VETERANS ADMINISTRATION CLAIMS VA BILLING TIPS AND RECOMMENDTIONS

VETERANS ADMINISTRATION CLAIMS VA BILLING: TIPS AND RECOMMENDTIONS FOR BEST RESULTS

Agenda What We Will Cover Today • Overview of Today’s VA • Types of VA Community Claims ▫ Emergent ▫ Purchased ▫ Champ. VA • Billing and Collecting VA • General Recommendations • Questions

A Look at The Veterans Health Administration • Provides health care services and benefits programs for American’s Veterans • Nation’s largest integrated health care system ▫ Over 1400 sites of care �Hospitals, clinics, nursing homes, counseling centers, etc. • Manages largest medical education and health professions training program in the US ▫ Train 90, 000 health professionals each year

So why is your volume of VA patients increasing? Increased volume of VA patients ▫ 9 million veterans ▫ 6 million are actively receiving treatment ▫ Downsizing Military means more VA traffic at non-VA facilities • VA facilities can not handle the volume alone • ▫ ▫ ▫ • Lack of available specialists Long wait times Distance between VA Medical Centers Recent legislation changes have made it easier for the Veteran to obtain care at a non-VA facility

What does it mean for most medical providers? • • • VA claim process can be tedious, time intensive and complicated A/R builds up quickly, even at smaller facilities Low reimbursement makes it hard to allocate the resources necessary for successful collection Lack of confidence in timely and accurate reimbursement Multiple changes are occurring as the VA restructures to fulfill commitments made in the Mission Act of 2018

MISSION Act of 2018 • Intent of the Mission Act ▫ Give Veterans access to health care where and when they need it �Replace Veteran’s Choice �Access to Urgent Care �Established Community Care Network ▫ Improve community care for Veterans, their families, community providers and VA employees

Benefit to Veterans ▫ Access to Urgent Care/Walk-In Clinics for emergency services without authorization ▫ Streamlined eligibility criteria ▫ Improved customer service ▫ Telehealth– care through phone or computer ▫ Easier Access to community care providers ▫ Better coordination between regions

Benefit to Community Providers • Easier interaction with the VA • Faster payment ▫ Electronic claims paid within 30 days �Denial response within 30 day ▫ Paper claims paid within 45 days �Denial response within 45 days • Electronic platform for submissions ▫ Late 2019

• Types of VA care Types of Non-VA Claims ▫ Emergency Care ▫ Purchased Care ▫ Champ VA

EMERGENT CARE • Title 38 • Mill Bill

EMERGENT CARE Title 38 (Service Connected) • Title 38 ▫ ▫ ▫ Service-Connected Conditions Adjunct conditions Patients with total permanent disability from SCC Chapter 31 Vocational Rehab Veterans Eligibility �Tx is for medical emergency that they believe would have negatively affected their health �Care at VA facility was not accessible or available ▫ Registration: �Ask patient: �Is this service connected? �Which VAMC are you assigned to for treatment? �Notify VA within 24 -72 hours �Obtain SS# �Submit to Tri. West/CCN contractor in accordance with timely filing requirements

EMERGENT CARE Title 38 (Service Connected) • File no later than 2 years from DOS • Facility Charges ▫ 837 EDI or UB-04 and Itemized bill ▫ Discharge Summary and ED records and notes ▫ VA form 5083 • Physician & other charge ▫ 837 EDI or CMS 1500 and Itemized bill ▫ Emergency department notes / progress notes ▫ VA form 5083 • Payment ▫ Generally, 100% of Medicare

EMERGENT CARE Mill Bill (not service connected) • MILL BILL ▫ Non-Service-Connected • Eligibility Requirements � Tx is for medical emergency that they believe would have negatively affected their health � Care at VA facility was not accessible or available � Patient must be registered with the VA � Patient must have been treated at the VA within the past 24 months � OHI is primary • Registration ▫ Ask Patient: � Are you registered with the VA? � What is the last date of treatment with the VA? � Do you have any other insurance ▫ Obtain SS# ▫ Notify VA within 24 -72 hours ▫ Submit to Tri. West/CCN contractor in accordance with timely filing requirements

