Vessel prep BTK Current Status Gunnar Tepe MD

Vessel prep BTK – Current Status Gunnar Tepe MD Ro. Med Rosenheim

Gunnar Tepe, MD. Disclosure I have to report this relationships: Study support: Bayer, BBraun, Bard, Biotronic, BSC, Gore, Medtronic, Phillips, Verian
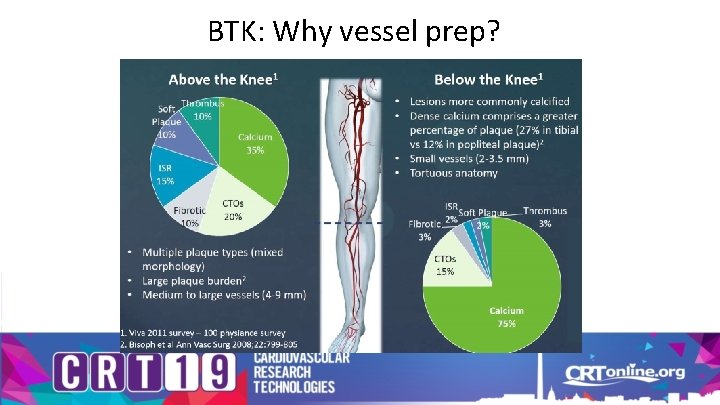
BTK: Why vessel prep?
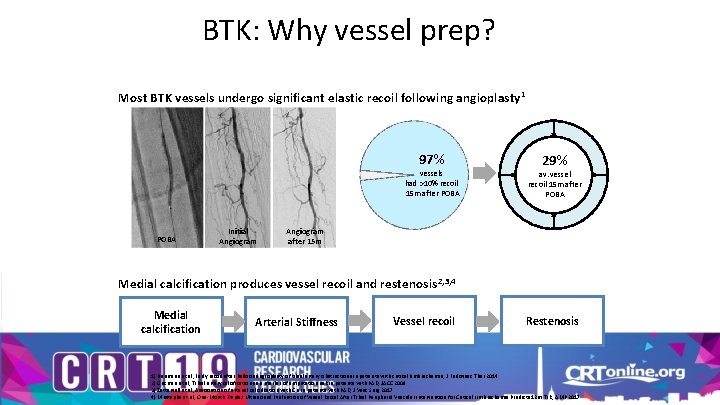
BTK: Why vessel prep? Most BTK vessels undergo significant elastic recoil following angioplasty 1 97% vessels had >10% recoil 15 m after POBA Initial Angiogram 29% av. vessel recoil 15 m after POBA Angiogram after 15 m Medial calcification produces vessel recoil and restenosis 2, 3, 4 Medial calcification Arterial Stiffness Vessel recoil Restenosis 1) Baumann et al, Early recoil after balloon angioplasty of tibial artery obstructions in patients with critical limb ischemia, J Endovasc Ther 2014 2) Guzman et al, Tibial artery calcification as a marker of amputation risk in patients with PAD, JACC 2008 3) Zettervall et al, Association of arterial calcification with CLI in patients with PAD, J Vasc Surg 2017 4) Mustapha et al, One-Month Duplex Ultrasound Evaluation of Vessel Recoil After Tibial Peripheral Vascular Intervention for Critical Limb Ischemia Predicts 12 m TLR, AMP 2017
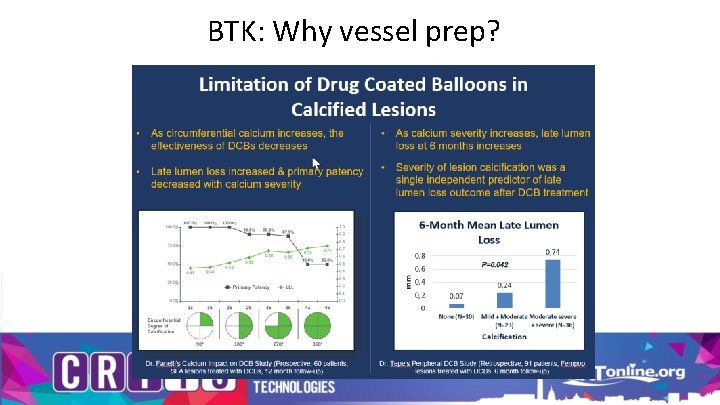
BTK: Why vessel prep?

