Vertigo Simplified Gary Kroukamp Kingsbury Hospital Tygerberg Hospital

Vertigo Simplified Gary Kroukamp Kingsbury Hospital Tygerberg Hospital



At the end of this talk… • Define vertigo • Diagnose - just by the history • Refer • Investigate • Manage

Definitions Dizziness/lightheadedness: A distorted sense of one’s spatial relationship Vertigo: Hallucination of rotatory motion Unsteadiness: Difficulty with gait/Tendency to fall to one side Blackouts: Loss of consciousness Giddiness – Who the hell knows?
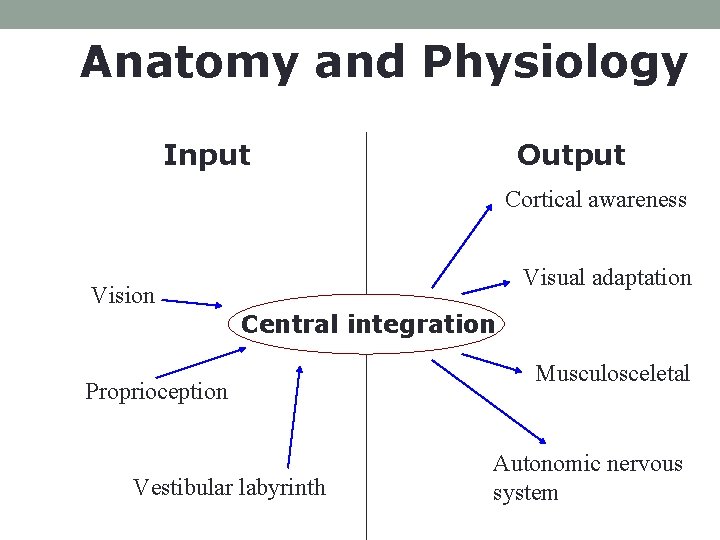
Anatomy and Physiology Input Output Cortical awareness Visual adaptation Vision Central integration Proprioception Vestibular labyrinth Musculosceletal Autonomic nervous system
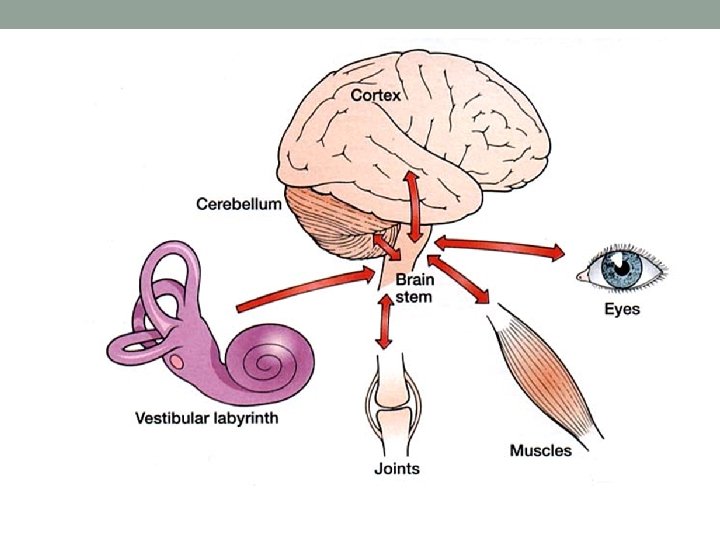