EMERGENT CARE Mill Bill • Billing �File within 90 days from DOS or date TPL action is exhausted • Facility Charges � 837 EDI or UB-04 and Itemized bill �Discharge Summary and ED records and notes �VA form 5083 • Physician & other charge � 837 EDI or CMS 1500 and Itemized bill �Emergency department notes / progress notes �VA form 5083 • Payment ▫ Generally, 70% of Medicare

EMERGENT CARE VA as Secondary Currently: • VA regulation ▫ Cannot pay Copay, Coinsurance or deductibles • Wolfe v. Wilkie United States court of Appeals for Veterans Claim ▫ Invalidated VA regulation ▫ VA must reimburse Veterans for out of pocket costs �Deductible and Coinsurance �Applies to private insurance. Unclear for Medicare ▫ Recommend submit to VA

PURCHASED CARE Pre-approved treatment at a non-VA facility

Purchased Care Programs (Pre-Approved Medical Care authorized by VA) ▫ Authorized by Veterans Choice Program (VCP) �Healthnet – ended 09/30/2018 ▫ Authorized by Patient-Centered Community Care Network (PC 3) �Tri. West- coverage ends 09/30/2020 ▫ Veterans Care Agreement ▫ Veterans Urgent Care Benefit ▫ Community Care Network- rolling out throughout 2019 �Optum �Tri. West Healthcare Alliance (dispute)

Authorizations • ALL VA Community Care from all programs require authorization in advance ▫ Initial start of care ▫ Reauthorization for a new episode of care • Local VAMCs manage consults, referrals and authorizations ▫ ▫ ▫ Receive/review consult or enter administrative consult Verify eligibility for Community Care Determine if prior authorization/clinical review is required Initiate and complete referral authorization and enter into system Manage secondary authorizations, obtain documents and close consult �VA 10 -7079 for Outpatient �VA 10 -7078 for Inpatient �Tri. West authorization form/ Standardized Episode of Care (SEOC)

VAMC Authorization/SEOC Form • VAMC Authorization ▫ ▫ Provider information Authorizing VAMC Veteran information Auth information � authorized care, authorization number, valid dates ▫ Initial appointment date ▫ Service description, duration and overview ▫ Outlines situations where additional auth is needed. ▫ Required on claim or claim will deny • SEOC Authorization ▫ ▫ Provider information Authorizing VAMC Veteran Information Auth information �authorized care, authorization number, valid dates ▫ Claim submission information ▫ Initial appointment date ▫ Service description, duration and overview ▫ Code Range: CPT codes that are covered under this authorization �If CPT code is not listed, a Secondary Authorization Request (SAR) must be submitted.

Purchased Care Treatment • Only provide tx as indicated by the authorization • Facility must be listed on the authorization • Pay attention to which VA is submitting the auth ▫ Contact the authorizing VA or submit SAR: �If care deviates from the approved care plan �Additional treatment is needed ▫ The claim must be submitted to the appropriate payer as indicated on auth �VAMC auth- submit claim and medical records directly to VAMC authorizing �Tri. West/SEOC- submit claim to Tri. West, submit medical records to authorizing VAMC.

Purchased Care Considerations • Pre-approval is not required if emergent care becomes necessary during the authorized care/treatment ▫ Contact the VA within 24 hours but no later than 72 hours ▫ If VA has capacity, patient must be transferred when stabilized ▫ If patient refuses transfer, VA will only pay for treatment up to the point of stabilization.

Purchased Care Claims and Payments • VA is the primary and exclusive payer for the Non-VA care it authorizes. • Both VA and other coverage can only be used if patient received authorized and non-authorized services and payers are not being billed for the same services. • Veterans may still be responsible for copayments ▫ Some Veterans are exempt from co-payments

Claim Submissions Preauthorized Claims • As soon as possible but no later than 2 years for NSC and 6 years for SC • Facility Charges ▫ 837 EDI or UB-04 and Itemized statement ▫ Hospital Discharge summary or outpatient tx records and progress notes ▫ Authorization Form • Physician or other professional fees ▫ 837 EDI or CMS 1500 and Itemized statement ▫ Outpatient Hospital Emergency tx records/progress notes ▫ Authorization form

VA Community Care Network (CCN) • 4 private sector contractors • Develop and administer regional networks of high performing licensed health care providers • Provides local flexibility and increased access to care • Contract vehicle for VA to purchase care in the community. • “The CCN contracts were developed with a focus on transparency, accountability, quality, and increased communications between VA and Veterans. ”- VA. gov • Health. Net and Tri. West were temporary solutions, CCN will be a permanent solution to providing veterans with flexible and increased access to care.

