Ventricular Tachycardia Ablation versus Enhanced Drug Therapy in

Ventricular Tachycardia Ablation versus Enhanced Drug Therapy in Structural Heart Disease (VANISH) Presenter: Emiliya Khazan, Pharm. D. PGY 2 Cardiology Pharmacy Resident West Palm Beach Veteran Affairs Medical Center Mentor: Kristen Campbell, Pharm. D. , BCPS (AQ-Cardiology) CPP Clinical Pharmacist & Senior Research Associate, Electrophysiology Director, PGY 2 Cardiology Residency Duke University Hospital DUMC 1

Disclosure Presenter has no conflicts of interest to report 2

Ventricular Tachycardia (VT) • Ventricular tachycardia post-MI is potentiated by re-entry circuits around conduction blocks in myocardial scar tissue • Significant risk for mortality in patients with structural heart disease (SHD) and reduced ejection fraction • Interventions – Implantable cardioverter defibrillator (ICD) • Restore normal rhythm – Antiarrhythmic drug (AAD) therapy • Suppress arrhythmia and reduce risk of recurrence – Catheter ablation • Eliminate arrhythmia 2006 ACC/AHA/ESC guidelines for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death. Journal of the American College of 3 Cardiology 48. 5 (2006): e 247 -e 346. Tung et al. Circulation. 2010; 122: e 389 -e 391.
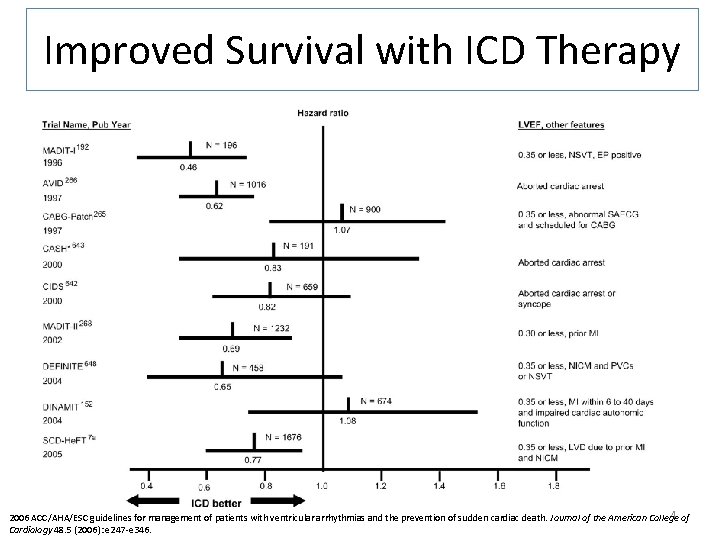
Improved Survival with ICD Therapy 4 of 2006 ACC/AHA/ESC guidelines for management of patients with ventricular arrhythmias and the prevention of sudden cardiac death. Journal of the American College Cardiology 48. 5 (2006): e 247 -e 346.

Antiarrhythmic Therapy • Most agents increase mortality risk in the setting of left ventricular dysfunction in absence of an ICD • Amiodarone reduces ventricular arrhythmias and cardiovascular mortality, but not all-cause mortality • Oral AAD options to reduce ICD shocks in patients with SHD • • Beta-blockers Amiodarone Sotalol Mexilitine Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614 Piccini JP et. al. European Heart Journal. 2009; 30(10): 1245 -53. Pacifico A et. al. N Engl J Med. 1999; 340(24): 1855 -62 Connolly SJ et. al. JAMA. 2006; 295(2): 165 -71 Little evidence exists to make specific recommendations for AAD in prevention and treatment of VT 5