BTK Clinical Problem
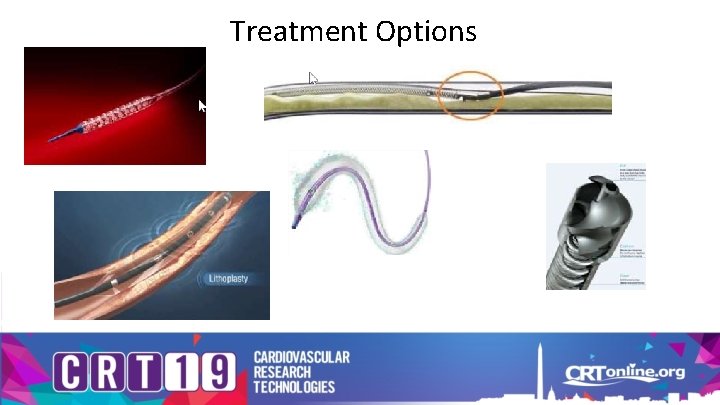
Treatment Options
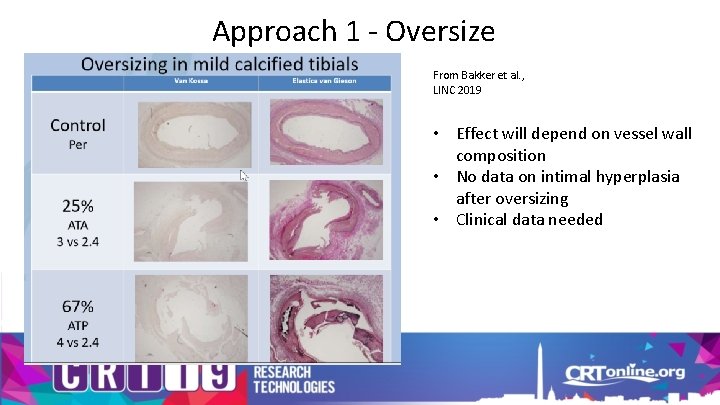
Approach 1 - Oversize From Bakker et al. , LINC 2019 • Effect will depend on vessel wall composition • No data on intimal hyperplasia after oversizing • Clinical data needed

Approach 2 – Special Balloon (Chocolate)
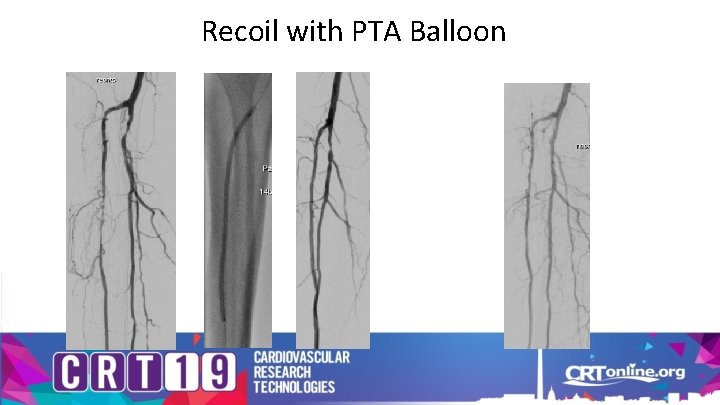
Recoil with PTA Balloon
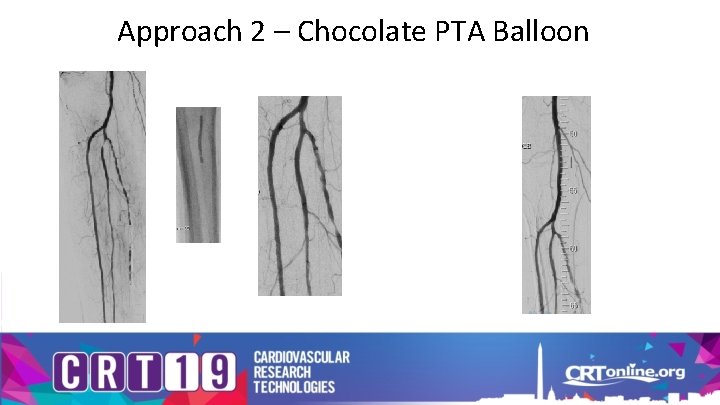
Approach 2 – Chocolate PTA Balloon