CCN Eligibility Criteria • • Best Medical Interest of the Veteran Required care or services are not offered by VA Lack of full-service medical facility Care or services are non-complaint with VA’s standards for quality • Care or services not provided within designated access standards • Grandfathered eligibility from Veterans Choice Program

CCN-Eligibility Access Standards ▫ Primary Care, Mental Health, Non-institutional Extended care �Drive Time 30 minutes �Wait time 20 days ▫ Specialty Care �Drive Time 60 minutes �Wait time 28 days
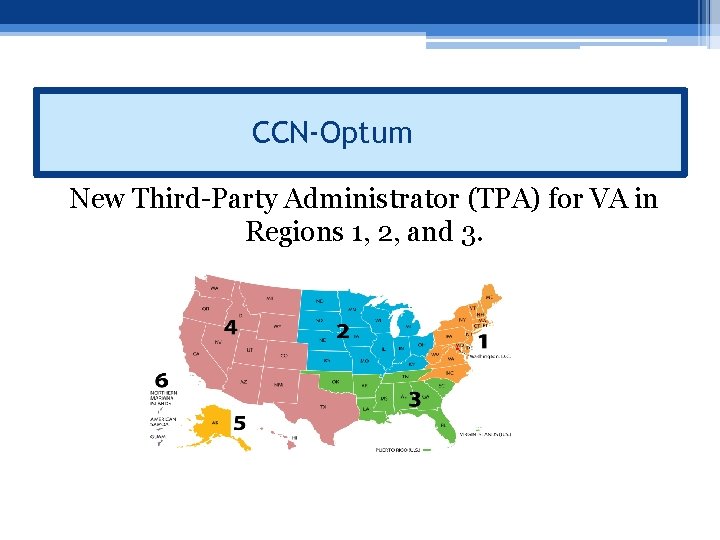
CCN-Optum New Third-Party Administrator (TPA) for VA in Regions 1, 2, and 3.

CCN-Tri. West • Previously awarded contract for Region 4. • As of 08/19/2019, under protest and “stop work order” until further notice. • Per Update from Veterans Health Administration: This does not impact community providers who are currently in partnership with Tri. West as PC 3.

CCN-Optum • Transition from Tri. West (PC 3) to Optum will take place: ▫ Region 1: July 29, 2019 -December 28, 2019 and will be deployed in 5 phases. ▫ Region 2: October 8, 2019 -April 9, 2020 and will be deployed in 5 phases. ▫ Region 3: TBD • Tri. West will continue authorize care during the 30 -day transitional phase of each VAMC. • For more information regarding which phase your VAMC is in and to sign up for training, visit: https: //provider. vacommunitycare. com/tpa-apweb/? nav. Deep. Dive=VACCN%20 public. News. Announcem ents. Menu

CCN-Optum To become a registered provider with Optum, send the following information to the email listed below: vaccnprovidercontracting@optum. com ▫ ▫ ▫ ▫ Business Name: State located: Phone number: Email Address: Tax ID: NPI: Provider Type (medical, behavioral health, physical health, home health, etc. ): ▫ How can we help you? : contract with VA CCN
CCN-Optum • Claim Submission Address: VA CCN Optum PO Box 202117 Florence, SC 29502 • Electronic Claim Submission Payer ID: VACCN

CHAMP VA

CHAMP VA • Health Care Benefits program shares the cost of health care services with eligible beneficiaries • Managed by the CBOPC in Denver, CO • Eligibility checked 24/7 via IVR ▫ 1 -800 -733 -8387 • No contract providers • Some pre-authorizations are required ▫ DME ▫ Mental Health/Substance Abuse ▫ Organ and Bone Marrow Transplants