Catheter Ablation • Alternative or adjunct to antiarrhythmic drug therapy for recurrent VT • SMASH-VT – ICD implant alone versus ICD implant with catheter ablation for secondary prevention (ICD events: 12% vs 33%; P=0. 007) – Patients were excluded if using AAD (Class I or Class III) • VTACH – ICD implant alone versus ICD implant with catheter ablation for secondary prevention (time to first recurrence: 5. 9 vs 18. 6 months) Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614 Reddy VY et. al. N Engl J Med. 2007; 357: 2657 -65. Kuck KH et. al. Lancet. 2010; 375(9708): 31 -40. 6

EHRA/HRS Expert Consensus on Catheter Ablation of Ventricular Arrhythmia: Indications in Structural Heart Disease Recommended • Symptomatic sustained monomorphic ventricular tachycardia, including VT terminated by an ICD, that recurs despite AAD therapy or when AAD not tolerated/desired • Recurrent sustained polymorphic VT/VF refractory to AAD with suspected trigger that can be targeted for ablation 7 2009 Consensus Document EHRA/HRS Expert Consensus on Catheter Ablation of Ventricular Arrhythmias. Europace 11. 6 (2009): 771 -817.
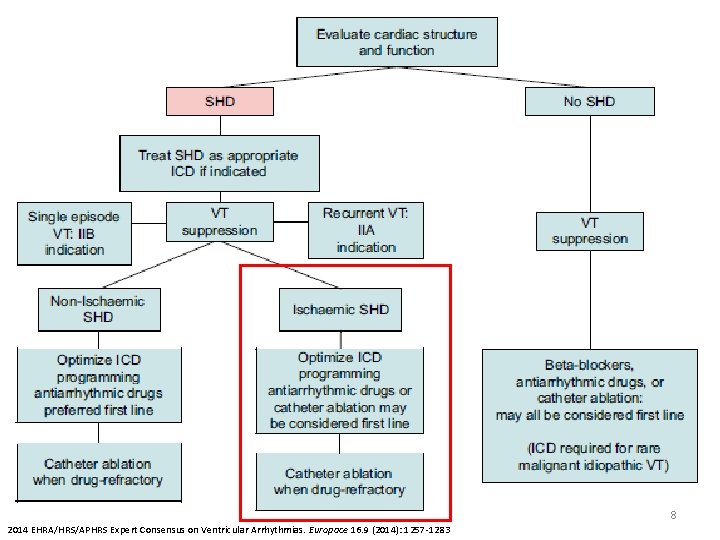
8 2014 EHRA/HRS/APHRS Expert Consensus on Ventricular Arrhythmias. Europace 16. 9 (2014): 1257 -1283