Approach 3 - Phoenix

Approach 3 - Phoenix
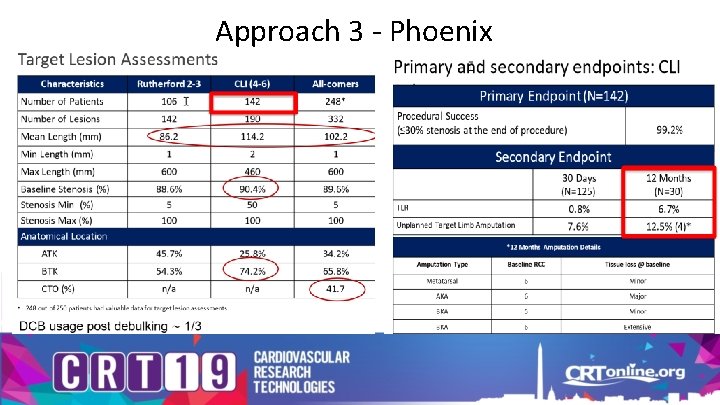
Approach 3 - Phoenix

Approach 3 – Phoenix + DCB

Approach 4 – Orbital Atherectomy

Approach 4 – Orbital Atherectomy

Approach 4 – Orbital Atherectomy

Approach 5 – Shockwave Litoplasty IVL Generator COMPACT & RECHARGABLE Portable, IV-pole Mountable Battery-Powered No External Connections IVL Connector Cable SIMPLE & QUICK Smart Magnetic Connection Push-Button Activated Integrated PTA Balloon IVL Catheter INTUITIVE & SAFE OTW System Any. 014” Guidewire Standard PTA Technique 180 Lithotripsy Pulses Lithotripsy Emitters The Shockwave IVL System consists of an IV pole-mountable generator, a connector cable, and a catheter that houses an array of lithotripsy emitters enclosed in an integrated balloon.

Sonic Pressure Waves Crack Calcium Inside Artery Wall After inflating the integrated balloon to 4 atm, a small spark at the emitters vaporizes the saline-contrast solution and creates a bubble which rapidly expands and collapses within the balloon; this expanding and collapsing bubble creates a short burst of sonic pressure waves. The sonic pressure waves travel through the vessel tissue, while reflecting off and cracking calcium with an effective pressure of ~50 atm. The emitters along the length of the device create a localized field effect within the vessel to fracture both intimal and medial calcium. The integrated balloon plays a unique role; its apposition to the vessel wall facilitates efficient energy transfer during IVL, after which, it is used to dilate the lesion to maximize lumen gain. 20