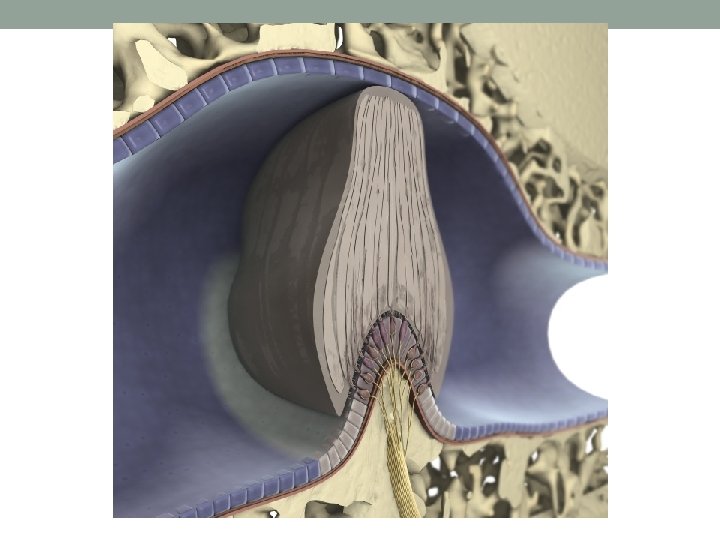
Anatomy and Physiology
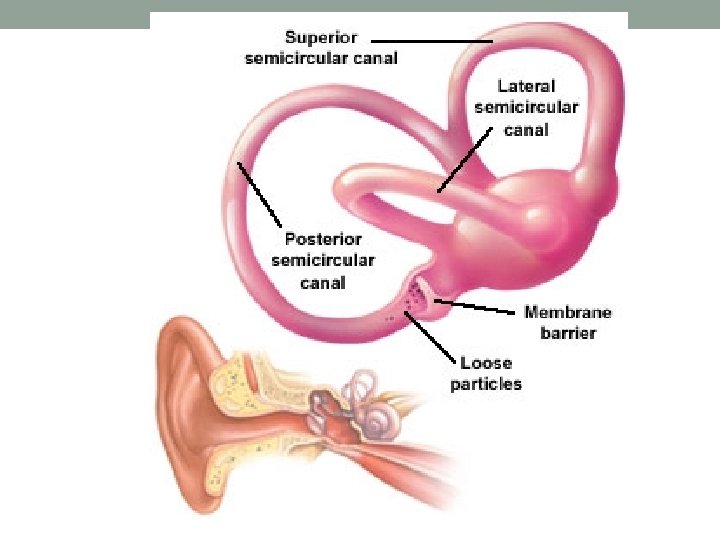
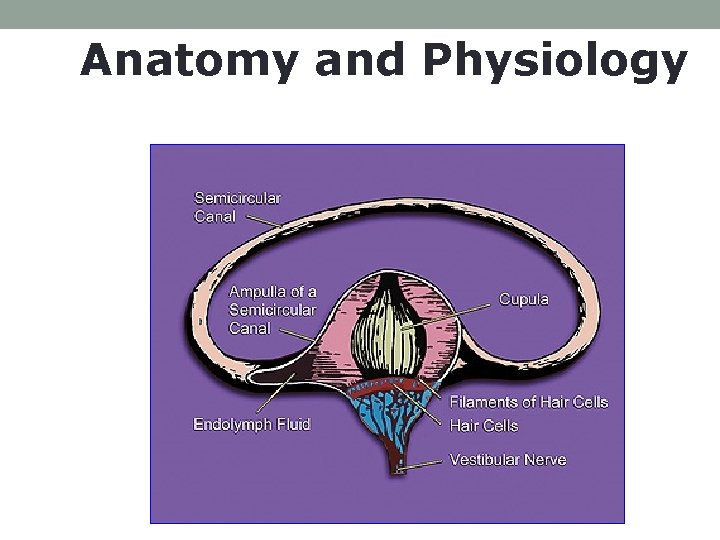
Anatomy and Physiology

History 1. 2. 3. 4. 5. 6. 7. Describing character of symptoms Onset – Sudden or Gradual Frequency Duration Severity Aggravating factors (activity, darkness) Associated symptoms (N+V, Tinnitus, Hearing loss) 8. Medical history (CVS, Psych, CNS) 9. Trauma 10. Medications/Alcohol
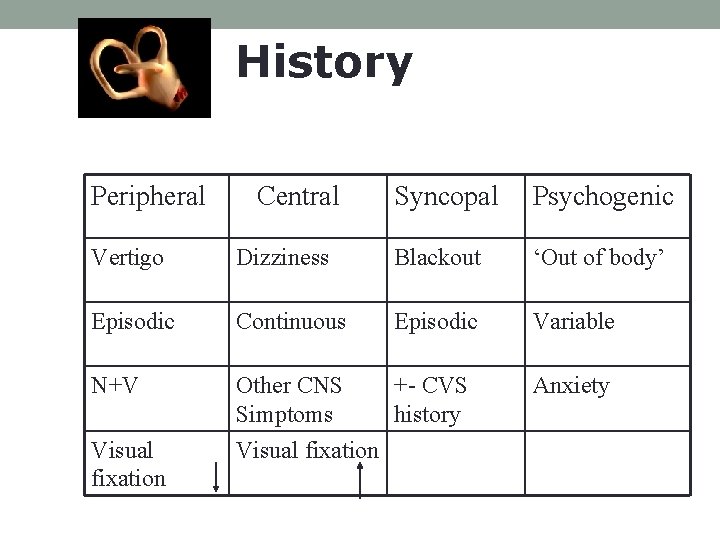
History Peripheral Central Syncopal Psychogenic Vertigo Dizziness Blackout ‘Out of body’ Episodic Continuous Episodic Variable N+V Other CNS Simptoms +- CVS history Anxiety Visual fixation
Examination 1. General 2. Vital signs 3. ENT -Middle ear disease, hearing(audiogram) 4. Neurologic -Cranial nerves, Cerebellum, Nystagmus 5. Cardiovascular -postural hypotension, pulse, carotid bruits, Cardiac murmurs 6. Manoeuvers -Hallpike

Special Investigations 1. FBC (Infection, leukemia) 2. VDRL, Bloodglucose, Thryroid functions 3. ECG (Arythmias, previous MI) 4. Electronystagmography, Videonystagmography 5. MRI

Causes Otological (Peripheral) vs Non-otological (Central)

Otological causes 1. External ear (Foreign body, impacted wax) 2. Middle ear disease 3. Trauma -Temporal bone fracture) 4. 5. 6. 7. Menière’s disease BPPV Labyrinthitis Vestibular neuronitis (Viral) 8. Other -Syphilis, Ototoxic drugs, Acoustic neuroma