VANISH Trial HYPOTHESIS Catheter ablation is superior to aggressive AAD for recurrent VT Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614 9
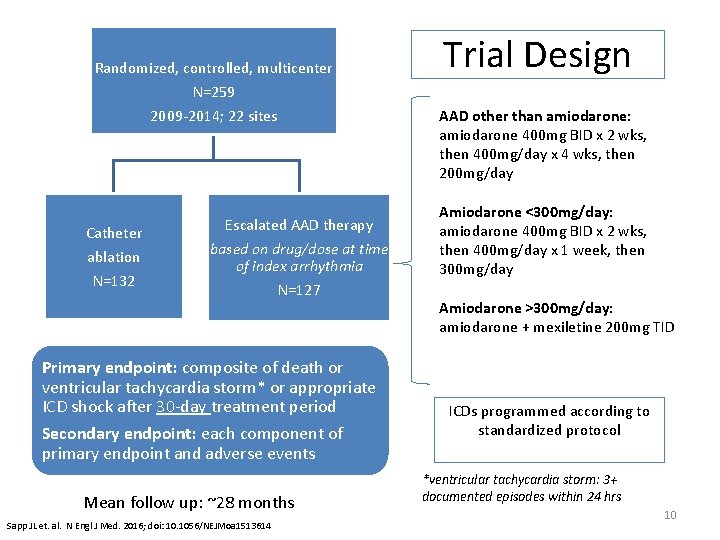
Randomized, controlled, multicenter N=259 2009 -2014; 22 sites Catheter ablation N=132 Escalated AAD therapy based on drug/dose at time of index arrhythmia N=127 Primary endpoint: composite of death or ventricular tachycardia storm* or appropriate ICD shock after 30 -day treatment period Secondary endpoint: each component of primary endpoint and adverse events Mean follow up: ~28 months Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614 Trial Design AAD other than amiodarone: amiodarone 400 mg BID x 2 wks, then 400 mg/day x 4 wks, then 200 mg/day Amiodarone <300 mg/day: amiodarone 400 mg BID x 2 wks, then 400 mg/day x 1 week, then 300 mg/day Amiodarone >300 mg/day: amiodarone + mexiletine 200 mg TID ICDs programmed according to standardized protocol *ventricular tachycardia storm: 3+ documented episodes within 24 hrs 10
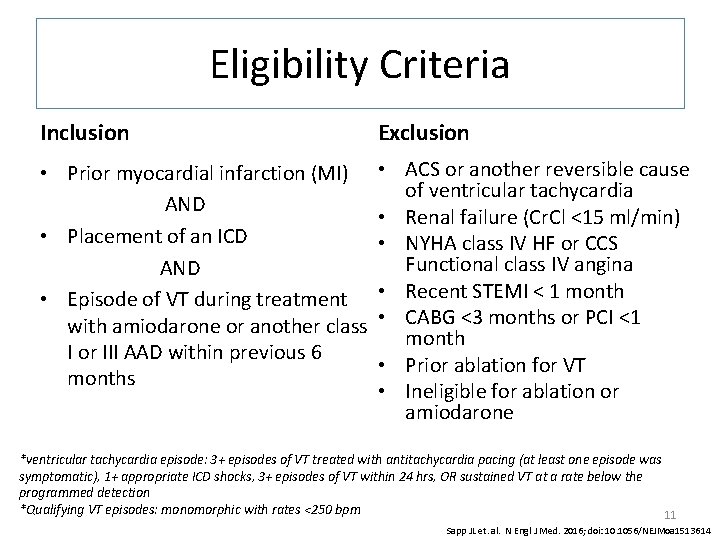
Eligibility Criteria Inclusion Exclusion • Prior myocardial infarction (MI) AND • Placement of an ICD AND • Episode of VT during treatment with amiodarone or another class I or III AAD within previous 6 months • ACS or another reversible cause of ventricular tachycardia • Renal failure (Cr. Cl <15 ml/min) • NYHA class IV HF or CCS Functional class IV angina • Recent STEMI < 1 month • CABG <3 months or PCI <1 month • Prior ablation for VT • Ineligible for ablation or amiodarone *ventricular tachycardia episode: 3+ episodes of VT treated with antitachycardia pacing (at least one episode was symptomatic), 1+ appropriate ICD shocks, 3+ episodes of VT within 24 hrs, OR sustained VT at a rate below the programmed detection *Qualifying VT episodes: monomorphic with rates <250 bpm 11 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614