DISRUPT BTK Study: Infrapopliteal Disease Design Key eligibility criteria • Rutherford category 1 -5 infrapopliteal disease • Infrapopliteal lesions ≥ 50% stenosis • RVD 2. 5– 3. 5 mm, ≤ 150 mm length • Moderate and severe calcification by angiography Endpoints Procedural • Primary Effectiveness: Acute reduction in % diameter stenosis Follow up: 30 days • Major adverse events (Death, MI, TLR, amputation) Objective: To study the safety and performance of the Shockwave Medical Peripheral Intravascular Lithotripsy System in the treatment of calcified, stenotic infrapopliteal peripheral arteries.
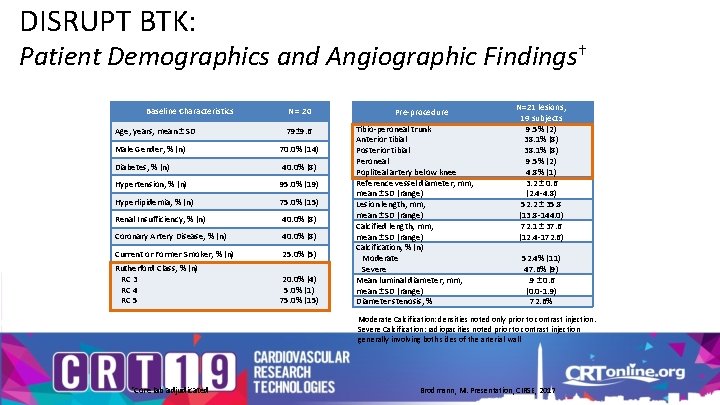
DISRUPT BTK: Patient Demographics and Angiographic Findings† Baseline Characteristics Age, years, mean ± SD N = 20 79± 9. 6 Male Gender, % (n) 70. 0% (14) Diabetes, % (n) 40. 0% (8) Hypertension, % (n) 95. 0% (19) Hyperlipidemia, % (n) 75. 0% (15) Renal Insufficiency, % (n) 40. 0% (8) Coronary Artery Disease, % (n) 40. 0% (8) Current or Former Smoker, % (n) 25. 0% (5) Rutherford Class, % (n) RC 3 RC 4 RC 5 20. 0% (4) 5. 0% (1) 75. 0% (15) Pre-procedure Tibio-peroneal trunk Anterior tibial Posterior tibial Peroneal Popliteal artery below knee Reference vessel diameter, mm, mean ± SD (range) Lesion length, mm, mean ± SD (range) Calcified length, mm, mean ± SD (range) Calcification, % (n) Moderate Severe Mean luminal diameter, mm, mean ± SD (range) Diameter stenosis, % N=21 lesions, 19 subjects 9. 5% (2) 38. 1% (8) 9. 5% (2) 4. 8% (1) 3. 2 ± 0. 6 (2. 4 -4. 8) 52. 2 ± 35. 8 (13. 8 -144. 0) 72. 1 ± 37. 6 (12. 4 -172. 6) 52. 4% (11) 47. 6% (9). 9 ± 0. 6 (0. 0 -1. 9) 72. 6% Moderate Calcification: densities noted only prior to contrast injection. Severe Calcification: radiopacities noted prior to contrast injection generally involving both sides of the arterial wall †Core lab adjudicated Brodmann, M. Presentation, CIRSE, 2017
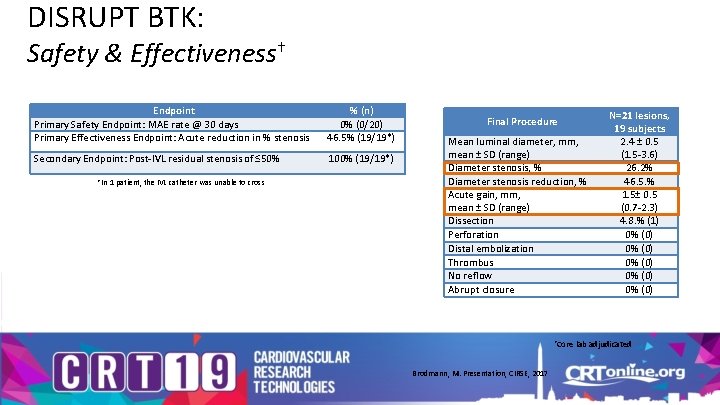