Characteristics of Inner Ear Disorders • Dysequilibrium, not fainting • Definite attacks/episodes • “True vertigo” • Severe • Often with N & V • Other Inner Ear symptoms

Clinical Scenario 1 • Mrs JW • 59 years old • 3 week h/o dizziness • Some nausea, no vomiting • Wakes her up at night • Worse on rolling over to the left • Worse on reaching up to high shelf
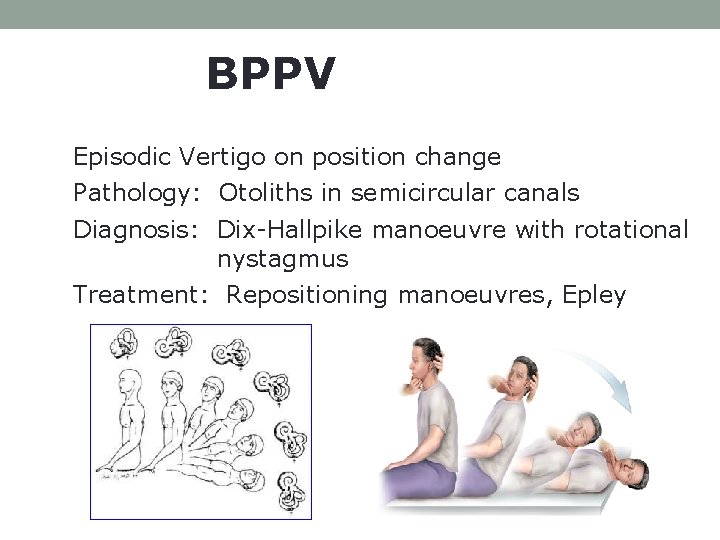
BPPV Episodic Vertigo on position change Pathology: Otoliths in semicircular canals Diagnosis: Dix-Hallpike manoeuvre with rotational nystagmus Treatment: Repositioning manoeuvres, Epley

Clinical Scenario 2 • Mr SP • 43 yo • Dizzy “attacks” for 3 years • 4 to 5 per year • Last 2 to 3 hours • N&V • Has to lie down • Tinnitus and muffled hearing left ear

Menière’s disease Endolymphatic hydrops 1. Young to middle age 2. Episodic attacks 3. Cardinal features -Vertigo, Tinnitus, Hearing loss, Fullness 4. Management - Reassurance and Vestibular sedatives - Reduction of Caffeine, smoking, salt, 3 L water - Medical -Serc, mild diuretics

Menière’s disease • Surgery now largely abandoned in favour of • Middle ear installation of Gentamycin • Middle ear installation of Steroids

Clinical scenario 3 • Mrs Rv. W • 36 yo • Sudden onset severe dizziness 2 days ago • N&V • Unable to stand/falls over • Normal hearing • Blurring of vision • Left beating nystagmus

Vestibular Neuronitis • Viral labyrinthitis • Nonspecific viral illness followed 6/52 by a sudden onset of vertigo, nausea + vomiting • Initially severe- gradual resolution over 10 days • Rx: Steroids • Vestibular suppressants

Labyrinthitis Infection of Vestibular labyrinth, associated with URTI Rapid onset vertigo with nystagmus and hearing loss First 24 hrs worse, normally resolve after 36 hrs

Clinical Scenario 4 • Mr AD • 74 yo man • Gradual onset hearing loss R ear – for years • Also tinnitus R ear • Vague poor balance • 1 episode vertigo 4 years ago • Hearing worse after this

Acoustic/Vestibular Schwannoma • Benign, slow-growing tumor in vestibular division of eighth cranial nerve • Not episodic vertigo • MRI with gadolinium is reliable +cost-effective • Rx: “Radiosurgery”Gamma knife/ Surgery

Characteristics of Central Causes • Continuous • Dysequilibrium more vague, not “True Vertigo” • Less severe imbalance, can still function

Non-otological (Central) 1. Vascular -Vertebrobasilar insufficiency, TIA, postural hypotension, Cardiac dysrythmias, Valvular lesions, Wallenberg syndrome, Medullary infarction, Internal auditory artery obstruction, Vertebrobasilar migraine, Subclavian Steel syndrome 2. Trauma -Head injury 3. Ageing -multifactorial 4. Infectious -Meningitis, Ramsay Hunt Syndrome

Non-otological (Central) 5. Demyelinating diseases eg. MS 6. Epilepsy 7. Toxic -Alcohol, Anticonvulsants 8. Psychogenic –Hyperventilation, Anxiety 9. Tumour 10. Metabolic -thyroid, hypo- and hyperglycaemia, Addison’s disease 11. Congenital -Familial episodic ataxia, Hydrocephalus, Arnold-Chiari malformation

Clinical Scenario 5 • Mrs TH • 28 yo • Poor balance and swaying 6 months • After a cruise Durban to Cape Town • Better with exercise • Better with alcohol

Mal de Debarquement Syndrome • After travel by ship • Improvement with exercise/alcohol • Psychogenic? /Anxiety • Overly focused on balance correction • Reassurance/exercise


Conclusion • History! • Clinical Picture • Not everyone has Meniere’s • Appropriate referral • Management according to diagnosis
- Slides: 36