Statistical Analysis • Intention-to-treat principle • Assumptions: primary outcomes in 35% of pts in escalated therapy group after 2 yrs – 260 pts provide 80% power to determine AR of 12. 25% lower in ablation group (RRR of 35%) – Primary outcome rate higher than expected at 63 months; thus, follow up cut to 1 yr which maintains power • Interim safety analysis at 6 month intervals • Survival-analysis techniques compared incidence of primary and secondary outcomes • Kaplan-Meier product-limit estimates • Cox proportional-hazards models Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614 12
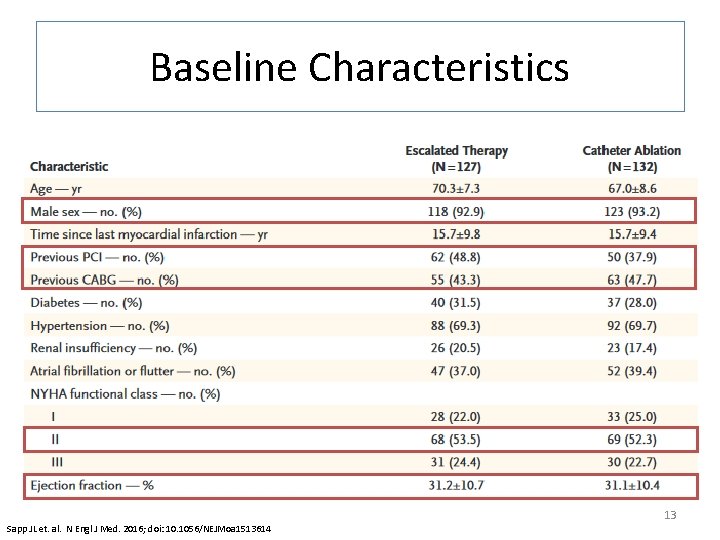
Baseline Characteristics 13 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
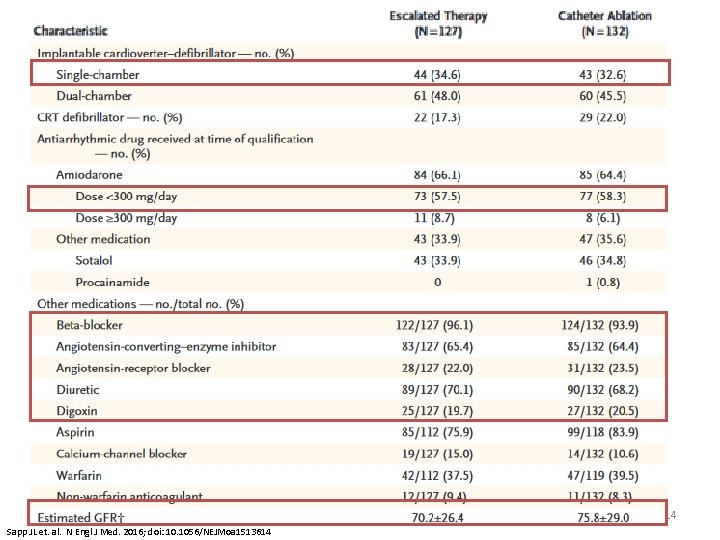