DISRUPT BTK: Safety & Effectiveness† Endpoint Primary Safety Endpoint: MAE rate @ 30 days Primary Effectiveness Endpoint: Acute reduction in % stenosis % (n) 0% (0/20) 46. 5% (19/19*) Secondary Endpoint: Post-IVL residual stenosis of ≤ 50% 100% (19/19*) *In 1 patient, the IVL catheter was unable to cross Final Procedure Mean luminal diameter, mm, mean ± SD (range) Diameter stenosis, % Diameter stenosis reduction, % Acute gain, mm, mean ± SD (range) Dissection Perforation Distal embolization Thrombus No reflow Abrupt closure N=21 lesions, 19 subjects 2. 4 ± 0. 5 (1. 5 -3. 6) 26. 2% 46. 5. % 1. 5± 0. 5 (0. 7 -2. 3) 4. 8. % (1) 0% (0) 0% (0) †Core lab adjudicated Brodmann, M. Presentation, CIRSE, 2017
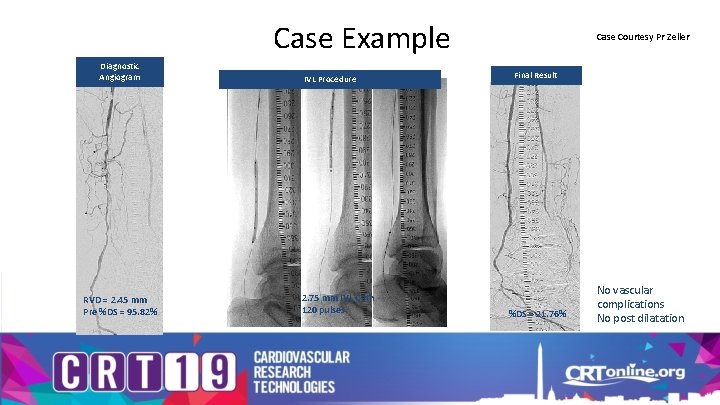
Case Example Diagnostic Angiogram RVD = 2. 45 mm Pre %DS = 95. 82% IVL Procedure 2. 75 mm IVL Cath 120 pulses Case Courtesy Pr Zeller Final Result %DS = 21. 76% No vascular complications No post dilatation
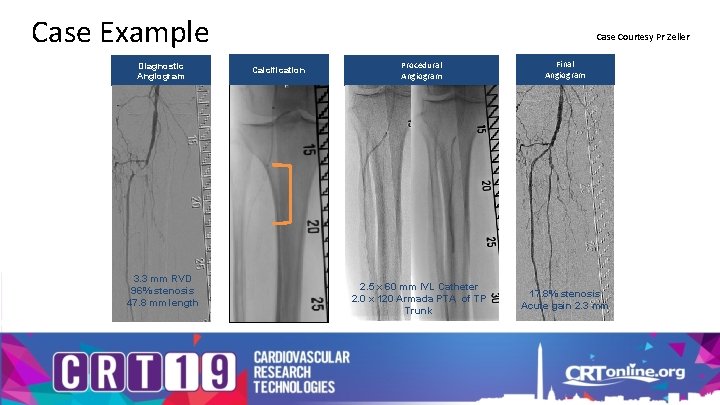
Case Example Diagnostic Angiogram 3. 3 mm RVD 96% stenosis 47. 8 mm length Case Courtesy Pr Zeller Calcification Procedural Angiogram Final Angiogram 2. 5 x 60 mm IVL Catheter 2. 0 x 120 Armada PTA of TP Trunk 17. 8% stenosis Acute gain 2. 3 mm

DISRUPT BTK: Summary • IVL is designed to treat both intimal and medial calcium allowing vessel expansion with minimal angiographic complications • Acute results show low residual stenosis with minimal vascular complications including no perforations, distal embolization, no reflow or abrupt closure • 30 day safety results report no MAE including revascularization or amputation. • Infrapopliteal results in a heavily calcified, CLI population are consistent with fempop IVL experience including low residual stenosis and minimal vascular complications.

Conclusion • POBA (+stent) BTK with high failure rate and RS • BTK arteries differ: more recoil, more calcium Vessel prep is needed • A lot of different approaches • Best way: unknown • Current studies: single arm, vs POBA, + DCB
- Slides: 27