Vestibulocolic reflex The Horizontal Rotational Vestibuloocular Reflex Head

Vestibulo-colic reflex

The Horizontal Rotational Vestibulo-ocular Reflex Head in space Eye in head Eye in space

Canals are excited when the head moves in their direction • Rotating the head to the left stimulates the left horizontal canal and inhibits the right horizontal canal, driving the eyes horizontally to the right. This excites • the left medial rectus • and right lateral rectus. • And inhibits the right medial rectus • and left lateral rectus
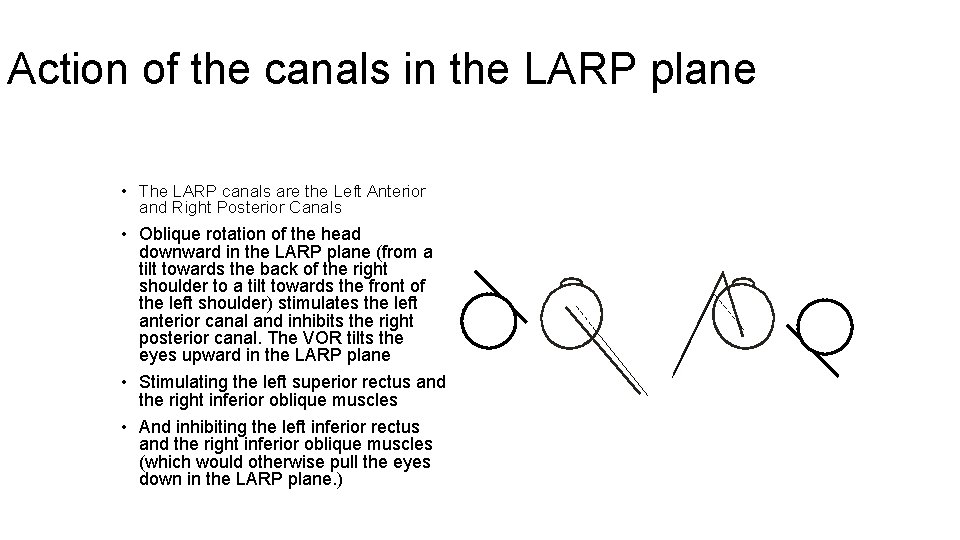
Action of the canals in the LARP plane • The LARP canals are the Left Anterior and Right Posterior Canals • Oblique rotation of the head downward in the LARP plane (from a tilt towards the back of the right shoulder to a tilt towards the front of the left shoulder) stimulates the left anterior canal and inhibits the right posterior canal. The VOR tilts the eyes upward in the LARP plane • Stimulating the left superior rectus and the right inferior oblique muscles • And inhibiting the left inferior rectus and the right inferior oblique muscles (which would otherwise pull the eyes down in the LARP plane. )

What about the cerebellum? • The cerebellum is necessary to suppress the vestibulo-ocular reflex when necessary. • The cerebellum is necessary to change the gain of the reflex. • Gain: the ratio of eye rotation to head rotation.

The VOR is plastic • It can be suppressed when you don’t want it. • Its gain can change. • How do you know if the VOR is doing a good job? • There is no motion on the retina when the head moves. • If a muscle is weakened, a given central signal will be inadequate, and the world will move on the retina. • This can be mimicked by spectacles that increase retinal slip. • In either case, the brain adjusts the VOR signal so the retinal slip is eliminated. • The cerebellum is necessary for both suppression of the VOR and for slipinduced gain change.

My favorite cerebellar sign – failure to suppress the VOR • Have the patient look at something that is rotating with the head. • Failure to suppress the VOR requires attention.
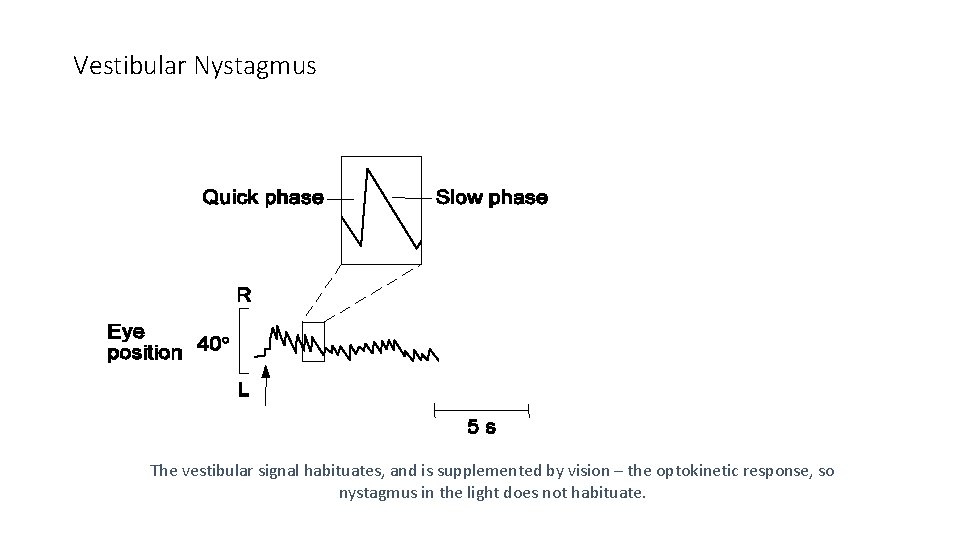
Vestibular Nystagmus The vestibular signal habituates, and is supplemented by vision – the optokinetic response, so nystagmus in the light does not habituate.