BILLING AND COLLECTING ON VA CLAIMS

VA Claims Processing VA encourages the use of electronic health care claims for timely payment. • Community Providers must use EDI for which care is authorized: ▫ PC 3/CCN to Tri. West or CCN Contractor (Optum) ▫ VCP Provider Agreements to VA ▫ Traditional Community Care (9/30/20) to VA

Claim Submission Process Overview • Past ▫ Mailed paper claims to local VA medical centers ▫ Manual entry and verification of paper claims ▫ Corrected errors manually throughout processing • Current ▫ Consolidating mailed paper claims and sending to single location ▫ Separating claims from attachments, scanning and converting to electronic format ▫ Automatically identifying errors up front based on industry standards ▫ Sending rejection letters to correct the errors • Future ▫ Nearly all claims will be submitted electronically ▫ Processing of exceptions for paper will require mailing to a new location directly for conversion to electronic format ▫ Enhancing current process to attach medical documentation to electronic claims submissions

Current Method for Submitting Claims • Submit electronically via Change Healthcare ▫ Preferred method �If not connected to Change Healthcare �Add payer ID to your EDI clearinghouse ▫ ‘ 12115’ for medical claims/ERA ▫ ‘VAFEE’ for an eligibility inquiry transaction (270/271) ▫ Expedites claims processing �Future will include adding EDI 275 Attachments as supporting medical documentation • Mailing Claims ▫ Mail to designated claims processing unit ▫ Use original UB or 1500 ▫ Strongly encouraged to transition to electronic format asap

Billing and Collection Resources • PFRAR ▫ Mailed weekly ▫ Explains the payment that will be issued or reason for denial/rejection ▫ Only access for any denial reasons • CEP- Customer Engagement Portal ▫ Obtain claim status- VA Fee Basis claims only ▫ Run payment reports • Availity ▫ Check eligibility ▫ Check VA Choice claim status • Tri. West Portal ▫ View authorization information ▫ View TW claim status • e. CAMS ▫ Modernizes the processing of claims received by community providers outside VA’s Community Care Network • HSRM • New portal allowing direct and immediate communication between VA provider and non-VA community care provider.

Classification of Processed Claims • Accepted ▫ Correctly billed and pre-authorized • Denied ▫ No pre-authorization ▫ Veteran not eligible for emergency care • Rejected ▫ Billing errors ▫ Additional information needed

Top Reasons for Rejected Claims • • • Duplicate Claims/Previously Paid Medical Records needed Billing/Coding Errors Submit claim to wrong Contractor Authorization Errors ▫ Exceeds Visits, Not Authorized, location of treatment, etc.

Top Reasons for Denied Claims • • Not Timely Filed Non Emergent Care Not Authorized Not registered and/or no treatment in 24 months • VA available • OHI

General Recommendations • Patient Access Training ▫ Identify correct VA payer � Check Auth form � Ask patient for SC emergency claims � Send NSC emergency to closest VA Medical Center ▫ Eligibility Determination � Use patient SS#, not DOD number or Benefits ID number � Is patient registered with the VA? � Last VA treatment date within 24 months? � Where are they assigned for treatment? ▫ Be proactive about authorizations ▫ Timely Notification Requirements • Take advantage of VA training webinars ▫ www. va. gov/COMMUNITYCARE/providers • Provide Patient Education ▫ Eligibility for Emergency Care ▫ Transfer refusal consequences and consent

• Billing ▫ Submit Electronically ▫ Submit paper claims quickly to allow time for scanning and identification within timely filing limitations • Follow up ▫ Establish process for PFRAR scanning ▫ Work with your VA to implement efficient follow up procedures ▫ Begin follow up at 30 days after claim submission* • Denials ▫ Track your denials to identify causes that can be corrected • Coding ▫ VA follows CMS guidelines ▫ Track your denials • Appeals ▫ Can be submitted with documentation within 1 year ▫ May need to involve the patient


QUESTIONS? Lori Lipocky, CPCU Lori. Lipocky@Aspirion. Health. com
- Slides: 45