VETERAN NEEDS ASSESSMENT Richard L Roudebusch Veterans Administration

VETERAN NEEDS ASSESSMENT Richard L. Roudebusch Veterans Administration (VA) Medical Center Julie Gregg, MSN, CRNA
VETERAN DEMOGRAPHICS Veterans Integrated Service Network (VISN)10 includes Michigan, Ohio, and Indiana. The number of veterans in VISN 10 with VA benefits is approximately 685, 000. Veterans are more likely to have been married, live above the poverty level, and have higher median incomes than the non-veteran.

VA veterans are older, with a median age above the veteran median age of 65 years. VA veterans are more likely to be unemployed and live below the poverty level. VA veterans are less likely to have received a high school diploma. The largest cohort is Vietnam War veterans. VA VETERAN DEMOGRAPHICS

MAJOR HEALTH NEEDS DIAGNOSIS, TREATMENT, AND VETERANCENTRIC CARE FOR THOSE WITH POSTTRAUMATIC STRESS DISORDER. CARE FOR AN ELDERLY COHORT WITH SPECIFIC FOCUS ON FRAILTY AND HEART DISEASE. DIAGNOSIS AND TREATMENT OF HEPATITIS C VIRUS. IMPROVED ACCESS TO CARE.

PTSD symptoms are grouped into four categories: Intrusive thoughts or flashbacks. Avoidance of people or places that may trigger memories of the trauma. Negative mood or thoughts associated with memory loss, guilt or detachment. Arousal or reactivity with hypervigilance, irritability and selfabusive behavior. MAJOR HEALTH NEEDS: PTSD

MAJOR HEALTH NEEDS: FRAILTY Frailty is a state where a person is at higher risk for health complications and falls. Frail patients can be described as weak, weary, and wasted. Frailty assessments have been developed to predict those patients at higher risk for postoperative complications, allowing health care professionals to intervene to reduce adverse outcomes. Frailty assessments can differentiate between those patients who may require targeted postoperative care from those at no increased risk.

MAJOR HEALTH NEEDS: MYOCARDIAL ISCHEMIA Myocardial ischemia is another risk associated with surgery in the elderly and is the most common cardiac complication. In the elderly, myocardial ischemia occurs without chest pain in 80% of the cases and is often not recognized by health care personnel because the symptoms (tachycardia, hypotension, confusion, nausea, and dyspnea) are common symptoms in the post-surgical patient. Myocardial infarction occurs most often on postoperative day one.

MAJOR HEALTH NEEDS: HEPATITIS C VIRUS Hepatitis C virus is the most common blood-borne infectious agent in the U. S. It affects VA veterans 2 -3 times more than non-veterans, making the VA the largest provider for Hepatitis C care in the world. The Hepatitis C virus affects the liver and can lead to serious liver complications and liver cancer.

MAJOR HEALTH NEEDS: ACCESS TO CARE In 2013, there was a 47. 6% increase in use of an anesthesia provider for sedation for endoscopy procedures for Medicare patients. In the VA system, demand for MAC sedation has more than doubled. Veterans Health Administration Directive-1230 mandates goal of less than a 30 -day wait for services. In 2017, the Richard L. Roudebush VA Medical Center Endoscopy Department had a wait of up to 120 days for scheduling patients requiring anesthesia services.

WHAT INFLUENCES SEDATION NEEDS? The reasons why there has been a need for expanded anesthesia coverage is unclear. What factors cause a patient to be difficult to sedate using medications administered by the nursing staff? One proposed reason is chronic cannabis use.

CANNABIS PREVALENCE RATES Cannabis is the most commonly used illicit drug. In VISN 10, the prevalence rate for cannabis use is 0. 74% to 0. 93% in veterans. However, some researchers report prevalence rates of 6. 3%. In one study, the rate of cannabis use increased 59% from the start of the study period (2002) until the end of the study period (2009). Substance abuse and PTSD are linked.

There is an association between anxiety and the use of cannabis: PTSD AND CANNA BIS USE • The rates of PTSD and CUD both increased from 2002 -2009 and the percentage of veterans with a CUD who also had a psychiatric diagnosis was 70%. • For veterans with PTSD and a Substance Use Disorder, cannabis was the substance implicated in 22. 7% of the patients. • For veterans who use cannabis, those that defined their cannabis use as medicinal (rather than recreational) had more symptoms of arousal when cued about experiences during combat. The link between CUD and PTSD is strong, but it is unknown if cannabis is used to self-medicate for the symptoms associated with PTSD or is unrelated.