The optokinetic signal • The vestibular system is imperfect • The cupula habituates in 5 seconds. • The brainstem and cerebellum extend this time to roughly 25 seconds, after which there is no further response to head acceleration. • The vestibular system is a poor transducer of very slow (<0. 1 Hz) rotation. • The visual system compensates for the inadequacies of the vestibular signal by providing a description of the retinal motion evoked by the head movement. • The optokinetic response is mediated by neurons in the accessory optic system in the pretectum, and the motion-sensitive areas in the cortex (MT and MST).

Vestibular Afternystagmus • When the head starts to rotate, the endolymph lags behind the cupula, and distorts the hair cells, causing a head movement signal. • When the fluid equilibrates, the hair cells are no longer distorted. • In the light the optokinetic reflex makes up for the silencing of the labyrinth. • When the head stops moving, the endolymph continues to move, distorting the hair cells in the opposite direction.

The vestibular nucleus combines visual and vestibular signals Rotate in Dark Rotate in Light Visual Motion

The Horizontal Translational VOR • Keeps the eyes still when the head moves laterally (for example when you are looking out of the window of the A train and trying to read the name of the station past which you are traveling). • Gain is dependent on viewing distance: during translation a far object moves less on the retina than a near object. • The rotational VOR is not dependent upon viewing distance. • Most head movement evokes a combination of the rotational (canal) and translation (otolith) VOR’s.

Ocular counter-rolling: testing the otolith system

Visual-vestibular conflict • Full-field visual stimulation is an effective stimulus for the vestibular nucleus. The neurons can’t tell the difference, nor can you! • Ordinarily the head movement implied by the visual and visual signals are equal. • Motion sickness – nausea and vomiting – occurs when the visual and vestibular signals are unequal.

Other sequelae of peripheral vestibular dysfunction • Head tilt. • Difficulty compensating for perturbations of head positon – functional imbalance. • Difficulty with path integration.

Peripheral causes of vestibular dysfunction • Benign positional vertigo: debris from the otoconia in the utricle float into the posterior canal, causing interference with cupula function, brought out by motion in the plane of the affected posterior canal. This can be treated by the Epley maneuver, that rotates the head to float the debris away.


Peripheral causes of vestibular dysfunction • Benign positional vertigo: debris from the otoconia in the utricle float into the posterior canal, causing interference with cupula function, brought out by motion in the plane of the affected posterior canal. This can be treated by the Epley maneuver, that rotates the head to float the debris away. • Acute viral labyrinthitis. • Alcohol – alcohol is lighter than blood, so the hair cells float in the endolymph. • Meniere’s disease – increased endolymphatic pressure. • Toxins – especially antibiotics like streptomycin and gentamycin and NSAIDS.