14 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
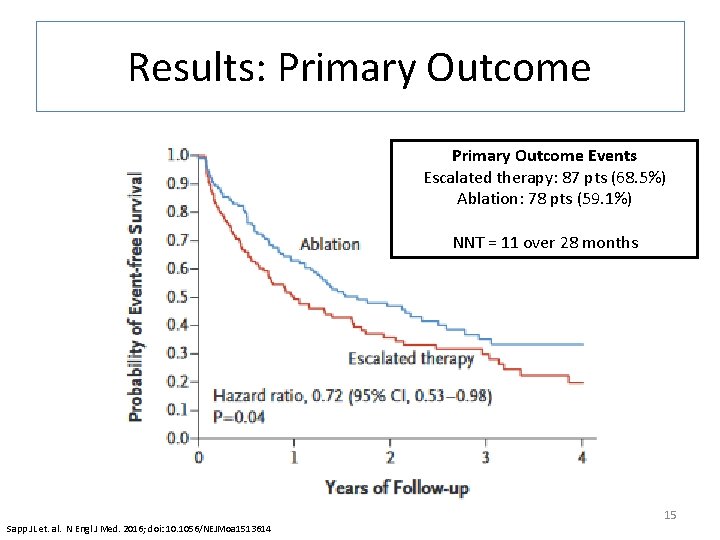
Results: Primary Outcome Events Escalated therapy: 87 pts (68. 5%) Ablation: 78 pts (59. 1%) NNT = 11 over 28 months 15 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
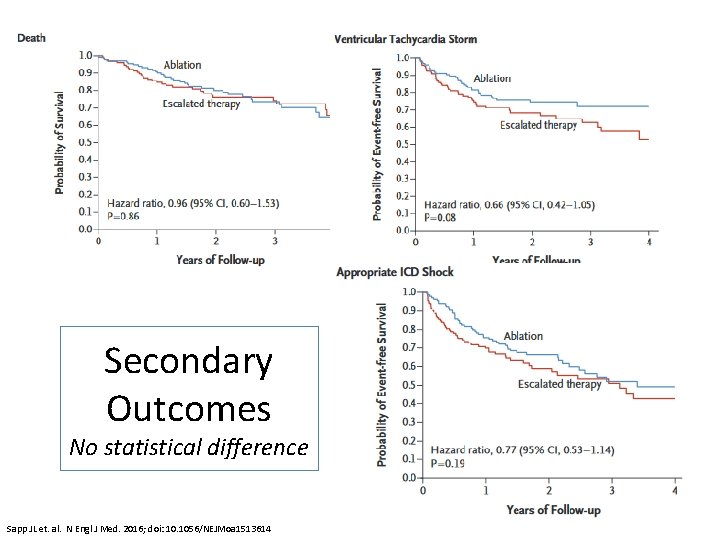
Secondary Outcomes No statistical difference 16 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
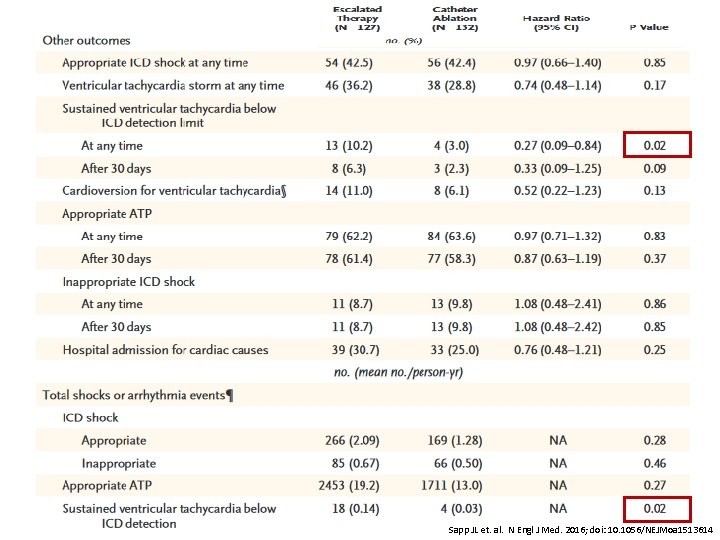
17 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
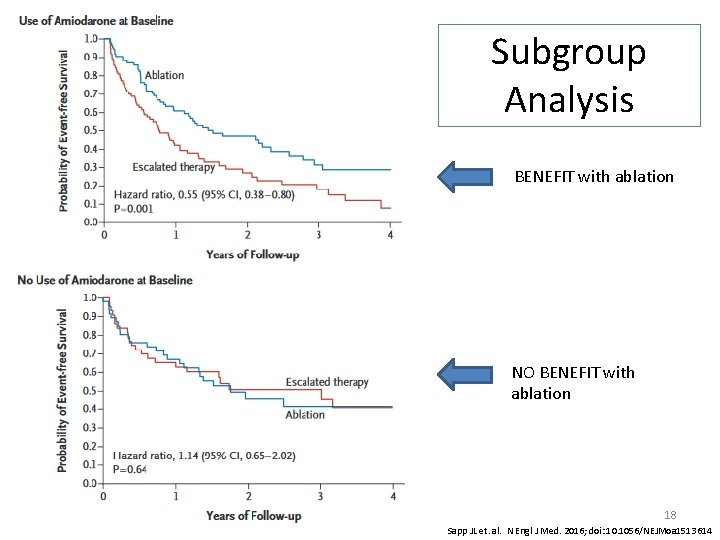
Subgroup Analysis BENEFIT with ablation NO BENEFIT with ablation 18 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614
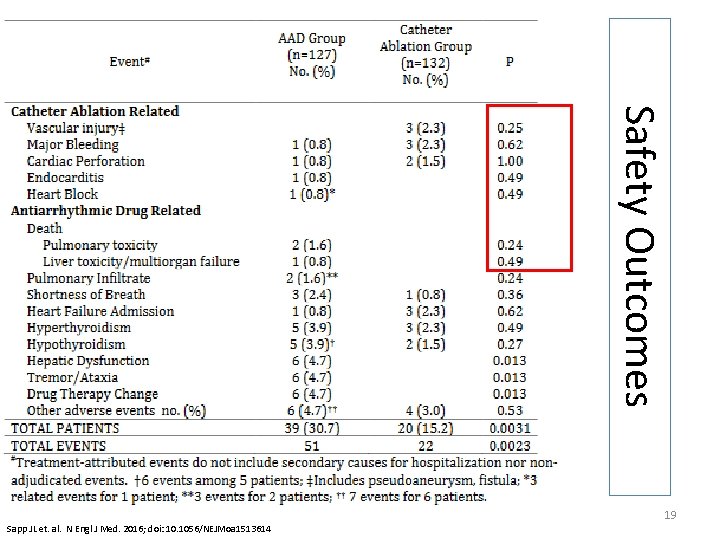
Safety Outcomes Adverse Events 19 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614