EFFECTS OF CANNABIS USE ON THE BODY CARDIOVASCULAR EFFECTS ARE RELATED TO AN INCREASE IN SYMPATHETIC AND A DECREASE IN PARASYMPATHETI C ACTIVITY. SYMPTOMS INCLUDE TACHYCARDIA, ELEVATED BLOOD PRESSURE, AND VASODILATION LEADING TO POSTURAL HYPOTENSION. ECG CHANGES CAN INCLUDE PREMATURE VENTRICULAR CONTRACTIONS (DUE TO VOLTAGE CHANGES) AND BRADYCARDIA (DUE TO DEPRESSION OF CARDIAC MUSCLE).

EFFECTS OF CANANBIS USE ON THE BODY Cananbis use increases myocardial oxygen use and can precipitate myocardial ischemia. The annual risk of Myocardial Ischemia is doubled with daily cannabis use.

PICO QUESTI ON Does chronic cannabis use increase the risk that Monitored Anesthesia Care (MAC) will be required for elective endoscopic procedures?

STUDY DESIGN A retrospective analysis will be performed from patients who underwent an elective colonoscopy from 2013 -2017. Records of patients with documented cannabis use will be analyzed for sedation requirements. A concurrent PTSD diagnosis will be considered as a confounding variable.

OUTCOMES The study aims to determine if chronic cannabis use leads to sedation tolerance. The study aims to determine if the concurrent diagnosis of PTSD with cannabis use influences sedation requirements. The study aims to understand past sedation requirements to predict future needs.
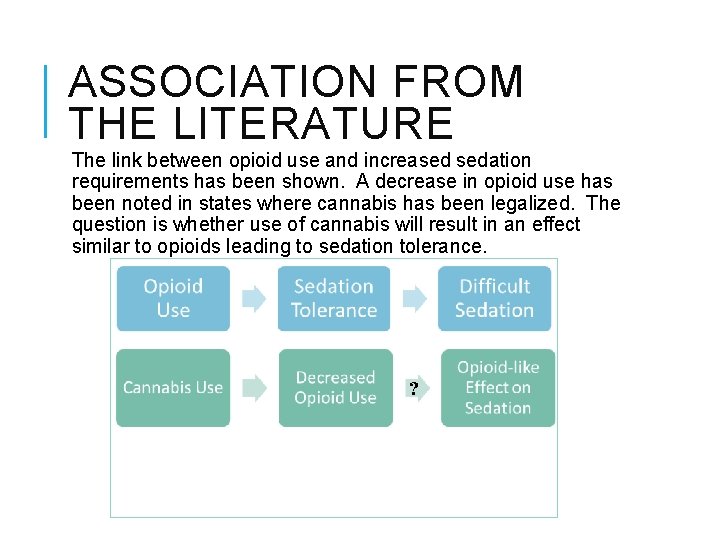
ASSOCIATION FROM THE LITERATURE The link between opioid use and increased sedation requirements has been shown. A decrease in opioid use has been noted in states where cannabis has been legalized. The question is whether use of cannabis will result in an effect similar to opioids leading to sedation tolerance. ?
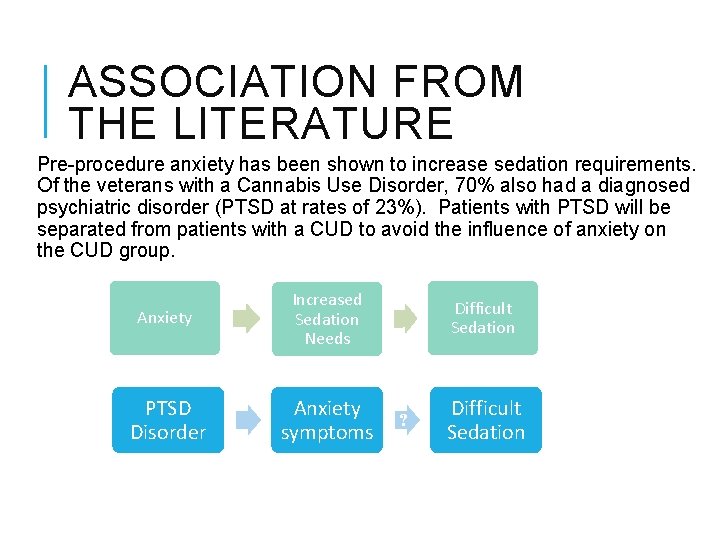
ASSOCIATION FROM THE LITERATURE Pre-procedure anxiety has been shown to increase sedation requirements. Of the veterans with a Cannabis Use Disorder, 70% also had a diagnosed psychiatric disorder (PTSD at rates of 23%). Patients with PTSD will be separated from patients with a CUD to avoid the influence of anxiety on the CUD group. Anxiety Increased Sedation Needs PTSD Disorder Anxiety symptoms Difficult Sedation ? Difficult Sedation

