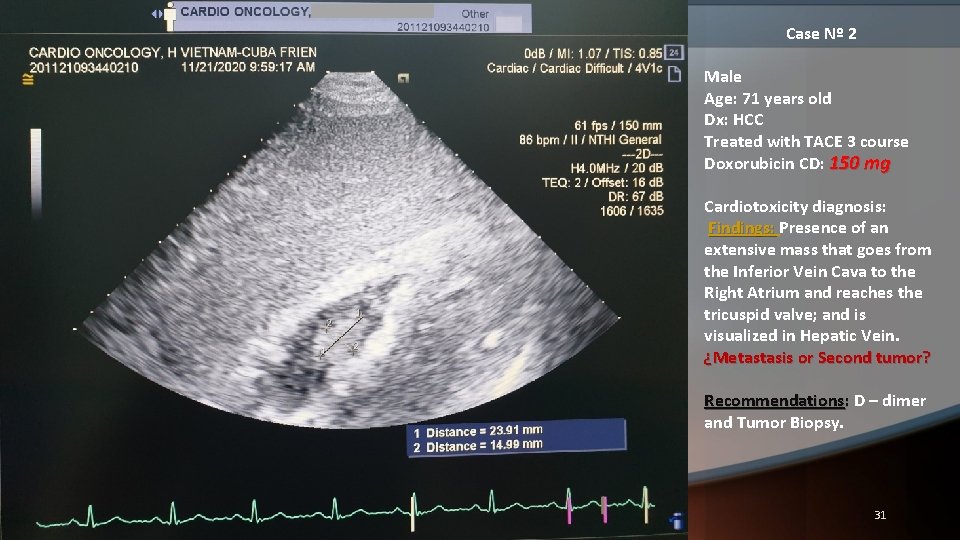
Case Nº 2 Male Age: 71 years old Dx: HCC Treated with TACE 3 course Doxorubicin CD: 150 mg Cardiotoxicity diagnosis: Findings: Presence of an extensive mass that goes from the Inferior Vein Cava to the Right Atrium and reaches the tricuspid valve; and is visualized in Hepatic Vein. ¿Metastasis or Second tumor? Recommendations: D – dimer and Tumor Biopsy. 31
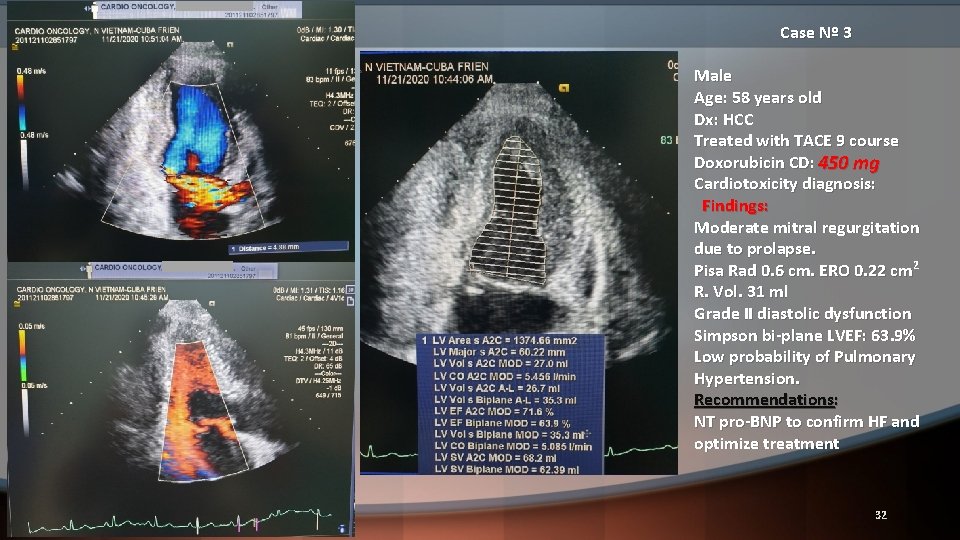
Case Nº 3 Male Age: 58 years old Dx: HCC Treated with TACE 9 course Doxorubicin CD: 450 mg Cardiotoxicity diagnosis: Findings: Moderate mitral regurgitation due to prolapse. Pisa Rad 0. 6 cm. ERO 0. 22 cm 2 R. Vol. 31 ml Grade II diastolic dysfunction Simpson bi-plane LVEF: 63. 9% Low probability of Pulmonary Hypertension. Recommendations: NT pro-BNP to confirm HF and optimize treatment 32

Brazil announces that Cardio/Oncology begins as a specialty. Dr. Marcelo Queiroga. President of Brazilian Society of Cardiology For the first time in the world, Cardio/Oncology specialists will be trained with its own specialty program in Cardio/Oncology 33

Thank you very much! Card iolog ist t s i g o l o c On Cardio-Oncology Unit 34
- Slides: 34