Conclusions • Ventricular tachycardia ablation was superior to escalation of antiarrhythmic therapy at reducing death, ventricular tachycardia storm, or ICD shocks • Treatment related adverse events were higher in the escalated-therapy group versus ablation 20 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614

Study Criticism Strengths • • Well designed Good follow up Standard ICD programming Canadian Institutes of Health Research involved in funding Limitations • May not generalize to unexperienced centers • New/improved ablation techniques since initiation of study • Mortality outcome was not powered • Small number of patients • Grant support and personal fees provided for author from manufacturer; author has patent on ablation method 21 Sapp JL et. al. N Engl J Med. 2016; doi: 10. 1056/NEJMoa 1513614

Considerations • Ablation offered no benefit in patients not on amiodarone at baseline • First 30 days excluded - appropriate for study design, but events still occurred • Death due to amiodarone toxicity may have been confounded by other disease states in these high risk patients • No deaths resulted from catheter ablation (generally safe) • Ablation will not eliminate the need for AAD (pts in ablation group continued baseline AAD) • Recurrence and death still very high; no decrease in mortality seen • Very high-risk patients/high disease burden • Unknown benefit of catheter ablation versus AAD for secondary prevention of VT in AAD naïve patients with an ICD 22

Acknowledgements Journal Club Mentor: • Kristen Campbell, Pharm. D. , BCPS (AQ-Cardiology) – CPP Clinical Pharmacist & Senior Research Associate, Electrophysiology Director, PGY 2 Cardiology Residency at Duke University Hospital DUMC Program Director: • Augustus Hough, Pharm. D. , BCPS-AQ Cardiology – Clinical Pharmacy Specialist – Cardiology, PGY 2 Cardiology Residency Director at West Palm Beach Veteran Affairs Medical Center ACCP Cardiology PRN Journal Club Coordinator: • Carrie S. Oliphant, Pharm. D. , FCCP, BCPS-AQ Cardiology – Cardiology/Anticoagulation Clinical Pharmacy Specialist at Methodist University Hospital ACCP Cardiology PRN Journal Club Facilitator: • Zachary Noel, Pharm. D. , BCPS – PGY 2 Cardiology Pharmacy Resident at University of Kentucky Healthcare 23

Ventricular Tachycardia Ablation versus Enhanced Drug Therapy in Structural Heart Disease (VANISH) Emiliya Khazan, Pharm. D. PGY 2 Cardiology Pharmacy Resident, West Palm Beach Veteran Affairs Medical Center West Palm Beach, FL 24
- Slides: 24