Central causes of vertigo and nystagmus. • Vestibular nuclei. • Cerebellum. • Peripherally caused nystagmus is worse with the eyes closed, because the normal cerebellum can use vision to suppress the nystagmus.
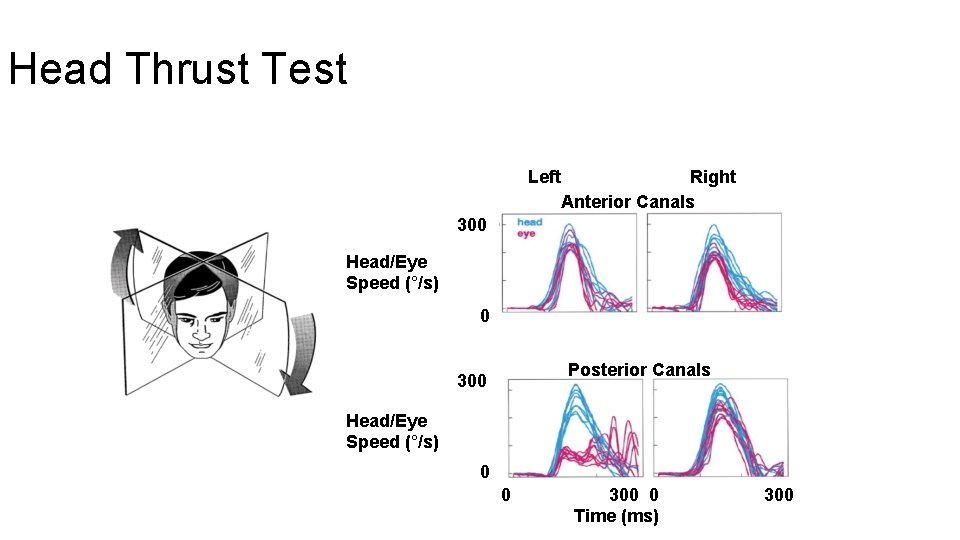
Head Thrust Test Left Right Anterior Canals 300 Head/Eye Speed (°/s) 0 Posterior Canals 300 Head/Eye Speed (°/s) 0 0 300 0 Time (ms) 300
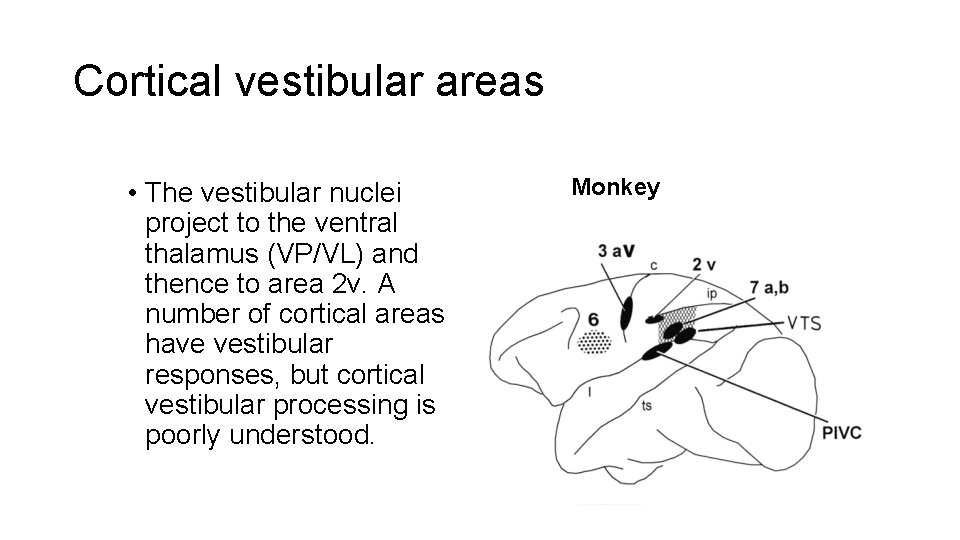
Cortical vestibular areas • The vestibular nuclei project to the ventral thalamus (VP/VL) and thence to area 2 v. A number of cortical areas have vestibular responses, but cortical vestibular processing is poorly understood. Monkey
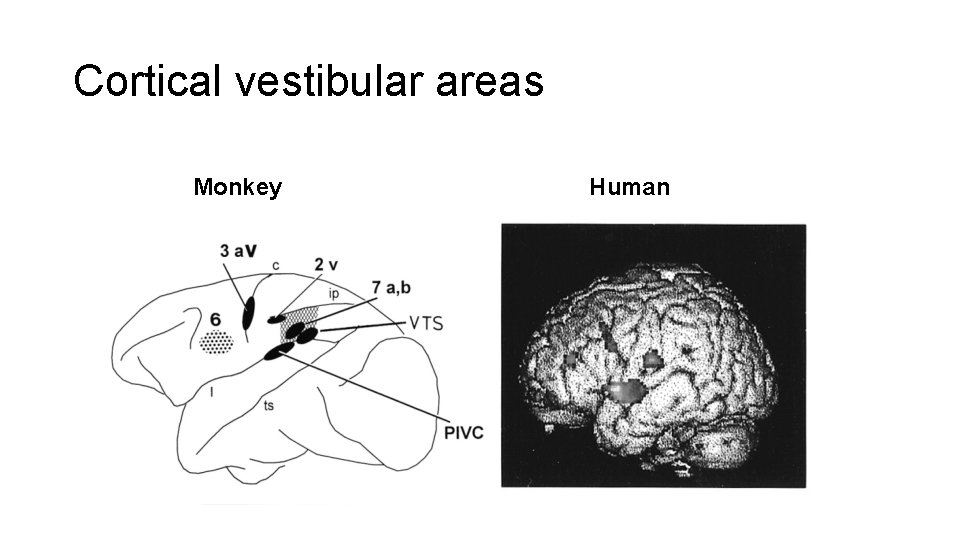
Cortical vestibular areas Monkey Human

Perceptual aspects of vestibular function • Self-motion. • Vertical orientation. • Patients with lesions of parietoinsular cortex have difficulty perceiving the vertical: they think vertical are tilted – usually but not always away from the lesion.
- Slides: 23