PROJEC T TEAM MEMBE RS Project Chair- Dr. Susan Eley Research Mentor- Dr. Gene Harker Project Advisory Team Member- Dr. Thomas Carr Project Advisory Team Member- Dr. Thomas Imperiale

Inclusion Criteria: INCLUSI ON AND EXCLUS ION CRITERI A Males, ages 50 -75, with a BMI over 21, who underwent an elective colonoscopy at the Richard L. Roudebush VAMC during 20132017. Exclusion Criteria: Based on the results of two studies [4, 8], all confounding variables identified as increasing sedation requirements, including female gender, low BMI, opioid and benzodiazepine use, an alcohol use disorder, and anxiety (PTSD), will be controlled. Patients with an alcohol use disorder, with an ICD-10 code F 10 or ICD-9 code of 303. 9 or 305. 0, will be excluded along with patients with an active prescription for opioids or benzodiazepines.

The goal is to determine the mean drug dose requirements of fentanyl and versed for the study groups. The groups will then be compared to determine the influence of cannabis use on sedation requirements and the impact of PTSD on sedation requirements. Study Group One: Patients with a CUD excluding those with an ICD code for PTSD. Study Group Two: Patients with a diagnosis of PTSD. Study Group Three: The control group, will consist of study participants excluding those with a CUD or PTSD diagnosis. Anxiety has been linked to increased sedation needs and cannabis has not, theoretically, Group Two with a diagnosis of PTSD, should have higher mean drug dosages compared to Groups One and Three. Additionally, the CUD group and the control group should have similar mean drug dosages. METHODS
POWER ANALYSIS A power analysis was performed using three different calculators. The power analysis was completed for independent-samples-ttest, to determine if the means of two separate groups are statistically different. The numbers of subjects required for each group is 31. 4.

STATIS TICAL ANALYS IS A multivariate analysis of variance (MANOVA) will be performed to evaluate the groups on the two dependent variables, the mean Fentanyl and mean Versed doses. The MANOVA analyses the two dependent variables as one and can determine if the difference in the means of the two groups happened by chance. Performing a MANOVA instead of multiple analyses on each of the dependent variables separately decreases the chance of a Type 1 error by decreasing the number of analyses done. A MANOVA analysis is appropriate for this study because it allows for more than two independent variables and two dependent variables that correlate with each other and are singular in nature as they both define sedation requirements. The mean scores of the Fentanyl and Versed doses for the groups are also analyzed separately in a MANOVA analysis.

PROJECT STATUS IRB approval was granted in December 2017. An application to the VINCI databank was initiated on August 15, 2018. Data set was made available on October 3, 2018. Project will be a review of patient records from the VAMC. All data analysis must be preformed on VAMC SPSS software.
STRENGTHS OF PROJECT There are no RCT in the literature concerning the effect of cannabis on sedation requirements. Studies on cannabis rely on retrospective reviews of the data. The strength of this study is the access to a large pool of data. Most studies found were poorly controlled with small numbers of subjects. Another strength is the ability to control many confounding variables.

THREATS TO PROJECT The major threat to this project is the study design relying on the accuracy and completeness of the patient record.

Strengths Superior team support. Familiarity with the data system. Clear vision of data needs and outcome measures. SWOT ANALYS IS Weaknesses Reliance on VA personnel for access to data. Retrospective study design. Opportunities Gather data that can change and improve the care given to veterans. Threats Difficulty accessing the correct data from the data tables.

DATA The initial data pool consisted of 8, 662 patients. 991 were excluded due to various alcohol/opioid/drug disorder diagnoses. 1087 more were excluded due to the requirement of MAC sedation. 41 women were excluded. 1115 were excluded for being over 75 years of age or younger than 50 years of age. After application of the BMI requirement and exclusion of those with incomplete data, over 4000 patients remained. A total of 76 had a Cannabis Use Disorder. Over 700 had a PTSD diagnosis.
- Slides: 29